Mastering Arthroscopic Preparation: Equipment, Positioning, and Fluid Management
Key Takeaway
Optimal arthroscopic outcomes depend on meticulous surgical preparation. This comprehensive guide details evidence-based protocols for instrument sterilization, joint distention fluid management, and patient positioning. It critically evaluates the biomechanics of circumferential leg holders versus lateral posts, the physiological impact of tourniquet application, and advanced perioperative pain management strategies, including the avoidance of chondrotoxic intraarticular pain pumps.
CARE AND STERILIZATION OF ARTHROSCOPIC INSTRUMENTS
The foundation of successful arthroscopic surgery begins long before the first incision, relying heavily on the meticulous care, handling, and sterilization of highly sensitive optical and mechanical equipment. Arthroscopic instruments represent a significant capital investment and are highly susceptible to degradation if improper sterilization modalities are employed.
Modalities of Sterilization
The selection of a sterilization method is dictated by the thermal and moisture tolerance of the specific instrument.
- Autoclaving (Steam Sterilization): Arthroscopy equipment that is strictly heat-stable and moisture-resistant—such as metallic trocars, blunt obturators, standard cannulas, and basic hand instruments (e.g., biters, graspers, probes)—may be safely autoclaved. Steam sterilization under pressure remains the most rapid, reliable, and cost-effective method for achieving absolute sterility in these robust items.
- Low-Temperature Hydrogen Peroxide Gas Plasma: Heat- or moisture-sensitive equipment, particularly delicate optical devices like the arthroscope itself, high-definition camera heads, and fiber-optic light cables, must never be subjected to the extreme temperatures of an autoclave. These items are optimally sterilized utilizing low-temperature hydrogen peroxide gas plasma (e.g., STERRAD systems). This modality effectively eradicates spores, bacteria, and viruses without degrading the delicate optical interfaces, lens adhesives, or electronic sensors.
- Historical and Suboptimal Modalities: Historically, low-temperature gas sterilization (Ethylene Oxide or EtO) and cold chemical sterilization (activated glutaraldehyde, such as Cidex) were widely utilized. However, contemporary evidence demonstrates that these methods are less effective, require prohibitively long aeration times (in the case of EtO), and carry a significantly higher potential for toxic side effects to both the patient (chemical synovitis) and operating room personnel. They are largely obsolete in modern high-volume orthopedic centers.
Surgical Warning: Residual activated glutaraldehyde on an arthroscope can cause severe, irreversible chemical chondrolysis and profound reactive synovitis. If cold sterilization must be used in austere environments, exhaustive rinsing with sterile saline is mandatory prior to joint insertion.
FLUID MANAGEMENT AND JOINT DISTENTION
Arthroscopy is fundamentally a procedure performed within a fluid medium. The continuous flow of irrigation fluid serves three critical functions: it distends the joint capsule to create a working space, it maintains hemostasis through hydrostatic pressure, and it clears the visual field of blood, synovial debris, and chondral fragments.
Delivery Systems: Gravity vs. Mechanical Pumps
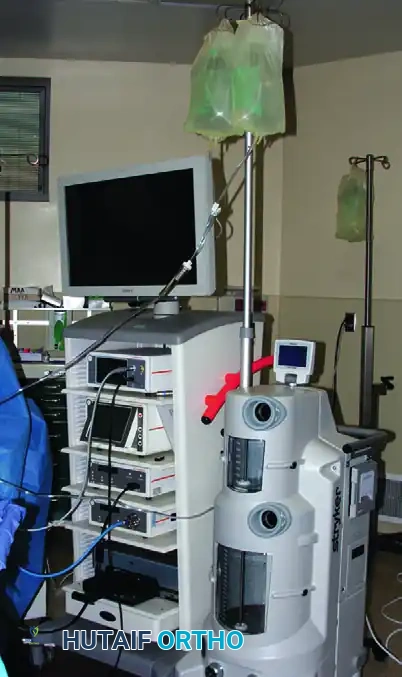
Fluid delivery can be achieved via simple gravity systems or sophisticated automated arthroscopic pumps.

