Intramedullary Fixation for Extra-Articular Distal Radius Malunions: A Comprehensive Surgical Guide
Key Takeaway
Intramedullary fixation offers a low-profile, biomechanically robust alternative to volar plating for extra-articular distal radius malunions. This technique utilizes a completely intraosseous implant, minimizing soft tissue irritation. Successful execution requires precise preoperative planning, meticulous dorsal approach, corrective osteotomy, and provisional reduction prior to nail insertion. This guide details the indications, step-by-step surgical technique, and postoperative protocols for optimal functional recovery.
INTRODUCTION TO DISTAL RADIUS MALUNIONS
Extra-articular malunions of the distal radius represent a complex reconstructive challenge, often resulting from nonoperative management of displaced fractures or secondary loss of reduction following initial fixation. The anatomic distortion—characterized by loss of radial length, altered radial inclination, and abnormal volar or dorsal tilt—profoundly disrupts the kinematics of the radiocarpal and distal radioulnar joints (DRUJ). Patients typically present with a constellation of symptoms including midcarpal pain, restricted range of motion, diminished grip strength, and ulnar-sided wrist pain secondary to ulnocarpal abutment.
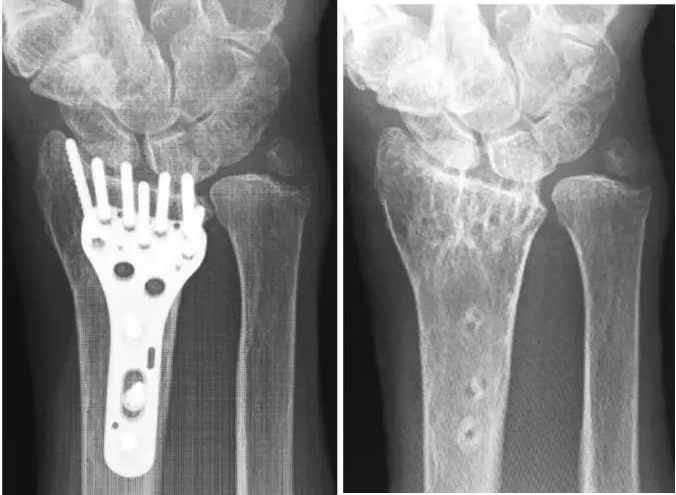
While volar locking plates have long been the workhorse for corrective osteotomies, they are not without complications, particularly regarding flexor tendon irritation and the necessity for extensive soft tissue stripping. Intramedullary fixation has emerged as a highly effective, low-profile alternative. Pioneered and validated by Ilyas et al., modern intramedullary implants (such as the MICRONAIL; Wright Medical, Memphis, TN) sit entirely within the medullary canal of the distal radius. This intraosseous position theoretically eliminates the risk of hardware-induced tendon rupture and provides a load-sharing biomechanical construct that is highly stable against bending and torsional forces.
BIOMECHANICS AND IMPLANT RATIONALE
The fundamental advantage of intramedullary fixation lies in its central mechanical axis. Unlike eccentric plating systems, which act as load-bearing devices subject to cantilever bending forces, an intramedullary nail acts as an internal splint. It shares the load with the surrounding cortical bone and the interpositional bone graft.
The implant is designed to be exceptionally low profile. Distal fixation is achieved via three interlocking nails placed in a divergent pattern, capturing the subchondral bone of the radial styloid, the dorsal rim, and the volar lunate facet. Proximal fixation utilizes two 2.7-mm bicortical interlocking screws directed from dorsal to volar, effectively neutralizing rotational forces and maintaining restored radial length.
💡 Clinical Pearl: Reduction Sequencing
A critical distinction between intramedullary nailing and volar plating in the distal radius is the sequence of reduction. A locking plate can often be applied to the distal fragment and used as a lever to assist in reduction. Conversely, the intramedullary nail is a fixed-angle, space-occupying device; the distal radius must be anatomically reduced and provisionally stabilized before the nail can be introduced into the medullary canal.
INDICATIONS AND CONTRAINDICATIONS
Patient selection is paramount for the success of intramedullary fixation in corrective osteotomies. The decision to proceed should be based on a combination of radiographic parameters and clinical symptomatology.
Radiographic Indications for Corrective Osteotomy
Surgical intervention utilizing intramedullary fixation is indicated when the distal radial deformity exceeds the following thresholds:
* Radial Inclination: Deformity resulting in greater than 15 degrees loss of normal radial inclination.
* Radial Length: Loss of radial length exceeding 4 mm (often correlating with positive ulnar variance).
* Ulnar Variance: Positive ulnar variance of 4 mm or greater, leading to symptomatic ulnocarpal impaction.
