Surgical Management of Hallux Valgus: A Comprehensive Academic Guide
Key Takeaway
Hallux valgus is a complex triplanar deformity of the first ray requiring meticulous surgical correction. This comprehensive guide details the biomechanics, clinical evaluation, and step-by-step operative techniques for various osteotomies, including Chevron, Scarf, Ludloff, and Lapidus procedures. Designed for orthopedic residents and consultants, it provides evidence-based protocols, surgical pearls, and complication management strategies to optimize patient outcomes and restore forefoot kinematics.
Acknowledgment
The foundational principles and extensive bibliographic research underlying this chapter acknowledge the contributions of Dr. Brian G. Donley, who contributed significantly to this work during his tenure as a Foot Fellow at the Campbell Clinic. Dr. Donley subsequently established his practice at the Cleveland Clinic, Cleveland, Ohio, advancing the field of forefoot reconstruction.
Introduction to Hallux Valgus Pathoanatomy
Hallux valgus is not merely a prominent medial eminence but a complex, progressive triplanar deformity of the first ray. It is characterized by lateral deviation and pronation of the hallux, medial deviation of the first metatarsal, and lateral subluxation of the sesamoid apparatus.
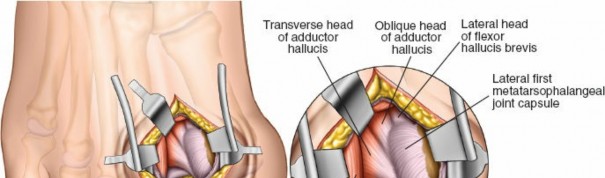
As the first metatarsal drifts medially, the abductor hallucis tendon plantarflexes and rotates beneath the metatarsal head, losing its abductor function. The adductor hallucis and the lateral head of the flexor hallucis brevis (FHB) become deforming forces, tethering the proximal phalanx and sesamoids laterally. This biomechanical cascade disrupts the windlass mechanism, leading to transfer metatarsalgia and progressive forefoot collapse.
Clinical Pearl: The sesamoids do not subluxate laterally; rather, the first metatarsal deviates medially off the sesamoid apparatus, which remains tethered to the second metatarsal via the deep transverse metatarsal ligament.
Clinical and Radiographic Evaluation
A rigorous preoperative assessment is mandatory to select the appropriate surgical intervention. Weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are standard.
Key Radiographic Parameters
- Hallux Valgus Angle (HVA): The angle between the longitudinal axes of the first metatarsal and proximal phalanx. Normal is <15°.
- Intermetatarsal Angle (IMA): The angle between the longitudinal axes of the first and second metatarsals. Normal is <9°.
- Distal Metatarsal Articular Angle (DMAA): The relationship of the articular surface of the first metatarsal head to its longitudinal axis. Normal is <10°. An increased DMAA indicates a congruent deformity requiring specific intra-articular or extra-articular correction.
- Sesamoid Station: Evaluated on the AP view (Hardy and Clapham classification) to determine the degree of lateral subluxation relative to the first metatarsal bisector.
Surgical Decision-Making Algorithm
The choice of procedure is dictated by the severity of the deformity, the presence of first tarsometatarsal (TMT) hypermobility, and the congruency of the first metatarsophalangeal (MTP) joint.
- Mild Deformity (HVA <30°, IMA <13°): Distal metatarsal osteotomy (e.g., Chevron) with distal soft tissue release.
- Moderate Deformity (HVA 30°-40°, IMA 13°-20°): Diaphyseal osteotomy (e.g., Scarf, Ludloff) or proximal osteotomy (e.g., Crescentic) combined with distal soft tissue release.
- Severe Deformity (HVA >40°, IMA >20°): Proximal osteotomy or first TMT arthrodesis (Lapidus procedure).
- Hypermobile First Ray: First TMT arthrodesis (Lapidus procedure).
- Hallux Rigidus with Valgus: First MTP joint arthrodesis.
Preoperative Positioning and Setup
- Anesthesia: Regional anesthesia (popliteal block or ankle block) combined with monitored anesthesia care (MAC) or general anesthesia.
- Positioning: Supine with a bump under the ipsilateral hip to internally rotate the leg to a neutral position, ensuring the foot rests flat on the operating table.
- Tourniquet: A calf or thigh tourniquet is applied. Exsanguination is performed using an Esmarch bandage prior to inflation (typically 250-300 mmHg).
