00:00
Start Quiz
Question 26
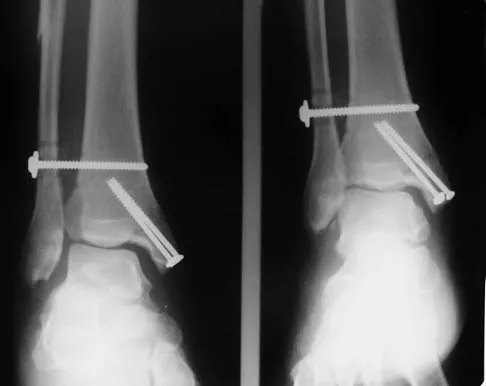
What nerve is at the highest risk for injury with a percutaneous repair of an Achilles tendon injury?
Explanation
Cadaver and clinical studies have shown that the sural nerve is at the highest risk for injury with a percutaneous repair of the Achilles tendon.
Question 27
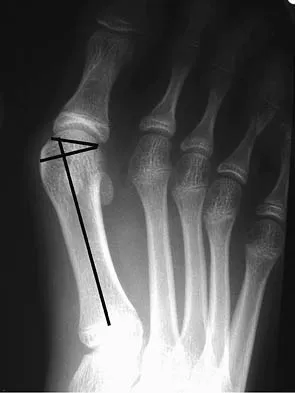
Which of the following tendons is the primary antagonist of the posterior tibialis tendon?
Explanation
The primary action of the posterior tibialis tendon is inversion of the foot; secondarily, it plantar flexes the ankle. The anterior tibialis tendon also inverts the foot and only partially antagonizes the posterior tibialis tendon. The primary action of the peroneus longus is plantar flexion of the first ray. It secondarily everts the posterior tibialis tendon. The action of the flexor digitorum longus tendon is synergistic with the posterior tibialis tendon. The primary action of the peroneus brevis tendon is eversion; therefore, it is the primary antagonist of the posterior tibialis tendon. Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993, pp 550-551.
Question 28
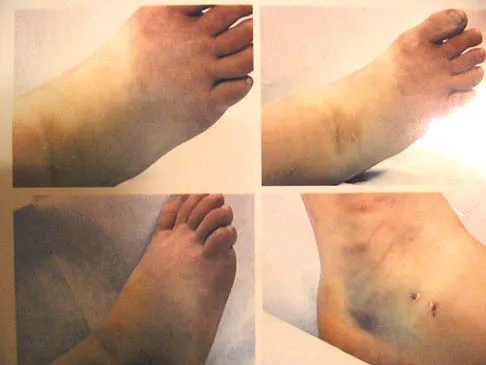
Which of the following is considered the most common infectious organism causing osteochondritis in pediatric puncture wounds of the foot?
Explanation
Pseudomonas aeruginosa is the most common infectious organism causing osteochondritis in pediatric puncture wounds of the foot. Eikenella corrodens is found in human bites, and Pasteurella multocida is characteristically seen with animal bites. Serratia marcescens and Proteus mirabilis have been reported but are much less likely. Jacobs RF, Adelman L, Sack CM, et al: Management of pseudomonas osteochondritis complicating puncture wounds of the foot. Pediatrics 1982;69:432-435.
Question 29
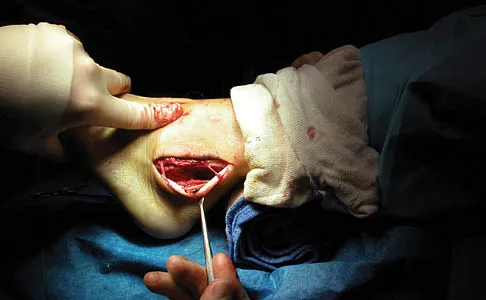
An 18-year-old man sustains an injury to his lateral ankle after being kicked while playing soccer. He reports persistent pain on the lateral ankle as well as a popping sensation with attempted ankle dorsiflexion and eversion. Which of the following structures anatomically restrains the retracted structure shown in Figure 12?
Explanation
The peroneus brevis and peroneus longus muscles are the main evertors of the hindfoot. As they descend along the posterior fibula, they pass through the retromalleolar sulcus, formed by the concavity of the retromalleolar fibula. This sulcus is deepened by a fibrocartilaginous rim. The superior peroneal retinaculum covers the fibular groove and stabilizes the peroneal tendons within the retromalleolar sulcus. It originates from the posterolateral ridge of the fibula and inserts onto the lateral calcaneus. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2003, pp 81-89.