As illustrated above, a gravity system with a water VAC system or an automated arthroscopic pump may be used to deliver fluid. Inflow may be directed through the arthroscopic sheath itself or via a separate dedicated inflow cannula.
- Gravity Inflow: Relies on the height of the fluid bags above the patient's joint. As a general rule, every 1 foot of elevation above the joint generates approximately 22 mm Hg of hydrostatic pressure. While safe and cost-effective, gravity systems often fail to provide the dynamic pressure adjustments required during complex reconstructive procedures.
- Automated Arthroscopic Pumps: These devices monitor and adjust inflow and outflow to maintain a constant intraarticular pressure and flow rate. The surgeon must be acutely aware of the individual variations of different pump flow dynamics and sensor mechanisms to prevent catastrophic fluid extravasation.
Joint-Specific Pressure Parameters
The optimal distention pressure varies significantly depending on the anatomic joint, the surrounding soft tissue envelope, and the patient's systemic hemodynamics.
- The Knee: Standard pump pressures for routine knee arthroscopy should be maintained between 60 to 80 mm Hg. This provides adequate distention of the suprapatellar pouch and compartments without causing excessive fluid extravasation into the calf or thigh.
- The Shoulder: Vision and hemostasis in the glenohumeral joint and subacromial space are usually optimized when the distention pressure is maintained approximately 30 mm Hg below the patient's systolic blood pressure. In healthy patients, controlled hypotensive anesthesia may be utilized by the anesthesia team to reduce the systolic pressure to approximately 100 mm Hg. At this level, a pump pressure of 70 to 80 mm Hg usually provides safe distention and crystal-clear vision without excessive bleeding.
- Small Joints (Elbow and Ankle): Because of the tight fascial compartments and the significantly increased likelihood of fluid extravasation leading to compartment syndrome, distention pressures in the elbow and ankle must be strictly maintained at approximately 40 to 60 mm Hg. We strongly recommend using gravity inflow rather than automated pumps for distention in small joints to mitigate the risk of catastrophic capsular rupture and neurovascular compromise.
Pharmacologic Adjuvants in Irrigation Fluid
The addition of epinephrine to the irrigation fluid is a well-established technique to enhance visualization. Olszewski et al., in a prospective, double-blinded, randomized study, demonstrated that the addition of epinephrine (1 mg per liter of normal saline) significantly increased intraarticular visibility and reduced the need for tourniquet inflation by 50% compared with a placebo group.
Similarly, Karaoglu et al. found that adding a small amount of epinephrine (50 mg/10 mL) to the local anesthetic mixture injected at the portal sites just before incision dramatically improved arthroscopic viewing by inducing local vasoconstriction.
Clinical Pearl: While epinephrine is highly effective for hemostasis, it is not without systemic risks. In patients with a history of severe hypertension, coronary artery disease, or cardiac arrhythmias, we strictly forgo the use of epinephrine in the irrigation fluid to prevent systemic absorption and subsequent cardiovascular events.
PATIENT POSITIONING AND LEG HOLDERS
Optimal positioning is critical for safe access to the intraarticular structures of the knee. The choice between a circumferential leg holder and a lateral post dictates the biomechanical forces that can be applied to the joint during the procedure.
Circumferential Leg Holders
The primary advantage of a circumferential leg holder is that it firmly secures the distal thigh, permitting the surgeon to apply significant valgus and external rotation stress. This biomechanical maneuver is essential to open the posteromedial compartment, allowing for better viewing, manipulation of the medial meniscus, and complex posterior horn meniscal surgery, especially in tight knees.
However, the routine use of a leg holder presents several distinct disadvantages:
1. Positional Limitation: Because the thigh is rigidly held, the number of different positions in which the leg can be placed is somewhat limited, making hyperflexion or figure-four positioning cumbersome.
