Shortening Oblique Metatarsal Osteotomy Guide
Key Takeaway
The shortening oblique metatarsal osteotomy is a highly effective surgical intervention for intractable plantar keratosis caused by an abnormally long metatarsal. By precisely shortening the metatarsal shaft by 5 to 6 millimeters, surgeons can restore the harmonious metatarsal parabola, effectively offloading the prominent metatarsal head. This guide details the step-by-step surgical technique, biomechanical principles, fixation strategies, and postoperative protocols required to achieve optimal clinical outcomes and avoid complications such as nonunion or transfer metatarsalgia.
INTRODUCTION TO INTRACTABLE PLANTAR KERATOSIS
Intractable plantar keratosis (IPK) represents a localized, severely painful hyperkeratotic lesion on the plantar aspect of the foot, most commonly located beneath one or more of the lesser metatarsal heads. Unlike diffuse callosities caused by generalized friction, an IPK is the direct clinical manifestation of altered forefoot biomechanics—specifically, a focal concentration of weight-bearing forces during the stance and propulsive phases of gait.
The primary structural etiology for a discrete IPK is an abnormally long or plantarflexed metatarsal. When a single metatarsal projects distally beyond the harmonious curve of the metatarsal parabola (the Maestro curve), it acts as a rigid pivot point, absorbing a disproportionate quantum of ground reaction force. Over time, the mechanical overload induces hypertrophy of the stratum corneum, leading to the formation of a dense, nucleated keratinous plug that drives into the underlying dermis, causing debilitating pain.
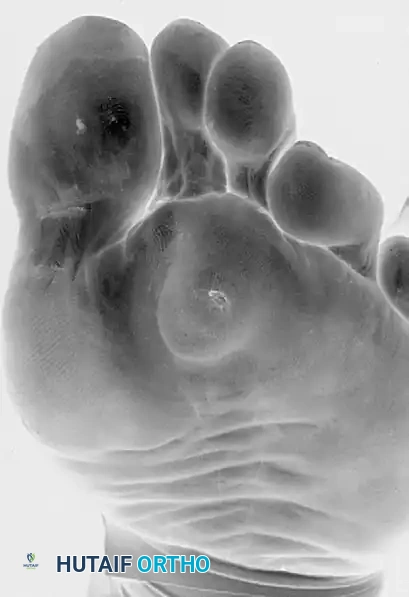
Clinical presentation of a severe, nucleated intractable plantar keratosis located beneath the second metatarsal head.
When conservative measures—such as custom orthoses with metatarsal offloading pads, aggressive debridement, and footwear modifications—fail to provide durable relief, surgical intervention is indicated. The Shortening Oblique Metatarsal Osteotomy (originally described by Giannestras and subsequently modified by Mann) is a powerful, structurally corrective procedure designed to decompress the affected metatarsophalangeal (MTP) joint by shortening the metatarsal shaft, thereby restoring a physiologic load distribution across the forefoot.
PREOPERATIVE EVALUATION AND BIOMECHANICAL PLANNING
Clinical Assessment
A meticulous clinical examination is paramount. The surgeon must differentiate an IPK from a plantar wart (verruca plantaris) or an inclusion cyst. An IPK will typically present directly beneath a bony prominence, exhibit maximum tenderness with direct vertical pressure (rather than side-to-side pinching), and reveal a deep central keratinous nucleus upon paring.
Evaluate the mobility of the tarsometatarsal (TMT) joints and the MTP joints. A rigid, plantarflexed metatarsal may require a different surgical approach (such as a basilar dorsiflexory wedge osteotomy) compared to a metatarsal that is simply excessively long.
Radiographic Evaluation
Standard weight-bearing radiographs of the foot (anteroposterior, lateral, and axial sesamoid/forefoot views) are mandatory for preoperative templating.
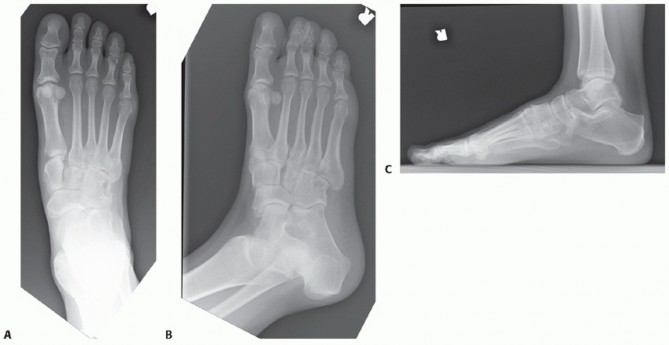
- Anteroposterior (AP) View: Assess the relative lengths of the metatarsals. The normal metatarsal parabola dictates that the second metatarsal is slightly longer than the first, with a smooth, cascading decrease in length from the second to the fifth metatarsal. An abrupt discrepancy indicates the offending digit.
