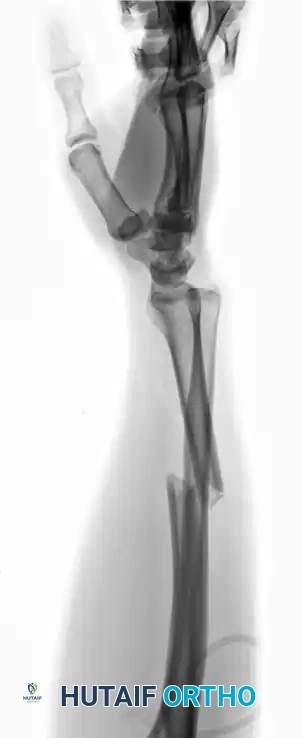
Distal Radius Malunion: Comprehensive Clinical Evaluation and Surgical Management
Key Takeaway
Distal radius malunions frequently present with pain, stiffness, weakness, and cosmetic deformity. Comprehensive clinical evaluation must differentiate mechanical radiocarpal or distal radioulnar joint (DRUJ) pathology from dystrophic pain. Surgical management is indicated for symptomatic functional deficits or in young patients with severe radiographic deformity. Treatment ranges from corrective intraarticular and extraarticular osteotomies to DRUJ reconstruction and salvage procedures, depending on patient demands and arthritic changes.
INTRODUCTION TO DISTAL RADIUS MALUNIONS
Distal radius fractures are among the most common orthopedic injuries, and despite advancements in internal fixation, malunion remains a frequent and functionally debilitating complication. A malunion alters the complex kinematics of the radiocarpal, midcarpal, and distal radioulnar joints (DRUJ). The resulting biomechanical derangement leads to altered load transmission across the wrist, predisposing the patient to post-traumatic arthrosis, carpal instability, and significant functional impairment.
The management of distal radius malunions requires a profound understanding of wrist pathoanatomy, meticulous clinical and radiographic evaluation, and precise surgical execution. This guide provides an exhaustive, evidence-based framework for the evaluation and operative management of these complex deformities.
CLINICAL EVALUATION
The clinical evaluation of a distal radial malunion must be systematic and exhaustive. Patients typically present with a combination of pain, stiffness, weakness, and cosmetic deformity. The primary objective of the physical examination is to isolate the exact anatomical source of the symptoms and differentiate mechanical pathology from dystrophic pain syndromes.
History and Symptom Localization
A detailed history should document the original injury mechanism, initial treatment modality, and the progression of symptoms. The site, intensity, and precipitating factors of the pain must be meticulously recorded:
* Radiocarpal Joint Pain: Typically exacerbated by extreme flexion or extension and loading of the wrist.
* Distal Radioulnar Joint (DRUJ) Pain: Often elicited during forearm rotation (pronation/supination) and gripping activities.
* Midcarpal Pain: May indicate secondary carpal instability patterns resulting from the altered radial articular geometry.
Physical Examination Parameters
- Range of Motion (ROM): Precise goniometric measurements of flexion, extension, radial deviation, ulnar deviation, pronation, and supination must be obtained and compared to the contralateral uninjured wrist.
- Grip Strength: Jamar dynamometer readings of the affected and uninjured wrists are critical for quantifying weakness and establishing a baseline for postoperative functional recovery.
- DRUJ Stability: Assessed via the DRUJ ballottement test in neutral, full pronation, and full supination.
- Soft Tissue Integrity: Evaluate the degree of scar formation, tendon gliding, and neurovascular status. Attritional ruptures of the extensor tendons—most commonly the extensor pollicis longus (EPL)—and, less frequently, the flexor tendons, must be ruled out.
Clinical Pearl: Mechanical symptoms (e.g., catching, locking, or pain strictly with movement) must be carefully distinguished from dystrophic pain (e.g., burning, hyperalgesia, allodynia), which may indicate impending or active Complex Regional Pain Syndrome (CRPS).
