Perioperative Management and Anesthesia in Foot and Ankle Surgery
Key Takeaway
Optimal perioperative management in foot and ankle surgery requires a meticulous approach to regional anesthesia, tourniquet application, and complication prophylaxis. This guide synthesizes evidence-based protocols for popliteal and ankle blocks, safe pneumatic tourniquet use, and preoperative skin preparation. By mastering these foundational principles, orthopedic surgeons can minimize postoperative pain, reduce surgical site infections, and mitigate thromboembolic risks, ultimately ensuring superior clinical outcomes in both ambulatory and inpatient settings.
Introduction to Perioperative Optimization in Foot and Ankle Surgery
The evolution of foot and ankle surgery has been profoundly shaped by advancements in perioperative management, particularly in the realms of regional anesthesia, hemostatic tourniquet control, and stringent infection prophylaxis. As the complexity of reconstructive procedures increases and the shift toward ambulatory surgery accelerates, the orthopedic surgeon must possess a masterful understanding of these foundational elements.
Drawing upon decades of foundational literature and evidence-based clinical trials, this comprehensive guide delineates the critical protocols required for optimizing patient outcomes. From the anatomical nuances of peripheral nerve blocks to the biomechanics of pneumatic tourniquets and the stratification of thromboembolic risks, this text serves as an authoritative resource for orthopedic residents, fellows, and practicing consultants.
Applied Surgical Anatomy and Topography
A profound comprehension of the descriptive and topographic anatomy of the foot and ankle is the bedrock of safe surgical intervention and effective regional anesthesia. The complex neurovascular arborization in this distal extremity demands meticulous attention to anatomical variations.
The Superficial Peroneal Nerve (SPN)
The superficial peroneal nerve is particularly vulnerable during anterolateral approaches to the ankle and hindfoot.
* Course and Penetration: The SPN typically pierces the crural fascia to become subcutaneous approximately 10 to 15 centimeters proximal to the tip of the lateral malleolus.
* Anatomical Variations: Classic anatomical studies (e.g., Adkinson et al.) have demonstrated significant variability in the course of the SPN. In a notable percentage of patients, the nerve may branch proximal to the ankle joint, or aberrant branches may cross directly over the surgical intervals used for fibular fracture fixation or lateral ligament reconstruction.
Surgical Warning: Always perform blunt subcutaneous dissection when utilizing the anterolateral approach to the ankle or the lateral approach to the fibula. The intermediate dorsal cutaneous branch of the SPN is highly variable and easily transected, leading to painful postoperative neuromas.
Topographic Zones of the Foot
Understanding the functional topography of the foot is essential for planning incisions that respect angiosomes and minimize wound healing complications. The dorsal skin is thin and pliable, accommodating significant edema but offering little protection to underlying tendons and nerves. Conversely, the plantar skin is highly specialized, tethered by robust fibrous septa to the plantar aponeurosis, designed to withstand immense shear and compressive forces.
Regional Anesthesia and Postoperative Analgesia
Regional anesthesia has revolutionized foot and ankle surgery, providing superior intraoperative conditions, profound postoperative analgesia, and facilitating early discharge in the ambulatory setting. The selection of the anesthetic modality depends on the surgical site, anticipated duration of surgery, and the patient's physiological status.
Popliteal Fossa Sciatic Nerve Block
The popliteal sciatic nerve block is the gold standard for major hindfoot, midfoot, and ankle reconstructions. By blocking the sciatic nerve proximal to its bifurcation into the tibial and common peroneal nerves, the surgeon achieves comprehensive anesthesia of the foot and ankle, sparing only the anteromedial skin innervated by the saphenous nerve.
- Indications: Arthrodesis (triple, subtalar, ankle), Achilles tendon repair, complex calcaneal or pilon fractures, and major forefoot reconstructions.
- Technique: Utilizing ultrasound guidance, the sciatic nerve is identified in the popliteal fossa. The injection of a long-acting local anesthetic (e.g., 0.5% Ropivacaine or 0.25% Bupivacaine) is delivered circumferentially around the nerve (the "donut sign") deep to the paraneural sheath.
- Continuous vs. Single-Shot: For highly painful procedures (e.g., Charcot reconstruction or extensive osteotomies), continuous popliteal sciatic nerve blocks via an indwelling catheter have been shown to significantly improve the quality of recovery, reducing opioid consumption and facilitating early rehabilitation.
