HY 2026
00:00
Start Quiz
Question 701
High Yield
A healthy 70-year-old man has a swollen knee after undergoing a knee replacement 10 years ago. Aspiration of the knee reveals cloudy, viscous synovial fluid. Laboratory studies show an erythrocyte sedimentation rate of 10 mm/h and a C-reactive protein level of less than 0.5. What is the most likely diagnosis?
Detailed Explanation
Polyethylene wear debris can result in significant synovitis and subsequent cloudy appearing synovial fluid. Typically, laboratory studies show a WBC of less than 30,000/mm3 no left shift. Cytologic examination can reveal intra-articular polyethylene particles. Infected total knee arthroplasty is extremely uncommon in a healthy, immune-competent patient who has a normal preoperative erythrocyte sedimentation rate and C-reactive protein level.
Question 702
High Yield
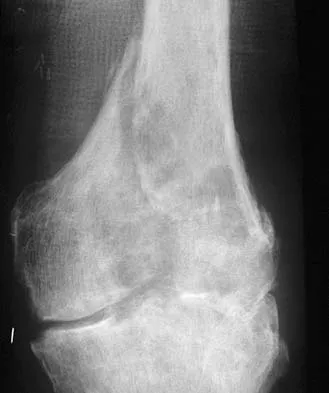
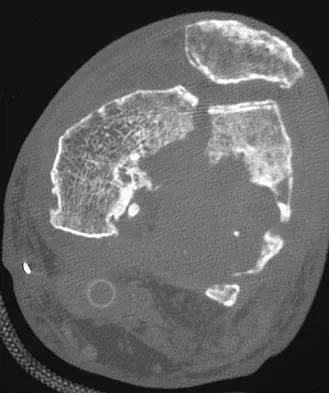
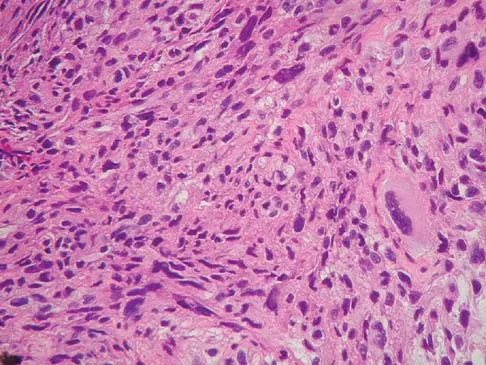
Figures 56a through 56c show the radiograph, CT scan, and biopsy specimen of a 44-year-old man who underwent chemotherapy and radiation therapy for lymphoma of the distal femur 20 years ago. His current problem is most likely related to
Detailed Explanation
The patient has changes consistent with radiation therapy to the femur, including osteopenia and an aggressive appearing neoplasm. The tumor is most likely a radiation-induced sarcoma. This is more likely than recurrent lymphoma at this late date. It is not related to steroid use or a primary lung tumor. Mirra J (ed): Bone Tumors: Clinical, Radiologic and Pathologic Correlations. Philadelphia, PA, Lea and Febiger, 1989, p 353.
Question 703
High Yield
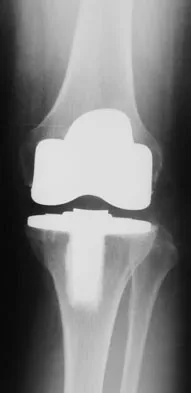
Figures 57a through 57c show the radiographs of a patient who has pain, discomfort, and a popping sensation localized to the posterior aspect of the knee after undergoing primary left total knee arthroplasty 6 months ago. Examination reveals that the patient is able to ambulate without a limp. There is no significant swelling, erythema, or effusion. Range of motion is 0 degrees to 115 degrees, and a palpable crepitation or snapping is detected at the posterior lateral joint line. What is the most likely diagnosis?

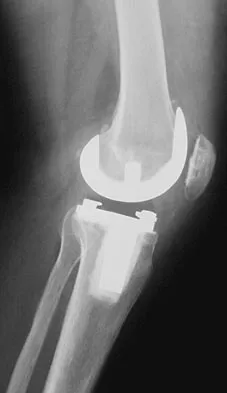
Detailed Explanation
Popliteal snapping syndrome represents the most likely diagnosis. Barnes and Scott noted that the popliteus tendon can be a potential source of internal derangement after total knee arthroplasty. They noted that it can be subluxated anteriorly and posteriorly over a retained lateral femoral condyle osteophyte. Allardyce and associates described the condition as a popliteus condition, snapping as it rolls over a retained lateral femoral condylar osteophyte. Patellar clunk syndrome is a distinct syndrome associated with the patella and has been reported in posterior stabilized knees. In addition to crepitation with range of motion, the patella literally snaps or jumps as the knee is taken from flexion to extension. Beight JL, Yao B, Hozack WJ, et al: The patellar "clunk" syndrome after posterior stabilized total knee arthroplasty. Clin Orthop 1994;299:139-142. Barnes CL, Scott RD: Popliteus tendon dysfunction following total knee arthroplasty. J Arthroplasty 1995;10:543-545.
Question 704
High Yield
The specificity of intraoperative frozen sections obtained for the evaluation of infected total hip arthroplasty may be improved by
Detailed Explanation
Lonner and associates conducted a prospective study to determine the reliability of analysis of intraoperative frozen sections for the identification of infection during 175 consecutive revision total joint arthroplasties (142 hips and 33 knees). The mean interval between the primary arthroplasty and the revision arthroplasty was 7.3 years (range, 3 months to 23 years). Of the 175 patients, 23 had at least 5 polymorphonuclear leukocytes per high-powered field on analysis of the frozen sections and were considered to have an infection. Of these 23 patients, five had 5 to 9 polymorphonuclear leukocytes per high-powered field and 18 had at least 10 polymorphonuclear leukocytes per high-powered field. The frozen sections for the remaining 152 patients were considered negative. On the basis of cultures of specimens obtained at the time of the revision surgery, 19 of the 175 patients were considered to have an infection. Of the 152 patients who had negative frozen sections, three were considered to have an infection on the basis of the results of the final cultures. Of the 23 patients who had positive frozen sections, 16 were considered to have an infection on the basis of the results of the final cultures; all 16 had frozen sections that showed at least 10 polymorphonuclear leukocytes per high-powered field. The sensitivity and specificity of the frozen sections were similar regardless of whether an index of 5 or 10 polymorphonuclear leukocytes per high-powered field was used. Analysis of the frozen sections had a sensitivity of 84% for both indices, whereas the specificity was 96% when the index was 5 polymorphonuclear leukocytes and 99% when it was 10 polymorphonuclear leukocytes. However, the positive predictive value of the frozen sections increased significantly (P < 0.05), from 70% to 89%, when the index increased from 5 to 10 polymorphonuclear leukocytes per high-powered field. The negative predictive value of the frozen sections was 98% for both indices. At least 10 polymorphonuclear leukocytes per high-powered field was predictive of infection, while 5 to 9 polymorphonuclear leukocytes per high-powered field was not necessarily consistent with infection. Less than 5 polymorphonuclear leukocytes per high-powered field reliably indicated the absence of infection. Feldman DS, Lonner JH, Desai P, Zuckerman JD: The role of intraoperative frozen sections in revision total joint arthroplasty. J Bone Joint Surg Am 1995;77:1807-1813. Lonner JH, Desai P, Dicesare PE, Steiner G, Zuckerman JD: The reliability of analysis of intraoperative frozen sections for identifying active infection during revision hip or knee arthroplasty. J Bone Joint Surg Am 1996;78:1553-1558. Spangehl MJ, Younger AS, Masri BA, Duncan CP: Diagnosis of infection following total hip arthroplasty, in Cannon WD Jr (ed): Instructional Course Lectures 47. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 285-295.
Question 705
High Yield
A 21-year-old professional baseball player has had painful catching and stiffness in his dominant right elbow for the past year. Examination reveals a flexion contracture of 2 degrees and mild pain with full elbow flexion. Radiographs are shown in Figures 33a and 33b. The most effective management should consist of
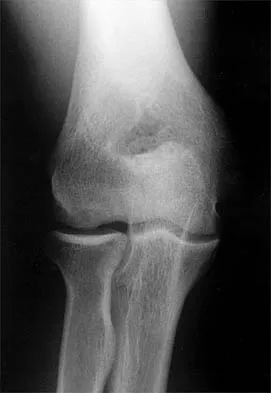
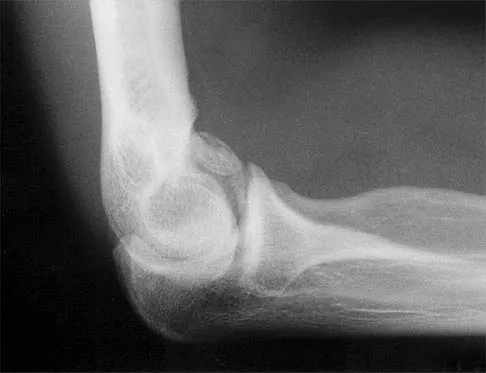
Detailed Explanation
The radiographs show osteochondritis dissecans of the capitellum and a loose body in the anterior compartment. Arthroscopic removal is indicated because symptoms referable to the loose body are present. Baumgarten TE: Osteochondritis dissecans of the capitellum. Sports Med Arthroscopy Rev 1995;3:219-223.
Question 706
High Yield
Figure 45 shows the current radiograph of an 11-year-old girl who sustained a simple nondisplaced fracture of the distal radius 4 weeks ago. Management at the time of injury consisted of application of a short arm cast but no manipulation. What is the major concern at this time?
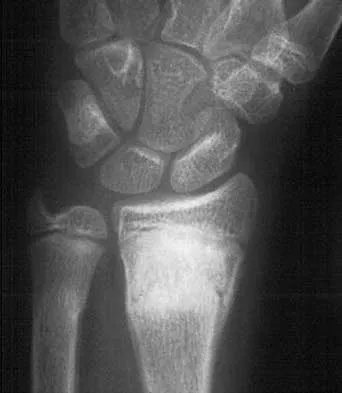
Detailed Explanation
The fracture pattern represents a Peterson type I physeal injury, which is a comminuted metaphyseal fracture in which the fracture lines extend up to the physis. Because there is no displacement of the physis and the fracture lines do not cross the physis, there may be a tendency to dismiss this injury as a simple metaphyseal fracture with no significant sequelae. A small percentage of patients (3% in Peterson's series) experience growth arrest. In this patient, a disabling ulnar plus deformity, defined as increased ulnar length in relationship to the distal radius, developed. Peterson HA: Physeal fractures: Part 2. Two previously unclassified types. J Pediatr Orthop 1994;14:431-438.
Question 707
High Yield
A 50-year-old laborer sustained an isolated closed injury to his heel after falling 11 feet off a wall. A radiograph and a CT scan are shown in Figures 4a and 4b. To minimize the patient's temporary disability and allow him to return to work most rapidly, management should consist of
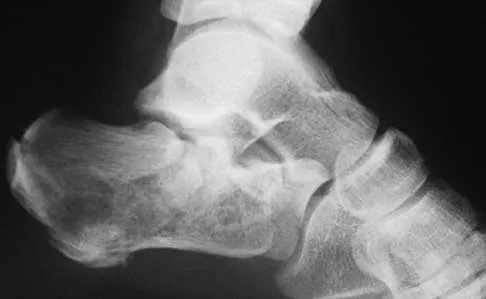
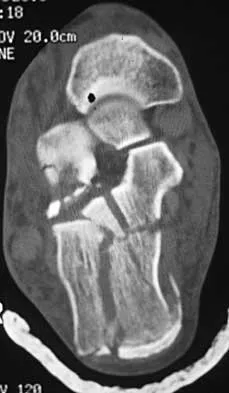
Detailed Explanation
With a severe articular injury to the calcaneus, the ability to achieve satisfactory results with open reduction and internal fixation diminishes. An arthrodesis is often needed to allow a person who works as a laborer to return to work. Recent literature suggests that this can be successfully performed primarily, improving the odds of an earlier return to the labor force at 1 year. Huefner T, Thermann H, Geerling J, Pape HC, Pohlemann T: Primary subtalar arthrodesis of calcaneal fractures. Foot Ankle Int 2001;22:9-14. Coughlin MJ: Calcaneal fractures in the industrial patient. Foot Ankle Int 2000;21:896-905.
Question 708
High Yield
A 35-year-old runner has pain beneath the second metatarsophalangeal joint. He reports that he has significantly decreased his running distance since the onset of the pain. He denies any history of trauma or injury to the foot. A radiograph is shown in Figure 14. Initial management should consist of
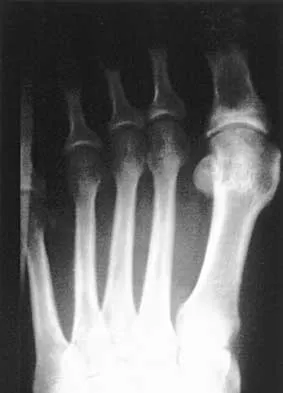
Detailed Explanation
The presence of the relatively long second metatarsal, along with the close approximation of the second and third metatarsal heads, are consistent with second metatarsophalangeal tenosynovitis. The hallmark of initial management is conservative. Modalities include taping, nonsteroidal anti-inflammatory drugs, metatarsal pads, and cortisone injections. Trepman and Yeo combined the use of a cortisone injection with a rocker bottom sole. Mizel and Michelson reported their results using an extended rigid steel shank shoe along with a cortisone injection. Trepman E, Yeo SJ: Nonoperative treatment of metatarsophalangeal joint synovitis. Foot Ankle Int 1995;16:771-777.
Question 709
High Yield
In Gustilo type III open tibial diaphyseal fractures, which of the following factors is associated with an increased risk of a poor functional outcome?
Detailed Explanation
According to the published outcomes analyses from the Lower Extremity Assessment Project (LEAP) study group of patients prospectively followed for 2 to 7 years, definitive fixation with an intramedullary nail has shown improved outcomes when compared to definitive external fixation. The findings showed that the timing of wound debridement (within 6 hours from injury as compared to within 6 to 24 hours), the timing of soft-tissue coverage (3 days or less from injury as compared to more than 3 days), and the timing of bone grafting after injury (within or after 3 months) did not impact the infection or union rates and had no effect on functional outcome. The LEAP study has shown at 7-year follow-up that patients who are definitively treated with external fixation have a significantly longer time to union, poorer functional outcomes, longer time to achieve full weight bearing, and more time in the hospital.
Question 710
High Yield
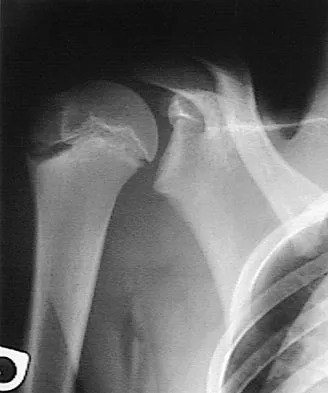
Figure 5 shows the radiograph of a 10-year-old girl who reports chronic shoulder pain after her gymnastics classes. Examination reveals pain on internal and external rotation but no instability. What is the most likely diagnosis?
Detailed Explanation
The patient has a very wide humeral growth plate, indicating the presence of a proximal humeral stress fracture, an uncommon diagnosis in gymnasts. Gymnasts are prone to stress fractures of the scaphoid, distal radius, elbow, and clavicle. Proximal humeral stress fractures are more commonly seen in those participating in racket or throwing sports. Stress fractures can lead to growth arrest or inhibition, particularly in the distal radius. The radiograph shows normal findings for the acromion, acromioclavicular joint, scapula, and triceps origin. Fallon KE, Fricker PA: Stress fracture of the clavicle in a young female gymnast. Br J Sports Med 2001;35:448-449. Sinha AK, Kaeding CC, Wadley GM: Upper extremity stress fractures in athletes: Clinical features of 44 cases. Clin J Sports Med 1999;9:199-202. Caine D, Howe W, Ross W, Bergman G: Does repetitive physical loading inhibit radial growth in female gymnasts? Clin J Sports Med 1997;7:302-308.
