00:00
Start Quiz
Question 76
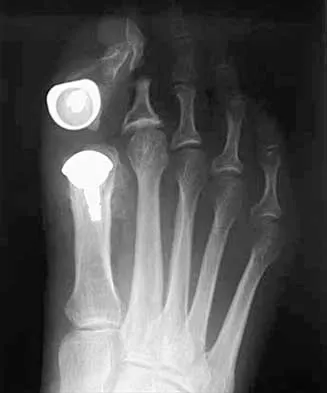
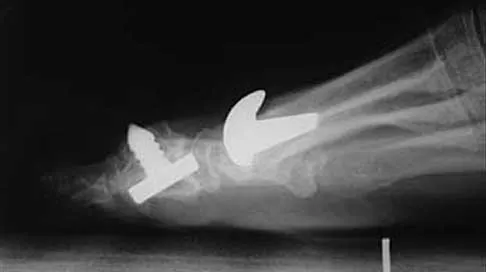
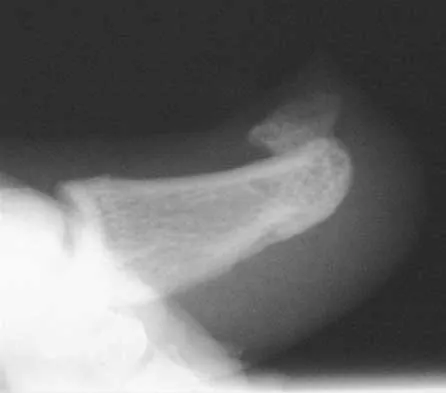
A 50-year-old woman who underwent a joint replacement of the hallux metatarsophalangeal joint 6 months ago now has pain and swelling about the great toe. Radiographs are shown in Figures 39a and 39b. What is the next most appropriate step in management?
Explanation
The radiographs show displacement of the prosthesis, and there has been large amounts of bone resected to insert the implant. Arthrodesis is indicated with interposition bone graft to stabilize the joint and restore length to the first ray.
Question 77
What is the most common foot and ankle deformity in patients with arthrogryposis?
Explanation
Clubfoot (talipes equinovarus) in patients with arthrogryposis is a rigid and resistant deformity. However, multiple studies document limited success with nonsurgical management. Manipulation and casting are generally a preliminary treatment before surgery; successful correction will most like require a talectomy. Guidera KJ, Drennan JC: Foot and ankle deformities in arthrogryposis multiplex congenita. Clin Orthop 1985;194:93-98. Handelsman JE, Badalamente MA: Neuromuscular studies in clubfoot. J Pediatr Orthop 1981;1:23-32.
Question 78
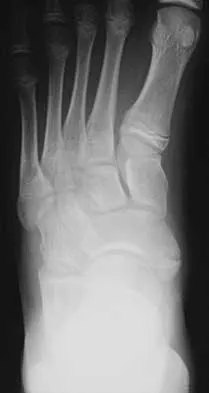
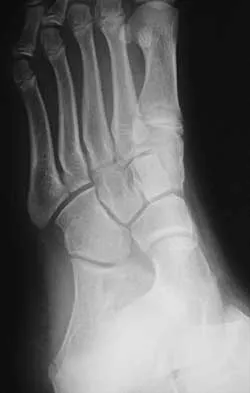
A 16-year-old girl has had pain and swelling along the medial arch of her left foot for the past 3 months. She also reports pain from shoe wear and while running. Nonsteroidal anti-inflammatory drugs have failed to provide relief. Radiographs are shown in Figures 40a through 40c. What is the next most appropriate step in management?
