Mastering the Posterolateral Approach and External Fixation for Tibial Pilon Fractures
Key Takeaway
The posterolateral approach to tibial pilon fractures provides excellent visualization of the posterior malleolus and fibula while minimizing anterior soft tissue complications. When combined with spanning external fixation, this technique effectively manages high-energy intra-articular comminution. This guide details the step-by-step surgical technique, biomechanical principles of limited internal fixation, and evidence-based postoperative protocols to optimize clinical outcomes in complex distal tibia fractures.
INTRODUCTION TO HIGH-ENERGY PILON FRACTURES
High-energy tibial pilon fractures (AO/OTA Type 43) represent one of the most formidable challenges in orthopedic traumatology. Historically, traditional open reduction and internal fixation (ORIF) of these injuries through extensive anterior incisions resulted in catastrophic soft tissue complications, including wound dehiscence, deep infection, and osteomyelitis. In response to these unacceptable outcomes, modern treatment algorithms have shifted toward soft-tissue-respecting strategies.
The posterolateral approach to the distal tibia, often combined with spanning external fixation and limited internal fixation, has emerged as a highly effective technique. This approach allows for direct visualization and reduction of the posterior articular fragments (Volkmann’s fragment) and the fibula through a single incision, utilizing a robust soft tissue envelope that is typically less traumatized than the anterior soft tissues.
PREOPERATIVE EVALUATION AND IMAGING
Thorough preoperative planning is paramount. Initial evaluation requires standard anteroposterior (AP), lateral, and mortise radiographs of the ankle, as well as full-length tibia/fibula films to rule out proximal extension or syndesmotic injury.
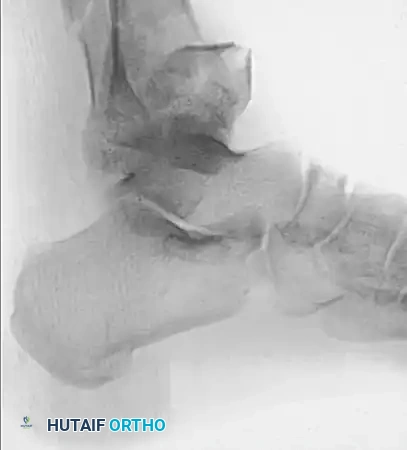
Figure 1: Anteroposterior (AP) radiograph demonstrating a severe, high-energy fracture-dislocation of the distal tibia and fibula.

Figure 2: Lateral radiograph of the same severe fracture-dislocation, highlighting the posterior displacement and articular comminution.
Following initial stabilization—typically with a temporary spanning external fixator—a fine-cut computed tomography (CT) scan with 2D and 3D reconstructions is mandatory. The CT scan delineates the fracture map, identifying the primary articular fragments: the anterolateral (Chaput), medial (medial malleolus), and posterior (Volkmann) fragments, alongside any central die-punch impaction.
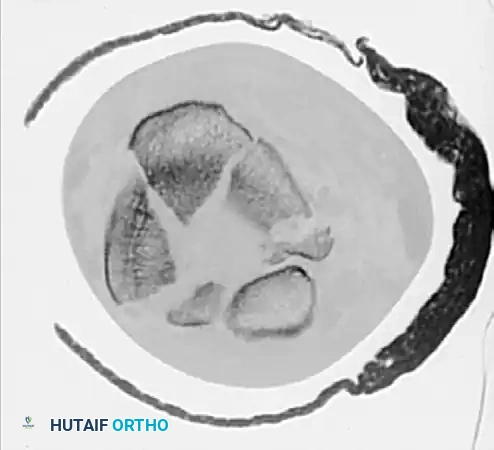
Figure 3: Axial CT scan slice clearly showing the complex fracture pattern, including severe articular comminution and displacement of the major plafond fragments.
Clinical Pearl: The posterior fragment is often the "keystone" of pilon fracture reduction. Anatomical restoration of the posterior plafond via a posterolateral approach provides a stable template against which the anterior and medial fragments can subsequently be reduced.