RADIOGRAPHIC EVALUATION AND BIOMECHANICS
Standard posteroanterior (PA), lateral, and oblique radiographs of both wrists are mandatory. Computed Tomography (CT) with 3D reconstructions is highly recommended for intraarticular malunions to assess articular step-offs and plan osteotomy trajectories.
Radiographic Criteria for Acceptable Healing
Surgical decision-making relies heavily on comparing the patient's anatomy to established radiographic criteria for acceptable healing. Deviation beyond these parameters significantly increases the risk of symptomatic arthrosis.
- Radioulnar Length: Radial shortening of < 5 mm at the DRUJ compared with the contralateral wrist.
- Radial Inclination: Inclination on the PA film ≥ 15 degrees.
- Radial Tilt: Sagittal tilt on the lateral projection between 15 degrees of dorsal tilt and 20 degrees of volar tilt.
- Articular Incongruity: Incongruity of an intraarticular fracture ≤ 2 mm at the radiocarpal joint.
Biomechanics and Pathoanatomy
The normal distal radius has an average volar tilt of 11 degrees and a radial inclination of 22 degrees. Alteration of these angles drastically shifts load-bearing forces.

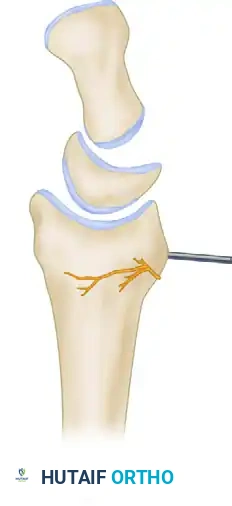
Figure A: Normal radiocarpal and intercarpal alignment in the sagittal plane.
Dorsal Malunion:
Dorsal tilting of the radius shifts the axial load dorsally onto the radiocarpal joint and increases the load transmitted through the ulna. This abnormal tilt may produce a carpal collapse pattern similar to that seen in dorsal intercalated segment instability (DISI), but notably without interosseous ligament disruption or secondary midcarpal instability.
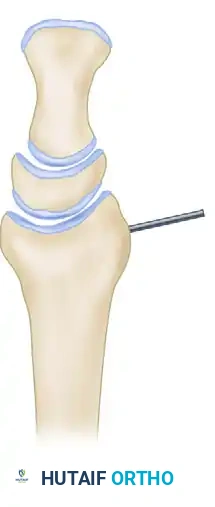
Figure B: Dorsal tilting of the radius producing a carpal collapse pattern.
Volar Malunion:
Conversely, excessive volar tilt, often seen in die-punch fractures of the lunate facet, shifts the carpus volarly. This can produce a malalignment pattern similar to volar intercalated segment instability (VISI).
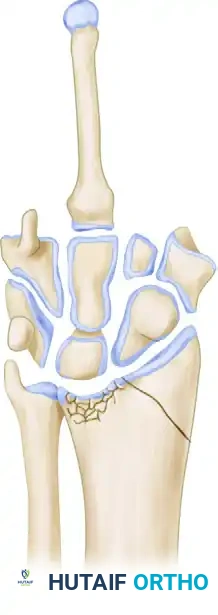
Figure C: Die-punch fracture of the lunate facet producing a volarly tilted malunion.
Surgical Warning: Lengthening of the distal radius by more than 6 mm during corrective osteotomy significantly increases pressure within the carpal tunnel, elevating the risk of acute postoperative median nerve neuropathy. Prophylactic carpal tunnel release should be strongly considered in these cases.
INDICATIONS AND CONTRAINDICATIONS FOR SURGERY
Operative Indications
Surgical intervention is primarily indicated for:
1. Pain and functional deficits severe enough to interfere significantly with daily activities.
2. Identifiable radiographic deformity of the distal radius, DRUJ, or both.
3. Early arthrosis of the radiocarpal or distal radioulnar joint in a symptomatic patient.
Operative treatment is seldom indicated for minimally symptomatic patients, regardless of the severity of the radiographic or cosmetic deformity.
