Osteoporosis in Orthopedics: Biomechanics, Fracture Patterns & Surgical Management
Key Takeaway
Osteoporosis significantly impacts orthopedic surgery by compromising bone strength, altering microarchitecture, and leading to complex fragility fractures. This necessitates specialized surgical approaches, considering reduced screw pull-out strength, increased comminution, and the need for robust fixation. Understanding bone biomechanics is crucial for effective preventive strategies and operative management of these challenging fractures.
Introduction & Epidemiology
Osteoporosis, characterized by compromised bone strength predisposing to an increased risk of fracture, represents a significant public health burden with profound implications for orthopedic surgery. It is defined by a bone mineral density (BMD) T-score of -2.5 or lower at the lumbar spine, femoral neck, total hip, or distal one-third radius, as measured by dual-energy X-ray absorptiometry (DEXA). Epidemiologically, it affects over 200 million individuals globally, with age-related prevalence increasing dramatically in postmenopausal women and older men. The lifetime risk of an osteoporotic fracture for women over 50 is approximately 1 in 2, comparable to the risk of coronary artery disease. For men, the risk is about 1 in 4.
The most clinically relevant sequelae of osteoporosis are fragility fractures, which occur from a fall from standing height or less, or with minimal trauma. Common sites include the proximal femur (hip), vertebrae, distal radius, and proximal humerus. Hip fractures, in particular, are associated with significant morbidity and mortality, with up to 20-30% mortality within one year post-fracture and a substantial proportion of survivors experiencing permanent disability and loss of independence. The societal economic impact, driven by acute surgical management, long-term rehabilitation, and loss of productivity, is immense and projected to rise with an aging global population. Understanding the biomechanical implications of osteoporotic bone is paramount for orthopedic surgeons in both preventive strategies and the operative management of these challenging fractures.
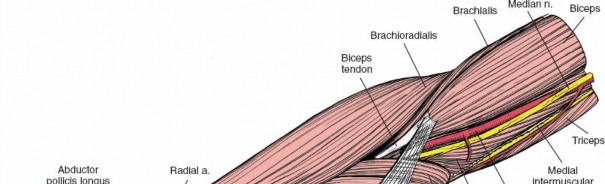
Surgical Anatomy & Biomechanics
The anatomical and biomechanical considerations in osteoporotic bone significantly alter fracture patterns, surgical approach, and fixation stability compared to normal bone. Osteoporosis is characterized by reduced bone mass, microarchitectural deterioration of bone tissue, and altered material properties.
Microarchitecture and Material Properties
- Cortical Bone: Thinning of cortical bone, increased porosity due to expansion of Haversian canals, and greater intracortical remodeling lead to reduced bending and torsional strength.
- Trabecular Bone: Loss of trabecular connectivity, thinning of individual trabeculae, and conversion of plate-like trabeculae to rod-like structures reduce the ability of cancellous bone to resist compressive loads. This significantly impacts metaphyseal regions, which are rich in trabecular bone (e.g., femoral neck, vertebral bodies, distal radius, proximal humerus).
- Material Properties: Beyond density, the intrinsic quality of the bone matrix (collagen cross-linking, mineral crystal size and orientation) can be compromised, leading to increased brittleness and reduced toughness. This makes osteoporotic bone more susceptible to comminution and less resilient during drilling and screw insertion.
Biomechanical Implications for Fracture Patterns and Fixation
- Increased Comminution: Osteoporotic bone tends to fragment extensively under load, resulting in multifragmentary and unstable fracture patterns. This creates challenges for reduction and obtaining adequate purchase for fixation.
- Reduced Pull-out Strength: Screws and other fixation devices have significantly reduced pull-out strength in osteoporotic bone due to poor bone stock. This necessitates careful consideration of implant design, number, and trajectory.
- Stress Risers and Load Sharing: Plates placed on osteoporotic bone act as stress risers at their ends, leading to periprosthetic fractures. Adequate load sharing between implant and bone is crucial, but difficult to achieve in severely osteoporotic bone.
- Intramedullary Fixation: While intramedullary nails can offer load-sharing benefits, screw purchase in the metaphysis can still be problematic. Cement augmentation around screws or specialized interlocking mechanisms are often employed.