Question 711
High Yield
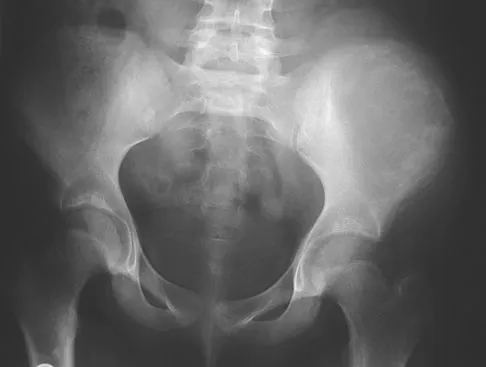
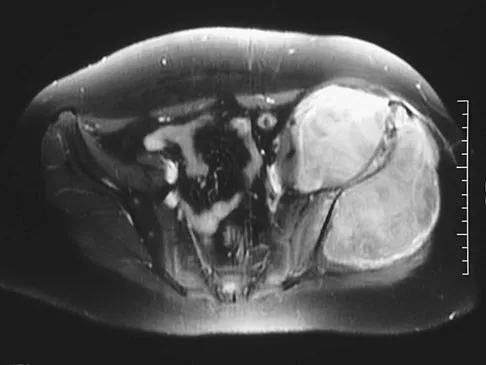
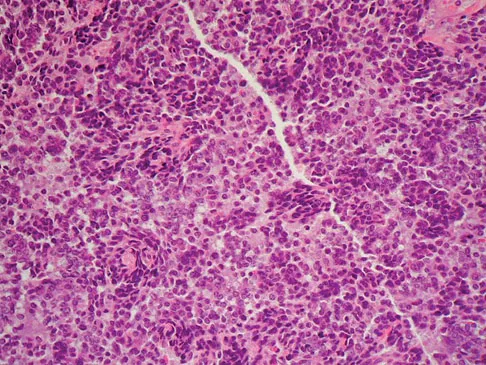
A 13-year-old girl has had increasing left hip pain for the past 4 months. A radiograph, bone scan, MRI scan, and photomicrograph are shown in Figures 1a through 1d. Which of the following immunohistochemistry results would confirm the most likely diagnosis?

Detailed Explanation
The imaging studies show a permeative lesion of the left hemipelvis with a large soft-tissue mass. The photomicrograph demonstrates a small blue cell tumor with pseudorosettes. The most likely diagnosis is primitive neuroectodermal tumor (Ewing's sarcoma family of tumors). MIC-2 is a highly sensitive and specific marker for this family of tumors. Cytokeratin is an epithelial marker. Vimentin is a mesenchymal marker. Thus, Ewing's sarcomas are cytokeratin negative and vimentin positive. Before discovery of the MIC-2 antigen, PAS and reticulin stains were commonly used to help differentiate Ewing's sarcoma from lymphoma. In contrast to lymphoma, Ewing's sarcomas are typically PAS positive and reticulin negative. Halliday BE, Slagel DD, Elsheikh TE, et al: Diagnostic utility of MIC-2 immunocytochemical staining in the differential diagnosis of small blue cell tumors. Diagn Cytopathol 1998;19:410-416.
Question 712
High Yield
Figure 21 shows the tomogram of a 26-year-old woman who sustained an axial load injury to her neck in a fall off a horse. What ligament is injured?

Detailed Explanation
Levine and Edwards, in their description of the classic C1 burst (Jefferson) fracture, noted that spread of the lateral masses of more than 7 mm is indicative of a transverse ligament rupture. Long-term C1-C2 instability, however, has not been described with this fracture pattern. Although long-term traction followed by halo vest immobilization has been described as the best technique for achieving an ideal result, treatment of this injury remains somewhat controversial. Levine AM, Edwards CC: Fractures of the atlas. J Bone Joint Surg Am 1991;73:680-691.
Question 713
High Yield
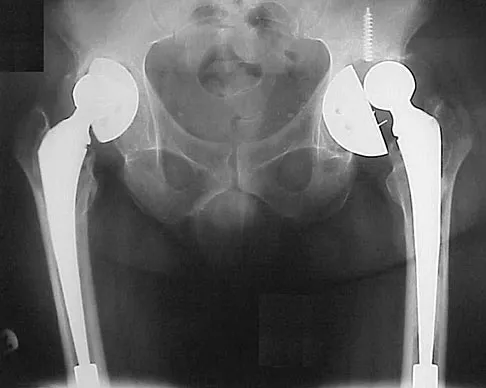
A 59-year-old woman who underwent a total hip arthroplasty 5 years ago now has recurrent dislocation following bariatric surgery and a weight loss of 200 lb. An attempt at converting to a larger head size and trochanteric advancement has failed. Her components are well aligned. What is the best course of action?
Detailed Explanation
When a patient has well-aligned components and soft-tissue tensioning with a larger femoral head and trochanteric advancement has failed, options are limited. The use of a constrained acetabular liner is the best option in this situation. Goetz and associates and Shrader and associates have demonstrated good results with these implants. Shrader used this device on 109 patients with recurrent instability with a successful outcome in all but 2 patients. Resection arthroplasty is a salvage situation and is not the best option at the present time. A hip abduction brace does not address the soft-tissue laxity. Conversion to a bipolar arthroplasty, although possibly minimizing the incidence of dislocation, will lead to groin pain and migration of the component with diminished functional results. Goetz DD, Capello WN, Callaghan JJ, et al: Salvage of recurrently dislocating hip prosthesis with use of a constrained acetabular component: A retrospective analysis of fifty-six cases. J Bone Joint Surg Am 1998;80:502-509. Shrader MW, Parvizi J, Lewallen DG: The use of constrained acetabular component to treat instability after total hip arthroplasty. J Bone Joint Surg Am 2003;85:2179-2183.
Question 714
High Yield
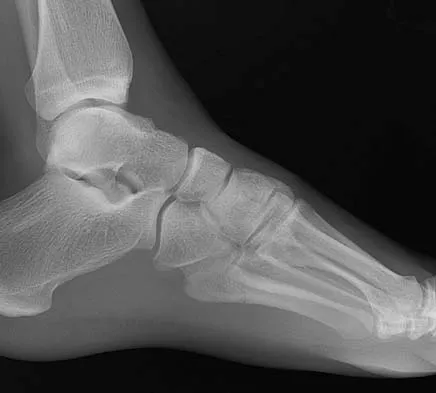
A 4-year-old girl sustains an isolated spiral femoral fracture after falling from her tricycle. Management should consist of
Detailed Explanation
Immediate spica casting is ideal for younger children with uncomplicated femoral fractures that are the result of relatively low-energy injury. Surgical stabilization of pediatric femoral fractures is most commonly performed in children who are older than age 6 years or in children with other factors associated with their femoral fracture, such as concomitant head injury, open fracture, floating knee, severe comminution, or vascular injury. Flynn JM, Skaggs DL, Sponseller PD, et al: The surgical management of pediatric fractures of the lower extremity. Instr Course Lect 2003;52:647-659. Sponseller PD: Surgical management of pediatric femoral fractures. Instr Course Lect 2002;51:361-365. Wright JG: The treatment of femoral shaft fractures in children: A systematic overview and critical appraisal of the literature. Can J Surg 2000;43:180-189.
Question 715
High Yield
A 46-year-old woman reports pain and a shortened appearance of her toe after undergoing a Keller resection arthroplasty 2 years ago for hallux rigidus. Examination reveals mild swelling and motion limited to 25 degrees at the metatarsophalangeal joint. Radiographs show large dorsal osteophytes on the first metatarsal head, 50% resection of the proximal phalanx, and complete loss of the metatarsophalangeal joint space. Which of the following is considered the most reliable procedure to improve her pain and the appearance of her toe?
Detailed Explanation
Because the patient has significant arthritis, arthrodesis is the treatment of choice. Adding a bone graft will prevent further shortening and add length to her toe, resulting in improved cosmesis. A cheilectomy will not alleviate her arthritis pain. The toe is too short for an effective Moberg phalangeal dorsiflexion osteotomy. A Waterman first metatarsal dorsal osteotomy will not address the degenerative joint disease or shortening. Silastic arthroplasty may help, but there is the risk of additional problems with foreign body reaction and a significant risk of failure known to occur with Silastic materials. Myerson MS, Schon LC, McGuigan FX, Oznur A:Result of arthrodesis of the hallux metatarsophalangeal joint using bone graft for restoration of length. Foot Ankle Int 2000;21:297-306. Mann RA, Coughlin MJ: Adult hallux valgus, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, pp 252-253.
Question 716
High Yield
The additional risk of complications in organ transplant patients receiving a total joint arthroplasty is attributed to
Detailed Explanation
Tannenbaum and associates found that patients who had a joint replacement after an organ transplantation had a rate of infection of 19% (five of 27 joint replacements in 16 patients). They retrospectively reviewed the results of 35 joint (hip or knee) replacements in 19 patients who had an organ transplant. The patients received a standard immunosuppressive induction regimen at the time of the transplantation and were maintained on a combination of prednisone, azathioprine, and cyclosporin A. All patients received antibiotics perioperatively, but antibiotic-impregnated bone cement was not used for any procedure. Six joint replacements in three patients (median patient age of 48.2 years at the time of the arthroplasty) were performed before a renal transplantation. Twenty-four joint replacements in 14 patients (average patient age of 40.9 years at the time of the arthroplasty) were performed after an organ transplantation. Two patients, with an average age of 53.8 years at the time of the arthroplasty, each had a joint replacement both before and after a liver transplantation (a total of five joint replacements). The average duration of follow-up after the first joint replacement was 8.8 years (range, 1 to 23 years). An infection developed around the implant in five patients who had undergone the joint replacement after a transplantation. The average interval from implantation of the prosthesis until detection of the infection was 3.4 years (range, 1 to 6 years). Of two patients who underwent a liver transplant, one had Pseudomonas aeruginosa infection and the other Escherichia coli infection. Of three patients who underwent a renal transplantation, one was infected with Staphylococcus epidermidis, one with Enterococcus, and one with Serratia marcescens.
Question 717
High Yield
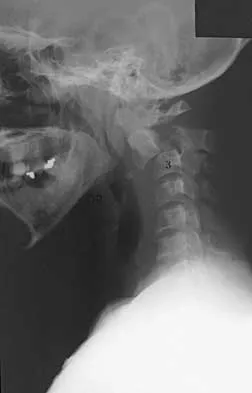
A 27-year-old man has neck pain after being involved in a motor vehicle accident. A lateral cervical radiograph is shown in Figure 21. What would be the most common neurologic finding?
Detailed Explanation
The radiographic findings are consistent with a type II Hangman's fracture or traumatic spondylolisthesis of C2. This occurs with more than 3 mm of displacement according to the classification of Levine and Edwards. Even though the radiograph reveals significant displacement, the overall space available for the neural elements is increased, therefore minimizing the risk of neural compromise. Neurologic injury is most frequently encountered in type III injuries that are associated with bilateral facet dislocations of C2 on C3 but is infrequent in type I (less than 3 mm displacement) and type II traumatic spondylolisthesis. When neurologic deficits are associated with type II injuries, it is usually the result of an associated head injury. Cruciate paralysis occurs as a result of the crossover of the motor and sensory tracts at different levels of the cord at the C1-C2 junction. This results in normal sensation but complete loss of motor function. Levine AM: Traumatic spondylolisthesis of the axis (Hangman's fracture), in Levine AM, Eismont FJ, Garfin S, Zigler JE (eds): Spine Trauma. Philadelphia, PA, WB Saunders, 1998, pp 287-288.
Question 718
High Yield
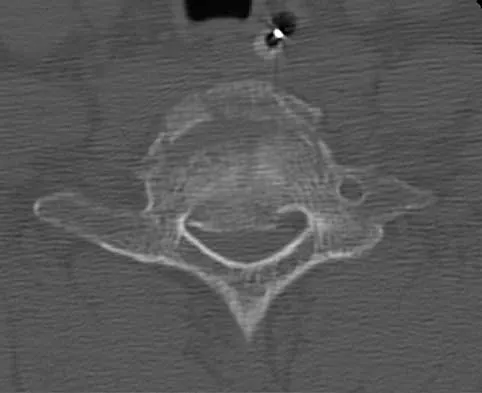
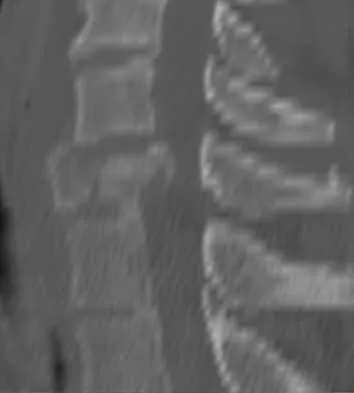
A 33-year-old woman sustains a C6 burst fracture diving into a swimming pool, resulting in a complete spinal cord injury. The canal compromise is shown in Figures 8a and 8b. Functional recovery would be maximized with
Detailed Explanation
Although the patient has sustained a complete spinal cord injury, an anterior decompression, even performed late, can gain an additional level of root function. In the quadriplegic patient, this can mean the difference between dependent and independent function. Posterior procedures do not afford adequate access to the retropulsed bony fragments compromising the canal. Bohlman HH, Anderson PA: Anterior decompression and arthrodesis of the cervical spine: Long-term motor improvement. Part I: Improvement in incomplete traumatic quadriparesis. J Bone Joint Surg Am 1992;74:671-682.
Question 719
High Yield
An eversion mechanism of injury is associated with which of the following ankle conditions?
Detailed Explanation
An inversion ankle injury typically involves ligamentous damage to the lateral ligaments of the ankle to include the anterior talofibular ligament and calcaneofibular ligament. Acute and particularly chronic ankle sprains also can have associated injuries. The inversion mechanism has been implicated in osteochondral and transchondral talar dome lesions, producing splits in the peroneus tendons, and in the development of meniscoid and soft-tissue impingement lesions in the anterolateral ankle. An inversion mechanism can also stretch the superficial peroneal nerve, leading to pain and paresthesias along its distribution. A fracture of the anterior colliculus is typically the result of an eversion mechanism resulting in a bony avulsion of the deltoid ligament from the anterior colliculus of the medial malleolus. Casillas MM: Ligament injuries of the foot and ankle in the athlete, in DeLee JC, Drez D, Miller MD (eds): Orthopaedic Sports Medicine: Principles and Practice, ed 2. Philadelphia, PA, WB Saunders, 2003, pp 2323-2357.
Question 720
High Yield
The brachialis muscle is innervated by what two nerves?
Detailed Explanation
The brachialis is innervated by two nerves: medially, the musculocutaneous nerve; laterally, the radial nerve. The muscle is split longitudinally to approach the humerus anteriorly. Henry AK: The distal part of the humerus and front of the forearm, in Henry AK (ed): Extensile Exposure, ed 2. Edinburgh, UK, Churchill Livingstone, 1973, pp 90-115.
Question 721
High Yield
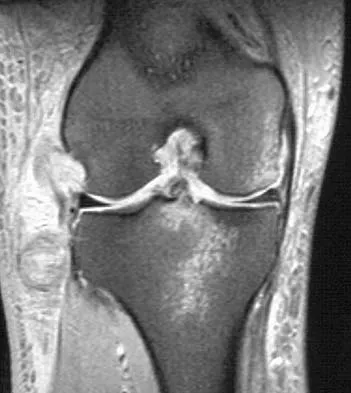
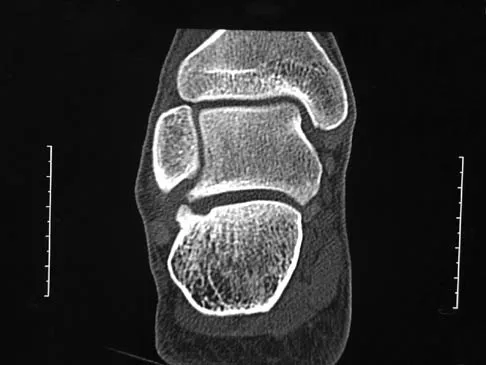
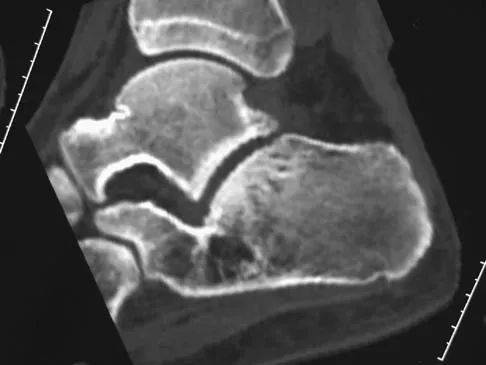
A 17-year-old patient sustained a closed calcaneal fracture when he jumped off of a roof 2 years ago, and he underwent nonsurgical management at the time of injury. The patient now reports lateral hindfoot pain that is worse with weight-bearing activities. Anti-inflammatory drugs and orthoses have failed to provide relief. Coronal and sagittal CT scans are shown in Figures 36a and 36b. What is the best course of action?
Detailed Explanation
The CT scans show evidence of a lateral wall blowout and malunion without significant arthrosis of the subtalar joint. In a young patient, it is preferable to avoid a fusion and allow residual motion by performing an exostectomy that decompresses the lateral subtalar joint and peroneal tendons. Chandler JT, Bonar SK, Anderson RB, et al: Results of in situ subtalar arthrodesis for late sequelae of calcaneus fractures. Foot Ankle Int 1999;20:18-24.
Question 722
High Yield
What neurologic structure is most at risk when performing intramedullary screw fixation of a fifth metatarsal base fracture?
