Mastering Hand Surgery Instrumentation and Tourniquet Physiology
Key Takeaway
Precision in hand surgery demands specialized instrumentation designed with fine working points and ergonomic handles. This guide details the core armamentarium—including scalpels, micro-forceps, and osseous tools—alongside critical tourniquet physiology. Mastering these instruments minimizes tissue trauma, optimizes neurovascular dissection, and ensures meticulous hemostasis, forming the foundation of successful operative outcomes in both elective and trauma hand surgery.
PRINCIPLES OF HAND SURGERY INSTRUMENTATION
The accurate and meticulous work required in hand surgery demands an armamentarium of highly specialized instruments. The fundamental biomechanical principle of hand surgery instrumentation dictates that tools must possess extremely fine, atraumatic working points, while their handles must be robust and ergonomically scaled to allow a firm, secure grip. This design minimizes intrinsic hand tremor and maximizes the surgeon's tactile feedback and mechanical advantage.
The philosophy of atraumatic tissue handling, originally championed by Sterling Bunnell, relies entirely on the appropriate selection and maintenance of these instruments. Using inappropriately sized or blunt instruments leads to crush injuries at the cellular level, subsequent tissue necrosis, excessive scarring, and ultimately, compromised functional outcomes.
The Core Soft Tissue Armamentarium
The foundation of soft tissue dissection in the hand relies on four basic instruments: the scalpel (knife), small tissue forceps, dissecting scissors, and the mosquito hemostat. Mastery of these four tools is the prerequisite for advanced reconstructive procedures.
The Scalpel (Knife)
The scalpel is the primary instrument for dissection. To avoid tearing through delicate fascial planes with blunt instruments, sharp dissection with a scalpel is universally preferred in hand surgery.
* Blade Selection: The No. 15 blade is the workhorse for skin incisions and deep dissection, while the No. 11 blade is reserved for precise puncture incisions (e.g., trigger finger release, abscess drainage).
* Maintenance: The blade must be firmly attached to the handle and changed frequently during the procedure. A dull blade requires excessive downward force, which compromises control and increases the risk of iatrogenic injury to underlying neurovascular structures.
Tissue Forceps (Pickups)
Because forceps touch the tissues more frequently than any other instrument, they must be rigorously inspected before surgery for cleanliness, alignment, and precision of closure.
* Biomechanics: Forceps should be held in a pencil grip. The spring tension must be light enough to prevent hand fatigue but firm enough to provide secure tissue purchase.
* Tissue Handling: Toothed forceps (e.g., Adson or micro-toothed) are preferred for skin and fascia as they puncture rather than crush the tissue. Smooth forceps should be reserved for handling delicate structures like nerves and vessels, though even these can cause crush injury if excessive pinch force is applied.
Dissecting Scissors
Scissors used in hand surgery must feature sharp double points.
* Design: Curved scissors (e.g., Stevens tenotomy scissors) are strongly preferred for dissecting neurovascular bundles.
* Technique: The curve of the scissor should always point away from the critical structure being dissected. The tips are used to gently spread tissues parallel to the neurovascular bundle, creating a safe plane before any cutting occurs.
Hemostats and Cautery
A bloodless field is essential, but when vessels must be controlled, precision is paramount.
* Clamping: A mosquito hemostat or specialized small forceps is preferred for clamping vessels because they cause minimal collateral tissue damage. Vessels should be clamped exactly as they are visualized, even when a pneumatic tourniquet is inflated, to prevent postoperative hematoma upon tourniquet deflation.
* Electrocautery: Bipolar electrocautery is the gold standard in hand surgery. Unlike monopolar cautery, which can channel current down a neurovascular bundle and cause distant thermal necrosis, bipolar cautery confines the thermal energy strictly to the tissue held between the forceps tines.
Surgical Warning: Never use monopolar electrocautery in close proximity to digital nerves or within the flexor tendon sheath. The risk of thermal conduction and subsequent irreversible nerve or tendon damage is unacceptably high. Always default to fine bipolar forceps.
RETRACTION AND EXPOSURE
Adequate exposure without excessive tissue tension is a delicate balance. Retractors in hand surgery must be carefully selected to avoid neuropraxia or ischemic necrosis of the skin edges.
