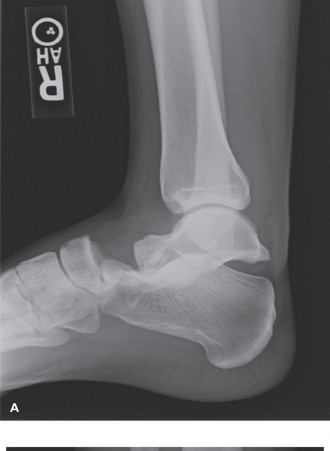
Lateral Plantar Nerve Entrapment (Baxter's Neuropathy): Comprehensive Guide to Diagnosis & Surgical Anatomy
Key Takeaway
Baxter's neuropathy, or lateral plantar nerve entrapment (LPNE), is a common yet often overlooked cause of chronic heel pain, affecting 10-20% of patients with refractory symptoms. It involves compression of the first branch of the lateral plantar nerve (FBLPN), often between foot muscles or bone, requiring precise diagnosis and understanding of its surgical anatomy for effective treatment.
Introduction & Epidemiology
Chronic heel pain is a prevalent musculoskeletal complaint, presenting a diagnostic challenge to the orthopedic surgeon. While plantar fasciitis remains the most common etiology, accounting for approximately 80% of cases, a significant subset of patients present with refractory symptoms despite exhaustive conservative management. Among these, entrapment of the first branch of the lateral plantar nerve, often referred to as Baxter's neuropathy or inferior calcaneal nerve entrapment, is a frequently overlooked cause. Recognizing this distinct neuropathic entity is critical for appropriate patient selection and successful surgical intervention.
Baxter's neuropathy is characterized by compression of the first branch of the lateral plantar nerve (FBLPN), which typically courses between the abductor hallucis muscle and the quadratus plantae muscle, adjacent to the medial calcaneal tuberosity. Its prevalence as a cause of heel pain is estimated to be between 10% and 20% in patients presenting with chronic plantar heel pain, making it the second most common cause after plantar fasciitis.
Epidemiologically, LPNE can affect individuals across a broad age spectrum, although it is more commonly observed in middle-aged adults, similar to plantar fasciitis. Both active individuals, particularly runners and athletes involved in high-impact activities, and those with sedentary lifestyles can be affected. Risk factors include:
*
Pes Cavus or Pes Planus Deformities:
Biomechanical abnormalities that alter foot loading patterns and tension on fascial structures.
*
Obesity:
Increased load on the plantar structures.
*
Calcaneal Osteophytes or Spurs:
These can directly impinge upon the nerve.
*
Hypertrophy of the Abductor Hallucis Muscle:
Often seen in athletes, contributing to a tighter anatomical tunnel.
*
Tarsal Tunnel Syndrome:
The FBLPN can be entrapped in isolation or as part of a more proximal tarsal tunnel syndrome.
*
Repetitive Microtrauma:
Mechanical stress from prolonged standing or impact activities.
The pathophysiology involves mechanical compression and repetitive microtrauma to the FBLPN, leading to demyelination, axonal degeneration, and subsequent neuropathic pain. The nerve is particularly vulnerable at three potential sites:
1. As it penetrates the deep fascia of the abductor hallucis muscle.
2. Between the deep fascia of the abductor hallucis muscle and the medial plantar aspect of the calcaneus.
3. Between the quadratus plantae muscle and the plantar aponeurosis/medial calcaneal tuberosity.
These compression points are often exacerbated by the anatomical confines and biomechanical forces within the medial plantar foot.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy of the medial ankle and plantar foot is paramount for the accurate diagnosis and effective surgical decompression of the lateral plantar nerve.
The tibial nerve descends posteriorly to the medial malleolus, passing through the tarsal tunnel. Within the tarsal tunnel or just distal to it, the tibial nerve typically trifurcates into the medial plantar nerve, the lateral plantar nerve, and the medial calcaneal nerve.
The lateral plantar nerve continues its course laterally and anteriorly beneath the abductor hallucis muscle. It then gives rise to its first branch, which is the focus of Baxter's neuropathy.
