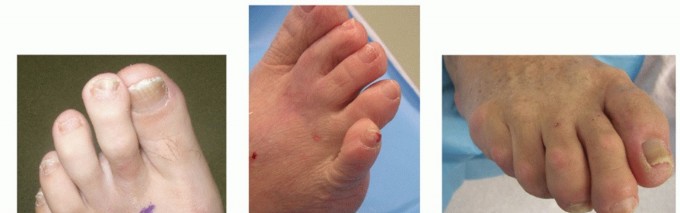
Resection Dermodesis and Revision Strategies for Hammer Toe Deformities
Key Takeaway
Resection dermodesis is a highly effective surgical technique for correcting rigid distal interphalangeal joint deformities in the lesser toes. This procedure combines a flexor digitorum longus tenotomy with bony resection and skin excision to achieve stable realignment. Careful preoperative planning, precise soft tissue handling, and appropriate intramedullary fixation are essential to minimize complications such as recurrent varus or valgus deformities and ensure optimal functional outcomes.
INTRODUCTION TO LESSER TOE DEFORMITIES AND RESECTION DERMODESIS
Lesser toe deformities, encompassing hammer toes, claw toes, and mallet toes, represent a complex spectrum of biomechanical imbalances involving the intrinsic and extrinsic musculature of the foot. A hammer toe is classically defined by an extension deformity at the metatarsophalangeal (MTP) joint and a flexion deformity at the proximal interphalangeal (PIP) joint, with the distal interphalangeal (DIP) joint remaining either extended or hyperextended. However, when rigid flexion deformities manifest at the DIP joint—often seen in severe mallet toes or complex multi-joint contractures—surgical intervention at the distal phalanx becomes mandatory.
Resection dermodesis is a highly reliable, time-tested surgical technique designed to address rigid DIP joint flexion deformities. The procedure synergizes three distinct surgical principles:
1. Soft Tissue Release: Tenotomy of the flexor digitorum longus (FDL) to eliminate the deforming plantarflexion force.
2. Bony Decompression: Resection of the middle phalanx head and neck to shorten the osseous column and relieve tension.
3. Dermodesis: Excision of a dorsal skin ellipse, utilizing the subsequent skin closure to act as a dynamic tension band that maintains the toe in a neutral, extended alignment.
This masterclass delineates the precise surgical steps of resection dermodesis, explores the biomechanical rationale behind the technique, and provides an exhaustive framework for managing complications and executing revision surgeries for failed hammer toe procedures.
SURGICAL ANATOMY AND BIOMECHANICS
A profound understanding of lesser toe anatomy is prerequisite for executing a flawless resection dermodesis and avoiding iatrogenic neurovascular injury.
The Extensor and Flexor Mechanisms
The stability of the lesser toes relies on a delicate equilibrium between the extrinsic tendons (extensor digitorum longus [EDL], extensor digitorum brevis [EDB], flexor digitorum longus [FDL], flexor digitorum brevis [FDB]) and the intrinsic musculature (lumbricals and interossei).
* Flexor Digitorum Longus (FDL): Inserts into the plantar base of the distal phalanx. In a rigid mallet or complex hammer toe, the FDL becomes contracted, tethering the DIP joint in acute flexion.
* Terminal Extensor Tendon: Formed by the convergence of the lateral slips of the extensor apparatus, it inserts into the dorsal base of the distal phalanx.
Neurovascular Anatomy
The plantar proper digital arteries and nerves course along the plantar-medial and plantar-lateral aspects of the toe, lying in close proximity to the flexor tendon sheath.
⚠️ Surgical Warning: Neurovascular Zones
When making the plantar transverse incision for the FDL tenotomy, the incision must be strictly confined to the central 5 to 6 millimeters of the flexion crease. Extending this incision laterally or medially risks transecting the proper digital neurovascular bundles, leading to a devastating ischemic or insensate distal digit.
PREOPERATIVE EVALUATION AND DECISION MAKING
Clinical Assessment
The cornerstone of preoperative evaluation is differentiating between flexible and rigid deformities.
* Flexible Deformities: Correct passively with manipulation or when the ankle is plantarflexed (indicating extrinsic tendon tightness). These may be amenable to percutaneous tenotomies or tendon transfers (e.g., Girdlestone-Taylor procedure).
* Rigid Deformities: Do not correct passively. Rigid DIP joint flexion necessitates bony resection and arthrodesis or dermodesis.
Radiographic Evaluation
Weight-bearing anteroposterior (AP), lateral, and oblique radiographs of the foot are mandatory. The surgeon must evaluate:
* The length of the metatarsals (to rule out a disproportionately long metatarsal driving the deformity).
* The congruency of the MTP joint (subluxation or dislocation must be addressed concurrently).
* The joint space and presence of osteoarthritis at the PIP and DIP joints.