Question 30
A 22-year-old man who sustained a Gustilo-Anderson grade IIIC open fracture of the right tibia and fibula was treated with an immediate open transtibial amputation. After two serial debridements, he underwent wound closure with a posterior myocutaneous soft-tissue flap. What is the preferred method of early rehabilitation?
Explanation
There is no evidence that early weight bearing enhances ultimate rehabilitation. At the other extreme, weight bearing should not be delayed for a prolonged period of time. In a young, healthy individual, the rigid plaster dressing appears to be the safest method of protecting the wound during the early postoperative period. If the wound appears to be secure, early partial weight bearing can be safely initiated. Burgess EM, Romano RL, Zettl JH: The Management of Lower Extremity Amputations. Washington, DC, US Government Printing Office, 1969, also at: www.prs-research.org.
Question 31
Figure 13 shows the clinical photograph of a 66-year-old man who has had an increasingly painful right foot deformity for the past 3 years. Examination reveals that the subtalar joint is fixed in 15 degrees of valgus, and forefoot supination can be corrected to 10 degrees from neutral. Nonsurgical management has failed to provide relief. Treatment should now consist of
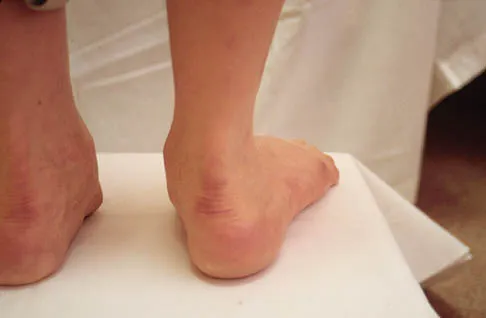
Explanation
The most important determining factor for correction of an adult flatfoot without an arthrodesis is the flexibility of the subtalar and transverse tarsal joints. Rigid deformities cannot be corrected with a medial sliding calcaneal osteotomy with FDL transfer or a subtalar arthroereisis. Isolated subtalar or talonavicular arthrodesis does not correct the deformities entirely. If the patient has forefoot supination that can be corrected to less than 7 degrees, an isolated subtalar fusion is a possible alternative.
Question 32
When evaluating a patient with hallux rigidus, what is the most important clinical factor indicating the need for an arthrodesis as opposed to a cheilectomy?
Explanation
Cheilectomy has been shown to provide satisfactory pain relief and improved function in long-term studies. It is important to select patients appropriately when choosing a cheilectomy versus an arthrodesis. Pain at the midrange of motion and loss of more than 50% of the metatarsal head cartilage are predictors of a poor outcome following cheilectomy, and these patients should receive an arthrodesis. Coughlin MJ, Shurnas PS: Hallux rigidus: Grading and long-term results of operative treatment. J Bone Joint Surg Am 2003;85:2072-2088.
Question 33
A patient who has recalcitrant medial plantar heel pain and pain directly over the medial side of the heel undergoes open release of the plantar fascia. After releasing a portion of the plantar fascia, the deep fascia of the abductor hallucis muscle is released to relieve pressure on which of the following structures?
Explanation
The deep fascia of the abductor hallucis muscle is released to relieve pressure on the first branch of the lateral plantar nerve. The tibial nerve lies more proximal to this area. The medial plantar nerve has already passed dorsally and medially, while the sural nerve lies on the lateral side of the foot. The flexor hallucis brevis muscle lies deep to the plantar fascia, not the abductor fascia. Baxter DE, Pfeffer GB: Treatment of chronic heel pain by surgical release of the first branch of the lateral plantar nerve. Clin Orthop 1992;279:229-236.
Question 34
A 47-year-old woman has a painful bunion of the right foot, and shoe wear modifications have failed to provide relief. Examination reveals a severe hallux valgus with dorsal subluxation of the second toe. Radiographs are shown in Figures 14a and 14b. The most appropriate management should include
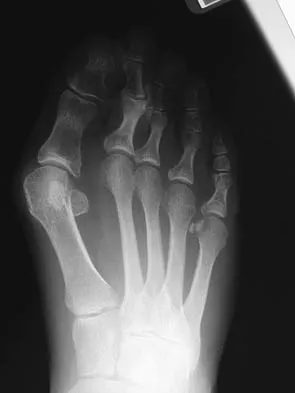
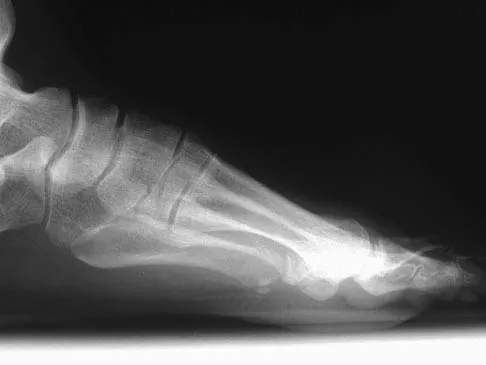
Explanation
The radiographs do not show significant arthrosis of the hallux metatarsophalangeal joint; therefore, arthrodesis is unnecessary. Orthotics will not correct the deformity. A distally based osteotomy will not achieve sufficient correction of the incongruity of deformity, and a Keller resection is not indicated in the younger population. The treatment of choice is a proximal metatarsal osteotomy with second toe correction.
