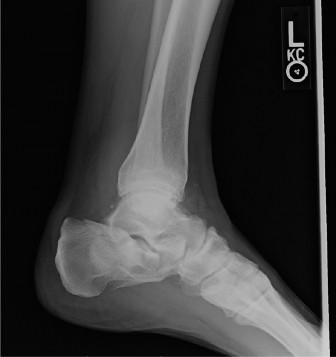
Hallux Valgus: Epidemiology, Pathophysiology, and Surgical Anatomy
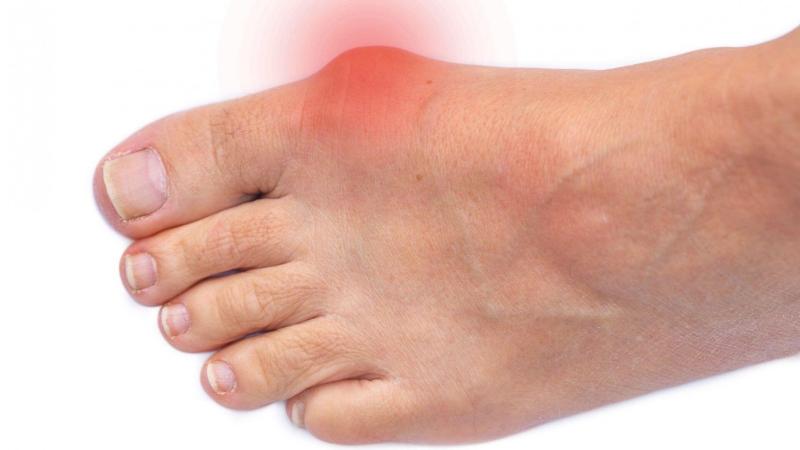
Key Takeaway
Hallux valgus (HV) is a complex, progressive multiplanar deformity of the first MTP joint, marked by lateral hallux deviation and a prominent bunion. Etiologies include intrinsic factors like foot morphology and extrinsic factors such as footwear. Pathophysiology involves osseous malalignment, soft tissue imbalance, and sesamoid subluxation, crucial for accurate diagnosis and management.
Introduction & Epidemiology
Hallux valgus (HV) is a common, complex, and progressive multiplanar deformity of the first metatarsophalangeal (MTP) joint, characterized by lateral deviation and pronation of the hallux relative to the first metatarsal (MT), and often medial deviation (varus) of the first MT. This complex malalignment results in a prominent medial eminence, often referred to as a bunion, which is a symptom rather than the primary deformity.
Epidemiologically, HV affects millions globally, with prevalence rates varying significantly across populations, ranging from 23% in adults aged 18-65 years to 35.7% in those over 65 years. The condition exhibits a strong female predominance, with a female-to-male ratio as high as 10:1. While often considered a progressive disorder, its initiation and rate of progression are influenced by a confluence of intrinsic and extrinsic factors.
Intrinsic etiologies include inherited foot morphology, such as a pronated foot type, ligamentous laxity, metatarsus primus varus, an abnormal first MTP joint shape (e.g., rounded metatarsal head), or a pathologically long first metatarsal. Neuromuscular conditions, inflammatory arthritides (e.g., rheumatoid arthritis, psoriatic arthritis), and certain collagen disorders also predispose individuals to HV deformity. Congenital deformities, while rare, can also contribute.
Extrinsic factors primarily involve footwear, particularly tight-fitting shoes with narrow toe boxes and high heels, which can exacerbate or accelerate the development of the deformity, though they are not considered the sole cause. Repeated foot stress or injuries may also contribute to the inflammatory cascade and subsequent joint remodeling.
Pathophysiologically, the deformity involves a cascade of changes:
*
Osseous Malalignment:
Medial deviation of the first metatarsal (increased intermetatarsal angle, IMA) and lateral deviation of the hallux (increased hallux valgus angle, HVA). The distal metatarsal articular angle (DMAA) may also be abnormal, indicating an oblique joint surface.