SURGICAL TECHNIQUE: RESECTION DERMODESIS (STEP-BY-STEP)
The following technique outlines the classic approach to resection dermodesis, optimizing both exposure and deformity correction while minimizing soft tissue trauma.
1. Positioning and Hemostasis
- The patient is positioned supine on the operating table.
- A regional ankle block or Mayo block is typically sufficient, supplemented with monitored anesthesia care (MAC).
- A forefoot or ankle tourniquet is applied to ensure a bloodless surgical field, which is critical for identifying the delicate neurovascular structures of the digit.
2. Plantar Approach and FDL Tenotomy
- Incision: Make a precise 5- to 6-mm transverse incision directly within the plantar flexion crease of the DIP joint.
- Isolation: Carefully dissect through the subcutaneous fat. Avoid wandering medially or laterally to protect the neurovascular bundles.
- Tenotomy: Introduce a small, single-pronged hook (e.g., a skin hook or fine tenaculum) into the wound. Blindly sweeping is discouraged; visualize the glistening fibers of the FDL tendon. Hook the FDL, draw it into the wound, and sharply divide it with a #15 blade.
💡 Clinical Pearl: Timing of the Tenotomy
Performing the plantar FDL tenotomy before the dorsal bony resection is highly recommended. Releasing the deforming flexor force first allows the surgeon to accurately gauge the exact amount of bone that must be resected dorsally to achieve neutral alignment. If bone is resected first, the surgeon may inadvertently remove too much bone to overcome a tight, undivided FDL.
3. Dorsal Approach and Joint Exposure
- Incision: Center a dorsal, transverse, elliptical incision directly over the DIP joint. The width of the ellipse dictates the degree of dorsal skin tensioning (dermodesis) achieved upon closure.
- Skin Resection: Sharply excise the skin within the ellipse.
- Extensions: Create short (2- to 3-mm) longitudinal or slightly oblique extensions at the medial and lateral apices of the elliptical incision. This crucial step facilitates adequate exposure of the collateral ligaments without excessive skin retraction, which can cause marginal necrosis.
- Capsulotomy: Sharply divide the collateral ligaments, the terminal extensor tendon, and the dorsal capsule to completely mobilize the DIP joint.
4. Bony Resection
- Exposure: Acutely flex the distal phalanx to 90 degrees, delivering the head and neck of the middle phalanx into the dorsal wound.
- Resection: Using a microsaw or a sharp double-action bone rongeur, resect the head and neck of the middle phalanx. The cut should be perpendicular to the long axis of the phalanx.
- Alternative Distal Resection: If the deformity is exceptionally severe, or if a broader cancellous bone bed is desired for a formal arthrodesis, the articular base of the distal phalanx may also be removed using a small saw or rongeur.
5. Hemostasis and Preparation for Fixation
- If a tourniquet was utilized, it is often advisable to deflate it prior to closure to secure hemostasis, particularly if there is concern regarding the vascularity of the toe.
- Copiously irrigate the wound with sterile saline to remove bone debris, which can act as a nidus for infection or heterotopic ossification.
6. Intramedullary Fixation
- K-wire Insertion: Drive a 0.045-inch (1.14 mm) Kirschner wire (K-wire) antegrade through the center of the distal phalanx, exiting the tip of the toe just plantar to the nail bed.
- Retrograde Pinning: Reduce the DIP joint, ensuring neutral rotation and alignment. Drive the K-wire retrograde into the intramedullary canal of the middle phalanx. Depending on concurrent procedures (e.g., PIP joint arthroplasty), the wire may be advanced into the proximal phalanx.
7. Closure and Dermodesis
- Dorsal Closure: The dorsal elliptical defect is closed to create the "dermodesis" effect. Place a horizontal mattress suture (using 4-0 or 5-0 non-absorbable monofilament) in the center of the wound to perfectly evert the skin edges and provide maximum tension. Supplement with simple interrupted sutures on each side.
- Plantar Closure: Close the small plantar transverse wound with 1 or 2 simple interrupted sutures.
POSTOPERATIVE PROTOCOL
Meticulous postoperative care is as critical as the surgical execution to prevent pin tract infections and loss of correction.
- Immediate Postoperative Care: Apply a sterile, non-adherent dressing. The affected toe must be splinted to an adjacent, structurally sound toe (buddy taping) to maintain rotational stability and offload the K-wire.
- Weight-Bearing: Patients are typically allowed heel-weight-bearing or flat-foot weight-bearing in a rigid-soled postoperative shoe.
- Suture Removal: Sutures are removed at 14 days postoperatively, provided the incisions are fully epithelialized.
- Pin Management: The 0.045-inch K-wire is generally removed in the clinic at 3 to 4 weeks postoperatively.
- Continued Splinting: Following pin removal, the toe should remain buddy-taped with a soft dressing for an additional 1 to 2 weeks to allow the soft tissues to mature and the dermodesis to solidify.