The
first branch of the lateral plantar nerve (FBLPN)
, also known as the inferior calcaneal nerve or Baxter's nerve, is a purely motor nerve in approximately 50-60% of individuals, supplying the abductor digiti minimi muscle, the quadratus plantae muscle (in some variations), and occasionally the flexor digitorum brevis. In the remaining cases, it may also provide sensory innervation to the calcaneal periosteum, the calcaneal fat pad, and the plantar skin of the heel. Its trajectory is crucial:
*
Origin:
It typically branches from the lateral plantar nerve distal to the medial malleolus, at the level of the sustentaculum tali.
*
Course:
It then passes inferiorly, laterally, and anteriorly, often diving between the deep fascia of the abductor hallucis muscle and the medial aspect of the calcaneal tuberosity. This is a primary site of entrapment. It then continues laterally, coursing either superficially or deep to the quadratus plantae muscle, heading towards the abductor digiti minimi muscle.
*
Compression Points:
1.
Proximal Entrapment:
Where it takes a sharp turn around the inferior margin of the calcaneus, particularly where it passes beneath the deep fascia of the abductor hallucis muscle. This fascial edge can be thickened and unyielding.
2.
Midfoot Entrapment:
As it runs between the quadratus plantae muscle and the medial plantar aspect of the calcaneus or overlying fascial structures. Hypertrophy of the quadratus plantae can contribute to this.
3.
Distal Entrapment:
Less common, but can occur near calcaneal spurs or a thickened plantar aponeurosis as the nerve courses more distally towards the abductor digiti minimi.
Adjacent anatomical structures are critical to consider during surgical decompression:
*
Abductor Hallucis Muscle:
Forms the medial boundary of the tarsal tunnel and is a significant compressive factor. Its deep fascial origin from the medial calcaneal tuberosity often forms the tight fibrous band that entraps the FBLPN.
*
Quadratus Plantae Muscle:
Lies deep to the abductor hallucis and is another potential site of compression for the FBLPN.
*
Medial Calcaneal Tuberosity:
The boney prominence around which the nerve takes a sharp turn. Calcaneal spurs can directly impinge upon the nerve.
*
Plantar Fascia:
Though often implicated in general heel pain, a thickened plantar fascia or its bony attachment can contribute to FBLPN compression.
*
Sural Nerve:
More posterior and lateral in its course, but must be protected during incision and retraction.
*
Medial Plantar Artery and Veins:
Run adjacent to the nerve and must be carefully preserved.
Representative anatomical illustration highlighting the course and potential compression points of the lateral plantar nerve and its first branch in relation to the abductor hallucis and quadratus plantae muscles.
Biomechanics:
Abnormal foot biomechanics play a significant role in the etiology of FBLPN entrapment.
*
Pronation:
Excessive or prolonged pronation can increase tension on the abductor hallucis muscle and the deep fascial structures that compress the nerve. It effectively lengthens the medial arch, potentially increasing strain on the nerve as it courses around the calcaneus.
*
Pes Cavus:
While seemingly counterintuitive, a high arch foot can also lead to compression by altering the load distribution and increasing muscle bulk of the intrinsic foot muscles.
*
Repetitive Impact:
Activities like running or prolonged standing subject the foot to repetitive impact loads, which can cause microtrauma, inflammation, and hypertrophy of surrounding muscles, thereby narrowing the nerve's anatomical tunnel.
*
Weight Bearing:
The FBLPN is under maximal tension during the toe-off phase of gait, particularly when the heel leaves the ground. This dynamic compression can contribute to chronic irritation.
Indications & Contraindications
Indications for Surgical Decompression
Surgical decompression of the FBLPN is considered when a clear diagnosis of Baxter's neuropathy has been established and non-operative management has failed to provide adequate symptom relief.
Operative Indications:
*
Chronic Plantar Heel Pain:
Persistent, localized pain on the medial plantar aspect of the heel, typically present for at least 6-12 months.
*
Failure of Comprehensive Non-Operative Management:
This is the cornerstone of surgical indication. Non-operative modalities must include:
* Activity modification.
* Custom orthotics (e.g., arch supports, heel cups).
* Physical therapy (stretching, strengthening, nerve gliding).
* Oral anti-inflammatory medications.
* Targeted corticosteroid injections (often transient relief, but diagnostic).
* Night splints.
* Pain localized to the specific course of the FBLPN.
*
Positive Clinical Examination Findings:
*
Tinel's Sign:
Reproduction or exacerbation of pain and/or paresthesia upon percussion over the nerve's course (medial plantar heel, deep to abductor hallucis).
*
Palpation Tenderness:
Exquisite tenderness to deep palpation along the course of the FBLPN, distinct from the plantar fascia origin.