The Prophylactic Exception:
One critical exception is the young, active patient (< 40 years old) with a severe deformity that is highly likely to become symptomatic over time. Prophylactic correction is justified in this demographic if they present with:
* Articular step-off > 2 mm.
* Evidence of carpal instability.
* > 20 to 30 degrees of dorsal angulation.
* A severely incongruent DRUJ.
Contraindications: Complex Regional Pain Syndrome (CRPS)
Surgery is strictly contraindicated in patients with active Reflex Sympathetic Dystrophy (RSD) syndrome, now more commonly known as Complex Regional Pain Syndrome (CRPS).
CRPS is a distressing complication characterized in its early stages by extreme soft-tissue swelling, exquisite tenderness to pressure, and pain on motion. As the condition progresses, definite circulatory changes occur; the skin becomes purplish, cold, and perspires excessively. In late stages, profound joint stiffness affects the fingers, wrist, and secondarily the shoulder and elbow due to voluntary immobilization.
Diagnosis and Management of CRPS:
* Radiography: May show mottled decalcification or periarticular osteoporosis in late stages, though 30% of patients exhibit no radiographic abnormalities.
* Bone Scan: Three-phase delayed image bone scanning is highly diagnostic. Kozin et al. suggested that an abnormal scan in any of the three phases correlates with CRPS, whereas Mackinnon and Holder indicated that only abnormalities in the third phase (delayed static phase) are definitively correlated.
* Treatment: CRPS must be aggressively treated and stabilized before any surgical intervention for malunion is considered. Treatment consists of minimal immobilization, active and passive ROM exercises, sympathetic nerve blocks (stellate ganglion blocks), and intensive occupational therapy. Surgery must be delayed until symptoms are relatively static or definite improvement is apparent.
SURGICAL MANAGEMENT STRATEGIES
Procedures used to treat malunions of the distal radius fall into three general categories. These can be used in isolation or combination, dictated by the specific deformity, functional demands, and degree of arthrosis.
1. Deformity Correction (Osteotomies)
Distal radial osteotomy (intraarticular or extraarticular) with or without bone grafting is the gold standard for young, active patients with significant radial deformity, good bone stock, and minimal arthritic changes. Correcting the radial deformity often spontaneously resolves DRUJ incongruence.
2. DRUJ Pathological Procedures
If DRUJ incongruity or ulnar impaction persists after radial correction, or if the primary pathology is isolated to the DRUJ, the following procedures are utilized:
* Ulnar Shortening Osteotomy: Ideal for positive ulnar variance with preserved DRUJ cartilage.
* Hemiresection Interposition Arthroplasty (Bowers): For DRUJ arthrosis.
* Sauvé-Kapandji Procedure: Arthrodesis of the DRUJ with creation of a proximal ulnar pseudarthrosis. Excellent for severe DRUJ arthrosis in high-demand patients.
* Darrach Procedure: Resection of the distal ulna. Reserved for low-demand, elderly patients due to the risk of ulnar stump instability.
3. Salvage Procedures
For advanced radiocarpal arthrosis or unsalvageable intraarticular deformities:
* Limited Intercarpal Arthrodesis (e.g., radioscapholunate fusion).
* Total Wrist Arthrodesis: The ultimate salvage for profound, painful arthrosis.
* Total Wrist Arthroplasty: For low-demand patients seeking motion preservation.
* Proximal Row Carpectomy (PRC): If the lunate facet is destroyed but the capitate is preserved.
STEP-BY-STEP SURGICAL TECHNIQUE: VOLAR CORRECTIVE OSTEOTOMY
The volar approach utilizing a fixed-angle locking plate is currently the workhorse for correcting extraarticular dorsal and volar malunions.
Preoperative Planning and Positioning
- Templating: Utilize contralateral normal wrist radiographs to determine the exact Center of Rotation of Angulation (CORA) and calculate the required opening wedge angle and graft size.
- Positioning: The patient is placed supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: A well-padded pneumatic tourniquet is applied to the proximal arm and inflated to 250 mmHg after exsanguination.