*
Soft Tissue Imbalance:
The abductor hallucis muscle and tendon typically migrate plantar and lateral to the first metatarsal head, converting its abduction force into an adduction-pronation force. Concurrently, the adductor hallucis tendon and the lateral MTP joint capsule become contracted, pulling the hallux laterally. The medial MTP joint capsule, conversely, becomes attenuated and lax.
*
Sesamoid Subluxation:
The fibular sesamoid subluxates laterally relative to the first metatarsal head, often eroding the crista of the metatarsal head and contributing to the hallux pronation and valgus deformity.
*
Plantar Plate Pathology:
Chronic stress can lead to attenuation or tearing of the plantar plate, further destabilizing the joint.
Understanding these interconnected factors is critical for accurate diagnosis, surgical planning, and long-term management of hallux valgus.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the first ray is paramount for successful hallux valgus correction. The first ray comprises the first metatarsal, proximal phalanx, distal phalanx, and two sesamoid bones, all articulated to form a functional unit.
Osseous Structures
- First Metatarsal (MT): Articulates proximally with the medial cuneiform (forming the Tarsometatarsal, TMT joint) and distally with the proximal phalanx (forming the MTP joint). The first MT is typically the shortest and strongest, designed for weight-bearing and propulsion. Its head is convex, allowing significant MTP motion. The medial eminence is the site of the characteristic "bunion" prominence.
- Proximal Phalanx: Articulates proximally with the first MT head and distally with the distal phalanx.
- Sesamoids: Two small, ovoid bones (tibial and fibular) embedded within the conjoined tendon of the flexor hallucis brevis (FHB). They articulate with the plantar grooves of the first MT head and are crucial for the mechanical advantage of the FHB and protection of the FHL. Their position relative to the metatarsal head crista is a key indicator of deformity.
Ligamentous & Capsular Structures
- Medial Collateral Ligament (MCL): Extends from the medial aspect of the metatarsal head to the medial side of the proximal phalanx. In HV, it becomes attenuated.
- Lateral Collateral Ligament (LCL): Extends from the lateral aspect of the metatarsal head to the lateral side of the proximal phalanx. In HV, it becomes contracted.
- Deep Transverse Metatarsal Ligament (DTML): Connects the plantar aspects of the metatarsal heads, providing stability and resisting splaying. Its contracture or involvement can contribute to lesser toe deformities.
- Plantar Plate: A thick fibrocartilaginous structure that reinforces the plantar aspect of the MTP joint capsule, providing stability and protecting the joint from hyperextension. The sesamoids are embedded within it.
- MTP Joint Capsule: A fibrous capsule surrounding the MTP joint, contributing to stability. Medial capsular laxity and lateral capsular contracture are hallmarks of HV.
Musculotendinous Structures
- Abductor Hallucis (AH): Originates from the medial tubercle of the calcaneus and inserts on the medial aspect of the proximal phalanx. Its primary action is to abduct the hallux. In HV, its tendon often migrates plantar and lateral to the first MT head, becoming a deforming force (adductor/flexor).
- Adductor Hallucis (AD): Comprises two heads: the oblique head (originating from the bases of the 2nd-4th metatarsals) and the transverse head (originating from the plantar plates of the 3rd-5th MTP joints). Both insert on the fibular sesamoid and the lateral aspect of the proximal phalanx. The AD is a primary deforming force, pulling the hallux laterally.
- Flexor Hallucis Brevis (FHB): Two heads, medial and lateral, insert into the medial and lateral sesamoids, respectively, which then attach to the proximal phalanx. It aids in MTP joint flexion.
- Extensor Hallucis Longus (EHL): Originates from the fibula and interosseous membrane, inserts on the dorsal aspect of the distal phalanx. It extends the hallux and aids in ankle dorsiflexion. Its tendon often bows laterally over the MTP joint in HV.