*
Provocative Tests:
Reproduction of symptoms with resisted abduction of the great toe (stretching the abductor hallucis) or with passive dorsiflexion and eversion of the foot.
*
Supportive Imaging:
*
MRI:
May demonstrate denervation changes (fatty atrophy, edema) in the abductor digiti minimi muscle, nerve edema, or hypertrophied abductor hallucis muscle/fascial bands. Crucially, MRI helps exclude other pathologies (e.g., stress fracture, bone tumor, severe plantar fasciitis, fat pad atrophy).
*
Ultrasound:
Can sometimes visualize nerve swelling or compression, though less definitive than MRI for deep structures.
*
Electrodiagnostic Studies (EMG/NCS):
While often falsely negative (due to the small caliber and purely motor nature in many cases), positive findings (e.g., denervation in abductor digiti minimi, slowed conduction velocity across the entrapment site) provide strong objective evidence.
*
Diagnostic Nerve Block:
Temporary relief (typically >50% reduction in pain for a defined period) following a precise injection of local anesthetic around the FBLPN, guided by ultrasound, is highly supportive.
Contraindications for Surgical Decompression
Absolute Contraindications:
*
Active Infection:
Local or systemic infection.
*
Unrealistic Patient Expectations:
Patients must understand the recovery process and potential for persistent symptoms.
*
Uncontrolled Systemic Comorbidities:
Severe peripheral neuropathy (e.g., advanced diabetic neuropathy), uncontrolled coagulopathy, or medical conditions that significantly increase surgical risk.
Relative Contraindications:
*
Pain Relief with Non-Operative Management:
If symptoms are adequately controlled, surgery is not indicated.
*
Lack of Clear Diagnosis:
Unexplained or diffuse heel pain without specific clinical or diagnostic corroboration of FBLPN entrapment.
*
Psychological Factors:
Significant psychiatric comorbidities or somatization disorder where pain is primarily psychogenic.
*
CRPS (Complex Regional Pain Syndrome):
Decompression surgery can exacerbate CRPS. Thorough evaluation for this condition is necessary.
*
Proximal Neuropathy:
Symptoms primarily originating from a more proximal nerve entrapment (e.g., lumbar radiculopathy, more proximal tarsal tunnel syndrome) should be addressed first.
Summary of Indications
| Feature | Non-Operative Management Indication | Operative Decompression Indication |
|---|---|---|
| Duration of Symptoms | Acute or subacute heel pain (typically < 6 months) | Chronic, persistent heel pain (> 6-12 months) |
| Response to Therapy | Responds to conservative interventions (PT, orthotics, injections) | Failed extensive and varied conservative management |
| Pain Localization | Diffuse heel pain, or specific to plantar fascial origin | Localized tenderness and pain along the course of FBLPN (medial plantar aspect of calcaneus, deep to abductor hallucis) |
| Clinical Signs | Limited or non-specific signs | Positive Tinel's sign, reproducible pain with specific palpation/provocation, absence of clear plantar fasciitis signs as primary issue |
| Imaging Findings | Variable, may show plantar fasciitis, normal heel X-rays | MRI showing denervation atrophy of ADM, nerve edema, hypertrophied muscle/fascia; negative for other significant pathologies |
| Electrodiagnostics | Not typically indicated or may be normal | May show motor abnormalities in ADM (if positive), but negative findings do not rule out LPNE |
| Diagnostic Nerve Block | Not required if responding to conservative care | Significant temporary relief with targeted FBLPN block (ultrasound-guided) |
| Patient Comorbidities | Suitable for all patients | Careful assessment of systemic comorbidities, psychological factors, and realistic expectations |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are essential for successful surgical outcomes and minimizing complications during FBLPN decompression.
Pre-Operative Planning
-
Comprehensive Patient Evaluation:
- Detailed History: Reconfirm the duration, character, location, and aggravating/alleviating factors of pain. Document all failed conservative treatments. Ascertain the impact on daily activities and quality of life. Inquire about any history of diabetes, peripheral neuropathy, or previous foot/ankle surgeries.
-
Thorough Physical Examination:
- Inspect the foot for deformities, swelling, skin changes, or atrophy (e.g., abductor digiti minimi).
- Palpate systematically for tenderness: medial calcaneal tuberosity, plantar fascia origin, abductor hallucis muscle origin, and the specific course of the FBLPN. Differentiate between fascial pain and neuropathic pain.