Question 35
What is the most appropriate orthosis for hallux rigidus?
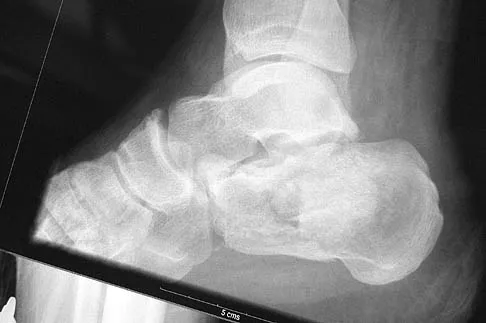
Explanation
A Morton's extension limits excursion of the first metatarsophalangeal joint. It also functions as a ground reaction stabilizer during the toe-off phase of gait and thus reduces torque and joint reaction force at the first metatarsophalangeal joint. The metatarsal arch pad and full-length semi-rigid longitudinal arch support may help by dorsiflexing the first metatarsal relative to the phalanx and thus decompress the first metatarsophalangeal joint. However, they are not as biomechanically effective as the Morton's extension. Both medial hindfoot and lateral forefoot posting are contraindicated because they increase ground reaction at the first metatarsophalangeal joint. Coughlin MJ: Arthritides, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, p 611.
Question 36
While experts disagree whether the postpolio syndrome is caused by a reactivation of the dormant virus or by an attritional aging phenomena of muscles that have been overworked over a period of time, both groups recommend which of the following guidelines for optimizing function in this population?
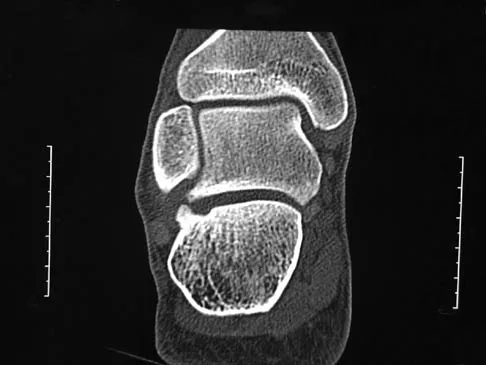
Explanation
Most leaders in orthopaedic surgery support Jacqueline Perry's theory that the postpolio syndrome is an attritional degenerative process that is the result of overuse of muscles and joints that are unable to adequately tolerate overload, and have little functional reserve. For that reason, aerobic conditioning and exercise are important. Overload and exhaustion of involved muscles should be avoided.