- Extensor Hallucis Brevis (EHB): Aids in hallux extension.
- Flexor Hallucis Longus (FHL): Passes beneath the sesamoids in a fibro-osseous tunnel, inserting into the distal phalanx. Contributes to hallux flexion and push-off.
Neurovascular Structures
- Nerves: The medial dorsal cutaneous nerve (branch of superficial peroneal nerve) crosses the operative field dorsomedially. The medial plantar nerve (branch of tibial nerve) supplies sensation to the plantar medial aspect of the hallux. Injury to these nerves can lead to paresthesias or painful neuromas.
- Arteries: The dorsal pedis artery gives off the first dorsal metatarsal artery, which branches into the dorsal digital arteries. The deep plantar arch, formed by the dorsal pedis artery and the lateral plantar artery, gives rise to plantar digital arteries. Careful dissection is required to protect the delicate vascular supply to the metatarsal head, particularly during distal osteotomies, to mitigate the risk of avascular necrosis.
Biomechanics of Deformity
The pathological biomechanics of HV involve:
1.
Medial Column Instability:
Often stemming from a hypermobile first TMT joint or a primary metatarsus primus varus, leading to increased IMA.
2.
Windlass Mechanism Disruption:
The plantar plate and FHL/sesamoid complex are crucial for maintaining the longitudinal arch and facilitating toe-off. Sesamoid subluxation and plantar plate attenuation compromise this mechanism.
3.
Mechanical Axis Shift:
The first MTP joint's mechanical axis shifts laterally, causing the EHL and FHL tendons to become bowstringed and contribute to the valgus deformity.
4.
Pronation:
The hallux not only deviates laterally but also pronates, leading to the nail plate facing medially. This is often linked to lateral sesamoid subluxation and attenuation of the plantar plate/medial capsule.
Surgical correction of HV must address all components of this multiplanar deformity, including osseous alignment, soft tissue balance, and sesamoid position, to achieve a stable and functionally sound foot.
Indications & Contraindications
The decision for operative intervention in hallux valgus is primarily driven by patient symptomatology and functional impairment, rather than solely by radiographic measurements. Surgical correction is considered when conservative measures have failed to provide adequate relief.
Operative Indications
-
Symptomatic Bunion:
- Persistent pain localized to the medial eminence or first MTP joint, not adequately controlled by non-operative measures.
- Difficulty or pain with shoewear, limiting activities of daily living or recreational pursuits.
- Development of secondary symptoms such as metatarsalgia (transfer pain to lesser metatarsals), painful callosities, or lesser toe deformities (e.g., hammertoes, crossover toe) due to the progressive HV deformity.
-
Failure of Conservative Management:
Typically, a trial of appropriate non-operative treatments for at least 3-6 months, including:
- Modified footwear (wide toe box, low heel).
- Custom or over-the-counter orthotics.
- Activity modification.
- Non-steroidal anti-inflammatory drugs (NSAIDs).
- Padding or bunion splints (primarily for symptom relief, not deformity correction).
- Progressive Deformity with Functional Impairment: While not an absolute indication in the absence of pain, severe, rapidly progressive deformity leading to significant functional limitations or impending joint destruction may warrant consideration.
-
Radiographic Parameters (General Guidelines, not stand-alone indications):
- Hallux Valgus Angle (HVA) > 20 degrees.
- Intermetatarsal Angle (IMA) > 9-10 degrees.
- Significant sesamoid subluxation (e.g., Hardy and Clapham grade > 2).
- Incongruent MTP joint.
- These parameters guide the choice of operative technique but are secondary to clinical symptoms.
Operative Contraindications
- Asymptomatic Deformity: Surgical intervention is generally not indicated for cosmetic reasons alone or in the absence of pain and functional limitations.
- Unrealistic Patient Expectations: Patients must understand the recovery process, potential complications, and expected outcomes.