2. Tourniquet Interference: Many commercial leg holders incorporate a tourniquet within the confines of the holder. In such an arrangement, wide fluctuations in tourniquet pressures may occur when heavy stress is applied to the leg.
3. Iatrogenic Injury: The leg-holding device fixes the distal femur so securely that aggressive applied stress can result in iatrogenic fractures around the knee or tearing of the medial collateral ligament (MCL). Such catastrophic occurrences have been documented in the literature.
The Lateral Post Alternative
An excellent alternative to an encompassing leg holder is a lateral post attached to the side rail of the operating table.
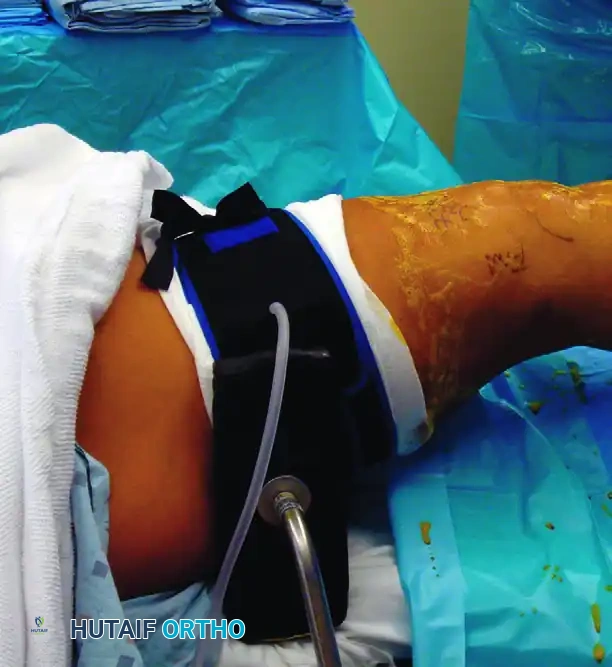
As seen above, the lateral aspect of the distal thigh can be levered against this post to apply valgus stress for opening the posteromedial compartment.
The lateral post does not confine or prevent the knee from being manipulated into an almost unlimited number of positions, including deep flexion and the figure-four position (required for lateral compartment access). It therefore possesses distinct advantages over many expensive commercial leg-holding devices. We preferentially utilize the lateral post for major knee reconstructive procedures, including multiligamentous repairs.
Surgical Decision Making: If the clinical evaluation suggests isolated medial compartment meniscal disease, a circumferential leg holder can be of significant assistance. Conversely, if a patellofemoral joint tracking issue, a lateral compartment problem, or an endoscopic repair of the anterior cruciate ligament (ACL) is anticipated, a lateral valgus stress post should be chosen. For ACL reconstruction, the end of the table should also be flexed to allow full, unobstructed knee flexion during tibial and femoral tunnel drilling.
TOURNIQUET APPLICATION IN ARTHROSCOPY
During arthroscopic procedures of the knee, ankle, elbow, and other distal joints, a pneumatic tourniquet is almost always applied to the proximal limb and inflated as needed to maintain a bloodless surgical field.
Indications and Contraindications
- Advantages: The primary advantage of tourniquet use is vastly increased visibility, particularly during synovectomies or when addressing highly vascularized pathology. Furthermore, there is no significantly increased postoperative morbidity when tourniquet times are strictly kept to less than 90 to 120 minutes.
- Disadvantages: Routine tourniquet use causes blanching of the synovium, which makes the visual differentiation and diagnosis of various subtle synovial disorders difficult. More importantly, prolonged tourniquet time (exceeding 120 minutes) carries the severe risk of ischemic damage to skeletal muscle and peripheral nervous tissue, potentially leading to neuropraxia or tourniquet paresis.
- Contraindications: Absolute contraindications to the use of a tourniquet include a documented history of deep vein thrombosis (DVT), thrombophlebitis, severe peripheral vascular disease (PVD), or sickle cell disease.
