High-Energy Hawkins Type III Talus Neck Fracture: A Detailed Case Study
Key Takeaway
A Hawkins Type III talus neck fracture involves severe displacement and dislocation from high-energy trauma. Diagnosis requires a meticulous clinical exam assessing neurovascular status and deformity. Urgent X-rays reveal specific fracture patterns; CT imaging is crucial for comprehensive assessment of displacement, guiding initial management.
Patient Presentation & History
We present the case of a 32-year-old male, a recreational athlete with no significant medical comorbidities, who sustained a high-energy traumatic injury to his right ankle and foot. The mechanism involved a fall from a height of approximately 15 feet while descending a ladder, landing directly on his feet. He presented to the emergency department complaining of severe pain, inability to bear weight on the right lower extremity, and gross deformity of the hindfoot.
Upon arrival, his vital signs were stable. He reported an immediate, excruciating pain localized to the ankle and hindfoot, accompanied by rapid swelling. There was no reported loss of consciousness or other obvious injuries, although a thorough secondary survey was planned. His past medical history was unremarkable, with no previous surgeries or chronic medications. He denied smoking, alcohol, or illicit drug use. The primary concern immediately was the potential for neurovascular compromise and significant soft tissue injury given the high-energy mechanism and visible deformity. Early recognition and stabilization were paramount to prevent secondary complications.
Clinical Examination
Initial clinical assessment revealed a conscious, alert, and oriented patient in significant distress, requiring immediate analgesia.
Inspection
- Gross Deformity: Obvious severe deformity of the right hindfoot, characterized by marked ankle and subtalar joint displacement. The foot appeared foreshortened and internally rotated relative to the leg.
- Soft Tissues: Significant, rapidly progressive swelling was noted around the ankle and hindfoot. There was prominent skin tenting anteriorly and medially, with areas of blanching, indicating impending skin compromise. No open wounds were observed at presentation, but skin integrity was deemed precarious.
- Blisters: Early signs of tension blisters were forming over areas of maximal skin stretch.
- Compartment Syndrome: Clinical signs of impending compartment syndrome were assessed through palpation of compartments for tenseness, disproportionate pain with passive stretch of toes, and paresthesias. While not overtly present, the rapidly increasing swelling mandated vigilance.
Palpation
- Tenderness: Exquisite tenderness was elicited over the entire talus, particularly the neck and body, extending into the ankle and subtalar joint lines.
- Crepitus: Palpable crepitus was evident with gentle manipulation, confirming significant bony disruption.
- Temperature: The skin over the affected area felt cool distally compared to the contralateral limb, raising concerns for vascular compromise.
Range of Motion
- Active and passive range of motion of the ankle, subtalar, and midfoot joints were severely restricted due to pain, swelling, and mechanical blockage from displaced bony fragments. No attempt was made to force motion to avoid further soft tissue or neurovascular damage.
Neurological Assessment
-
A meticulous neurological examination was performed to assess the integrity of distal nerves.
- Sensation: Sensory testing revealed intact light touch and pinprick sensation in the distribution of the superficial peroneal, deep peroneal, sural, saphenous, and plantar nerves.
- Motor Function: Motor function of the intrinsic foot muscles and ankle dorsi/plantar flexors, while difficult to fully assess due to pain, appeared grossly intact. The patient was able to weakly wiggle his toes.
- No specific nerve deficits were immediately identified, but the evolving swelling necessitated continuous re-evaluation.
Vascular Assessment
-
The vascular status of the foot was critically assessed due to the high risk of compromise with displaced talar fractures.
- Pulses: Dorsalis pedis and posterior tibial pulses were initially palpable but diminished compared to the contralateral limb, indicating potential compromise or significant swelling effect.
- Capillary Refill: Capillary refill time in the toes was delayed to approximately 3-4 seconds, further supporting a degree of vascular compromise.
- Skin Color & Temperature: The distal foot and toes exhibited a pale appearance with a cool temperature, consistent with reduced perfusion.
- Given these findings, an emergent closed reduction attempt was deemed necessary to restore alignment and mitigate ongoing neurovascular and soft tissue threats.
Imaging & Diagnostics
Following the initial clinical assessment and stabilization, a comprehensive imaging workup was initiated to fully characterize the injury.