- Perform Tinel's sign over the FBLPN path.
- Assess motor strength of intrinsic foot muscles, especially abductor digiti minimi.
- Evaluate sensation to light touch, pinprick, and two-point discrimination in the nerve distribution.
- Assess ankle and subtalar joint range of motion.
- Evaluate gait and foot posture (pes planus, pes cavus).
- Review of Imaging and Electrodiagnostics: Critically review MRI scans for FBLPN findings (edema, atrophy of ADM), exclude other pathologies (stress fracture, tumor, severe plantar fasciitis, fat pad atrophy). Consider EMG/NCS findings. Review plain radiographs for calcaneal spurs or bone pathology.
- Discussion with Patient: Clearly explain the diagnosis, the rationale for surgery, the proposed procedure, potential risks (nerve damage, infection, scar, persistent pain, CRPS), expected outcomes, and the post-operative rehabilitation protocol. Manage expectations regarding pain relief and recovery timeline. Obtain informed consent.
-
Surgical Site Marking:
- Pre-operatively, while the patient is awake and able to provide feedback, mark the area of maximal tenderness and a tentative incision line. This helps guide the skin incision and reduce variability once the patient is anesthetized.
-
Anesthesia:
- Typically, regional anesthesia (e.g., popliteal block, ankle block) combined with monitored anesthesia care (MAC) or general anesthesia. A regional block can provide excellent post-operative pain control.
-
Tourniquet:
- A thigh tourniquet is routinely used to provide a bloodless field, which is critical for nerve identification and dissection. The tourniquet time should be carefully monitored.
Patient Positioning
- Supine Position: The patient is placed supine on the operating table.
-
Foot Positioning:
- The operative foot is typically placed in a slightly externally rotated position.
- The hip is mildly abducted and externally rotated, with the knee flexed to allow for easier access to the medial aspect of the foot.
- A soft bolster or blanket roll can be placed under the ipsilateral hip to achieve neutral rotation of the lower extremity, or under the calf to slightly elevate the foot, optimizing exposure.
- The foot should be positioned to allow easy access to the medial heel and arch without undue tension on the neurovascular structures or skin.
-
Sterile Preparation and Draping:
- The entire lower extremity, from the knee to the toes, is prepped with an antiseptic solution (e.g., chlorhexidine gluconate or povidone-iodine).
- Sterile drapes are applied to isolate the surgical field, ensuring wide exposure for potential extension of the incision if necessary. A sterile stockinette or surgical drape can be used to cover the foot, allowing manipulation.
Detailed Surgical Approach / Technique
Surgical decompression of the first branch of the lateral plantar nerve (FBLPN) requires a meticulous, layered dissection to identify and release the nerve without causing iatrogenic injury. The goal is to relieve all potential compression points along its course.
1. Incision
- A curvilinear longitudinal incision is made on the medial aspect of the heel. The incision typically extends from approximately 1-2 cm posterior to the medial malleolus, curving distally along the junction of the plantar and medial skin, just superior to the weight-bearing surface. It usually terminates around the navicular tuberosity or slightly beyond, depending on the anticipated extent of decompression required.
- The length of the incision is generally 4-6 cm. It is positioned to avoid direct weight-bearing scars.
- Incise the skin and subcutaneous tissue cautiously. The medial calcaneal nerve branches, arising from the tibial nerve (or sometimes the medial plantar nerve), are superficial and supply sensation to the medial heel. While every effort is made to preserve them, small sensory branches may be encountered and, if necessary, ligated or carefully retracted.
2. Exposure of the Abductor Hallucis Muscle
- Once through the skin and subcutaneous fat, the deep fascia overlying the abductor hallucis muscle is identified. This muscle originates from the medial process of the calcaneal tuberosity and inserts into the medial aspect of the proximal phalanx of the great toe.
- Carefully incise this investing fascia longitudinally, parallel to the muscle fibers. This exposes the belly of the abductor hallucis muscle.
- The abductor hallucis muscle is then gently retracted superiorly (or dorsally, away from the plantar aspect). This maneuver requires careful dissection to avoid undue traction on the muscle and its underlying structures.
3. Identification and Decompression of the FBLPN
- With the abductor hallucis muscle retracted, the search for the lateral plantar nerve and its first branch begins.
