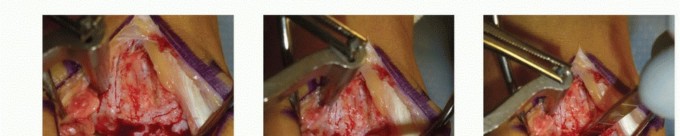
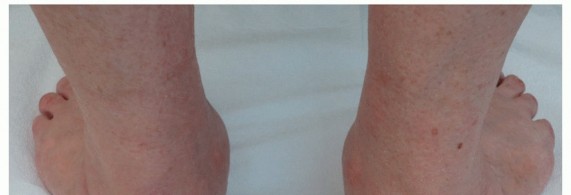
Febrile Foot Ulcers: A Deep Dive into Diagnosis, Surgical Anatomy, and Indications for Orthopedic Management
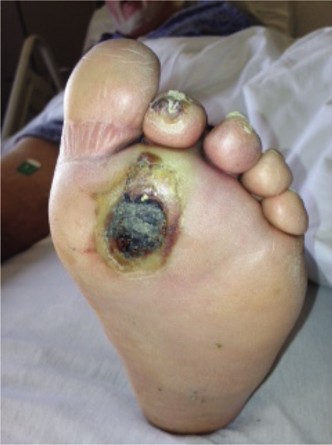
Key Takeaway
Febrile foot ulcers signal systemic infection, often indicating deep space infection or osteomyelitis, particularly in diabetic patients. Orthopedic management involves prompt diagnosis using clinical signs, elevated ESR/CRP, and advanced imaging. Surgical intervention is crucial for source control, especially with abscesses, confirmed osteomyelitis, or necrotizing fasciitis, requiring a thorough understanding of foot anatomy and biomechanics.
Introduction & Epidemiology
Foot ulcers, particularly those in patients with diabetes mellitus, represent a significant global health burden, frequently leading to infection, osteomyelitis, and ultimately, limb amputation. The lifetime risk of developing a diabetic foot ulcer (DFU) is estimated to be between 15% and 25%, with approximately 50% of these ulcers becoming infected. Infection is the most common precipitating factor for lower extremity amputation in patients with diabetes. The presence of fever in a patient with a foot ulcer is a cardinal sign of systemic infection and demands immediate and thorough investigation for deep space infection or osteomyelitis.
The pathogenesis of DFUs is multifactorial, encompassing neuropathy (sensory, motor, and autonomic), peripheral artery disease (PAD), and immunocompromise. Sensory neuropathy abrogates protective sensation, leading to repetitive microtrauma. Motor neuropathy results in muscle atrophy and intrinsic muscle imbalance, predisposing to foot deformities (e.g., Charcot arthropathy, hammer toes) and abnormal pressure points. Autonomic neuropathy compromises sweat gland function, leading to dry, fissured skin prone to breakdown. PAD impairs healing and exacerbates infection severity.
The diagnostic challenge lies in differentiating superficial soft tissue infection (cellulitis) from deep space infection, abscess formation, or underlying osteomyelitis. Clinical signs of inflammation can be blunted in neuropathic feet. Systemic inflammatory markers, such as the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP), play a crucial role in risk stratification and guiding further diagnostic evaluation. While non-specific, an elevated ESR (typically >70 mm/hr, though thresholds vary) in the context of a febrile foot ulcer significantly increases the pre-test probability of osteomyelitis, necessitating advanced imaging and potentially bone biopsy. Conversely, a normal ESR and CRP can often rule out osteomyelitis in the absence of other strong clinical indicators.
Surgical Anatomy & Biomechanics
A thorough understanding of foot anatomy and biomechanics is paramount for effective surgical management of infected foot ulcers. The foot is a complex structure designed for weight-bearing, propulsion, and adaptation to uneven surfaces.
