Achilles Tendon Rupture: Comprehensive Guide to Epidemiology, Anatomy, Biomechanics, and the Critical Watershed Zone
Key Takeaway
An Achilles tendon rupture is a common injury in middle-aged 'weekend warriors.' Most ruptures occur in the hypovascular 'watershed zone,' 2-6 cm proximal to the calcaneal insertion. This critical zone's limited blood supply contributes to degenerative changes and reduced healing, making its understanding paramount for effective diagnosis and management.
Introduction & Epidemiology
Acute Achilles tendon rupture represents a common and debilitating injury, primarily affecting middle-aged individuals involved in recreational sports. The typical patient profile is a male, aged 30-50 years, often referred to as a "weekend warrior," engaging in activities requiring sudden push-off movements or rapid changes in direction, such as basketball, tennis, or soccer. Less frequently, ruptures can occur in sedentary individuals or in association with systemic conditions like diabetes mellitus, rheumatoid arthritis, or corticosteroid use, which may compromise tendon integrity.
The incidence of Achilles tendon rupture is reported to be increasing, with estimates ranging from 5 to 30 per 100,000 population annually. This trend is often attributed to an aging, yet increasingly active, demographic. The mechanism of injury typically involves a sudden eccentric load applied to the actively contracting gastrocnemius-soleus complex, often during ankle dorsiflexion simultaneous with knee extension (e.g., jumping, sprinting, or falling from a height). Patients typically describe a sudden "pop" or "snap" sensation, often likening it to being struck from behind, followed by immediate pain and difficulty with push-off.
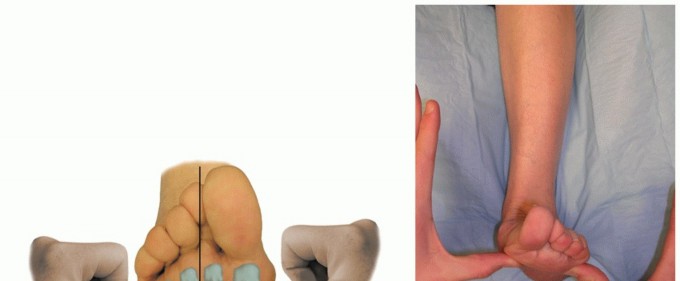
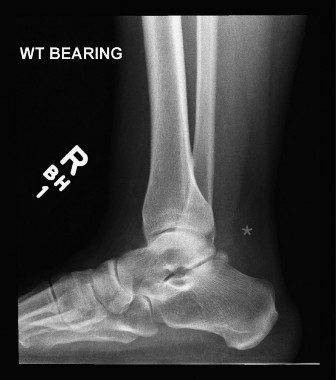
Clinically, the diagnosis is usually straightforward, characterized by a palpable gap in the tendon, weakness in plantarflexion, and a positive Thompson test. Imaging, particularly MRI, can confirm the diagnosis, delineate the extent of rupture, quantify gap size, and rule out other pathologies, though it is not always necessary for acute cases. The vast majority of acute ruptures occur within the mid-substance of the tendon, specifically in a region approximately 2-6 cm proximal to its calcaneal insertion. This region is critically important due to its relatively hypovascular nature, often referred to as the "watershed zone" or "critical zone," which significantly impacts both the etiology of rupture and the subsequent healing process, irrespective of treatment modality. Understanding the specific characteristics of this watershed zone is paramount for effective management and prognostication.
Surgical Anatomy & Biomechanics
The Achilles tendon, or calcaneal tendon, is the thickest and strongest tendon in the human body, formed by the conjoined aponeuroses of the gastrocnemius and soleus muscles (triceps surae complex) and inserting into the posterior aspect of the calcaneus.
Tendon Structure and Composition
The Achilles tendon is composed predominantly of type I collagen fibers, arranged in a highly organized, parallel fashion, providing significant tensile strength. Collagen fibers are grouped into fascicles, which are enveloped by endotenon. The entire tendon is surrounded by a paratenon, a loose connective tissue sheath that facilitates gliding and contains a rich vascular network. Unlike tendons with a true synovial sheath, the Achilles tendon's paratenon provides its primary external blood supply. The fascicles within the Achilles tendon exhibit a characteristic spiraling course along its length, undergoing up to 90 degrees of rotation from proximal to distal. This helical arrangement is thought to distribute stress evenly across the tendon during movement and contribute to its biomechanical efficiency.
