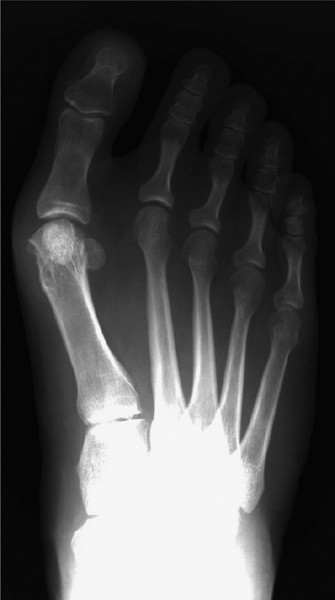
Proximal Chevron First Metatarsal Osteotomy: Comprehensive Surgical Guide
Key Takeaway
The proximal chevron first metatarsal osteotomy is a powerful surgical technique indicated for moderate-to-severe hallux valgus deformities. By utilizing a distally directed apex at the diaphyseal-metaphyseal junction, this osteotomy provides superior intrinsic biomechanical stability compared to traditional proximal crescentic cuts. Successful outcomes rely on meticulous lateral soft tissue release, precise 45-degree osteotomy execution, rigid internal screw fixation, and strategic capsulorrhaphy to restore the first ray's anatomic alignment and sesamoid articulation.
Introduction and Biomechanical Rationale
The proximal chevron first metatarsal osteotomy, prominently described and refined by Sammarco and Conti, is a highly effective surgical intervention for the correction of moderate-to-severe hallux valgus deformities. While distal osteotomies (such as the standard distal chevron) are generally reserved for mild-to-moderate deformities, severe metatarsus primus varus requires a proximal correction to achieve the necessary geometric translation and angular reduction of the first intermetatarsal (IM) angle.
Historically, the proximal crescentic osteotomy was the gold standard for severe deformities; however, it is inherently unstable in the sagittal plane, predisposing the first ray to dorsal elevation and subsequent transfer metatarsalgia. The primary biomechanical advantage of the proximal chevron osteotomy is its multiplanar stability. The V-shaped configuration, with its apex directed distally, provides significant intrinsic resistance to dorsal displacement and rotational forces. Furthermore, the broad cancellous surface area at the metaphyseal-diaphyseal junction promotes rapid and robust osseous union. Despite this inherent stability, rigid internal fixation with a lag screw or specialized pin is mandatory to maintain the corrected alignment during the critical early phases of bone healing.
Indications and Contraindications
Indications
- Moderate-to-Severe Hallux Valgus: Typically defined by a Hallux Valgus Angle (HVA) greater than 30 to 40 degrees.
- Increased Intermetatarsal Angle: An IM angle exceeding 13 to 15 degrees.
- Congruent or Incongruent First Metatarsophalangeal (MTP) Joint: Can be utilized in both scenarios, provided the distal soft tissue balancing is executed correctly.
- Adequate Bone Stock: Sufficient metaphyseal bone quality to support internal screw fixation.
Contraindications
- First Tarsometatarsal (TMT) Joint Hypermobility or Arthritis: In the presence of frank TMT instability or degenerative joint disease, a Lapidus procedure (first TMT arthrodesis) is the preferred alternative.
- Severe First MTP Joint Osteoarthritis: Warrants arthrodesis or arthroplasty rather than a joint-sparing osteotomy.
- Inadequate Vascularity: Peripheral arterial disease or compromised microcirculation.
- Active Infection: Absolute contraindication for any elective osteotomy.
Preoperative Planning and Patient Positioning
Thorough preoperative radiographic evaluation is essential. Standard weight-bearing anteroposterior (AP), lateral, and sesamoid axial views of the foot must be obtained. The surgeon should template the osteotomy to determine the exact degree of lateral translation required and to select the appropriate hardware length (typically a 4.0 mm partially threaded cancellous screw, approximately 34 mm in length).
The patient is placed in the supine position on the operating table. A well-padded calf or thigh tourniquet is applied to ensure a bloodless surgical field, which is critical for identifying delicate neurovascular structures and the precise anatomical attachments of the sesamoid apparatus. Intravenous prophylactic antibiotics are administered prior to tourniquet inflation.
