Deep Posterior Chronic Exertional Compartment Syndrome: Advanced Diagnosis & Surgical Indications
Key Takeaway
Deep posterior chronic exertional compartment syndrome (CECS) is exertional leg pain distinct from shin splints, involving tibialis posterior, FDL, and FHL muscles. Caused by increased intracompartmental pressure within inelastic fascia during exercise, it leads to ischemia and nerve compression. Diagnosis relies on clinical symptoms and objective intracompartmental pressure measurements, often requiring surgical decompression after conservative failure.
Introduction & Epidemiology
Deep posterior compartment pain in the lower leg presents a significant diagnostic and therapeutic challenge, often masquerading as or coexisting with more commonly recognized medial tibial stress syndrome (MTSS) or "shin splints." However, a critical distinction lies in the underlying pathology and anatomical localization. While MTSS typically involves periostitis or bone stress along the posteromedial tibial cortex, deep posterior compartment pain implicates structures contained within the deep posterior fascial compartment, primarily the tibialis posterior, flexor digitorum longus (FDL), and flexor hallucis longus (FHL) muscles, and their associated neurovascular bundle. The most prevalent cause of surgically indicated deep posterior compartment pain is chronic exertional compartment syndrome (CECS).
CECS is characterized by exercise-induced pain, tightness, and sometimes neurological symptoms (paresthesia, weakness) that resolve with rest. These symptoms arise from a transient increase in intracompartmental pressure during exertion, leading to ischemia and nerve compression. While anterior and lateral compartments are more frequently affected, isolated or combined deep posterior compartment CECS is well-documented and requires precise diagnosis. Its incidence is particularly high in athletes engaged in repetitive impact activities such as long-distance running, soccer, basketball, and military training. Epidemiological data suggest that CECS accounts for up to 20% of exertional leg pain in athletes, with deep posterior involvement being a substantial subset, though specific rates for isolated deep posterior CECS are less clear and often reported in conjunction with other compartments. Males and females appear equally affected, typically in the second and third decades of life. A high index of suspicion is crucial, as misdiagnosis often leads to prolonged symptoms and ineffective conservative management. Differential diagnoses are broad and include MTSS, tibial stress fractures, nerve entrapments (e.g., tibial nerve), popliteal artery entrapment syndrome, tendinopathy, and vascular claudication.
Surgical Anatomy & Biomechanics
The deep posterior compartment of the lower leg is a distinct anatomical space critical for ankle and foot function. Its boundaries are formed anteriorly by the interosseous membrane and the posterior surface of the tibia and fibula, posteriorly by the deep transverse crural fascia, medially by the tibia, and laterally by the fibula and the intermuscular septum separating it from the lateral compartment.
Contained within this compartment are three primary muscles:
*
Tibialis Posterior (TP):
Originating from the interosseous membrane and posterior surfaces of the tibia and fibula, it inserts onto the navicular tuberosity, cuneiforms, and bases of metatarsals 2-4. It is the primary inverter and plantarflexor of the foot, essential for dynamic arch support.
*
Flexor Digitorum Longus (FDL):
Originating from the posterior surface of the tibia, it courses medially to insert into the distal phalanges of the lateral four toes. Its action is flexion of the lateral four toes and plantarflexion of the ankle.
*
Flexor Hallucis Longus (FHL):
Originating from the posterior surface of the fibula, it courses laterally to pass beneath the sustentaculum tali before inserting into the distal phalanx of the great toe. Its primary action is great toe flexion, contributing to push-off during gait, and also assists in ankle plantarflexion.
The neurovascular bundle of the deep posterior compartment consists of the tibial nerve, posterior tibial artery, and its concomitant veins. These structures lie superficial to the muscles of the deep posterior compartment but deep to the soleus, running between the superficial and deep posterior fascial layers. The tibial nerve provides motor innervation to all muscles of the deep posterior compartment and sensory innervation to the sole of the foot. The posterior tibial artery supplies these muscles and gives off branches to the ankle and foot.