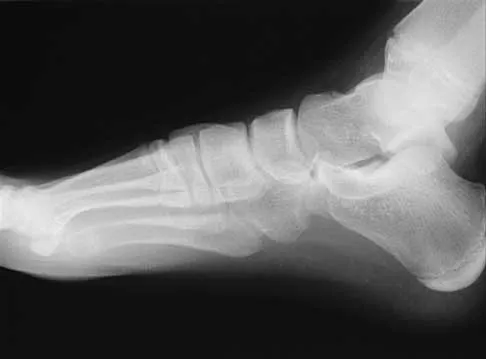
Explanation
Nonsurgical management of a symptomatic accessory navicular should be attempted prior to surgery. Good relief is often obtained with a semi-rigid orthosis with a medial arch support. Myerson MS: Foot and Ankle Disorders. Philadelphia, PA, WB Saunders, 2000, p 655.
Question 79
A 28-year-old man was shot in the foot with a .22 caliber handgun approximately 2 hours ago. Examination reveals an entrance wound dorsally and a plantar exit wound. The foot is neurovascularly intact. Radiographs reveal a nondisplaced fracture of the third metatarsal. Soft-tissue management for this injury should consist of
Explanation
The patient has sustained a low-velocity, low-caliber gunshot wound to the foot. Because the injury occurred within a period of 8 hours, this is classified as a type I wound. Several studies support the use of surface debridement, cleansing, and sterile dressings as the treatment of choice. More aggressive measures are reserved for high-velocity injuries and shotgun injuries. Brettler D, Sedlin ED, Mendes DG: Conservative treatment of low velocity gunshot wounds. Clin Orthop 1979;140:26-31. Hampton OD: The indications for debridement of gunshot bullet wounds of the extremities in civilian practice. J Trauma 1961;1:368-372.
Question 80
The photomicrograph seen in Figure 41 shows which of the following conditions?
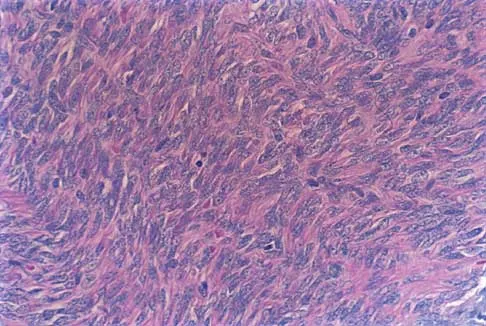
Explanation
The photomicrograph shows a synovial cell sarcoma with a characteristic histology of a biphasic pattern of pleomorphic spindle cells and well-differentiated cuboidal to columnar cells forming gland-like spaces. The glandular zones contain mucous-like material that stains positively with periodic acid Schiff. Microscopic calcifications are usually found. Synovial cell sarcoma has a high rate of local recurrence as well as metastases. It is the most common malignancy found in the foot. Krall RA, Kostianovsky M, Patchefsky AS: Synovial sarcoma: A clinical, pathological and ultrastructural study of 26 cases supporting the recognition of a monophasic variant. Am J Surg Pathol 1981;5:137-151.
Question 81
A 33-year-old man had his foot run over by a forklift 1 hour ago. Examination reveals that the head of the fifth metatarsal is extruded through the plantar aspect of the foot. The foot is severely swollen and pale, there is no sensation in the toes, and the pulses are not palpable. Radiographs are shown in Figures 42a and 42b. Emergent management should consist of
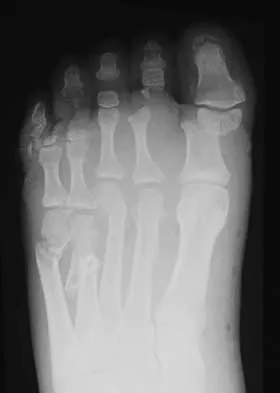
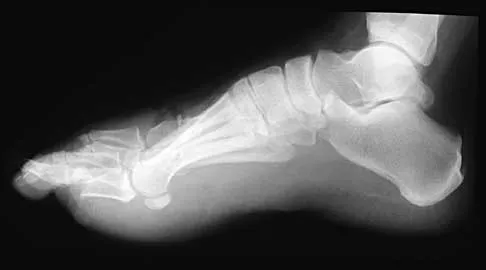
Explanation
Following a severe crush injury, the patient has an acute compartment syndrome. Even though there is an open fracture, this is not sufficient to decompress the compartment syndrome. Therefore, splinting and observation are not appropriate. The surgical treatment of choice is fasciotomy with fixation of the multiple fractures. A primary amputation is not indicated because there is potential for salvage of this devastating injury. Fakhouri AJ, Manoli A II: Acute foot compartment syndromes. J Orthop Trauma 1992;6:223-228. Myerson MS: Management of compartment syndromes of the foot. Clin Orthop 1991;271:239-248.