-
Severe Systemic Comorbidities:
- Uncontrolled diabetes mellitus, particularly with neuropathy or peripheral vascular disease, significantly increases the risk of complications (infection, wound healing issues, nonunion).
- Active systemic infection or local soft tissue infection in the surgical field.
- Severe peripheral vascular disease (critical limb ischemia).
- Significant neuropathy, predisposing to Charcot arthropathy.
- Bleeding dyscrasias.
- Inability to Comply with Post-Operative Rehabilitation: The success of HV surgery heavily relies on adherence to post-operative protocols.
- Inadequate Bone Stock: Severe osteoporosis or osteopenia may preclude stable internal fixation.
- Active Inflammatory Arthritis Flare: Surgery should be postponed until the inflammatory process is controlled.
- Smokers: While not an absolute contraindication, smoking significantly increases the risk of wound healing complications, infection, and nonunion. This risk must be thoroughly discussed.
Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Symptoms | Mild, intermittent pain; no significant functional limitation. | Persistent, disabling pain; difficulty with shoewear; functional impairment. |
| Deformity Severity | Mild radiographic changes (HVA < 20°, IMA < 10°); no rapid progression. | Moderate to severe radiographic deformity (HVA > 20°, IMA > 10-15°). |
| Response to Conservative | Symptoms adequately controlled by non-operative measures. | Failure of at least 3-6 months of adequate conservative management. |
| Patient Factors | High surgical risk; unrealistic expectations; non-compliance; asymptomatic. | Compliant patient; good general health; realistic expectations; willing to undergo rehab. |
| Associated Pathology | Isolated HV, no significant MTP arthritis or secondary toe deformities. | Concomitant MTP arthritis, transfer metatarsalgia, progressive lesser toe deformities. |
| Activity Level | Sedentary or low-impact activities where symptoms are manageable. | Active individual desiring return to higher function and pain-free activities. |
| Footwear Challenge | Able to find comfortable footwear with minimal difficulty. | Significant challenge in finding appropriate and comfortable footwear. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for predictable outcomes in hallux valgus surgery, integrating clinical assessment, radiographic analysis, and patient education.
Clinical Evaluation
- History: Detailed history focusing on symptom duration, character, location, aggravating/alleviating factors, previous treatments (including their efficacy), medical comorbidities (diabetes, peripheral neuropathy, inflammatory arthritides), current medications (anticoagulants), and allergies. Crucially, assess patient expectations regarding pain relief, functional improvement, and cosmetic appearance.
-
Physical Examination:
- Observation: Assess foot posture (pes planus, cavus), presence of callosities, skin integrity (especially over the bunion and plantar foot), lesser toe deformities.
- Palpation: Localize tenderness (medial eminence, MTP joint, plantar plate, sesamoids).
- Range of Motion (ROM): Assess MTP joint passive and active ROM in both weight-bearing and non-weight-bearing states. Evaluate reducibility of the deformity (dynamic vs. fixed). Assess pronation of the hallux.
- Stability: Evaluate TMT joint hypermobility (first ray instability) and MTP joint stability.
- Neurovascular Status: Dorsalis pedis and posterior tibial pulses, capillary refill, sensation (light touch, two-point discrimination, monofilament testing) to rule out significant neuropathy or peripheral vascular disease.
- Gait Analysis: Observe the patient's gait for compensatory mechanisms, forefoot loading patterns, and pain response.
- Shoewear Assessment: Review current and desired footwear to understand functional limitations.
Radiographic Evaluation
Standard weight-bearing radiographs are indispensable for surgical planning.
1.
Anteroposterior (AP) View:
*
Hallux Valgus Angle (HVA):
Angle between the longitudinal axis of the first metatarsal and the proximal phalanx (Normal: < 15°).
*
Intermetatarsal Angle (IMA):
Angle between the longitudinal axes of the first and second metatarsals (Normal: < 9°). A higher IMA indicates metatarsus primus varus.
