00:00
Start Quiz
Question 51
During total knee arthroplasty, what component position aids in proper tracking and stability of the patellar component?
Explanation
The femoral component should be implanted with enough external rotation to facilitate patellar tracking. Proper tracking requires a normal Q angle and is affected by axial and rotational alignment of the femur and tibia. An excessive Q angle can result from internal rotation of either component, medialization of the tibial tray, or lateralization of the patellar component. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 559-582.
Question 52
An otherwise healthy 57-year-old woman has limited range of motion and moderate effusion after undergoing total knee arthroplasty 6 months ago. One of two cultures of joint aspirate reveals methicillin-resistant Staphylococcus epidermidis. Management should now consist of
Explanation
The rapidly increasing prevalence of infection from Staphylococcus epidermidis has made this the most frequently cultured organism. In most patients, the infection occurred intraoperatively, thereby resulting in a chronic infection if not detected within the first 6 weeks after surgery. Irrigation of the joint may be successful during this time in 60% of patients, but the most successful treatment is extirpation for 6 weeks, followed by delayed reimplantation. This approach may result in a salvage rate of as high as 90% in some patients. Drancourt M, Stein A, Argenson JN, et al: Oral rifampin plus ofloxacin for treatment of staphylococcus-infected orthopedic implants. Antimicrob Agents Chemother 1993;37:1214-1218. Duncan CP, Beauchamp C: A temporary antibiotic-loaded joint replacement system for the management of complex infections involving the hip. Orthop Clin North Am 1993;24:751-759.
Question 53
Figure 13 shows the radiographs of a 56-year-old woman who has pain and varus knee deformity after undergoing total knee arthroplasty 8 years ago. Aspiration and studies for infection are negative. During revision surgery, management of the tibial bone loss is best achieved by
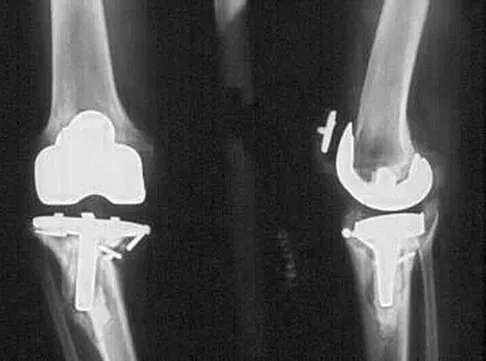
Explanation
Massive bone loss encountered in revision total knee arthroplasty remains a significant challenge. Recent reports have shown high success rates using structural allograft to reconstruct massive bone defects. Custom and hinged prostheses in this setting are no longer favored. The defect shown is segmental and is too large to be filled with cement or iliac crest bone graft. Mow CS, Wiedel JD: Structural allografting in revision total knee arthroplasty. J Arthroplasty 1996;11:235-241. Engh GA, Herzwurm PJ, Parks NL: Treatment of major defects of bone with bulk allografts and stemmed components during total knee arthroplasty. J Bone Joint Surg Am 1997;79:1030-1039.
Question 54
Varus intertrochanteric osteotomy for coxa valga commonly produces which of the following results?
Explanation
The greater trochanter is raised as a by-product of varus osteotomy, and a temporary abductor lag and lurch is common for 6 months following surgery. In the absence of hip joint subluxation, varus intertrochanteric osteotomy has no effect on the center edge angle of Wiberg. Varus osteotomy typically increases femoral offset, thereby improving the abductor lever arm and reducing the hip joint reaction force. Even without taking a wedge, varus osteotomy always produces some degree of shortening.