Cutaneous and Subcutaneous Structures
The skin of the plantar foot is thick and specialized for protection against shear and pressure. Areas most prone to ulceration are those subjected to high peak pressures, such as the plantar aspects of the metatarsal heads, the hallux, the heel, and the dorsal aspects of hammertoes. Neuropathy compromises the integrity of this protective barrier, leading to breakdown. The subcutaneous layer can facilitate rapid spread of infection, particularly in the plantar spaces.
Musculoskeletal Anatomy
The foot comprises 26 bones, 33 joints, and over 100 muscles, tendons, and ligaments.
*
Bones:
Tarsals (talus, calcaneus, navicular, cuboid, cuneiforms), metatarsals, and phalanges. Osteomyelitis most commonly affects the metatarsal heads, phalanges, and calcaneus, often through direct contiguous spread from an overlying ulcer.
*
Joints:
The intricate network of joints (e.g., ankle, subtalar, midtarsal, MTP, IP) provides flexibility and shock absorption. Septic arthritis can occur, often as an extension of adjacent osteomyelitis.
*
Muscles and Tendons:
Extrinsic muscles originate in the leg and insert in the foot (e.g., tibialis anterior, Achilles tendon), while intrinsic muscles are entirely within the foot (e.g., lumbricals, interossei). Neuropathic atrophy of intrinsic muscles contributes to clawing and hammertoe deformities, shifting weight to the metatarsal heads. Tendon sheath infections can track proximally.
Neurovascular Bundles
The foot's neurovascular supply is critical for tissue viability and healing.
*
Arterial Supply:
Primarily from the posterior tibial artery (medial and lateral plantar arteries) and anterior tibial artery (dorsalis pedis artery). Peripheral artery disease significantly impairs the ability of the foot to heal wounds and clear infection. Adequate perfusion is a prerequisite for successful surgical intervention and wound healing.
*
Nerves:
The tibial nerve (medial and lateral plantar nerves) and deep/superficial fibular nerves provide sensation and motor function. Neuropathy renders the foot insensate, preventing awareness of trauma or infection.
Biomechanics of Weight Bearing
Pathologic biomechanics, often a consequence of motor neuropathy and deformity (e.g., Charcot neuroarthropathy), leads to abnormally high plantar pressures. These sustained pressures, coupled with repetitive shear forces, cause tissue ischemia and breakdown, initiating the ulceration process. Surgical correction of deformities and offloading strategies are crucial to prevent recurrence.
Indications & Contraindications
The decision for operative intervention in a febrile foot ulcer complicated by infection is nuanced and requires careful consideration of the patient's overall health, the extent of local pathology, and the potential for limb salvage.
Indications for Operative Management
Surgical intervention is indicated when non-operative measures fail or when the severity of infection demands immediate source control.
- Deep Space Infection/Abscess: Clinically evident fluctuance, spreading cellulitis with systemic signs, or imaging (MRI, ultrasound) confirming purulent collection.
-
Osteomyelitis:
- Confirmed osteomyelitis: Via positive bone biopsy cultures and/or histopathology.
- Highly suspected osteomyelitis: Based on clinical findings (probe-to-bone test positive), elevated ESR/CRP, characteristic imaging changes (X-ray, MRI, bone scan).
- Failed medical management: Persistent infection despite appropriate antibiotic therapy.
- Necrotizing Fasciitis: A surgical emergency requiring immediate and aggressive debridement to prevent rapid tissue destruction and systemic sepsis.
- Wound Debridement: Extensive necrotic tissue, gangrene, or non-viable soft tissue that impedes healing and serves as a nidus for infection.
- Structural Deformity Requiring Correction: If an underlying foot deformity (e.g., Charcot foot, severe hammertoe) is the primary cause of recurrent ulceration and infection, surgical correction may be indicated for definitive limb salvage.
- Critical Limb Ischemia: While not directly for ulcer management, revascularization procedures (endovascular or open bypass) are often prerequisite to allow healing of infected ulcers in ischemic limbs.