Clinical Pearl: When performing a popliteal block as the sole anesthetic, remember to supplement with a saphenous nerve block (or a local field block at the medial malleolus) if the surgical incision extends to the medial aspect of the ankle or midfoot.
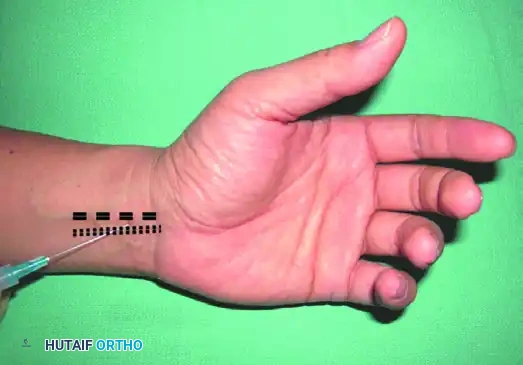
The Ankle Block
The ankle block is a highly reliable, low-risk technique ideal for forefoot and midfoot procedures. It involves the systematic blockade of the five terminal nerves supplying the foot.
Step-by-Step Execution:
1. Tibial Nerve: The primary nerve of the plantar aspect. Blocked posterior to the medial malleolus, deep to the flexor retinaculum, adjacent to the posterior tibial artery.
2. Deep Peroneal Nerve: Blocked at the anterior ankle joint line, between the tendons of the extensor hallucis longus (EHL) and extensor digitorum longus (EDL), lateral to the dorsalis pedis artery.
3. Superficial Peroneal Nerve: Blocked via a subcutaneous wheal extending from the anterior tibial crest to the lateral malleolus.
4. Sural Nerve: Blocked via a subcutaneous injection between the lateral malleolus and the Achilles tendon.
5. Saphenous Nerve: Blocked via a subcutaneous wheal anterior to the medial malleolus, adjacent to the great saphenous vein.
- Efficacy: Prospective analyses of large cohorts (e.g., 1,000+ patients) demonstrate success rates exceeding 95% when performed meticulously. It is exceptionally well-tolerated and avoids the motor blockade of the proximal leg musculature.
Intravenous Regional Anesthesia (IVRA / Bier Block)
IVRA is a viable alternative for short-duration (< 60 minutes) outpatient foot and ankle procedures, such as hardware removal or simple forefoot corrections.
- Mechanism: A double pneumatic tourniquet is applied to the calf. Following exsanguination, a local anesthetic (historically Prilocaine or Lidocaine) is injected intravenously, providing rapid onset anesthesia.
- Safety Protocols: Slow injection rates and high tourniquet inflation pressures are mandatory to prevent premature systemic release of the anesthetic, which could precipitate Local Anesthetic Systemic Toxicity (LAST).
Pitfall: IVRA provides zero postoperative analgesia once the tourniquet is deflated. The surgeon must perform a supplemental local infiltration block prior to wound closure to prevent severe rebound pain in the recovery room.
Tourniquet Application and Hemostasis
A bloodless surgical field is imperative in foot and ankle surgery to identify delicate neurovascular structures and ensure optimal integration of orthopedic implants. However, tourniquet use is not benign and requires strict adherence to safety parameters.
Pneumatic Ankle vs. Calf Tourniquets
The choice between an ankle and a calf tourniquet depends on the surgical exposure required and patient anatomy.
- Ankle Tourniquets: Highly effective for midfoot and forefoot operations (e.g., bunionectomies, Weil osteotomies). Placed just proximal to the malleoli, they require lower absolute inflation pressures due to the lack of bulky muscle mass. They are exceptionally well-tolerated under local anesthesia alone.
- Calf Tourniquets: Required for hindfoot and ankle procedures. They must be placed over the bulky gastrocnemius muscle. Clinical safety studies confirm their efficacy, though they are associated with higher rates of tourniquet pain, necessitating regional or general anesthesia.
Tourniquet Pressure and Time Parameters
- Pressure Settings: The modern standard is to base tourniquet pressure on the patient's Limb Occlusion Pressure (LOP) or systolic blood pressure. A common formula is Systolic BP + 100 mmHg for the lower extremity, typically resulting in pressures between 225 and 250 mmHg.
- Time Limits: Ischemic time should ideally not exceed 120 minutes. If surgery extends beyond this, the tourniquet should be deflated for 15-20 minutes to allow for reperfusion and clearance of acidic metabolites before reinflation.