* Sagittal Tilt: Deformity exceeding 15 degrees of dorsal tilt or 20 degrees of volar tilt.
Contraindications
- Absolute: Active local or systemic infection; intra-articular malunions (the nail cannot independently reduce or compress articular step-offs); skeletal immaturity (open physes).
- Relative: Severe osteopenia or osteoporosis (which may compromise the purchase of the distal divergent interlocking nails); diaphyseal deformities that preclude the passage of the straight intramedullary device.
PREOPERATIVE PLANNING
Meticulous preoperative planning is the cornerstone of a successful corrective osteotomy. Standard posteroanterior (PA) and lateral radiographs of both the affected and contralateral (normal) wrists are mandatory. The contralateral wrist serves as the anatomic template for restoring length, tilt, and inclination.
Advanced imaging, specifically a fine-cut Computed Tomography (CT) scan with 3D reconstructions, is highly recommended. CT imaging allows for precise mapping of the malunion apex, evaluation of the DRUJ congruity, and assessment of bone stock. Preoperative templating should determine the exact site of the osteotomy, the size of the structural bone graft required (typically corticocancellous graft from the iliac crest), and the appropriate length and diameter of the intramedullary nail.
SURGICAL TECHNIQUE: STEP-BY-STEP
1. Patient Positioning and Preparation
- Place the patient in the supine position with the affected extremity extended on a radiolucent hand table.
- Apply a well-padded proximal arm tourniquet.
- Position the image intensifier (C-arm) parallel to the table to allow for seamless AP and lateral fluoroscopic imaging without compromising the sterile field.
- Prepare and drape the arm, as well as the ipsilateral iliac crest (for structural bone graft harvesting), in a standard sterile fashion.
2. Surgical Approach
- Incision: Make a 3-cm dorsal longitudinal incision centered over Lister’s tubercle, extending proximally over the radial shaft.
- Superficial Dissection: Carry sharp dissection through the skin only to preserve the dorsal sensory branches of the radial nerve and the dorsal cutaneous branch of the ulnar nerve. Perform blunt dissection down to the level of the extensor retinaculum.
- Tendon Management: Identify the third dorsal compartment. Open the compartment, identify the extensor pollicis longus (EPL) tendon, release it from its sheath, and transpose it radially.
- Deep Dissection: Develop the interval between the transposed EPL tendon and the extensor digitorum communis (EDC) tendons of the fourth compartment. Retract the EDC ulnarly to expose the dorsal aspect of the distal radius and the malunion site.
- Preparation of the Osteotomy Site: Meticulously débride the overlying hypertrophied periosteum and scar tissue to clearly delineate the bony anatomy.
3. The Corrective Osteotomy
- Execution: Perform the osteotomy at the apex of the malunion using a fine oscillating saw or a sharp osteotome, under continuous saline irrigation to prevent thermal necrosis.
- Dorsal Malunions: For classic dorsally malunited fractures (Colles-type), use an osteotome to carefully free the distal radius. Hinge the osteotomy on the intact volar cortex. Insert a laminar spreader into the dorsal osteotomy site to gently open the wedge, restoring volar tilt and radial length.
- Complex/Shortened Malunions: If the volar cortex is not intact, or if there is severe shortening with overlap of the cortices, the osteotomy must be taken circumferentially through both the dorsal and volar cortices.
- Soft Tissue Release: Maximize the mobilization of the distal radial fragment. It is imperative to release the surrounding contracted soft tissues.
⚠️ Surgical Warning: The Brachioradialis
The brachioradialis tendon is a primary deforming force that contributes to radial shortening and loss of inclination. Failure to completely release the brachioradialis insertion from the radial styloid will make restoration of radial length nearly impossible and place excessive tension on the hardware.
4. Reduction and Provisional Fixation
- Once the distal fragment is fully mobilized, manually restore radial length, radial inclination, and volar tilt.
- Provisionally fix the reduction using a 0.062-inch Kirschner wire (K-wire). Place the K-wire dorsally, directing it along the ulnar column of the radius to avoid interfering with the central medullary canal where the nail will be inserted.
- Confirm the provisional reduction using multi-planar fluoroscopy. Ensure that the anatomical parameters match the preoperative template.
5. Intramedullary Nail Insertion and Fixation
- Canal Preparation: With the reduction held provisionally, create a starting portal in the distal radius (typically at the dorsal lip of the radial articular surface, taking care not to breach the radiocarpal joint). Use the system-specific awl and reamers to prepare the medullary canal.
- Nail Insertion: Insert the selected intramedullary nail (e.g., MICRONAIL) over a guide wire until it is completely countersunk beneath the cortical surface.