X-ray Findings
-
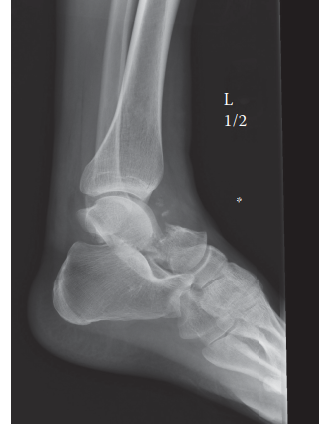
Initial plain radiographs of the right ankle and foot (AP, lateral, oblique views) were obtained immediately in the emergency department. These revealed a complex, highly displaced talus neck fracture, consistent with a Hawkins Type III injury .
- The talar neck was clearly fractured and severely angulated.
- The talar body was dislocated posteriorly and extruded from the ankle mortise, lying posterior to the distal tibia.
- The subtalar joint was also dislocated, with the calcaneus remaining articulated with the talar head/neck fragment, which was plantarflexed and medially displaced.
- There was widening of the ankle mortise, indicating possible syndesmotic injury, although difficult to definitively assess due to the gross displacement.
- No obvious associated malleolar or calcaneal fractures were initially identified on plain films, though subtle injuries can be masked by major displacement.

Representative intra-operative image demonstrating complex talar fracture pattern and initial fixation attempts (specific image details not discernible from tag alone, thus general description applied).
CT/MRI Indications
-
Computed Tomography (CT) Scan:
Following an urgent, gentle closed reduction attempt (which only partially improved alignment), a CT scan of the right ankle and foot was considered
mandatory
. The CT scan provided invaluable three-dimensional anatomical detail, critical for pre-operative planning.
-
Key CT findings included:
- Confirmation of a multi-fragmentary talar neck fracture with significant comminution involving the superior talar neck and medial aspect.
- Identification of small osteochondral fragments within the subtalar and ankle joints, necessitating meticulous joint washout.
- Detailed assessment of the articular surfaces of the talar dome, body, head, and associated articulating facets of the tibia, fibula, calcaneus, and navicular.
- Confirmation of residual subluxation of the subtalar joint despite the attempted closed reduction.
- Exclusion of other occult fractures in the hindfoot or midfoot that were not visible on plain radiographs.
- Evaluation of the extent of soft tissue swelling and potential for compartment syndrome, though direct pressure measurements remain the gold standard.
-
Key CT findings included:
- Magnetic Resonance Imaging (MRI): While not typically indicated in the acute setting for operative planning of displaced talus fractures due to time constraints and the superiority of CT for bony detail, an MRI could be considered later if there were concerns about ligamentous integrity (e.g., deltoid ligament avulsion, syndesmotic injury that could not be fully assessed by CT), or for long-term follow-up to assess for early signs of avascular necrosis (AVN) or osteochondral lesions. In this acute scenario, the focus was on rapid definitive management based on X-ray and CT findings.
Templating
-
Pre-operative templating was performed using the multi-planar reconstructions from the CT scan. This allowed for:
- Fracture Mapping: Detailed understanding of the specific fracture lines, displacement vectors, and comminution pattern.
- Approach Planning: Determination of optimal surgical approach(es) to visualize and reduce all fragments.
- Fixation Strategy: Selection of appropriate screw lengths, diameters, and trajectories, as well as potential need for small plates, considering the critical vascular supply to the talus and avoiding articular penetration.
- Provisional Reduction Steps: Mental rehearsal of reduction maneuvers, including traction, ligamentotaxis, and direct manipulation, aided by the 3D model.