COMPLICATIONS OF HAMMER TOE SURGERY
Despite meticulous technique, hammer toe surgery is fraught with potential complications. A less-than-perfect outcome demands a rigorous, analytical approach rather than immediate surgical re-intervention.
Analyzing the Failed Hammer Toe
Decision-making for a patient with a suboptimal outcome begins with a thorough clinical analysis. The surgeon must ask:
1. Were there unrealistic expectations? Patients must be counseled preoperatively that a surgically corrected toe will never be entirely "normal." It will be stiffer, potentially slightly thicker, and may have minor residual deviations.
2. What are the specific complaints? Is the issue pain, shoe-wear difficulty, or purely cosmetic?
3. Has sufficient time elapsed? Postoperative swelling and edema (the "sausage toe") can be protracted. The final size, shape, and contour of the toe are often not completely defined until 9 to 12 months postoperatively.
4. Where is the deformity located? Is the recurrence at the DIP, PIP, or MTP joint?
5. Is there satisfactory structural support? A revision procedure requires adequate remaining bone stock.
Common Complications
- Varus or Valgus Deformity at the PIP Joint: This is arguably the most common complication following PIP joint resection arthroplasty or arthrodesis. It frequently results from an overly aggressive, asymmetric resection of the proximal phalanx head, leading to collateral ligament incompetence and subsequent deviation.
- Bone Overgrowth: Inadequate resection or aggressive periosteal stripping can lead to hypertrophic bone formation at the resection site, causing a recurrent, painful prominence.
- Flail Toe: Excessive bone resection combined with failure to achieve soft tissue tensioning results in a floppy, functionless toe that retracts dorsally.
- Vascular Compromise: The dreaded "white toe" occurs due to arterial spasm, excessive tension on the neurovascular bundles (often from over-lengthening a chronically contracted toe), or direct surgical injury.
⚠️ Surgical Warning: The "White Toe" Protocol
If a toe appears ischemic postoperatively, immediate action is required. Remove all dressings. Place the foot in a dependent position. Apply warm compresses to the proximal limb to induce reflex vasodilation. If a K-wire is causing excessive longitudinal tension, it must be removed or backed out immediately. If ischemia persists, vascular surgery consultation and exploration may be warranted.
REVISION SURGERY FOR HAMMER TOE DEFORMITIES
When conservative measures (e.g., custom orthotics, extra-depth footwear, toe crests) fail to alleviate the symptoms of a failed hammer toe procedure, revision surgery may be indicated.
Prerequisites for Revision
Before addressing the interphalangeal joints, the surgeon must evaluate the metatarsophalangeal (MTP) joint. It is a fundamental rule of forefoot reconstruction that any MTP joint instability, subluxation, or dislocation must be corrected prior to, or concurrent with, revision of the toe deformity. Failure to stabilize the MTP joint (e.g., via a Weil osteotomy or plantar plate repair) will inevitably lead to recurrence of the distal deformity.
Techniques for Recurrent Deformity
Many of the primary procedures (resection arthroplasty, arthrodesis) can be utilized in a revision setting, but they must be tailored to the specific anatomical deficit.
The Role of Internal Stents
For recurrent deformities, particularly those complicated by bone loss or instability, an internal stent is highly effective in producing lasting deformity correction.
* Absorbable Intramedullary Devices: The use of bioabsorbable pins has gained significant traction in revision forefoot surgery. These devices provide rigid internal fixation without the need for percutaneous K-wires, thereby eliminating the risk of pin tract infections and the psychological burden of exposed hardware.
* Material Selection: The biomechanical properties of the implant matter. Research by Konkel et al. demonstrated improved clinical and radiographic results with the use of stiffer poly-L-lactate absorbable pins compared to the more flexible polydioxanone absorbable pins. The increased rigidity of poly-L-lactate provides superior resistance to the deforming forces of the intrinsic musculature during the critical early phases of bone and soft tissue healing.
Bone Grafting
In cases of severe flail toe with massive bone loss, structural interpositional bone grafting (using autograft from the calcaneus or allograft) may be required to restore the length and tension of the digital column. This is a technically demanding procedure that requires robust internal fixation, often utilizing specialized digital fusion plates or intramedullary compression screws.
CONCLUSION
Resection dermodesis remains an elegant, highly effective solution for rigid distal interphalangeal joint deformities. By combining a plantar flexor release with dorsal bony decompression and skin tensioning, the surgeon can achieve a stable, well-aligned digit. However, the margin for error in lesser toe surgery is narrow. Meticulous handling of the neurovascular structures, precise bony resection, and strict adherence to postoperative protocols are paramount.
When faced with complications, a systematic, patient-centric approach is required. Surgeons must allow adequate time for postoperative edema to resolve before declaring a failure. When revision surgery is necessary, addressing proximal MTP joint pathology and utilizing modern fixation techniques, such as poly-L-lactate intramedullary stents, can salvage complex deformities and restore both function and comfort to the patient's foot.
You Might Also Like