- Systemic Sepsis with Local Source: Any foot infection causing systemic inflammatory response syndrome (SIRS) or sepsis requires aggressive source control, typically surgical.
Contraindications for Operative Management
Absolute contraindications are rare and usually relate to the patient's inability to tolerate surgery or futility of intervention.
- Uncontrolled Systemic Sepsis/Shock: The patient must be resuscitated and stabilized prior to non-emergent surgical intervention. However, surgery may be life-saving for source control in severe sepsis.
- Severe Irreversible Ischemia: A foot without viable blood supply that is not amenable to revascularization may not benefit from local surgical debridement or limb salvage attempts, making primary amputation the more pragmatic approach.
- Patient Refusal: The patient's informed consent is paramount.
- Prohibitive Comorbidities: Extremely poor surgical candidates (e.g., severe cardiac failure, end-stage renal disease, advanced malignancy with limited prognosis) may not be offered extensive reconstructive procedures; palliation or primary amputation may be considered. These are generally relative contraindications requiring careful risk-benefit analysis.
Operative vs. Non-Operative Indications
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Infection Severity | Deep abscess, necrotizing fasciitis, osteomyelitis, systemic sepsis | Superficial cellulitis, uninfected ulcer, localized infection responsive to oral antibiotics |
| Tissue Viability | Necrotic tissue, gangrene, extensive slough, non-viable bone | Viable tissue, healthy granulation, clean wound bed |
| Underlying Pathology | Unstable Charcot deformity, severe structural deformity leading to recurrent ulceration | Stable Charcot foot, minor deformities manageable with orthoses, non-infected neuropathic ulcer |
| Vascular Status | Critical limb ischemia requiring revascularization as adjunct to wound healing | Adequate perfusion for healing (ABI > 0.8, TcPO2 > 40 mmHg), wound healing progressing with conservative care |
| Response to Treatment | Failure of prolonged appropriate antibiotic therapy, worsening infection despite conservative measures | Resolution of infection with antibiotics, progressive wound healing with local wound care and offloading |
| Diagnostic Need | Bone biopsy required for definitive diagnosis of osteomyelitis if non-invasive methods inconclusive | ESR/CRP normal, imaging non-conclusive for osteomyelitis, positive probe-to-bone test absent |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for successful outcomes in patients with infected foot ulcers, especially those with systemic involvement. These patients often have multiple comorbidities.
Multidisciplinary Team Approach
Involving a team of specialists improves outcomes:
*
Endocrinologist:
For optimal glycemic control (HbA1c <7%, but avoid hypoglycemia perioperatively).
*
Infectious Disease Specialist:
Guiding antibiotic selection, duration, and management of resistant organisms.
*
Vascular Surgeon:
Assessing and addressing peripheral arterial disease (PAD) through revascularization if indicated.
*
Nephrologist/Cardiologist:
Managing renal dysfunction, cardiac issues, and hypertension.
*
Podiatrist/Wound Care Specialist:
For adjunct wound management and offloading.
*
Rehabilitation Specialist:
Planning post-operative recovery and long-term offloading.
Diagnostic Workup
-
Laboratory Studies:
- Complete Blood Count (CBC): Leukocytosis, left shift.
- Erythrocyte Sedimentation Rate (ESR) & C-Reactive Protein (CRP): Critical for assessing inflammation. Elevated ESR (e.g., >70 mm/hr) and CRP (e.g., >3.0 mg/dL) are highly suggestive of osteomyelitis, particularly if the duration of symptoms is long. These markers also aid in monitoring response to treatment.
- Blood Cultures: Essential for identifying systemic bacteremia, especially in febrile patients.
- Glycemic Control Markers: HbA1c, random glucose.
- Renal and Hepatic Function Tests: To guide drug dosing and assess overall health.