- Vertebral Anatomy: The vertebral body, rich in trabecular bone, is particularly susceptible to compression fractures. The weakened endplates and posterior elements contribute to instability and progressive kyphosis.
- Proximal Femur: The femoral neck and intertrochanteric regions, critical weight-bearing areas, are prone to fracture. The weakened trabecular network in the femoral head and neck can lead to challenges in achieving stable fixation with dynamic hip screws or cephalomedullary nails.
- Distal Radius & Proximal Humerus: These metaphyseal regions often exhibit severe trabecular bone loss, leading to articular collapse, comminution, and difficulty in maintaining reduction, particularly in complex fractures.
Indications & Contraindications
The decision-making process for operative versus non-operative management of osteoporotic fractures is complex, balancing fracture stability, patient comorbidities, functional demands, and bone quality.
General Principles
- Non-Operative: Typically reserved for stable, minimally displaced fractures that are amenable to immobilization and can heal without significant functional impairment or pain. Patient compliance, pain tolerance, and the ability to tolerate prolonged immobilization are key considerations.
- Operative: Indicated for unstable fractures, significantly displaced fractures, fractures that compromise neurovascular structures, those leading to unacceptable pain, or those where non-operative management would result in poor functional outcomes (e.g., non-union, malunion, protracted recovery). The goal is to restore anatomical alignment, provide stable fixation for early mobilization, and reduce pain.
Table: Operative vs. Non-Operative Indications for Common Osteoporotic Fractures
| Fracture Type | Operative Indications | Non-Operative Indications |
|---|---|---|
| Proximal Femur | All displaced femoral neck fractures (arthroplasty/fixation). | Minimally displaced/impacted femoral neck fractures in low-demand patients (rare). |
| (Hip) | Unstable intertrochanteric fractures (IMN). | Stable, undisplaced intertrochanteric fractures in non-ambulatory patients (rare). |
| Subtrochanteric fractures (IMN). | ||
| Vertebral Body | Progressive neurological deficit (decompression/stabilization). | Stable, isolated vertebral compression fractures with mild pain. |
| (Spine) | Instability, severe kyphosis, intractable pain after conservative trial (vertebroplasty/kyphoplasty, fusion). | |
| Distal Radius | Intra-articular displacement > 2mm, dorsal/volar tilt > 10-20°, radial shortening > 3mm, severe comminution. | Stable, minimally displaced extra-articular fractures. |
| Open fractures. | Displaced fractures in patients unable to tolerate surgery. | |
| Proximal Humerus | Displaced surgical neck fractures (unstable, poor healing potential). | Undisplaced/minimally displaced 2-part fractures. |
| Displaced 3- or 4-part fractures (ORIF, arthroplasty). | Stable valgus-impacted fractures. | |
| Head-split fractures, articular incongruity. | Fractures in very frail patients with limited functional goals. |
Contraindications
Absolute contraindications to surgery are rare but include an uncorrectable severe medical comorbidity making the risks of anesthesia and surgery prohibitive (e.g., active sepsis, intractable coagulopathy). Relative contraindications may include:
*
Severe uncontrolled comorbidities:
Unstable cardiac disease, acute cerebrovascular event, uncontrolled diabetes.
*
Severe cognitive impairment:
Where patient cooperation for post-operative rehabilitation is impossible, and surgery offers no functional benefit over palliation.
*
Terminal illness:
Where life expectancy is very short and surgery would only add burden.
*
Poor skin condition:
Active infection, severe dermatological issues over the surgical site.
*
Extremely poor bone stock:
In some cases, the bone quality may be so poor that even advanced fixation techniques are unlikely to achieve stable construct, potentially leading to immediate failure or excessive complications. In such scenarios, palliative measures or different reconstructive options (e.g., arthroplasty vs. ORIF for a proximal humerus fracture) may be prioritized.
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes in osteoporotic fracture patients, given their inherent fragilities and potential for complications.
