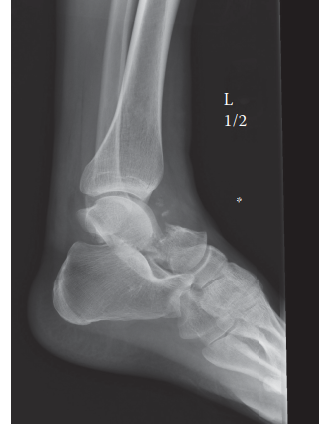
Reduction and Fixation of Anterior Tibial Margin and Complex Ankle Fractures
Key Takeaway
Anterior tibial margin fractures require meticulous articular reduction and stable fixation to prevent post-traumatic arthritis. This guide details the anterolateral surgical approach, fixation strategies for comminuted fragments, and the management of complex variants, including open fractures and diabetic neuropathic ankles. Emphasizing rigid internal fixation, spanning external fixation, and soft tissue management, these evidence-based protocols optimize outcomes in high-risk patients with unstable ankle fracture-dislocations.
INTRODUCTION TO ANTERIOR TIBIAL MARGIN FRACTURES
Anterior tibial margin fractures represent a complex subset of ankle trauma, frequently occurring as a component of high-energy pilon fractures or severe rotational ankle fracture-dislocations. The anterior tibial margin (often involving the Chaput tubercle or a larger anterior plafond segment) plays a critical biomechanical role in preventing anterior subluxation of the talus. Failure to anatomically reduce and rigidly fix these fragments inevitably leads to altered tibiotalar contact mechanics, accelerated articular wear, and debilitating post-traumatic osteoarthritis.
The management of these injuries is frequently complicated by patient-specific comorbidities, most notably diabetes mellitus with peripheral neuropathy, and the presence of open soft-tissue envelopes. This comprehensive guide details the operative techniques for isolated anterior margin fractures, while expanding upon the evidence-based management of open ankle fractures and the highly challenging diabetic ankle.
SURGICAL ANATOMY AND PREOPERATIVE PLANNING
Successful reduction of the anterior tibial margin requires an intimate understanding of the anterior ankle anatomy. The anterior tibial plafond is bordered laterally by the distal tibiofibular syndesmosis and medially by the medial malleolus. The primary restraint to anterior talar translation is the congruity of the osseous mortise, supplemented by the anterior joint capsule and the anterior talofibular ligament (ATFL).
Preoperative planning must include orthogonal plain radiographs and a fine-cut computed tomography (CT) scan with 3D reconstructions. CT imaging is mandatory to delineate the size of the anterior fragment, the degree of articular comminution, the presence of central die-punch impaction, and the trajectory of fracture lines, which dictate plate placement and screw vectors.
💡 Clinical Pearl: The "Die-Punch" Fragment
Always scrutinize the preoperative CT for a central articular "die-punch" fragment hidden behind the primary anterior margin piece. Failure to elevate and bone-graft this impacted segment will result in a residual articular step-off, leading to rapid joint degeneration.
SURGICAL TECHNIQUE: REDUCTION AND FIXATION OF ANTERIOR TIBIAL MARGIN FRACTURES
The following protocol outlines the standard anterolateral approach and fixation strategy for anterior tibial margin fractures.
1. Patient Positioning and Setup
- Position: Place the patient supine on a radiolucent operating table. A bump may be placed under the ipsilateral hip to internally rotate the leg to a neutral position, facilitating access to the anterolateral ankle.
- Tourniquet: Apply a well-padded thigh or proximal calf tourniquet.
- Fluoroscopy: Position the C-arm on the contralateral side of the table to allow for unhindered anteroposterior (AP), mortise, and lateral imaging.
2. The Anterolateral Surgical Approach
- Incision: Make a longitudinal anterolateral incision approximately 7.5 to 10 cm in length, centered over the anterior joint line, just lateral to the crest of the tibia.
- Superficial Dissection: Carefully incise the skin and subcutaneous tissues. Identify and protect the branches of the superficial peroneal nerve, which frequently cross the surgical field in the distal third of the incision.
- Deep Dissection: Incise the extensor retinaculum. Identify the interval between the extensor digitorum longus (EDL) and the extensor hallucis longus (EHL).
- Exposure: Retract the extensor tendons, the anterior tibial artery, and the deep peroneal nerve medially. Continue the deep dissection until the entire anterior surface of the ankle joint capsule is exposed. Perform a longitudinal capsulotomy to visualize the articular surface.
3. Joint Preparation and Debridement
- Hematoma Evacuation: Irrigate the joint copiously to remove fracture hematoma.
- Fragment Management: Meticulously remove small, devitalized, and loose osteochondral fragments that cannot be incorporated into the fixation construct. It is paramount to preserve as much of the intact articular surface as possible.
- Inspection: Inspect the talar dome for concomitant osteochondral lesions, which are common in high-energy fracture-dislocations.
4. Articular Reduction
- Talar Reduction: Reduce any anterior subluxation of the talus. This restores the anatomical template against which the anterior tibial margin can be reduced.