- The tibial nerve is typically identified first, just distal to the medial malleolus within the tarsal tunnel. It bifurcates into the medial and lateral plantar nerves. The lateral plantar nerve then runs distally and laterally.
- The first branch of the lateral plantar nerve (FBLPN) usually originates from the lateral plantar nerve approximately 1-2 cm distal to the tibial nerve bifurcation. It courses inferiorly and laterally.
- The primary compression point for the FBLPN is often a fibrous fascial band, part of the deep fascia of the abductor hallucis muscle, or a thickening of the fascia overlying the quadratus plantae. This band is incised longitudinally, releasing the nerve.
-
Step-by-step Dissection and Decompression:
- Identify the Abductor Hallucis Muscle: Retract it superiorly.
- Locate the Medial Calcaneal Tuberosity: The FBLPN often curves sharply around this bony landmark.
- Identify the Deep Fascia: This strong, fibrous band runs from the medial calcaneal tuberosity, deep to the abductor hallucis muscle. This is the main compressive structure. Incise this band completely, from its origin to where it blends into more distal structures. Use sharp dissection (e.g., tenotomy scissors, scalpel with #15 blade) and loupe magnification is highly recommended for precision.
- Trace the Nerve: Once the primary band is released, meticulously trace the FBLPN proximally to ensure all potential compression from the main lateral plantar nerve is relieved, and distally towards the abductor digiti minimi muscle.
-
Examine for Secondary Compression Points:
- Between Abductor Hallucis and Quadratus Plantae: Gently separate the abductor hallucis from the more deeply lying quadratus plantae muscle. The FBLPN may be found running between these two muscles. Ensure adequate release of any restrictive fascial borders between them.
- Near Calcaneal Spur/Plantar Fascia: If a large calcaneal spur or thickened plantar fascia is present and seen to directly impinge on the nerve, a partial release of the plantar fascia or spur removal might be considered, but only if directly compressing the nerve. This is not a routine plantar fascia release for plantar fasciitis.
- External Neurolysis: If the nerve appears scarred or constricted by perineural fibrosis, a gentle external neurolysis can be performed using fine-tipped instruments to free the nerve sheath, ensuring the epineurium is not violated.

Intraoperative view illustrating the meticulous dissection required to identify and decompress the first branch of the lateral plantar nerve (often visualized as a glistening white structure), typically after retraction of the abductor hallucis muscle.
- Confirmation of Decompression: Visually confirm that the nerve appears unconstricted throughout its course. A blunt probe should be able to pass freely along the nerve's pathway without resistance.
4. Closure
- Hemostasis: Achieve meticulous hemostasis using bipolar cautery to prevent hematoma formation, which can lead to post-operative scarring and recurrent compression.
- Irrigation: Copiously irrigate the wound with sterile saline.
-
Layered Closure:
- The abductor hallucis muscle is allowed to fall back into its anatomical position. The incised deep fascia of the abductor hallucis is typically left open to prevent re-entrapment, or loosely approximated without tension if necessary.
- Close the subcutaneous layer with absorbable sutures (e.g., 3-0 or 4-0 absorbable suture) to approximate the skin edges and minimize dead space.
- Close the skin with non-absorbable sutures (e.g., 3-0 or 4-0 nylon) using an interrupted or running subcuticular technique.
- Dressing: Apply a sterile, non-adherent dressing, followed by soft gauze and a compression bandage (e.g., conforming roll or elastic wrap). A posterior splint or walking boot may be applied for initial immobilization and protection.
Complications & Management
While generally safe, surgical decompression of the first branch of the lateral plantar nerve (FBLPN) is not without potential complications. A thorough understanding of these complications, their incidence, and appropriate management strategies is crucial for the orthopedic surgeon.
General Surgical Complications
-
Infection:
Superficial or deep wound infection. Incidence is low in foot surgery (typically <2%).
- Management: Superficial infections may respond to oral antibiotics; deep infections require surgical debridement and intravenous antibiotics.
-
Hematoma:
Collection of blood in the surgical site. Can cause pain, swelling, and increase risk of infection or nerve compression.
- Management: Small hematomas may resolve spontaneously; larger or symptomatic hematomas may require surgical evacuation. Meticulous hemostasis during surgery is key.
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE):
Risk is low in isolated foot surgery but must be considered, especially in patients with pre-existing risk factors.
