Mastering Carpal Salvage: Excision of Scaphoid Fragments and Proximal Row Carpectomy
Key Takeaway
Excision of the proximal scaphoid fragment and proximal row carpectomy (PRC) are critical salvage procedures for advanced carpal collapse and scaphoid nonunion. Proximal excision is indicated for small, avascular fragments, while PRC transforms the wrist into a simple hinge joint for widespread degenerative changes. This guide details the biomechanical rationale, precise surgical techniques, and postoperative protocols required to optimize patient outcomes and preserve functional wrist motion.
INTRODUCTION TO CARPAL SALVAGE PROCEDURES
The management of scaphoid nonunions and subsequent carpal collapse presents a formidable challenge in operative orthopaedics. The scaphoid serves as the critical biomechanical link between the proximal and distal carpal rows. Disruption of this link—whether through recalcitrant nonunion, avascular necrosis (osteonecrosis), or severe fracture-dislocation—inevitably alters carpal kinematics, leading to predictable patterns of degenerative arthrosis, most notably Scaphoid Nonunion Advanced Collapse (SNAC).
When joint preservation or anatomic reconstruction is no longer viable, salvage procedures must be employed to alleviate pain while preserving a functional range of motion. This comprehensive guide details the indications, biomechanical rationale, and precise surgical techniques for excision of scaphoid fragments and Proximal Row Carpectomy (PRC).
BIOMECHANICS AND PATHOANATOMY OF SCAPHOID EXCISION
Excising both fragments of the scaphoid as an isolated procedure is biomechanically unsound and highly discouraged. While the immediate postoperative result may appear satisfactory regarding pain relief, the eventual derangement of the wrist is inevitable.
As classically reported by Soto-Hall and Haldeman, the complete removal of the scaphoid uncouples the proximal and distal carpal rows, leading to the gradual proximal migration of the capitate into the space previously occupied by the scaphoid. Although severe disability may not become clinically apparent for 5 to 7 years, the resulting carpal collapse is profound. Therefore, if excision of the entire scaphoid is considered, it is imperative to perform a concomitant stabilizing procedure, such as a capitolunate or capital-lunate-triquetral-hamate (four-corner) arthrodesis.
Conversely, excising only the proximal scaphoid fragment is often highly satisfactory, provided strict anatomical criteria are met. The loss of one-fourth or less of the scaphoid volume typically causes minimal impairment to overall wrist kinematics. Because the required postoperative immobilization is brief, functional range of motion usually returns rapidly, though patients should be counseled to expect a mild to moderate decrease in grip strength.
EXCISION OF THE PROXIMAL SCAPHOID FRAGMENT
Indications for Proximal Pole Excision
The decision to excise the proximal fragment of a scaphoid nonunion hinges on the size of the fragment, its viability, and the presence of localized arthrosis. The primary indications include:
- Fragment Size (≤ 25%): The proximal fragment constitutes one-fourth or less of the total scaphoid volume. Regardless of its viability, attempting to bone graft such a diminutive fragment frequently results in failure due to inadequate vascularity and insufficient bone stock for stable internal fixation.
- Sclerotic, Comminuted, or Severely Displaced Fragments: If a small fragment (≤ 25%) is severely comminuted or displaced, it should be excised early to prevent the rapid onset of radioscaphoid arthrosis. A severely displaced fragment that cannot be accurately reduced via closed manipulation or limited open techniques is a prime candidate for excision.
- Failed Previous Grafting: A small proximal fragment (≤ 25%) where previous vascularized or non-vascularized bone grafting has failed. (Note: If a nonviable proximal fragment represents more than 25% of the scaphoid, excision alone will leave an unmanageable dead space and destabilize the carpus; alternative treatments, such as scaphoid excision with four-corner fusion, are preferable).
- Concomitant Radial Styloid Arthrosis: The presence of localized arthritic changes in the region of the radial styloid necessitates a concomitant radial styloidectomy in conjunction with the excision of the proximal fragment to eliminate impingement.