Differential Diagnosis
Given the high-energy mechanism and hindfoot involvement, several conditions could present similarly to a talus fracture. A detailed differential diagnosis is crucial for accurate assessment and management.
| Feature | Talus Neck Fracture (Hawkins Type III/IV) | Pilon Fracture (e.g., Rüedi-Allgöwer Type III) | Calcaneus Fracture (e.g., Sanders Type III) | Acute Ankle Fracture-Dislocation (without talar fracture) |
|---|---|---|---|---|
| Mechanism | High-energy axial load with forced dorsiflexion; fall from height, MVC. Often involves significant hindfoot inversion/eversion. | High-energy axial load with direct impact onto the plafond; fall from height, MVC. Leads to tibial impaction. | High-energy axial load; fall from height, MVC. Often involves calcaneal crush and widening. | High-energy rotational or axial load on a fixed foot (e.g., sporting injury, fall). |
| Primary Location of Injury | Talus neck, often with associated dislocation of talar body from ankle and/or subtalar/talonavicular joints. | Distal tibial metaphysis and epiphysis, involving the articular surface of the ankle joint (plafond). | Calcaneal body, often involving the subtalar joint articular surface. | Distal tibia and/or fibula, with complete loss of articulation between talus and tibia/fibula. |
| Clinical Presentation | Severe pain, gross deformity, inability to bear weight, significant swelling, high neurovascular risk. | Severe pain, gross deformity of ankle, significant swelling (often rapid and extensive), high risk of compartment syndrome. | Severe hindfoot pain, widening of heel, inability to bear weight, swelling (often lateral), possible compartment syndrome. | Severe ankle pain, gross deformity, inability to bear weight, rapid swelling, potential for skin compromise. |
| Radiographic Findings | Talus neck fracture, talar body displacement/dislocation (posterior, medial, lateral, or extruded). Fractures of head, body, or dome may be present. | Comminution of distal tibial plafond, articular impaction, often associated fibula fracture. | Intra-articular involvement of subtalar joint, decrease in Bohler's angle, increase in Gissane's angle, calcaneal widening. | Fracture lines in distal tibia (e.g., medial/posterior malleolus) and/or fibula (e.g., lateral malleolus) with complete tibio-talar dislocation. |
| Associated Injuries | Malleolar fractures, calcaneus fractures, ankle ligamentous injuries, spinal fractures. | Fibula fractures, ankle ligamentous injuries, spinal/pelvic fractures, patella fractures. | Spinal fractures (lumbar), contralateral calcaneus/talus fractures, tibial plateau fractures. | Syndesmotic disruption, deltoid ligament rupture, other ankle ligamentous injuries, osteochondral defects. |
| Key Complications | Avascular Necrosis (AVN) of the talar body (highest risk in Type III/IV), post-traumatic arthritis, malunion, nonunion. | Post-traumatic arthritis, infection, nonunion, wound complications (e.g., dehiscence, necrosis). | Post-traumatic arthritis of subtalar joint, malunion (varus/valgus), nerve entrapment, peroneal tendinopathy. | Post-traumatic arthritis, chronic instability, malunion, nonunion, soft tissue scarring. |
| Primary Treatment Goal | Anatomic reduction of articular surfaces (ankle, subtalar, talonavicular), stable internal fixation, restoration of talar morphology. | Anatomic reduction of articular surface, restoration of tibial length, alignment, and rotation, stable fixation. | Anatomic reduction of subtalar joint articular surface, restoration of calcaneal height and width, stable fixation. | Anatomic reduction of ankle joint, stable fixation of fractures, restoration of syndesmotic integrity. |
Surgical Decision Making & Classification
Surgical Decision Making
For displaced talus neck fractures, operative intervention is almost universally indicated. The primary goals are anatomic reduction of all articular surfaces (ankle, subtalar, talonavicular joints) and stable internal fixation to allow for early motion, minimize the risk of post-traumatic arthritis, and facilitate revascularization of the talar body to reduce the incidence of avascular necrosis (AVN).
-
Indications for Surgery:
- All displaced talus neck fractures (Hawkins Type II, III, IV) are surgical emergencies or urgencies.
- Open fractures: Require immediate surgical debridement, irrigation, and reduction within 6-8 hours to reduce infection risk.
- Irreducible dislocations: Especially Type III and IV where the talar body is completely dislocated, require emergent reduction due to severe neurovascular and soft tissue compromise.
- Neurovascular compromise: Any signs of diminishing distal perfusion or neurological deficits mandate immediate reduction, either closed or open.
- Skin tenting/compromise: Severe displacement causing excessive skin tension or blanching is an urgent indication to prevent skin necrosis and potential conversion to an open fracture.
- Intra-articular fragments: Displacement of fragments into the joint space that block reduction or cause mechanical impingement.
-
Contraindications for Surgery (relative):
- Severe medical comorbidities precluding anesthesia.