Musculotendinous Complex
The gastrocnemius muscle originates from the medial and lateral femoral condyles and is primarily a knee flexor and ankle plantarflexor. The soleus muscle originates from the posterior tibia and fibula and is a pure ankle plantarflexor. Both contribute significantly to activities requiring push-off, propulsion, and stabilization during gait. The plantaris tendon, when present, lies deep to the medial head of the gastrocnemius and superficial to the soleus, eventually merging with the Achilles tendon or inserting separately. While its contribution to plantarflexion is minimal, it can be harvested as an autograft for tendon augmentation.
Innervation and Vascularity
The triceps surae complex is innervated by the tibial nerve (S1, S2). Of particular surgical relevance is the sural nerve, a sensory nerve arising from the tibial and common peroneal nerves, which courses subcutaneously along the posterior calf, often running close to the lateral border of the Achilles tendon. It is highly susceptible to iatrogenic injury during posterior surgical approaches.
The vascular supply to the Achilles tendon is complex and multifaceted, arising from three primary sources:
1.
Musculotendinous junction (proximal):
Branches from the posterior tibial artery and peroneal artery supply the proximal third.
2.
Paratenon (mid-substance):
A robust network of vessels within the paratenon provides the primary supply to the tendon's mid-portion.
3.
Osseotendinous junction (distal):
Branches from the peroneal artery, posterior tibial artery, and calcaneal arterial arcade supply the insertion site.
Critically, a relatively hypovascular zone, the "watershed zone," exists approximately 2-6 cm proximal to the calcaneal insertion. This region receives its blood supply predominantly from the paratenon, with fewer direct penetrating vessels compared to the proximal and distal ends. This relative paucity of direct vascularity renders the watershed zone particularly susceptible to degenerative changes, reduced healing capacity, and is consequently the most common site for acute ruptures. The vascular compromise in this zone is thought to contribute to the degenerative changes that precede rupture and can complicate healing, making robust surgical repair and biological augmentation strategies particularly relevant for injuries in this region.

Biomechanics of Rupture
The Achilles tendon can withstand significant tensile forces, estimated at up to 10 times body weight. Rupture typically occurs when an acute load exceeds the tendon's ultimate tensile strength, often in the presence of underlying degenerative changes. Such degenerative changes, including myxoid degeneration, collagen disorganization, and tenocyte apoptosis, are frequently observed histologically in ruptured tendons, even in seemingly healthy individuals, and are more pronounced in the hypovascular watershed zone. The most common mechanism involves a sudden, forceful ankle dorsiflexion while the gastrocnemius-soleus complex is contracting eccentrically (e.g., landing from a jump, sudden acceleration). The mechanical stress, coupled with compromised local vascularity, culminates in macroscopic tendon failure.
Indications & Contraindications
The management of acute Achilles tendon ruptures remains a subject of ongoing debate, with both operative and non-operative strategies demonstrating comparable functional outcomes in many studies, albeit with different risk profiles. The decision-making process is individualized, taking into account patient factors, injury characteristics, and surgeon preference.
Operative Indications
Operative management is generally favored for patients seeking to maximize strength and power, aiming for a faster return to high-level athletic activity, or in situations where non-operative treatment has a higher likelihood of failure.
- Young, active individuals: Especially athletes or those with high functional demands.
- Large tendon gap (>1 cm) on clinical examination or imaging: Indicates significant retraction and makes non-operative healing less predictable.
- Delayed presentation (typically >2-4 weeks post-injury): Chronic ruptures often require surgical intervention due to scarring, retraction, and poor healing potential of the gap.
- Rerupture following non-operative treatment: Suggests insufficient healing capacity or inadequate initial management.
- Failed non-operative treatment: Persistent pain, weakness, or inability to perform a single-leg heel raise.