Surgical Approach (Modified Henry)
- Incision: Make a longitudinal incision over the flexor carpi radialis (FCR) tendon, extending from the distal wrist crease proximally for 8-10 cm.
- Superficial Dissection: Incise the superficial fascia. Identify and retract the FCR tendon ulnarly. Caution: Protect the palmar cutaneous branch of the median nerve, which lies ulnar to the FCR.
- Deep Dissection: Incise the floor of the FCR sheath. Retract the flexor pollicis longus (FPL) and the median nerve ulnarly. Retract the radial artery radially.
- Pronator Quadratus Elevation: Identify the pronator quadratus (PQ) muscle. Make an L-shaped incision along its radial and distal borders. Elevate the PQ off the radius from radial to ulnar, preserving its ulnar attachment for later repair.
Osteotomy Execution
- Marking the Osteotomy: Under fluoroscopic guidance, mark the planned osteotomy site at the CORA using a surgical marker or a shallow score with an oscillating saw.
- Provisional Fixation: Insert two parallel K-wires into the distal fragment (parallel to the articular surface) and two into the proximal fragment (perpendicular to the radial shaft). These serve as joysticks to manipulate the fragments.
- The Cut: Perform the osteotomy using a fine-toothed oscillating saw. Cool the blade continuously with saline to prevent thermal necrosis.
- Correction: Use the K-wire joysticks, lamina spreaders, or specialized osteotomy distractors to open the osteotomy site, restoring volar tilt, radial inclination, and length.
Fixation and Grafting
- Plate Application: Apply a volar locking plate. Secure the distal fragment first with locking screws placed subchondrally to support the articular surface.
- Proximal Fixation: Reduce the proximal shaft to the plate. If an opening wedge was created, a structural void will be present.
- Bone Grafting: Fill the defect with a structural autograft (iliac crest) or a robust structural allograft/synthetic bone substitute. The rigid fixed-angle plate often allows for the use of cancellous chips or substitutes if the volar cortex is structurally bridged by the plate.
- Fluoroscopic Verification: Confirm restoration of radiographic parameters (tilt, inclination, length) and ensure no screws are penetrating the radiocarpal or DRUJ spaces.
Closure
- PQ Repair: Meticulously repair the pronator quadratus over the plate to isolate the flexor tendons from the hardware, minimizing the risk of attritional rupture.
- Skin Closure: Close the subcutaneous tissues and skin in a standard fashion.
- Splinting: Apply a bulky soft dressing and a volar short-arm splint in neutral position.
POSTOPERATIVE PROTOCOL AND REHABILITATION
Successful outcomes depend heavily on a structured, phased rehabilitation program.
- Phase I (0-2 Weeks): The wrist is immobilized in a splint. Immediate active range of motion of the digits, elbow, and shoulder is initiated to prevent stiffness and reduce edema. Edema control measures (elevation, compressive wraps) are critical.
- Phase II (2-6 Weeks): Sutures are removed at 10-14 days. The patient is transitioned to a removable thermoplastic splint. Gentle active and active-assisted ROM of the wrist and forearm begins. Passive stretching is generally avoided until radiographic evidence of early consolidation is present.
- Phase III (6-12 Weeks): Once clinical and radiographic union is confirmed (typically around 6-8 weeks), the splint is discontinued. Progressive strengthening, proprioceptive training, and dynamic splinting (if ROM deficits persist) are instituted.
- Return to Activity: Heavy lifting and high-impact activities are restricted until 3 to 4 months postoperatively, contingent upon complete radiographic union and restoration of near-normal grip strength.
CONCLUSION
The management of distal radius malunions is a technically demanding endeavor that requires precise preoperative planning, respect for soft tissue envelopes, and an intimate understanding of wrist biomechanics. By adhering to strict radiographic criteria, carefully selecting the appropriate surgical intervention, and vigilantly managing complications such as CRPS, the orthopedic surgeon can reliably restore function and alleviate pain in this challenging patient population.
You Might Also Like