Detailed Explanation
The sural nerve and its terminal branches course through the lateral hindfoot and midfoot area and are directly at risk in surgeries involving the peroneal tendon complex and the fifth metatarsal. The first branch of the lateral plantar nerve originates in the tarsal tunnel region and courses across the plantar heel area to innervate the abductor digiti minimi; it is not at direct risk with fifth metatarsal surgery. The saphenous, superficial peroneal, and deep peroneal nerves are not at risk anatomically with a lateral midfoot incision. Donley BG, McCollum MJ, Murphy GA, Richardson EG: Risk of sural nerve injury with intramedullary screw fixation of fifth metatarsal fractures: A cadaver study. Foot Ankle Int 1999;20:182-184.
Question 723
High Yield
When using the direct lateral (or Hardinge) approach for hip arthroplasty, three muscles are detached from the femur. In addition to the vastus lateralis, they include the
Detailed Explanation
This approach is criticized for the episodic limp associated with the muscle detachment and reattachment. Classically, two thirds of the gluteus medius is detached as a sleeve with the vastus lateralis. This exposes the gluteus minimus and the ligament of Bigelow. These must also be detached to allow dislocation of the hip and osteotomy of the femoral neck. The rectus femoris lies medially and anteriorly and does not need to be addressed. The piriformis and obturator internus are exposed during the posterior approach. Neither the gluteus maximus nor tensor fascia lata attach to the anterior femur. The sartorius and iliopsoas are not exposed during this dissection. Hoppenfeld S, deBoer P (eds): Surgical Exposures in Orthopaedics: The Anatomic Approach. Philadelphia, PA, JB Lippincott, 1984, pp 333-335.
Question 724
High Yield
An axillary nerve lesion may cause weakness in the deltoid and the
Detailed Explanation
While the most prominent functional deficit from axillary nerve lesions occurs from denervation of the deltoid, denervation of the teres minor also occurs.
Question 725
High Yield
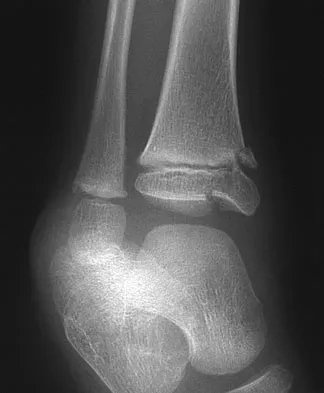
An 11-year-old boy sustained an ankle injury while playing football. Figure 20 shows an AP radiograph obtained the day of injury. Treatment should consist of
Detailed Explanation
The child has an injury involving both the growth plate and the articular surface of the ankle. Because of the significant displacement, open reduction and internal fixation is indicated to realign the physis and joint surface. The best method of fixation to avoid growth arrest is one that does not cross the physis. This is usually achieved by a transverse epiphyseal screw parallel to the physis. If the metaphyseal fragment was large enough, a transverse metaphyseal screw could be used instead. The incidence of growth arrest following physeal ankle injuries is as high as 50%, and long-term follow-up is indicated. Cass JR, Peterson HA: Salter-Harris Type-IV injuries of the distal tibial epiphyseal growth plate, with emphasis on those involving the medial malleolus. J Bone Joint Surg Am 1983;65:1059-1070.
Question 726
High Yield
Which of the following variables has been shown to have the greatest influence on the higher rate of anterior cruciate ligament (ACL) tears in women when compared to men for similar sports?
Detailed Explanation
All of the variables have been proposed as possible causes for the increased incidence of ACL tears in women versus men. The general differences in the level of neuromuscular training however, specifically conditioning and muscle strength, have been shown to play the greatest role. Harmon KJ, Ireland ML: Gender differences in noncontact anterior cruciate ligament injuries. Clin Sports Med 2000;19:287-302. Arendt EA: Knee injury patterns among men and women in collegiate basketball and soccer. Am J Sports Med 1995;23:694-701.
Question 727
High Yield
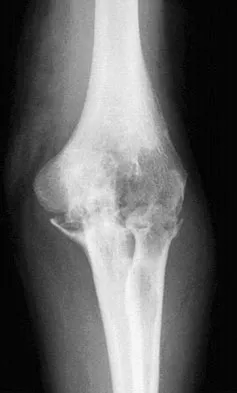
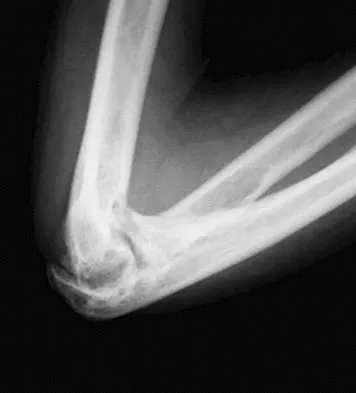
A 61-year-old woman with a long-standing history of rheumatoid arthritis reports progressive elbow pain for the past 12 months. She denies any recent trauma to the elbow; however, she notes increasing pain and decreased joint motion that are now compromising her function. Radiographs are shown in Figures 57a and 57b. What is the most appropriate treatment at this time?
Detailed Explanation
The patient has end-stage arthritis of the elbow with advanced joint destruction. At this point, nonsurgical management is unlikely to provide much relief of symptoms. Arthroscopic procedures can provide relief, but it is likely to be incomplete and unpredictable. The most reliable surgical option is total elbow arthroplasty. Currently, semiconstrained components are generally preferred because constrained components have been associated with a high rate of early prosthetic loosening. Little CP, Graham AJ, Karatzas G, et al: Outcomes of total elbow arthroplasty for rheumatoid arthritis: Comparative study of three implants. J Bone Joint Surg Am 2005;87:2439-2448.
Question 728
High Yield
Which of the following best characterizes bone mineralization?
Detailed Explanation
Mineralization occurs at the site of hole zones between the collagen fibrils. Crystals begin from the necessary ions of the lattice that come together with the correct orientation to form the first stable crystal. Formation of this critical nucleus is the most energy-demanding step of crystallization. Enzymes within the extracellular matrix vesicles degrade inhibitors such as adenosine triphosphate, pyrophosphate, and proteoglycans found in the surrounding extracellular matrix. Bone mineral consists of numerous impurities (carbonate, magnesium) that are more soluble, allowing the bone to act as a reservoir for calcium, phosphate, and magnesium ions. Crystals may form by addition of ions or ion clusters to the critical nucleus in many directions, with 'kink' sites forming to branch and exponentially proliferate the crystals. Macromolecules facilitate formation of the critical nucleus and increasing local concentrations of necessary ions. Once the crystals are formed and proliferating, macromolecules bind to the surface and block the growth of the crystal, regulating size, shape, and number of crystals. Lian JB, Stein GS, Canalis E, et al: Bone formation: Osteoblast lineage cells, growth factors, matrix proteins, and the mineralization process, in Favus MJ (ed): Primer on Metabolic Bone Diseases and Disorders of Mineral Metabolism, ed 4. Philadelphia, PA, Lippincott Williams & Wilkins, 1999, pp 14-29.
Question 729
High Yield
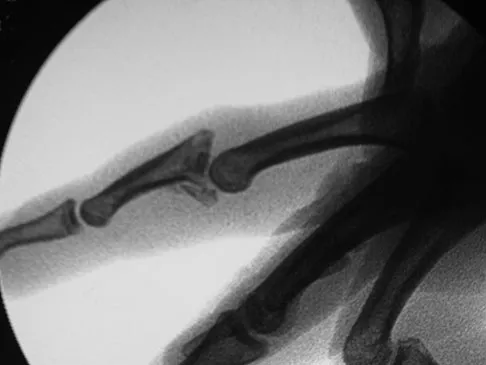
A 30-year-old woman injured the ring finger of her nondominant hand while playing baseball 5 weeks ago. She now reports pain and limited motion of the proximal interphalangeal (PIP) joint. A lateral fluoroscopy image is shown in Figure 36. Treatment of the PIP joint should consist of
Detailed Explanation
The patient has a neglected PIP joint fracture-dislocation with comminution involving more than 40% of the volar articular surface of the middle phalanx. Volar plate arthroplasty has been advocated for the treatment of acute unstable and chronic dorsal fracture-dislocations. The volar plate is incised laterally and released from the collateral ligaments. The volar fragments of the middle phalanx are removed and a trough is created for advancement of the volar plate, which is secured with sutures secured on the dorsum of the middle phalanx beneath the extensor mechanism. Dionysian E, Eaton RG: The long-term outcome of volar plate arthroplasty of the proximal interphalangeal joint. J Hand Surg Am 2000;25:429-437. Eaton RG, Malerich MM: Volar plate arthroplasty of the proximal interphalangeal joint: A review of ten years' experience. J Hand Surg Am 1980;5:260-268.
Question 730
High Yield
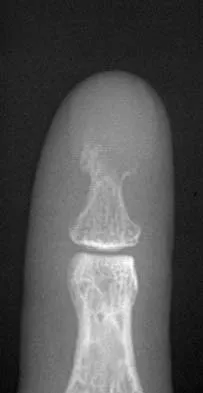
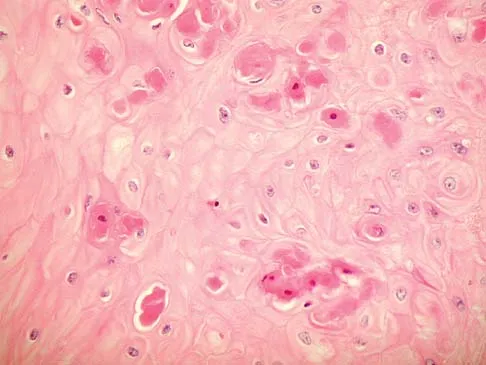
A 60-year-old man has pain at the tip of the index finger. A radiograph and biopsy specimen are shown in Figures 40a and 40b. Management should consist of
Detailed Explanation
The radiograph and histology findings are most consistent with squamous cell carcinoma. This tumor is best treated with wide surgical resection margins alone in the absence of metastasis; in this patient, management should consist of amputation through the distal interphalangeal joint. The other treatments are not indicated. Soltani K, Krunic A: Non melanoma skin neoplasms, in Vokes E, Golomb H (eds): Oncologic Therapies, ed 2. Berlin, Germany, Springer, pp 646-647.
Question 731
High Yield
What structure is most at risk with anterior penetration of C1 lateral mass screws?
Detailed Explanation
Posterior screw fixation of the upper cervical spine has gained a great deal of popularity due to its stable fixation, obviating the use of halo vest immobilization, and its high fusion rates. The use of screws in this location, however, has introduced a whole new set of potential complications. Vertebral artery injury is one of the most feared complications associated with screws in the C1/C2 region. This structure, however, is lateral and posterior at the C2 level and then penetrates the foramen transversarium of C1 to lie cephalad to the arch of C1 before entering the foramen magnum. It is the internal carotid artery that lies immediately anterior to the arch of C1 that is particularly at risk by anterior penetration of C1 lateral mass or C1-C2 transarticular screws as demonstrated by Currier and associates. The internal carotid artery lies posterior to the pharynx. The external carotid artery and the glossopharyngeal nerve are not at risk with this method of fixation. Currier BL, Todd LT, Maus TP, et al: Anatomic relationship of the internal carotid artery to the C1 vertebra: A case report of cervical reconstruction for chordoma and pilot study to assess the risk of screw fixation of the atlas. Spine 2003;28:E461-E467. Grant JC: Grant's Atlas of Anatomy, ed 6. Baltimore, MD, Williams & Wilkins, 1972.
Question 732
High Yield
Which of the following vertebrae has the smallest pedicle isthmic width in a nondeformity patient?
Detailed Explanation
The smallest pedicle isthmic width is at L1, whereas T12 has the largest pedicle width in the upper lumbar and lower thoracic spine. Although smaller in diameter than T12, both T10 and T11 have larger pedicle widths than L1.
Question 733
High Yield
What spinal nerves in the cauda equina are primarily responsible for innervation of the bladder?
Detailed Explanation
The spinal nerves primarily responsible for bladder function are the S2, S3, and S4 nerve roots. With significant compression of the cauda equina by either disk herniation, tumor, or degenerative stenosis, bladder dysfunction may result. Hoppenfeld S: Physical Examination of the Spine and Extremities. Norwalk, CT, Appleton-Century-Crofts, 1976, p 254.
Question 734
High Yield
A 29-year-old man reports severe knee instability and popliteal pain. History reveals that he had polio of the left lower extremity as a child and has been brace-free his entire life. Examination reveals that he walks with 40 degrees of knee hyperextension and has a fixed ankle equinus deformity of 30 degrees. He has no active motors about the knee or ankle. Which of the following methods will provide knee stability and pain relief?
Detailed Explanation
The ankle equinus allows the patient to keep his weight-bearing line anterior to the axis of the hyperextended knee joint. With time, pain has developed because of continued stretching and now incompetence of the posterior capsule of the knee joint. Several soft-tissue and bony procedures have been designed to provide knee stability in this situation; however, the results have been either short-lived or inconsistent. Tenodeses, capsular plications, and bony blocks have had limited success and generally fail over time. Current orthotic technology makes soft-tissue release and orthotic control the most predictable option. To decrease the hyperextension moment on the knee joint, the ankle deformity also must be corrected. The most predictable method of achieving stability and diminished pain during walking is with soft-tissue release of the ankle and a knee-ankle-foot orthosis with a locked ankle and drop-lock knee joint.
Question 735
High Yield
A 56-year-old man with a history of chronic lower back pain from lumbar spondylosis reports a 2-day history of acute incapacitating back pain. He denies any history of acute trauma, although he reports the pain starting after a coughing spell. He also reports difficulty urinating and some fecal incontinence. Examination reveals generalized lower extremity weakness, saddle paresthesia, hyporeflexia in the lower extremities, and loss of rectal tone. What is the most appropriate management at this time?
Detailed Explanation
Cauda equina syndrome is a medical emergency that must be quickly diagnosed and treated to avoid long-term complications. Cauda equina syndrome typically presents with low back pain, unilateral or usually bilateral sciatica, saddle sensory disturbances, bladder and bowel dysfunction, and variable lower extremity motor and sensory loss. Although a number of pathologies can cause cauda equina syndrome, in a patient with a history of chronic back pain, disk pathology is the most common cause of acute onset cauda equina syndrome. Whereas radiographs may be useful in a traumatic onset of symptoms, MRI is the most appropriate study. Cauda equina syndrome should be evaluated on an emergent basis and admission for work-up is appropriate. Ahn UM, Ahn NU, Buchowski JM, et al: Cauda equina syndrome secondary to lumbar disc herniation: A meta-analysis of surgical outcomes. Spine 2000;25:1515-1522.
Question 736
High Yield
A positive Froment sign indicates weakness of which of the following muscles?
Detailed Explanation
Thumb adduction is powered by the adductor pollicis (ulnar nerve). Testing involves having the patient forcibly hold a piece of paper between the thumb and radial side of the index proximal phalanx. When this muscle is weak or nonfunctioning, the thumb interphalangeal joint flexes with this maneuver, resulting in a positive Froment sign. The paper is held by action of the thumb flexion (flexor pollicis longus and flexor pollicis brevis; median innervated).
Question 737
High Yield
Figure 28 shows the postoperative radiograph of a 36-year-old patient. The cerclage cable was placed for a minimal medial calcar fracture seen during femoral preparation. In the immediate postoperative period, what is the highest level of activity that would be safely permitted?
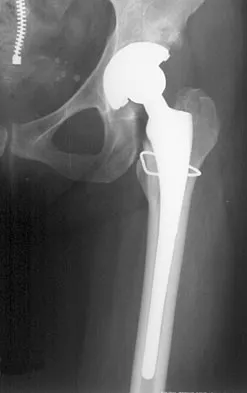
Detailed Explanation
The incidence of femoral fracture in primary cementless total hip arthroplasty ranges from 1.5% to 27.8%. It is imperative that the implant and fracture are stable both intraoperatively and postoperatively. Cerclage wiring or cerclage cabling is the current recommended treatment for nondisplaced calcar fractures and minimally displaced proximal fractures. Berend and associates reviewed the results of 58 total hips in 55 patients with intraoperative calcar fracture managed with single or multiple cerclage wires or cables and immediate full weight bearing. Follow-up averaged 7.5 years, and there were no revisions of the femoral component. No patients had severe thigh pain. Berend KR, Lombardi AV Jr, Mallory TH, et al: Cerclage wires or cables for the management of intraoperative fracture associated with a cementless, tapered femoral prosthesis: Results at 2 to 16 years. J Arthroplasty 2004;19:17-21. Schmidt AH, Kyle RF: Periprosthetic fractures of the femur. Orthop Clin North Am 2002;33:143-152.