- Desire for stronger, more reliable repair: Reduces the risk of rerupture compared to non-operative treatment, though this benefit is debated in modern rehabilitation protocols.
Non-Operative Indications
Non-operative treatment is increasingly utilized, especially with advancements in functional rehabilitation protocols that incorporate early protected motion and weight-bearing. It is often preferred for patients where the risks of surgery outweigh the potential benefits.
- Elderly or sedentary individuals: Lower functional demands and reduced desire for high-level athletic return.
- Significant medical comorbidities: Patients with diabetes, peripheral vascular disease, immunosuppression, or other conditions that increase surgical risks (e.g., wound healing complications, infection, DVT).
- Small tendon gap (<1 cm) and good apposition: Suggests a higher likelihood of successful non-operative healing.
- Patients unwilling or unable to undergo surgery: Due to personal preference, social factors, or financial constraints.
- High risk for surgical complications: History of previous wound complications, significant skin issues, or known sural nerve neuropathy.
- Non-compliant patient: Patients unlikely to adhere to strict post-operative rehabilitation protocols.
Contraindications
Absolute Contraindications for Surgery:
* Active local or systemic infection.
* Severe peripheral vascular disease with critical limb ischemia.
* Uncontrolled diabetes with severe microvascular complications or neuropathy.
* Non-ambulatory status.
* Severe medical comorbidities precluding safe anesthesia and surgery.
Relative Contraindications for Surgery:
* Extensive skin damage or open wounds in the surgical field.
* Extremely fragile or thin skin (e.g., due to long-term corticosteroid use).
* Patient non-compliance with post-operative regimen.
Summary Table: Operative vs. Non-Operative Indications
| Feature / Indication | Operative Management (Favored) | Non-Operative Management (Favored) |
|---|---|---|
| Patient Age | Young (<60 years) | Elderly (>60-65 years) |
| Activity Level | Active, Athlete, High demand | Sedentary, Low demand |
| Tendon Gap (Acute) | Large (>1 cm) | Small (<1 cm), good apposition |
| Time from Injury | Acute, Delayed (>2-4 weeks) | Acute (within 1-2 weeks) |
| Rerupture | Yes | No prior rerupture |
| Comorbidities | Few, well-controlled | Multiple, poorly controlled (DM, PVD) |
| Desired Outcome | Maximize strength, quick return to sport | Avoid surgical risks, acceptable function |
| Surgical Risk | Acceptable | High (e.g., wound, infection) |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is critical for optimizing surgical outcomes and minimizing complications. This includes meticulous patient evaluation, appropriate imaging, patient education, and detailed surgical setup.
Pre-Operative Assessment
- History and Physical Examination: Confirm diagnosis, assess neurological status (especially sural nerve function), evaluate skin integrity, and document any comorbidities.
-
Imaging:
While clinical diagnosis is often sufficient, MRI or ultrasound can provide valuable information, especially for delayed presentations or ambiguous cases.
- MRI: Accurately delineates the rupture site, gap size, extent of tendon retraction, quality of tendon tissue, and can identify chronic changes, scar tissue, or associated pathologies (e.g., plantaris rupture). This is particularly useful when planning for augmentation in chronic cases.
- Ultrasound: Dynamic assessment of the gap, though operator-dependent. Can be used for real-time guidance in percutaneous repairs.
- Medical Optimization: Ensure all comorbidities (e.g., diabetes, hypertension) are optimally managed. Cessation of smoking is strongly encouraged to improve wound healing.
- DVT Prophylaxis: Assess DVT risk based on Caprini score and institute appropriate pharmacological and mechanical prophylaxis.
- Antibiotics: Administer intravenous broad-spectrum antibiotics (e.g., Cefazolin) within 60 minutes prior to incision, as per institutional protocol, and continue for 24 hours post-operatively if deemed necessary.
- Patient Education: Comprehensive discussion regarding the surgical procedure, potential risks (infection, wound complications, sural nerve injury, rerupture), expected recovery timeline, and the importance of strict adherence to the post-operative rehabilitation protocol.
Patient Positioning
- Prone Position: This is the standard position for posterior approaches to the Achilles tendon. The patient is carefully positioned prone on the operating table.