Clinical Pearl: The "Space Filler" Debate
In the past, Silastic (silicone) implants were frequently utilized as "space fillers" following proximal pole excision. However, due to the high incidence of silicone particulate synovitis and subsequent destructive carpal cysts, this practice has been largely abandoned. Contemporary evidence-based practice dictates leaving the dead space empty, or alternatively, utilizing a folded or rolled autologous tendon graft (e.g., palmaris longus) as a biological interpositional anchovy to fill the defect.
Surgical Technique: Proximal Fragment Excision
1. Positioning and Approach
* Place the patient supine with the operative arm extended on a radiolucent hand table. Apply a well-padded proximal tourniquet.
* Make a 5 cm transverse skin incision on the dorsoradial aspect of the wrist, centered directly over the scaphoid at the level of the radial styloid process.
* Meticulously dissect through the subcutaneous tissues, identifying and protecting the superficial radial nerve (SRN) and its terminal sensory branches. Neuroma formation in this region is a devastating complication.
2. Retinacular Release and Tendon Retraction
* Release the radial side of the extensor retinaculum via a longitudinal incision along the radial border of the first dorsal compartment.
* Reflect the retinacular flap medially toward the second and third extensor compartments.
* Protect and retract the tendons of the abductor pollicis longus (APL) and extensor pollicis brevis (EPB) in a palmar direction. Retract the tendon of the extensor pollicis longus (EPL) in a dorsal and ulnar direction to expose the underlying joint capsule.
3. Capsulotomy and Fragment Identification
* Create a radially based triangular flap of the dorsal capsule. Incise along the distal border of the dorsal radiotriquetral and dorsal intercarpal ligaments to expose the proximal scaphoid.
* CRITICAL STEP: To avoid the catastrophic error of excising a normal carpal bone (such as the lunate), place a Kirschner wire (K-wire) into the suspected proximal fragment of the scaphoid. Obtain an anteroposterior (AP) fluoroscopic radiograph to definitively confirm the identity of the fragment.
4. Excision and Joint Assessment
* Once confirmed, grasp the proximal fragment with a towel clip or strong toothed forceps. Apply steady traction and carefully remove the fragment by sharply dividing its remaining volar soft tissue and ligamentous attachments.
* Alternatively, the proximal pole can be removed piecemeal using a rongeur.
* Assess the capitolunate joint. If there is excessive laxity in the wrist allowing the capitate to migrate proximally into the newly created defect, proceed immediately to a scaphocapitate fusion or alternative stabilizing procedure.
* Move the wrist through a full, dynamic range of motion under direct vision. Ensure that the irregular surfaces of the remaining distal scaphoid do not impinge on the articular surface of the radius.
5. Closure
* Reattach the reflected dorsal and palmar capsuloligamentous flaps. This can be achieved using non-absorbable sutures passed through transosseous drill holes in the distal radius, or by utilizing small suture anchors.
* Repair the extensor retinaculum with absorbable sutures, ensuring the EPL is left transposed subcutaneously if necessary to prevent attrition rupture.
* Close the skin in layers and apply a bulky sterile dressing supported by an anterior splint extending from the palmar crease to the proximal forearm.
Postoperative Care
The postoperative regimen is designed to balance soft tissue healing with the early restoration of motion.
* Days 10 to 14: Remove the postoperative splint and skin sutures.
* Week 3: Transition the patient to a custom-molded removable splint and initiate a formal program of active range-of-motion (ROM) exercises.
* The removable splint should be worn between exercise sessions and during heavy activities until satisfactory function, grip strength, and pain-free motion are restored to the hand and wrist.
EXCISION OF THE DISTAL SCAPHOID
While less common than proximal pole excision, resection of the distal scaphoid pole has demonstrated satisfactory outcomes in the treatment of specific scaphoid nonunions complicated by localized radioscaphoid arthritis.
If advanced capitolunate arthritis is present concurrently, distal scaphoid excision alone is insufficient; an additional stabilizing procedure, such as a limited intercarpal arthrodesis (e.g., capitolunate fusion), must be added. The surgical approach, capsular management, and postoperative rehabilitation protocols for distal scaphoid excision are virtually identical to those described for proximal pole excision.