Question 738
High Yield
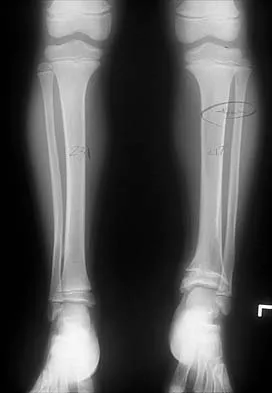
A 14-year-old boy has a midshaft fibular lesion. Biopsy results are consistent with Ewing's sarcoma. Following induction chemotherapy, local control typically consists of
Detailed Explanation
Current treatment regimens for Ewing's sarcoma typically involve induction chemotherapy followed by local control and further chemotherapy. Local control consists of surgery alone, radiation therapy alone, or a combination of the two. In bones that are easily resectable (or expendable) with wide margins, surgery alone is usually recommended. For areas that are unresectable (ie, large, bulky pelvic tumors), radiation therapy alone is sometimes the preferred method of local control. If surgery is chosen and margins are close, radiation therapy can be used as an adjuvant. Amputation rarely is required for an isolated fibular lesion. Observation without adequate local therapy results in local recurrence. Nesbit ME Jr, Gehan EA, Burgert EO Jr, et al: Multimodal therapy for the management of primary, nonmetastatic Ewing's sarcoma of bone: A long-term follow-up of the First Intergroup study. J Clin Oncol 1990;8:1664-1674.
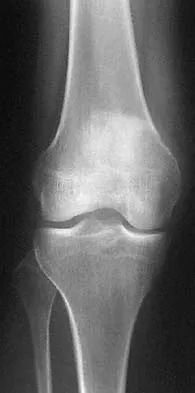
Question 739
High Yield
Examination of a 23-year-old female college basketball player who has had anterior knee pain for the past 3 weeks reveals tenderness and fullness over the inferior patella and proximal patellar tendon. There is no patellofemoral crepitus, patella apprehension sign, or anterior or posterior instability. Initial management should include
Detailed Explanation
The patient has patellar tendinitis (jumper's knee). It is a common overuse condition seen in runners, volleyball players, soccer players, and jumpers but can be seen in any activity in which repeated extension of the knee is required. In the acute setting, the pain is well localized and there is tenderness and sometimes swelling of the tendon. MRI is recommended for evaluating chronic cases and for surgical planning. In the acute phases, ice, rest, and avoidance of the offending activity are recommended. Weakness of the quadriceps and hamstring muscle are thought to contribute to this problem; therefore, stretching and isometric exercise in a limited range of motion are important. Complete rest and intratendinous injections of steroids are detrimental to tendon physiology. Stanish WD, Rubinovich RM, Curwin S: Eccentric exercise in chronic tendinitis. Clin Orthop 1986;208:65-68.
Question 740
High Yield
Figure 8 shows the radiograph of a 76-year-old man who has knee pain and swelling. History reveals that he underwent total knee arthroplasty 18 years ago. What is the most likely diagnosis?
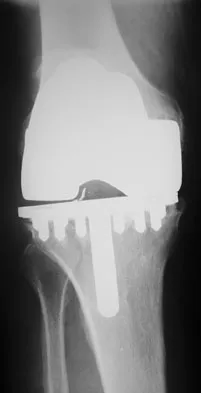
Detailed Explanation
The radiograph reveals complete loss of joint space with particulate metal debris consistent with total polyethylene failure and metal-on-metal articulation. The components appear to be well fixed and minimal osteolysis is evident. Kilgus DJ, Moreland JR, Finerman GA, et al: Catastrophic wear of tibial polyethylene inserts. Clin Orthop Relat Res 1991;273:223-231.
Question 741
High Yield
In a longitudinal study of children with spastic diplegia, analysis of long-term function will most likely reveal
Detailed Explanation
In a longitudinal study of 18 patients with spastic diplegia over a period of 32 months, three-dimensional gait analysis revealed a deterioration of gait stability with increases in double support time and decreases in single support time. Kinematic data also identified a loss of excursion about the knee, ankle, and pelvis. Interestingly, the static examination of the children showed a decrease in the popliteal angle over time. The authors concluded that ambulatory ability tends to worsen over time in children with spastic diplegia.
Question 742
High Yield
Figures 25a and 25b show the clinical photographs of a 19-year-old baseball outfielder who has shoulder pain after sliding headfirst into second base. He reports pain while batting, sliding, and catching. Examination reveals a posterior prominence during midranges of forward elevation, which then disappears with a palpable clunk during terminal elevation and abduction. What is the most likely diagnosis?
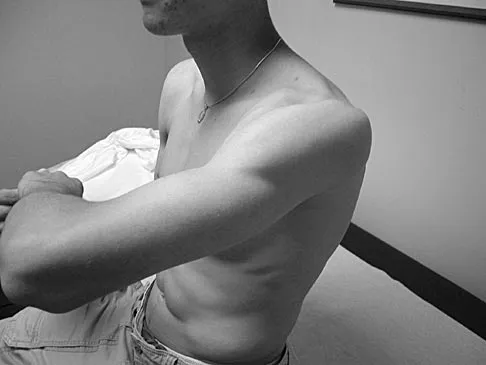
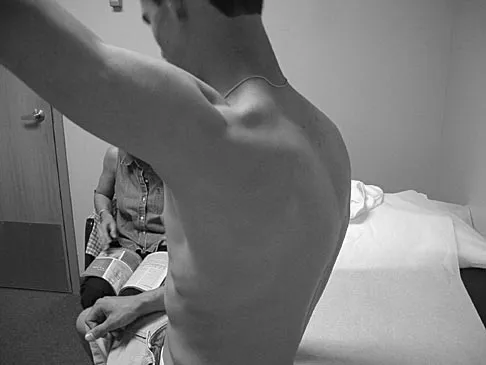
Detailed Explanation
A headfirst slide with the arm extended can injure the posterior shoulder. Winging of the scapula is dynamic and is considered a compensatory effort to prevent subluxation; it is not related to nerve injury. Posterior glenohumeral subluxation can be present during the initiation of a bat swing. Rotator cuff function, interval tears, and superior labrum tears can be painful but do not produce winging. Kuhn JE, Plancher KD, Hawkins RJ: Scapular winging. J Am Acad Orthop Surg 1995;3:319-325.
Question 743
High Yield
A 55-year-old patient is seeking a surgical consultation for a painful flatfoot deformity that has failed to respond to nonsteroidal anti-inflammatory drugs, shoe and activity modifications, and orthoses. The patient is of medium build, a nonsmoker, and has no history of diabetes mellitus. Radiographs are shown in Figures 43a through 43c. Based on these findings, treatment should consist of
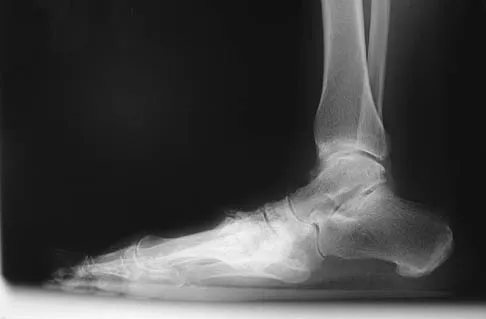
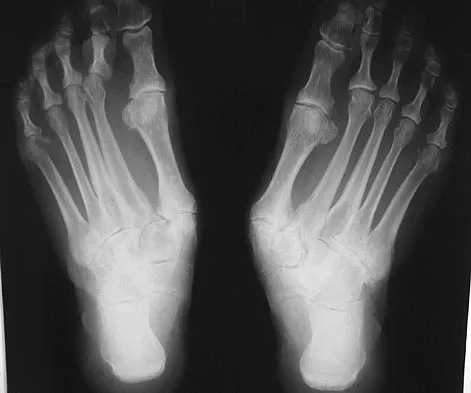
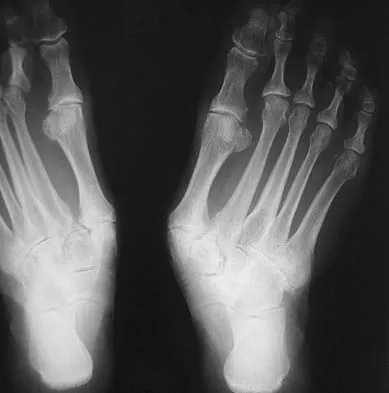
Detailed Explanation
The patient has a degenerative collapse of the midfoot through the tarsometatarsal joints with significant forefoot abduction; therefore, a midfoot arthrodesis is required to address the arthritic joints and deformity at the tarsometatarsal articulation. All of the other procedures correct hindfoot deformities and therefore would not be appropriate treatment. Brage M: Degenerative joint disease of the midfoot. Foot Ankle Clin 1999;4:355-367.
Question 744
High Yield
Examination of a 12-year-old girl with bilateral anterior knee pain reveals excessive femoral anteversion and excessive external tibial torsion. The patient has no patellofemoral instability. Nonsurgical management consisting of muscle strengthening and nonsteroidal medication has failed to relieve the patient's pain. Treatment should now consist of
Detailed Explanation
Children with symptomatic severe torsional malalignment of the lower extremity and patellofemoral pathology show excessive femoral anteversion and external tibial torsion on physical examination and analysis of gait. The functional effect of this torsional malalignment is centered about the knee joint. If nonsurgical management fails to alleviate patellofemoral pain, definitive surgical treatment should consist of corrective osteotomies, including internal rotation of the distal part of the tibia or external rotation of the femur, or both. Patients with surgical correction by osteotomy show an improved gait pattern and appearance of the extremity and a marked decrease in knee pain. External rotation of the distal part of the tibia or internal rotation of the distal part of the femur worsens the torsional malalignment. No additional soft-tissue realignment procedures, including retinacular release or patellar realignment, are required.
Question 745
High Yield
A 16-year-old girl was involved in a motorcycle accident that resulted in a significant right tibial fracture with soft-tissue loss over the distal 4 cm of the anterior medial tibia. The patient has had two irrigations and debridements and recently had an intramedullary nail placed for the skeletal injury. Vacuum-assisted closure (VAC) has been used to cover the defect since the injury. The risk of infection developing in the tibia is
Detailed Explanation
The risk of infection in a 3B open tibia fracture is most directly related to the timing of the soft-tissue coverage and less related to the size or location of the wound. The wound VAC does not lower or raise the risk of infection in open fractures. It does appear to increase the window of time to obtain coverage without increasing the risk of infection. Additionally, the wound VAC may decrease the probability of needing free tissue coverage. Intramedullary nailing has not been shown to lower the risk of infection in 3B fractures. Godina M: Early microsurgical reconstruction of complex trauma of the extremities. Plast Reconstr Surg 1986;78:285-292. Dedmond BT, Kortesis B, Punger K, et al: The use of negative-pressure wound therapy (NPWT) in the temporary treatment of soft-tissue injuries associated with high-energy open tibia shaft fractures. J Orthop Trauma 2007;21:11-17.
Question 746
High Yield
Which of the following findings best describes the effects of increasing conformity of a fixed tibial bearing component and femoral component in total knee arthroplasty?
Detailed Explanation
In the design of tibial and femoral components, a compromise must be made between contact stresses and constraint. Increased conformity increases constraint, limits motion, and potentially increases stress on the knee-cement interface. By increasing conformity, the surface area over which force is applied is increased, resulting in decreased peak contact stresses and decreased component wear rates. Pellicci PM, Tria AJ Jr, Garvin KL (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 265-274.
Question 747
High Yield
A patient undergoes excision of a 3- x 3-cm soft-tissue sarcoma. The final histology results show tumor at the surgical margin. The surgical procedure performed is classified as
Detailed Explanation
Surgical margins are classified according to the plane of dissection in relation to the tumor. An intralesional procedure is where the plane of dissection passes through the tumor. A marginal resection involves a resection where the plane of dissection is through the reactive zone of the tumor. A wide resection is through completely normal tissue outside of the reactive zone. A radical resection removes all of the muscles and/or bone of the compartment that are involved by the tumor.
Question 748
High Yield
The hallucal sesamoids are held together by which of the following structures?
Detailed Explanation
The two sesamoids of the metatarsophalangeal joint are embedded in the tendons of the short flexor of the great toe. They are held together by the intersesamoid ligament and the plantar plate, which inserts on the base of the proximal phalanx of the hallux. The flexor hallucis longus tendon inserts onto the distal phalanx of the great toe. The plantar calcaneonavicular (spring) ligament, by supporting the head of the talus, principally maintains the arch of the foot. The plantar fascia inserts distally onto the skin and to the flexor tendons and transverse metatarsal ligaments at each metatarsophalangeal joint. The intermetatarsal ligament attaches to the base of the second through fifth metatarsals. Lewis WH (ed): Gray's Anatomy of the Human Body, ed 20. Philadelphia, PA, Lea & Febiger, 2000.
Question 749
High Yield
Which of the following structures is most commonly involved in lateral epicondylitis?
Detailed Explanation
The most common specific site of involvement is the origin of the extensor carpi radialis brevis. It is usually caused by overuse activities, such as the eccentric overload exhibited during a backhand in tennis. In most patients, the characteristic friable, grayish tissue described as angiofibroblastic hyperplasia or hyaline degeneration is seen at the extensor carpi radialis brevis origin. Nirschl RP: Elbow tendinosis/tennis elbow. Clin Sports Med 1992;11:851-870.
Question 750
High Yield
Calcitonin acts as an antiresorptive agent by
Detailed Explanation
Calcitonin is a hormone that binds to osteoclasts and acts to decrease both osteoclast activity and number. Calcitonin is most effective in reducing vertebral compression fractures in high-turnover osteoporosis. It is also effective in treating regional osteoporosis. Because of its analgesic effect, it is helpful in treating painful acute compression fractures associated with osteoporosis.
Question 751
High Yield
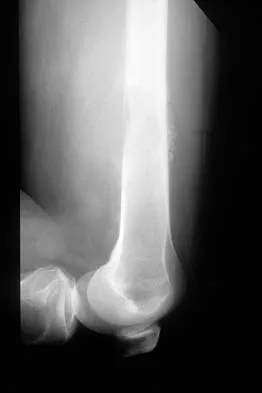
A 51-year-old woman has had progressively increasing right knee pain for the past 6 months. She has a history of metastatic renal cell carcinoma to the lung and the skeletal system. Radiographs are seen in Figures 18a and 18b. The next step in management of the right distal femur lesion should consist of
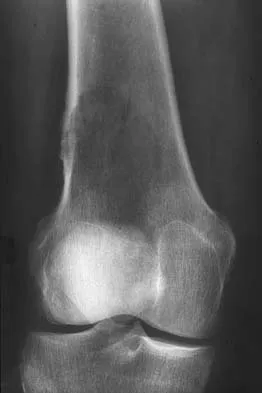
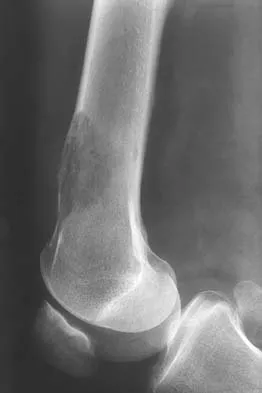
Detailed Explanation
In a patient with known metastatic disease, the surgeon must rule out additional lesions throughout the femur prior to surgical management. Lesions located in the diaphysis or in the peritrochanteric region may influence the surgical procedure. Frassica FJ, Gitelis S, Sim FH: Metastatic bone disease: General principles, pathophysiology, evaluation, and biopsy. Instr Course Lect 1992;41:293-300.
Question 752
High Yield
A 66-year-old man reports a 2-week history of worsening low back and leg pain. He reports that his pain is aggravated by lying down and relieved by standing and walking. He notes that he has been losing weight recently and that his pain has been awakening him during the night. His medical history is significant for hypertension, coronary artery disease, and prostate cancer. His physical examination is essentially unremarkable. Lumbar radiographs are within normal limits. What is the most appropriate management for this patient?
Detailed Explanation
In the initial assessment of acute low back pain in adults, no diagnostic testing is indicated during the first 4 weeks in the absence of "red flags" for a serious underlying condition. The purpose of the initial assessment of acute low back pain in adults is to rule out serious underlying conditions presenting as low back pain. The Agency for Healthcare Policy and Research, in its 1994 clinical practice guideline, identified four serious conditions that may present with low back pain, including fracture, tumor, infection, and cauda equina syndrome. This patient has five "red flags" for a spinal tumor as a possible etiology of his low back pain, including age of older than 50 years, constitutional symptoms (recent weight loss), pain worse when supine, severe nighttime pain, and a history of cancer. Of these, his history of cancer is most significant, as greater than 90% of spinal tumors are metastatic. In order of frequency, breast, prostate, lung, and kidney make up approximately 80% of all secondary spread to the spine. In the presence of "red flags" for tumor or infection, it is recommended that the clinician obtain a CBC count, ESR, and a urinalysis. If these are within normal limits and suspicions still remain, consider consultation or seek further evidence with a bone scan, radiographs, or additional laboratory studies. Negative radiographs alone are insufficient to rule out disease. If radiographs are positive, the anatomy can be better defined with MRI. Agency for Health Care Policy and Research, Bigos SJ (ed): Acute Low Back Problems in Adults. Rockville, MD, US Department of Health and Human Services, AHCPR Publication 95-0642, Clinical Practice Guideline #14, 1994.
Question 753
High Yield
What is the most common cause of errors that harm patients?
Detailed Explanation
The AMA report identified communication breakdown as the most common cause of errors that harm patients. It is extremely important to learn to communicate effectively with your patients. Understanding cultural and language differences helps avoid communication errors. Jimenez R, Lewis VO (eds): Culturally Competent Care Guidebook. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2007. American Medical Association ethical force program report: "Improving communication - Improving care", 2006
References:
- http://www.ama-assn.org/ama/pub/category/16245.html.