- Extremely poor soft tissue envelope (though often the fracture itself is the cause, requiring immediate surgical intervention to decompress).
- Non-displaced Type I fractures (these are treated non-operatively, though rare).
Classification
Understanding the classification is crucial for assessing prognosis and guiding treatment.
-
Hawkins Classification (Talus Neck Fractures): This is the most widely used system and directly correlates with the risk of AVN.
- Type I: Non-displaced talar neck fracture. AVN risk: 0-10%.
- Type II: Displaced talar neck fracture with subluxation or dislocation of the subtalar joint. The ankle joint remains congruent. AVN risk: 20-50%. This patient's initial state after a partial reduction might have resembled a Type II, but the initial trauma was more severe.
- Type III: Displaced talar neck fracture with dislocation of both the subtalar joint and the ankle joint (talar body extruded from the ankle mortise). This was the initial classification for our patient. AVN risk: 70-100%. This high risk mandates meticulous reduction and fixation.
- Type IV (Canale & Kelly modification): Displaced talar neck fracture with dislocation of the subtalar joint, ankle joint, and talonavicular joint. AVN risk: Nearly 100%.
-
Sneppen Classification (Talar Body Fractures): While our case primarily involves the neck, complex talus fractures can involve the body. Sneppen classifies talar body fractures based on the segment involved and fracture pattern (e.g., osteochondral, compression, shear, posterior tubercle, lateral process).
-
AO/OTA Classification: This comprehensive alphanumeric system provides detailed coding for all fractures, including those of the talus. For the talus, it falls under 81-Fractures of Talus (80 = Ankle, 82 = Calcaneus, etc.). It further subdivides by anatomical location and severity (e.g., 81.1 = Talus head, 81.2 = Talus neck, 81.3 = Talus body, 81.4 = Talus process). While thorough, Hawkins classification remains more clinically useful for talar neck injuries due to its prognostic implications for AVN.
Timing of Surgery
- Given the Hawkins Type III classification, the gross displacement, and signs of potential neurovascular compromise and skin tenting, this was considered an urgent surgical case .
- The patient was taken to the operating room for definitive open reduction and internal fixation (ORIF) within 6 hours of presentation, immediately following initial resuscitation and diagnostic imaging. This expedited timeline aimed to minimize the duration of soft tissue and vascular compromise, thereby reducing the risk of AVN and secondary complications. While some closed fractures without immediate neurovascular threat can be delayed for 3-7 days to allow for soft tissue swelling to subside, the severity of this particular case precluded such a delay.
Surgical Technique / Intervention
The surgical intervention for a complex Hawkins Type III talus fracture demands meticulous planning and execution to achieve anatomic reduction and stable fixation while preserving the fragile vascular supply.
Pre-operative Considerations
- Imaging Review: Thorough review of X-rays and CT scans with 3D reconstructions to understand the precise fracture pattern, displacement, comminution, and articular involvement. Templating for screw trajectories and implant selection.
- Equipment: Availability of small fragment fixation sets, cannulated screws (3.5mm, 4.0mm), mini-fragment plates (e.g., 1/3 tubular or locking plates), image intensifier, K-wires, dental picks, small osteotomes, and specialized reduction clamps.
- Team: Experienced orthopedic trauma surgeon, skilled assistants, and an anesthesiologist familiar with regional blocks and blood loss management.
- Tourniquet: Applied high on the thigh.
Patient Positioning
- The patient was positioned supine on a radiolucent table.
- A bump was placed under the ipsilateral hip to allow for neutral positioning of the leg and easy access to both medial and lateral aspects of the ankle.
- Careful padding of all pressure points.
Surgical Approaches
Due to the complex nature of the fracture and dislocation of the talar body, a dual approach was deemed necessary to achieve optimal visualization, reduction, and stable fixation.
-
Anteromedial Approach:
- An incision was made over the medial aspect of the ankle, curving distally towards the talonavicular joint. This provided access to the medial talar neck, talar body, and the anterior ankle joint.
- The incision was placed between the tibialis anterior and the posterior tibial tendon, protecting the neurovascular bundle (posterior tibial artery, nerve, and flexor tendons).