- Padding: Meticulous padding of all pressure points (face, chest, iliac crests, knees, ankles, dorsum of feet) is essential to prevent pressure sores or nerve palsies. A gel roll or similar device can be placed longitudinally under the chest to allow for diaphragmatic excursion.
- Tourniquet: A high thigh tourniquet is applied to the ipsilateral leg to achieve a bloodless field, crucial for precise dissection and identification of delicate structures. The tourniquet cuff should be adequately padded.
- Sterile Prep and Drape: The entire lower extremity, from the midthigh to the toes, is prepared with an antiseptic solution (e.g., chlorhexidine or povidone-iodine) and draped in a sterile fashion, ensuring adequate exposure of the Achilles tendon and calcaneal insertion. A sterile stockinette can be applied, and the foot positioned for easy manipulation (e.g., slightly plantarflexed).
- Ankle Position: The ankle is often held in slight plantarflexion (approximately 15-20 degrees) during repair to reduce tension on the tendon ends, although this can be adjusted during the repair process. This position can be maintained with a bolster under the ankle or by an assistant.
Detailed Surgical Approach / Technique
The goal of Achilles tendon repair is to achieve a strong, anatomically reduced repair that allows for early functional rehabilitation while minimizing complications, particularly wound issues and sural nerve injury. The choice between open, mini-open, or percutaneous repair depends on surgeon experience, patient factors, and acute vs. chronic presentation. This section focuses on a standard open repair, as it allows for direct visualization and robust tissue handling, particularly critical for injuries within the watershed zone.
Open Repair Technique
-
Incision:
- Longitudinal Posterior Incision: Traditionally, a straight midline posterior incision (10-15 cm) centered over the rupture site is used. While offering excellent exposure, it carries a higher risk of wound healing complications due to the relatively poor vascularity of the skin in this region and direct pressure from footwear.
- Medial or Lateral Para-Achilles Incision: A more favorable approach involves a longitudinal incision placed slightly medial or lateral to the midline (e.g., 1-2 cm medial to the palpable tendon). This allows for tendon exposure while preserving a vascularized skin bridge over the repair site. The lateral para-Achilles incision is often preferred as it places the incision further away from the path of the sural nerve, which typically courses inferolaterally.
-
Soft Tissue Dissection:
- Careful incision of the skin and subcutaneous tissue is performed.
- Sural Nerve Identification and Protection: Immediately after incising the skin, identify and protect the sural nerve. The sural nerve typically crosses the lateral border of the Achilles tendon around 10-15 cm proximal to the calcaneal insertion and then runs inferolaterally towards the fifth metatarsal. It can often be visualized or palpated beneath the superficial fascia. Gently dissect and retract the nerve laterally to prevent iatrogenic injury. This is a critical step.
- Incise the paratenon longitudinally. Preserve as much of the paratenon as possible, as it is a vital source of blood supply to the tendon, especially in the watershed zone.
-
Debridement and Tendon End Preparation:
- Identify the ruptured tendon ends. The proximal end is usually retracted significantly, often several centimeters cephalad, due to the unopposed pull of the gastrocnemius-soleus complex. The distal end remains attached to the calcaneus.
- Evacuate any hematoma and meticulously debride necrotic or severely frayed tendon tissue. The goal is to create clean, viable tendon stumps, but excessive debridement should be avoided to preserve tendon length and intrinsic healing potential. The watershed zone often shows evidence of chronic degenerative changes, which should be carefully assessed for viability.
-
Tendon Reduction and Suture Placement:
- Position the foot in approximately 15-20 degrees of plantarflexion to relax the gastrocnemius-soleus complex and facilitate apposition of the tendon ends. An assistant can maintain this position.
- A strong, non-absorbable suture material (e.g., FiberWire, Ethibond #2 or #5) is typically used.
- The modified Kessler suture or Krakow locking loop stitch are common techniques. Multiple strands (e.g., 4 or 6 strands) are often preferred for maximal strength.
- For the Krakow stitch : Pass the suture longitudinally through the tendon substance, locking it with transverse bites. This creates multiple loops and minimizes gapping. Start proximally and work distally, and vice versa.