Question 55
A 65-year-old woman has nausea, vomiting, and abdominal distention after undergoing total knee arthroplasty 48 hours ago. An abdominal radiograph is shown in Figure 14. Associated risk factors for this disorder include
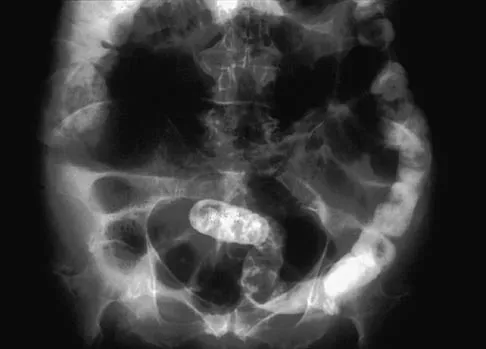
Explanation
The prevalence of postoperative ileus associated with total joint arthroplasty has been reported to be as high as 3%. Metabolic abnormalities such as hypokalemia are believed to contribute to the onset of ileus and Ogilvie's syndrome (acute pseudo-obstruction of the colon). Prolonged bed rest also has been associated with the development of ileus and Ogilvie's syndrome. Untreated Ogilvie's syndrome can result in cecal perforation. Ileus usually is not accompanied by mechanical obstruction. Antibiotic administration and the type of anesthesia used have not been correlated with development of ileus. Administration of warfarin has been associated with elevated prothrombin time/partial thromboplastin time and international normalized ratio levels when ileus is managed with a nasogastric tube and suction. Metabolic imbalances must be corrected to reverse the ileus process. Iorio R, Healy WL, Appleby D: The association of excessive warfarin anticoagulation and postoperative ileus after total joint replacement surgery. J Arthroplasty 2000;15:220-223.
Question 56
A 77-year-old woman with osteoporosis who underwent cemented total hip arthroplasty 12 years ago fell down a flight of stairs. A radiograph is shown in Figure 15. What is the best option for treating this fracture?
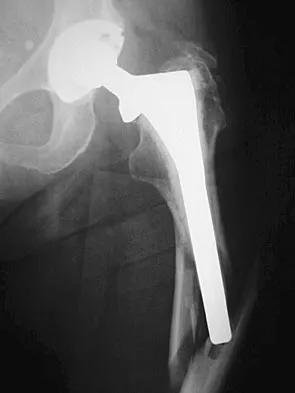
Explanation
Type I fractures are trochanteric fractures usually secondary to osteolysis. Type II fractures are located around the stem. Type III fractures are distal to the stem. If the fracture and prosthesis are stable, the fracture can be treated nonsurgically. If the fracture is unstable, the stability of the prosthesis should be assessed. If the prosthesis is unstable (type IIB), treatment should consist of revision to a long stem prosthesis that bypasses the fracture by two cortical diameters. If, as in this patient, the prosthesis is not loose (type IIA), open reduction and internal fixation is the appropriate option. Proximal femoral allograft is appropriate for type IIIC fractures in which the proximal bone is significantly compromised and the femoral component is loose. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 455-492.
Question 57
Total hip arthroplasty in a patient with a long-standing hip fusion on the contralateral side is most likely to result in
Explanation
Contralateral total hip arthroplasty in patients with hip fusions results in a 40% higher rate of mechanical failure and loosening. During gait, motion of the contralateral hip is increased and more time is spent bearing weight on that hip. In patients with hip fusions, gait efficiency is only 53%, with a greater rate of oxygen consumption. Garvin KL, Pellicci PM, Windsor RE, et al: Contralateral total hip arthroplasty or ipsilateral total hip arthroplasty in patients who have long-standing fusion of the hip. J Bone Joint Surg Am 1989;71:1355-1362. Gore DR, Murray MP, et al: Walking patterns of men with unilateral surgical hip fusion. J Bone Joint Surg Am 1975;57:759-765.
Question 58
A 60-year-old woman reports anterior knee pain 2 years after undergoing primary total knee arthroplasty for rheumatoid arthritis. A Merchant view of the patella is shown in Figure 16. What is the most likely cause of her pain?