-
Imaging:
- Plain Radiographs (X-rays): Initial imaging. May show soft tissue swelling, gas (abscess), loss of cortical integrity, periosteal reaction, osteopenia, or sequestrum/involucrum in chronic osteomyelitis. Changes can be delayed, sometimes appearing weeks after infection onset.
- Magnetic Resonance Imaging (MRI): Gold standard for diagnosing osteomyelitis. High sensitivity and specificity for differentiating soft tissue infection from bone involvement. Shows bone marrow edema, cortical destruction, and soft tissue collections. Crucial for surgical planning.
- Computed Tomography (CT): Useful for visualizing bone destruction, sequestrum, and complex bony architecture, especially in Charcot foot, but less sensitive than MRI for early marrow edema.
- Bone Scintigraphy (Triple-Phase Bone Scan with Indium-111 or Technetium-99m labeled WBC scan): Can be useful when MRI is contraindicated or inconclusive, but less specific than MRI, especially in Charcot neuroarthropathy.
-
Vascular Assessment:
- Ankle-Brachial Index (ABI) and Toe-Brachial Index (TBI): Screening for PAD. Note: ABIs can be falsely elevated in diabetic patients due to medial arterial calcification.
- Transcutaneous Oxygen Pressure (TcPO2): Objective measure of tissue oxygenation, predictive of wound healing potential.
- Duplex Ultrasound: Assesses arterial patency and flow.
- Angiography (CT Angiography, MR Angiography, or Digital Subtraction Angiography): Definitive assessment of arterial anatomy and degree of stenosis/occlusion, guiding revascularization decisions.
- Wound Culture: Deep tissue or bone cultures (obtained intraoperatively or via biopsy) are critical for guiding targeted antibiotic therapy. Superficial swab cultures are often unreliable due to polymicrobial colonization.
Pre-Operative Optimization
- Glycemic Control: Aim for blood glucose levels between 100-180 mg/dL (5.5-10 mmol/L) perioperatively to reduce infection risk and promote healing.
- Antibiotics: Initiate empiric broad-spectrum intravenous antibiotics immediately after cultures are obtained, covering Gram-positive, Gram-negative, and anaerobic organisms. Adjust based on culture sensitivities.
- Nutritional Support: Address any nutritional deficiencies.
- Cardiopulmonary Optimization: Manage existing cardiac or pulmonary conditions.
Patient Positioning
- Supine Position: Most common, with the affected limb externally rotated and supported on a padded bolster or leg holder.
- Pneumatic Tourniquet: Application to the thigh or calf is common to provide a bloodless field, crucial for precise debridement and identification of vital structures. Tourniquet time should be minimized, especially in ischemic limbs.
- Sterile Preparation: Wide surgical prep from mid-thigh to toes.

Detailed Surgical Approach / Technique
The surgical approach to an infected foot ulcer with suspected osteomyelitis aims for complete source control, debridement of non-viable tissue, and preservation of maximal functional length. The specific technique varies based on the extent of infection, bone involvement, vascularity, and desired reconstructive goals.
Principles of Debridement
- Wide Excision of Non-Viable Tissue: This includes all necrotic skin, subcutaneous tissue, muscle, tendon, and bone. The goal is to achieve bleeding, healthy tissue margins.
- Pulsatile Lavage: High-pressure saline irrigation to mechanically remove debris and bacteria.
- Bone Biopsy: Crucial for definitive diagnosis of osteomyelitis and pathogen identification. Samples should be taken from affected bone (cortex and cancellous bone) for both microbiology and histopathology. Send separate samples for aerobic, anaerobic, and fungal cultures.
- Abscess Drainage: Thoroughly explore and drain all purulent collections.
Surgical Steps (General Approach for Infected Foot Ulcer with Osteomyelitis)
1. Incision and Exposure
- Incision Planning: Design incisions to allow wide exposure for debridement while preserving vascularity and avoiding tension. Avoid incisions directly over pressure points if possible. Often, the ulcer itself can be incorporated into the incision.