The deep transverse crural fascia, also known as the deep posterior compartment fascia, is a strong, inelastic fascial layer that encapsulates these muscles and neurovascular structures. In the context of CECS, this fascia becomes rigid and unable to accommodate the normal exercise-induced increase in muscle volume (up to 20%). This inelasticity leads to elevated intracompartmental pressure, compressing the neurovascular bundle and compromising muscle perfusion, resulting in ischemic pain and neurological symptoms. The biomechanical role of these muscles, particularly the Tibialis Posterior in foot stability and shock absorption during gait, means they are highly active during weight-bearing activities. Overuse or repetitive loading can lead to hypertrophy, further exacerbating pressure increases within a restrictive fascial envelope. Understanding this precise anatomical relationship and the inelastic nature of the deep transverse fascia is paramount for successful surgical decompression.

Indications & Contraindications
The decision for surgical intervention for deep posterior compartment pain, primarily deep posterior chronic exertional compartment syndrome (CECS), is predicated on a thorough diagnostic workup and failure of exhaustive conservative measures.
Operative Indications
- Failure of Non-Operative Management: Persistent and debilitating exertional deep posterior leg pain despite a minimum of 3-6 months of dedicated conservative therapy, including activity modification, physical therapy (stretching, strengthening), orthotics, biomechanical gait analysis, and anti-inflammatory medications.
-
Diagnostic Intracompartmental Pressure Measurements:
Objective confirmation of CECS in the deep posterior compartment, typically using a Stryker needle or similar device. Standardized diagnostic criteria often include:
- Resting pressure > 15 mmHg.
- 1-minute post-exercise pressure > 30 mmHg.
- 5-minute post-exercise pressure > 20 mmHg.
- Variations exist, but the dynamic elevation of pressure with exertion and its slow return to baseline are key.
- Measurements should reproduce the patient's symptoms during the exercise provocation.
- Reproducible Symptoms: Consistent and predictable onset of deep posterior leg pain, tightness, and/or paresthesia during specific exertional activities, which resolves with rest.
- Exclusion of Other Pathologies: Thorough exclusion of other potential causes of exertional leg pain, such as stress fractures (tibial, fibular), nerve entrapment (e.g., popliteal artery entrapment syndrome, lumbar radiculopathy), tendinopathy (e.g., Tibialis Posterior tendinopathy refractory to conservative care), vascular claudication (atherosclerotic), and popliteal artery entrapment syndrome. Imaging (MRI, X-ray, CT, vascular studies) and neurological examination are vital.
Non-Operative Indications
- Initial Presentation/Mild Symptoms: Patients presenting with mild, intermittent symptoms that do not significantly impact daily or athletic activities.
- Early Stages of Diagnosis: All patients typically undergo a trial of conservative management as the first-line treatment.
- Pressure Measurements Not Meeting Surgical Criteria: Intracompartmental pressures that do not definitively meet the diagnostic thresholds for CECS, despite suggestive clinical symptoms.
- Patient Preference or Co-morbidities: Patients unwilling or medically unfit for surgery, or those with underlying conditions that make surgery high-risk.
- Alternative Diagnoses: If the pain is attributable to MTSS, stress fracture, or tendinopathy, which are often managed non-operatively.
Contraindications
-
Absolute Contraindications:
- Active local or systemic infection.
- Uncorrected coagulopathy.
- Acute compartment syndrome (requires emergent fasciotomy, distinct from CECS).
-
Relative Contraindications:
- Patient non-compliance with post-operative rehabilitation protocols.
- Unrealistic patient expectations regarding surgical outcomes.
- Misdiagnosis or presence of alternative, non-surgical pathologies.
- Poor general health status or significant medical co-morbidities that increase surgical risk.