Explanation
Patellar complications commonly occur after primary total knee arthroplasty; therefore, proper component positioning is critical in obtaining a successful result. This patient has lateral tilting and subluxation of the patellar component. Internal rotation of the femoral component has the most deleterious effect on patellar tracking. Lateral placement of the femoral component, medial placement of the patellar component, and external rotation of the tibial component have beneficial effects on patellar tracking. Elevation of the joint line, if not excessive, should not impact patellar tracking. Rand JA: Patellar resurfacing in total knee arthroplasty. Clin Orthop 1990;260:110-117.
Question 59
The anterior portal of a hip arthroscopy places what structure at greatest risk for injury?
Explanation
The average location of the anterior portal is 6.3 cm distal to the anterior superior iliac spine. The lateral femoral cutaneous nerve typically has divided into three or more branches at the level of the anterior portal. The portal usually passes within several millimeters of the most medial branch. Injury to the nerve can lead to meralgia paresthetica. The femoral nerve lies an average minimum distance of 3.2 cm from the anterior portal. The ascending branch of the lateral circumflex artery lies approximately 3.7 cm inferior to the anterior portal. Neither the ascending branch of the medial circumflex artery nor the superior gluteal nerve are at risk. Byrd JWT: Operative Hip Arthroscopy. New York, NY, Thieme Medical Publishers, 1998, pp 83-91.
Question 60
Figure 17 shows the radiograph of an 80-year-old woman who has left groin pain. She underwent a total hip arthroplasty 15 years ago and has no history of hip dislocation; however, she now reports that the pain results in functional impairment. Preoperative findings reveal that the component used has been discontinued, the locking mechanism is poor, and there is no replacement polyethylene available from the company. During surgery, the acetabular component is found to be well fixed, it is in satisfactory position, and adequate access can be obtained through the screw holes in the component to debride the osteolytic cavities. What is the best course of action for revision?
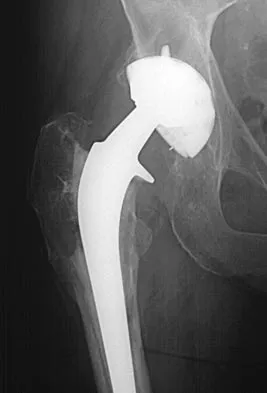
Explanation
The clinical result in this patient has been good, with no dislocations, suggesting that the components are in reasonably good position. The radiograph and examination at the time of surgery suggest that the acetabular component is well fixed. The surrounding bone of the acetabulum is osteopenic and there would most likely be considerable bone loss if the acetabular component is removed. Access to the osteolytic lesions is possible. Cementing an acetabular component into the retained socket will cause the least amount of bone loss, shorten the procedure, and most likely result in a functional hip. Maloney WJ: Socket retention: Staying in place. Orthopedics 2000;23:965-966.
Question 61
The need for postoperative allogeneic blood transfusions after total hip arthroplasty has been shown to be reduced when using
Explanation
In a prospective study, 216 patients were randomized into three groups consisting of low-dose preoperative erythropoietin, high-dose preoperative erythropoietin, and placebo control. All patients were treated for 4 weeks prior to total hip arthroplasty. Both the low- and high-dose erythropoietin groups had a significantly lower rate of blood transfusions (p < 0.001) after surgery. Waddell JP: Evidence-based orthopedics. J Bone Joint Surg Am 2001;83:788.
Question 62
Which of the following is considered a major characteristic of hyaluronate?
Explanation
Hyaluronate is a naturally occurring compound that is the backbone of the central core of the proteoglycan aggregate. Cartilage is made of two principal tissue structures. The connective tissue component includes collagen, which forms the framework for structural strength and elasticity. The proteoglycan aggregate provides a unique property of water incorporation and friction reduction capabilities. Hyaluronate forms the base or central core of the aggregate on which a link protein binds a protein core. Chondroitin sulfate and keratin sulfate are then bound to this protein core, forming the terminal extension of the aggregate. Callaghan JJ, Dennis DA, Paprosky WA, Rosenberg AG (eds): Orthopedic Knowledge Update: Hip and Knee Reconstruction. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1995, pp 69-78. Felson DT: Osteoarthritis. Rheum Dis Clin North Am 1990;16:499-512.