Question 37
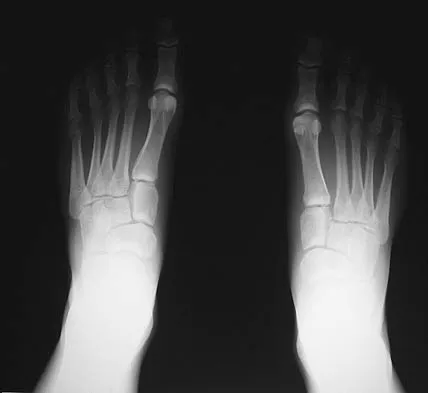
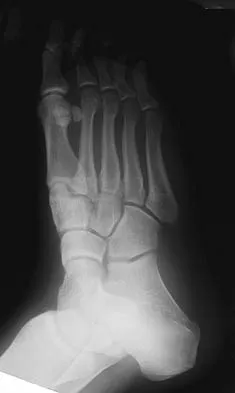
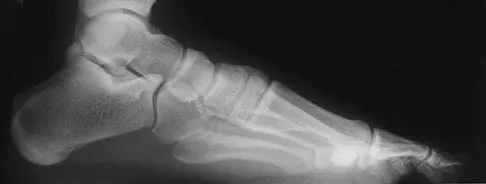
Figures 15a through 15c show the radiographs of a 23-year-old football player who was injured when another player fell on his flexed and planted foot. He reports severe pain in the midfoot with a feeling of numbness on the dorsum of the foot, and he is unable to bear weight on the limb. Examination reveals mild swelling. Management should consist of
Explanation
Myerson and associates studied the outcomes of 19 patients with tarsometatarsal joint injuries during athletic activity. Injuries were classified as first- or second-degree sprains of the tarsometatarsal joint or a third-degree sprain with diastasis between the metatarsals or cuneiforms. Poor functional results were seen in those with a delay in diagnosis and with inadequate treatment. For patients with third-degree sprains, poor results were obtained with nonsurgical management. These patients required open reduction and internal fixation for optimal return to function. The anatomic reduction is critical to the outcome; therefore, open reduction is preferred. Baxter DE: The Foot and Ankle in Sport, ed 1. St Louis, MO, Mosby, 1995, pp 107-123. Curtis MJ, Myerson M, Szura B: Tarsometatarsal joint injuries in the athlete. Am J Sports Med 1993;21:497-502. Kuo RS, Tejwani NC, DiGiovanni CW, et al: Outcome after open reduction and internal fixation of Lisfranc joint injuries. J Bone Joint Surg Am 2000;82:1609-1618.
Question 38
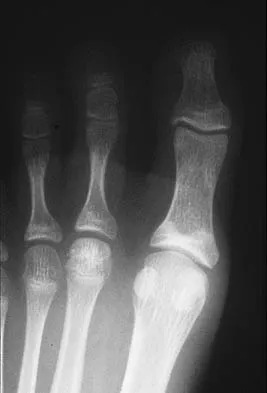
Which of the following methods best aids in diagnosis of an interdigital neuroma?
Explanation
History and physical examination are still the gold standard for diagnosis of an interdigital neuroma. Ultrasound and MRI may be helpful adjuncts but are dependent on equipment and operator expertise. Web space injection may be helpful for diagnostic and therapeutic purposes. Electromyography and nerve conduction velocity studies are of little benefit for distal lesions. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 145-147.
Question 39
A 58-year-old man has had a 3-year history of recurrent ulcerations of the left ankle and instability despite multiple attempts at custom bracing, contact casting, and surgical debridement. He has an ankle-brachial index of 0.76. A clinical photograph and radiographs are shown in Figures 16a through 16c. Treatment should now consist of
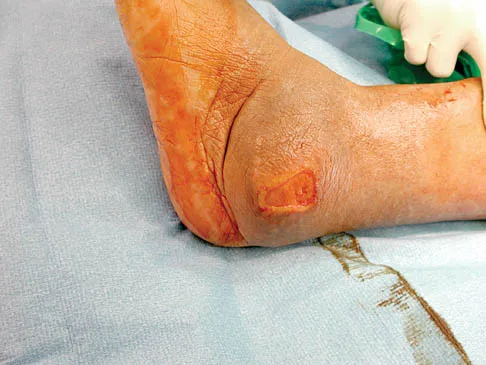
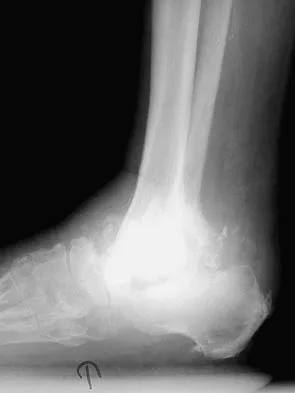
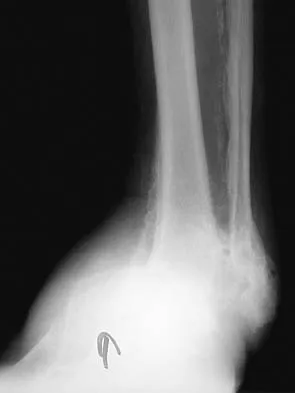
Explanation
Nonsurgical management has failed to provide relief; therefore, the treatment of choice is arthrodesis with an intramedullary nail. Amputation may be indicated if the arthrodesis fails. The patient does have adequate circulation for an attempt at salvage. Total ankle arthroplasty is not indicated in a neuropathic patient. Pinzur MS, Kelikian A: Charcot ankle fusion with a retrograde locked intramedullary nail. Foot Ankle Int 1997;18:699-704.
