Management of Ankle Fractures in Patients with Diabetes: A Comprehensive Surgical Guide
Key Takeaway
The management of ankle fractures in diabetic patients presents a profound orthopedic challenge due to compromised bone quality, peripheral neuropathy, and microvascular disease. While nonoperative treatment risks malunion and Charcot arthropathy, operative intervention carries a 43% complication rate. Successful outcomes demand meticulous soft-tissue handling, augmented rigid internal fixation—often utilizing multiple syndesmotic or trans-articular screws—and strictly prolonged postoperative immobilization to prevent catastrophic construct failure and neuroarthropathic collapse.
INTRODUCTION TO DIABETIC ANKLE FRACTURES
Although malleolar fractures are generally considered to be relatively benign injuries in the healthy, active population, their occurrence in patients with diabetes mellitus represents a limb-threatening pathology. The operative treatment of ankle fractures in diabetic patients is fraught with significant challenges and is associated with a markedly elevated complication profile. These patients are frequently older and present with a triad of systemic compromises: peripheral vascular disease, peripheral neuropathy, and compromised bone mineral density.
Historically, complication rates in the diabetic cohort have been reported to be as high as 43%, standing in stark contrast to the 15.5% complication rate observed in age-matched patients without diabetes. The spectrum of these complications is severe, encompassing deep and superficial surgical site infections, catastrophic loss of fixation, malunion, nonunion, wound necrosis, and ultimately, major lower extremity amputation.
Clinical Pearl: The "Diabetic Ankle" must never be treated as a standard ankle fracture. The presence of peripheral neuropathy fundamentally alters the biomechanical feedback loop, allowing patients to inadvertently overload and destroy standard fixation constructs.
Despite these risks, the paradigm of care requires a nuanced approach. While nonoperative treatment in diabetic patients has historically demonstrated a high frequency of loss of reduction and malunion, these patients are often minimally symptomatic due to their neuropathy. However, inadequate immobilization or unstable alignment can rapidly precipitate Charcot neuroarthropathy. Therefore, if surgical treatment of the ankle fracture is biomechanically indicated, it should not be delayed or avoided simply because the patient carries a diagnosis of diabetes.
PREOPERATIVE EVALUATION AND EVIDENCE-BASED RISK STRATIFICATION
The decision-making process for a diabetic ankle fracture hinges on a meticulous preoperative evaluation of the host's physiological envelope.
Assessing the Diabetic Triad
- Neuropathy: The loss of protective sensation (LOPS) must be documented using a 5.07 Semmes-Weinstein monofilament. Neuropathic patients lack the pain response necessary to protect a healing fracture or a surgical construct, necessitating augmented fixation and prolonged immobilization.
- Angiopathy: Microvascular and macrovascular disease impair wound healing and immune response. Palpable pulses do not rule out microvascular ischemia. Non-invasive vascular studies, including Ankle-Brachial Indices (ABI) and Transcutaneous Oxygen Measurements (TcPO2), should be considered if vascular compromise is suspected. A TcPO2 > 30-40 mmHg is generally required for adequate wound healing.
- Osteopenia/Osteoporosis: Advanced glycation end-products (AGEs) alter collagen cross-linking in diabetic bone, rendering it brittle and prone to hardware pull-out.
Literature Context and Complication Rates
Recent literature provides a more stratified view of operative risks in the diabetic population. A pivotal study by Guo et al. compared patients with preoperatively neglected type 2 diabetes against a nondiabetic matched cohort. They found no significant increase in postoperative infection rates following the immediate operative stabilization of closed ankle fractures, provided the soft tissue envelope was respected.
Similarly, Jones et al. demonstrated that operatively treated ankle fractures in diabetic patients without end-organ comorbidities had complication rates comparable to nondiabetic patients. However, the presence of diabetic comorbidities—and in particular, a history of Charcot arthropathy—exponentially increased the likelihood of postoperative failure.