Surgical Approaches and Techniques
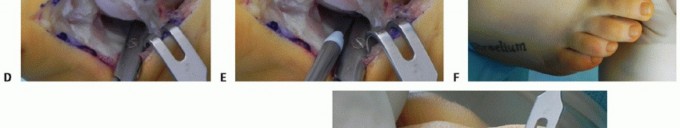
1. Distal Soft Tissue Release (Modified McBride)
The distal soft tissue release is foundational to nearly all hallux valgus corrections. It addresses the lateral tethering structures.
Step-by-Step Technique:
1. Incision: A dorsal first web space incision is made, taking care to protect the terminal branches of the deep peroneal nerve.
2. Dissection: Deepen the incision to identify the adductor hallucis tendon inserting onto the base of the proximal phalanx and the fibular sesamoid.
3. Release: Transect the adductor hallucis tendon at its insertion. Release the deep transverse metatarsal ligament connecting the first and second metatarsal heads.
4. Sesamoid Mobilization: Release the lateral sesamoid suspensory ligament. Ensure the fibular sesamoid is mobile.
5. Capsulotomy: Perform a lateral capsulotomy of the first MTP joint if severe contracture persists.
Surgical Pitfall: Routine excision of the fibular sesamoid should be avoided, as it significantly increases the risk of iatrogenic hallux varus and alters the biomechanics of the FHB.
2. Distal Chevron Osteotomy
Indicated for mild to moderate deformities. It is a V-shaped, horizontally directed displacement osteotomy of the metatarsal head.
Step-by-Step Technique:
1. Medial Approach: A medial longitudinal incision is made over the first MTP joint.
2. Capsulotomy: An inverted L-shaped or longitudinal medial capsulotomy is performed.
3. Exostectomy: The medial eminence is resected parallel to the medial border of the foot, preserving the sagittal groove to avoid "staking the head."
4. Osteotomy: A 0.045-inch K-wire is driven centrally into the metatarsal head to mark the apex. A microsaw is used to create a 60-degree V-osteotomy, with the dorsal arm exiting proximal to the articular cartilage and the plantar arm exiting proximal to the sesamoids.
5. Translation: The capital fragment is translated laterally by 30% to 50% of the metatarsal width.
6. Fixation: The osteotomy is secured with a single 2.5 mm or 3.0 mm headless compression screw or K-wires.
7. Closure: The medial capsule is imbricated to correct pronation and secure the medial repair.
Surgical Pearl: Ensure the apex of the Chevron cut is central within the metatarsal head. If placed too dorsally, the plantar fragment becomes unstable; if too plantar, the dorsal fragment is prone to avascular necrosis (AVN).
3. Scarf (Diaphyseal) Osteotomy
The Scarf osteotomy is a versatile Z-step cut in the diaphysis, allowing for significant lateral translation, shortening, or lengthening, and correction of the DMAA.
Step-by-Step Technique:
1. Exposure: An extended medial longitudinal incision exposes the entire first metatarsal shaft.
2. Osteotomy Design: The longitudinal cut is made in the mid-diaphysis, parallel to the plantar aspect of the foot. The dorsal transverse cut is made distally, and the plantar transverse cut is made proximally.
3. Displacement: The plantar-distal fragment is translated laterally. If DMAA correction is required, the distal fragment can be rotated medially.
4. Fixation: Two cortical screws (typically 2.5 mm or 3.0 mm) are placed from dorsal to plantar to secure the osteotomy.
5. Contouring: The overhanging medial cortical bone of the proximal fragment is resected flush with the translated distal fragment.
Surgical Pitfall: "Troughing" occurs when the hard cortical bone of the translated fragment collapses into the softer cancellous bone of the metaphysis, leading to unintended elevation (dorsiflexion) of the first ray and subsequent transfer metatarsalgia.
4. First Tarsometatarsal Arthrodesis (Lapidus Procedure)
The Lapidus procedure is the gold standard for severe hallux valgus, especially in the presence of first ray hypermobility or TMT joint arthritis.
Step-by-Step Technique:
1. Incision: A dorsal incision is made over the first TMT joint, lateral to the extensor hallucis longus (EHL) tendon.
2. Joint Preparation: The capsule of the first TMT joint is incised. The articular cartilage of the base of the first metatarsal and the medial cuneiform is meticulously resected using a saw, osteotomes, or curettes. Subchondral bone is fenestrated to promote arthrodesis.
3. Correction: The first metatarsal is translated laterally and plantarflexed to correct the IMA and restore the medial longitudinal arch. Pronation of the hallux is corrected by supinating the metatarsal.
4. Fixation: Rigid fixation is achieved using crossed compression screws (e.g., 3.5 mm or 4.0 mm), a dorsal or medial locking plate, or a combination of both.