SURGICAL ANATOMY AND BIOMECHANICS
The posterolateral approach exploits the internervous plane between the peroneal tendons (superficial peroneal nerve) and the Achilles tendon/deep posterior compartment (tibial nerve).
Key anatomical considerations include:
* Sural Nerve and Lesser Saphenous Vein: These structures cross the surgical field from medial to lateral, typically lying just lateral to the Achilles tendon in the distal third of the leg. They must be meticulously identified and protected.
* Flexor Hallucis Longus (FHL): The FHL muscle belly serves as a critical anatomical landmark and a protective barrier. Retracting the FHL medially protects the posterior tibial artery and tibial nerve from iatrogenic injury during exposure of the posterior tibia.
* Posterior Malleolus: The posterior tibial plafond is accessed by elevating the deep fascia and periosteum off the posterior tibia, allowing direct visualization of the fracture lines.
STEP-BY-STEP SURGICAL TECHNIQUE: POSTEROLATERAL APPROACH
1. Anesthesia and Positioning
- Administer prophylactic intravenous antibiotics prior to tourniquet inflation.
- With the patient under general or regional anesthesia, remove any temporary external fixator that was previously placed for initial damage control.
- Position the patient prone on radiolucent chest rolls to facilitate ventilation and allow unobstructed fluoroscopic imaging.
- Pad all bony prominences. Exsanguinate the extremity and inflate the proximal thigh tourniquet to the appropriate pressure.
2. Incision and Superficial Dissection
- Make a longitudinal posterolateral incision midway between the posterior border of the fibula and the lateral border of the Achilles tendon.
- The incision typically begins 5 to 10 cm proximal to the ankle joint and extends distally toward the tip of the lateral malleolus. It can be extended proximally as dictated by the fracture pattern.
- Carefully dissect through the subcutaneous tissues. Identify, mobilize, and protect the sural nerve and the lesser saphenous vein. Retract them either medially or laterally depending on their anatomical course and the required exposure.
3. Deep Dissection and Joint Distraction
- Incise the superficial fascia of the leg.
- Identify the interval between the peroneal tendons laterally and the FHL medially.
- Retract the peroneal tendons laterally to expose the posterior border of the fibula.
- Retract the FHL medially. Do not dissect medial to the FHL, as this risks injury to the posterior tibial neurovascular bundle.
- If necessary to gain length, achieve ligamentotaxis, or visualize the impacted articular surface, apply a femoral distractor. Insert a 5.0-mm Schanz pin into the intact tibial diaphysis proximally and another into the posterior tuberosity of the calcaneus distally.
Surgical Warning: When applying distraction across the ankle joint, monitor the tension on the posterior neurovascular structures. Over-distraction can lead to tethering of the tibial nerve and subsequent tarsal tunnel syndrome or ischemic complications.
4. Fibular Plating
- If the fibula is fractured and its fixation is planned, address it through the lateral window of the same incision.
- Achieve anatomical reduction of the fibula to restore the lateral column length and rotation.
- Fix the fibula using a 3.5-mm one-third tubular plate or a precontoured distal fibula plate. In B-type injuries, an antiglide plating technique on the posterior border of the fibula is biomechanically advantageous and minimizes hardware prominence.
5. Articular Reduction and Tibial Fixation
- Elevate the periosteum off the posterior tibia to expose the fracture.
- Obtain articular reduction by direct manipulation of the posterior fracture fragments. Use a dental pick or Freer elevator to disimpact any central die-punch fragments.
- Confirm the articular reduction with multiplanar fluoroscopy.
- Fix the articular fragments provisionally with Kirschner wires, followed by definitive fixation using 3.5-mm cortical lag screws or 4.0-mm partially threaded cancellous screws.
- For the metaphyseal component, apply an appropriate plate. Severe C-type injuries typically require a robust 3.5-mm precontoured periarticular plate.
- Bone Grafting: For large metaphyseal voids created by the elevation of impacted articular segments, utilize autologous iliac crest bone graft or an appropriate osteoconductive bone graft substitute to provide structural support and prevent late subsidence.
6. Closure and Postoperative Care
- Deflate the tourniquet and achieve meticulous hemostasis.
- Insert a subfascial closed suction drain.