Question 63
Which of the following is considered an important factor in improved cemented femoral stem survivorship?
Explanation
Cement technique, relative stem to canal size and position, stem design, surgical technique, and femoral anatomy are important factors in cemented stem survivorship. Varus stem position, a wide diaphyseal to metaphyseal ratio (stovepipe femur), thin cement mantles (1 mm or less), and nonrounded femoral stem designs are negative prognostic factors for stem survivorship. Precoating with methylmethacrylate has not been shown to provide any increased survivorship over nonprecoated stems. Noble PC, Collier MB, Maltry JA, Kamaric E, Tullos HS: Pressurization and centalization enhance the quality and reproducibility of cement mantles. Clin Orthop 1998;355:77-89. Crowninshield RD, Brand RA, Johnston RC, Milroy JC: The effect of femoral stem cross-sectional geometry on cement stresses in total hip reconstruction. Clin Orthop 1980;146:71-77.
Question 64
An acetabular reinforcement cage is most often indicated for which of the following conditions?
Explanation
An acetabular reinforcement cage is required infrequently except when there is pelvic discontinuity in which there is no posterior column support of the acetabular cup. A larger cup inserted with cement and morselized bone graft is an effective technique for contained cavitary and anterior wall defects. Zone 1 osteolysis and a medial wall defect are essentially the same as a contained cavitary defect and can be reconstructed using cementless cups. Berry DJ, Lewallen DG, Hanssen A, Cabanela ME: Pelvic discontinuity in revision total hip arthroplasty. J Bone Joint Surg Am 1999;81:1692-1702.
Question 65
What is the most common short-term complication following femoral impaction grafting for revision total hip arthroplasty?
Explanation
Impaction grafting is an alternative for severe femoral bone deficiency; however, stem subsidence is commonly observed during the first few months. Slight subsidence is felt to be integral to the success of the procedure. Predictable bone graft incorporation and stable stem fixation have been reported in the medium-term. The incidence of periprosthetic fractures has been reported as high as 24%. Mikhail MWE, Weidenhielm L, Jazrawi LM, et al: Collarless, polished, tapered stem failure. J Bone Joint Surg Am 2000;82:1513-1514.
Question 66
Which of the following is considered the most predictive factor in determining whether a patient will need a blood transfusion after total knee arthroplasty?
Explanation
Multiple studies have shown that the preoperative hemoglobin level is the most predictive factor in determining whether a transfusion will be necessary after total hip or total knee arthroplasty. Studies have not shown any correlation with the other options. Salido JA, Marin LA, Gomez LA, Zorrilla P, Martinez C: Preoperative hemoglobin levels and the need for transfusion after prosthetic hip and knee surgery: Analysis of predictive factors. J Bone Joint Surg Am 2002;84:216-220. Sculco TP, Gallina J: Blood management experience: Relationship between autologous blood donation and transfusion in orthopedic surgery. Orthopedics 1999;22:S129-S134.
Question 67
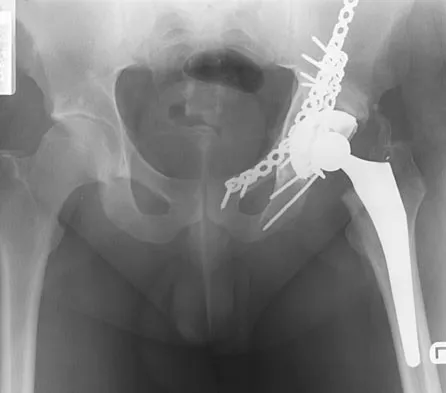
A 32-year-old man has posttraumatic arthritis after undergoing open reduction and internal fixation of a left acetabular fracture. A total hip arthroplasty is performed, and the radiograph is shown in Figure 18. What is the most common mode of failure leading to revision in this group of patients?