- Management: Prophylaxis with early mobilization, mechanical compression devices, and consideration of anticoagulation in high-risk patients. Treatment involves anticoagulation.
-
Sural Nerve Injury:
The sural nerve is located more laterally and posteriorly, but can be at risk if the incision is placed too far laterally or if retraction is aggressive.
- Management: Prevention through careful anatomical dissection. If injured, exploration and repair (epineurial repair) may be indicated for complete transections. Neuropathic pain management for partial injuries.
Specific Complications of FBLPN Decompression
-
Persistent or Recurrent Pain (Inadequate Relief):
This is the most common and challenging complication, occurring in 10-30% of patients. It may be due to:
- Incomplete Decompression: Missed compression points (e.g., further distally, or incomplete release of the abductor hallucis fascia).
- Misdiagnosis: The original pain source was not truly FBLPN entrapment (e.g., undiagnosed plantar fasciitis, tarsal tunnel syndrome, radiculopathy, stress fracture, fat pad atrophy).
- Perineural Scarring/Fibrosis: Formation of scar tissue around the nerve post-operatively, leading to re-entrapment or neuroma-in-continuity.
- CRPS (Complex Regional Pain Syndrome): A severe, chronic pain condition that can be triggered by surgery.
- Management: Meticulous re-evaluation to determine the precise cause. This may include repeat clinical exam, imaging (MRI, ultrasound), electrodiagnostics, and diagnostic blocks. Revision surgery may be indicated for incomplete decompression or severe scarring (neurolysis, possibly nerve wrapping). Pharmacological management (gabapentin, pregabalin, tricyclic antidepressants), physical therapy, and pain management specialist referral are often necessary for neuropathic pain or CRPS.
-
Nerve Damage (Direct Trauma/Neuropraxia):
Direct injury to the FBLPN or adjacent nerves during dissection or retraction.
- Management: Prevention through meticulous technique, loupe magnification, and careful handling of neural tissue. Most neuropraxias resolve spontaneously over weeks to months. Severe or complete transections may warrant exploration and microsurgical repair.
-
Scar Hypersensitivity/Painful Scar:
The incision site can be sensitive or develop a painful neuroma within the scar tissue.
- Management: Desensitization exercises, silicone gel sheeting, topical analgesics. Local injections of anesthetic/corticosteroid may help. Excision of a symptomatic neuroma may be required in refractory cases.
-
Weakness of Abductor Digiti Minimi:
Rare, as the FBLPN is usually motor to this muscle. May indicate nerve injury or incomplete recovery.
- Management: Physical therapy focusing on intrinsic foot muscle strengthening. If due to nerve injury, management as above.
-
Medial Calcaneal Nerve Injury:
Can cause sensory loss or dysesthesia over the medial heel.
- Management: Prevention by careful dissection and retraction. Management similar to other sensory nerve injuries.
Summary of Complications & Management
| Complication | Incidence (Approx.) | Salvage Strategies / Management |
|---|---|---|
| Persistent/Recurrent Pain | 10-30% | Thorough re-evaluation (clinical, imaging, electrodiagnostics, blocks). Revision surgery (if incomplete decompression/scarring). Pharmacological management (neuropathic pain agents). Physical therapy. Pain management referral. |
| Infection | <2% | Oral antibiotics for superficial, debridement + IV antibiotics for deep. |
| Hematoma | Low | Observation for small, evacuation for large/symptomatic. Meticulous hemostasis. |
| Nerve Damage (FBLPN/Sural) | Low | Meticulous technique, loupe magnification. Observation for neuropraxia. Microsurgical repair for complete transections. |
| Scar Hypersensitivity/Painful Scar | Low | Desensitization, silicone sheeting, topical agents. Local injections. Excision of symptomatic neuroma. |
| CRPS (Complex Regional Pain Syndrome) | Rare | Early recognition. Aggressive multimodal pain management (pharmacology, nerve blocks, PT, psychological support). |
| DVT/PE | Rare | Prophylaxis (early mobilization, mechanical). Anticoagulation for treatment. |
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical to optimize outcomes, reduce complications, and facilitate a timely return to function following FBLPN decompression. The protocol generally phases from protection and pain management to early mobilization, then progressive strengthening and functional training.
Phase 1: Immediate Post-Operative (Days 0-14)
Goals: Protect surgical site, manage pain and swelling, promote wound healing.