Summary of Operative vs. Non-Operative Indications
| Feature | Operative Indication | Non-Operative Indication |
|---|---|---|
| Symptom Severity | Debilitating, impacting quality of life/athletic performance | Mild to moderate, manageable with activity modification |
| Duration | >3-6 months of failed conservative treatment | Initial presentation, early stages of symptoms |
| Pressure Testing | Positive intracompartmental pressure studies | Negative or equivocal pressure studies |
| Symptom Nature | Reproducible, exertional pain/paresthesia | Intermittent, less predictable pain |
| Imaging | Rules out other pathologies, confirms no stress fracture, etc. | May reveal non-surgical pathology (e.g., mild tendinosis) |
| Patient Desire | Strongly desires surgical intervention for definitive relief | Prefers conservative approach, unwilling/unfit for surgery |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential to ensure a safe and effective deep posterior fasciotomy. This phase involves diagnostic confirmation, patient education, surgical strategy formulation, and careful patient positioning.
Pre-Operative Planning
- Diagnostic Review: Reconfirm the diagnosis of deep posterior CECS, reviewing all clinical notes, diagnostic imaging (plain radiographs to rule out stress fracture, MRI to rule out other soft tissue pathologies, rule out vascular issues with appropriate studies if indicated), and crucially, the intracompartmental pressure measurements. Ensure the pressures were taken accurately, reproduced symptoms, and meet accepted criteria for surgical intervention.
- Patient Education: Comprehensive discussion with the patient regarding the surgical procedure, expected outcomes (typically 80-90% success in symptom resolution), potential risks (nerve injury, infection, hematoma, recurrence), and the importance of post-operative rehabilitation compliance. Manage expectations regarding complete resolution of symptoms and return to peak performance.
- Anesthesia Consultation: Discuss anesthesia options with the patient and anesthesiologist. General anesthesia is commonly employed, often combined with a regional nerve block (e.g., popliteal block) for enhanced post-operative pain control.
-
Equipment Preparation:
- Standard soft tissue surgical tray.
- Laminar flow operating room.
- Tourniquet (pneumatic, proximal thigh).
- Bipolar cautery.
- Headlamp and loupe magnification for enhanced visualization.
- Nerve stimulator (optional, but useful for identifying the tibial nerve if dissection becomes challenging).
- Marking pen for incision planning.
- Sterile dressings and splinting material (e.g., soft bulky dressing, posterior slab).
- Incision Planning: Pre-operative marking of the planned incision while the patient is awake and standing (if possible) or supine. The incision for deep posterior fasciotomy is typically a longitudinal curvilinear incision along the posteromedial aspect of the tibia, usually 15-20 cm in length, centered over the area of maximal tenderness and muscle bulk of the deep posterior compartment. Palpate the posteromedial border of the tibia and mark the course of the great saphenous vein (GSV) and saphenous nerve to aid in their protection.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Leg Support: A bolster or gel pad is placed under the ipsilateral hip/buttock to slightly externally rotate the leg, facilitating access to the posteromedial aspect of the calf. The knee is usually slightly flexed.
- Tourniquet Application: A pneumatic tourniquet is applied high on the proximal thigh of the operative leg. This provides a bloodless field, crucial for identifying delicate neurovascular structures and the fascial planes. The tourniquet is inflated after exsanguination of the limb.
- Sterile Preparation and Draping: The entire lower limb, from the iliac crest down to the toes, is prepped with an antiseptic solution (e.g., chlorhexidine or povidone-iodine) and allowed to dry. The limb is then draped sterilely, ensuring adequate exposure of the surgical site and allowing for manipulation of the foot and ankle if needed. A stockinette can be used, with appropriate fenestration for the incision. Ensure the operative field is wide enough to extend the incision if necessary and to manage any unexpected events.
Detailed Surgical Approach / Technique: Medial Deep Posterior Fasciotomy
The primary surgical technique for deep posterior compartment syndrome is a medial fasciotomy, which aims to release the deep transverse crural fascia. This approach provides direct access to the deep posterior compartment while minimizing disruption to other structures.
Incision
- A longitudinal curvilinear incision, approximately 15-20 cm in length, is made along the posteromedial aspect of the tibia. This incision is typically positioned 2-3 cm posterior to the palpable posteromedial border of the tibia, extending from the proximal to the mid-calf region. This placement minimizes the risk of injury to the great saphenous vein and saphenous nerve, which lie more anteriorly.