Evidence-Based Tourniquet Protocols
The necessity of routine tourniquet inflation has been challenged in recent literature. Kirkley et al., in a prospective, randomized clinical trial, found no significant differences in functional outcomes between patients in whom a tourniquet was used and those without tourniquet use. Interestingly, there was a trend toward less early postoperative pain and slightly better isokinetic strength testing at 2 weeks in the non-tourniquet group, although intraoperative visibility was rated by surgeons as three times better with tourniquet use. They concluded that a tourniquet inflated to 300 mm Hg did not significantly affect overall long-term functional outcome.
Similarly, in a prospective, randomized trial including 109 patients undergoing arthroscopic knee surgery, Johnson et al. found no significant differences between tourniquet and non-tourniquet groups with respect to operative view, duration of operation, pain scores, analgesic requirement, or complication rates. Because the routine use of a tourniquet did not definitively improve the operative view in their cohort (likely due to adequate pump pressures and epinephrine use), these authors recommended against the routine inflation of a tourniquet for standard arthroscopic knee surgery, reserving it only for cases where hemostasis cannot be otherwise achieved.
ANESTHESIA AND PERIOPERATIVE PAIN MANAGEMENT
The choice of anesthesia and the execution of a multimodal pain management protocol are vital for facilitating early postoperative mobilization and ensuring patient satisfaction. While the majority of major reconstructive procedures are performed under general or regional (spinal) anesthesia, diagnostic arthroscopy and simple meniscectomies can be successfully performed under local anesthesia.
Local Anesthesia Protocols
If a purely local anesthetic technique is chosen, the tourniquet is generally not inflated, as ischemic pain will become intolerable for the awake patient within 20 to 30 minutes.
Yoshiya et al. reported excellent results utilizing a 1:1 mixture of 1% lidocaine (for rapid onset) and 0.25% bupivacaine (for prolonged duration).
* Intraarticular Injection: Usually, 50 mL of this mixture is injected directly into the intraarticular space prior to the procedure.
* Portal Infiltration: At each anticipated portal site, an additional 5 mL of this mixture is injected into the skin and capsule.
* Adjuvants: When a longer procedure is expected, a small amount of epinephrine is added to the mixture to help maintain hemostasis and to increase the duration of action of the anesthetic agents by delaying systemic absorption.
Surgical Warning: Surgeons must exercise extreme mathematical care when utilizing bupivacaine to ensure they do not exceed its maximal safe systemic dosage (2 mg/kg of body weight), as bupivacaine cardiotoxicity is profound and difficult to reverse.
Postoperative Multimodal Analgesia
Postoperative pain should be preemptively managed using a multimodal approach:
* NSAIDs: Pain and reactive synovitis may be significantly diminished by the use of oral nonsteroidal anti-inflammatory drugs (NSAIDs) administered both preoperatively and postoperatively, or via intravenous administration (e.g., Ketorolac) intraoperatively. NSAIDs have been definitively shown to reduce hemarthrosis, decrease swelling, and increase the range of motion in the early postoperative period.
* Corticosteroids: The routine use of oral or intraarticular corticosteroids has not proved effective for routine postoperative pain control and may increase the risk of surgical site infection.
* Intraarticular Analgesia: Beneficial analgesic effects have been well-documented following the intraarticular injection of 30 mL of 0.25% bupivacaine, with or without the addition of 3 mg of preservative-free morphine, at the conclusion of the procedure.
The Danger of Intraarticular Pain Pumps
While single-shot intraarticular injections are safe and effective, the continuous infusion of local anesthetics must be strictly avoided.
Pitfall: We strongly condemn and do not recommend the use of prolonged intraarticular pain pump catheters (particularly those infusing bupivacaine with epinephrine). Overwhelming clinical evidence has linked these devices to catastrophic, irreversible chondrocyte toxicity, leading to devastating conditions such as postarthroscopic glenohumeral chondrolysis (PAGCL). Pain management should rely on systemic multimodal pathways and single-shot blocks rather than continuous intraarticular local anesthetic exposure.
You Might Also Like