- Weight Bearing: Non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) with crutches or walker. The foot is typically protected in a rigid sole shoe, CAM walker boot, or posterior splint for comfort and protection.
- Elevation & Ice: Maintain constant elevation of the foot above heart level to minimize swelling. Apply ice packs to the surgical site for 15-20 minutes every 2-3 hours.
- Pain Management: Prescribed oral analgesics and anti-inflammatory medications. Regional nerve blocks performed pre-operatively can provide significant immediate post-operative pain relief.
- Wound Care: Keep the dressing clean and dry. Inspect the wound for signs of infection or hematoma at regular intervals. Suture removal typically at 10-14 days post-op.
- Gentle Range of Motion (ROM): Begin gentle active ankle dorsiflexion and plantarflexion, and toe curls, avoiding excessive inversion/eversion or forced great toe abduction initially, to prevent tension on the healing nerve. Start only once initial pain is controlled and wound integrity is stable (often after 3-5 days).
Phase 2: Early Mobilization & Healing (Weeks 2-6)
Goals: Gradually increase weight-bearing, restore pain-free ROM, begin gentle soft tissue mobilization.
- Weight Bearing: Gradually progress from NWB/TDWB to partial weight-bearing (PWB), then full weight-bearing (FWB) in the protective boot, as tolerated and based on surgeon's discretion and patient comfort. Transition from crutches to a single crutch or cane as strength improves.
-
Therapeutic Exercises:
- Ankle ROM: Continue active and gentle passive ankle ROM exercises (dorsiflexion, plantarflexion, inversion, eversion).
- Subtalar ROM: Gentle subtalar joint mobilization.
- Toe Flexion/Extension: Continue with intrinsic foot muscle activation.
- Nerve Gliding Exercises: Once sutures are removed and wound is stable, initiate gentle nerve gliding exercises for the tibial and plantar nerves to prevent adhesion formation and promote nerve mobility. (e.g., seated straight leg raise with foot dorsiflexion, then plantarflexion with neck flexion/extension).
- Soft Tissue Mobilization: Gentle scar massage and desensitization around the incision site to prevent adhesions and reduce scar hypersensitivity.
- Modalities: Continue ice as needed for swelling. Consider ultrasound or electrical stimulation for pain and tissue healing, if indicated.
- Footwear: Once FWB in the boot, transition to supportive athletic shoes with good arch support. Custom orthotics may be considered if pre-existing biomechanical abnormalities were a contributing factor.
Phase 3: Strengthening & Functional Progression (Weeks 6-12)
Goals: Restore full strength, endurance, proprioception, and return to normal activities.
- Footwear: Transition fully to supportive shoes.
-
Strengthening Exercises:
- Intrinsic Foot Muscles: Towel curls, marble pick-ups, short foot exercises.
- Ankle Strengthening: Theraband exercises for ankle dorsiflexion, plantarflexion, inversion, and eversion. Calf raises (bilateral to unilateral).
- Balance & Proprioception: Single leg stance, wobble board/BAPS board exercises, uneven surface walking.
- Stretching: Gentle stretching of the calf muscles (gastroc-soleus complex) and plantar fascia (if co-existing tightness).
-
Progressive Activity:
- Gradual return to daily activities.
- Low-impact cardio (e.g., stationary cycling, elliptical).
- Walking progression: gradually increase distance and speed.
- Nerve Gliding: Continue regular nerve gliding exercises.
- Advanced Neuromuscular Control: Incorporate exercises that challenge the foot and ankle in functional patterns.
Phase 4: Return to Sport / High-Impact Activities (Weeks 12+)
Goals: Achieve full functional return, prevent recurrence.
- Sport-Specific Training: Gradually introduce sport-specific drills, agility training, plyometrics, and higher-impact activities, ensuring adequate warm-up and cool-down.
- Running Progression: Begin with a walk/jog program, progressively increasing jogging time and distance, ensuring no exacerbation of symptoms.
- Orthotics Review: Re-evaluate the need for custom orthotics or shoe inserts to optimize foot mechanics and reduce recurrence risk.
- Maintenance: Continue a home exercise program focusing on strength, flexibility, and nerve mobility.
Expected Outcomes and Return to Activity:
Most patients experience significant improvement in pain by 3-6 months. Full recovery and return to pre-injury activity levels can take 6-12 months. Some residual numbness, tingling, or scar sensitivity may persist but typically does not significantly impair function. Patient compliance with the rehabilitation protocol is crucial for optimal results.