- The incision is carried through the skin and subcutaneous tissue.
Dissection (Step-by-Step)
-
Superficial Structures:
- Carefully identify and protect the great saphenous vein (GSV) and the accompanying saphenous nerve (a branch of the femoral nerve, providing sensory innervation to the medial leg and foot). These structures are often encountered within the subcutaneous fat layer, slightly anterior to the planned deep dissection. They should be gently retracted anteriorly or posteriorly using blunt dissection and appropriate retractors.
-
Superficial Posterior Fascia:
- Incise the superficial fascia overlying the medial belly of the gastrocnemius muscle. This exposes the gastrocnemius.
-
Gastrocnemius and Soleus Retraction:
- The medial gastrocnemius muscle is then retracted posteriorly and laterally.
- Deep to the gastrocnemius, the soleus muscle is encountered. The soleus muscle is bluntly dissected off its posterior attachment to the tibia and retracted posteriorly and laterally as well. This maneuver exposes the deep fascial layer and the structures within.
-
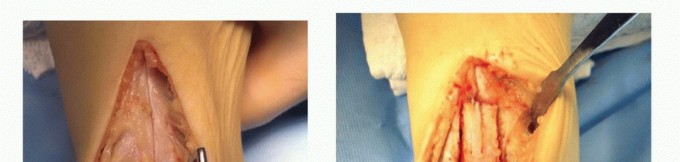
Identifying the Deep Transverse Crural Fascia:
- After retracting the soleus muscle, the surgeon will visualize a glistening, dense fascial layer. This is the deep transverse crural fascia , which encloses the deep posterior compartment. This is the primary target for release.
- Crucially, the tibial nerve and posterior tibial artery and veins lie immediately superficial to this deep transverse fascia, nestled between the soleus and the deep compartment muscles. Extreme caution is required at this stage to avoid inadvertent injury.
-
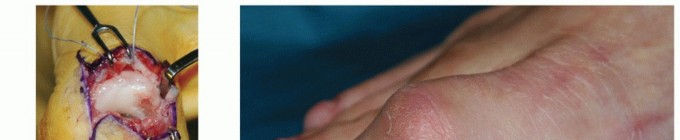
Integrate Image Here:
 - Image Context : This image would typically depict a surgical view during deep posterior fasciotomy, showing the deep transverse fascia exposed, with the soleus retracted, and the neurovascular bundle carefully identified and protected.
-
Fascial Release:
- Using a scalpel or electrocautery, a full-length incision is made along the entire length of the deep transverse crural fascia, from proximal to distal. The incision should extend from just below the popliteal fossa to just above the malleoli.
- Ensure that the release is complete and extends into the lateral aspect of the compartment where the FHL lies. Some surgeons advocate for separate fascial incisions for FDL and FHL, but a thorough, full-length incision of the deep transverse fascia usually provides adequate decompression for all muscles within the compartment.
- Carefully inspect the released compartment. The muscles of the deep posterior compartment (Tibialis Posterior, FDL, FHL) should visibly bulge through the incised fascia, indicating successful decompression.
-
Inspection and Hemostasis:
- Thoroughly inspect the compartment for any remaining tight bands of fascia.
- Achieve meticulous hemostasis using bipolar cautery.
Internervous Planes & Protection of Neurovascular Structures
While not strictly an internervous plane approach in the classical sense, the key to this procedure is understanding the relationship of the tibial nerve and posterior tibial vessels to the deep transverse fascia. They lie superficial to the fascia being incised. Therefore, the primary internervous plane of surgical importance is the space between the soleus muscle and the deep transverse crural fascia , where the neurovascular bundle resides. Blunt dissection and careful retraction are paramount to protect these vital structures throughout the procedure. Proximally, the tibial nerve lies more medially, and distally it crosses posterior to the posterior tibial artery. Consistent visualization and careful technique are non-negotiable.
Wound Closure
- The deep fascia is left open to prevent recurrence of compartment syndrome.
- The subcutaneous tissue can be loosely approximated.