Pre-Operative Planning
-
Patient Assessment:
- Medical Optimization: Comprehensive medical evaluation to identify and optimize comorbidities (cardiac, pulmonary, renal, endocrine, nutritional status). Anemia correction, electrolyte balance, and glycemic control are paramount. Co-management with internal medicine or geriatric specialists is often beneficial.
- Medication Review: Identify antiplatelet or anticoagulant medications and plan their management perioperatively. Review medications for osteoporosis (bisphosphonates, denosumab, teriparatide) as these may impact bone healing and should be continued if possible, or adjusted as per guidelines.
- Cognitive Status: Assess baseline cognitive function to anticipate post-operative delirium risk and plan appropriate interventions.
- Social Support: Evaluate home environment and available social support for post-operative care and rehabilitation.
-
Radiographic Evaluation:
- Standard X-rays: Obtain adequate orthogonal views.
- CT Scan: Essential for complex intra-articular fractures (e.g., distal radius, proximal humerus, tibial plateau) and for evaluating vertebral fractures. It provides detailed information on comminution, articular step-off, and bone loss, aiding in implant selection and surgical strategy.
- DEXA Scan History: Review existing DEXA results if available, to confirm the diagnosis of osteoporosis and understand the patient's baseline bone density. While not always feasible acutely, it informs the overall strategy.
- Bone Quality Assessment: While DEXA is the gold standard for diagnosis, intra-operative assessment of bone quality via drilling resistance or tactile feedback is crucial for screw purchase. Newer CT-based methods like finite element analysis are emerging but not yet standard.
-
Implant Selection and Strategy:
- Augmented Fixation: Plan for strategies to enhance screw purchase, such as polymethylmethacrylate (PMMA) cement augmentation (e.g., vertebroplasty/kyphoplasty, selected plating in proximal humerus, calcaneus, or tibia), locked plating systems with multiple points of fixation, or larger diameter screws.
- Specific Implants: Utilize implants designed for osteoporotic bone, such as angle-stable locked plates, intramedullary nails with multiple locking options, or arthroplasty for severely comminuted intra-articular fractures.
- Pre-Contouring: Pre-contouring plates based on contralateral anatomy or 3D models can save time and improve fit.
- Reduction Techniques: Plan indirect reduction techniques to minimize soft tissue stripping, preserving periosteal blood supply.
- Anesthesia Consultation: Discuss anesthetic risks with the anesthesiologist, especially considering the advanced age and comorbidities common in this patient population. Regional anesthesia may be considered to reduce systemic effects.
- Antibiotic Prophylaxis & DVT Prophylaxis: Standard protocols are applied, often with extended duration DVT prophylaxis given the increased risk in this population.
Patient Positioning
Proper positioning is paramount to allow adequate exposure, fluoroscopic access, and to prevent iatrogenic injuries.
*
General Principles:
*
Padding:
Meticulous padding of all pressure points (heels, sacrum, elbows, ulnar nerve, peroneal nerve) to prevent decubitus ulcers and nerve palsies, especially in thin, frail patients.
*
Temperature Regulation:
Maintain normothermia to reduce perioperative complications.
*
Fluoroscopy Access:
Ensure positioning allows unobstructed C-arm access for intra-operative imaging in multiple planes without requiring patient repositioning.
*
Specific Examples:
*
Proximal Femur Fractures:
Typically supine on a fracture table for intramedullary nailing, allowing for traction and rotation. Lateral decubitus for plating if necessary. Careful attention to perineal post padding.
*
Distal Radius Fractures:
Supine on a hand table, with the arm abducted and externally rotated on a radiolucent arm board. Traction tower may be used.
*
Proximal Humerus Fractures:
Beach chair position (for plating or arthroplasty) or supine with the arm draped free. Careful attention to head/neck support and nerve protection.
*
Vertebral Compression Fractures (for Vertebroplasty/Kyphoplasty):
Prone position on a radiolucent table, ensuring the abdomen is free to reduce epidural venous pressure.
Detailed Surgical Approach / Technique
The surgical approach to osteoporotic fractures requires adaptation due to compromised bone quality and increased comminution. The goal is stable fixation with minimal biological insult, allowing early mobilization. General principles include: gentle tissue handling, indirect reduction techniques, stable internal fixation, and often augmentation strategies.