Summary of Key Literature / Guidelines
The understanding and management of lateral plantar nerve entrapment, or Baxter's neuropathy, have evolved through seminal clinical observations and advancements in diagnostic imaging and surgical techniques. While not as extensively studied as common conditions like plantar fasciitis, a consistent body of literature supports its recognition and surgical decompression in carefully selected patients.
-
Seminal Work by Baxter: Dr. Donald E. Baxter's work in the 1980s was pivotal in delineating the clinical entity of FBLPN entrapment as a distinct cause of chronic heel pain. His initial descriptions highlighted the anatomical course of the nerve and the common compression sites, bringing attention to this often-misdiagnosed condition. He emphasized the characteristic pain pattern and the importance of specific physical examination findings, particularly tenderness to palpation and Tinel's sign.
-
Diagnostic Modalities:
- MRI: Multiple studies have emphasized the utility of MRI as the preferred imaging modality. Features such as denervation atrophy (fatty infiltration) and edema within the abductor digiti minimi muscle, or directly visualizing nerve edema or thickening, are highly suggestive of FBLPN entrapment. However, it is crucial to note that normal MRI findings do not definitively rule out the condition. MRI also serves to exclude other causes of heel pain.
- Electrodiagnostic Studies (EMG/NCS): While considered an objective diagnostic tool for nerve entrapments, the diagnostic yield of EMG/NCS for FBLPN is variable and often low, reported to be positive in only 30-60% of cases. This is attributed to the nerve's small caliber, primarily motor function, and deep location. Consequently, a negative EMG/NCS does not preclude the diagnosis.
- Diagnostic Block: The most consistently cited diagnostic tool for confirming FBLPN entrapment is a targeted, ultrasound-guided diagnostic injection of local anesthetic around the nerve. Significant, temporary pain relief (e.g., >50% reduction) is considered highly predictive of a positive surgical outcome.
-
Surgical Efficacy and Outcomes:
- Studies on surgical decompression of the FBLPN consistently report good to excellent outcomes in 70-90% of appropriately selected patients. Success is highly correlated with accurate pre-operative diagnosis and the absence of other underlying pathologies.
- Various surgical approaches (open vs. endoscopic) have been described. The traditional open medial approach, as detailed above, remains the most common and provides excellent visualization for complete decompression of all potential entrapment sites. Endoscopic techniques have been explored but may carry a higher risk of incomplete release or direct nerve injury due to limited visualization.
- Factors influencing outcome include duration of symptoms (shorter duration often associated with better outcomes), absence of diffuse neuropathy (e.g., severe diabetes), and patient motivation.
-
Differentiation from Plantar Fasciitis: A significant focus in the literature has been on differentiating FBLPN entrapment from recalcitrant plantar fasciitis. While both cause heel pain, the pain characteristics, location of maximal tenderness, and response to specific interventions (e.g., nerve blocks vs. plantar fascia injections) often help distinguish them. It is important to recognize that they can co-exist. Some surgeons advocate for a concomitant partial plantar fasciotomy if a thickened fascia is directly impinging the nerve during decompression, but this is not routinely performed for isolated FBLPN entrapment.
-
Controversies and Future Directions:
- Optimal Diagnostic Pathway: The ideal sequence and weight of diagnostic tests (clinical exam, MRI, EMG, diagnostic block) remain a subject of debate, particularly given the limitations of objective tests.
- Role of Dynamic Compression: Further research into the dynamic biomechanical factors contributing to FBLPN compression during gait and activity may refine diagnostic and surgical strategies.
- Revision Surgery: Management of persistent pain after initial FBLPN decompression continues to be challenging, with variable outcomes for revision neurolysis.
- Endoscopic vs. Open: Comparative studies with robust methodology are needed to definitively establish the superiority of one surgical approach over the other regarding efficacy and complication rates.
In conclusion, FBLPN entrapment is an important, though often overlooked, cause of chronic heel pain. A meticulous clinical evaluation, supported by targeted imaging and diagnostic blocks, is essential for accurate diagnosis. Surgical decompression, performed with a thorough understanding of the regional anatomy, offers a reliable solution for recalcitrant cases, providing significant relief for a substantial number of patients. Continued research will undoubtedly refine our diagnostic capabilities and treatment paradigms for this challenging condition.
Clinical & Radiographic Imaging

You Might Also Like