00:00
Start Quiz
Question 76
What is the average linear wear rate of a conventional, noncross-linked ultra-high molecular weight polyethylene liner used in total hip arthroplasty?
Explanation
Several studies have shown that ultra-high molecular weight polyethylene liners used in total hip arthroplasties wear at a rate of 0.1 to 0.2 mm/yr. The orthopaedic surgeon performing total hip arthroplasties should be aware of the average wear rate so that potential problems can be identified when following patients postoperatively. Callaghan JJ, Albright JC, Goetz DD, Olejniczak JP, Johnston RC: Charnley total hip arthroplasty with cement: Minimum twenty-five year follow-up. J Bone Joint Surg Am 2000;82:487-497.
Question 77
A 68-year-old woman underwent a successful total right hip arthroplasty with a metal-on-metal articulation and cementless porous-coated components. Three months later, she underwent identical surgery on the left hip. Three months after surgery on the left hip, she reports groin pain on ambulation. Examination reveals significant groin discomfort with passive hip motion, particularly at the extremes of motion. Radiographs are shown in Figures 21a and 21b. Laboratory studies show an erythrocyte sedimentation rate of 35 mm/h and a C-reactive protein of 0.9. Aspiration yields scant growth of Staphylococcus epidermidis in the broth only, with no evidence of loosening on arthrography. A second aspiration yields scant growth of Staphylococcus epidermidis in the broth only. What is the most likely cause of the patient's pain?
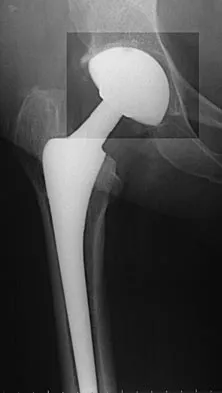
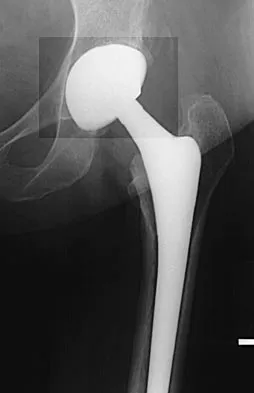
Explanation
The difference in the clinical results combined with the laboratory findings points to infection. While there is a significant risk of false-positive findings with aspiration, the fact that two successive aspirations grew the same organism strongly suggests infection. The radiograph shows that there is more radiolucency around the left acetabular component than the right component. White RE: Evaluation of the painful total hip arthroplasty, in Callaghan JJ, Rosenberg AG, Rubash HE (eds): The Adult Hip. Philadelphia, PA, Lippincott-Raven, 1998, vol 2, pp 1377-1385.
Question 78
Etanercept is a recombinant genetically engineered fusion protein used to treat rheumatoid arthritis. What is its mode of action?
Explanation
Etanercept is a molecule consisting of the Fc portion of IgG fused to the extracellular domain of the p76 human THF-a receptor. It is soluble and binds TNF-a. Infliximab is the monoclonal antibody that binds TNF-a. IL-1 receptor antagonists are still in development. Leflunomide is a drug that inhibits pyrimidine synthesis and is similar to methotrexate as an antimetabolite.
Question 79
Which of the following bearing materials is most resistant to scratching from third-body debris?
Explanation
Alumina is the hardest of all the materials listed. Clinical retrieval demonstrates resistance to scratching from third-body debris.
Question 80
Which of the following surgical techniques is associated with an increased incidence of patellar complications after total knee arthroplasty?
Explanation
Surgical technique in patellar resurfacing has been found to be one of the critical factors in the success or failure of total knee arthroplasty. Theoretically, metal-backed patellar components are an excellent way of evenly distributing joint forces from the polyethylene button to bone (similar to the tibial component). However, despite this theoretical advantage, metal-backed patellae have been associated with a higher failure rate. Some of the observed problems include poor bone ingrowth, peg failure, dissociation of the metal plate and polyethylene button, and component fracture. Because of these factors, all-polyethylene patellae have proved to be the standard if patellar resurfacing is attempted. Medialization of the patellar component, a symmetrically thick patella, and external rotation of the femoral and tibial components improve patellar tracking. Pellicci PM, Tria AJ Jr, Garvin KL (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 323-337.
Question 81
A large circumferential proximal femoral allograft is to be used in the reconstruction of a failed femoral component in a total hip arthroplasty. To enhance fixation of the graft to the implant, which of the following strategies should be used?