Question 82
A 2-year-old boy has been referred for musculoskeletal evaluation. Examination reveals shortened proximal limbs, hip and knee flexion contractures, an abducted thumb, and ear abnormalities. His parents are concerned about his deformed feet. What is the most common foot deformity associated with this patient's diagnosis?
Explanation
The patient has diastrophic dysplasia. Affected individuals have rhizomelic short stature, cauliflower ears, severe joint contractures (especially knees and hips), hitchhiker's thumb, and a cleft palate. The most common foot abnormality is a rigid equinovarus deformity. Surgical results are poorer than those for idiopathic clubfeet and often require bony procedures or talectomy. Ryoppy S, Poussa M, Merikanto J, Marttinen E, Kaitila I: Foot deformities in diastrophic dysplasia: An analysis of 102 patients. J Bone Joint Surg Br 1992;74:441-444.
Question 83
A 31-year-old woman has a history of a painful ankle that has failed to respond to conservative management. She has associated night pain that is relieved with nonsteroidal anti-inflammatory drugs. MRI and technetium Tc 99m scans are consistent with an osteoid osteoma. Management should now consist of
Explanation
Surgical curettage or en bloc resection is the treatment of choice for osteoid osteoma. Night pain and relief of symptoms with nonsteroidal anti-inflammatory drugs are classic findings for osteoid osteoma. Donley BG, Philbin T, Rosenberg GA, Schils JP, Recht M: Percutaneous CT guided resection of osteoid osteoma of the tibial plafond. Foot Ankle Int 2000;21:596-598. Kenzora JE, Abrams RC: Problems encountered in the diagnosis and treatment of osteoid osteoma of the talus. Foot Ankle 1981;2:172-178.
Question 84
A 13-year-old girl has had pain in her ankle and difficulty with sporting activities for the past 6 months. Nonsteroidal anti-inflammatory drugs and use of a short leg cast have provided minimal relief. A radiograph and MRI scan are shown in Figures 43a and 43b. What is the next most appropriate step in treatment?
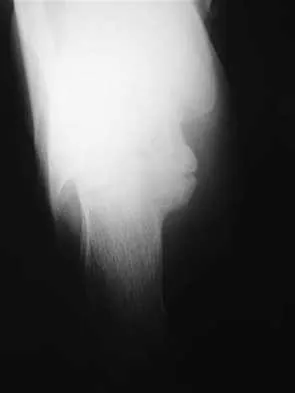
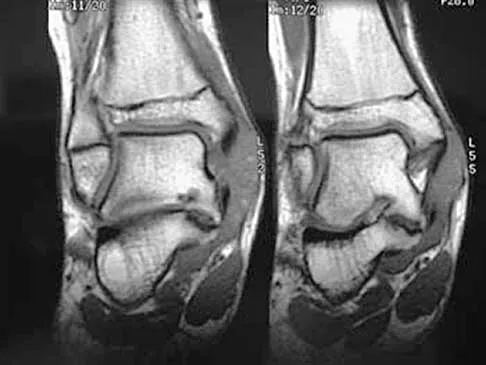
Explanation
The MRI scan shows an obvious talocalcaneal coalition of the medial facet. Because nonsurgical management has failed, surgical resection of the coalition is indicated. Arthrodesis would be indicated only if resection fails to relieve pain or if advanced degeneration of the hindfoot joints is present. McCormack TJ, Olney B, Asher M: Talocalcaneal coalition resection: A 10-year follow-up. J Pediatr Orthop 1997;17:13-15.