Hand-Held Retractors
Retractors should generally be of the small single-hook (e.g., skin hooks) or double-hook (e.g., Senn) variety. A critical design feature is the handle length: handles must be long enough to keep the surgical assistant’s hands completely out of the primary surgeon’s working area and focal visual field.
Specialized and Dental Instruments
In many instances, standard orthopedic retractors are too bulky for the intricate anatomy of the carpus or digits. Certain dental instruments have been highly adapted for the dissection of fine ligaments and the elevation of periosteum from small bones.

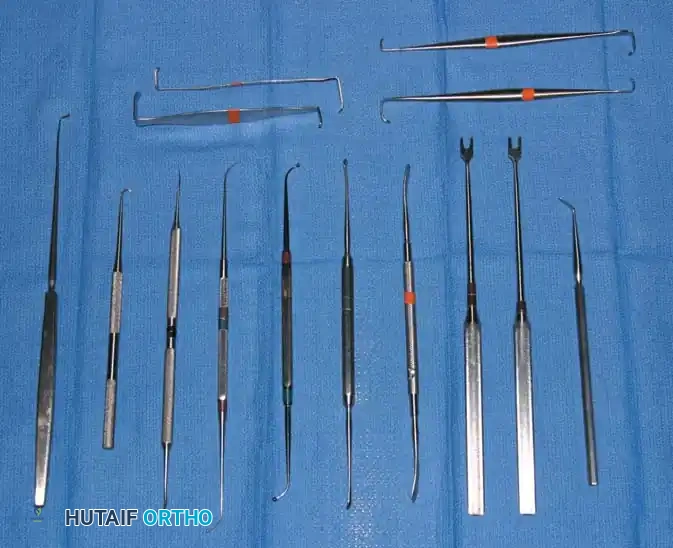
Fig. 61-11 A, Certain dental instruments are often useful for dissection of ligaments and bone. Retractors of numerous designs have been used in hand surgery, but modified tonsil prong (left) has proved to be most useful.
The modified tonsil prong is particularly useful for retracting neurovascular bundles or flexor tendons gently out of the operative field during deep palmar or digital dissection. Small self-retaining retractors (e.g., Alm retractors) are also highly valuable, particularly in procedures where an assistant is unavailable, though care must be taken to release tension periodically to allow skin edge perfusion.
OSSEOUS INSTRUMENTATION IN THE HAND
Surgical intervention on the phalanges, metacarpals, and carpal bones requires miniaturized versions of standard orthopedic equipment. The application of excessive force with oversized instruments frequently leads to iatrogenic comminution of small tubular bones.
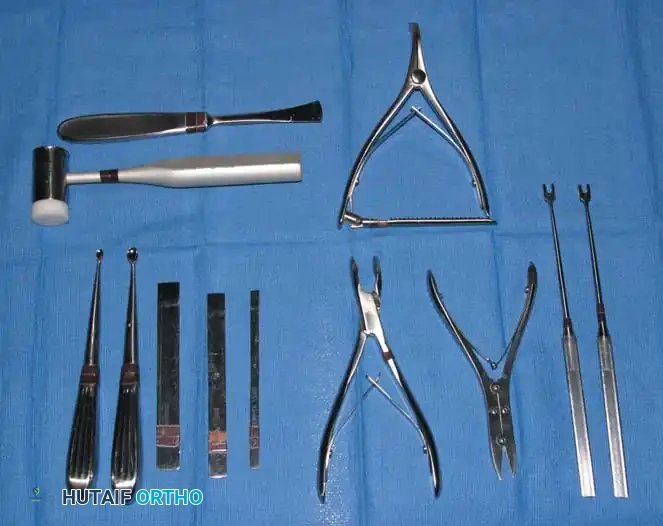
Fig. 61-9 Instruments for small bone surgery include osteotomes, bone cutter, rongeur, awl, small curet, and small hammer.
Bone Preparation and Resection
- Osteotomes: Small, razor-sharp osteotomes (single and double-beveled) are essential for corrective osteotomies. A lightweight mallet ensures that the surgeon can deliver controlled, incremental taps.
- Rongeurs and Bone Cutters: Fine-action rongeurs are utilized for contouring bone edges, such as in terminal phalangeal amputations or osteophyte excision in osteoarthritis.
- Curettes: Small curettes are vital for debriding enchondromas, cysts, or preparing fracture surfaces for bone grafting.