Principles of Fixation in Osteoporotic Bone
- Indirect Reduction: Minimize periosteal stripping and avoid devascularization of bone fragments to preserve the biological environment for healing. Use ligamentotaxis, traction, and external manipulators where possible.
-
Stable Fixation Constructs:
- Locked Plating Systems: These are preferred over conventional plates as screws lock into the plate, creating a fixed-angle construct that bypasses poor bone quality for screw purchase. This construct acts as an internal fixator, providing relative stability. Ensure adequate working length and screw distribution.
- Intramedullary Nailing: Offers load-sharing benefits and is a preferred option for diaphyseal and many metaphyseal fractures (e.g., proximal femur). Requires careful reaming and interlocking to prevent loss of reduction.
- Cement Augmentation: Injection of PMMA cement around screws or within the bone cavity (e.g., vertebroplasty, kyphoplasty, cement-augmented screws in proximal humerus or tibia) significantly enhances pull-out strength and stability.
- Polished vs. Rough Surfaces: For arthroplasty, consider cemented components, as ingrowth surfaces may not achieve adequate purchase in osteoporotic bone.
- Screw Selection and Technique: Use larger diameter screws where appropriate. Consider bicortical fixation whenever anatomically safe. Avoid over-drilling or over-tapping which can strip compromised bone. Low-profile implants and care to avoid hardware prominence are important, especially in superficial locations.
Illustrative Examples of Surgical Techniques for Common Osteoporotic Fractures
1. Proximal Femur Fractures (e.g., Intertrochanteric)
- Approach: Lateral approach (vastus ridge approach for IMN) or modified Hardinge approach.
- Internervous Plane: Varies by specific approach, often working between gluteus medius and vastus lateralis.
- Reduction: Closed reduction on a fracture table under fluoroscopy. Traction, internal/external rotation, and valgus/varus adjustments are critical to restore alignment. For unstable patterns, percutaneous clamps or K-wires may aid.
-
Fixation:
- Cephalomedullary Nailing: Most common and preferred. After closed reduction, ream femoral canal. Insert nail. Obtain proper screw position in femoral head (center-center or inferior-central on AP, central-central on lateral) for optimal biomechanics and cut-out resistance. Distal interlocking screws are crucial.
- Dynamic Hip Screw (DHS): For stable intertrochanteric patterns with an intact lateral wall. Requires meticulous placement of the lag screw in the femoral head. Augmentation with trochanteric stabilization plate may be considered.
2. Vertebral Compression Fractures (VCFs) - Kyphoplasty/Vertebroplasty
- Approach: Percutaneous, transpedicular approach.
- Internervous Plane: None, direct needle insertion.
- Reduction: For kyphoplasty, balloon inflation aims to create a cavity and restore vertebral height before cement injection. Vertebroplasty is purely for stabilization and pain relief.
-
Technique:
- Patient Positioning: Prone on a radiolucent table.
- Access: Unilateral or bilateral transpedicular approach under biplanar fluoroscopy. Incise skin, advance cannula/trocar into the vertebral body, confirming position.
- Kyphoplasty Specific: Insert balloon tamp through cannula. Inflate balloon to create a void and reduce kyphosis. Deflate and remove balloon.
- Cement Injection: Inject low-viscosity PMMA cement under continuous fluoroscopic visualization. Monitor for extravasation into spinal canal, neural foramen, or major vessels. Stop injection immediately if extravasation occurs.
- Removal: Remove cannula and close skin.
3. Distal Radius Fractures
- Approach: Volar approach (Henry approach) or dorsal approach. Volar is increasingly common due to better stability in osteoporotic bone.
- Internervous Plane: Volar approach between flexor carpi radialis and radial artery.
- Reduction: Often closed reduction under fluoroscopy with traction, then open reduction. Articular fragments are reduced first.
-
Fixation:
- Volar Locking Plate (VLP): Most common. Plate positioned volar to the watershed line. Distal locking screws capture articular fragments. Proximal screws provide diaphyseal fixation. Augmentation with cement or cancellous bone graft may be considered for severe comminution.
- Dorsal Plating: Less common but indicated for significant dorsal comminution or irreducible dorsal fragments. Higher risk of extensor tendon irritation.