- Lateral View: Evaluate the sagittal alignment of the metatarsals to rule out structural plantarflexion.
- Axial Forefoot View: This view is critical for visualizing the coronal plane alignment of the metatarsal heads and identifying any abnormal plantar prominence.
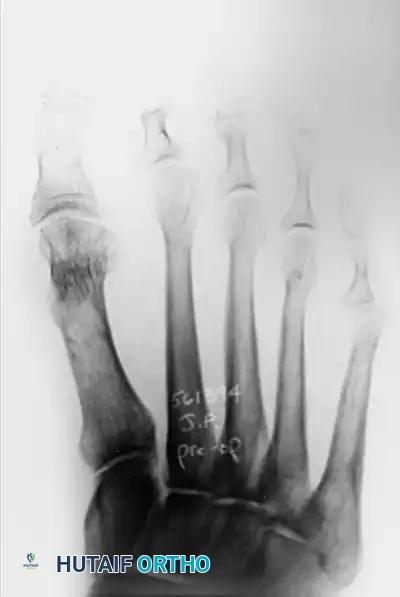
Preoperative weight-bearing AP radiograph demonstrating an excessively long second metatarsal, disrupting the normal forefoot parabola.
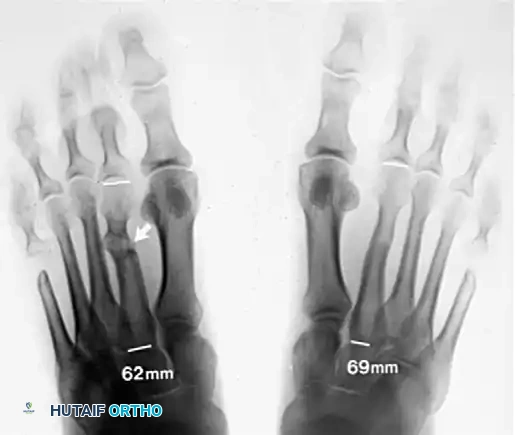
Comparative radiographic evaluation highlighting the length discrepancy. Precise measurement (e.g., 69mm vs. 62mm) is critical for determining the exact amount of shortening required.
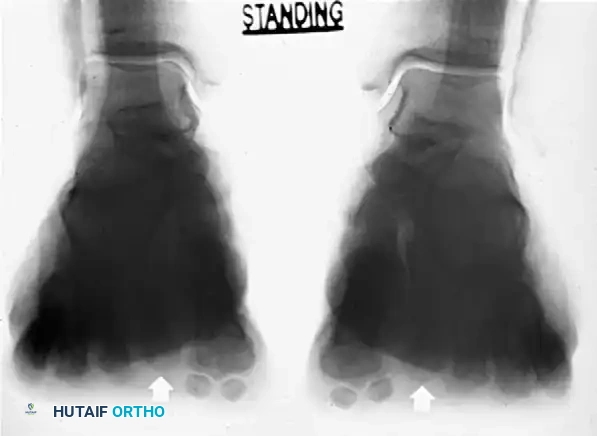
Axial standing forefoot radiographs. Note the abnormal plantar projection and elevation dynamics of the metatarsal heads (arrows), which correlate directly with the location of the plantar keratosis.
Clinical Pearl: The goal of the shortening oblique osteotomy is to create a smooth metatarsal arch. Preoperative templating should determine the exact amount of shortening needed—usually not more than 5 to 6 mm. Over-shortening is a catastrophic error that predictably leads to transfer metatarsalgia beneath the adjacent metatarsal heads.
SURGICAL TECHNIQUE: SHORTENING OBLIQUE METATARSAL OSTEOTOMY
The modified Giannestras/Mann technique utilizes a diaphyseal oblique osteotomy. The oblique nature of the cut provides a significantly larger surface area for bone healing compared to a transverse osteotomy, and it allows for rigid interfragmentary compression, drastically reducing the risk of nonunion.
1. Positioning and Anesthesia
- Anesthesia: The procedure can be performed under regional anesthesia (ankle block or popliteal block) with intravenous sedation, or under general anesthesia.
- Positioning: Supine position with a calf or thigh tourniquet applied to ensure a bloodless surgical field.
- Preparation: Standard orthopedic prep and drape of the entire foot and ankle.