Question 85
A 16-year-old female dancer has persistent posterior ankle pain, particularly after a vigorous dancing schedule. Examination reveals tenderness both posteromedially and posterolaterally. MRI scans are seen in Figures 44a and 44b. What is the most likely diagnosis?
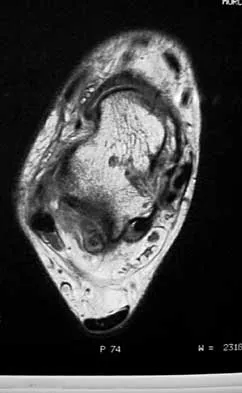
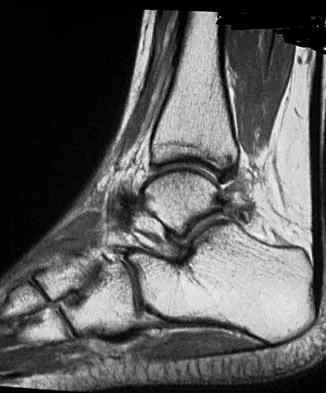
Explanation
Posterior ankle impingement or os trigonum syndrome is well described in dancers, and it is often associated with flexor hallucis longus tendinitis. High-quality MRI imaging will reveal the inflammation about the os trigonum and flexor hallucis longus tendinitis. Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont IL, American Academy of Orthopaedic Surgeons, 1998, pp 315-332.
Question 86
Which of the following nerves is most commonly injured during ankle arthroscopy?
Explanation
The superficial peroneal nerve, which is adjacent to the location of the lateral arthroscopic portal is most commonly injured. Ferkel RD, Heath DD, Guhl JF: Neurological complications of ankle arthroscopy. Arthroscopy 1996;12:200-208.
Question 87
An obese 56-year-old woman with hypertension has had posterior heel pain for the past 6 months. She also notes some enlargement over the posterior aspect of the heel. Examination reproduces pain with palpation at the insertion of the Achilles tendon. A lateral radiograph is shown in Figure 45. What is the most likely diagnosis?
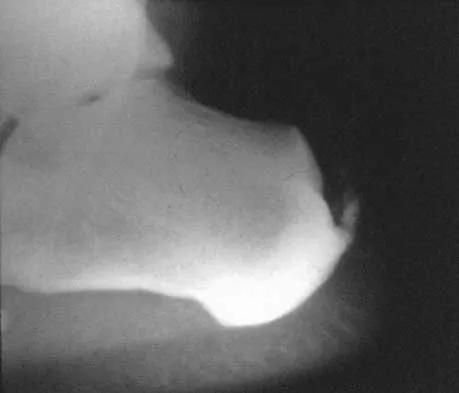
Explanation
The lateral radiograph shows a traction spur consistent with tendinopathy of the Achilles tendon. There is no displacement of the spur to suggest a rupture of the Achilles tendon, and os trigonum is not seen on the radiograph. The examination findings are not consistent with nerve entrapment. Schepsis AA, Wagner C, Leach RE: Surgical management of Achilles tendon overuse injuries: A long-term follow-up study. Am J Sports Med 1994;22:611-619.
Question 88
A 42-year-old woman has a history of nontraumatic ankle swelling with tenderness over the Achilles tendon and plantar fascia. She reports that while vacationing in Connecticut 2 months ago she noted the presence of a "red bull's eye" rash. Management should consist of
Explanation
The most likely diagnosis is Lyme disease because of the patient's recent vacation in an area with a high risk of exposure. The most effective treatment is doxycycline. Neu HC: A perspective on therapy of Lyme infection. Ann NY Acad Sci 1988;539:314-316.