- Fragment Apposition: Appose the large anterior triangular fragment to the intact shaft of the tibia in its anatomical position. Use a dental pick or a small periosteal elevator to manipulate the fragment.
- Provisional Fixation: Secure the reduction temporarily with 1.25 mm or 1.6 mm Kirschner wires (K-wires). Verify the articular reduction fluoroscopically and, if possible, under direct visualization.
5. Definitive Fixation Strategies
The choice of fixation depends entirely on the size and comminution of the anterior fragment.
- Large, Non-Comminuted Fragments: Transfix the fragment with one or two 3.5 mm or 4.0 mm partially threaded cancellous lag screws directed from anterior to posterior. Ensure the screw heads are countersunk to prevent anterior soft-tissue irritation.
- Small Fragments: If the fragment is too small to accept a screw without shattering, utilize multiple threaded K-wires or bioabsorbable pins.
- Comminuted Fragments: If the anterior margin is comminuted, lag screw fixation alone is insufficient and will lead to secondary displacement. In these cases, apply a low-profile, small fragment buttress plate (e.g., a 2.7 mm or 3.5 mm T-plate or a pre-contoured anatomic anterior pilon plate).
- Articular Depression: If there is a depressed articular segment, elevate it through the fracture window. Support the elevated subchondral bone with cancellous autograft, allograft, or a synthetic bone substitute before applying the buttress plate.
🚨 Surgical Warning: Soft Tissue Tension
The anterior ankle has a notoriously thin soft-tissue envelope. When utilizing buttress plates, ensure the hardware is strictly low-profile. Excessive hardware prominence can lead to wound dehiscence, extensor tendon attrition, and deep infection.
MANAGEMENT OF ANKLE FRACTURES IN DIABETIC PATIENTS
Ankle fractures in patients with diabetes mellitus—particularly those with peripheral neuropathy and autonomic dysfunction—represent one of the most formidable challenges in orthopedic traumatology. The literature consistently demonstrates that patient age, fracture type, and diabetic status profoundly affect outcomes.
Complication Rates and Risk Factors
Diabetic patients experience significantly higher rates of mortality, prolonged hospital stays, and elevated total hospital charges following operatively treated ankle fractures.
* Vascular Compromise: Approximately 83% of diabetic patients with absent pedal pulses develop severe postoperative complications.
* Neuropathy: An astounding 92% of patients with preoperative dense peripheral neuropathy develop complications, including wound breakdown, deep infection, hardware failure, and Charcot neuroarthropathy.
Augmented Fixation Strategies
While standard fixation techniques may be employed in well-controlled diabetics with normal sensation, patients deemed at high risk for fixation failure require a paradigm shift in surgical strategy. The goal is to achieve ultra-rigid fixation that can withstand the repetitive, unperceived microtrauma characteristic of the neuropathic patient.
Modified fixation strategies include:
1. Bicortical Medial Malleolar Fixation: Abandon standard unicortical cancellous screws. Utilize fully threaded cortical screws that engage the lateral tibial cortex to maximize pull-out strength.
2. Enhanced Syndesmotic Fixation: Place multiple (three or four) quadricortical transfibular or transtibial syndesmotic position screws. These are often left in place permanently to prevent late syndesmotic diastasis.
3. Locking Plate Technology: Utilize anatomically contoured locking plates for the fibula and tibia to create a fixed-angle construct, which is biomechanically superior in osteoporotic diabetic bone.
4. Tibiotalar Transfixion: In extreme cases of neuropathy, retrograde trans-calcaneal Steinmann pins or a spanning external fixator may be used to temporarily neutralize the ankle joint and protect the internal hardware.
Salvage and Primary Arthrodesis
In diabetic patients presenting with unstable bimalleolar ankle fractures complicated by pre-existing or acute Charcot arthropathy, standard open reduction and internal fixation (ORIF) frequently fails.
Ayoub's landmark research on tibiotalar arthrodesis in 17 diabetic patients with unstable fractures and Charcot arthropathy highlighted the efficacy of primary fusion.
* Optimal Timing: Results were significantly better when surgery was performed within 3 to 6 months of onset.
* Patient Selection: Favorable outcomes correlated with the absence of dense peripheral neuropathy and satisfactory extremity oxygenation.
* Amputation Risk: Despite aggressive management, amputation was ultimately required in 17.6% of these high-risk patients, underscoring the severity of the disease process.
MANAGEMENT OF OPEN ANKLE FRACTURES
Open ankle fractures are high-energy injuries that demand emergent surgical intervention. Interestingly, open ankle fractures caused by indirect rotational injury are two to four times more likely to present with medial wounds than lateral wounds. This occurs as the talus forcefully extrudes medially, tearing through the medial soft tissues following a lateral-sided failure.
Surgical Timing and Debridement
Historically, open fractures were managed with delayed fixation or immediate provisional fixation with K-wires. However, contemporary evidence strongly supports the advantages of primary internal fixation for open ankle fractures, including severe Gustilo-Anderson Type III wounds. Immediate internal fixation, performed concurrently with meticulous surgical debridement, provides skeletal stability, which is the foundation of soft-tissue healing and infection prevention.