*
Distal Metatarsal Articular Angle (DMAA) / Proximal Phalangeal Articular Angle (PPAA):
Angle between the perpendicular to the articular surface of the first metatarsal head and the longitudinal axis of the first metatarsal. Reflects joint congruity and head orientation (Normal: < 10°).
*
Sesamoid Position:
Classified (e.g., Hardy and Clapham scale) relative to the first metatarsal head. Lateral subluxation indicates pronation and deforming forces.
*
Joint Congruity:
Assess for subluxation or degenerative changes (joint space narrowing, osteophytes).
*
Metatarsal Length:
Evaluate for relative shortening or lengthening of the first metatarsal compared to the second.
2.
Lateral View:
*
First Metatarsal Plantarflexion Angle:
Assess for elevation or depression of the first metatarsal, which can affect transfer metatarsalgia.
*
MTP Joint Degeneration:
Identify dorsal osteophytes or joint space narrowing.
*
TMT Joint Stability:
Assess for dorsal gapping or degenerative changes, suggestive of first ray hypermobility.
3.
Oblique View:
Assists in visualizing the TMT joint and lesser metatarsal heads.
4.
Additional Imaging:
CT or MRI are rarely needed for routine HV surgery but may be considered for complex deformities, suspected avascular necrosis, significant MTP arthritis, or stress fractures.
Surgical Planning
- Deformity Analysis: Categorize deformity (mild, moderate, severe) based on HVA, IMA, DMAA, and sesamoid position.
-
Osteotomy Selection:
Choose appropriate osteotomy (distal, shaft, proximal metatarsal, TMT fusion) and adjunct procedures (Akin osteotomy, soft tissue release/plication) based on deformity characteristics.
- Mild (IMA < 13°, HVA < 20°): Distal osteotomies (Chevron/Austin, Reverdin).
- Moderate (IMA 13-16°, HVA 20-40°): Shaft osteotomies (Scarf, Ludloff).
- Severe (IMA > 16°, HVA > 40°): Proximal osteotomies (crescentic, opening wedge), or first TMT arthrodesis (Lapidus) particularly with first ray hypermobility or TMT arthritis.
- Fixation Choice: Plan for K-wires, screws (headless compression, cortical, locking), or plates based on osteotomy stability and anticipated weight-bearing.
Anesthesia
- Regional Anesthesia: An ankle block (tibial, sural, superficial peroneal, deep peroneal, saphenous nerves) provides excellent post-operative pain control. Popliteal block can also be utilized.
- General Anesthesia: Often combined with regional anesthesia for patient comfort during the procedure.
- Sedation: Can be an alternative for minor procedures or in conjunction with regional blocks.
Patient Positioning
- Supine Position: Patient is positioned supine on the operating table.
- Tourniquet: A pneumatic tourniquet is applied to the ipsilateral thigh or ankle to ensure a bloodless field.
- Leg Positioning: The operative leg is positioned to allow optimal access to the medial and dorsal aspects of the foot. A bump under the ipsilateral hip may facilitate internal rotation of the limb for improved medial access.
- C-arm Access: Ensure the operating table and positioning allow unrestricted C-arm fluoroscopy for intraoperative radiographic confirmation of correction and fixation. Radiolucent hand tables or extension platforms can be beneficial.
- Sterile Field: The foot and ankle are prepped and draped in a sterile fashion, ensuring adequate exposure and room for instrumentation.
Detailed Surgical Approach / Technique
The goal of hallux valgus surgery is to achieve multiplanar correction of the deformity, restore the anatomy of the first MTP joint, and address the underlying biomechanical imbalances. While numerous techniques exist, a common approach involves a combination of soft tissue balancing and an osseous osteotomy tailored to the severity of the deformity. Below, we outline a general approach often combined with a distal or shaft osteotomy, followed by specific considerations for different osteotomy types.