Step-by-Step Surgical Technique
Incision and Deep Exposure
- Skin Incision: Following standard sterile preparation and draping, a 6-cm curvilinear incision is made along the medial aspect of the first ray. The incision begins at the level of the proximal phalanx medially, curves plantarward beneath the medial eminence (bunion) just above the glabrous skin of the sole, and continues proximally along the medial shaft of the first metatarsal. The incision terminates approximately 1 cm distal to the first metatarsocuneiform (TMT) joint.
- Tissue Dissection: Divide the deep tissues meticulously in line with the skin incision. Care must be taken to identify and protect the dorsal medial cutaneous nerve and the medial marginal vein.
- Capsulotomy: Create a dorsal and plantar capsular flap to expose the medial condyle of the first metatarsal head. Resect any redundant tissue from the dorsal flap to prevent postoperative impingement.
💡 Clinical Pearl: Incision Placement
Curving the incision slightly plantarward at the level of the MTP joint avoids placing the final scar directly over the medial prominence, reducing postoperative shoe-wear irritation and minimizing the risk of painful neuromas.
Medial Eminence Resection (Exostectomy)
- Identify the Sagittal Sulcus: Locate the sagittal groove (sulcus) on the distal metatarsal articular surface, which delineates the medial eminence from the true articular cartilage.
- Exostectomy: Using an oscillating microsaw, resect the exostosis exactly 1 mm medial to the sulcus. The saw blade should be directed in line with the medial cortex of the first metatarsal shaft.
⚠️ Surgical Warning: Over-resection
Avoid excessive resection of the medial eminence. Violating the sagittal sulcus or cutting into the metatarsal shaft can compromise the medial collateral ligament origin, leading to iatrogenic hallux varus and destabilizing the MTP joint.
Distal Soft Tissue Release and Sesamoid Mobilization
A critical component of this procedure is the transarticular lateral soft tissue release, which allows the sesamoid apparatus to reduce anatomically beneath the metatarsal head.
- Plantar Release: Release the proximal plantar capsular attachment at the metatarsal neck. This step is vital to mobilize the sesamoids, which are often rigidly contracted laterally in severe deformities.
- Joint Distraction: Apply longitudinal traction to the great toe while holding it in slight plantar flexion. Elevate the first metatarsal neck with a small bone hook to expose the fibular (lateral) sesamoid.
- Sesamoid Retraction: Working directly beneath the metatarsal head and neck, insert a skin hook or small retractor to grasp the lateral border of the fibular sesamoid, pulling it medially.
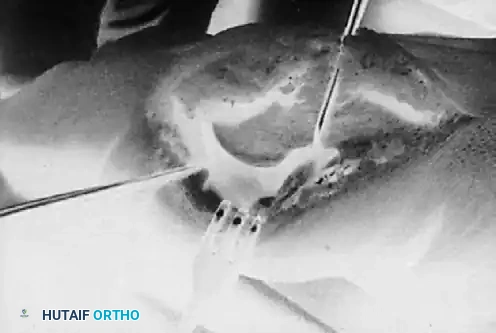
- Adductor Hallucis Release: Using sharp dissection, carefully detach the fibular sesamoid-metatarsal ligament. Identify the conjoined tendon of the adductor hallucis muscle inserting onto the lateral aspect of the sesamoid. Cut the fibers of the conjoined tendon under direct vision as they become taut.
- Neurovascular Protection: Applying continuous medial traction on the sesamoid pulls the lateral capsule and adductor tendon away from the first web space neurovascular bundle, protecting it from inadvertent injury during the release.
- Phalangeal Release: Release the fibers of the conjoined tendon longitudinally from the fibular sesamoid-phalangeal ligament and from their distal attachment to the base of the proximal phalanx.
- Lateral Capsulotomy: Extend the incision dorsally at the level of the proximal phalanx to release the contracted lateral capsule.
- Preserve the Transverse Ligament: Do not divide the deep transverse metatarsal ligament. Preserving this structure prevents postoperative splaying of the forefoot and maintains the structural integrity of the lesser metatarsal arch.
- Verification: Manipulate the hallux through a full range of motion to ensure that all tight lateral structures have been adequately released and that the toe can rest in a neutral or slightly varus position without tension.
Suture Anchor Preparation for Intermetatarsal Lashing
The Sammarco and Conti technique utilizes a unique "lashing" suture to dynamically hold the IM angle reduction and offload the proximal osteotomy during healing.