Question 40
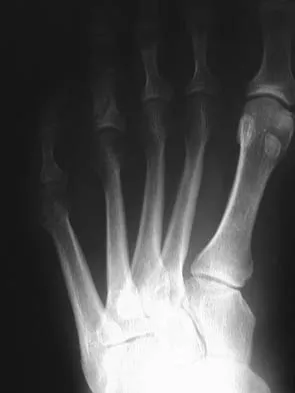
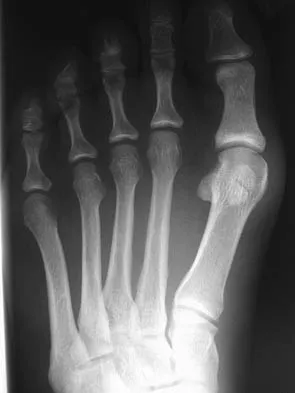
Figures 17a and 17b show the radiographs of a 32-year-old professional athlete who sustained an injury to the first metatarsal. A view of the opposite noninjured side is shown in Figure 17c. Management of the fracture should consist of
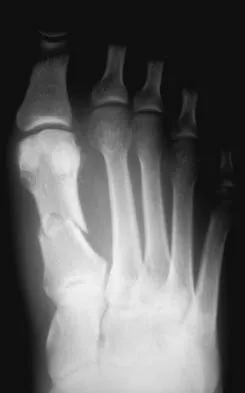
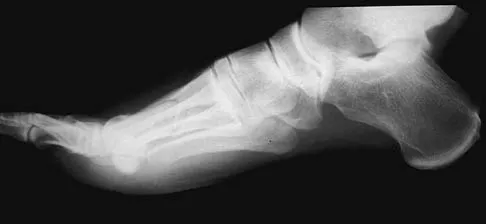
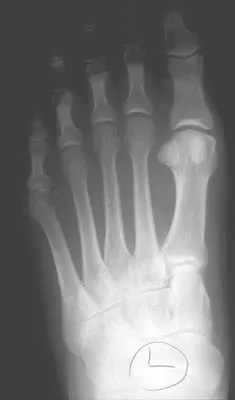
Explanation
Parameters for first metatarsal fracture management are different than for shaft fractures of the central second, third, and fourth metatarsals. The first metatarsal carries a greater load and if malunited, can create transfer lesions by virtue of uneven weight distribution; therefore, nonsurgical management is not indicated for this patient. Percutaneous pinning is not as likely to result in an anatomic reduction as open reduction and internal fixation. As his livelihood depends on an expeditious return to function, the choice of open reduction and internal fixation allows for earlier motion and rehabilitation. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 64-65.
Question 41
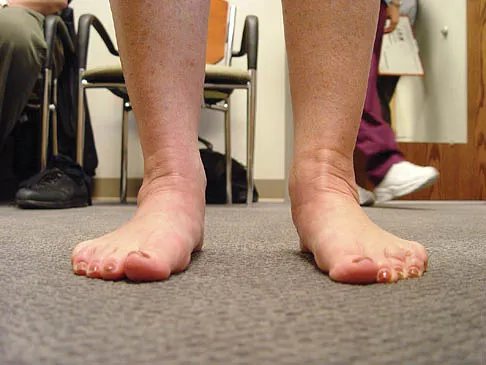
Which of the following are considered appropriate nonsurgical bracing/orthotic options for a supple adult-acquired flatfoot deformity with forefoot abduction, secondary to posterior tibial tendon insufficiency?
Explanation
The initial stages of posterior tibial tendon insufficiency, where the deformity remains supple, may be treated with bracing or an orthotic for pain relief. The Arizona brace was introduced in 1988, and assists in pain relief and deformity correction by minimizing hindfoot valgus alignment, lateral calcaneal displacement, and medial ankle collapse. It is particularly helpful in those patients with advanced disease that cannot tolerate an ankle-foot orthosis. All other choices are incorrect because of the addition of lateral posting, which is not advantageous in valgus deformities. The addition of medial posting to any of the above choices would render them correct alternatives. A heel lift is applicable in Achilles tendon disorders, not posterior tibial tendon disorders. Chao W, Wapner KL, Lee TH, et al: Nonoperative management of posterior tibial tendon dysfunction. Foot Ankle Int 1996;17:736-741.
Question 42
A 28-year-old man underwent open reduction and internal fixation of a closed, displaced, intra-articular calcaneal fracture 8 weeks ago. Examination now reveals that the lateral wound is red and draining purulent material. Cultures obtained from the wound grow out Staphylococcus aureus. Radiographs show early healing of the fracture. What is the next most appropriate step in management?