- Perform a layered closure, ensuring the deep fascia is not closed under tension to prevent compartment syndrome. Close the subcutaneous tissue and skin with non-absorbable sutures.
- Postoperative Protocol: The leg is placed in a bulky Jones splint and elevated strictly for 48 hours. The closed suction drain is typically removed at 24 to 48 hours. Early active and passive ankle range of motion is encouraged with physical therapy once the soft tissue envelope permits and sutures are removed (usually at 2 to 3 weeks). Weight-bearing is strictly deferred until 10 to 12 weeks postoperatively, contingent upon radiographic evidence of robust callus formation.
COMBINED EXTERNAL AND LIMITED INTERNAL FIXATION
In response to reports of unacceptable complication rates (up to 30-50% deep infection and wound necrosis) associated with traditional extensive plating of high-energy tibial pilon fractures, the paradigm has shifted. External fixation combined with limited internal fixation of the fibula and the tibial articular surface is now a widely advocated alternative.
This hybrid approach minimizes secondary surgical trauma to the already compromised soft tissue envelope. Studies comparing this technique to traditional extensive plating have demonstrated a significantly decreased incidence of deep infection. However, surgeons must remain vigilant, as pin-tract infections and delayed wound healing over the fibular incision can still occur in up to 20% of cases.
Long-Term Outcomes of Spanning External Fixation
In a landmark long-term follow-up study (5 to 12 years) by Marsh et al., 35 pilon fractures were treated with monolateral spanning external fixation. The radiographic reduction was rated as good in 14, fair in 15, and poor in six patients.
Interestingly, while osteoarthrosis developed in the majority of patients (grade 0 in three, grade 1 in six, grade 2 in 20, and grade 3 in six), the degree of arthrosis correlated with the initial severity of the injury and the quality of reduction, but did not strictly correlate with the final clinical result. Clinically, 15 patients rated their outcome as excellent, 10 as good, 7 as fair, and 1 as poor. Notably, despite acceptable functional scores, 27 of 31 patients were permanently unable to run, highlighting the life-altering nature of high-energy pilon fractures.
Similarly, Dickson et al. evaluated 37 high-energy pilon fractures (AO B3 and C3) treated with spanning external fixation followed by a staged open reduction of the articular surface at 10 to 21 days. They reported 81% good to excellent results. Complications included an 8% infection rate, 11% loss of reduction, 8% secondary arthrosis, and one amputation (3%) in a diabetic patient following a failed arthrodesis.
TECHNIQUES IN SPANNING EXTERNAL FIXATION
Traditional half-pin external fixation that spans the ankle joint offers the distinct advantage of requiring minimal soft tissue dissection. By leaving no large implants in a subcutaneous position, it theoretically reduces wound complications, making it the treatment of choice for open fractures or severe closed injuries (Tscherne Grade II/III).
Biomechanics and Application
Half-pins (typically 4.0-mm or 5.0-mm) are placed into the calcaneus and the talar neck distally, and connected via carbon fiber rods to half-pins in the intact tibial diaphysis proximally. The fracture is reduced via distraction and ligamentotaxis.
If the articular surface does not reduce anatomically via ligamentotaxis alone, limited open reduction is mandated. The articular surface is manipulated percutaneously under fluoroscopic guidance or through limited, strategically placed incisions directly over the fracture lines. The articular reduction is then secured with 3.5-mm or 4.0-mm independent lag screws.
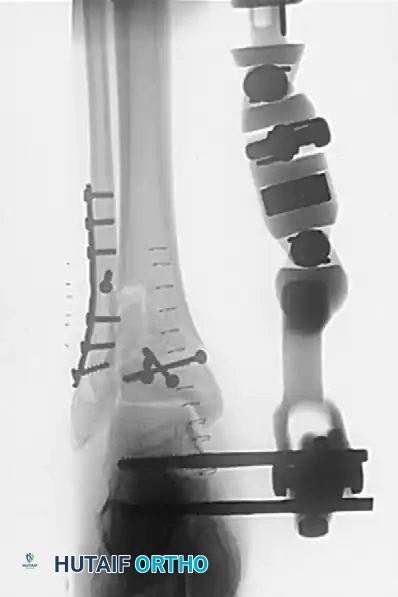
Figure 4: Postoperative AP radiograph demonstrating an articulated spanning external fixator, fibular plate, and independent tibial lag screws restoring the articular block.