2. Surgical Approach and Dissection
- Incision: Make a 5-cm longitudinal dorsal incision centered over the diaphysis of the affected metatarsal. The incision should begin just distal to the tarsometatarsal (TMT) joint and extend distally toward the metatarsal neck.
- Neurological Protection: Carefully deepen the incision through the subcutaneous tissue. Identify and meticulously retract the dorsal cutaneous nerve branches (typically branches of the superficial peroneal nerve). Neuroma formation in this region is highly symptomatic and must be avoided.
- Tendon Retraction: Identify the extensor digitorum longus (EDL) and extensor digitorum brevis (EDB) tendons. Retract them laterally or medially to expose the dorsal periosteum of the metatarsal.
- Periosteal Elevation: Perform a sharp, longitudinal incision through the periosteum. Use a Freer or Key elevator to perform a subperiosteal dissection circumferentially around the shaft of the metatarsal.
Surgical Warning: Limit the subperiosteal stripping strictly to the diaphyseal region required for the osteotomy and fixation. Excessive stripping, particularly distal toward the metatarsal neck, compromises the vascular supply to the capital fragment and increases the risk of delayed union or avascular necrosis.
3. The "Two Nicks" Measurement Technique
Accurate shortening is the most critical step of this procedure. Once the bone is cut, the oblique angle and the saw kerf make it exceptionally difficult to judge how much length has been resected.
* Prior to making the osteotomy, use a microsaw or a sharp osteotome to make two small, transverse cortical "nicks" on the dorsal aspect of the metatarsal shaft.
* These nicks must be placed at a precise, fixed distance from each other (e.g., exactly 10 mm apart), spanning the planned osteotomy site.
* After the osteotomy is performed and the bone is shortened, the distance between these two nicks is measured again. If the initial distance was 10 mm, and the goal is 5 mm of shortening, the fragments are manipulated until the nicks are exactly 5 mm apart.
4. Executing the Osteotomy
- Orientation: The osteotomy is made in an oblique fashion, typically running from dorsal-proximal to plantar-distal. This orientation resists dorsal displacement of the distal fragment during weight-bearing.
- Instrumentation: Perform the cut using a small sagittal saw under continuous saline irrigation to prevent thermal necrosis of the bone. Alternatively, an osteotome can be used through predrilled holes, though a saw provides a cleaner, more precise cut.
- Resection: Remove the pre-calculated amount of bone (usually 5 to 6 mm) based on the preoperative radiographic template.
5. Reduction and Fixation
Once the bone is shortened, the fragments must be rigidly stabilized to prevent rotation, dorsal elevation, or nonunion.
* Reduction: Use a small pointed bone-holding forceps (e.g., a Weber clamp) to hold the osteotomy in its newly shortened, anatomically aligned position. Verify the shortening by measuring the distance between the pre-marked dorsal nicks.
* Fixation Option A (Wire Fixation): Drill a transverse hole through both cortical fragments using a 0.045-inch Kirschner wire. Pass a 20-gauge stainless steel cerclage wire through the hole and wrap it around the osteotomy to secure the fixation. Fold the sharp ends of the wire flat against the metatarsal shaft to prevent soft tissue irritation.
Postoperative AP radiograph demonstrating fixation of the oblique osteotomy using the 20-gauge wire technique.
- Fixation Option B (Interfragmentary Compression Screw): This is the preferred modern technique due to superior biomechanical stability. Place a 2.0-mm or 2.4-mm cortical lag screw across the osteotomy perpendicular to the cut surface. Overdrill the near cortex to create a gliding hole, drill the far cortex, countersink the near cortex to prevent stress risers, measure, tap, and insert the screw to achieve rigid interfragmentary compression.
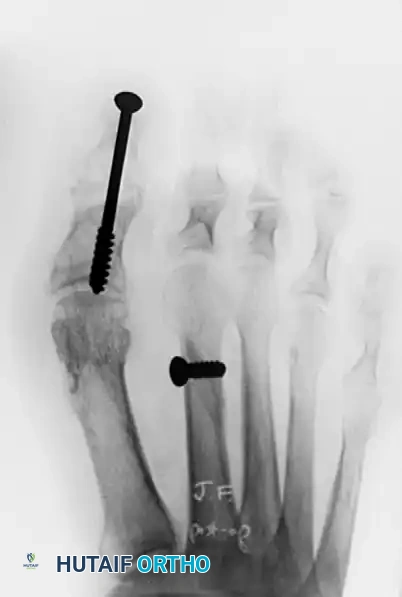
Postoperative AP radiograph showing rigid fixation of the shortened second metatarsal with an interfragmentary compression screw. Note the concurrent arthrodesis of the interphalangeal joint of the hallux for a varus deformity.