Question 754
High Yield
A 20-year-old athlete sustains a 2- x 3-cm grade IV chondral injury to the right knee. After failure of nonsurgical management, which of the following procedures would ensure the highest percentage of hyaline-like cartilage?
Detailed Explanation
Autologous chondrocyte implantation was first reported by Brittberg in 1994 and has resulted in predominantly type II collagen (hyaline-like articular cartilage) in the repair tissue. The extracellular matrix in articular cartilage is made up primarily of type II collagen, proteoglycans, and water. Arthroscopic chondroplasty, microfracture, drilling, and abrasion arthroplasty all result eventually in fibrocartilage fill of the defect (predominantly type I collagen). Brittberg M, Lindahl A, Nilsson A, et al: Treatment of deep cartilage defects in the knee with autologous chondrocyte transplantation. N Engl J Med 1994;331:889-895.
Question 755
High Yield
Design and manufacturing of a metal-on-metal articulation has an important influence on the tribology. Which of the following statements best characterizes the type of contact that is best for metal-on-metal articulations?
Detailed Explanation
It is important that the radii of a metal-on-metal head to cup articulation be such that there is polar contact. As the radii become closer to equal, conditions favor higher frictional torque and equatorial seizing. The "bedding in" of metal-on-metal surfaces and their stiffness are both components of the properties considered in the design of polar contact surfaces.
Question 756
High Yield
Analysis of primary total hip arthroplasty using press-fit acetabular components without supplementary screw fixation reveals that screw fixation
Detailed Explanation
Using mechanical failure of fixation as the end point, Udomkiat and associates demonstrated a 12-year survivorship of 99.1% for titanium press-fit acetabular components without supplementary screw fixation. This study suggests that it is unlikely that the use of supplementary screws would lead to improved results. In addition, polyethylene wear debris tends to migrate through screw holes and along the course of screws. Screw holes also decrease the available surface for bone ingrowth. Screws that back up may be a source of backside polyethylene wear. This suggests that screw holes and the use of screws should be avoided when they are unnecessary for cup fixation.
Question 757
High Yield
A 42-year-old woman reports that she has low back pain and had a transient loss of consciousness after falling off a horse. She denies having neck pain but notes that she was involved in a motor vehicle accident 2 years ago and had neck pain at that time. Examination reveals full range of motion of the neck and no localized tenderness. The neurologic examination is normal. A lateral radiograph of the cervical spine is obtained. Figures 41a and 41b show CT and MRI scans. What is the most likely diagnosis?
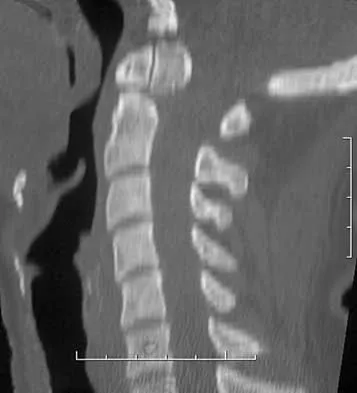
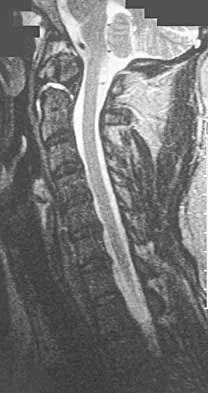
Detailed Explanation
The examination findings do not correlate with an acute injury (full range of cervical motion and the absence of pain). Radiographically, the fracture appears old based on the smooth contour of the fracture fragments and the absence of soft-tissue swelling. Flexion-extension radiographs can be obtained to determine potential instability; if present, stabilization and fusion should be considered. Schatzker J, Rorabeck CH, Waddell JP: Non-union of the odontoid process: An experimental investigation. Clin Orthop 1975;108:127-137.
Question 758
High Yield
A 25-year-old woman who fell on her outstretched hand reports chronic pain over the hypothenar eminence region and some dorsal ulnar wrist pain. She also notes difficulty playing golf and tennis. Plain radiographs of the hand and wrist are unremarkable. A CT scan is shown in Figure 36. What is the next most appropriate step in management?
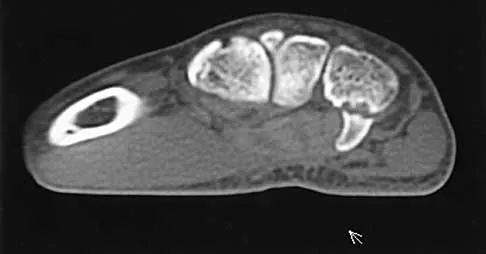
Detailed Explanation
The CT scan reveals a hook of the hamate nonunion with irregular resorption at the fracture site, which is at the base of the hamate. Symptomatic relief of the pain and discomfort has been well documented after excision of the hook of the hamate. Ultrasound therapy will not provide long-term symptomatic relief or induce nonunion healing. MRI for further soft-tissue evaluation is inappropriate because this is a bony problem; the bony architecture of the wrist is best visualized by CT. Open reduction and internal fixation of the hook of the hamate does not provide the symptomatic relief that is found with excision of the hook of the hamate. In addition, the technical difficulties and relative risk of persistent nonunion after open reduction and internal fixation are not merited when hamate excision can be effected easily and causes no long-term untoward effects. Electrodiagnostic evaluation is inappropriate because there is no history of the persistent numbness and tingling that is found in peripheral compression neuropathies. Stark HH, Chao EK, Zemel NP, Rickard TA, Ashworth CR: Fracture of the hook of the hamate. J Bone Joint Surg Am 1989;71:1206-1207. Failla JM: Hook of hamate vascularity: Vulnerability to osteonecrosis and nonunion. J Hand Surg Am 1993;18:1075-1079. Carter PR, Easton RG, Littler JW: Ununited fracture of the hook of the hamate. J Bone Joint Surg Am 1977;59:583-588.
Question 759
High Yield
What complication is frequently associated with the Weil lesser metatarsal osteotomy (distal, oblique) in the treatment of claw toe deformities?
Detailed Explanation
Weil osteotomies are useful in achieving shortening of a lesser metatarsal with preservation of the distal articular surface. The osteotomy is oriented from distal-dorsal to proximal-plantar; therefore, proximal displacement of the distal fragment is associated with plantar (not dorsal) displacement as well. Plantar displacement can result in the intrinsics acting dorsal to the center of the metatarsophalangeal joint and the development of an extended or "floating toe." Nonunion, osteonecrosis, and inadequate shortening are infrequent complications associated with the Weil lesser metatarsal osteotomy. Trnka HJ, Nyska M, Parks BG, et al: Dorsiflexion contracture after the Weil osteotomy: Results of cadaver study and three-dimensional analysis. Foot Ankle Int 2001;22:47-50.
Question 760
High Yield
The incidence of ipsilateral phrenic nerve blockade after an interscalene block approaches
Detailed Explanation
The most common side effect of an interscalene block is ipsilateral phrenic nerve blockade. The phrenic nerve arises chiefly from the fourth cervical ramus (with contributions from the third and fifth) and is the sole motor supply to the diaphragm. Phrenic nerve palsy usually is well tolerated in healthy patients but should be avoided in patients with limited pulmonary function (severe restrictive or obstructive lung disease, myasthenia gravis, or contralateral hemidiaphragmatic dysfunction). The incidence of ipsilateral phrenic nerve blockade afer interscalene block approaches 100%. Long T, Wass C, Burkle C: Perioperative interscalene blockade: An overview of its history and current clinical use. J Clin Anesthesia 2002;14;546-556.
Question 761
High Yield
The essential lesion responsible for posterolateral rotatory instability of the elbow is disruption of the
Detailed Explanation
Posterolateral rotatory instability (PLRI) of the elbow represents a three-dimensional injury pattern of rotational displacement of the ulna from the trochlea and the radius from the capitellum. The ulna supinates (externally rotates) past its normal limit and the radiocapitellar joint subluxates posterolaterally, permitting the coronoid process to slide beneath the trochlea. In cadaver studies, the lateral ulnar collateral ligament has been shown to be the essential lesion responsible for PLRI. The medial collateral ligament (of which the anterior bundle is the most important) is the primary restraint to valgus instability. The posterolateral capsule and radial collateral ligament may be disrupted in a complete posterolateral dislocation but are not essential injuries for PLRI. The primary function of the annular ligament is to stabilize the proximal radioulnar joint. O'Driscoll SW, Jupiter JB, King GJW, Hotchkiss RN, Morrey BF: The unstable elbow. J Bone Joint Surg Am 2000;82:724-738. Olsen BS, Sojbjerg JO, Dalstra M, Sneppen O: Kinematics of the lateral constraints of the elbow. J Shoulder Elbow Surg 1996;5:333-341.
Question 762
High Yield
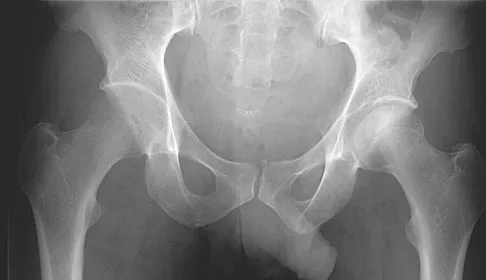
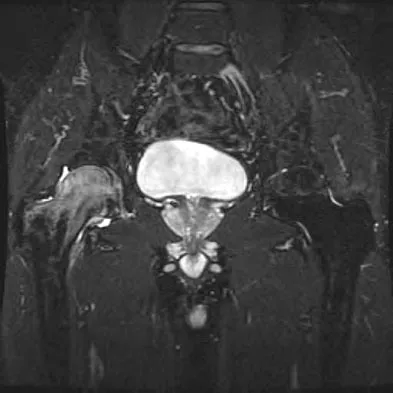
A 42-year-old man reports the recent onset of right hip pain. A radiograph and MRI scan are shown in Figures 38a and 38b. A WBC count, erythrocyte sedimentation rate, and hip aspiration are within normal limits. Management should now consist of
Detailed Explanation
Transient osteoporosis of the hip is an uncommon problem, usually affecting women in the last trimester of pregnancy and middle-aged men. Symptoms include pain in the involved hip with temporary osteopenia; however, there is no joint space involvement. In this patient, the imaging findings are consistent with transient osteoporosis. Short TR/TE (repetition time/echo time) images reveal diffusely decreased signal intensity in the femoral head and intracapsular region of the femoral neck. Increased signal intensity is seen with increased T2-weighting. Within a few months, the pain, as well as the imaging findings, will completely resolve without intervention. Distinguishing the diffuse features of transient osteoporosis of the hip from the segmental findings of osteonecrosis is essential. Unlike transient osteoporosis of the hip, osteonecrosis will have a double-density signal on MRI and may progress radiographically. Surgical intervention and oral corticosteriods are not indicated for treatment. Protected weight bearing until the pain resolves may decrease symptoms while the transient osteoporosis resolves. Potter H, Moran M, Scheider R, et al: Magnetic resonance imaging in diagnosis of transient osteoporosis of the hip. Clin Orthop 1992;280:223-229. Bijl M, van Leeuwen MA, van Rijswijk MH: Transient osteoporosis of the hip: Presentation of typical cases for review of the literature. Clin Exp Rheumatol 1999;17:601-604.
Question 763
High Yield
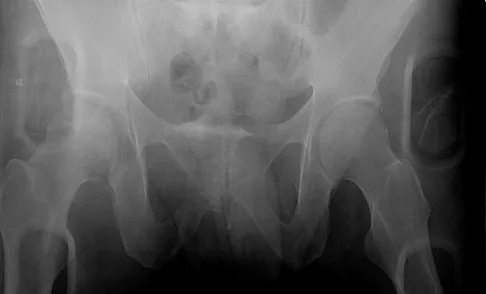
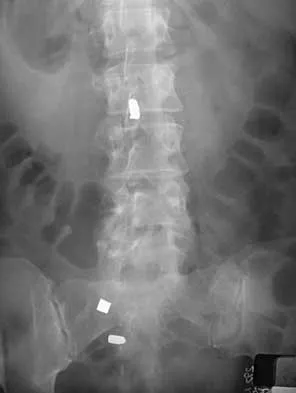
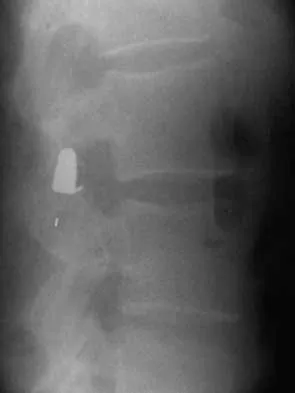
A 40-year-old woman has local back pain and intense burning pain in her perianal region after being shot twice in the back. Motor and sensory examination of her lower extremities reveals no apparent deficit. She has present but decreased sensation in her perianal region, an intact anal wink, good rectal tone, and an intact bulbocavernosus reflex. Radiographs and CT scans are shown in Figures 3a through 3d. What is the next most appropriate step in management?
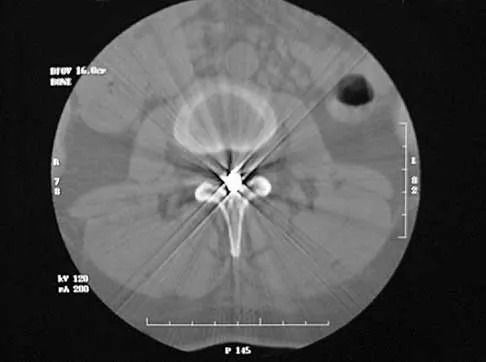
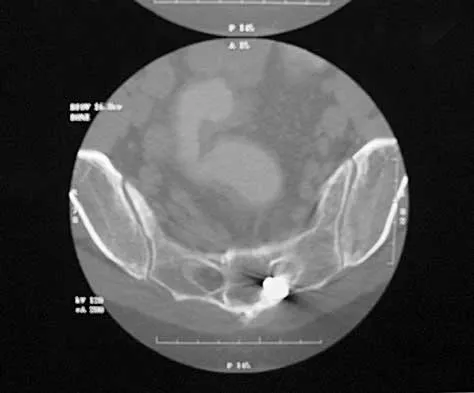
Detailed Explanation
Because the patient has an apparent compressive neuropathy secondary to the metallic fragments, removal of the fragments in this incomplete lesion at the cauda equina level can be expected to improve her sensory dysesthesias and pain. Steroids are not indicated in a root lesion secondary to a penetrating injury. MRI will have significant artifact effect and will not provide much additional information. The posterior bony elements are not significantly injured; therefore, stabilization is not indicated. Bracken MB, Shepard MJ, Holford TR: Administration of methylprednisolone for 24 or 48 hours or tirilazad mesylate for 48 hours in the treatment of acute spinal cord injury. JAMA 1997;277:1597-1604. Waters RL, Adkins RH: The effects of removal of bullet fragments retained in the spinal canal: A collaborative study by the National Spinal Cord Injury Model Systems. Spine 1991;16:934-939.
Question 764
High Yield
Which of the following ligaments are the primary static restraints to inferior translation of the arm when the shoulder is in 0 degrees of abduction and neutral rotation?
Detailed Explanation
Biomechanical ligament sectioning studies have implicated both the superior glenohumeral and coracohumeral ligaments as restraints to inferior translation when the shoulder is in 0 degrees of abduction and neutral rotation. Although there is controversy over the significance of each ligament, both are involved to some degree. The middle glenohumeral ligament is more important in the midranges of abduction, and the inferior ligament is more important at 90 degrees of abduction. The coracoacromial and coracoclavicular ligaments play no role in glenohumeral restraint. Warner JJ, Deng XH, Warren RF, et al: Static capsuloligamentous restraints to superior-inferior translation of the glenohumeral joint. Am J Sports Med 1992;20:675-685.
Question 765
High Yield
A 37-year-old man has had isolated chronic knee swelling for the past 6 months. He denies any history of specific trauma. Examination reveals a large effusion with a stable knee, but the remainder of the examination is normal. Plain radiographs are unremarkable. An MRI scan reveals a large effusion without meniscal injury. An arthroscopic image of the suprapatellar pouch is shown in Figure 23. What is the most likely diagnosis?
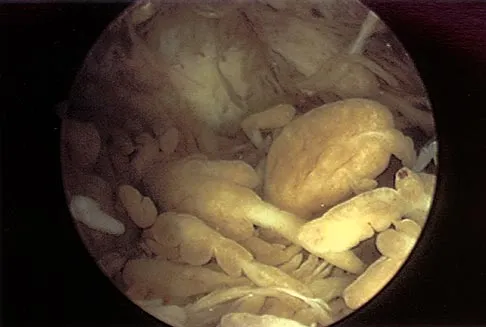
Detailed Explanation
The history and physical examination are consistent with a monoarticular joint condition but not typical of joint sepsis. The arthroscopic appearance of brownish proliferative synovium is typical of PVNS. PVNS is a monoarticular synovial disease of unknown etiology and is treated with total synovectomy. The proliferative synovitis is not consistent with chondromalacia. Synovial cell sarcoma is an extracapsular disease. Rheumatoid arthritis typically is polyarticular, and the synovial appearance is not associated with hemosiderin deposition. Flandry FC, Hughston JC, Jacobson KE, Barrack RL, McCann SB, Kurtz DM: Surgical treatment of diffuse pigmented villonodular synovitis of the knee. Clin Orthop 1994;300:183-192.