Explanation
The optimum treatment is cementing the implant to the allograft. Press-fit stability is unreliable. Wires and screws may be used for an incomplete proximal femoral allograft but cannot be used to anchor a complete proximal femoral allograft. Allan DG, Lavoie GJ, Rudan JF, et al: The use of allograft bone in revision total hip arthroplasty, in Friedlaender GE, Goldberg VM (eds): Bone and Cartilage Allografts: Biology and Clinical Applications. Park Ridge, IL, American Academy of Orthopaedic Surgeons, 1991, pp 263-264. Gross AE, Lavoie MV, McDermott P, Marks P: The use of allograft bone in revision of total hip arthroplasty. Clin Orthop 1985;197:115-122.
Question 82
Which of the following design features of a femoral component used in a total knee arthroplasty best minimizes the patellar component contact stresses?
Explanation
Several studies have shown that design of the femoral component, especially the trochlear groove portion, largely influences patellar tracking and patellofemoral contact stresses. A deep, curved anatomic femoral trochlear groove has been shown to have the lowest contact stresses. Petersilge WJ, Oishi CS, Kaufman KR, Irby SE, Colwell CW Jr: The effect of trochlear design on patellofemoral shear and compressive forces in total knee arthroplasty. Clin Orthop 1994;309:124-130. Theiss SM, Kitziger KJ, Lotke PS, Lotke PA: Component design affecting patellofemoral complications after total knee arthroplasty. Clin Orthop 1996;326:183-187.
Question 83
Figure 22 shows the radiograph of a 67-year-old woman who has an infected left total hip arthroplasty. The most efficient means to remove the distal cement mantle includes the use of
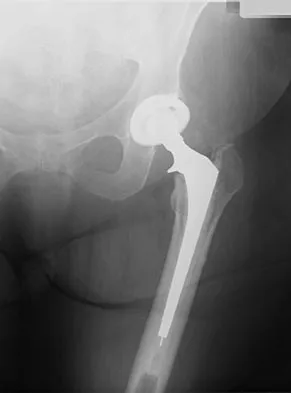
Explanation
An extended trochanteric osteotomy has been shown to be very efficient in removing a well-fixed distal implant and cement with minimal complications. Direct lateral, posterior, and transtrochanteric osteotomy exposures do not provide exposure of the midfemur.
Question 84
Which of the following findings best describes the effects of increasing conformity of a fixed tibial bearing component and femoral component in total knee arthroplasty?
Explanation
In the design of tibial and femoral components, a compromise must be made between contact stresses and constraint. Increased conformity increases constraint, limits motion, and potentially increases stress on the knee-cement interface. By increasing conformity, the surface area over which force is applied is increased, resulting in decreased peak contact stresses and decreased component wear rates. Pellicci PM, Tria AJ Jr, Garvin KL (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 265-274.
Question 85
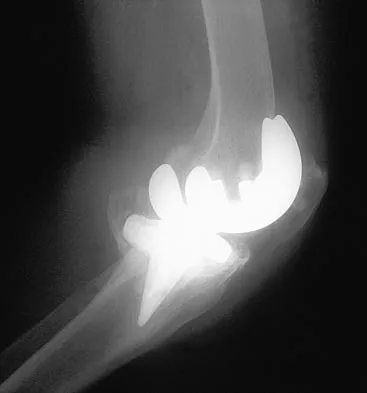
Figures 23a and 23b show the AP and lateral radiographs of a 67-year-old woman who has severe left knee pain when ambulating. History reveals that she underwent primary total knee arthroplasty 7 years ago. The patient reports increasing deformity over the past several years and uses a knee brace and a cane. Examination reveals that she walks with a varus thrust and has an uncorrectable varus deformity with valgus force. What is the primary reason for implant failure?
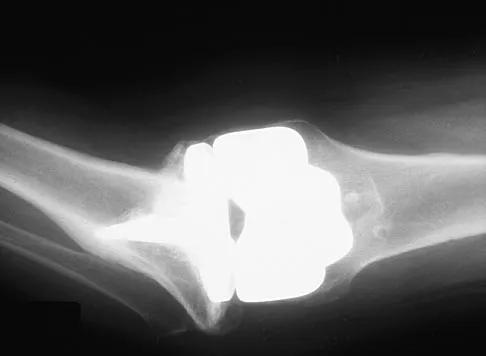
Explanation
Both cemented and cementless total knee arthroplasties depend on adequate fixation of the tibial component to promote long-term survivorship. An effective stem and adequate peripheral fixation of the tibial component to the cancellous-cortical portion of the proximal tibia are necessary for cementless fixation. Peripheral screws and pegs can serve as adjunctive fixation to decrease micromotion and shear forces and allow bone ingrowth to occur. Careful preparation of the proximal tibial surface can minimize fixation failure. Cemented fixation of the tibial stem should be performed in addition to the plateau. Osteolysis, polyethylene wear, and failure at the insert/tray locking mechanism have not occurred. Posterior cruciate ligament retention has not caused the tibial component fixation failure.