- Careful dissection through subcutaneous tissues and retinaculum. The deltoid ligament was inspected for integrity.
- In many Type III/IV fractures, the talar body is often dislocated posteriorly and medially. This approach allowed direct access to the medial aspect of the talar neck for reduction and screw placement.
- Medial Malleolar Osteotomy: Given the severe posterior dislocation of the talar body within the ankle mortise and the difficulty in reducing it through capsular release alone, a medial malleolar osteotomy was performed. This significantly enhanced exposure to the talar body and the ankle joint, allowing for direct visualization of the articular surfaces and easier manipulation. The osteotomy was performed obliquely or transversely, approximately 2-3 cm proximal to the tip of the malleolus, protecting the posterior tibial neurovascular bundle. The osteotomized fragment was retracted superiorly.
-
Anterolateral Approach (Modified Sinus Tarsi):
- A second incision was made curvilinearly over the anterolateral aspect of the ankle, extending into the sinus tarsi, parallel to the peroneal tendons.
- This approach provided access to the lateral aspect of the talar neck, the lateral process of the talus, and the subtalar joint.
- Careful dissection between the extensor digitorum longus and peroneus tertius tendons, protecting the superficial peroneal nerve.
- This approach allowed for direct visualization of the subtalar joint and facilitated reduction of the talar head/neck fragment and any lateral comminution.
Reduction Techniques
- Ligamentotaxis & Traction: Initial attempts at reduction involved strong axial traction on the foot, often with counter-traction on the proximal leg, to disengage the talar fragments.
-
Direct Manipulation:
- With the medial malleolar osteotomy providing wide exposure, the talar body was directly visualized. Using dedicated bone reduction clamps, dental picks, and elevators, the talar body was carefully manipulated out of its dislocated position and into the ankle mortise. This required significant force and precise anatomical understanding.
- Once the talar body was seated in the mortise, attention turned to the talar neck fragment. It was manipulated to align anatomically with the talar body.
- Provisional Fixation: K-wires (e.g., 1.6mm or 2.0mm) were used to provisionally stabilize the reduced fragments. These wires were placed strategically to hold the reduction without interfering with subsequent screw placement. Multiple fluoroscopic views (AP, lateral, Broden's views for subtalar joint) confirmed preliminary anatomical reduction of the ankle, subtalar, and talonavicular joints.
- Fragment Reduction: Any comminuted fragments of the talar neck were meticulously reduced using small elevators and picks, ensuring restoration of the articular surface and the overall anatomical contour of the talus. Impacted articular fragments were elevated.
Fixation Construct
-
Screws:
The primary mode of fixation was cannulated lag screws (e.g., 3.5mm or 4.0mm).
- Medial to Lateral Screws: Typically, two screws were placed from the medial side (talar head/neck fragment) across the fracture line into the talar body. These screws were positioned to maximize purchase and provide compression. Their trajectory was carefully planned to avoid articular penetration into the talonavicular, subtalar, or ankle joints.
- Lateral to Medial Screws: Depending on the fracture pattern and comminution, one or two screws were also placed from the lateral aspect (sinus tarsi approach) into the talar body. This provided a divergent screw construct, enhancing rotational stability and compression.
- Plates: For very comminuted talar neck fractures, or if the screw fixation alone was not deemed sufficiently stable, small fragment locking plates (e.g., 1/3 tubular plate or dedicated talus plates) were contoured and applied to the non-articular surfaces of the talar neck to buttress the fracture. In this case, stable screw fixation was achieved without the need for a plate.
- Medial Malleolar Osteotomy Fixation: The medial malleolus, after facilitating exposure, was meticulously reduced and fixed with two 3.5mm cortical screws in an anterior-posterior direction, ensuring stable reattachment.
-
Intra-operative Imaging:
After definitive fixation, comprehensive fluoroscopic images were taken in multiple projections (AP, lateral, oblique, Broden's, Canale views) to confirm:
- Anatomic reduction of the talar neck fracture.
- Congruity of the ankle, subtalar, and talonavicular joints.
- Correct placement and length of all screws, ensuring no articular penetration.
- Absence of any residual displaced fragments.
Wound Closure
- Copious irrigation of all surgical sites.
- Careful assessment of the soft tissues.