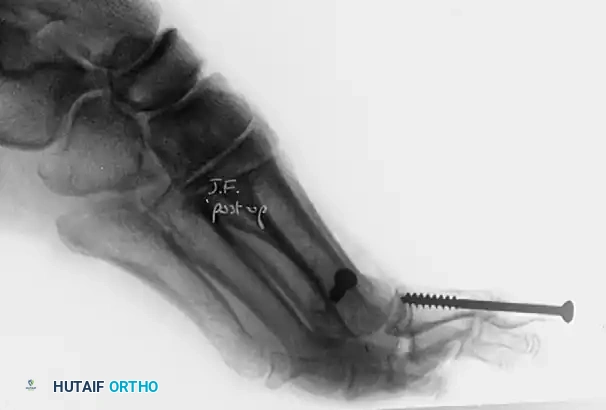
Lateral postoperative radiograph of the same patient, confirming excellent sagittal alignment of the metatarsal osteotomy and flush seating of the compression screw.
ALTERNATIVE TECHNIQUE: BASILAR DORSAL CLOSING WEDGE OSTEOTOMY
In cases where the primary pathology is a rigidly plantarflexed metatarsal rather than an excessively long one, a basilar dorsal closing wedge osteotomy may be indicated.
Technique 83-16 Parameters:
- Location: The osteotomy is performed at the metaphyseal-diaphyseal junction proximally.
- Resection Limit: Do not remove more than a 2 to 3-mm dorsal wedge of bone. Removing a larger wedge will result in excessive dorsal elevation of the metatarsal head, completely offloading it and guaranteeing transfer metatarsalgia.
- Fixation: Rigid internal fixation (typically a dorsal plate or crossed K-wires) is required.
- Postoperative Care: The foot must be casted for 6 weeks. The patient is kept strictly non-weight-bearing for the first 3 weeks to protect the proximal osteotomy hinge.
POSTOPERATIVE PROTOCOL
Successful healing of a diaphyseal metatarsal osteotomy requires strict adherence to postoperative immobilization protocols.
- Immediate Post-Op (Weeks 0-4): The patient is placed in a well-padded, short-leg weight-bearing cast equipped with a toe plate. The toe plate is critical to support the digits and prevent dorsal contracture of the MTP joints.
- Weight-Bearing Status: For the standard shortening oblique osteotomy, protected weight-bearing in the cast is generally permitted immediately, provided rigid screw fixation was achieved. If wire fixation was used, or bone quality is poor, a period of non-weight-bearing may be advised.
- Transition (Weeks 4-6): At 4 weeks, the cast is removed. Clinical healing (absence of pain on palpation) and radiographic healing (callus formation) are assessed. The patient is transitioned to a stiff-soled postoperative shoe or a controlled ankle motion (CAM) boot for an additional 2 to 4 weeks.
- Long-Term: Return to standard, supportive footwear is typically achieved by 8 to 10 weeks. High-impact activities are restricted until complete radiographic union is confirmed (usually 3 to 4 months).
COMPLICATIONS AND MANAGEMENT
While highly effective, metatarsal osteotomies carry a distinct risk profile. The diaphysis of the metatarsal has a relatively tenuous blood supply compared to the metaphysis, making it susceptible to healing complications.
1. Nonunion and Delayed Union
Nonunion is the most dreaded complication of the diaphyseal osteotomy. It is usually the result of inadequate fixation, excessive periosteal stripping, or thermal necrosis during the saw cut. Patients present with persistent dorsal midfoot pain, swelling, and a palpable, tender mass at the osteotomy site.
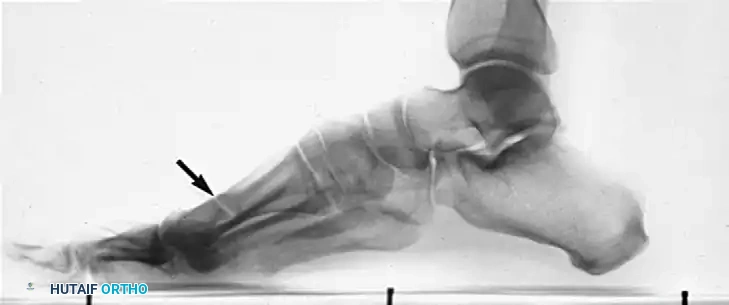
Lateral radiograph demonstrating a painful nonunion of a transverse metatarsal osteotomy (arrow). Note the dorsal angulation and hypertrophic callus formation attempting to bridge the unstable gap.