- External Fixation: Can be used as a temporizing measure or as definitive fixation for highly comminuted open fractures. Often combined with K-wires.
4. Proximal Humerus Fractures
- Approach: Deltopectoral approach (most common) or deltoid-splitting approach (limited use for specific patterns).
- Internervous Plane: Deltopectoral: between deltoid (axillary nerve) and pectoralis major (medial and lateral pectoral nerves).
- Reduction: Gentle manipulation. Use sutures through rotator cuff tendons as "joysticks" to control head fragments.
-
Fixation:
- Locked Plating: Requires careful placement to avoid impingement. Multiple screws into the humeral head, often augmented with cement or cancellous bone graft. Evaluate screw length to avoid penetration of articular surface.
- Intramedullary Nailing: Less common for complex fractures but can be used for selected two-part surgical neck fractures.
- Arthroplasty (Hemiarthroplasty or Reverse Shoulder Arthroplasty): Indicated for highly comminuted 3- or 4-part fractures, head-split fractures, or fractures with significant head devascularization, especially in older, lower-demand patients. Cemented stem fixation is often preferred in osteoporotic bone.
Complications & Management
Osteoporotic fractures and their surgical management are associated with a distinct set of complications, often amplified by the patient's age and comorbidities. Proactive identification and management are crucial.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Salvage Strategies |
|---|---|---|
| Non-union/Malunion | 5-15% (variable by site/fracture type) | Revision ORIF with bone grafting (autograft/allograft), plate augmentation, re-nailing, specialized fixation (e.g., internal fixation with external fixator). For failed shoulder/hip, arthroplasty (hemi/reverse/THA). |
| Implant Failure/Cut-out | 2-10% (especially proximal femur, humerus) | Revision surgery (e.g., longer nail, thicker plate, cement augmentation, arthroplasty). |
| Infection (SSI) | 1-5% (superficial), 0.5-2% (deep) | Debridement, lavage, antibiotics. For deep infection, hardware removal, staged reconstruction. |
| Periprosthetic Fracture | 1-2% (after arthroplasty), 5-10% (around plates/nails) | Revision surgery, longer implant, cables, cerclage wires. Specific plating for stable fixation around existing hardware. |
| Avascular Necrosis (AVN) | 10-30% (femoral neck, humeral head) | Arthroplasty (hip: THA, shoulder: hemi/reverse). |
| DVT/Pulmonary Embolism | 10-20% (DVT, symptomatic 1-5%), 1-2% (PE) | Therapeutic anticoagulation. IVC filter for contraindication to anticoagulation or recurrent PE. |
| Delirium/Cognitive Decline | 15-50% (post-op, esp. hip #) | Medical management (hydration, pain control, early mobilization, reorientation), consult geriatrics. |
| Wound Dehiscence/Skin Necrosis | 5-10% | Local wound care, primary closure (if small), debridement, negative pressure wound therapy, flap reconstruction. |
| Pressure Ulcers | 5-15% (post-op) | Prevention through meticulous padding, turning protocols, early mobilization. Wound care, debridement. |
| Cardiovascular/Pulmonary | 5-10% | Optimization of medical comorbidities, close monitoring in ICU/step-down unit. |
General Management Principles for Complications
- Early Detection: Vigilant monitoring for signs of infection (fever, erythema, discharge), neurovascular compromise, or changes in cognitive status.
- Multidisciplinary Approach: Involve infectious disease specialists, internal medicine, geriatrics, pain management, and physical therapy.
- Revision Surgery: Requires careful planning, often involving specialized implants, bone grafting, and potentially more extensive approaches. The decision to revise must weigh the potential benefits against the risks in a frail patient.
- Medical Optimization: Address underlying systemic issues that contribute to complications (e.g., nutritional deficiencies, poor glycemic control, medication side effects).
- Prevention: The best management is prevention. This includes meticulous surgical technique, appropriate antibiotic and DVT prophylaxis, aggressive medical optimization, and early, appropriate rehabilitation.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation in patients with osteoporotic fractures is critical for restoring function, preventing secondary complications, and mitigating future fracture risk. Protocols must be tailored to the individual patient's pre-injury functional status, cognitive abilities, and the specific fracture type and fixation stability. The primary goals are early mobilization, pain control, and progressive strengthening and balance training.