General Principles
- Incisions: Typically dorsomedial longitudinal incision over the first MTP joint, extending proximally along the first metatarsal. Some prefer a purely medial incision.
- Protection of Neurovascular Structures: The medial dorsal cutaneous nerve (branch of the superficial peroneal nerve) is vulnerable dorsomedially. Careful dissection and retraction are crucial.
- Medial Bunionectomy (Exostectomy): Resection of the prominent medial eminence of the first metatarsal head.
- Lateral Soft Tissue Release: Release of contracted structures on the lateral aspect of the first MTP joint, including the adductor hallucis tendon, lateral collateral ligament, and lateral capsule.
- Osteotomy: Creation of an intentional bone cut in the first metatarsal (or proximal phalanx) to correct the IMA, HVA, and/or DMAA.
- Fixation: Stable internal fixation of the osteotomy.
- Medial Capsular Plication: Tightening of the attenuated medial capsule to maintain correction and stabilize the joint.
Step-by-Step for a Common Technique (e.g., Chevron/Scarf Osteotomy with Lateral Release and Medial Capsular Plication)
-
Incision and Exposure:
- Perform a dorsomedial longitudinal incision centered over the first MTP joint and extending proximally along the first metatarsal.
- Carefully dissect through subcutaneous tissues. Identify and protect the medial dorsal cutaneous nerve and superficial veins, retracting them dorsally or plantarly.
- Perform an L-shaped or inverted L-shaped medial capsulotomy, with the transverse limb extending along the plantar aspect of the metatarsal head and the longitudinal limb along the medial aspect of the first metatarsal. Alternatively, a straight longitudinal capsulotomy can be used.
-
Medial Bunionectomy:
- Retract the medial capsule and expose the medial eminence of the first metatarsal head.
- Using an oscillating saw, resect the prominent medial eminence. The cut should be parallel to the medial aspect of the first metatarsal shaft and should not violate the sagittal groove (crista) for the sesamoids. Avoid over-resection, which can destabilize the sesamoid complex.
-
Lateral Soft Tissue Release:
- This is typically performed through the existing medial incision by distracting the joint and passing instruments laterally, or through a separate small incision dorsolaterally between the first and second metatarsals.
- A small lateral incision (1-2 cm) between the first and second MTP joints provides direct access to the adductor hallucis and DTML.
- Carefully dissect to identify and release the adductor hallucis tendon from its insertion on the lateral aspect of the proximal phalanx and the fibular sesamoid.
- Release the lateral collateral ligament and the lateral aspect of the MTP joint capsule.
- If using the medial approach, distract the first MTP joint. Pass a small scalpel or curved osteotome laterally to release the adductor tendon, lateral capsule, and DTML. Confirm adequate release by passively correcting the hallux valgus deformity to a neutral position. Crucial: Protect the neurovascular structures in the first web space during lateral release.
-
First Metatarsal Osteotomy (Choice depends on deformity severity):
-
Chevron (Austin) Osteotomy (for mild-moderate IMA, HVA):
- Mark a V-shaped osteotomy on the first metatarsal head, typically with an apex angle of 60 degrees. The apex points distally (standard) or proximally (reversed).
- The plantar limb of the osteotomy should be approximately 3-5mm proximal to the articular cartilage.
- Make the cuts with an oscillating saw, ensuring both dorsal and plantar cortices are fully cut.
- Laterally translate the distal fragment (metatarsal head) by 2-5mm to correct the IMA. Ensure the osteotomy is stable and the cut surfaces are well apposed.
- Optional: Plantarflexion of the head can be achieved by angling the translation.
- Fixation: Typically with one or two small headless compression screws or a single K-wire. The K-wire is often removed post-op.
-
Scarf Osteotomy (for moderate-severe IMA, HVA, and pronation):
- This is a Z-shaped osteotomy extending along the shaft of the first metatarsal, allowing for significant translation, rotation, and length adjustment.