Question 89
A 50-year-old woman has a painful hallux valgus and a painful callus beneath the second metatarsal head. A radiograph is shown in Figure 46. To correct these problems, treatment of the great toe deformity should consist of
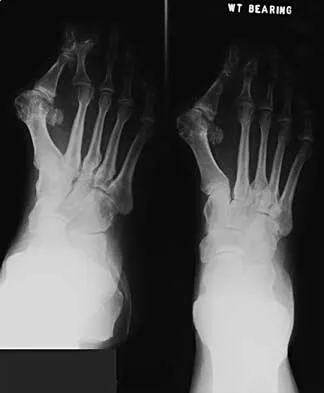
Explanation
The patient has a significant hallux valgus and instability of the first ray, causing transfer metatarsalgia to the second metatarsal head. Therefore, the best procedure is fusion of the metatarsal cuneiform joint with soft-tissue realignment of the first metatarsophalangeal joint. This procedure provides the best chance of relieving symptoms under the second metatarsal head, as well as correcting the hallux valgus.
Question 90
The lower extremity motor dysfunction in Charcot-Marie-Tooth disease most commonly involves which of the following muscles?
Explanation
The motor dysfunction in Charcot-Marie-Tooth disease involves the tibialis anterior muscle. Charcot-Marie-Tooth disorders most commonly cause distal motor dysfunction in the foot intrinsics, anterior compartment musculature, and peroneals. There is evidence that the peroneus brevis is affected selectively and the peroneus longus is spared. This is based on clinical muscle testing, muscle cross-sections on MRI, and electrodiagnostic testing. Mann RA, Missirian J: Pathophysiology of Charcot-Marie-Tooth disease. Clin Orthop 1988;234:221-228.
Question 91
Fixed hyperextension of the metatarsophalangeal joint is associated with
Explanation
Claw toe and hammer toe deformities are associated with dorsal subluxation of the interossei, which can no longer serve to flex the metatarsophalangeal joint. The extensor digitorum longus then loses its tenodesing effect on the proximal interphalangeal and distal interphalangeal joints and works unopposed to extend the metatarsophalangeal joint and the proximal phalanx. Without the antagonistic action of the extensor digitorum longus, the extrinsic flexors become unopposed flexors of the proximal and distal interphalangeal joints. Marks RM: Anatomy and pathophysiology of lesser toe deformities. Foot Ankle Clin 1998;3:199-213.
Question 92
The orthosis shown in Figure 47 is commonly used for
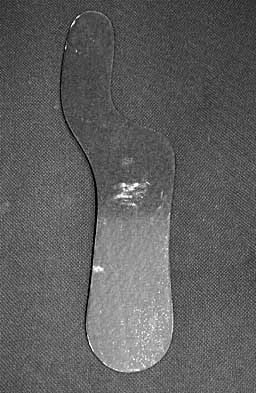
Explanation
The orthosis shown is a carbon reinforced Morton's extension, and it is commonly used for hallux rigidus. It decreases motion of the first metatarsophalangeal joint and subsequently decreases pain.
Question 93
A 14-year-old boy has medial ankle pain, progressive unilateral flatfoot deformity, and pain with most activities of daily living. He denies any recent injury. His parents recall that at age 7 years he sustained an injury that was treated as a sprain. Examination reveals valgus deformity with painless, unrestricted passive motion of the ankle. He has grossly equal limb lengths. A radiograph of the affected ankle is shown in Figure 48a, and the contralateral ankle is shown in Figure 48b. Management should consist of
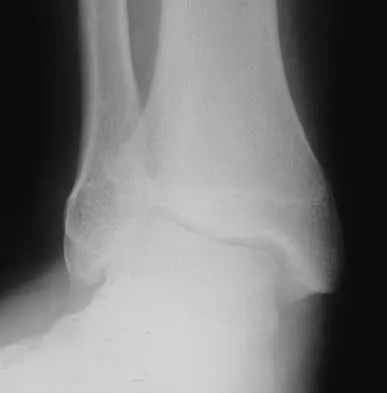
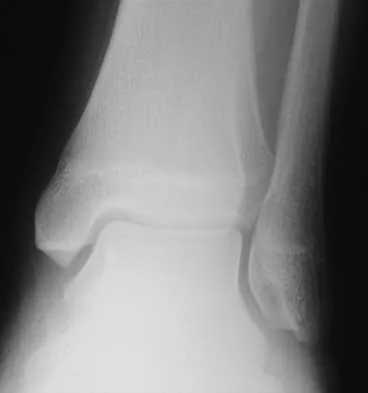
Explanation
Angular deformities of the ankle can occur following physeal injury. While an orthosis may be beneficial, the deformity is at the level of the ankle rather than the hindfoot. An epiphysiodesis or physeal bar resection would not be indicated as the growth plates are closed. Correction of the angular deformity should level the ankle joint and normalize the weight-bearing stresses on the ankle. This is most easily achieved with a closing wedge distal tibial osteotomy with or without concomitant osteotomy of the fibula. Thompson DM, Calhoun JH: Advanced techniques in foot and ankle reconstruction. Foot Ankle Clin 2000;5:417-442. Ting AJ, Tarr RR, Sarmiento A, Wagner K, Resnick C: The role of subtalar motion and ankle contact pressure changes from angular deformities of the tibia. Foot Ankle 1987;7:290-299.