General Principles
- Early Mobilization: As soon as surgically and medically safe, patients should be mobilized. This prevents complications such as DVT/PE, pneumonia, muscle atrophy, joint contractures, and pressure ulcers. For most surgically treated osteoporotic fractures, weight-bearing status or range of motion restrictions are guided by implant stability.
- Pain Management: Comprehensive, multimodal pain control is essential to facilitate participation in therapy. This includes opioids, NSAIDs (if not contraindicated), acetaminophen, regional blocks, and adjunctive medications.
- Risk Factor Modification: Address fall risk factors (environmental hazards, polypharmacy, visual impairment, orthostatic hypotension, sarcopenia).
- Nutritional Support: Ensure adequate protein, calcium, and vitamin D intake to support bone healing and overall recovery.
- Bone Health Management: Initiate or continue pharmacotherapy for osteoporosis (e.g., bisphosphonates, denosumab, teriparatide) under the guidance of an endocrinologist or primary care physician. Fracture liaison services (FLS) are highly effective in ensuring secondary fracture prevention.
Site-Specific Rehabilitation Considerations
1. Proximal Femur Fractures (Hip)
- Weight-Bearing (WB): Typically early weight-bearing (WBAT - weight-bearing as tolerated) for stable IMN or arthroplasty. For less stable fixation, protected WB (PWB) or touch-down WB (TDWB) may be required initially.
-
Phase 1 (Acute - Inpatient):
- Pain management, DVT prophylaxis.
- Bed mobility, transfers (bed to chair), short distance ambulation with assistive device (walker).
- Gentle range of motion (ROM) exercises for hip and knee, ankle pumps.
- Education on hip precautions if arthroplasty performed (e.g., no extreme flexion, adduction, internal rotation for posterior approach).
-
Phase 2 (Subacute - Skilled Nursing/Home):
- Progressive ambulation, stair training.
- Strengthening exercises for hip abductors, extensors, quadriceps (e.g., straight leg raises, hip abduction with resistance).
- Balance training, proprioceptive exercises.
- Occupational therapy for ADL retraining.
-
Phase 3 (Community/Home):
- Advanced strengthening, endurance training.
- Return to prior leisure activities, fall prevention programs.
2. Vertebral Compression Fractures (VCFs)
-
Post-Vertebroplasty/Kyphoplasty:
Immediate pain relief often allows rapid mobilization.
- Activity: Progressive ambulation as tolerated. Avoid heavy lifting and twisting for 6-8 weeks.
- Bracing: Typically not required after successful vertebroplasty/kyphoplasty. May be used for unstable non-operative VCFs.
- Therapy: Focus on core strengthening, postural re-education, and gentle extension exercises to counteract kyphosis. Avoid flexion exercises initially.
- Non-Operative VCFs: Gradual increase in activity as pain allows. Bracing (TLSO) may be used for symptom relief and to prevent further collapse.
3. Distal Radius Fractures
- Immobilization: If surgically fixed with a stable construct, often no immobilization beyond a short splint (e.g., sugar tong) for comfort for 1-2 weeks.
-
Phase 1 (Early - 0-2 weeks):
- Pain control, edema management (elevation, gentle massage).
- Full ROM for shoulder and elbow. Gentle finger ROM.
- Protected wrist ROM (e.g., dart-throwers motion) if stable fixation.
-
Phase 2 (Intermediate - 2-6 weeks):
- Active and passive ROM for wrist (flexion, extension, pronation, supination).
- Gentle grip strengthening.
- Scar massage.
-
Phase 3 (Advanced - 6+ weeks):
- Progressive strengthening with resistance bands, weights.
- Functional activities, return to sports.
4. Proximal Humerus Fractures
- Immobilization: Sling for comfort, typically 4-6 weeks, with careful removal for exercises.
-
Phase 1 (Early - 0-4 weeks):
- Pain management.
- Elbow, wrist, hand ROM and strengthening.