Question 766
High Yield
What is the primary concern for arthrodesis of a failed infected total knee arthroplasty using internal fixation?
Detailed Explanation
Arthrodesis of the failed infected total knee arthroplasty may be accomplished by external fixation, intramedullary rod fixation, and dual plates and screws. External fixation runs the risk of pin tract infection, although after its removal, there are no metal surfaces left in place. Intramedullary rods have been used successfully in the treatment of infected total knees, although they also leave metal within the region of the infection. The dual plate technique of knee fusion is useful in patients with rheumatoid arthritis who require fusion in the absence of infection because it provides good initial stability and avoids the use of external pins. However, in the face of infection, the large surface area of the screws and plates may serve as a site for bacteria to hide within a glycocalyx and make eradication of the infection almost impossible.
Question 767
High Yield
A 75-year-old woman began a walking program 2 months after undergoing right total knee arthroplasty. She had to stop the program after 4 weeks because of hindfoot pain and ankle swelling. Radiographs are shown in Figures 42a and 42b. What is the most likely diagnosis?
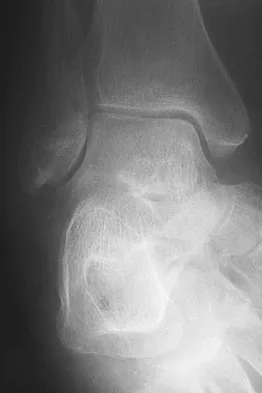
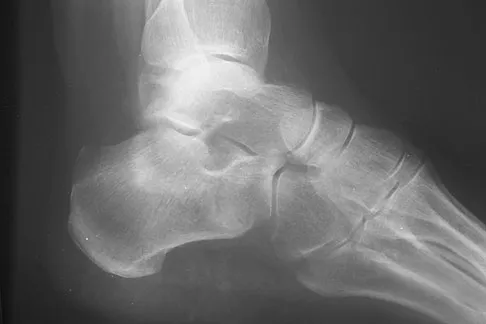
Detailed Explanation
It is often tempting to assign a diagnosis of plantar fasciitis in patients with hindfoot pain. In this patient, the radiographs confirm a diagnosis of a calcaneal insufficiency fracture. The dense condensation of bone on the lateral view confirms the diagnosis. There is no radiographic evidence of a heel spur, osteochondral lesions, or chondrocalinosis. Resnick D: Diagnosis of Bone and Joint Disorders, ed 3. Philadelphia, PA, WB Saunders, 1995, p 2591. Kearon C: Natural history of venous thromboembolism. Semin Vasc Med 2001;1:27-37.
Question 768
High Yield
A 21-year-old man has had posterior neck discomfort for the past 6 months. Radiographs, an MRI scan, and a photomicrograph of the biopsy specimen are shown in Figures 17a through 17d. What is the most likely diagnosis?
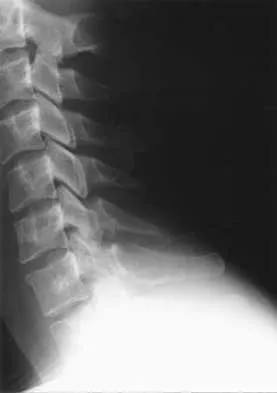
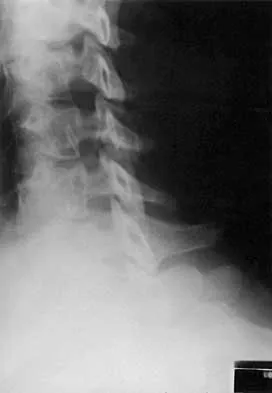
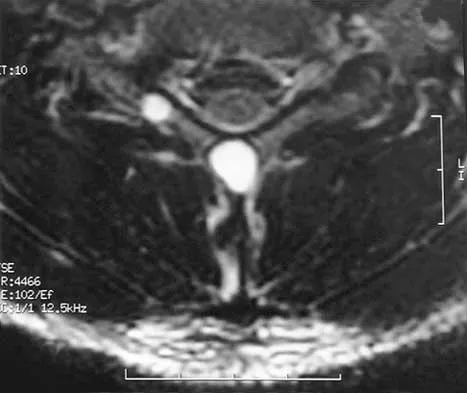
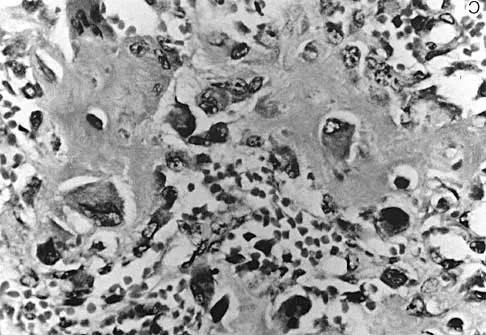
Detailed Explanation
Forty percent of osteoblastomas occur in the spine, and they can become large and locally aggressive lesions. They generally occur in the posterior elements but can occur in the ribs and transverse processes. Microscopic analysis of the lesion will reveal hyperchromatic osteoblasts separated by incompletely mineralized bars of bone. Recommended treatment is en bloc excision. Fibrous dysplasia, giant cell tumor, and hemangioma can have similar radiographic appearances; therefore, biopsy may be required to differentiate them from more aggressive lesions. Osteochondromas are characterized by an osteocartilaginous growth arising from the cortex. Bridwell KH, Ogilvie JW: Primary tumors of the spine, in Bridwell KH, DeWald RL (eds): The Textbook of Spinal Surgery. Philadelphia, PA, JB Lippincott, 1991, vol 2, pp 1143-1174.
Question 769
High Yield
A 24-year-old man who was involved in a high speed motor vehicle accident is transferred for definitive care after having been diagnosed with an acute spinal cord injury from a fracture-dislocation at C6-7. He has a complete C6 neurologic level and it is now approximately 10 hours from his injury. What is the most appropriate pharmacologic treatment at this time?
Detailed Explanation
The standard practice in the pharmacologic treatment of a spinal cord injury in the United States has been the administration of methylprednisolone with an initial bolus of 30 mg/kg followed by 5.4 mg/kg for 24 hours, in accordance with the findings of the second and third National Acute Spinal Cord Injury Studies (NASCIS). Although the studies have subsequently drawn criticism for their methodology and outcomes, it has been generally accepted that beneficial neurologic outcomes were anticipated in patients who were able to start the protocol within 8 hours of their initial injury. Further improvement was noted in patients receiving the methylprednisolone within 3 hours of their injury and continuing an infusion for 48 hours. In this patient, who is outside the 8-hour treatment window, no studies have supported starting the methylprednisolone protocol at this time. Braken MB, Shepard MJ, Holford TR, et al: Administration of methylprednisolone for 24 or 48 hours or tirilazad mesylate for 48 hours in the treatment of acute spinal cord injury: Results of the third National Acute Spinal Cord Injury Randomized Controlled Trial. National Acute Spinal Cord Injury Study. JAMA 1997;277:1597-1604.
Question 770
High Yield
A 25-year-old man has a mass on the medial aspect of the left knee. He reports that the mass has been present for several years, but a recent increase in physical activity has resulted in periodic tenderness. Radiographs are shown in Figures 13a and 13b. What is the most likely diagnosis?
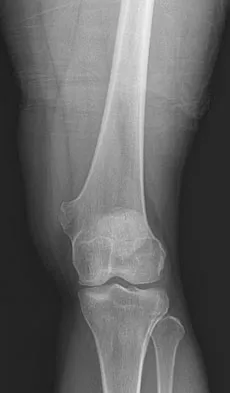
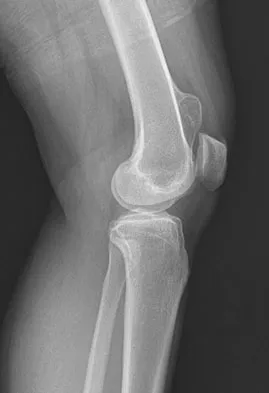
Detailed Explanation
The radiographs reveal a sessile lesion projecting from the medial aspect of the distal femur. The lesion shares the cortex with the bone and the base communicates with the medullary space of the femur. This is the classic appearance of an osteochondroma, the most common benign tumor of bone. Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 103-111.
Question 771
High Yield
What is the primary benefit of using rhBMP-2 instead of autogenous bone graft inside an anterior spinal fusion cage?
Detailed Explanation
Radiographic fusion success rates are best described as slightly rather than substantially improved. Hospital stay and time to fusion also are not substantially decreased. Use of BMP does eliminate the need for autograft harvest for anterior lumbar interbody fusion/cage. The need for postoperative bracing is not altered based on graft choice. Early studies of posterolateral fusion applications appear to show a greater potential benefit of rhBMP-2 over autograft. Not all BMP formulations perform the same with regard to safety and effectiveness. Other osteoinductive proteins in clinical trials (BMP-7, GDF-5) will require individual analysis of these properties.
Question 772
High Yield
Which of the following statements correctly describes the results of gamma irradiation of musculoskeletal allograft?
Detailed Explanation
Low dose gamma irradiation (less than 3.0 megarads) with antibiotic soaks is one of the most common techniques for secondary sterilization. Elimination of HIV with gamma irradiation requires doses estimated to be greater than 3.5 megarads. Gamma irradiation levels of 4 megarads have been shown to alter the mechanical properties of human infrapatellar tendons. Ethylene oxide, also used for allograft sterilization, has been associated with a chronic inflammatory process that resolved after graft removal. Jackson DW, Windler GE, Simon TM: Intraarticular reaction associated with the use of freeze-dried, ethylene oxide-sterilized bone-patella tendon-bone allografts in the reconstruction of the anterior cruciate ligament. Am J Sports Med 1990;18:1-10. Conway B, Tomford W, Mankin HJ, et al: Radiosensitivity of HIV-1: Potential application to sterilization of bone allografts. AIDS 1991;5:608-609.
Question 773
High Yield
A 20-year-old man has a large soft-tissue mass behind his knee. MRI scans are shown in Figures 10a through 10c. Figure 10d shows a clinical photograph of his chest. The patient's condition is most likely a result of a defect in what gene?
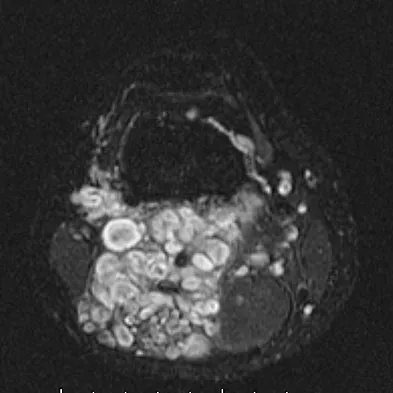
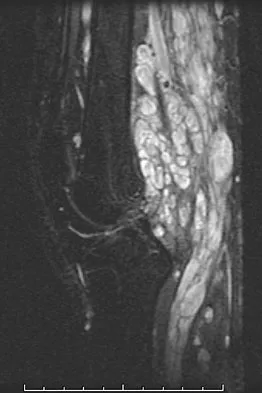
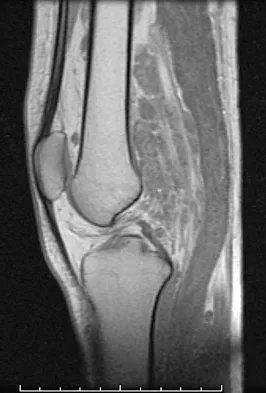
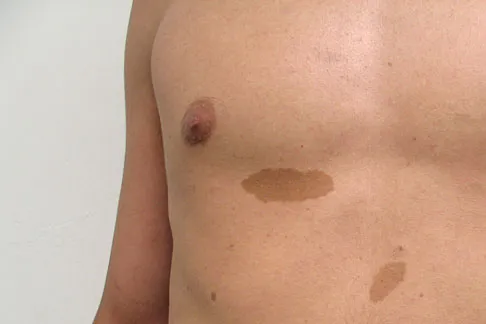
Detailed Explanation
The patient has a plexiform neurofibroma and multiple café-au-lait spots, all characteristic of von Recklinghausen's neurofibromatosis. This disease has been linked to a defect of the gene NF1 on chromosome 17. EWS is one of the genes associated with the 11;22 translocation found in Ewing's sarcoma and several other sarcomas. EXT1 is the most common gene affecting patients with multiple hereditary exostosis. P53 and Rb are tumor suppressor genes whose inactivation has been associated with tumors in conditions such as Li-Fraumeni and retinoblastoma, respectively. Theos A, Korf BR, American College of Physicians, et al: Pathophysiology of neurofibromatosis Type 1. Ann Intern Med 2006;144:842-849.
Question 774
High Yield
Figure 13 shows the clinical photograph of a 66-year-old man who has had an increasingly painful right foot deformity for the past 3 years. Examination reveals that the subtalar joint is fixed in 15 degrees of valgus, and forefoot supination can be corrected to 10 degrees from neutral. Nonsurgical management has failed to provide relief. Treatment should now consist of
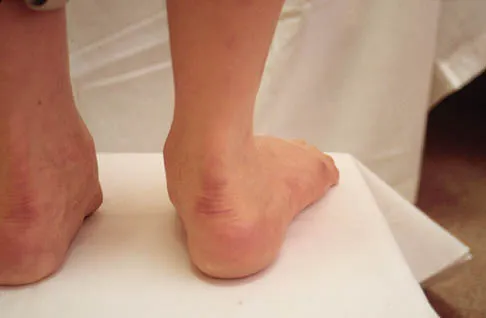
Detailed Explanation
The most important determining factor for correction of an adult flatfoot without an arthrodesis is the flexibility of the subtalar and transverse tarsal joints. Rigid deformities cannot be corrected with a medial sliding calcaneal osteotomy with FDL transfer or a subtalar arthroereisis. Isolated subtalar or talonavicular arthrodesis does not correct the deformities entirely. If the patient has forefoot supination that can be corrected to less than 7 degrees, an isolated subtalar fusion is a possible alternative.
Question 775
High Yield
Figure 48a shows the full-leg standing radiograph of a patient with a prior femoral fracture. Figure 48b shows the lateral view of the same joint. The patient is scheduled to undergo total knee arthroplasty. Because the mechanical axis of the lower extremity in patients with a prior femoral fracture may be disrupted, which of the following should be used during surgery to restore the mechanical axis of the lower extremity in this patient?
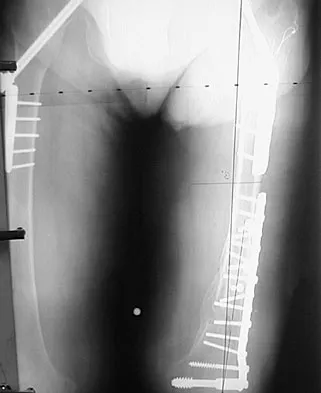
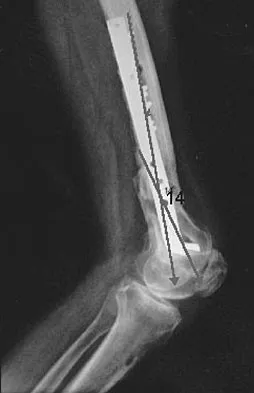
Detailed Explanation
The radiograph shows hardware that was used for fixation of a prior femoral fracture. The mechanical axis of the lower extremity in this patient is nearly normal (3 degrees valgus), and the deformity at the healed fracture site (14 degrees) does not appear to affect the joint alignment and is acceptable. Use of a routine knee prosthesis will be possible in this patient. To avoid hardware removal, extramedullary jigs and/or computerized navigation may be used to measure and restore the long axis of the femur. The use of a hinged prosthesis does not influence the mechanical axis directly. Extra-articular osteotomy is occasionally needed to reverse severe deformities. Papadopoulos EC, Parvizi J, Lai CH, et al: Total knee arthroplasty following distal femoral fractures. Knee 2002;9:267-274.
Question 776
High Yield
Fixed hyperextension of the metatarsophalangeal joint is associated with
Detailed Explanation
Claw toe and hammer toe deformities are associated with dorsal subluxation of the interossei, which can no longer serve to flex the metatarsophalangeal joint. The extensor digitorum longus then loses its tenodesing effect on the proximal interphalangeal and distal interphalangeal joints and works unopposed to extend the metatarsophalangeal joint and the proximal phalanx. Without the antagonistic action of the extensor digitorum longus, the extrinsic flexors become unopposed flexors of the proximal and distal interphalangeal joints. Marks RM: Anatomy and pathophysiology of lesser toe deformities. Foot Ankle Clin 1998;3:199-213.