Question 94
What is the most common organism found following a nail puncture wound through tennis shoes in a host without immunocompromise?
Explanation
The association of a nail puncture wound with a gram-negative infection (Pseudomonas aeruginosa) has been attributed to the local environmental factors in shoes. Osteomyelitis is rare, occurring only in about 1% of patients. Tetanus prophylaxis should be given if it is not up to date. While the remaining organisms listed are periodically involved, they are more common in patients who are immunocompromised or who have diabetes mellitus. Therefore, obtaining a culture of the infected wound is appropriate in such individuals because of the multifactorial nature of the infection. Green NE, Bruno J III: Pseudomonas infections of the foot after puncture wounds. South Med J 1980;73:146-149.
Question 95
Examination of a 28-year-old woman reveals a moderate hallux valgus deformity and a prominence of the medial eminence. She reports that she can participate in all activities, wear 3-inch heels with minimal discomfort, and walk in a 1-inch heel with no pain. However, she is concerned that the deformity will get worse and requests recommendations regarding surgical correction. What is the best course of action?
Explanation
Because the patient is essentially asymptomatic, the most appropriate course of action is observation. Prophylactic hallux valgus surgery is not medically indicated. Steroid injection would only risk infection, as well as joint and capsule damage. There are no data to support the use of a custom orthosis to delay the progression of a hallux valgus deformity. Special shoe wear or an extra-depth shoe is not necessary and is unlikely to be accepted by the patient. Donley BG, Tisdel CL, Sferra JJ, Hall JO: Diagnosing and treating hallux valgus: A conservative approach for a common problem. Cleve Clin J Med 1997;64:469-474.
Question 96
A 25-year-old man has ankle instability and a lateral foot callosity. Radiographs are shown in Figures 49a through 49c. Management options are best determined by the
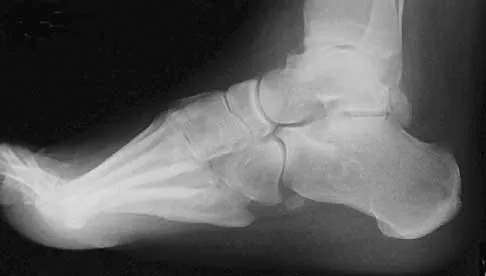
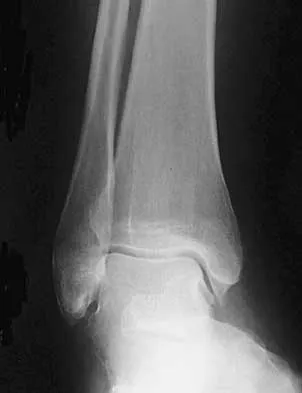
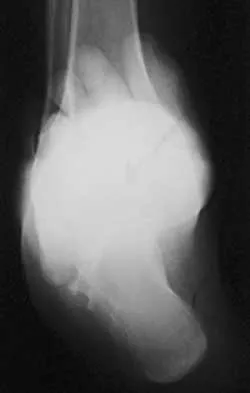
Explanation
The patient has a cavovarus deformity that has resulted in lateral foot overload and stressing of the lateral ligaments. Further treatment depends on the ability to correct the deformity. The Coleman block test indicates whether a deformity is fixed or supple. A supple deformity will respond to orthotic management or soft-tissue procedures, while a fixed deformity requires corrective osteotomy or fusion. Physical therapy, casting, and injection will not address the underlying pathophysiology. There is no indication that this is a neuropathic problem.
