Methods and Indications for Orthopedic Skin Closure
Key Takeaway
Soft tissue reconstruction in orthopedic surgery demands a systematic approach, progressing from primary closure to complex microvascular free flaps. Successful skin closure requires aggressive debridement, rigid skeletal stabilization, and meticulous handling of the soft tissue envelope. This guide details the indications, biomechanics, and surgical techniques for direct suturing, local and distant flaps, and the integration of advanced skin substitutes to optimize functional limb salvage.
INTRODUCTION TO SOFT TISSUE RECONSTRUCTION
The management of soft tissue defects in orthopedic trauma and reconstructive surgery is as critical as the management of the underlying osseous structures. The soft tissue envelope dictates the survival of bone, the healing of fractures, and the ultimate functional outcome of the extremity. A compromised soft tissue envelope can lead to deep infection, osteomyelitis, nonunion, and ultimately, amputation.
Orthopedic surgeons must possess a comprehensive understanding of the "reconstructive ladder"—a conceptual framework that begins with the simplest, least invasive method of closure (healing by secondary intention or direct suture) and progresses to highly complex procedures (microvascular free tissue transfer). Recently, this concept has evolved into the "reconstructive elevator," suggesting that the surgeon should bypass simpler steps if a more complex immediate reconstruction provides superior functional and aesthetic outcomes.
FUNDAMENTAL PRINCIPLES OF WOUND MANAGEMENT
Before any method of skin closure is attempted, the wound bed must be meticulously prepared. The initial management of severe extremity trauma dictates the success or failure of subsequent soft tissue coverage.
Clinical Pearl: The most common cause of flap failure or wound dehiscence in orthopedic trauma is inadequate initial debridement. The "zone of injury" often extends far beyond the visible wound margins.
Core Tenets of Acute Soft Tissue Reconstruction
- Prevention of Further Injury: The extremity must be splinted, and neurovascular structures protected immediately upon presentation to prevent secondary ischemic or mechanical damage.
- Aggressive Surgical Debridement: All necrotic, contaminated, and nonviable tissue—including devitalized bone, muscle, and fascia—must be radically excised. This process may require serial debridements over 48 to 72 hours.
- Rigid Skeletal Stabilization: Bone stability is the foundation of soft tissue reconstruction. Whether achieved via external fixation or internal osteosynthesis, a stable skeletal bed reduces dead space, minimizes ongoing soft tissue trauma, and promotes angiogenesis.
- Timely Acute Coverage: Coverage should ideally be achieved within the first 5 to 7 days post-injury, utilizing the simplest technique that reliably covers the wound and exposed vital structures (tendons, nerves, vessels, bone devoid of periosteum).
- Anticipation of Secondary Reconstructions: Future procedures (e.g., tendon transfers, bone grafting, tenolysis) must be considered during the primary soft tissue coverage. The chosen flap must allow for future surgical re-entry.
- Composite Tissue Considerations: When massive soft tissue loss occurs, composite reconstructions (e.g., osteocutaneous or myocutaneous flaps) should be considered early.
- Amputation vs. Salvage: In cases of insensate, severely crushed limbs with massive composite tissue loss, primary amputation may offer a superior functional outcome and lower morbidity than prolonged, multi-staged limb salvage attempts.
DIRECT SUTURE AND PRIMARY CLOSURE
Direct suturing remains the most fundamental method of skin closure. Unless the wound is severely contaminated, crushed, or under excessive tension, primary closure should be the first consideration for every wound.
Indications and Biomechanics
Primary closure is indicated for clean, sharply incised wounds with minimal tissue loss. The biomechanics of skin closure dictate that tension must be minimized across the wound edges to prevent microvascular ischemia, which leads to marginal necrosis and dehiscence.
Surgical Technique
- Undermining: Gentle undermining of the subdermal plexus can mobilize adjacent skin, reducing tension. However, in crush injuries, undermining is strictly contraindicated as it further devascularizes the already traumatized skin edges.
- Suture Selection: Deep dermal layers should be approximated with absorbable sutures (e.g., Polydioxanone or Polyglactin) to eliminate dead space and offload tension from the epidermal layer. The epidermis is then closed with non-absorbable monofilament sutures (e.g., Nylon or Prolene) to minimize tissue reactivity.
Surgical Warning: Never force a primary closure. If the skin edges blanch upon tying the suture, the tension is too high. Ischemic skin will inevitably necrose, converting a simple wound into a complex defect requiring flap coverage.
BIOMECHANICS AND VASCULARITY OF FLAPS
When direct suture is impossible due to tissue loss or excessive tension, flap coverage is required. Flaps are broadly categorized by their blood supply into random pattern flaps and axial pattern flaps.
Random Pattern Flaps
Random pattern flaps rely on the unnamed, diffuse musculocutaneous and subdermal vascular plexuses. Because they lack a primary, named artery and vein, their survival is strictly dependent on their geometry.
* Geometric Constraints: To ensure survival, the base of a random pattern flap must be as wide as its length. The length-to-width ratio should generally not exceed 1:1 in the lower extremity or 1.5:1 to 2:1 in the highly vascularized face and upper extremity.