In a large series analyzing high-risk cohorts, Costigan et al. reported on 84 patients who underwent Open Reduction and Internal Fixation (ORIF) for acute closed ankle fractures. They identified open fractures, insulin dependence, and peripheral neuropathy as the primary independent risk factors for construct failure and deep infection.
INDICATIONS FOR TREATMENT MODALITIES
Nonoperative Management
Nonoperative treatment is generally reserved for specific clinical scenarios:
* Patient Profile: Older diabetic patients with exceptionally low functional demands or those with prohibitive medical comorbidities precluding anesthesia.
* Fracture Pattern: Nondisplaced or minimally displaced fractures with a demonstrably stable configuration.
* Protocol: Closed management requires prolonged casting (often utilizing a total contact cast principle) and mandates exceptionally close clinical and radiographic supervision.
* Warning: Inadequate immobilization in the nonoperative setting may lead to rapidly developing Charcot neuropathy. Even minor displacements can alter joint contact pressures, initiating the neuroarthropathic cascade.
Operative Management
If the fracture is displaced, and either considerable manipulation is necessary to reduce it or molding is required to maintain the reduction, an open approach with internal fixation is strictly recommended.
Surgical Warning: Do not allow a displaced, unstable ankle fracture in a diabetic patient to remain unreduced under the guise of "avoiding surgery." The resulting soft tissue compromise from bony pressure, combined with the inevitable malunion and Charcot collapse, carries a higher amputation risk than a meticulously executed ORIF.
BIOMECHANICS AND PRINCIPLES OF DIABETIC FIXATION
Standard AO principles of internal fixation are often insufficient for the neuropathic diabetic ankle. The surgeon must employ the "Rule of Double": double the fixation density and double the duration of postoperative immobilization.
Maximizing Construct Rigidity
Because of the patient's poor bone quality and lack of protective pain sensation, the fixation construct must withstand supraphysiologic loads.
* Locking Plate Technology: Essential for osteoporotic bone to prevent screw toggle and pull-out.
* Augmented Syndesmotic Fixation: Standard single or double syndesmotic screws are prone to failure. Diabetic constructs often require multiple trans-syndesmotic or transfibular/transtibial screws that engage 3 to 4 cortices each, deliberately bypassing the standard dynamic syndesmotic principles in favor of absolute rigidity.
* Intramedullary Devices: Fibular nails or tibiotalocalcaneal (TTC) nails may be utilized to bypass poor soft tissue envelopes and provide load-sharing biomechanics.
SURGICAL APPROACHES AND STEP-BY-STEP TECHNIQUES
1. Standard ORIF with Augmentation
The primary goal is rigid stabilization with minimal soft tissue stripping.
Step 1: Soft Tissue Handling
Incision placement must respect the angiosomes of the foot and ankle. Full-thickness flaps are mandatory. "No-touch" techniques should be employed for the skin edges, utilizing self-retaining retractors minimally and avoiding excessive tension.
Step 2: Fibular Reduction and Fixation
The lateral malleolus is approached via a direct lateral or posterolateral incision. Following anatomic reduction, a locking plate is applied. In diabetic patients, the plate should ideally span a longer segment of the fibula to distribute stress.
Step 3: Medial Malleolar Fixation
Standard partially threaded cancellous screws may fail in diabetic osteoporotic bone. Consider using fully threaded screws, tension band wiring, or medial buttress plating to prevent catastrophic failure of the medial column.
Step 4: Construct Augmentation (The Transfibular/Transtibial Technique)
Consider the scenario of an elderly patient with osteoporosis, diabetes mellitus, and peripheral neuropathy who sustains an open comminuted bimalleolar ankle fracture-dislocation.