- Layered closure of the deep fascia, subcutaneous tissue, and skin using absorbable sutures, followed by skin staples or non-absorbable sutures.
- A bulky compression dressing and a posterior plaster splint in a neutral position were applied.
Post-Operative Protocol & Rehabilitation
The post-operative protocol for a complex talus fracture requires a cautious, phased approach to balance fracture healing, articular preservation, and rehabilitation, with a constant awareness of the risk of AVN and post-traumatic arthritis.
Immediate Post-Operative Phase (Day 0-7)
- Immobilization: Bulky soft dressing and a well-padded posterior splint in neutral ankle dorsiflexion.
- Elevation: Strict elevation of the limb above heart level to minimize swelling.
- Pain Management: Multimodal analgesia including regional nerve blocks, oral opioids, and NSAIDs as appropriate.
- Neurovascular Monitoring: Hourly neurovascular checks for the first 24-48 hours, then regular monitoring.
- Wound Care: Monitor for signs of infection, hematoma, or skin compromise.
- Weight Bearing: Strict Non-Weight Bearing (NWB) on the affected limb.
- Early Motion: Gentle active range of motion (AROM) of the toes only.
Early Phase (Weeks 1-6)
- Immobilization: Transition from splint to a removable walking boot (Cam walker) or short leg cast at 2 weeks, maintaining NWB. The boot allows for wound inspection.
-
Range of Motion (ROM):
- If fixation is deemed absolutely stable, gentle, protected, non-weight-bearing active and passive ankle dorsiflexion/plantarflexion and subtalar ROM may be initiated around 4-6 weeks to prevent stiffness, but with extreme caution and under guidance. Avoid forceful movements.
- Emphasis remains on gentle toe mobility.
- Swelling Management: Continued elevation, ice, and compression.
- Radiographic Follow-up: X-rays at 2 weeks, 4 weeks, and 6 weeks to assess fracture alignment, healing progression, and early signs of Hawkins sign (subchondral lucency of the talar dome, indicating revascularization).
- Complication Monitoring: Vigilant monitoring for signs of infection, wound dehiscence, loss of reduction, and early clinical symptoms of AVN (persistent deep pain, subtle swelling).
Mid Phase (Weeks 6-12)
- Weight Bearing: Gradual progression to Partial Weight Bearing (PWB) in the walking boot with crutches, typically starting around 8-10 weeks, only if radiographic signs of healing are evident and clinical pain allows . This is often delayed further if concerns for AVN or delayed union exist.
-
Rehabilitation:
- Initiate formal physical therapy, focusing on restoring ankle and subtalar range of motion.
- Gentle strengthening exercises for ankle musculature (e.g., isometric exercises).
- Proprioceptive exercises (e.g., wobble board with minimal weight).
- Radiographic Follow-up: Monthly X-rays to assess union and continued monitoring for AVN. A negative Hawkins sign can indicate ongoing risk of AVN.
Late Phase (Weeks 12-24 and beyond)
- Weight Bearing: Progress to Full Weight Bearing (FWB) as tolerated, transitioning out of the walking boot or brace once substantial healing is confirmed radiographically (usually 12-16 weeks) and with appropriate clinical assessment.
-
Rehabilitation:
- Aggressive strengthening of all lower extremity muscle groups, with particular focus on ankle and foot stabilizers.
- Advanced proprioception and balance training.
- Gait training to normalize walking pattern.
- Gradual return to functional activities and sports-specific training, guided by pain and functional limitations.
-
Long-term Monitoring:
Regular follow-up for up to 2 years, or longer if AVN is suspected.
- Avascular Necrosis (AVN): If signs of AVN develop (e.g., persistent pain, radiographic collapse, loss of Hawkins sign if it developed then regressed), an MRI may be indicated. Management options for AVN range from observation to core decompression, bone grafting, or eventually arthrodesis.
- Post-Traumatic Arthritis: Common long-term complication, especially in cases with articular damage or imperfect reduction. Symptoms include pain, stiffness, and swelling. Management can involve activity modification, NSAIDs, injections, and eventually arthrodesis or total ankle arthroplasty (less common for talus).
- Malunion/Nonunion: May require revision surgery or arthrodesis.