The Esmark Bandage as a Tourniquet
For brief forefoot procedures, a tightly wrapped Esmark bandage applied from the toes to the supramalleolar region can serve as both an exsanguinator and a tourniquet. While cost-effective and efficient, the exact pressure applied is uncalibrated and can easily exceed 300 mmHg. Therefore, its use should be strictly limited to short-duration cases (< 45 minutes) to prevent neurapraxia.
Preoperative Skin Preparation and Infection Control
Surgical site infections (SSIs) in foot and ankle surgery can lead to catastrophic outcomes, including osteomyelitis and amputation. The unique microflora of the foot, particularly within the toe web spaces and nail folds, necessitates aggressive preoperative decontamination.
Optimal Skin Preparation Protocols
The foot harbors a high density of resident flora, including Staphylococcus epidermidis, Staphylococcus aureus, and various Gram-negative bacilli and fungi.
- Mechanical vs. Chemical Prep: Studies evaluating preoperative skin preparation of the foot and ankle have definitively shown that chemical application alone is insufficient. The use of bristles and alcohol-based solutions (e.g., Chlorhexidine gluconate in isopropyl alcohol) is significantly superior to standard iodine paints.
- The Scrubbing Technique: The surgeon or assistant must mechanically scrub the foot, paying particular attention to the interdigital web spaces and the periungual folds. Mechanical friction disrupts the biofilm and desquamates dead stratum corneum, allowing the bactericidal agent to penetrate effectively.
Clinical Pearl: Preprocedure toe cultures frequently yield polymicrobial growth. If operating near the nail beds (e.g., great toe fusion or terminal Syme amputation), consider a formal nail avulsion or aggressive mechanical debridement of the nail folds prior to the final sterile prep.
Thromboembolism (DVT) Prophylaxis
While the incidence of deep vein thrombosis (DVT) and pulmonary embolism (PE) following foot and ankle surgery is historically lower than that of major joint arthroplasty (hip/knee), it remains a critical medicolegal and clinical concern.
Incidence and Risk Stratification
Multicenter studies indicate that the overall incidence of symptomatic DVT in foot and ankle surgery is approximately 1% to 4%, depending on the procedure and immobilization protocol. However, asymptomatic DVT rates may be significantly higher.
High-Risk Factors Include:
* Achilles tendon ruptures (highest risk category in foot/ankle).
* Major hindfoot trauma (e.g., calcaneus or pilon fractures).
* Prolonged postoperative cast immobilization and non-weight-bearing status.
* Patient-specific factors: Obesity, prior history of VTE, oral contraceptive use, and known thrombophilias.
Prophylactic Strategies
The decision to initiate chemical prophylaxis must balance the risk of VTE against the risk of postoperative hematoma, which can compromise wound healing in the delicate soft tissue envelope of the foot.
- Mechanical Prophylaxis: Early mobilization and the use of sequential compression devices (SCDs) on the contralateral limb are universally recommended.
- Chemical Prophylaxis: For patients with elevated risk profiles or those undergoing major hindfoot reconstruction requiring prolonged non-weight-bearing, low-molecular-weight heparin (LMWH) or direct oral anticoagulants (DOACs) should be considered. Routine chemical prophylaxis for simple, ambulatory forefoot surgery in healthy patients is generally not indicated.
Postoperative Rehabilitation and Proprioceptive Considerations
The immediate postoperative phase requires a delicate balance between protecting the surgical repair, managing pain, and initiating rehabilitation.
The Effect of Anesthetic Blockade on Proprioception
Surgeons must be acutely aware of the biomechanical and proprioceptive deficits induced by regional anesthesia. Anesthetic blockade of the ankle not only eliminates nociception but also profoundly alters proprioception by blocking the afferent signals from ligamentous and capsular mechanoreceptors.
- Fall Risk: Patients discharged with an active popliteal or ankle block have a significantly diminished sense of joint position. This functional deafferentation drastically increases the risk of falls and inadvertent weight-bearing on a reconstructed limb.
- Mitigation: Strict non-weight-bearing instructions, mandatory use of crutches or a knee scooter, and the application of a rigid protective splint or cast are imperative until the block has completely resolved.
Conclusion
Mastery of foot and ankle surgery extends far beyond the execution of osteotomies and the placement of hardware. It demands a rigorous, evidence-based approach to the entire perioperative continuum. By integrating advanced regional anesthesia techniques, employing safe and effective tourniquet protocols, executing meticulous skin preparation, and stratifying thromboembolic risks, the orthopedic surgeon establishes the optimal environment for surgical success. Adherence to these textbook principles ensures not only the preservation of limb function but also the highest standards of patient safety and postoperative recovery.
You Might Also Like