5. Bone Grafting: Local autograft from the medial eminence resection can be packed into the arthrodesis site.
5. Proximal Phalangeal Osteotomy (Akin Procedure)
The Akin osteotomy is an adjunctive procedure, rarely used in isolation. It is a medial closing-wedge osteotomy of the proximal phalanx indicated for hallux valgus interphalangeus or residual clinical valgus after metatarsal correction.
Step-by-Step Technique:
1. Exposure: The medial incision is extended distally over the proximal phalanx.
2. Osteotomy: A medial closing wedge is created 5 to 10 mm distal to the MTP joint line. The lateral cortex must remain intact to act as a hinge.
3. Closure and Fixation: The osteotomy is closed, correcting the valgus, and secured with a staple, K-wire, or headless compression screw.
Postoperative Protocols
Rehabilitation protocols vary based on the stability of the osteotomy or arthrodesis.
- Distal Osteotomies (Chevron): Patients are typically allowed immediate heel-weight-bearing in a rigid postoperative shoe. Dressings are changed at 2 weeks, and toe spica taping is maintained for 6 weeks to protect the medial capsular repair.
- Diaphyseal/Proximal Osteotomies (Scarf, Ludloff): Protected weight-bearing in a CAM boot for 4 to 6 weeks, depending on radiographic evidence of healing.
- Lapidus Procedure: Strict non-weight-bearing for 2 to 4 weeks, followed by progressive weight-bearing in a CAM boot for an additional 4 weeks. Radiographic consolidation must be confirmed before transitioning to regular footwear.
- Physical Therapy: Active and passive MTP joint range of motion exercises are initiated at 2 to 4 weeks (except in MTP arthrodesis) to prevent arthrofibrosis.
Complications and Salvage Strategies
1. Iatrogenic Hallux Varus
Hallux varus is a devastating complication resulting from overcorrection. Causes include aggressive medial eminence resection ("staking the head"), over-tightening of the medial capsule, complete fibular sesamoidectomy, or excessive lateral translation of the metatarsal head.
* Management: Flexible deformities may be treated with soft tissue reconstruction (e.g., EHL transfer under the deep transverse metatarsal ligament). Rigid deformities or those with MTP joint arthrosis require first MTP joint arthrodesis.
2. Avascular Necrosis (AVN) of the Metatarsal Head
AVN is a risk when a distal osteotomy is combined with an extensive lateral soft tissue release, which can disrupt the intraosseous and extraosseous blood supply to the capital fragment.
* Management: Conservative management includes offloading. Severe collapse with secondary arthrosis necessitates first MTP joint arthrodesis.
3. Recurrence of Deformity
Recurrence is often due to undercorrection of the IMA, failure to address a hypermobile first ray, or inadequate medial capsular imbrication.
* Management: Revision surgery must address the underlying biomechanical failure, often requiring a more proximal procedure such as a Lapidus arthrodesis.
4. Nonunion and Malunion
Nonunion is most common following the Lapidus procedure or proximal osteotomies. Malunion (typically dorsiflexion elevation of the first ray) leads to transfer metatarsalgia.
* Management: Symptomatic nonunions require revision arthrodesis with bone grafting and rigid plate fixation. Dorsiflexion malunions may require a plantarflexing opening wedge osteotomy or revision arthrodesis.
Key Academic References
The evidence-based protocols detailed in this chapter are supported by extensive orthopedic literature, including but not limited to:
- Acevedo JI, et al. Mechanical comparison of cyclic loading in five different first metatarsal shaft osteotomies. Foot Ankle Int 23:711, 2002.
- Akin OF. The treatment of hallux valgus: a new operative procedure and its results. Med Sentinel 33:678, 1925.
- Barouk LS. Scarf osteotomy for hallux valgus correction. Local anatomy, surgical technique, and combination with other forefoot procedures. Foot Ankle Clin 5:525, 2000.
- Coetzee JC, et al. The Lapidus procedure as salvage after surgical treatment of hallux valgus: a prospective cohort study. J Bone Joint Surg 86A:60, 2003.
- Coughlin MJ. Hallux valgus. J Bone Joint Surg 78A:932, 1996.
- Johnson KA, et al. Chevron osteotomy for hallux valgus. Clin Orthop Relat Res 142:44, 1979.
- Mann RA, Coughlin MJ. Arthrodesis of the first metatarsophalangeal joint as salvage for the failed Keller procedure. J Bone Joint Surg 69A:68, 1987.
You Might Also Like