Explanation
Acetabular component loosening has been reported as the most common mode of failure following total hip arthroplasty in patients with a previous acetabular fracture. Following acetabular fracture and subsequent open reduction and internal fixation, the bone quality and vascularity are compromised, thus reducing the success rate of acetabular component cementless fixation. Jimenez ML, Tile M, Schenk RS: Total hip replacement after acetabular fracture. Orthop Clin 1997;28:435-446.
Question 68
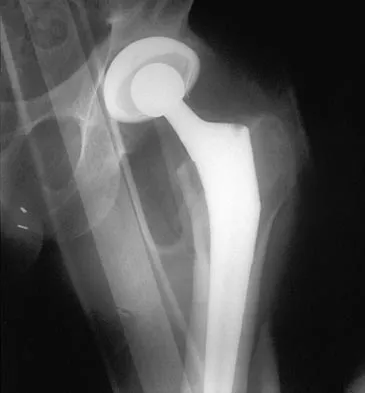
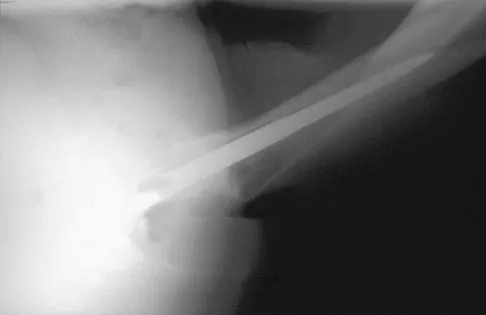
A 42-year-old man sustained the periprosthetic fracture shown in Figures 19a and 19b. The femoral component is well fixed. What is the next most appropriate step in management?
Explanation
The patient has a periprosthetic fracture below the femoral stem. The component is porous coated and well fixed. Open reduction and internal fixation, leaving the stem in place, can be performed when bone quality is good. Plating with or without allograft struts and supplemental cerclage fixation generally is acceptable. If the component is loose, revision to a longer device is recommended with appropriate stabilization of the fracture using the aforementioned methods. If bone loss has occurred, allograft supplementation or a tumor prosthesis may be indicated. Fractures located well below the stem tip can be treated without regard for the prosthesis. Closed reduction and bracing is not associated with good results for periprosthetic femoral fractures. Retrograde intramedullary nailing is not appropriate for this fracture. Duncan CP, Masri BA: Fractures of the femur after hip replacement. Instr Course Lect 1995;44:293-304.
Question 69
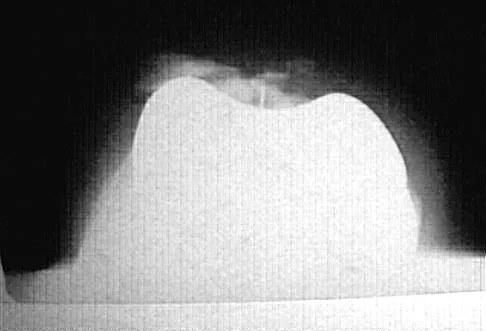
A 58-year-old man has anterior knee pain after undergoing total knee arthroplasty for osteoarthritis 2 years ago. He denies any history of trauma. A Merchant view is shown in Figure 20. What is the most likely cause of his pain?
Explanation
The patient has a patellar stress fracture after resurfacing in a total knee arthroplasty. Several studies have shown that over-resection of the patella to less than 12 to 15 mm increases anterior patellar surface strains to a point where the risk of fracture is increased. Increasing the patellar thickness, positioning of the femoral component, lateral releases, and component types have not been clearly associated with increased fracture risk. Reuben JD, McDonald CL, Woodard PL, Hennington LJ: Effect of patella thickness on patella strain following total knee arthroplasty. J Arthroplasty 1991;6:251-258. Hsu HC, Luo ZP, Rand JA, An KN: Influence of patellar thickness on patellar tracking and patellofemoral contact characteristics after total knee arthroplasty. J Arthroplasty 1996;11:69-80.