Drilling and Wire Fixation
For drilling holes in bone, small steel twist drill points provided in most surgical drill sets are satisfactory.
* Sizing: Drill points with a 2-mm diameter, or small, sharp-pointed Kirschner wires (K-wires) ranging from 0.028 to 0.062 inches, are most frequently required.
* Power Equipment: Air-powered or battery-powered micro-drills allow for the precise, high-speed placement of drill holes and wires.
Clinical Pearl: When drilling small bones of the hand, always use copious chilled saline irrigation. High-speed drilling without irrigation generates significant friction, leading to thermal osteonecrosis, which can result in pin-tract infections, hardware loosening, and delayed union.
MICROVASCULAR AND PERIPHERAL NERVE INSTRUMENTS
The advent of microsurgery has revolutionized the management of complex hand trauma, replantations, and free tissue transfers. This requires an entirely separate, highly specialized tray of instruments handled with extreme care.
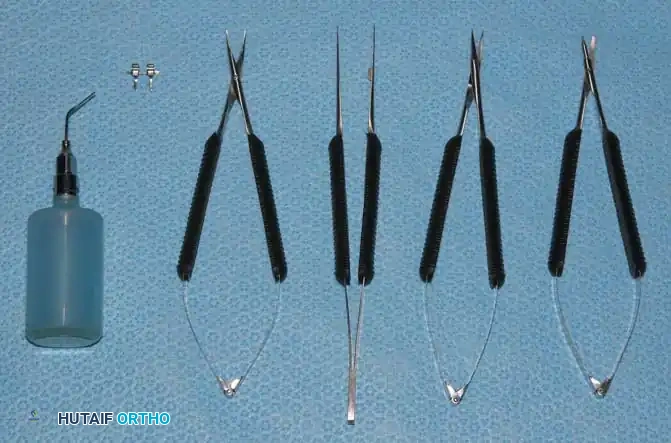
Fig. 61-10 Instruments useful in microvascular and digital nerve surgery include small irrigation bulb, microvascular clamp, microneedle holder, pickups, and scissors of assorted lengths.
The Microsurgical Setup
- Microneedle Holders: These feature narrow, cylindrical noses and smooth, non-serrated jaws. Serrations would damage the ultra-fine monofilament sutures (8-0 to 11-0) used in microvascular anastomoses. The cylindrical handle allows the surgeon to rotate the instrument between the thumb and index finger to drive the needle through tissue without requiring wrist pronation or supination.
- Micro-Pickups (Forceps): Jewelers' forceps (e.g., No. 3 or No. 5) are used to handle the adventitia of vessels and the epineurium of nerves. They must never be used to grasp the intima of a vessel.
- Microvascular Clamps: Acland-style double approximating clamps are used to secure vessels without causing crush injury to the endothelium. The closing pressure of these clamps is precisely calibrated.
- Irrigation: A small irrigation bulb with a blunt micro-cannula is essential for flushing vessel lumens with heparinized saline to visualize the intima and clear micro-thrombi.
Sutures
Sufficient varieties of wire and synthetic sutures are available to meet the needs of all tissue types. Most sutures utilized in hand surgery are available with swaged, straight, or curved needles. For flexor tendon repairs, a robust core suture (e.g., 3-0 or 4-0 braided synthetic) is paired with a fine epitendinous suture (e.g., 5-0 or 6-0 monofilament).
OPTICAL MAGNIFICATION
Fine surgery on soft tissues, nerves, and vessels is impossible without adequate optical magnification. The choice of magnification depends on the anatomical structure and the required field of view.

Fig. 61-12 Magnifying glasses for fine surgery on soft tissues. A, It is possible to achieve magnification of 6x with magnification lens on glasses frame. The magnification lens becomes too heavy for mounting, however, if more than 6x magnification is needed.
Surgical Loupes
For routine hand surgery, including tendon repairs and digital nerve coaptation, surgical loupes are standard.
* Magnification Levels: Standard Galilean loupes provide 2.5x to 3.5x magnification, offering a wide field of view and excellent depth of field. Prismatic (expanded field) loupes can provide up to 6x magnification.