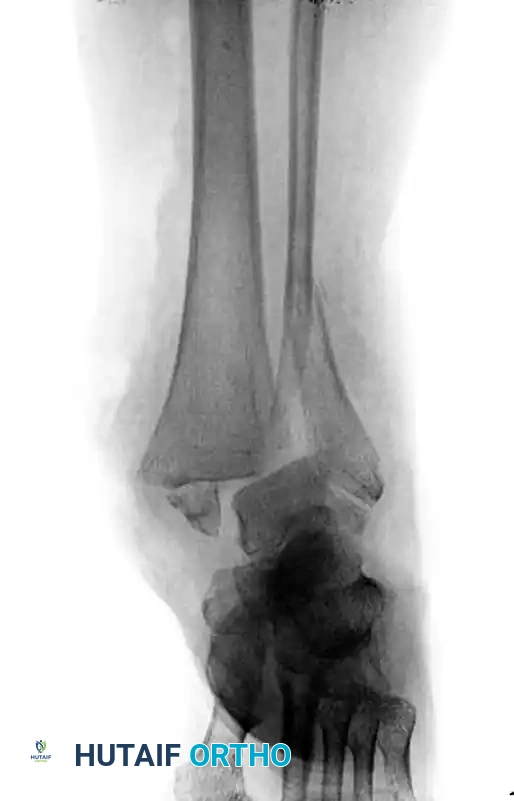
Preoperative radiograph demonstrating a highly unstable, comminuted bimalleolar fracture-dislocation in a neuropathic diabetic patient.
Following meticulous surgical débridement of the open wound, the fracture must be definitively treated with internal fixation. Because of the patient’s profoundly poor bone quality, standard fixation is inadequate. To achieve the necessary stability, the construct is augmented. Multiple transfibular/transtibial screws are utilized to significantly increase fixation purchase, locking the fibula to the tibia and effectively neutralizing the syndesmosis and the distal tibiofibular articulation.
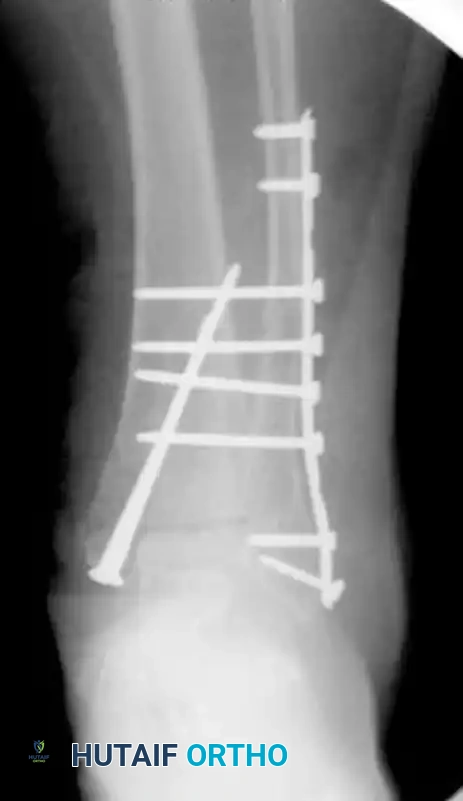
Postoperative radiograph illustrating definitive internal fixation. Note the use of multiple long transfibular/transtibial screws traversing the syndesmosis to maximize cortical purchase in osteoporotic bone.
2. Alternative and Salvage Stabilization Techniques
In scenarios where the soft tissue envelope is catastrophically compromised, or where existing hardware/bone loss precludes standard ORIF, alternative stabilization methods must be employed.
Tibiotalocalcaneal (TTC) Pinning (Historical and Salvage)
Historically, when open reduction was contraindicated, percutaneous techniques were utilized.
* The Childress Technique: Childress recommended this technique strictly as a last resort but found it useful in limb-salvage scenarios. The ankle is stabilized by a large Steinmann pin inserted longitudinally through the plantar aspect of the calcaneus, across the talus, and directly into the medullary canal of the tibia.
* The Laskin Technique: Under similar dire circumstances, Laskin advocated for closed reduction stabilized with a smooth Steinmann pin inserted transversely through the calcaneus, and a second pin inserted transversely through the proximal tibia. The pins are then incorporated into a rigid plaster cast, effectively creating a primitive circular frame construct.
Modern Percutaneous TTC Pinning Modifications
The use of a percutaneous tibiotalocalcaneal pin is today reserved for very rare instances in which existing hardware precludes external fixation placement, and absolute stability is necessary for soft tissue protection.