Explanation
Intravenous antibiotics alone will not adequately treat this infection. At 8 weeks after surgery, the hardware must be removed because Staphylococcus aureus is a virulent microbe. VAC therapy alone is not adequate without debridement and hardware removal, but it may play a role in postoperative wound care. Calcanectomy is a salvage procedure for calcaneal osteomyelitis or recalcitrant heel ulceration. Benirschke SK, Kramer PA: Wound healing complications in closed and open calcaneal fractures. J Orthop Trauma 2004;18:1-6. Lim EV, Leung JP: Complications of intra-articular calcaneal fractures. Clin Orthop 2001;391:7-16.
Question 43
A 37-year-old man with a history of congenital flatfoot reports worsening pain on the medial aspect of his ankle for the past year. The pain is worse with weight bearing and is better with rest and the use of an ankle brace. What findings are shown on the MRI scans shown in Figures 18a through 18c?
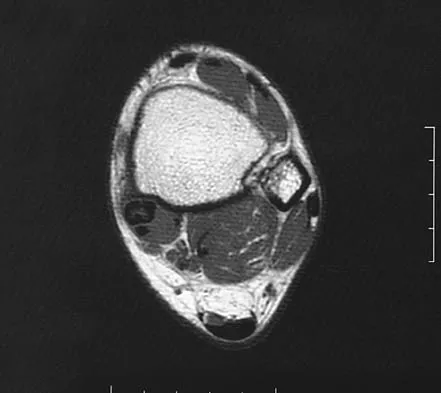
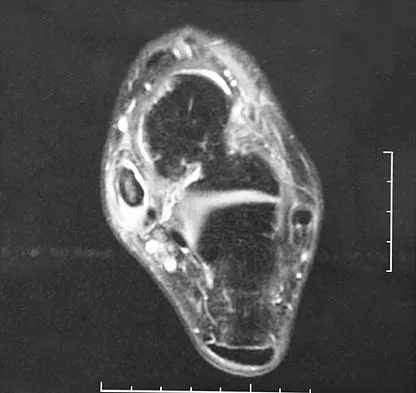
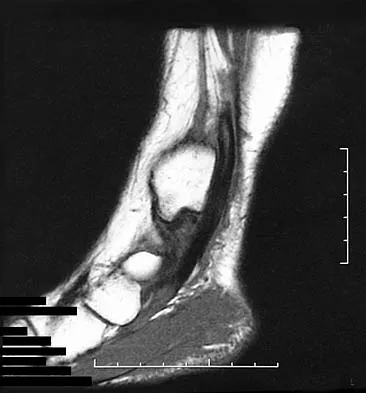
Explanation
The MRI scans reveal an enlarged posterior tibial tendon, with degenerative signal within the tendon and an excessive amount of fluid in its sheath. This is a type II tear, as noted by Conti and associates, which is the most commonly seen tear. Slovenkai MP: Clinical and radiographic evaluation (Adult flatfoot: Posterior tibial tendon dysfunction). Foot Ankle Clin 1997;2:241-260.
Question 44
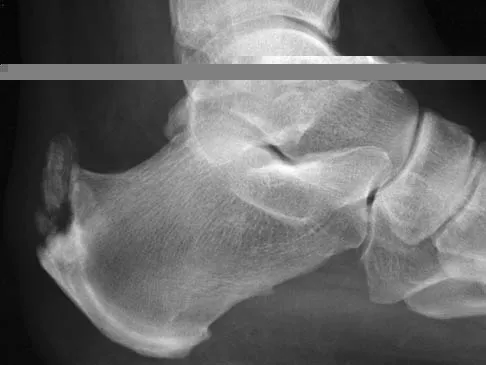
A 60-year-old man reports increasing pain in his right foot with limited ankle dorsiflexion and anterior ankle pain after sustaining a fracture of the calcaneus in a fall several years ago. Bracing, nonsteroidal anti-inflammatory drugs, and cortisone injections have failed to provide significant relief. Radiographs are shown in Figures 19a and 19b. What is the next most appropriate step in management?