Question 86
Which of the following bearing surface combinations has shown the lowest in vivo wear rates in total hip arthroplasty?
Explanation
Ceramic bearings, made of alumina, have the lowest in vivo wear rates of any bearing combination, 0.5 to 2.5 Mm per component per year. Laboratory wear rates for metal-on-metal are lower than those for metal-on-polyethylene bearings, ranging from 2.5 to 5.0 Mm per year. Titanium used for bearing surfaces has a high failure rate because of a poor resistance to wear and notch sensitivity. Wear rates for ceramic-on-polyethylene bearings have varied, ranging from 0 to 150 Mm. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 47-53.
Question 87
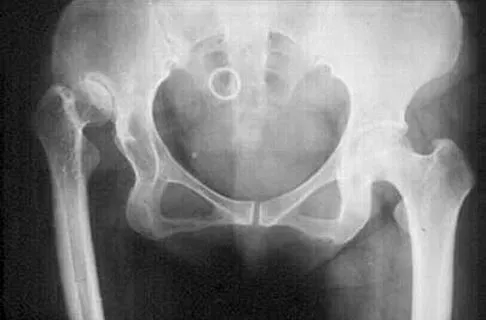
Figure 24 shows the radiograph of a 47-year-old woman who has severe right hip pain and a limp. Management should consist of
Explanation
Femoral shortening osteotomy for a Crowe type IV hip dislocation has been shown to provide superior results with minimal complications. Cementless fixation of the stem allows for modular implants that greatly simplify the reconstruction.
Question 88
When planning revision of a total hip arthroplasty where an acetabular reconstruction will be required, what prerequisite is important to ensure long-term success of a cementless component?
Explanation
In bone defects where host bone support is less than 50%, the failure rate is 70% at 5.1 years. The presence or absence of columns or hip position is of relatively little importance if the supportive bone is not present in at least 50% of the surface area around the future acetabular implant.
Question 89
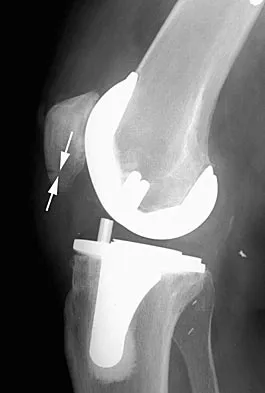
A 62-year-old man who underwent total knee arthroplasty 6 months ago now reports pain after falling on the anterior portion of the knee. Examination reveals weakness of knee extension but no extensor lag. Flexion that had once measured 115 degrees is now limited to 70 degrees because of pain. A radiograph is shown in Figure 25. Management should now consist of
Explanation
The patient has a type IIIB patellar fracture (inferior pole fracture with an intact patellar tendon). Nonsurgical management is the treatment of choice if there is little displacement and the extensor mechanism is intact. Brown TE, Diduch DR: Fractures of the patella, in Insall JN, Scott WN (eds): Surgery of the Knee, ed 3. Philadelphia, PA, Churchill Livingstone, 2001, vol 2, pp 1290-1312.
Question 90
Failure of high tibial osteotomy (HTO) is most closely associated with which of the following factors?
Explanation
Long-term survivorship studies have attempted to clarify patient factors related to good outcomes in HTO. One particular study showed that a patient age of less than 50 years was related to good outcomes in those who had good preoperative knee flexion. The same study found no relation between HTO failure and the presence of postoperative infection or deep venous thrombosis. The presence of a lateral tibial thrust is a contraindication to performing this surgery. As expected, good patient selection is critical to obtaining good long-term results with HTO. Naudie D, Borne RB, Rorabeck CH, Bourne TJ: Survivorship of the high tibial valgus osteotomy: A 10- to 22-year followup study. Clin Orthop 1999;367:18-27. Rinonapoli E, Mancini GB, Corvaglia A, Musiello S: Tibial osteotomy for varus gonarthrosis: A 10- to 21-year followup study. Clin Orthop 1998;353:185-193.
Question 91
During a posterior cruciate ligament-sacrificing total knee arthroplasty with anterior referencing, 8 mm of distal femur is resected. It is noted that the flexion gap is tight and the extension gap appears stable. What is the next most appropriate step in management?