- For the modified Kessler : A central core stitch is passed through the tendon ends, with locking loops at the periphery.
- Ensure adequate tendon purchase, typically 2-3 cm from the ruptured edge, especially in the watershed zone where tissue quality might be compromised. The sutures should engage healthy tendon tissue to prevent pull-out.
- Once sutures are placed in both proximal and distal ends, bring the tendon ends together under appropriate tension. The goal is to achieve an anatomical reduction with firm apposition of the tendon ends without excessive tension. Knot tying is performed, usually with the foot in the desired plantarflexed position. The knots should be buried where possible to minimize irritation.
-
Augmentation (as indicated):
- For chronic ruptures, large gaps, poor tissue quality in the watershed zone, or reruptures, augmentation may be necessary.
- Plantaris Tendon Autograft: If present, the plantaris tendon can be harvested (typically via the same incision, deep to the gastrocnemius) and used to augment the repair by weaving it across the repair site.
- Flexor Hallucis Longus (FHL) Transfer: For chronic ruptures with significant retraction or tissue loss, FHL transfer is a robust option. The FHL tendon is harvested from the plantar foot or posteromedial ankle, released distally, rerouted through the calcaneus or through the Achilles tendon, and fixed with interference screws or sutures.
- Gastrocnemius Recession/V-Y Lengthening: In chronic cases with significant muscle-tendon unit contracture, these procedures may be necessary to gain length and allow for tension-free repair.
- Allografts/Synthetics: Rarely used for acute ruptures, but can be considered for revision surgery or extensive defects.
-
Closure:
- Carefully repair the paratenon with absorbable sutures (e.g., 3-0 or 4-0 Vicryl). This provides an important gliding layer and helps to contain the repair, facilitating revascularization.
- Close the subcutaneous tissue with absorbable sutures.
- Close the skin with interrupted non-absorbable sutures or staples.
- Apply a sterile dressing.
- Post-operative Immobilization: Apply a posterior splint or short leg cast, maintaining the ankle in a slight plantarflexion (typically 15-20 degrees) to protect the repair and reduce tension.
Minimally Invasive / Percutaneous Techniques
These techniques utilize smaller incisions, aiming to reduce wound complications and sural nerve injury.
*
Percutaneous techniques:
Small stab incisions are made, and sutures are passed using specialized needles (e.g., Achillon device, various suture passer systems). Less direct visualization, potentially leading to less robust repairs or inclusion of peritenon. Higher rerupture rate in some studies, but lower wound complication rate.
*
Mini-open techniques:
A small, typically transverse, incision is made directly over the rupture site, allowing limited direct visualization of the tendon ends for suture placement. Can be combined with percutaneous suture passage.
While these techniques offer cosmetic and potentially wound-related benefits, the open technique provides direct visualization of the integrity of the tendon ends within the watershed zone, allowing for precise debridement and robust suture placement, which can be crucial for successful healing in this compromised area.
Complications & Management
Despite advancements in surgical techniques and rehabilitation, Achilles tendon repair is associated with a range of potential complications. Understanding their incidence and appropriate management strategies is critical for orthopedic surgeons.
General Complications
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE):
Incidence varies (0.5-2.0% for DVT, lower for PE). Prophylaxis is crucial.
- Management: Pharmacological (low molecular weight heparin, oral anticoagulants) and mechanical (TED hose, pneumatic compression devices) prophylaxis. Early mobilization.
-
Infection:
Superficial (2-5%) vs. Deep (<1%). Higher rates in open repairs.
- Management: Superficial infections may respond to oral antibiotics and local wound care. Deep infections typically require surgical debridement, IV antibiotics, and possibly hardware removal if augmentation was used.
Specific Surgical Complications
-
Wound Healing Complications:
Incidence ranges from 5-20% for open repairs, significantly lower for percutaneous/mini-open. Includes dehiscence, necrosis, delayed healing. The skin over the Achilles is thin with poor vascularity, especially in the watershed area.
- Management: Conservative management for minor dehiscence (dressing changes, offloading). Debridement, wound VAC, and potentially plastic surgery consultation (local flaps, skin grafts) for significant necrosis or deep infection.