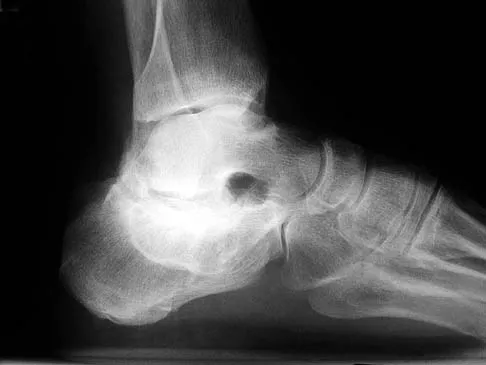
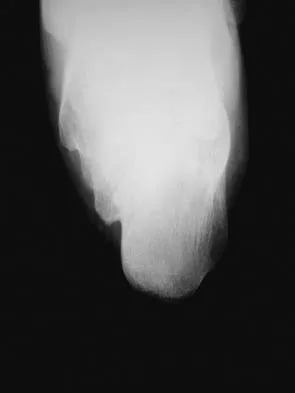
Explanation
Following a calcaneal fracture, the patient has severe subtalar arthritis with loss of talar declination and shortening of the heel; therefore, the treatment of choice is subtalar distraction arthrodesis. Orthotics will not provide significant relief as bracing has failed. Ankle arthrodesis will not be beneficial because the arthritis is in the subtalar joint. Subtalar arthroscopy would only be helpful for a small area of arthrosis, and calcaneal osteotomy would not be beneficial given the extent of the arthritis of the subtalar joint.
Question 45
A 58-year-old woman sustained a ruptured Achilles tendon 1 year ago, and management consisted of an ankle-foot orthosis. She now reports increasing difficulty with ambulation and increasing pain. An MRI scan shows a 6-cm defect in the right Achilles tendon. Management should now consist of
Explanation
With a gap of less than 4 cm, a V-Y repair would be appropriate without a tendon transfer. For gaps greater than 5 cm, a lengthening with augmentation is the most appropriate treatment. Therefore, the treatment of choice is an Achilles tendon turndown with flexor hallucis longus tendon transfer. The plantaris tendon is not a strong enough repair, and direct repair is not possible given the large defect in the Achilles tendon. Continued use of the ankle-foot orthosis will not provide adequate relief for this patient.
Question 46
A 29-year-old woman reports dysesthesias and burning after undergoing bunion surgery that consisted of a proximal crescentic first metatarsal osteotomy 6 months ago. Examination reveals a positive Tinel's sign at the proximal aspect of the healed incision. What injured nerve is responsible for her continued symptoms?
Explanation
Painful incisional neuromas after bunion surgery frequently involve the dorsomedial cutaneous branch of the superficial peroneal nerve. This is the medial branch of the superficial peroneal nerve that terminates as the dorsomedial cutaneous nerve to the hallux. Branches of the deep peroneal nerve to this area are rare, and no branches to this area exist from the sural nerve. The saphenous nerve branches are generally more proximal, and the medial plantar nerve lies plantarly. Kenzora JE: Sensory nerve neuromas: Leading to failed foot surgery. Foot Ankle 1986;7:110-117.
Question 47
Figure 20 shows the clinical photograph of a man who has had diabetes mellitus controlled with oral medication for the past 10 years. He wears soft-soled shoes and only uses leather-soled shoes for important business meetings. Examination reveals palpable dorsalis pedis and posterior tibial pulses, although they are somewhat diminished. He is insensate to pressure with the Semmes-Weinstein 5.07 monofilament. The ulcer heals after treatment with a full contact cast. What is the best course of action at this time?
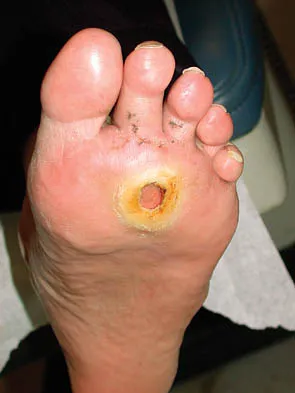
Explanation
The patient has not undergone a trial of foot-specific patient education and accommodative/therapeutic shoe wear. He must use therapeutic shoe wear at all times, as even the occasional use of pressure-concentrating shoe wear has a high likelihood of leading to the development of a diabetic foot ulcer. Pinzur MS, Kernan-Schroeder D, Emmanuele NV, et al: Development of a nurse-provided health system strategy for diabetic foot care. Foot Ank Int 2001;22:744-746. Pinzur MS, Shields N, Goelitz B, et al: American Orthopaedic Foot & Ankle Society shoe survey of diabetic patients. Foot & Ankle Int 1999;20:703-707.