- Deep Dissection: Carefully dissect through subcutaneous tissue. Identify and protect vital neurovascular structures. The internervous planes in the foot are less a focus for debridement than in proximal limb surgery, but understanding the anatomical corridors of infection spread is critical.
2. Debridement of Soft Tissues
- Skin and Subcutaneous Tissue: Excise all edematous, discolored, or malodorous tissue. Undermine skin edges to assess viability.
- Muscle and Tendon: Debride any muscle that does not contract or bleed. Remove necrotic tendon.
3. Debridement of Bone
- Identification of Infected Bone: Visually inspect exposed bone for discoloration (e.g., gray, black), lack of bleeding, or crumbly texture. Use a probe to assess for areas of cortical destruction or a "soft" feel.
- Resection: Use a rongeur, osteotome, or bone saw to resect all visibly infected and non-viable bone. The extent of resection may range from saucerization of a superficial cortical lesion to formal ray amputation or partial foot amputation. The goal is to reach healthy, bleeding bone margins.
- Specimen Collection: Ensure adequate bone samples are sent for microbiological culture and histopathology. This is paramount for guiding antibiotic therapy.
4. Abscess Management
- Thoroughly explore and evacuate any pus. Irrigate with copious amounts of saline.
- Consider placing drains (e.g., Penrose or suction drains) if a significant cavity remains or if ongoing drainage is anticipated.
5. Reconstruction and Closure
- Wound Management: After adequate debridement, the wound may be left open and managed with serial debridements, negative pressure wound therapy (NPWT), or wet-to-dry dressings.
- Delayed Primary Closure: If the infection is controlled and wound bed is healthy, delayed primary closure or skin grafting may be considered.
- Flap Reconstruction: For larger defects or exposed critical structures (e.g., tendons, joints, hardware), local, regional, or free flaps may be required.
- Amputation: If limb salvage is not feasible due to extensive infection, irreversible ischemia, or uncontrolled sepsis, various levels of amputation may be performed (e.g., toe amputation, ray amputation, transmetatarsal amputation, Chopart, Syme, transtibial amputation). The goal is to perform the lowest level amputation that achieves a healthy, durable stump.
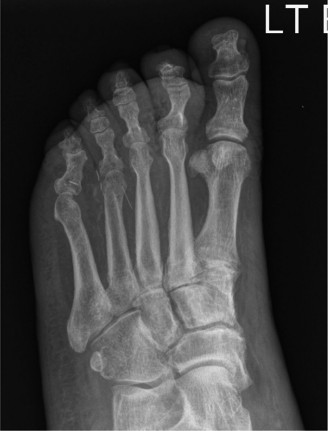
Specific Surgical Techniques
- Toe Amputation: For isolated toe osteomyelitis or gangrene. Disarticulation through the MTP joint is common, ensuring adequate soft tissue coverage.
- Ray Amputation: Resection of the entire metatarsal and corresponding phalanges. Often used for extensive infection of a single metatarsal head. Careful consideration of adjacent ray stability and future weight-bearing.
- Transmetatarsal Amputation (TMA): Amputation through the metatarsal shafts. Provides a stable weight-bearing platform if performed correctly with balanced soft tissue closure and Achilles lengthening to prevent equinus deformity.
- Partial Calcanectomy: For calcaneal osteomyelitis, often from heel pressure ulcers. Involves resection of infected bone while preserving the plantar fat pad and soft tissue envelope.
- Charcot Reconstruction/Arthrodesis: For unstable Charcot foot complicated by ulceration and infection. Involves debridement of infected bone, correction of deformity, and often internal or external fixation (e.g., ring fixators) to stabilize the foot and promote fusion. This is a complex procedure for highly selected patients.
Fixation Considerations
In the context of infected foot ulcers, fixation is primarily considered for:
*
Charcot Neuroarthropathy:
External or internal fixation to stabilize the joints after debridement and realignment, facilitating fusion and preventing recurrent ulceration.