- Mark a longitudinal dorsal cut and a longitudinal plantar cut along the first metatarsal shaft. These cuts should be parallel.
- Connect the longitudinal cuts with two oblique transverse cuts at the proximal and distal ends, creating the Z-shape. The proximal oblique cut typically goes from dorsoproximal to plantar-distal, and the distal oblique cut from dorsodistal to plantar-proximal.
- Using an oscillating saw, carefully perform the osteotomy, creating two interlocking fragments.
- Translate the distal fragment laterally to correct the IMA.
- Derotate the fragment to correct pronation if present.
- Optional: Minor lengthening or shortening, plantarflexion or dorsiflexion can be achieved.
- Fixation: Typically with two screws (e.g., 2.7mm or 3.0mm cortical screws or headless compression screws) placed perpendicularly to the osteotomy planes.
-
Lapidus Procedure (First Tarsometatarsal Arthrodesis, for severe IMA, first ray hypermobility, or TMT arthritis):
- Incision: Dorsomedial incision over the first TMT joint.
- Exposure: Dissect down to the first TMT joint, identifying and protecting neurovascular structures.
- Cartilage Resection: Resect articular cartilage from the medial cuneiform and the base of the first metatarsal.
- Correction: Reduce the metatarsus primus varus (correct IMA) and elevate the first metatarsal if hypermobility is present. Correct for any pronation.
- Fixation: Secure arthrodesis with screws (e.g., crossing cancellous screws), a locking plate, or a combination. The goal is rigid stabilization.
-
-
Akin Osteotomy (Adjunct for Hallux Valgus Interphalangeus):
- If residual hallux valgus deformity or hallux valgus interphalangeus (lateral deviation of the distal phalanx relative to the proximal phalanx) persists after metatarsal osteotomy.
- Perform a medial closing wedge osteotomy at the base of the proximal phalanx.
- Fixation: Secure with a K-wire or a small staple.
-
Medial Capsular Plication:
- After osseous correction and fixation, the medial capsule will be lax.
- Overlap and plicate the medial capsule with non-absorbable sutures (e.g., 2-0 or 3-0 braided polyester) to tighten it and maintain the hallux in a corrected position.
-
Closure:
- Perform layered closure of the subcutaneous tissues and skin.
- Apply a sterile dressing, often incorporating a splint or surgical boot to maintain the correction.
Internervous Planes
While specific internervous planes are less distinct in foot surgery compared to large joint approaches, critical neurovascular structures are always at risk.
* The
medial dorsal cutaneous nerve
typically lies superficial to the abductor hallucis muscle and tendon, directly in the path of a medial incision. Dissection should be performed either directly on the bone (subperiosteal) or carefully superficial to the nerve to protect it.
* The
neurovascular bundle
in the first web space (first dorsal metatarsal artery, deep peroneal nerve branches) is vulnerable during lateral soft tissue release. Dissection for the lateral release should be meticulous and performed under direct visualization, usually through a separate small incision or by careful distraction and blunt dissection from the medial side.
Reduction and Fixation Principles
- Anatomical Reduction: The goal is to restore normal HVA, IMA, DMAA, and sesamoid position.
- Stable Fixation: The osteotomy must be rigidly fixed to allow for early, protected motion and bone healing. This typically involves compression or locking screws appropriate for the bone quality and osteotomy type.
- Multidirectional Correction: Address all components of the deformity: valgus, varus (of the metatarsal), and pronation.
- Prevent Overcorrection: Overcorrection can lead to iatrogenic hallux varus, a challenging complication.
Complications & Management
Despite significant advancements, hallux valgus surgery carries potential complications. A thorough understanding of these risks, their incidence, and appropriate management strategies is crucial for academic surgeons.
Common Complications and Management Strategies
| Complication | Incidence (approx.) | Salvage Strategies
You Might Also Like