* Ergonomic Limitations: As demonstrated in Figure 61-12, while it is possible to achieve 6x magnification on a glasses frame, the lenses become excessively heavy. Magnification beyond 6x requires a heavy optical housing that can cause severe cervical strain for the surgeon over long cases. Therefore, for procedures requiring >6x magnification (e.g., digital artery anastomosis), an operating microscope is strictly indicated.
TOURNIQUET PHYSIOLOGY AND ISCHEMIC TIME
The use of a pneumatic tourniquet is ubiquitous in hand surgery to provide the bloodless field necessary for the safe identification of microscopic structures. However, the application of a tourniquet induces profound local ischemia, leading to a cascade of metabolic derangements in the limb.
Understanding the physiological impact of tourniquet ischemia is critical for patient safety. The classic data by Wilgis (1971) perfectly illustrates the progressive metabolic acidosis and hypoxia that occurs within the isolated limb.
Metabolic Consequences of Tourniquet Ischemia
Table 61-1: Tourniquet Time and Revascularization Physiology
(Adapted from Wilgis EFS: Observations on the effects of tourniquet ischemia, J Bone Joint Surg 53A:1343, 1971)
| Tourniquet Time | pH (Mean) | pH (Range) | PO₂ (Mean, mm Hg) | PO₂ (Range) | PCO₂ (Mean, mm Hg) | PCO₂ (Range) |
|---|---|---|---|---|---|---|
| Preinflation | 7.40 | 7.38 - 7.42 | 45 | 40 - 50 | 38 | 35 - 40 |
| 0.5 Hours | 7.31 | 7.29 - 7.35 | 24 | 22 - 27 | 50 | 45 - 53 |
| 1.0 Hour | 7.19 | 7.15 - 7.22 | 20 | 19 - 22 | 62 | 60 - 66 |
| 1.5 Hours | 7.04 | 7.02 - 7.10 | 10 | 6 - 16 | 85 | 80 - 88 |
| 2.0 Hours | 6.90 | 6.88 - 6.96 | 4 | 0 - 6 | 104 | 92 - 110 |
Analysis of Ischemic Progression
- Oxygen Depletion (PO₂): Within the first 30 minutes, the partial pressure of oxygen (PO₂) drops precipitously from a baseline of 45 mm Hg to 24 mm Hg. By 2 hours, the limb is in a state of near-total anoxia (Mean PO₂ of 4 mm Hg).
- Hypercapnia (PCO₂): As cellular metabolism shifts from aerobic to anaerobic pathways, carbon dioxide accumulates rapidly. The PCO₂ nearly triples from a baseline of 38 mm Hg to 104 mm Hg at the 2-hour mark.
- Profound Acidosis (pH): The combination of lactic acid accumulation (from anaerobic glycolysis) and hypercapnia drives the local pH down severely. At 2 hours, the mean pH is 6.90. At this level of acidosis, cellular membranes begin to destabilize, and capillary endothelium becomes highly permeable.
Surgical Warning: The absolute maximum safe continuous tourniquet time in the upper extremity is 2 hours (120 minutes). Beyond this point, the profound acidosis (pH < 6.9) and anoxia lead to irreversible muscle necrosis, severe reperfusion injury, and a high risk of post-tourniquet syndrome (prolonged edema, stiffness, and neuropraxia).
Postoperative Protocols and Tourniquet "Let-Down"
If a surgical procedure is anticipated to exceed 2 hours, the surgeon must employ a "let-down" protocol.
* Reperfusion Phase: The tourniquet is deflated, and the limb is elevated and packed with warm, moist laparotomy sponges. Direct pressure is applied to the wound.
* Duration: The limb must be allowed to reperfuse for a minimum of 15 to 20 minutes (approximately 5 minutes of reperfusion for every 30 minutes of ischemia). This allows the accumulated lactic acid and CO₂ to be flushed into the systemic circulation and cleared by the lungs and kidneys, while fresh oxygen restores local cellular ATP stores.
* Systemic Effects: The anesthesia team must be warned prior to tourniquet deflation, as the sudden influx of acidotic, hyperkalemic blood into the systemic circulation can cause transient hypotension, tachycardia, or arrhythmias, particularly in elderly or medically compromised patients.
By combining a profound respect for tissue physiology with the masterful application of specialized instrumentation, the orthopedic hand surgeon can consistently achieve superior functional outcomes while minimizing iatrogenic morbidity.
You Might Also Like