- Second Metatarsal Passage: Using a heavy cutting needle, percutaneously pass a large, non-absorbable braided polyester suture (e.g., #2 or #5 Dacron) around the lateral neck of the second metatarsal. The needle should emerge beneath the first metatarsal into the primary surgical wound.
- Suture Retrieval: Pass a curved hemostat over the first and second metatarsal necks, tunneling beneath the extensor hallucis longus and brevis tendons, to exit through the needle puncture wound. Grasp the free dorsal end of the suture with the hemostat and pull it medially beneath the skin and tendons, allowing it to emerge over the first metatarsal.
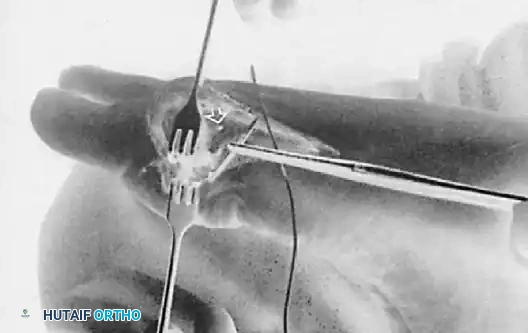
- First Metatarsal Drill Hole: Drill a 2-mm transverse hole through the dorsal half of the first metatarsal at the head-neck junction.
- Suture Placement: Using a suture passer, draw the deep (plantar) leg of the Dacron suture through this 2-mm drill hole from lateral to medial. The two ends of the suture are now staged medially, ready to be tied later in the procedure.
The Proximal Chevron Osteotomy
- Marking the Osteotomy: Identify the diaphyseal-metaphyseal junction of the proximal first metatarsal. The apex of the chevron cut must be directed distally.
- Executing the Cut: Using an oscillating saw, create a transverse chevron osteotomy with an exact angle of 45 degrees between the dorsal and plantar arms.
- Proximal Extension Limit: Ensure that the proximal arm of the osteotomy ends at least 1.5 cm distal to the metatarsocuneiform joint. Violating the TMT joint capsule can lead to degenerative arthritis and destabilize the base of the metatarsal.
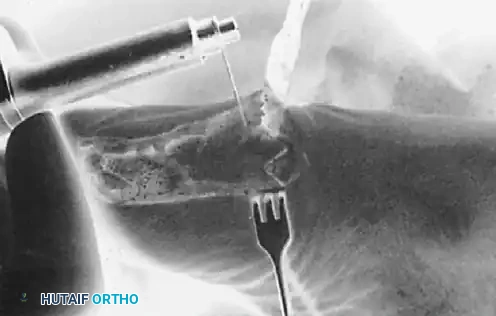
💡 Clinical Pearl: Osteotomy Angulation
Maintaining a precise 45-degree angle is critical. An angle that is too acute (e.g., 30 degrees) creates long, thin bone fragments that are prone to fracture during fixation. An angle that is too obtuse (e.g., 60-70 degrees) sacrifices the inherent multiplanar stability of the chevron geometry.
Deformity Correction and Internal Fixation
- Translation: Manually rotate and translate the distal fragment of the osteotomy laterally to correct the metatarsus primus varus (IM angle). The inherent V-shape will guide the translation while resisting dorsal elevation.
- Provisional Fixation: Once the desired correction is achieved, hold the osteotomy rigidly in place with a smooth 0.062-inch Kirschner wire (guide pin).
- Radiographic Confirmation: Utilize intraoperative fluoroscopy (image intensification) to verify the reduction of the IM angle, the alignment of the MTP joint, and the position of the guide pin.
- Screw Preparation: Prepare for the insertion of a 4.0-mm partially threaded cancellous screw (average length 34 mm).
- Countersinking: It is absolutely imperative to use a countersink on the near cortex before screw insertion. The proximal metaphyseal cortex is thin; failure to countersink will almost certainly result in a stress riser and longitudinal splitting of the metatarsal shaft when the screw head is seated.
- Screw Insertion: Insert the screw from the plantar aspect of the distal fragment, directing it laterally and dorsally across the osteotomy site into the proximal fragment. Ensure the screw threads fully bypass the osteotomy line to achieve interfragmentary compression. The screw must not cross the tarsometatarsal joint.