Question 97
A 17-year-old boy underwent open reduction and internal fixation of a navicular fracture 5 days ago. A follow-up examination now reveals a tensely swollen foot with erythema and multiple skin bullae. The patient is febrile and has marked pain with palpation of the entire forefoot and hindfoot. What is the next step in management?
Explanation
Necrotizing fasciitis is a rapidly progressive soft-tissue infection with the potential to threaten both life and limb. Patients who are immunocompromised (HIV infection, diabetes mellitus, alcohol abuse) are at increased risk. However, any patient in the immediate postoperative phase is susceptible to wound infection. Early detection is the key. Necrotizing fasciitis is primarily a surgical problem that requires urgent debridement and broad-spectrum IV antibiotics. Rapid diagnosis and prompt treatment help to reduce mortality, which may approach 30%. Debridement of the bullae and observation are not indicated. Although elevation and close follow-up may be warranted early on, in this patient, surgical debridement is the next step. Ault MJ, Geiderman J, Sokolov R: Rapid identification of group A streptococcus as the cause of necrotizing fasciitis. Ann Emerg Med 1996;28:227-230.
Question 98
A 14-year-old girl has had mild pain and nail deformity of the great toe for the past 4 months. A radiograph is shown in Figure 50. What is the most likely etiology of the lesion?
Explanation
The lesion is typical of a subungual exostosis, which is most often found on the medial aspect of the great toe in children and young adults. The diagnosis is confirmed on radiographs and usually requires excision for relief. Lokiec F, Ezra E, Krasin E, Keret D, Wientraub S: A simple and efficient surgical technique for subungual exostosis. J Pediatr Orthop 2001;21:76-79. Letts M, Davidson D, Nizalik E: Subungual exostosis: Diagnosis and treatment in children. J Trauma 1998;44:346-349.
Question 99
The third plantar intrinsic muscle layer of the foot consists of which of the following structures?
Explanation
The plantar intrinsic muscles are divided into four layers with respect to depth from the plantar fascia. They are (from superficial to deep): 1) abductor hallucis, flexor digitorum brevis, abductor digiti minimi; 2) quadratus plantae, lumbricals; 3) flexor digiti minimi, flexor hallucis brevis, adductor hallucis brevis; and 4) dorsal and plantar interosseous muscles. The flexor hallucis brevis and adductor hallucis brevis originate from the midtarsal bones, encompass the sesamoids, and insert into the base of the proximal phalanx. The adductor hallucis brevis consists of two muscle bellies forming a conjoined tendon and inserting into the lateral portion of the proximal phalanx and the lateral sesamoid. The adductor hallucis brevis is stronger than the abductor hallucis brevis, which may contribute to hallux valgus. The flexor digitorum minimi travels under the fifth metatarsal, arising at the base and inserting into the lateral base of the fifth proximal phalanx.
Question 100
Which of the following results cannot be achieved with an in-shoe orthosis?
Explanation
Depending on the type of materials used, an orthotic can be fabricated to achieve a variety of results. While a rigid fixed deformity can be stabilized or cushioned, an orthotic will not correct a deformity that is not passively correctable. Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 55-64. Bono CM, Berberian WS: Orthotic devices: Degenerative disorders of the foot and ankle. Foot Ankle Clin 2001;6:329-340.