Question 777
High Yield
The mother of a 5-year-old child reports that he has had a fever of 103 degrees F (39.4 degrees C), leg swelling, and has been unwilling to bear weight on his right lower leg for the past 7 days. Examination reveals point tenderness at the distal femur. Aspiration at the metaphysis yields 10 mL of purulent fluid, and a Gram stain reveals gram-positive cocci. In addition to hospital admission, management should include
Detailed Explanation
The patient has a subperiosteal abscess. Because aspiration revealed 10 mL of purulent fluid, the treatment of choice is surgical incision and drainage of the abscess, followed by immobilization to reduce the risk of pathologic fracture. With an adequate response to IV antibiotics and a susceptible bacteria, the patient may then be switched to oral antibiotics.
Question 778
High Yield
Which of the following factors has the most effect on the pullout strength of lumbar transpedicular screw fixation?
Detailed Explanation
Although all of the factors listed contribute to the pullout strength of transpedicular screw fixation, low bone density generally is felt to be the most influential. Wittenberg RH, Shea M, Swartz DE, Lee KS, White AA III, Hayes WC: Importance of bone mineral density in instrumented spine fusions. Spine 1991;16:647-652.
Question 779
High Yield
Figures 20a and 20b show the sagittal and coronal T1-weighted MRI scans of a patient's left knee. Abnormal findings include
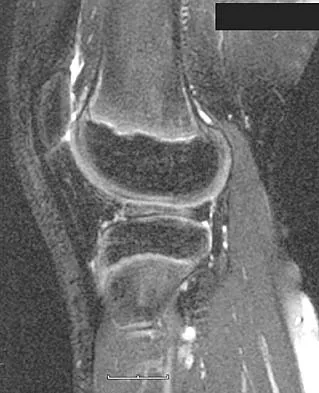
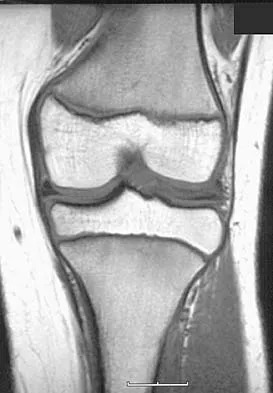
Detailed Explanation
The MRI scans show meniscal tissue extending across the entire lateral compartment, revealing a discoid lateral meniscus. The increased signal within the lateral meniscal tissue indicates a tear. Discoid lateral menisci are congenital variants that often present with mechanical symptoms in adolescents. The other structures in the knee are normal. Ahn JH, Shim JS, Hwang CH, et al: Discoid lateral meniscus in children: Clinical manifestations and morphology. J Pediatr Orthop 2001;21:812-816.
Question 780
High Yield
When compared with the normal anterior cruciate ligament (ACL), placement of an anterior cruciate ligament graft in the over-the-top position on the femoral side has what effect on its function?
Detailed Explanation
The placement of ACL graft with respect to its femoral and tibial attachments has a significant effect on its function. Evidence has shown that if the graft is placed in the over-the-top position, the graft will become lax in flexion and more taut with extension. Conversely, if the graft is placed too anterior on the femoral side, it will tighten in flexion and become lax in extension. Azar FM: Revision anterior cruciate ligament reconstruction. Instr Course Lect 2002;51:335-342. Draganich LF, Hsieh YF, Sherwin SH, et al: Intra-articular anterior cruciate ligament graft placement on the average most isometric line on the femur: Does it reproducibly restore knee kinematics? Am J Sports Med 1999;27:329-334.
Question 781
High Yield
A 34-year-old woman has had painful snapping and popping in the elbow since falling while in-line skating 6 months ago. The popping also occurs when she pushes off with her hands to rise from a seated position. Initial radiographs were normal, and she was told that she had sprained her elbow. Examination reveals few findings except that she is very apprehensive when the forearm is forcefully supinated with the elbow extended or partially flexed. A radiograph taken in that position is shown in Figure 24. Treatment should consist of
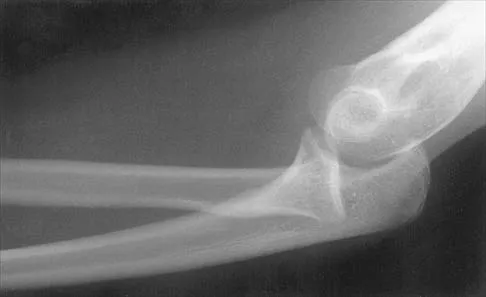
Detailed Explanation
The radiograph reveals posterolateral rotatory subluxation of the radiohumeral and ulnohumeral joints. The space between the ulna and trochlea is enlarged, particularly posteriorly at the olecranon. These findings are diagnostic of posterolateral rotatory instability, which causes recurrent subluxation and reduction as the elbow is flexed from an extended and supinated position with valgus load. The posterolateral rotatory instability apprehension test was performed on this patient and the result was positive. The lateral pivot-shift test causes a clunk as the elbow reduces but is more difficult to perform, even under general anesthesia. The patient does not have isolated subluxation of the radial head, although these findings can be mistakenly diagnosed as such. The radial head is normally shaped and does not represent a congenital dislocation. There are no findings here to suggest osteochondritis dissecans or loose bodies. O'Driscoll SW, Bell DF, Morrey BF: Posterolateral rotatory instability of the elbow. J Bone Joint Surg Am 1991;73:440-446. Burgess RC, Sprague HH: Post-traumatic posterior radial head subluxation: Two case reports. Clin Orthop 1984;186:192-194.
Question 782
High Yield
Figures 43a and 43b show the clinical photographs of a 4-month-old child with bilateral popliteal pterygium. The fixed knee contractures measure 100 degrees bilaterally. What future treatment is most likely to successfully correct this deformity?
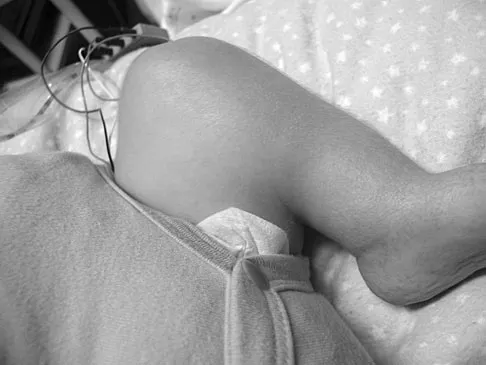
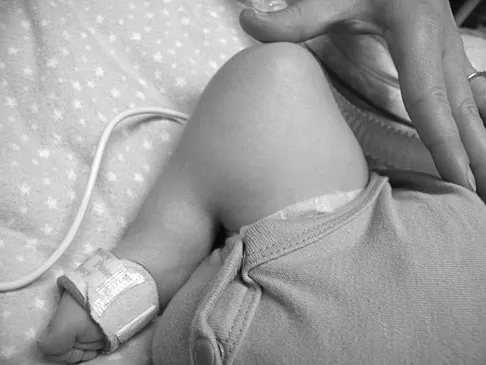
Detailed Explanation
Congenital popliteal webbing with contractures of 60 degrees is a difficult deformity to correct. The anatomy of the web is of considerable importance. MRI can delineate the extent of the posterior fibrous band that often stretches from the ischium to the calcaneus. The sciatic nerve, usually shortened, most often runs just anterior to this fibrous band. For mild contractures of less than 20 degrees, nonsurgical management is usually adequate. Hamstring lengthening and postoperative splinting are usually sufficient for contractures of 20 degrees to 40 degrees. Moderate contractures of up to 60 degrees usually require Z-plasties in the popliteal fossa and postoperative serial casting to avoid undue tension on neurovascular structures. Contractures of more than 60 degrees require a femoral shortening osteotomy or gradual correction with an external fixator. However, rapid recurrence following fixator removal is common if formal soft-tissue procedures and postoperative splinting are not performed. Parikh SN, Crawford AH, Do TT, et al: Popliteal pterygium syndrome: Implications for orthopaedic management. J Pediatr Orthop B 2004;13:197-201.
Question 783
High Yield
A 37-year-old laborer falls 12 feet and sustains a comminuted tibial plafond fracture. Three years after treatment using standard techniques, what will be the most likely outcome?
Detailed Explanation
Two recent studies by Pollak and associates and Marsh and associates have focused on function after high-energy tibial plafond fractures. Findings are unfavorable even when anatomic reduction is performed in the best centers and patients are provided excellent rehabilitation. Function improves up to 2 years after injury, but even basic walking skills remain adversely affected. Virtually all patients have long-term adverse general health effects compared to their gender and age-matched peers. Posttraumatic degenerative arthritis is present in most ankles. Patients should be told early about the long-term prognosis, and early vocational/psychological counseling should be given. Despite these adverse outcomes, only a minority of patients require fusion or arthroplasty. Pollak AN, McCarthy ML, Bess RS, et al: Outcomes after treatment of high-energy tibial plafond fractures. J Bone Joint Surg Am 2003;85:1893-1900.
Question 784
High Yield
A 14-year-old girl has had progressive heel pain for the past several months. Based on the radiograph, MRI scan, and biopsy specimens shown in Figures 37a through 37d, treatment should include
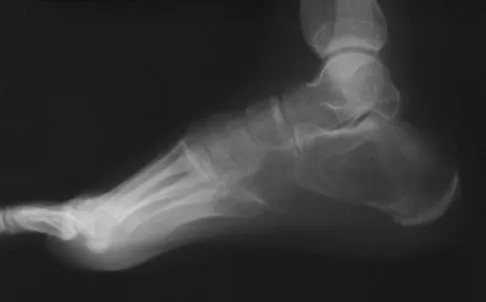
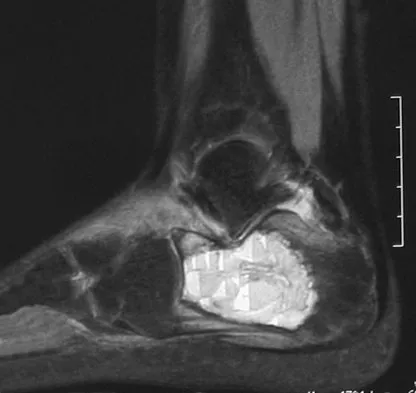
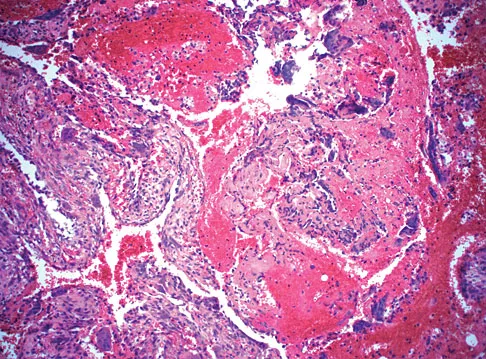
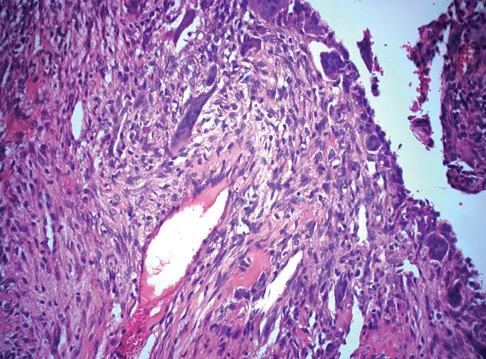
Detailed Explanation
An aneurysmal bone cyst is a benign, locally destructive lesion of bone. Most are seen in patients in the second decade of life. The clinical presentation varies, but most patients have pain, tenderness, swelling, and/or pathologic fracture. Radiographs show a radiolucent lesion sometimes with expansile remodeling of the cortex. MRI best detects the commonly seen fluid-fluid levels associated with this lesion. Histologic findings include blood-filled spaces with bland fibrous connective tissue septa. The stroma has histiocytes, fibroblasts, scattered giant cells, hemosiderin, and occasional inflammatory cells. Treatment of these lesions consists of extended curettage, plus or minus the use of adjuvants (liquid nitrogen, phenol, argon beam coagulation), and finally filling the bone void (allograft or other bone substitute). Gibbs CP Jr, Hefele MC, Peabody TD, et al: Aneurysmal bone cyst of the extremities: Factors related to local recurrence after curettage with a high-speed burr. J Bone Joint Surg Am 1999;81:1671-1678.
Question 785
High Yield
Which of the following factors is considered most important when assessing an ankle fracture for surgical treatment?
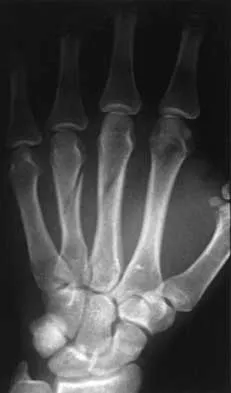
Detailed Explanation
Although all of these factors may influence the decision to perform surgery, the most important is the position of the talus in the mortise. The goal of treatment of ankle fractures is to maintain the talus centered in the mortise. If it is in this position, the other factors do not enter into the decision to intervene surgically. Stover MD, Kellam JF: Articular fractures: Principles, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 105-119. Hahn DM, Colton CL: Malleolar fractures, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 559-581.
Question 786
High Yield
A 60-year-old man is evaluated in the ICU after a rollover motor vehicle accident 3 days ago. He has multiple upper and lower extremity trauma and was found unresponsive at the accident scene. Surgery is planned for the extremity trauma once the patient is medically stable. He remains intubated and the cervical spine is immobilized in a semi-rigid collar. Examination reveals mild erythema in the posterior occipital cervical region. Initial AP and lateral radiographs of the cervical spine have not revealed any obvious fracture. What is the most appropriate treatment option at this time?
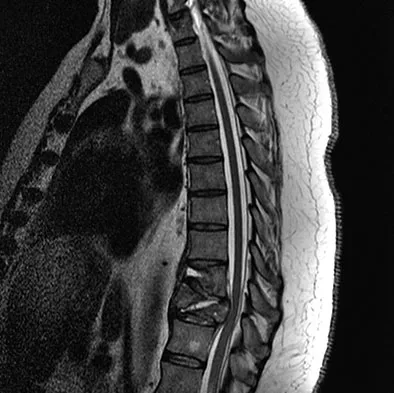
Detailed Explanation
Ackland and associates demonstrated that the failure to achieve early spinal clearance in an unconscious blunt trauma patient predisposed the patient to increased morbidity secondary to the prolonged used of cervical immobilization. They demonstrated that the four significant predictors of collar-related ulcers were ICU admission, mechanical ventilation, the necessity for cervical MRI, and the time to cervical spine clearance and collar removal. The risk of pressure-related ulceration increased by 66% for every 1-day increase in Philadelphia collar time and this highlights the need for definitive C-spine clearance. Ackland HM, Cooper DJ, Malham GM, et al: Factors predicting cervical collar-related decubitus ulceration in major trauma patients. Spine 2007;32:423-428.
Question 787
High Yield
What region of the thoracic curve is most dangerous for pedicle screw insertion while performing a posterior fusion for adolescent idiopathic scoliosis?
Detailed Explanation
Morphologic and anatomic studies confirm the pedicle is smaller on the concave side of thoracic curves. The dura is also closer to the pedicle on the concave side of the curves. Liljenqvist U, Allkemper T, Hackenberg L, et al: Analysis of vertebral morphology in idiopathic scoliosis with use of magnetic resonance imaging and multiplanar reconstruction. J Bone Joint Surg Am 2002;84:359-368.
Question 788
High Yield
Figures 52a and 52b show the plain radiographs of a 12-year-old girl who has right distal leg pain. She reports that symptoms are present with weight-bearing activities and improve with rest. Examination reveals diffuse tenderness over the distal tibial metaphysis and mild swelling. A photomicrograph of the biopsy specimen is shown in Figure 52c. What is the most likely diagnosis?
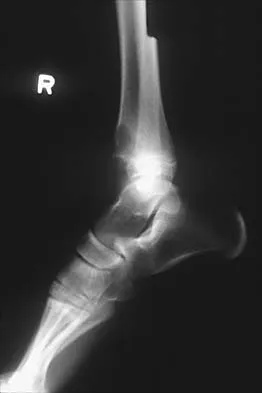
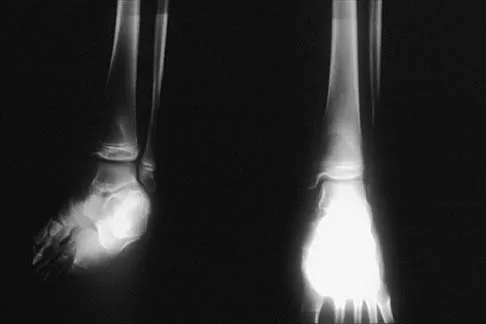
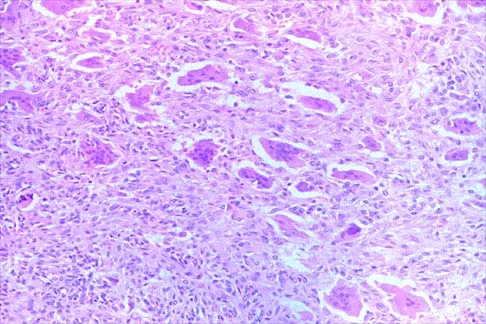
Detailed Explanation
This lytic lesion is in the epiphyseal-metaphyseal region of the distal tibia. The most common lesion in this area is a giant cell tumor. Although these lesions are most commonly seen in adults, they can also occur in the skeletally immature patient. The photomicrograph shows a lesion with multiple giant cells, the nuclei of which are similar to those in the background stroma; this finding is characteristic of giant cell tumors. Giant cells can be seen in many benign lesions, including aneurysmal bone cysts, Brown tumors, and eosinophilic granuloma. These lesions usually have fewer giant cells with less nuclei. The location of this lesion in the epiphyseal-metaphyseal area is not seen in aneurysmal bone cysts, unicameral bone cysts, Ewing's sarcoma, or eosinophilic granuloma.