PROXIMAL ROW CARPECTOMY (PRC)
Proximal Row Carpectomy is a highly effective, motion-preserving reconstructive procedure utilized for advanced posttraumatic degenerative conditions of the wrist. By excising the scaphoid, lunate, and triquetrum, the complex multi-articulating carpus is converted into a simple hinge joint between the proximal pole of the capitate and the lunate fossa of the distal radius.
Indications and Patient Selection
PRC is widely supported as a superior alternative to total wrist arthrodesis for patients who desire the preservation of wrist mobility and are willing to accept the possibility of minimal persistent pain and reduced grip strength.
Primary Indications:
* Scaphoid Nonunion Advanced Collapse (SNAC) - Stages II and III.
* Scapholunate Advanced Collapse (SLAC) - Stages II and III.
* Kienböck’s disease (avascular necrosis of the lunate) with carpal collapse.
* Severe, unsalvageable open carpal fracture-dislocations characterized by massive disruption of bony architecture and blood supply to the proximal row.
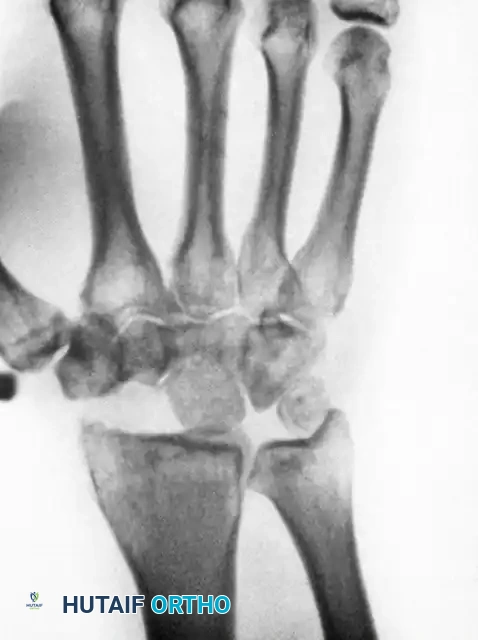
Above: Long-standing scaphoid nonunion demonstrating advanced arthrosis, osteonecrosis, collapse of the proximal pole, and the pathological settling of the capitate into the proximal carpal row.
Contraindications & Prerequisites:
The absolute prerequisite for a successful PRC is the presence of healthy, intact articular cartilage on both the lunate fossa of the radius and the proximal articular surface of the capitate.
Surgical Warning: Capitolunate Arthrosis
Historically, arthrosis at the capitolunate joint was considered an absolute contraindication to PRC. However, modern techniques have evolved. If mild to moderate capitate degeneration is present, the proximal pole of the capitate can be excised and resurfaced using a dorsal capsular flap interposition (Radiocapitate Capsular Interposition - RCPI), yielding satisfactory functional results. Nevertheless, if severe, eburnated degenerative changes are visualized radiographically or intraoperatively on these critical surfaces, PRC should be aborted in favor of a total wrist arthrodesis or four-corner fusion.
Furthermore, manual laborers or patients with high-demand, heavy-loading occupational requirements are generally better candidates for a total wrist arthrodesis, as PRC may fail under chronic heavy axial loading.
Surgical Technique: Proximal Row Carpectomy
1. Exposure and Carpal Assessment
* Utilize a dorsal longitudinal approach centered over Lister's tubercle.
* Elevate the third and fourth extensor compartments and perform a ligament-sparing dorsal capsulotomy (e.g., Berger's flap) to expose the proximal carpal row.
* Inspect the articular surfaces of the capitate head and the lunate fossa. Confirm that the cartilage is sufficient to support the new radiocapitate articulation.
2. Excision of the Proximal Row
* The objective is the complete excision of the triquetrum, lunate, and entire scaphoid.