- Pendulum exercises, passive external rotation to tolerance. Avoid active shoulder elevation.
- For arthroplasty, specific precautions (e.g., no active internal rotation for reverse TSA).
-
Phase 2 (Intermediate - 4-12 weeks):
- Initiate active-assisted ROM (AA/ROM) for shoulder elevation, abduction, rotation.
- Gentle isometric strengthening.
-
Phase 3 (Advanced - 12+ weeks):
- Progressive strengthening for rotator cuff and deltoid.
- Return to functional activities, overhead work.
Summary of Key Literature / Guidelines
The management of osteoporotic fractures is continuously evolving, driven by clinical research and the development of new technologies. Several key organizations publish guidelines that inform evidence-based practice.
Key Guidelines and Recommendations:
-
American Academy of Orthopaedic Surgeons (AAOS):
- Management of Hip Fractures in Older Adults: Guidelines emphasize early surgery (within 48 hours), use of regional anesthesia, early mobilization, multidisciplinary care, and post-operative pharmacological intervention for osteoporosis. Specifically, intramedullary nailing is generally recommended over sliding hip screw for unstable intertrochanteric fractures, and arthroplasty (hemi or total) over internal fixation for displaced femoral neck fractures in active older adults.
- Management of Distal Radius Fractures: Guidelines support surgical fixation for displaced intra-articular fractures and unstable extra-articular fractures to restore anatomy and improve function, with volar locking plates being a common choice.
-
National Osteoporosis Foundation (NOF):
- Clinician's Guide to Prevention and Treatment of Osteoporosis: While not surgical, this guide provides the foundation for identifying and managing osteoporosis, which is critical for secondary fracture prevention. It recommends calcium and vitamin D supplementation, lifestyle modifications, and pharmacotherapy (oral bisphosphonates as first-line for most) for patients with a fragility fracture or high fracture risk.
-
International Osteoporosis Foundation (IOF) / European Federation of National Associations of Orthopaedics and Traumatology (EFORT):
- Global Call to Action: Both organizations advocate for systematic Fracture Liaison Services (FLS) to identify, investigate, and initiate treatment for patients presenting with fragility fractures, aiming to reduce the risk of subsequent fractures.
-
Spine and Vertebral Fractures:
- For painful, stable VCFs unresponsive to conservative management, vertebroplasty or kyphoplasty can be considered for pain relief, though evidence for consistent kyphosis correction with kyphoplasty remains debated. The decision to intervene surgically for VCFs should weigh potential benefits against risks of cement extravasation and adjacent level fractures.
-
Proximal Humerus Fractures:
- Literature supports non-operative management for many 2-part fractures. For displaced 3- and 4-part fractures, surgical options include locking plate fixation, hemiarthroplasty, or reverse shoulder arthroplasty. The choice between ORIF and arthroplasty depends heavily on patient age, functional demands, bone quality, and fracture pattern severity. Reverse shoulder arthroplasty is gaining favor in older, lower-demand patients with comminuted fractures due to its more predictable outcomes and lower reoperation rates compared to ORIF or hemiarthroplasty in this population.
Evolving Concepts and Research Directions:
- Augmented Fixation: Ongoing research into various methods of screw and plate augmentation (e.g., calcium phosphate cements, bioactive materials) to improve construct stability in compromised bone.
- Biologic Enhancement: Exploration of growth factors and cell-based therapies to enhance bone healing in osteoporotic patients.
- Advanced Imaging: Development of quantitative CT (QCT) and finite element analysis (FEA) to better predict fracture risk and guide surgical planning.
- Patient-Specific Implants: 3D printing and custom implants are emerging for complex reconstructions.
- Role of Anti-osteoporotic Medications: Better understanding of the optimal timing of anti-osteoporotic medication initiation/continuation around surgery and their impact on bone healing. For instance, teriparatide may accelerate healing, while bisphosphonates might need a temporary hold in specific scenarios.
Orthopedic surgeons managing osteoporotic fractures must remain abreast of these developments, integrating both surgical expertise and comprehensive bone health management into their practice to achieve the best functional outcomes and prevent the devastating cascade of recurrent fragility fractures.
You Might Also Like