*
Post-Amputation Stability:
Occasionally, minor internal fixation might be used for bone stabilization in specific partial foot amputations, although soft tissue closure is usually paramount.
*
Hardware Removal:
If existing hardware is present and infected, it must be removed. New hardware may be placed only after infection is cleared or in a staged fashion.
Complications & Management
Complications following surgical management of infected foot ulcers can be severe and limb-threatening, reflecting the complexity of the patient population and the nature of the disease. Proactive identification and aggressive management are critical.
Common Complications and Management Strategies
| Complication | Incidence | Salvage Strategy / Management |
|---|---|---|
| Wound Dehiscence/Infection | High (up to 30-50% in high-risk patients) | Aggressive local wound care, serial debridements, negative pressure wound therapy (NPWT), culture-directed antibiotics, offloading, nutritional optimization. May require secondary closure, skin graft, or flap. |
| Recurrence of Ulcer/Infection | Very high (up to 70% within 5 years) | Meticulous long-term offloading (TCC, specialized footwear), regular foot checks, patient education on foot hygiene, glycemic control, vascular surveillance, prompt treatment of new calluses/blisters, surgical correction of residual deformities. |
| Progression to Higher Level Amputation | Significant (up to 20-30% after initial surgery) | Early identification of failing limb salvage (persistent infection, worsening ischemia, non-healing wounds, uncontrolled sepsis). Re-evaluation of vascular status, further debridement, consideration of prosthetic needs. Timely decision for higher-level amputation to save life or achieve functional rehabilitation. |
| Flap/Graft Necrosis | Variable (depends on flap type and patient factors) | Debridement of necrotic tissue. If partial, local wound care and NPWT. If complete, further debridement and reconstruction with another flap or graft, or consideration of amputation for exposed critical structures. Vascular assessment crucial. |
| Residual Osteomyelitis | 10-20% after initial surgical debridement | Prolonged culture-directed intravenous antibiotics (often 4-6 weeks), serial inflammatory markers (ESR/CRP) to monitor response. If indicators remain high or imaging shows persistence, repeat debridement or bone resection may be necessary. Consider antibiotic-impregnated bone cement beads. |
| Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) | ~5-15% in orthopedic surgery, higher in diabetic/infected patients | Prophylactic anticoagulation (LMWH or unfractionated heparin) perioperatively. Early mobilization. Compression stockings. If diagnosed, therapeutic anticoagulation. |
| Systemic Sepsis / Multi-Organ Failure | Variable (depends on initial severity) | Aggressive supportive care (ICU management), source control (further surgical debridement), broad-spectrum antibiotics, vasopressors, fluid resuscitation, management of organ dysfunction. |
| Neuropathic Pain | Common post-amputation or with chronic neuropathy | Pharmacological management (gabapentinoids, TCAs, SNRIs), physical therapy, nerve blocks, spinal cord stimulators, psychological support. |
| Charcot Recurrence/Collapse | 15-30% in reconstructed Charcot feet | Long-term offloading, custom bracing. Close radiographic surveillance. If collapse or new ulceration occurs, repeat surgical intervention (debridement, osteotomy, arthrodesis, revisional fixation) may be necessary. |
| Antibiotic Resistance | Increasing concern, especially with chronic ulcers | Obtain deep tissue/bone cultures to guide therapy. Consult infectious disease specialists. Use narrowest effective spectrum. Consider combination therapy. Monitor for efficacy. |
| Psychological Impact | High (depression, anxiety, reduced QOL) | Comprehensive psychological assessment and support, counseling, peer support groups, addressing body image concerns. Early involvement of social work. |
Monitoring Post-Operatively
- Clinical Surveillance: Daily wound checks, assessment for signs of worsening infection (fever, erythema, purulent drainage, increasing pain, systemic signs).
- Laboratory Markers: Serial ESR and CRP values are critical to monitor the response to surgical debridement and antibiotic therapy. A decreasing trend indicates resolution of inflammation. Persistent elevation suggests ongoing infection or inadequate source control.