Explanation
If the flexion gap is tight and the extension gap is correct, it is preferable to change only the flexion gap and leave the extension gap unchanged; therefore, the treatment of choice is to decrease the size of the femoral component. The smaller component will be smaller in both medial-lateral as well as anterior-posterior dimensions. A smaller anterior-posterior size will allow more space for the flexion gap without significantly affecting the extension gap. Decreasing the size of the tibial polyethylene insert thickness or cutting more proximal tibia will affect both the flexion and extension gaps. Cutting more distal femur will increase the extension gap and not change the flexion gap, making the described situation worse. Cutting both the proximal tibia and distal femur will increase both the flexion and extension gaps.
Question 92
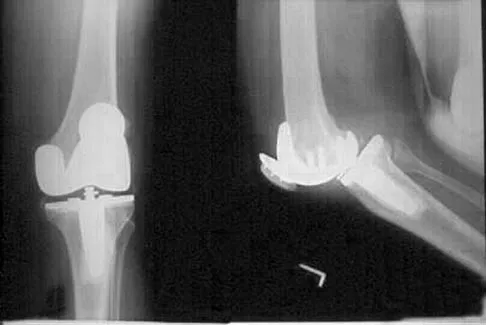
A 72-year-old woman with rheumatoid arthritis who underwent primary total knee arthroplasty 2 years ago has had diffuse knee pain that developed shortly after the surgery. The patient has difficulty with stair descent and arising from chairs. Evaluation for infection is negative. AP and lateral radiographs are shown in Figure 26. Management should now consist of
Explanation
The radiographs show posterior flexion instability that is the result of flexion-extension gap imbalance and/or posterior cruciate ligament incompetence after a posterior cruciate-retaining total knee arthroplasty. The radiographs also show anterior femoral displacement on the tibia. Pagnano and associates reported on a series of patients with painful total knee arthroplasties who had been previously diagnosed as having pain of unknown etiology, showing that the pain was secondary to flexion instability. Pain relief was achieved by revision to a posterior stabilized implant. Pagnano MW, Hanssen AD, Lewallen DG, Stuart MJ: Flexion instability after primary posterior cruciate retaining total knee arthroplasty. Clin Orthop 1998;356:39-46. Fehring TK, Valadie AL: Knee instability after total knee arthroplasty. Clin Orthop 1994;299:157-162.
Question 93
A homebound 75-year-old woman with diabetes mellitus has had progressive left knee pain and swelling for the past 6 weeks. She is febrile with a temperature of 103 degrees F (39.5 degrees C). History reveals that she underwent arthroplasty 5 years ago. Examination shows passive range of motion of 0 to 100 degrees with no active extension. Knee aspiration reveals purulent fluid with a Gram stain showing gram-negative rods. A radiograph is shown in Figure 27. In addition to IV antibiotics, which of the following management options offers the best chance of a successful outcome?
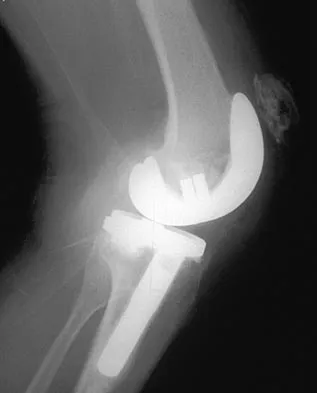
Explanation
The patient has an infected total knee arthroplasty and an interrupted extensor mechanism. A late infection of a total knee arthroplasty in a patient with diabetes mellitus and a virulent organism requires removal of the components, debridement, antibiotic spacers, and surveillance to ensure eradication of the infection. Reconstruction of an incompetent extensor mechanism in an infected knee is extremely unlikely to be successful. Arthrodesis is the procedure of choice if a revision total knee arthroplasty is not likely to succeed. Resection arthroplasty is recommended only as a long-term solution if the patient is medically unable to undergo further surgery. Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgery, 2002, pp 513-536.
Question 94
Design and manufacturing of a metal-on-metal articulation has an important influence on the tribology. Which of the following statements best characterizes the type of contact that is best for metal-on-metal articulations?
Explanation
It is important that the radii of a metal-on-metal head to cup articulation be such that there is polar contact. As the radii become closer to equal, conditions favor higher frictional torque and equatorial seizing. The "bedding in" of metal-on-metal surfaces and their stiffness are both components of the properties considered in the design of polar contact surfaces.