Axial Pattern Flaps
Axial pattern flaps are supplied by a direct, named cutaneous artery and its accompanying venae comitantes running along the longitudinal axis of the flap.
* Geometric Advantages: Because of this robust, defined blood supply, the length-to-width ratio can safely exceed 3:1 (e.g., the groin pedicle flap based on the superficial circumflex iliac artery).
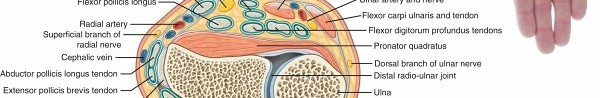
Anatomical Considerations: Dorsum vs. Palm
The anatomical location of a flap significantly impacts its viability, particularly in the hand. The vascular architecture and skin mobility differ drastically between the dorsal and volar surfaces.

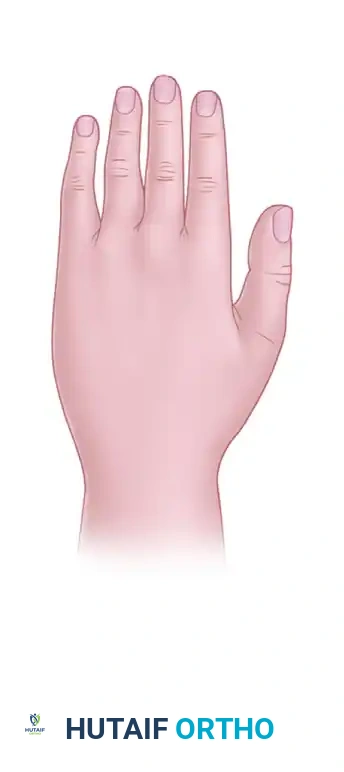
Figure A: Dorsum of the hand.
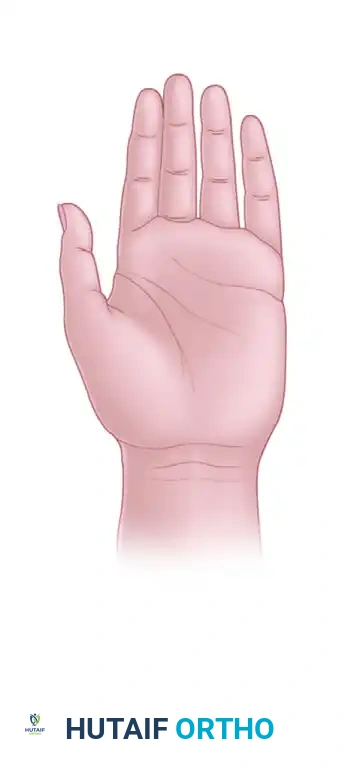
Figure B: Palm of the hand.
A distally attached, random pattern flap raised on the dorsum of the hand (Figure A) is significantly less likely to survive than a similarly designed flap on the palm (Figure B).
* Pathophysiology of Dorsal Flap Failure: The dorsal skin is highly mobile and relies on a delicate subdermal venous plexus. A distally based flap on the dorsum forces venous blood to drain against gravity and against the natural flow of the venous valves, leading to rapid venous congestion, thrombosis, and subsequent flap necrosis.
* Palmar Advantage: The palmar skin is tethered by robust fascial septa and possesses a dense, highly arborized vascular network that is more resilient to retrograde flow and shear forces.
REGIONAL AND LOCAL FLAP TECHNIQUES
Skin defects on the hand, palm, or dorsum that expose vital structures (tendons without paratenon, bone without periosteum, nerves, or joints) cannot be treated with split-thickness skin grafts. They require vascularized flap coverage.
The Cross-Finger Flap
The cross-finger flap is the workhorse for covering volar soft tissue defects of the digits, particularly those exposing the flexor tendon sheath.
- Indications: Volar defects of the middle or distal phalanges.
- Technique: The flap is raised from the dorsal surface of an adjacent, uninjured finger. It extends from the mid-lateral line of one side of the donor digit to the mid-lateral line of the other. The flap is designed to be slightly wider than the recipient defect to accommodate the hinge and prevent tension. The donor site on the dorsum of the finger is then covered with a full-thickness or thick split-thickness skin graft.
- Contraindications: The reverse cross-finger flap (raising a flap from the volar surface to cover a dorsal defect) is never indicated. Volar skin is highly specialized, glabrous, and essential for tactile sensation and pinch grip. Harvesting volar skin creates unacceptable donor site morbidity and severe flexion contractures.
The Filleted Finger Flap
In severe hand trauma where a digit is deemed unsalvageable (e.g., severe crush with irreversible neurovascular compromise and comminuted fractures), the skin of that digit can be utilized as a "spare part."
* Technique: The bone and tendinous structures are meticulously excised (filleted) from the amputated or unsalvageable digit, preserving the neurovascular bundles feeding the skin envelope. This creates an excellent, highly vascularized, and sensate pedicle graft to cover adjacent large defects on the palm or dorsum of the hand.
Local Rotation and Advancement Flaps
Local flaps utilize adjacent skin laxity to cover defects.