- Imaging: Follow-up X-rays to assess bone healing or persistence of osteomyelitis. MRI if clinical suspicion of persistent deep infection remains despite improving labs.
- Vascular Reassessment: If healing is slow or new ischemic signs appear, re-evaluate vascular status.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgery itself for achieving successful limb salvage, preventing recurrence, and maximizing functional outcomes. It is a long-term, multidisciplinary commitment.
Phase 1: Immediate Post-Operative (Hospitalization)
-
Wound Care:
- Initial surgical dressings are changed according to surgeon preference, often daily or every few days.
- Negative Pressure Wound Therapy (NPWT): Frequently used for large defects, heavily contaminated wounds, or as a bridge to secondary closure/grafting. Provides a controlled environment, removes exudate, promotes granulation tissue, and reduces bacterial load.
- Regular wound inspection for signs of infection, dehiscence, or necrosis.
- Pain Management: Multimodal analgesia (NSAIDs, acetaminophen, opioids, regional blocks) to control pain and facilitate early mobilization.
- Antibiotic Therapy: Continue culture-directed intravenous antibiotics for the prescribed duration (often 2-6 weeks, depending on the extent of infection and eradication of osteomyelitis). Monitor ESR/CRP for response.
- Glycemic Control: Strict control of blood glucose levels to optimize healing and reduce infection risk.
- Vascular Surveillance: Monitor perfusion. If revascularization was performed, assess patency of grafts/stents.
- Early Mobilization: As soon as surgically safe, initiation of bed mobility, transfers, and protected weight-bearing (if allowed). DVT prophylaxis continues.
Phase 2: Subacute Rehabilitation (Weeks to Months)
-
Offloading:
This is the cornerstone of DFU prevention and healing.
- Total Contact Casting (TCC): Gold standard for offloading plantar ulcers, even after debridement. Distributes pressure evenly across the entire foot and lower leg. Requires careful application and regular changes. Contraindications include active infection, deep abscess, or severe ischemia.
- Removable Cast Walkers (RCWs) / Walking Boots: Less effective than TCC but can be used for milder ulcers or after initial healing, provided patient compliance is excellent.
- Custom Orthoses/Bracing: For structural deformities or Charcot foot to redistribute pressure and provide stability.
- Wheelchair/Crutches: For non-weight-bearing periods, particularly after major debridement or amputation.
-
Physical Therapy:
- Range of Motion (ROM): Prevent joint contractures, especially at the ankle (equinus deformity).
- Strengthening: Rebuild muscle strength, particularly in the lower extremity and core.
- Gait Training: Re-education on proper gait mechanics, balance, and use of assistive devices or prosthetics.
- Prosthetic Fitting (Post-Amputation): For patients undergoing major amputations (e.g., transtibial), early prosthetic fitting is crucial for functional recovery.
- Skin Care: Patient education on daily foot inspection, moisturizing, proper nail care, and avoiding trauma.
- Nutrition: Continued focus on adequate protein and micronutrient intake for wound healing.
Phase 3: Long-Term Maintenance & Prevention (Months to Years)
- Custom Footwear: Prescribe specialized shoes with extra depth, width, and protective inserts to accommodate deformities and reduce pressure points.
-
Regular Follow-Up:
Lifelong follow-up with the orthopedic surgeon, endocrinologist, podiatrist, and vascular specialist.
- Frequent foot examinations to identify new calluses, pre-ulcerative lesions, or early signs of recurrent infection.
- Monitoring of ESR/CRP if there is any concern for chronic infection or new inflammatory events.
- Radiographic surveillance for Charcot foot or signs of osteomyelitis recurrence.
- Patient Education: Empower patients with knowledge about their condition, the importance of adherence to offloading, glycemic control, daily foot checks, and seeking immediate medical attention for any new foot problems.