* Technique Modification: We have modified the traditional plantar-entry procedure so that the pin is directed to exit the anterior distal tibial metaphysis. This critical modification facilitates later extraction in the outpatient clinic or should the implant fail, avoiding the need to retrieve a migrated pin from the plantar fat pad.
External Fixation
Our preferred method of stabilization in the presence of severe soft tissue compromise (e.g., massive blistering, active infection, or open wounds precluding internal hardware) is the application of a uniplanar or circular external fixator.
* Forefoot Inclusion: It is imperative to include the forefoot in the frame construct if warranted. Neuropathic patients will rapidly develop an Achilles contracture. Pinning the forefoot prevents forefoot equinus posturing, which is vital should the frame become necessary for definitive, long-term management.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
Regardless of the method of treatment—whether nonoperative casting, augmented ORIF, or external fixation—prolonged immobilization is absolutely necessary to prevent the development of Charcot neuropathy and hardware failure.
Phase 1: Immediate Postoperative (Weeks 0-6)
- Immobilization: The patient is placed in a well-padded, rigid splint or bivalved cast.
- Weight-Bearing: Strict Non-Weight-Bearing (NWB) status is mandatory.
- Monitoring: Weekly or bi-weekly wound checks are required. Sutures are left in place longer than in non-diabetic patients (typically 3 to 4 weeks) to prevent wound dehiscence.
Phase 2: Intermediate Healing (Weeks 6-12)
- Immobilization: Transition to a total contact cast (TCC) or a locked Charcot Restraint Orthotic Walker (CROW) boot.
- Weight-Bearing: NWB status is generally maintained for a minimum of 8 to 12 weeks. Radiographic evidence of bridging callus must be definitively visualized before any weight-bearing is permitted. The standard 6-week radiographic healing timeline does not apply to the neuropathic diabetic patient.
Phase 3: Gradual Return to Function (Months 3-6)
- Weight-Bearing: Progressive weight-bearing is initiated exclusively within a CROW boot or a custom-molded ankle-foot orthosis (AFO).
- Surveillance: The patient must be monitored closely for signs of unilateral erythema, swelling, or warmth—the hallmark signs of an acute Charcot event. If these occur, the patient must immediately revert to strict NWB status and total contact casting.
COMPLICATIONS AND MANAGEMENT STRATEGIES
Surgical Site Infection and Wound Necrosis
Diabetic patients are at a high risk for marginal wound necrosis. If superficial necrosis occurs, it should be managed with local wound care and oral antibiotics. Deep infections involving hardware require aggressive surgical débridement. If the hardware is stable, it may be retained until union is achieved, utilizing suppressive intravenous antibiotics. If the hardware is loose, it must be removed, and the ankle stabilized with a spanning external fixator.
Loss of Fixation and Malunion
Neuropathic patients may walk on a fractured ankle despite instructions, leading to catastrophic hardware failure. Salvage typically requires revision ORIF with extended TTC nailing or heavy locking plates, supplemented with bone grafting.
Charcot Neuroarthropathy
The most devastating non-infectious complication is the postoperative development of Charcot arthropathy. This presents as a swollen, warm, erythematous foot with rapidly progressive joint subluxation and periarticular fragmentation. Immediate offloading is required. Definitive management often necessitates complex midfoot or hindfoot arthrodesis once the acute inflammatory phase has subsided.
Clinical Pearl: In the diabetic patient, a swollen, warm ankle postoperatively is Charcot neuroarthropathy or deep infection until proven otherwise. Never assume it is standard postoperative edema.
CONCLUSION
The management of ankle fractures in patients with diabetes requires a high index of suspicion for complications, a deep understanding of altered bone biomechanics, and a willingness to deviate from standard fixation principles. By employing augmented fixation strategies—such as multiple transfibular screws—respecting the fragile soft tissue envelope, and enforcing strictly prolonged postoperative immobilization, the orthopedic surgeon can successfully navigate these complex injuries, achieving stable union and preserving the patient's limb.
You Might Also Like