-
Sural Nerve Injury:
Incidence 2-10%, higher in percutaneous repairs if not careful, but also a risk in open approaches, especially with lateral incisions not performed meticulously. Can result in numbness, paresthesias along the lateral foot, or painful neuroma.
- Management: Conservative management for neurapraxia (symptoms often resolve). Surgical exploration and neurolysis for persistent, debilitating symptoms or proven transection. Neuroma excision if refractory.
-
Rerupture:
Incidence 1-5% for operative repairs, historically higher for non-operative but recent studies suggest similar rates with accelerated rehab.
- Management: Often requires revision surgery. For acute rerupture, direct repair might be possible. For chronic rerupture, augmentation (FHL transfer, gastrocnemius flap, allograft) is typically necessary.
-
Adhesions/Stiffness:
Incidence 5-15%. Scar tissue can tether the tendon, restricting motion.
- Management: Aggressive physical therapy, stretching, early range of motion. Manipulation under anesthesia or surgical adhesiolysis in refractory cases.
-
Tendon Lengthening/Weakness:
Over-lengthening (lax repair) leads to persistent weakness in push-off.
- Management: Often managed conservatively with strengthening exercises. Revision surgery with shortening or augmentation may be considered in severe cases causing significant functional impairment.
-
Suture Irritation/Granuloma:
Knots, especially if superficially placed, can cause pain and irritation.
- Management: Local injection for mild irritation. Surgical excision of granuloma or superficial knots if conservative measures fail.
Summary Table: Common Complications and Management
| Complication | Incidence (Approximate) | Salvage Strategies / Management |
|---|---|---|
| Wound Dehiscence/Necrosis | 5-20% (open); 1-5% (percut.) | Local wound care, serial debridement, VAC, plastic surgery (flaps, grafts) |
| Sural Nerve Injury | 2-10% | Observation (neurapraxia), neurolysis, neuroma excision |
| Rerupture | 1-5% (operative) | Revision direct repair, FHL transfer, allograft augmentation |
| Infection | Superficial: 2-5%; Deep: <1% | Oral/IV antibiotics, surgical debridement, hardware removal |
| Adhesions/Stiffness | 5-15% | Aggressive PT, manipulation under anesthesia, adhesiolysis |
| Tendon Lengthening/Weakness | Varies | Concentric/eccentric strengthening, revision shortening/augmentation |
| DVT/PE | 0.5-2.0% | Pharmacological & mechanical prophylaxis, early mobilization |
| Suture Irritation | <5% | Local injection, surgical knot/granuloma excision |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as crucial as the surgical repair itself for achieving optimal functional outcomes and minimizing complications. Protocols have evolved significantly from prolonged immobilization to early protected motion and weight-bearing, aiming to balance tendon healing with prevention of stiffness and muscle atrophy. While specific protocols may vary slightly between institutions and surgeons, the underlying principles remain consistent.
Phases of Rehabilitation
Phase 1: Early Immobilization & Protection (Weeks 0-2/3)
*
Goal:
Protect the repair, reduce pain and swelling, initiate wound healing.
*
Immobilization:
Initial posterior splint or short leg cast (non-weight-bearing) with the ankle in 15-20 degrees of plantarflexion.
*
Weight-Bearing:
Strictly non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) with crutches.
*
Exercises:
* Toe wiggles to promote circulation.
* Knee flexion/extension (if splint allows).
* Hip exercises.
* Upper body conditioning.
*
Wound Care:
Meticulous wound care, elevation, ice.
*
Transition:
At 1-2 weeks, sutures/staples are removed. The splint is typically replaced with a controlled ankle motion (CAM) boot or brace.
Phase 2: Graduated Protected Motion & Partial Weight-Bearing (Weeks 2/3 - 6/8)
*
Goal:
Gradually restore range of motion (ROM), initiate controlled weight-bearing, maintain muscle function.
*
Immobilization:
CAM boot.
*
Weight-Bearing:
Gradual increase from partial weight-bearing (PWB) to full weight-bearing (FWB) over 4-6 weeks, as tolerated, while in the CAM boot. Often initiated at 2-3 weeks post-op.