Question 95
A 52-year-old man has had groin and deep buttock pain for the past 2 months. Examination reveals that hip range of motion is mildly restricted, and he has pain with both weight bearing and at rest. An MRI scan is shown in Figure 28. Management should consist of
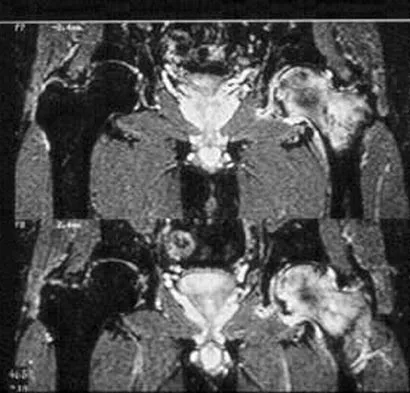
Explanation
The MRI findings show highly increased signal through the entire femoral head and neck that is diagnostic of transient osteoporosis of the femoral head. This recently described entity is often seen in middle-aged men and should be treated nonsurgically with protected weight bearing and anti-inflammatory drugs. The natural history is that of self-resolution. Guerra JJ, Steinberg ME: Distinguishing transient osteoporosis from avascular necrosis of the hip. J Bone Joint Surg Am 1995;77:616-624.
Question 96
Polyethylene wear of the bearing surface has been recognized as a mode of failure in total knee arthroplasty; therefore, many patients are offered polyethylene exchange. In terms of success rates, this surgical procedure has been reported to have a
Explanation
Engh and associates reported on the results of 63 knees (56 patients) following polyethylene exchange. The mean interval between exchange and the index total knee arthroplasty was 59 months. The mean follow-up after exchange was 7.4 years. Seven of 48 knees with adequate follow-up failed. Greater failure occurred if there was more severe wear before the exchange. Greater undersurface wear also resulted in a higher failure rate. Perioperative osteolysis or intraoperative observation of metallosis did not have an impact on the failure of polyethylene exchange. The risk of infection is no different from other total knee arthroplasty revisions. Wasielewski RC, Parks N, Williams I, et al: Tibial insert undersurface as a contributing source of polyethylene wear debris. Clin Orthop 1997;345:53-59.
Question 97
Which of the following types of ultra-high molecular weight polyethylene has been associated with the poorest clinical performance?
Explanation
Numerous studies have documented the poor performance of heat-pressed ultra-high molecular weight polyethylene used in the porous-coated anatomic tibial inserts of both total knee and unicompartmental arthroplasty. The other processing and sterilization methods have not been associated with significantly high failure rates. Wright TM, Rimnac CM, Stulberg SD, et al: Wear of polyethylene in total joint replacements: Observations from retrieved PCA knee implants. Clin Orthop 1992;276:126-134. Landy MM, Walker PS: Wear of ultra-high molecular-weight polyethylene components of 90 retrieved knee prostheses. J Arthroplasty 1988;3:S73-S85.
Question 98
Which of the following is considered the best method for the prevention of wrong-site surgery?
Explanation
The best method of preventing wrong-site surgery is for the surgeon to initial the surgical site in the preoperative holding area after discussion and confirmation of the site with the patient. This should be done before sedating medications are administered. A recent study found that patient noncompliance with specific preoperative instructions to mark the site with a "yes" at home was surprisingly high; only 59% of the patients marked the extremity correctly and 37% made no mark. Noncompliance was higher in those with workers' compensation claims (70%) and those with previous related surgery (51%). DeGiovanni CW, Kang L, Manuel J: Patient compliance in avoiding wrong site surgery. J Bone Joint Surg Am 2003;85:815-819.
Question 99
During the implantation of a cementless acetabular component in total hip arthroplasty, placement of a screw in the anterior superior quadrant puts which of the following structures at risk for damage?
Explanation
A knowledge of the safe quadrants for screw placement for acetabular component implantation is essential when performing total hip arthroplasty. The external iliac vessels are on the inner wall of the pelvis, corresponding to the anterior superior quadrant of the acetabulum. Keating EM, Ritter MA, Faris PM: Structures at risk from medially placed acetabular screws. J Bone Joint Surg Am 1990;72:509-511.
Question 100
What is the most frequent complication following primary total hip arthroplasty?
Explanation
Thromboembolic disease can occur in up to 58% of unprotected patients and up to 20% of protected patients depending on the type of prophylaxis used, even though most thrombi are small and have little clinical consequence. The primary goal of prophylaxis is to prevent symptomatic deep venous thrombosis and fatal pulmonary emboli. Dislocation has been reported in up to 10% of primary cases, but generally acceptable rates of less than 5% are the norm. Component loosening following primary total hip arthroplasty is rare prior to a 10-year follow-up, and 90% to 95% of patients should reach the 10-year follow-up without the need for revision for any reason. Metal hypersensitivity is unusual, and nickel found in cobalt-chromium alloys is the most common offending agent. Infection of primary total hip arthroplasty is less than 1%. Eftekhar N: Total Hip Arthroplasty. St Louis, MO, Mosby,1993, pp 1445-1676.