- The skin is then loosely closed with interrupted sutures, staples, or adhesive strips. Due to the swelling and muscle herniation, the skin closure may appear slightly under tension, or a "skin-only" closure might be performed. Occasionally, if there is significant skin tension preventing primary closure, a delayed primary closure or even skin grafting (rare for deep posterior only) may be considered, though this is more typical for combined four-compartment releases with greater soft tissue swelling.
- A bulky, soft dressing is applied, often with a posterior splint or elastic bandage to provide gentle compression and support.
Complications & Management
While deep posterior fasciotomy is generally a safe and effective procedure, like any surgical intervention, it carries inherent risks. A thorough understanding of potential complications, their incidence, and appropriate management strategies is crucial for academic orthopedic surgeons.
Table of Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (%) | Management & Salvage Strategies |
|---|---|---|
| Nerve Injury | 5-15% |
Prevention:
Meticulous dissection, loupe magnification, clear identification and protection of saphenous nerve (medial incision) and tibial nerve (between soleus and deep fascia).
Management: - Saphenous Nerve: Paresthesia/neuroma; often resolves. Neuropathic pain management, rarely surgical excision of neuroma. - Tibial Nerve: Most severe. Immediate exploration if suspected intraoperatively. Post-op, observe for motor/sensory recovery. Neuropathic pain management. If no recovery, potentially neurolysis, nerve repair, or grafting. |
| Vessel Injury | <5% |
Prevention:
Careful dissection, avoid aggressive retraction, use blunt dissection around neurovascular bundle.
Management: - Great Saphenous Vein: Ligation is generally well-tolerated. - Posterior Tibial Artery/Veins: Immediate repair by vascular surgeon if significant. Ligation of veins is generally acceptable. |
| Infection (Superficial/Deep) | 1-3% |
Prevention:
Strict aseptic technique, prophylactic antibiotics, careful wound management.
Management: Oral or IV antibiotics based on culture. Superficial wound debridement for cellulitis. Deep infection may require surgical debridement, washout, and prolonged antibiotics. |
| Hematoma/Seroma | 2-7% |
Prevention:
Meticulous hemostasis, compression dressing.
Management: Small hematomas/seromas often resolve spontaneously. Larger, symptomatic ones may require aspiration under ultrasound guidance or surgical drainage. |
| Recurrence of Symptoms/Incomplete Release | 5-10% |
Prevention:
Ensuring a full-length, complete fascial release verified by muscle bulging.
Management: Re-evaluation with clinical examination and repeat compartment pressure testing. Revision fasciotomy may be necessary. Explore for persistent fascial bands or scar tissue. |
| Persistent Pain/CRPS | <2% |
Prevention:
Meticulous surgical technique, adequate pain management, early mobilization.
Management: Multidisciplinary pain management, physical therapy, sympathetic blocks, medications (e.g., gabapentinoids). |
| Scarring/Cosmetic Issues | Common |
Prevention:
Careful incision placement, neat skin closure.
Management: Scar massage, silicone sheeting, camouflage makeup. Rarely, scar revision. |
| Muscle Herniation | Common |
Prevention:
Often unavoidable as a consequence of fascial release.
Management: Usually asymptomatic and requires no specific treatment. May cause cosmetic concern; rarely requires fascial repair (with risk of recurrence) or mesh repair for significant symptoms. |
| Deep Vein Thrombosis (DVT) | <1% |
Prevention:
Early mobilization, prophylactic anticoagulation for high-risk patients.
Management: Anticoagulation, pulmonary embolism prophylaxis. |
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical for optimizing outcomes following deep posterior fasciotomy. The goals are to minimize complications, restore full range of motion (ROM), rebuild strength, and facilitate a safe return to sport or desired activities.
Phase 1: Immediate Post-Operative (Days 0-14)
- Goals: Pain control, wound healing, minimize swelling, initiate gentle ROM.
- Weight Bearing: Usually immediate full weight-bearing as tolerated, unless specific circumstances dictate otherwise.