- Distal Locking: Utilize the targeting guide to place the three distal interlocking nails. These are inserted in a divergent pattern to capture the maximum volume of subchondral bone in the radial styloid and lunate facet.
- Proximal Locking: Drill and insert two 2.7-mm bicortical interlocking screws through the proximal aspect of the nail. These screws are directed from dorsal to volar. This step locks in the restored length and rotational alignment.
6. Bone Grafting
- The opening wedge osteotomy creates a structural void that must be filled to prevent delayed union, nonunion, or hardware failure.
- Harvest a corticocancellous bone graft from the ipsilateral anterior iliac crest.
- Shape the graft to precisely match the dimensions of the osteotomy defect.
- Impact the interpositional graft into the defect. The intramedullary nail provides the mechanical stability, while the graft provides the osteoconductive and osteoinductive scaffold for healing.
7. Assessment of the Distal Radioulnar Joint (DRUJ)
- Following rigid fixation of the radius, meticulously assess the DRUJ for stability and congruity.
- Evaluate passive pronation and supination of the forearm.
- Management of Residual DRUJ Pathology: In many cases, restoring the anatomic alignment of the radius will spontaneously relocate and stabilize the DRUJ. However, if there is residual articular incongruity of the sigmoid notch, or if there is a persistent loss of passive forearm rotation despite stable radial fixation, a concomitant DRUJ procedure is required.
- Options include a DRUJ arthroplasty, a Darrach procedure (distal ulnar resection), or a Sauvé-Kapandji procedure (DRUJ arthrodesis with proximal ulnar pseudoarthrosis), depending on patient age, functional demands, and the specific pathology.
8. Closure
- Thoroughly irrigate the wound.
- Leave the EPL tendon transposed radially, outside of its original compartment, to prevent attrition and rupture against the dorsal hardware or osteotomy site.
- Close the extensor retinaculum loosely over the EDC tendons.
- Perform a layered closure of the subcutaneous tissue and skin.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol must balance the need for early mobilization to prevent stiffness with the necessity of protecting the osteotomy site until biological union occurs.
- Immediate Postoperative Phase (0-2 Weeks): The wrist is immobilized in a well-padded volar splint in a neutral position. Elevation and active digit range of motion are highly encouraged immediately to minimize edema and prevent tendon adhesions.
- Extended Immobilization (If Applicable): If the corrective osteotomy required a significant lengthening of 10 mm or more, the tension on the soft tissues and the graft site is substantial. In these specific cases, the patient is transitioned to a well-molded below-elbow cast for a total of 6 weeks.
- Early Rehabilitation (2-6 Weeks): For standard corrections (<10 mm lengthening), the volar splint is removed at 2 weeks. The patient is transitioned to a removable thermoplastic splint. Supervised physical therapy is initiated, focusing on active and active-assisted range of motion of the wrist and forearm. Activities of daily living (ADLs) are permitted within the limits of pain.
- Strengthening Phase (8+ Weeks): Activities against resistance, heavy lifting, and manual labor are strictly prohibited until radiographic union is definitively confirmed. This is rarely achieved before 8 weeks postoperatively. Once bridging trabeculae are visible across the osteotomy and graft sites, progressive strengthening exercises are introduced.
- Hardware Removal: Due to the intraosseous, low-profile nature of the intramedullary nail, routine hardware removal is not indicated. The plate and screws are removed only in the rare event of symptomatic hardware irritation or if explicitly requested by the patient after complete bony consolidation.
COMPLICATIONS AND PITFALLS
While intramedullary fixation of distal radius malunions yields excellent outcomes in appropriately selected patients, surgeons must be vigilant regarding potential complications:
- Inadequate Reduction: Because the nail cannot be used to reduce the fracture, failure to achieve perfect provisional reduction prior to reaming will result in the nail locking the bone in a malaligned position.
- Hardware Prominence: If the proximal interlocking screws are excessively long, they may protrude through the volar cortex, risking irritation or rupture of the flexor tendons (e.g., Flexor Pollicis Longus). Precise depth measurement is critical.
- Nonunion/Delayed Union: Failure to adequately pack the osteotomy defect with high-quality corticocancellous graft can lead to nonunion, eventually resulting in fatigue failure of the intramedullary nail.
- Iatrogenic Fracture: Overzealous reaming or forceful insertion of the nail in a narrow medullary canal can cause iatrogenic splitting of the radial diaphysis.
By adhering to strict indications, executing meticulous preoperative planning, and respecting the biomechanical principles of intramedullary fixation, orthopedic surgeons can reliably restore function and anatomy in patients suffering from extra-articular distal radius malunions.
You Might Also Like