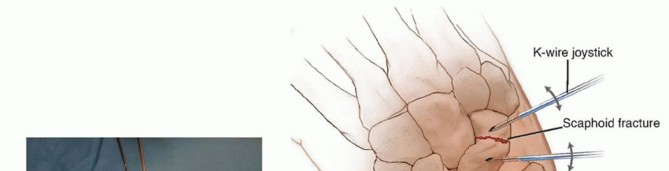
* Technique Pearl: The bones are usually removed piecemeal to minimize trauma to the surrounding volar ligaments. Threaded Kirschner wires or small Schanz screws can be inserted into the carpal bones to act as "joysticks." These handles provide excellent leverage to manipulate and deliver the bones out of the deep radiocarpal space.
* The Pisiform: Excision of the pisiform is unnecessary. Because it functions as a sesamoid bone within the tendon of the flexor carpi ulnaris (FCU), it does not interfere with the new radiocapitate articulation.
3. Management of the Distal Scaphoid and Radial Styloid
* In certain cases, the distal pole of the scaphoid (at its articulation with the trapezium and trapezoid) can be retained to provide a more stable bony base for the thumb ray.
* However, if the distal scaphoid pole is left intact, a radial styloidectomy is absolutely mandatory. Failure to resect the radial styloid will result in severe bony impingement between the retained distal scaphoid/trapezium and the radial styloid during radial deviation.
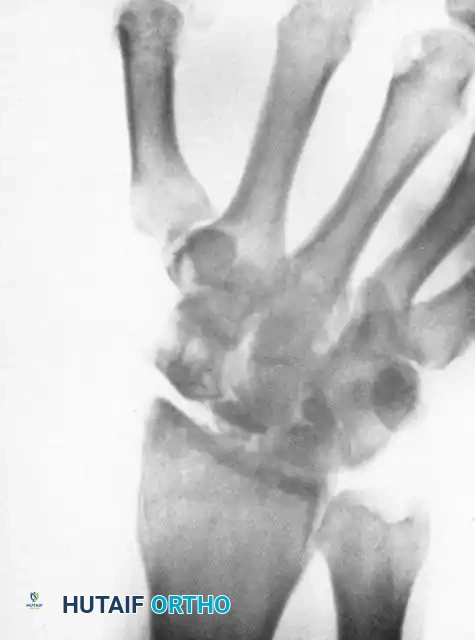
Above: Postoperative radiographic appearance following a Proximal Row Carpectomy (PRC) combined with a radial styloidectomy. Note the smooth articulation of the capitate within the lunate fossa.
4. Ligamentous Preservation
* CRITICAL PITFALL: When performing the carpectomy and the radial styloidectomy, meticulous care must be taken to avoid injuring the volar radiocapitate ligament (Radioscaphocapitate ligament). This stout volar ligament is the primary restraint preventing the ulnar translation of the remaining carpus off the distal radius. Disruption of this ligament will lead to catastrophic ulnar subluxation of the wrist.
5. Closure
* Copiously irrigate the joint space to remove all bone debris.
* Repair the dorsal capsule securely to stabilize the new joint construct.
* Close the extensor retinaculum and skin in standard layered fashion.
* Apply a well-padded anterior splint extending from the palmar crease to the elbow, holding the wrist in neutral to slight extension.
Postoperative Care and Salvage Options
- Immobilization: The wrist is strictly immobilized in the postoperative splint for 2 weeks to allow for capsular healing.
- Suture Removal: Sutures are removed at 10 to 14 days postoperatively.
- Rehabilitation: At 2 weeks, the patient is transitioned to a custom-molded removable splint. A rigorous program of active and active-assisted ROM exercises is initiated. The splint is gradually weaned as dynamic stability and satisfactory function are restored.
- (Note: If a limited intercarpal arthrodesis was performed concurrently, the immobilization period is extended to 6-8 weeks until radiographic union is achieved).
Salvage of a Failed PRC:
While PRC provides excellent long-term pain relief and functional motion for the majority of appropriately selected patients, progressive radiocapitate arthrosis can occur over time. If a proximal row carpectomy ultimately fails to meet the patient’s functional needs due to intractable pain or progressive weakness, conversion to a total wrist arthrodesis remains a highly reliable and definitive salvage option.
===
You Might Also Like