- Lifestyle Modification: Smoking cessation, weight management, and active management of comorbidities (hypertension, hyperlipidemia).
Summary of Key Literature / Guidelines
The management of infected foot ulcers with fever, particularly those complicated by osteomyelitis, is guided by robust evidence and multidisciplinary consensus guidelines. Key principles emphasize early diagnosis, aggressive source control, appropriate antibiotic therapy, revascularization when indicated, and meticulous long-term offloading.
Infectious Diseases Society of America (IDSA) Guidelines
The IDSA provides comprehensive guidelines for the diagnosis and treatment of diabetic foot infections (DFI).
*
Diagnosis:
Emphasizes clinical assessment, probe-to-bone test, and imaging (X-ray, MRI as gold standard for osteomyelitis).
*
Role of Inflammatory Markers:
IDSA guidelines recognize ESR and CRP as useful adjunctive tools. An ESR >70 mm/hr and/or CRP >3.0 mg/dL in the context of DFI strongly suggests osteomyelitis. Declining values are indicators of treatment efficacy.
*
Bone Biopsy:
Strongly recommends bone biopsy (with histology and culture) for definitive diagnosis of osteomyelitis, especially when imaging is equivocal or prior antibiotic exposure complicates cultures.
*
Antibiotic Therapy:
Recommends empiric broad-spectrum antibiotics followed by culture-directed therapy. Duration varies based on severity, typically 2-4 weeks for soft tissue infection and 4-6 weeks (or longer) for osteomyelitis, often after surgical debridement.
*
Surgical Intervention:
Stresses the importance of surgical debridement for non-viable tissue, abscess drainage, and bone resection for osteomyelitis.
International Working Group on the Diabetic Foot (IWGDF) Guidelines
The IWGDF provides comprehensive, evidence-based guidelines for the prevention and management of diabetic foot disease.
*
Risk Classification:
Utilizes a classification system (e.g., Wagner, University of Texas) to guide management.
*
Management Algorithm:
Outlines a step-wise approach involving debridement, infection control, revascularization, offloading, and wound care.
*
Offloading:
Consistently highlights total contact casting (TCC) as the most effective method for healing plantar DFUs.
*
Multidisciplinary Team:
Reaffirms the critical role of a multidisciplinary team for optimal patient care and outcomes.
Society for Vascular Surgery (SVS) Guidelines
These guidelines focus on the assessment and management of peripheral artery disease (PAD) in patients with diabetic foot ulcers.
*
Vascular Assessment:
Recommendations for screening tests (ABI, TBI, TcPO2) and diagnostic imaging (duplex ultrasound, angiography).
*
Revascularization:
Emphasizes that revascularization is often a prerequisite for wound healing and limb salvage in ischemic foot ulcers, sometimes performed before or concurrently with surgical debridement.
Orthopedic Literature
- Numerous studies highlight the importance of aggressive surgical debridement and complete removal of infected bone to eradicate osteomyelitis and reduce recurrence rates.
- Research on Charcot neuroarthropathy emphasizes the need for stable surgical reconstruction and prolonged offloading to prevent collapse and subsequent ulceration.
- The role of ESR/CRP as prognostic indicators for successful treatment and recurrence of osteomyelitis is well-documented, guiding the duration of antibiotic therapy. Persistent elevation mandates re-evaluation for residual infection or non-eradicated osteomyelitis.
In summary, the febrile foot ulcer demands immediate and aggressive intervention. ESR serves as a critical biomarker, raising suspicion for deep infection, particularly osteomyelitis, prompting further diagnostic workup. Surgical management, guided by a multidisciplinary team, involves meticulous debridement, source control, and, where appropriate, reconstruction or amputation, followed by rigorous post-operative rehabilitation and long-term preventive strategies to preserve limb function and patient quality of life. The current academic landscape underscores precision in diagnosis, surgical execution, and patient-centered, evidence-based care.
You Might Also Like