- Pain Management: Opioids initially, transitioning to NSAIDs/acetaminophen. Regional nerve blocks are highly beneficial for initial pain control.
-
Swelling Management:
- Elevation of the limb (above heart level).
- Cryotherapy (ice packs) for 15-20 minutes, several times a day.
- Compression dressing initially; transition to compression stocking.
- Wound Care: Keep incision clean and dry. Monitor for signs of infection (redness, warmth, purulent discharge). Suture/staple removal typically at 10-14 days.
-
Gentle Range of Motion (ROM):
- Ankle plantarflexion and dorsiflexion within pain-free limits.
- Toe flexion and extension.
- Gentle ankle circumduction.
- No forceful stretching of the posterior compartment muscles.
Phase 2: Early Rehabilitation (Weeks 2-6)
- Goals: Restore full pain-free ROM, initiate muscle activation and low-impact cardiovascular fitness.
- Physical Therapy: Commence formal physical therapy sessions.
-
ROM & Flexibility:
- Continue gentle ankle ROM exercises.
- Initiate gentle calf and deep posterior compartment stretching (gastroc/soleus, Tibialis Posterior, FDL, FHL) once wound is healed. Hold stretches for 20-30 seconds, 3-5 repetitions.
-
Strengthening (Isometric/Light Resistance):
- Isometric ankle plantarflexion, dorsiflexion, inversion, eversion.
- Gentle resistance band exercises for all ankle movements.
- Toe curls.
- Core stability exercises.
-
Cardiovascular Fitness:
- Stationary cycling (light resistance).
- Swimming (avoiding vigorous kicking initially).
- Elliptical trainer (low resistance).
- Scar Management: Begin scar massage once the wound is well-healed to prevent adhesions and reduce sensitivity. Silicone sheeting may also be used.
Phase 3: Intermediate Rehabilitation (Weeks 6-12)
- Goals: Progress strengthening, improve proprioception, gradual return to impact activities.
-
Strengthening (Progressive):
- Advance resistance band exercises.
- Calf raises (bilateral to unilateral).
- Eccentric strengthening of calf muscles.
- Theraband walks (forward, backward, sideways).
- Leg press, seated calf raise machines.
-
Proprioception & Balance:
- Single leg balance exercises (eyes open/closed).
- Wobble board, Bosu ball exercises.
- Dynamic balance activities.
-
Return to Impact Activities (Gradual):
- Begin with brisk walking.
- Progress to short intervals of light jogging on soft surfaces (grass, track).
- Closely monitor for any recurrence of pain. If pain occurs, reduce intensity and duration.
Phase 4: Advanced Rehabilitation & Return to Sport (Weeks 12+)
- Goals: Maximize functional strength and endurance, sport-specific training, safe return to full activity.
-
Sport-Specific Training:
- Gradual introduction of agility drills (shuttle runs, figure-of-8).
- Plyometric exercises (box jumps, hopping, bounding) at increasing intensity.
- Progress running distance, speed, and incorporate uphill/downhill components.
-
Criteria for Return to Sport:
- Full pain-free ROM and strength symmetry (isokinetic testing if available).
- Ability to perform sport-specific drills without symptoms.
- Achieve pre-injury fitness levels.
- Psychological readiness.
- Maintenance: Continued stretching and strengthening program. Emphasize proper warm-up and cool-down. Consider addressing any underlying biomechanical issues (e.g., overpronation, tight hamstrings).
- Monitoring: Continued vigilance for any return of symptoms. Recurrence is rare but can occur due to incomplete release or scar tissue formation.
The exact timeline for each phase can vary based on individual patient progress, sport demands, and surgeon preference. Communication between the surgeon, physical therapist, and athlete is paramount.
Summary of Key Literature / Guidelines
The diagnosis and management of deep posterior compartment pain, particularly Chronic Exertional Compartment Syndrome (CECS), are well-established in orthopedic literature, though specific nuances regarding the deep posterior compartment warrant distinct consideration.