⚠️ Surgical Warning: Fixation Trajectory
Inserting the screw from plantar-distal to dorsal-proximal utilizes the biomechanical tension band principle. During weight-bearing, the plantar cortex is under tension. A plantar-based screw resists these tensile forces, preventing dorsal gapping of the osteotomy.
Medial Capsulorrhaphy and Soft Tissue Balancing
- Intermetatarsal Lashing: Before the final, definitive tightening of the osteotomy screw, tie the large Dacron "lashing" suture that was previously staged. Tying this suture pulls the first metatarsal laterally toward the second metatarsal, locking in the IM angle correction and shielding the osteotomy from excessive mechanical stress.
- Final Screw Tightening: Once the lashing suture is secure, perform the final tightening of the 4.0-mm screw. Re-check the construct with fluoroscopy to confirm proper screw positioning and partial reduction of the sesamoids.
- Capsular Closure: To fully correct the hallux valgus and anatomically reduce the sesamoids beneath the metatarsal head, perform a meticulous medial capsulorrhaphy.
- Suturing Technique: Use 2-0 absorbable mattress sutures. Place the sutures in a specific vector: from dorsal-distal to plantar-proximal. When tied, this vector dynamically derotates the hallux out of pronation, pulls the plantar capsular structures (and the embedded sesamoids) medially beneath the first metatarsal head, and corrects the valgus deviation.
Final Closure
- Irrigation: Thoroughly irrigate the wound with sterile saline to remove bone debris.
- Skin Closure: Close the skin incision using a running subcuticular 4-0 absorbable suture to optimize cosmetic outcomes.
- Dressing: Apply a sterile, mildly compressive dressing. The dressing should be applied in a manner that splints the great toe in a neutral, slightly plantarflexed, and slightly varus position to protect the medial capsular repair.
Postoperative Protocol and Rehabilitation
The postoperative management is designed to protect the osteotomy while it achieves clinical union, while simultaneously preventing stiffness of the first MTP joint.
- Weeks 0-2: The patient is placed in a rigid postoperative wooden clog or a specialized stiff-soled surgical shoe. Weight-bearing is strictly limited to the heel and the lateral border of the foot. The foot must be elevated strictly to minimize edema, which can compromise wound healing.
- Weeks 2-6: At the first postoperative visit (10-14 days), sutures are assessed (if non-absorbable were used) or the wound is checked. Radiographs are obtained to verify the maintenance of alignment and hardware integrity. The patient continues to use the rigid-soled shoe. Gentle, passive plantar flexion exercises of the MTP joint may be initiated to prevent capsular adhesions, but active dorsiflexion is restricted to protect the plantar soft tissue repair.
- Weeks 6-8: Clinical and radiographic union is typically observed around 6 weeks. Once bridging trabeculae are visible on radiographs and there is no tenderness at the osteotomy site, the patient may transition to a wide, supportive athletic shoe.
- Months 2-4: Physical therapy is escalated to include active range of motion, intrinsic foot muscle strengthening, and gait retraining. Full, unrestricted activity and return to high-impact sports are generally permitted between 4 to 6 months, depending on the patient's progress and bone healing.
Complications and Pitfalls
While highly successful, the proximal chevron osteotomy carries specific risks that the surgeon must actively mitigate:
- Dorsal Malunion (Elevation): The most common biomechanical failure. If the osteotomy is not rigidly fixed or if the patient bears weight prematurely on the forefoot, the distal fragment can elevate. This results in a loss of weight-bearing function of the first ray and subsequent transfer metatarsalgia to the lesser metatarsals.
- Avascular Necrosis (AVN) of the Metatarsal Head: Although less common with proximal osteotomies compared to distal ones, aggressive lateral soft tissue stripping combined with medial capsulotomy can disrupt the vascular ring of the metatarsal head. Meticulous, targeted dissection is required.
- Hallux Varus: Over-resection of the medial eminence, over-tightening of the medial capsule, or excessive lateral translation of the capital fragment can lead to iatrogenic hallux varus. The "dorsal-distal to plantar-proximal" capsular closure must be tensioned appropriately, not excessively.
- Cortical Blowout: Failure to countersink the proximal metaphyseal bone prior to screw insertion will cause the screw head to split the cortex, resulting in catastrophic loss of fixation.
-
Hardware Irritation: If the screw head is left proud on the plantar-medial aspect, it can cause significant pain during weight-bearing, necessitating hardware removal after osseous union is complete.
You Might Also Like