Question 48
Figures 21a and 21b show the clinical photograph and radiograph of a 15-year-old girl who has a deformity of her feet. Her parents are concerned because there is a family history of Charcot-Marie-Tooth disease. The patient reports some mild instability of the ankle and has noticed mild early callosities; however, she is not having any significant pain. Coleman block testing reveals a forefoot valgus and supple hindfoot. She has weakness to eversion and dorsiflexion. Initial management should consist of
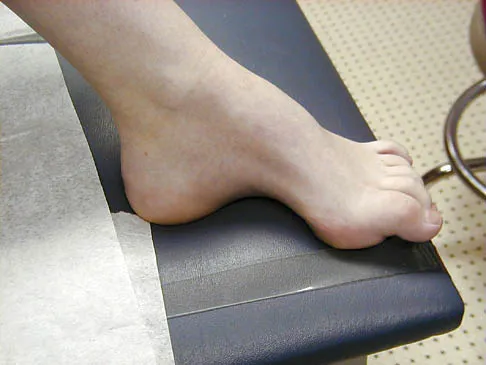
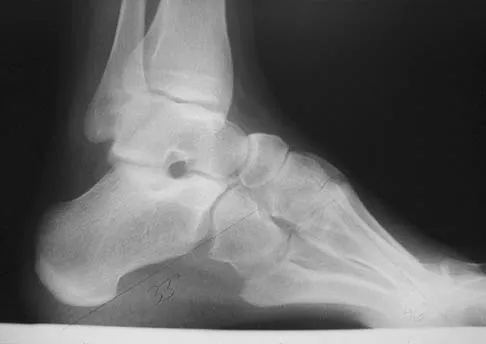
Explanation
Initial management of a young patient with a cavovarus deformity of the foot and a family history of Charcot-Marie-Tooth disease should focus on mobilization and strengthening of the weakening muscular units and an accommodative insert. Surgical intervention should be delayed until progression of the deformity begins to cause symptoms and/or weakness of the muscular units, resulting in contractures of the antagonistic muscle units. Pinzur MS: Charcot's foot. Foot Ankle Clin 2000;5:897-912. Holmes JR, Hansen ST Jr: Foot and ankle manifestations of Charcot-Marie-Tooth disease. Foot Ankle 1993;14:476-486.
Question 49
A 50-year-old woman reports a burning sensation on the plantar aspect of her left forefoot, distal to the metatarsal heads between her third and fourth digits. Palpation of the third web space recreates her symptoms. Which of the following will most accurately aid in confirming a diagnosis?
Explanation
The diagnosis of an interdigital neuroma is best made by a thorough history and careful physical examination. Radiographs are helpful in excluding other pathologic processes such as a metatarsal stress fracture. MRI and ultrasound have both been reported to aid in the diagnosis of an interdigital neuroma. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2003, pp 145-151.
Question 50
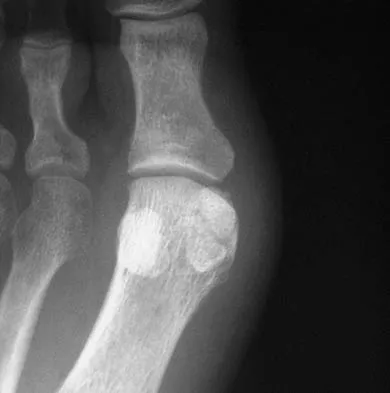
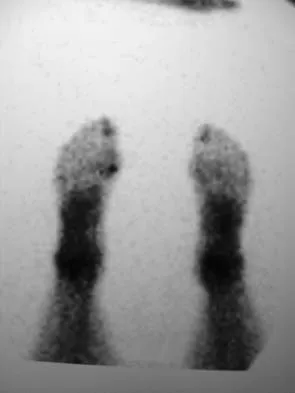
A 21-year-old collegiate track athlete increased her training 4 months ago in anticipation of starting the season. Two months into her training program, she reported pain followed by a 1-month history of diffuse pain in the first metatarsophalangeal joint that was aggravated by weight bearing. A removable walker boot partially relieved the pain, and she was able to complete the season. Her pain has now returned; however, she denies any history of injury. Examination reveals tenderness over the medial sesamoid but no deformities. A radiograph and bone scan are shown in Figures 22a and 22b. What is the best treatment option at this time?
Explanation
The radiograph reveals either a fractured or bipartite sesamoid. The bone scan shows asymmetrically increased uptake over the medial sesamoid. Given the history and physical examination, a stress fracture is the most likely diagnosis. Medial sesamoidectomy reliably improves pain, and athletes return to sports on an average of 7 weeks after excision. Immobilization typically requires more than 4 to 8 weeks and is not always successful; however, it would be appropriate management for a patient who is not an elite athlete. Sanders R: Fractures of the midfoot and forefoot, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby, 1999, pp 1601-1603.