Question 70
A 30-year-old patient has acetabular dysplasia and moderate secondary osteoarthrosis. Which of the following studies will best help predict the success of periacetabular osteotomy?
Explanation
Improvement in the appearance of the hip joint on functional radiographic evaluation (abduction/adduction views) has been shown to be predictive of outcome following joint preserving surgery. CT and MRI findings have not been shown to be predictive of outcome.
Question 71
Which of the following is considered a specific advantage of using COX-2 inhibitors over COX-1 inhibitors?
Explanation
Inflammation is mediated through two isoforms of cyclooxygenase that convert arachidonic acid to prostaglandins. Selectivity, but not specificity, is one of the unique characteristics of this process that has been able to provide more protection from the effects of gastric mucosal alterations using the COX-2 selective inhibitors. The use of COX-1 selective inhibitors is associated with side effects such as ulcerative conditions and platelet interference, both of which have been difficult to control in the past until the advent of the COX-2 inhibitors. PGE2 inhibition by COX-1 in the intestinal track can then be bypassed, thereby reducing ulceration complications associated with use of nonsteroidal anti-inflammatory drugs. Lane JM: Anti-inflammatory medications: Selective COX-2 inhibitors. J Am Acad Orthop Surg 2002;10:75-78. Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002.
Question 72
Which of the following is not a reported mode of failure for a constrained acetabular component?
Explanation
There is no evidence of increased polyethylene wear in constrained acetabular components. The rates of wear appear to be the same using standard or constrained liners. Lachiewicz PF, Kelley SS: Constrained components in total hip arthroplasty. J Am Acad Orthop Surg 2002;10:233-238. Anderson MJ, Murray WR, Skinner HB: Constrained acetabular components. J Arthroplasty 1994;9:17-23.
Question 73
Which of the following factors is most likely to be associated with prolonged survival of total knee arthroplasty?
Explanation
In a survivorship study of 9,200 total knee arthroplasties, Rand and Ilstrup identified four independent variables associated with a significantly lower risk of failure: primary total knee arthroplasty, diagnosis of rheumatoid arthritis, age of 60 years or older, and use of a condylar prosthesis with a metal-backed tibial component. Other clinical studies report the use of a posterior stabilized prosthesis to be comparable to a total condylar prosthesis with retained posterior cruciate ligament. Rand JA, Ilstrup DM: Survivorship analysis of total knee arthroplasty: Cumulative rates of survival of 9200 total knee arthroplasties. J Bone Joint Surg Am 1991;73:397-409. Stern SH, Insall JN: Posterior stabilized prosthesis: Results after follow-up of nine to twelve years. J Bone Joint Surg Am 1992;74:980-986.
Question 74
Analysis of primary total hip arthroplasty using press-fit acetabular components without supplementary screw fixation reveals that screw fixation
Explanation
Using mechanical failure of fixation as the end point, Udomkiat and associates demonstrated a 12-year survivorship of 99.1% for titanium press-fit acetabular components without supplementary screw fixation. This study suggests that it is unlikely that the use of supplementary screws would lead to improved results. In addition, polyethylene wear debris tends to migrate through screw holes and along the course of screws. Screw holes also decrease the available surface for bone ingrowth. Screws that back up may be a source of backside polyethylene wear. This suggests that screw holes and the use of screws should be avoided when they are unnecessary for cup fixation.
Question 75
Dislocation following primary total hip arthroplasty is more likely to occur in which of the following situations?
Explanation
Dislocation following total hip arthroplasty is twice as common in women than in men. It is more likely to occur in older patients. There is no clear association between dislocation and the method of fixation or the type of bearing, so long as the bearing diameter is the same.