* Pitfalls in Trauma: While highly useful in elective tumor resections, local rotation flaps are notoriously unreliable in acute trauma. If the surrounding skin has been crushed or contused, the microvasculature is already compromised. Extensive undermining to mobilize a rotation flap in this setting will almost certainly result in ischemic necrosis of the flap margins.
DISTANT PEDICLE FLAPS
When local tissue is unavailable or severely traumatized, distant pedicle flaps are required. These flaps bring healthy, uninjured tissue from a remote site to the zone of injury.
Cross-Arm and Cross-Forearm Flaps
Historically used for large hand defects, these flaps involve suturing the injured hand to a flap raised on the contralateral arm.
* Disadvantages: The primary drawback is the requirement to immobilize both upper extremities together for 2 to 3 weeks while the flap revascularizes from the recipient bed. This leads to severe patient discomfort, loss of independence, and significant joint stiffness in both limbs. They have largely been superseded by axial and free flaps.
Arterialized Axial Flaps (Same Limb)
Utilizing an axial flap from the ipsilateral extremity (e.g., the radial forearm flap or posterior interosseous artery flap) provides robust coverage without tethering the patient to their contralateral limb. This allows for comfortable positioning and earlier mobilization of the uninvolved joints.
Abdominal and Groin Flaps
For massive defects of the hand and forearm, the injured limb can be temporarily buried under a pedicled flap raised on the abdomen or groin.
* The Groin Flap: Based on the superficial circumflex iliac artery, this is a classic axial pattern flap. Because of its axial blood supply, its length-to-width ratio can safely exceed 3:1.
* Management: The raw, undersurface of the pedicle that does not make contact with the recipient defect must be grafted with a split-thickness skin graft or tubed to prevent infection and exudative fluid loss. The flap is typically divided at 3 weeks once neovascularization from the recipient bed is confirmed.
MICROVASCULAR FREE TISSUE TRANSFER
In complex, high-energy trauma with massive composite tissue loss, local and distant pedicle flaps may be insufficient. Free tissue transfer utilizing microvascular anastomoses represents the pinnacle of the reconstructive ladder.
- Indications: Large defects exposing bone, joint, or hardware; cases requiring composite reconstruction (e.g., a fibula free flap for a segmental bone defect combined with a skin paddle); or when local tissue is entirely within the zone of injury.
- Technique: Tissue (muscle, fascia, or skin) is harvested from a distant donor site (e.g., Anterolateral Thigh, Latissimus Dorsi, or Gracilis) along with its primary artery and vein. The vessels are then anastomosed under a microscope to recipient vessels outside the zone of injury in the traumatized limb.
ADVANCED SKIN SUBSTITUTES AND BIOLOGICS
The advent of bioengineering has introduced "artificial skin" and dermal substitutes into the orthopedic armamentarium. These are particularly valuable for the initial coverage of severe hand wounds, extensive burns, and the release of severe burn contractures.
Bilayer Dermal Matrices
Products such as Integra® consist of a porous matrix of cross-linked bovine tendon collagen and glycosaminoglycans, covered by a temporary silicone epidermal substitute.
* Mechanism: The matrix acts as a scaffold for the ingrowth of fibroblasts and endothelial cells from the wound bed, generating a "neodermis." After 2 to 3 weeks, the silicone layer is removed, and an ultra-thin split-thickness skin graft is applied over the vascularized neodermis.
* Limitations: These products are not substitutes for adequate surgical debridement. They require a meticulously clean wound bed and will fail catastrophically in the presence of infection or necrotic tissue.
Biological Dressings: Allografts and Xenografts
- Allografts (Human Cadaveric Skin): Used as a temporary biological dressing. They provide excellent barrier function, reduce pain, and stimulate the development of a healthy capillary bed. However, because they contain foreign antigens, they will eventually undergo immunological rejection and must be replaced with an autograft.
- Xenografts (e.g., Porcine Skin): Serve a similar temporary function, acting as a biological bridge to definitive closure while the wound bed optimizes.
POSTOPERATIVE PROTOCOLS AND FLAP MONITORING
The success of any skin closure or flap technique relies heavily on meticulous postoperative care.
- Immobilization: The reconstructed area must be rigidly immobilized in a neutral, tension-free position. Splints should be well-padded to avoid external compression on the flap pedicle.
- Elevation: The extremity must be elevated above the level of the heart to promote venous drainage and minimize interstitial edema, which can compress the microvasculature.
- Flap Monitoring: Flaps must be monitored clinically every 1 to 2 hours for the first 48 hours.
- Arterial Insufficiency: Characterized by a pale, cool flap with sluggish or absent capillary refill.
- Venous Congestion: Characterized by a swollen, bluish/purple flap with brisk, almost instantaneous capillary refill and dark bleeding when pricked. Venous congestion is the most common cause of flap failure and requires immediate surgical re-exploration.
-
Rehabilitation: Once flap integration is secure (typically 2 to 3 weeks for pedicled flaps, or earlier for stable free flaps), a carefully graduated rehabilitation protocol guided by a specialized hand or orthopedic therapist is initiated to restore tendon glide and joint kinematics.
You Might Also Like