*
ROM:
* Boot initially locked in plantarflexion (e.g., 15-20 degrees).
* Gradually decrease plantarflexion by 5-10 degrees every 1-2 weeks, allowing incremental dorsiflexion.
* Active plantarflexion exercises initiated. Gentle, passive dorsiflexion (within boot limits) if specified.
* Non-weight-bearing ankle ROM exercises (e.g., alphabet, gentle active plantar/dorsiflexion without resistance) when out of the boot for hygiene.
*
Exercises:
* Stationary bike with heel on pedal (no resistance initially).
* Hip and knee strengthening.
* Core stability.
Phase 3: Progressive Strengthening & Full Weight-Bearing (Weeks 6/8 - 12/16)
*
Goal:
Regain full active and passive ROM, normalize gait, restore strength and endurance.
*
Immobilization:
Transition out of CAM boot and into supportive athletic shoes. Some protocols advocate a heel lift initially.
*
Weight-Bearing:
Full weight-bearing without restrictions.
*
ROM:
Progress to full active and passive dorsiflexion. Continue gentle stretching.
*
Exercises:
* Progressive resistance exercises for plantarflexors (seated and standing calf raises, initially bilateral, then unilateral).
* Theraband exercises for all ankle planes.
* Proprioceptive training (balance board, single-leg stance).
* Elliptical trainer, swimming, stationary bike with resistance.
* Gait training to normalize walking pattern.
* Light functional activities.
Phase 4: Return to Activity & Advanced Strengthening (Months 4-6+)
*
Goal:
Prepare for return to sport/high-impact activities, achieve maximal strength and power, prevent rerupture.
*
Exercises:
* Plyometric exercises (box jumps, hopping, jumping rope) – initiated cautiously.
* Sport-specific drills (cutting, agility).
* Gradual return to running (start with jogging, progress to sprinting).
* Eccentric calf strengthening (e.g., calf raises over a step).
* Continue maintenance strengthening and flexibility.
*
Return to Sport:
Typically not before 6 months, and only after meeting objective criteria:
* Full pain-free ROM.
* Near-normal calf girth.
* Single-leg heel raise endurance (e.g., >20 repetitions on affected side, >80-90% of unaffected side).
* Satisfactory performance on hop tests and sport-specific functional tests.
* Psychological readiness.
Key Considerations
- Individualization: Protocols must be tailored to the patient's age, activity level, tissue quality (especially in the watershed zone), compliance, and progress.
- Pain-Guided Progression: Progression should be guided by pain and swelling, not strictly by timeline.
- Communication: Close communication between the surgeon, physical therapist, and patient is essential.
- Eccentric Training: Crucial for tendon remodeling and strengthening in later phases.
Modern accelerated rehabilitation protocols, which incorporate early protected weight-bearing and motion, have demonstrated superior outcomes in terms of earlier functional return and reduced stiffness, without increasing the rerupture rate compared to traditional prolonged immobilization. This approach facilitates better nutrient exchange and collagen organization in the healing tendon, potentially benefiting the compromised vascularity of the watershed zone.
Summary of Key Literature / Guidelines
The management of acute Achilles tendon ruptures has been a subject of extensive research and debate, with various meta-analyses and randomized controlled trials attempting to define optimal treatment strategies. Key areas of focus include comparing operative versus non-operative management, evaluating different surgical techniques, and defining optimal rehabilitation protocols.
Operative vs. Non-Operative Management
Historically, operative repair was favored due to a perceived lower rerupture rate. However, modern non-operative protocols, employing functional bracing and early protected weight-bearing, have significantly narrowed this gap.
*
Rerupture Rate:
Multiple systematic reviews and meta-analyses (e.g., studies by Soroceanu et al., Bhandari et al., and Olsson et al.) generally indicate a statistically lower rerupture rate with operative management (around 2-5%) compared to non-operative treatment (around 5-15% historically, but reducing to 5-8% with modern protocols). This difference, while statistically significant, may not always be clinically significant for all patient groups, especially with advanced non-operative protocols.