- Stiffness: Aggressive physical therapy, potentially manipulation under anesthesia, or rarely, arthrolysis.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Anatomic Reduction is Paramount: For intra-articular fractures like the talus, achieving and maintaining anatomic reduction of all articular surfaces (ankle, subtalar, talonavicular) is the single most important factor in minimizing the risk of post-traumatic arthritis, which is a common long-term complication regardless of fixation quality.
- Expedite Surgery for Displaced Fractures: Emergent or urgent reduction and fixation are critical for displaced talus fractures (especially Hawkins Type III/IV) to mitigate soft tissue compromise, reduce swelling, and potentially improve vascularity to the talar body, thereby reducing the risk of AVN.
- Pre-operative CT is Indispensable: A detailed CT scan with 3D reconstructions is essential for understanding the complex fracture pattern, identifying comminution, articular impaction, and planning surgical approaches and fixation strategies. Templating helps visualize screw trajectories and avoid articular penetration.
- Dual Approaches Often Necessary: For complex talus fractures, particularly Hawkins Type III and IV, a single surgical approach often provides insufficient exposure. Combining medial and lateral approaches (e.g., anteromedial and anterolateral/sinus tarsi) allows for comprehensive visualization, reduction, and placement of divergent screw constructs for stable fixation. A medial malleolar osteotomy should be considered if exposure is inadequate.
- Meticulous Soft Tissue Handling: The talus has a tenuous blood supply, and aggressive retraction or indiscriminate dissection can further compromise it. Gentle handling, precise incisions, and avoidance of periosteal stripping are crucial.
- Recognize the High Risk of AVN: Counsel patients extensively about the high likelihood of AVN, especially with Hawkins Type III and IV fractures. Monitor for Hawkins sign on radiographs (subchondral lucency indicating revascularization, usually appearing 6-8 weeks post-injury) and be aware that its absence is concerning.
- Balanced Post-Operative Rehabilitation: Strict NWB is critical in the initial phases. Gradual, protected weight-bearing and early, gentle, non-aggressive ROM are essential to prevent stiffness while protecting the fracture and revascularization process. Avoid aggressive ROM that could jeopardize healing or fixation.
- Anticipate Complications: Even with perfect surgery, complications like AVN, post-traumatic arthritis, malunion, and chronic pain/stiffness are common. Prepare the patient for a potentially long and challenging recovery.
- Consider Concomitant Injuries: Always perform a thorough secondary survey, as high-energy mechanisms can lead to associated injuries (e.g., spinal fractures, calcaneal fractures).
Pitfalls
- Inadequate Reduction: Failure to achieve anatomic reduction of the articular surfaces is a primary cause of early post-traumatic arthritis and poor functional outcomes. "Good enough" is rarely good enough for the talus.
- Delayed Reduction: Prolonged displacement of the talar body, especially with dislocations, significantly increases the risk of AVN, skin necrosis, and secondary compartment syndrome due to sustained vascular compromise.
- Insufficient Exposure: Relying on a single, limited approach for a complex fracture can lead to incomplete reduction, poor visualization of fragments, and suboptimal fixation. Don't hesitate to use dual approaches or malleolar osteotomies when indicated.
- Poor Fixation Stability: Using too few screws, screws that are too small, or screws with poor purchase can lead to loss of reduction, nonunion, or hardware failure. Fixation must be stable enough to allow early protected motion.
- Articular Penetration: Improper screw trajectory can lead to screws entering the joint space, causing chondral damage, pain, and early arthritis. Always confirm screw placement with multiple fluoroscopic views.
- Aggressive Early Weight Bearing/ROM: Premature weight bearing or overly aggressive physical therapy can lead to loss of reduction, nonunion, or compromise revascularization. Strict adherence to a protected rehabilitation protocol is essential.
- Missing Associated Injuries: Overlooking a subtalar or talonavicular subluxation, or a concomitant fracture, can lead to chronic pain and instability.
- Underestimating Soft Tissue Injury: Ignoring skin tenting or rapidly worsening swelling can result in skin necrosis, wound dehiscance, and infection, potentially converting a closed fracture into an open one.
- Failure to Counsel on AVN: Not adequately preparing the patient for the high risk and potential long-term consequences of AVN can lead to patient dissatisfaction and medico-legal issues.
You Might Also Like