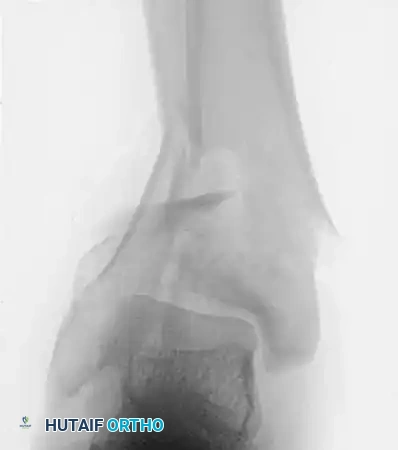
Figure 5: Postoperative lateral radiograph showing the restoration of the tibial plafond and the application of the external fixator frame.
Articulated vs. Rigid Fixation
The articulated half-pin fixator was developed with a hinge aligned to the true transmalleolar axis of the ankle joint. The theoretical advantage is that the hinge can be unlocked to allow early ankle motion, preventing capsular contracture and promoting cartilage nutrition.
However, clinical superiority remains debated. Marsh et al. compared 19 patients treated with rigid spanning fixation against 22 patients treated with an articulated fixator allowing early motion (within 2 weeks). They found no statistically significant differences between the groups regarding final range of motion, pain, or functional scores, though they cautioned that the sample size was small.
Surgical Pearl: When using a spanning external fixator as definitive treatment, bone grafting of metaphyseal defects is necessary in 25% to 60% of cases to prevent delayed union or varus collapse upon frame removal. This can be performed acutely if the soft tissue envelope is pristine, or delayed 4 to 6 weeks.
CONTROVERSIES: EXTERNAL FIXATION AND FIBULAR PLATING
While fibular plating is a cornerstone of the AO principles for ORIF of pilon fractures, its role is highly controversial when external fixation is utilized as the definitive treatment for the tibia.
Potential Advantages of Fibular Plating:
* Restores lateral column length and alignment.
* Assists in the indirect reduction of the anterolateral (Chaput) tibial fragment via the anterior inferior tibiofibular ligament (AITFL).
* Increases overall construct stability.
Potential Disadvantages of Fibular Plating:
* Requires additional incisions, increasing the risk of wound necrosis over the lateral malleolus.
* Restricts the ability of the external fixator to be dynamized.
* May lead to delayed tibial union or varus malunion if the tibial metaphyseal defect is not adequately bone grafted, as the rigid fibula holds the tibia in distraction.
Evidence-Based Perspectives
Williams et al. evaluated patients treated with spanning external fixation and concomitant fibular plating. They reported significant complications, including fibular wound infections (23%), fibular nonunions (9%), and angular malalignment (4.5%). Conversely, patients treated without fibular plating experienced angular malunions (19%) and tibial wound infections (3%). The authors concluded that good results can be obtained without fibular fixation, and avoiding it may spare the patient significant lateral wound complications.
Watson et al. analyzed 39 pilon fractures treated with external fixation that were considered "treatment failures." They discovered that 64% of these failures (malunion or nonunion at the diaphyseal-metaphyseal junction) occurred in fractures with plated or intact fibulas combined with unrecognized, un-grafted tibial bone loss. The rigid fibula prevented axial loading of the comminuted tibia.
Clinical Recommendation: There is no universal consensus on fibular fixation in the setting of definitive external fixation. The risks and benefits must be individualized. If a posterolateral approach is already being utilized to reduce a posterior tibial fragment, the fibula can be safely plated through the same incision. However, if a spanning frame is applied percutaneously, routine open plating of the fibula should be approached with caution, particularly in the presence of severe lateral soft tissue injury. In such cases, percutaneous intramedullary Kirschner wires or a simple syndesmotic screw may maintain fibular length without compromising the soft tissue envelope.
You Might Also Like