💡 Clinical Pearl: The "Vacuum Effect" at the Syndesmosis
Ngcelwane made a critical observation regarding medial open wounds: dirt, grass, and debris are frequently found lodged deep within the lateral syndesmosis. This occurs due to a "vacuum effect" created during the transient dislocation of the ankle, which sucks contaminants from the medial wound across the joint space into the lateral compartment.
Surgical Implication: For displaced Danis-Weber Type B and C fractures with medial open wounds (especially those showing gas shadows on radiographs), a formal lateral incision is highly recommended to facilitate cross-irrigation and ensure complete decontamination of the syndesmosis.
Fixation Protocols for Contaminated Wounds
- Clean Wounds: Following thorough debridement (typically 6 to 9 liters of normal saline), immediate ORIF is preferred.
- Severely Contaminated Wounds: If the wound remains severely contaminated or if the soft-tissue envelope is crushed and non-viable, internal fixation should be deferred. Instead, apply a temporary spanning external fixator (e.g., a Delta frame utilizing tibial shaft pins and a trans-calcaneal pin). Open reduction is performed sequentially once the wound is judged to be clean, soft-tissue swelling has subsided, and the "wrinkle sign" is present.
- Supplemental External Fixation: In addition to internal fixation, a temporary external fixator that spans the ankle joint can be utilized to neutralize forces, protect the soft-tissue repair, and facilitate complex wound care (e.g., negative pressure wound therapy or flap coverage). The fixator is removed once soft-tissue healing is complete.
Prognosis and Outcomes in Open Fractures
The prognosis for open ankle fractures is guarded compared to closed injuries.
* Return to Function: While Wiss et al. noted that approximately 80% of patients can expect to return to work after fracture union, only a dismal 18% return to their pre-injury recreational or athletic levels.
* Infection Rates: The rate of deep infection in open ankle fractures hovers around 5% in the general population.
* Diabetic Open Fractures: Open ankle fracture-dislocations in diabetic patients—especially those with neuropathy—are exceptionally problematic. These injuries frequently progress to deep infection, catastrophic hardware failure, and ultimately, amputation. Supplemental external fixation is strongly advisable in this demographic to provide maximum stability.
UNSTABLE ANKLE FRACTURE-DISLOCATIONS AND SOFT TISSUE COMPROMISE
In certain clinical scenarios, standard operative treatment of an unstable ankle fracture-dislocation is rendered inadvisable due to severe local soft-tissue compromise. This situation most frequently arises when there is a deep abrasion, fracture blisters, or a superficial infection directly overlying the planned surgical incision sites.
Alternative and Salvage Techniques
When the soft-tissue envelope precludes standard incisions, the surgeon must rely on alternative methods to maintain joint reduction and prevent skin necrosis from a subluxated talus.
- The Childress Method: Historically, Childress described a method utilizing trans-calcaneal skeletal traction or percutaneous pinning to maintain length and alignment when open surgery was contraindicated.
- Modern Spanning External Fixation: Today, the modern equivalent of the Childress concept is the application of a joint-spanning external fixator. By placing pins well outside the zone of injury (proximal tibia and calcaneus/midfoot), the surgeon can achieve ligamentotaxis, restore length, and hold the talus reduced beneath the tibial plafond without violating the compromised soft tissues. Once the abrasions heal or the superficial infection clears, the external fixator can be removed, and definitive ORIF can be safely performed.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol for anterior tibial margin fractures and complex ankle injuries must be tailored to the stability of the fixation and the patient's comorbidities.
Standard Protocol (Healthy Patients)
- Immobilization: The limb is placed in a well-padded posterior splint with the ankle in neutral dorsiflexion immediately postoperatively.
- Wound Check: At 10 to 14 days, the splint is removed, wounds are inspected, and sutures are removed. The patient is transitioned to a controlled ankle motion (CAM) boot or a short-leg cast.
- Weight-Bearing: The patient remains strictly non-weight-bearing (NWB) for 6 weeks.
- Rehabilitation: Early active range of motion (ROM) exercises are initiated at 2 to 4 weeks if the fixation is rigid and the wound is healed. Progressive weight-bearing begins at 6 weeks, guided by radiographic evidence of callus formation.
Modified Protocol (Diabetic and High-Risk Patients)
- Prolonged Immobilization: Diabetic patients require a total contact cast (TCC) or a locked CAM boot for an extended period.
- Extended Non-Weight-Bearing: The NWB period is routinely doubled to 10 to 12 weeks to prevent hardware failure and Charcot collapse.
- Vigilant Monitoring: Frequent clinical and radiographic follow-up is mandatory to detect early signs of infection, hardware loosening, or loss of reduction. Transition to weight-bearing must be gradual and is often supported by custom orthoses or a Charcot Restraint Orthotic Walker (CROW) boot.
You Might Also Like