Diagnostic Criteria and Pressure Measurement
The cornerstone of diagnosis for CECS across all compartments, including the deep posterior, remains
intracompartmental pressure testing
. Early seminal work by Pedowitz et al. (1986, 1990) established the widely accepted diagnostic criteria, defining abnormal pressures as:
* Resting pressure ≥ 15 mmHg.
* 1-minute post-exercise pressure ≥ 30 mmHg.
* 5-minutes post-exercise pressure ≥ 20 mmHg.
These values, or slight variations thereof, are commonly cited in textbooks and guidelines. It is crucial that pressure measurements are taken using a validated technique (e.g., Stryker manometer) and, critically, that the test reproduces the patient's symptoms. False positives and negatives can occur, highlighting the importance of clinical correlation.
Imaging Modalities
While imaging is not diagnostic for CECS, it plays a vital role in ruling out differential diagnoses.
*
Plain radiographs
are essential to exclude stress fractures, bony tumors, or other skeletal pathologies.
*
MRI
with and without contrast can be useful to rule out tendinopathy, muscle strains, tumors, or early stress reactions not visible on X-ray. It can sometimes show fascial thickening or muscle edema post-exertion, but these findings are non-specific.
*
Doppler ultrasound or MRA
may be indicated if vascular pathologies like popliteal artery entrapment syndrome are suspected, particularly in younger, athletic individuals with exertional claudication-like symptoms that mimic CECS.
Conservative Management Efficacy
Literature consistently supports an initial trial of conservative management for CECS, emphasizing activity modification, physical therapy, biomechanical analysis, and orthotics. However, the success rate for conservative management of symptomatic, objectively diagnosed CECS (especially with pressures meeting surgical criteria) is generally low, often quoted in the range of 10-30%. This reinforces the notion that surgical intervention is frequently necessary for definitive relief in these patients. For deep posterior CECS, conservative measures targeting Tibialis Posterior, FDL, and FHL function, along with appropriate footwear, are explored prior to surgery.
Surgical Outcomes and Techniques
Fasciotomy
remains the gold standard treatment for CECS refractory to conservative care.
*
Outcomes:
Success rates for deep posterior fasciotomy, in terms of symptom resolution and return to activity, are reported between 80-95%. A meta-analysis by Sperandio et al. (2014) reported high success rates for deep posterior compartment releases, similar to other compartments. However, some patients may experience persistent mild symptoms or develop complications.
*
Open Fasciotomy:
The described medial approach is the most widely adopted and robust technique for deep posterior compartment release. It allows for direct visualization of the deep transverse crural fascia and protection of the neurovascular bundle. Early studies by Detmer and Sharpe (1990) and others have detailed the efficacy and technique of this approach.
*
Endoscopic Fasciotomy:
While endoscopic techniques have gained popularity for anterior and lateral compartment releases due to smaller incisions and potentially faster recovery, their application for the deep posterior compartment is less common and technically more challenging. The anatomy of the deep posterior compartment and the proximity of the tibial nerve and posterior tibial vessels make it a higher-risk endeavor, and most academic centers still favor an open approach for definitive release. Limited literature exists on endoscopic deep posterior fasciotomy, and it is not considered the standard of care.
*
Incomplete Release:
A common reason for recurrence or persistent symptoms is incomplete fascial release. The literature emphasizes the importance of releasing the entire length of the deep transverse fascia to ensure adequate decompression.
Rehabilitation Principles
Post-operative rehabilitation protocols are consistently highlighted in the literature as crucial for optimal recovery. Early mobilization, progressive strengthening, proprioceptive training, and a gradual return to activity are universally recommended. A systematic review by Edwards et al. (2016) underscored the importance of a structured rehabilitation program, noting that adherence contributes significantly to favorable outcomes and minimizes the risk of re-injury.
In summary, deep posterior compartment pain due to CECS is a distinct clinical entity requiring careful diagnostic differentiation. While conservative measures are the initial step, a high percentage of patients with objectively confirmed CECS will ultimately require surgical fasciotomy. The medial open approach remains the most reliable technique, offering excellent outcomes when performed meticulously, followed by a disciplined and progressive rehabilitation program.
You Might Also Like