Management of Nonunion:
Symptomatic nonunions require revision surgery. The fibrous nonunion must be aggressively debrided down to bleeding, viable bone. Rigid internal fixation (usually a dorsal plate) is applied, supplemented by an autologous onlay bone graft (often harvested from the calcaneus or proximal tibia) to stimulate osteogenesis.
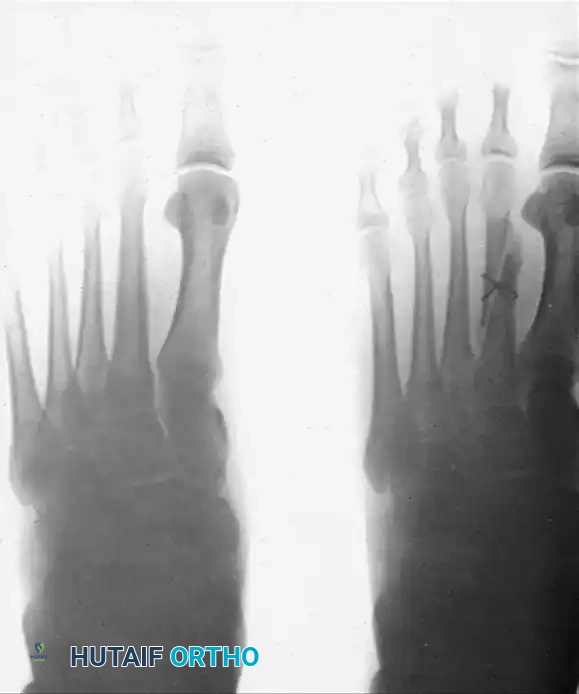
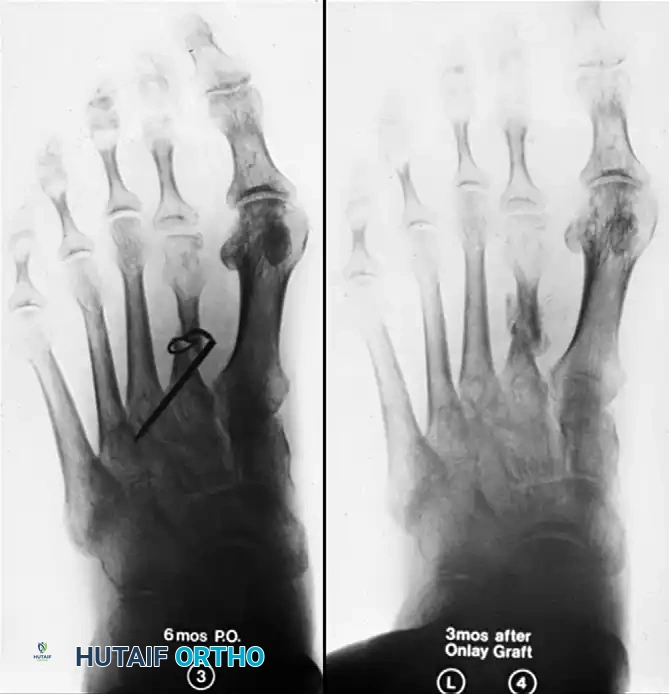
Radiographic progression of nonunion management. (Left) AP view at 6 months post-op showing failed wire fixation and nonunion. (Right) AP view 3 months after revision surgery utilizing an onlay bone graft, demonstrating successful consolidation. The patient was walking comfortably in a firm, solid shoe.
2. Malunion and Transfer Metatarsalgia
If the metatarsal is shortened excessively (greater than 6 mm) or if the distal fragment is allowed to elevate dorsally during healing, the affected metatarsal head will no longer participate in weight-bearing. The ground reaction forces will immediately transfer to the adjacent, relatively longer metatarsal heads.
This results in transfer metatarsalgia—the development of a new, often more painful intractable plantar keratosis beneath the adjacent metatarsal (e.g., curing a 2nd metatarsal IPK only to create a 3rd metatarsal IPK).
Prevention is the only acceptable management strategy. The surgeon must meticulously calculate the required shortening preoperatively, utilize the "two nicks" technique for intraoperative accuracy, and secure the osteotomy with rigid interfragmentary compression to prevent dorsal drift. If severe symptomatic transfer metatarsalgia occurs, corrective osteotomy of the newly overloaded metatarsal may be required.
You Might Also Like