*
Complications:
Operative management carries a higher risk of wound complications (e.g., infection, dehiscence, sural nerve injury), while non-operative management has a higher risk of rerupture. The overall complication rates, when all adverse events are considered, are often found to be similar between the two approaches.
*
Functional Outcomes:
Most studies demonstrate comparable functional outcomes (e.g., using Achilles Tendon Rupture Score [ATRS] or Calf Muscle Performance Index) between operative and non-operative groups at 1-2 years post-injury, provided both are followed by structured rehabilitation. Operative repair may lead to slightly greater plantarflexion strength and endurance in some cohorts, particularly younger, active individuals.
*
Cost-Effectiveness:
Studies on cost-effectiveness are mixed, with some suggesting non-operative treatment to be more cost-effective due to fewer surgical complications, while others find operative treatment to be cost-effective in the long run due to lower rerupture rates.
Surgical Techniques
- Open Repair: Provides direct visualization, allowing for meticulous debridement and robust suture placement, which is particularly beneficial when dealing with poor tissue quality in the watershed zone or chronic ruptures. It carries a higher risk of wound complications.
- Minimally Invasive/Percutaneous Repair: Aims to reduce wound complications and sural nerve injury. Meta-analyses suggest these techniques may have a lower wound complication rate compared to open repair but potentially a slightly higher rerupture rate in some older studies, possibly due to less robust repair. Sural nerve injury remains a concern if proper technique and anatomical knowledge are not strictly adhered to. Recent advancements in percutaneous devices have improved outcomes.
Rehabilitation Protocols
-
Early Functional Rehabilitation:
The paradigm has shifted from prolonged immobilization to early protected weight-bearing and controlled range of motion. Systematic reviews consistently show that early functional rehabilitation (starting within 2-3 weeks post-op) results in:
- Faster return to activity.
- Reduced calf atrophy and improved strength.
- Decreased incidence of deep vein thrombosis.
- No increased risk of rerupture compared to traditional immobilization.
- Improved patient satisfaction and quality of life.
- Weight-Bearing Progression: Current guidelines generally advocate for early protected weight-bearing (e.g., touch-down weight-bearing or partial weight-bearing) in a CAM boot, gradually increasing to full weight-bearing over 4-6 weeks, with careful monitoring of tendon integrity.
Specific Considerations for the Watershed Zone
The hypovascular nature of the 2-6 cm watershed zone proximal to the insertion is consistently highlighted in anatomical and clinical literature as a key factor in Achilles pathology.
*
Rupture Etiology:
The relative avascularity contributes to degenerative changes, making this the most common site of rupture.
*
Healing Implications:
The diminished blood supply implies that the intrinsic healing capacity of the tendon in this region may be compromised. This provides a biological rationale for surgical intervention, especially robust repairs that aim to achieve strong apposition and maintain the paratenon for extrinsic revascularization. Augmentation techniques (e.g., plantaris, FHL transfer) are particularly relevant for chronic ruptures or cases with significant tissue loss in this zone, as they introduce additional vascularized tissue.
*
Rehabilitation:
While early motion benefits overall healing, the surgeon must be mindful of the potentially slower biological healing rate in the watershed zone and balance aggressive functional rehabilitation with adequate protection to prevent rerupture during the initial phases.
Current Guidelines and Consensus
There is no universal consensus on a single "best" treatment for all Achilles ruptures. The decision remains individualized.
* For young, active individuals seeking to return to high-level sports, operative repair combined with early functional rehabilitation is often preferred due to a potentially lower rerupture rate and better strength outcomes.
* For older, less active individuals, or those with significant comorbidities, non-operative management with an accelerated rehabilitation protocol is a viable and often preferred option, particularly for ruptures with small gaps.
* Regardless of the treatment chosen, comprehensive, supervised rehabilitation is paramount to achieving satisfactory functional recovery. The emphasis in current literature is shifting towards patient-centered care, balancing the risks and benefits of each approach based on patient goals and individual characteristics. Further research, particularly large, multicenter randomized controlled trials, continues to refine our understanding and guide best practices in Achilles tendon rupture management.
You Might Also Like