Question 789
High Yield
A patient who sustained a cerebrovascular accident (CVA) 18 months ago has a long-standing spastic adduction contracture of the shoulder with a rigid block to passive external rotation. Significant hygiene problems exist with maceration and continued skin breakdown. Management should consist of
Detailed Explanation
Following a CVA, the muscular imbalance often leads to a fixed contracture of the shoulder in adduction, internal rotation, and flexion. The responsible muscles include the pectoralis major, subscapularis, teres major, and latissimus dorsi. If stretching cannot produce enough improvement for axillary hygiene, then surgery is an option. If the shoulder resists external rotation during examination with the arm at the side, as in this patient, then the subscapularis is spastic and contributing to the deformity as well and needs to be released along with the pectoralis. Phenol nerve blocks are most effective and best given within 6 months of the initial CVA to be effective. Lidocaine blocks may be helpful in determining whether a deformity is caused by a fixed soft-tissue contracture or by spasticity but play no role once the contracture is present. The modified L'Episcopo procedure is indicated in patients with contracture secondary to brachial plexus birth palsies. Braun RM, Botte MJ: Treatment of shoulder deformity in acquired spasticity. Clin Orthop 1999;368:54-65.
Question 790
High Yield
A purulent flexor tenosynovitis of the thumb may communicate with the small finger flexor through which of the following structures?
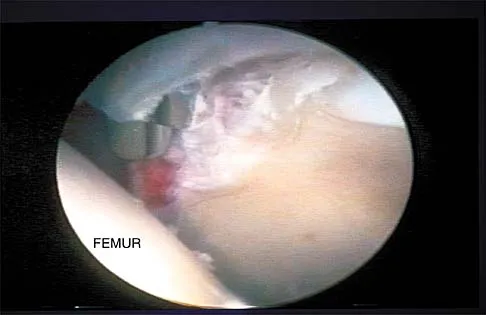
Detailed Explanation
Only the flexor sheaths of the thumb and small finger are continuous from the digit through the carpal canal and into the distal forearm. If one of the sheaths ruptures from synovitis, it may contaminate the other sheath through Parona's space in the distal forearm. This potential space lies superficial to the pronator quadratus and deep to the flexor tendons. Green DP, Hotchkiss RN, Pederson WC (eds): Operative Hand Surgery, ed 4. New York, NY, Churchill Livingstone, 1999, pp 1044-1045.
Question 791
High Yield
A 3-year-old child has bilateral genu varum and short stature. Radiographs show physeal widening and generalized osteopenia. The femora and tibiae show anterolateral bowing. Laboratory studies show low normal serum calcium values, significantly decreased serum phosphate levels, and normal parathyroid hormone (PTH), alkaline phosphatase, and vitamin-D levels. These findings are consistent with
Detailed Explanation
Children with vitamin D-resistant rickets are short in stature and have genu varum, physeal widening, and generalized osteopenia. The abnormality in inherited vitamin D-resistant rickets is the renal tubule's inability to resorb phosphate leading to hypophosphatemia. Laboratory findings in the condition are normal or near normal serum calcium values, significantly decreased serum phosphate levels, elevated alkaline phosphatase levels, and normal PTH and vitamin-D levels. The most common form is inherited as an X-linked dominant trait. Nutritional rickets has a normal or low serum phosphate levels, normal or low serum calcium values, and decreased levels of 25(OH) vitamin D and 1,25-dihydroxyvitamin D. Hypophosphatasia is a rare condition characterized by a deficiency of alkaline phosphatase in the serum and tissues, leading to generalized abnormal mineralization of bone. Primary hyperparathyroidism usually is caused by a parathyroid adenoma, and the child generally has abdominal problems and hypercalcemic crisis. Laboratory findings include elevated serum calcium values, alkaline phosphatase levels, and PTH levels, and decreased serum phosphate levels. Children with renal osteodystrophy tend to have genu valgum, and laboratory findings include elevated serum phosphate, alkaline phosphatase, and PTH levels, and low serum calcium values. Findings of renal disease include elevated BUN and creatinine. Herring JA: Metabolic and endocrine bone diseases, in Herring JA (ed): Tachdjian's Pediatric Orthopaedics, ed 3. Philadelphia, PA, WB Saunders, 2002, pp 1686-1710.
Question 792
High Yield
What is the most common primary malignant tumor of bone in childhood?
Detailed Explanation
Osteosarcoma is the most common primary malignant tumor of bone in childhood, followed by Ewing's sarcoma. Rhabdomyosarcoma is a soft-tissue sarcoma of childhood. Chondrosarcoma rarely occurs in childhood. Osteochondroma is a benign tumor of bone. Simon MA, Springfield DS, et al: Osteogenic Sarcoma: Surgery for Bone and Soft Tissue Tumors. Philadelphia, PA, Lippincott Raven, 1998, p 266.
Question 793
High Yield
A 32-year-old man has a closed oblique displaced fracture at the junction of the lower and middle third of the humeral shaft and a complete radial nerve palsy. Closed reduction is performed and is felt to be acceptable. Management of the radial nerve palsy should consist of
Detailed Explanation
In patients who have radial nerve dysfunction associated with a closed humeral fracture, nerve function usually will return to normal without surgical exploration. If clinical findings or electromyographic studies show no improvement at 3 months, surgical exploration and repair can be performed. Tendon transfers are performed if nerve repair is deemed unsuccessful. Pollock FH, Drake D, Bovill EG, et al: Treatment of radial neuropathy associated with fractures of the humerus. J Bone Joint Surg Am 1981;63:239-243.
Question 794
High Yield
An 86-year-old woman sustained a fracture of the humerus and underwent surgical fixation 8 weeks ago. There was no radial nerve function below the elbow after surgery. Radiographs are shown in Figures 51a and 51b. What is the most appropriate management at this time?
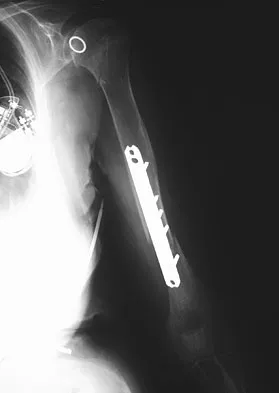
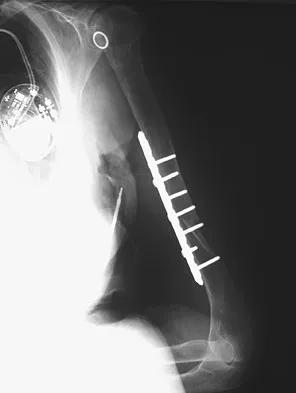
Detailed Explanation
Most radial nerve palsies associated with closed fractures of the humerus resolve spontaneously, including Holstein-Lewis lesions (radial nerve palsy associated with oblique distal third fractures of the humerus). Initial sign of recovery at the brachioradialis may not occur for 4 months. There has been no evidence of deleterious effects occurring during this observation period. There are advocates of early exploration of the nerve. Exploration in the intermediate period between 1 and 4 months is not supported. As overall alignment of the fracture is acceptable, there is no need for hardware exchange until nonunion is clearly identified. Shao YC, Harwood P, Grotz MR, et al: Radial nerve palsy associated with fractures of the shaft of the humerus: A systematic review. J Bone Joint Surg Br 2005;87:1647-1652.
Question 795
High Yield
Examination of a 30-year-old professional singer who has persistent neck and shoulder pain reveals a positive Hoffman's sign and clonus because of anterior C2-3 cord compression. The MRI scan shown in Figure 11a and the cervical CT scan shown in Figure 11b reveal focal anterior cord compression at the C2-3 level. Which of the following surgical approaches would least affect her professional career?
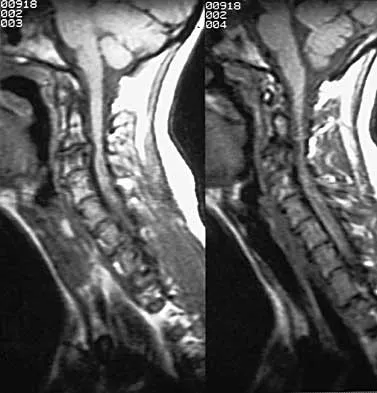
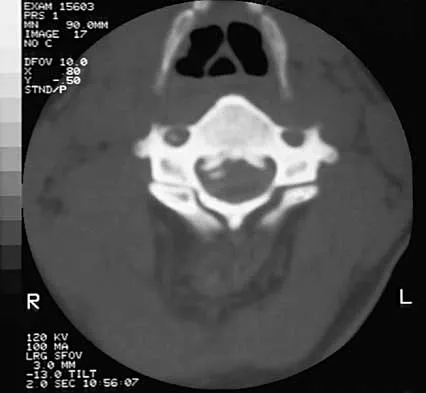
Detailed Explanation
Protection of the superior laryngeal nerve is critical in a professional singer. The nerve is easily injured with retraction when using vertical extension of common anterior surgical approaches to gain exposure to the C2-3 level. McAfee and associates reported on 17 patients with C1-2 and C2-3 pathology. They used a modified submandibular approach as an anterior retropharyngeal exposure with modification of the superior extension of the Smith-Robinson technique that allows visualization of the superior laryngeal nerve and surrounding structures. No incidences of superior laryngeal nerve injury were recorded. The transoral approach should be avoided because of the high rate of infection and limited exposure. McAfee PC, Bohlman HH, Reilly LH Jr, Robinson RA, Southwick WO, Nachlas NE: The anterior retropharyngeal approach to the upper part of the cervical spine. J Bone Joint Surgery Am 1987;69:1371-1383.
Question 796
High Yield
What is the mechanism of action of an intramuscular injection of botulinum type A toxin in reducing spasticitiy?
Detailed Explanation
The use of intramuscular botulinum type A toxin has been shown to be a useful adjuvant in the management of dynamic deformity in patients with cerebral palsy. Botulinum type A toxin is a neurotoxin produced by Clostridium botulinum that works by interfering with presynaptic acetylcholine release at cholinergic nerve terminals. At the cellular level, the mechanism involves endocytosis of the intact botulinum toxin molecule by cells in the end plate, followed by disulfide cleavage and translocation of the light chain into the cytosol where it disrupts the normal binding of the synaptosomal vesicles to the axon terminal membrane. Neither the nerve terminal nor the neuromuscular junction is damaged. The muscle paralysis is reversible and dose-dependent. Baclofen is a neuropharmacologic agent that functions as a GABA agonist. Dorsal rhizotomy is a neurosurgical procedure that reduces spasticity by dividing afferent (excitatory) fibers in the posterior rootlet of the spinal nerves. Koman LA, Mooney JF III, Smith B, Goodman A, Mulvaney T: Management of cerebral palsy with botulinum-A toxin: Preliminary investigation. J Pediatr Orthop 1993;13:489-495.
Question 797
High Yield
A 64-year-old woman has left wrist pain and deformity after falling on her hand. Examination shows intact skin and no neurologic or vascular injuries. Radiographs are shown in Figures 43a and 43b. What is the most appropriate management for the injury?
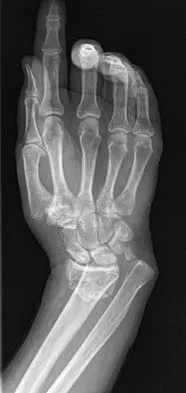
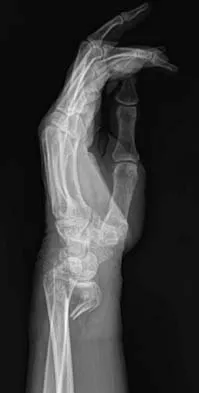
Detailed Explanation
The patient has a volar displaced two-part intra-articular distal radial fracture-dislocation of the wrist. Although a closed reduction is usually easily obtained, it is very difficult to maintain the reduction without internal fixation. The approach is determined by the direction of the dislocation, in this case volar. Stabilization with a buttress plate neutralizes the axial loading forces on the fractured fragment. A dorsal placed angular stable plate will not provide this buttress effect and will make the reduction difficult.
Question 798
High Yield
A 40-year-old man underwent an ankle arthroscopy 6 months ago for a talus osteochondral defect. He continues to have pain and burning on the lateral portal but states that the pain is now more superficial than his original pain. Examination reveals that he has shooting pain to his medial foot and ankle when his lateral portal is tapped. A previous injection around the lateral portal gave him relief for about 2 weeks. What treatment will best eliminate his pain?
Detailed Explanation
The patient clearly has entrapment of the superficial peroneal nerve in the lateral portal. It is most likely only the medial branch by examination. If the nerve is in good condition, it can simply be released. If the nerve is cut or severely thinned, it is better excised and buried. The sural nerve most likely would be caught in a posterior-lateral portal. Jobe MT, Wright PE: Peripheral nerve injuries, in Canale ST (ed): Campbell's Operative Orthopaedics. St Louis, MO, Mosby, 1998, pp 3839-3844.
Question 799
High Yield
Which of the following positions of immobilization has been shown to best approximate the anterior labrum against the glenoid rim following anterior dislocation of the shoulder?
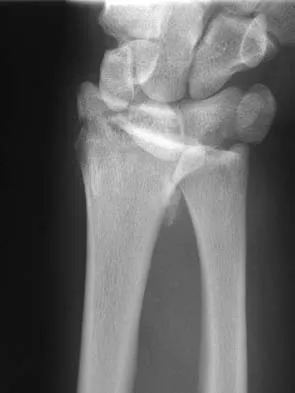
Detailed Explanation
Following anterior dislocation of the shoulder, the affected arm is typically placed in a sling with the shoulder in adduction and internal rotation. A recent study has shown that placement in this position actually results in laxity of the anterior supporting structures of the shoulder, allowing the postinjury hemarthrosis to push the labrum and capsular ligaments away from the anterior glenoid rim. Thus, immobilization in this position may actually impede healing of these structures. Alternatively, resting the arm in a position of adduction and external rotation allows the anterior supporting structures to abut against the anterior glenoid rim by forcing the hemarthrosis posteriorly. Placing the arm in this position following anterior dislocation is believed to allow for better healing of the anterior labrum and ligaments.
Question 800
High Yield
A 12-year-old pitcher has had a 2-month history of pain in his right dominant shoulder after throwing. He reports that the pain has gradually progressed to the point where he cannot throw without pain. He also notes that the pain now awakens him at night if he has been active. Anti-inflammatory drugs have failed to provide relief. Examination reveals no abnormalities except for some localized tenderness over the proximal humerus. Figures 32a and 32b show radiographs of both shoulders. What is the most likely diagnosis?
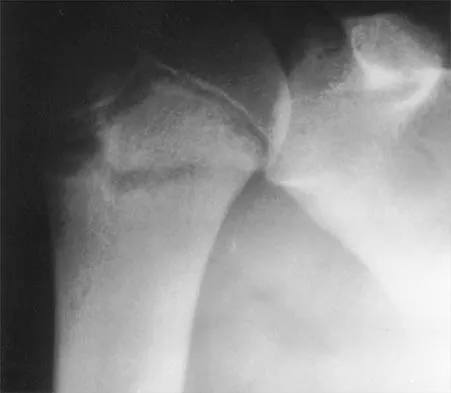
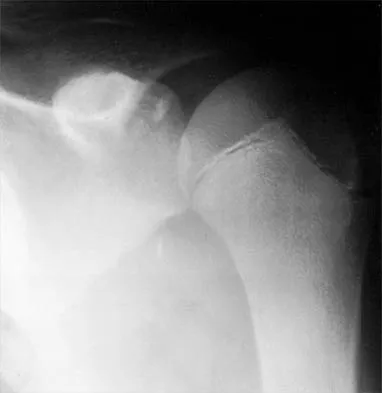
Detailed Explanation
The history, examination, and radiographs are pathognomonic for Little League shoulder, a stress syndrome of the proximal humeral physis caused by overuse. Complete fracture rarely occurs, and recovery usually occurs with rest. Night pain is always a serious concern and further work-up is needed if the patient does not respond to activity modification. Occult instability is not a real concern in this patient, although it should be included in the differential diagnosis. Albert MJ, Drvaric DM: Little League shoulder: Case report. Orthopedics 1990;13:779-781.
