Mastering Forefoot Reconstruction: Metatarsal Distraction Osteogenesis and Management of Acquired Hallux Varus
Key Takeaway
Distraction osteogenesis for metatarsal shortening requires precise external fixator placement to restore the windlass mechanism. Conversely, acquired hallux varus is a complex iatrogenic deformity often resulting from overzealous lateral release or fibular sesamoidectomy during bunion correction. This guide details the step-by-step surgical protocols, biomechanical principles, and postoperative management strategies essential for correcting these challenging forefoot pathologies and restoring optimal foot biomechanics.
DISTRACTION OSTEOGENESIS FOR METATARSAL SHORTENING
Metatarsal shortening, whether congenital (e.g., brachymetatarsia) or iatrogenic (e.g., post-osteotomy shortening), significantly disrupts the biomechanics of the forefoot. The primary goal of distraction osteogenesis in this setting is to restore the normal parabolic cascade of the metatarsal heads, thereby re-establishing the critical "windlass" mechanism of Hicks. This procedure relies heavily on the principles of callotasis, requiring meticulous surgical technique to preserve the periosteal sleeve and precise external fixator application to control the biomechanical vectors during the lengthening phase.
Preoperative Planning and Biomechanical Principles
Successful distraction osteogenesis requires a comprehensive understanding of forefoot biomechanics. The first metatarsal bears approximately twice the weight of the lesser metatarsals during the stance phase of gait. Shortening of the first ray leads to transfer metatarsalgia, altered gait kinematics, and potential lesser toe deformities.
Surgical Pearl: The vector of distraction is paramount. The natural pull of the extensor hallucis longus (EHL) and flexor hallucis longus (FHL) during lengthening will inherently drive the metatarsal head into dorsiflexion. To counteract this, the external fixator pins must be oriented to provide a relative plantarflexion force to the distal fragment.
Surgical Technique: Step-by-Step Protocol
1. Patient Positioning and Fixator Templating
* After the induction of general or regional anesthesia, place the patient supine on the operating table.
* Perform a standard sterile preparation and draping of the affected foot and lower leg.
* Utilize intraoperative fluoroscopic control to template the chosen external fixator. Determine the optimal trajectory and position for the pin holes to ensure the fixator sits parallel to the longitudinal axis of the metatarsal in the transverse plane, while allowing for the necessary sagittal plane adjustments.
2. Percutaneous Pin Placement
* Using a 1.5-mm Kirschner wire, pre-drill the holes percutaneously along the medial aspect of the first metatarsal.
* Insert four self-tapping half-pins. The recommended pin dimensions are 2.5-mm tapered threads with 3.0-mm diameter shafts to provide adequate stiffness without causing excessive stress risers in the relatively small metatarsal bone.
* Critical Sequence: Place the distal two pins first, followed by the proximal two pins.
* Vector Control: To achieve the necessary plantarflexion orientation, place the two distal pins in the plantar half of the distal metatarsal fragment. This eccentric placement creates a relatively plantarward distraction vector, neutralizing the dorsiflexion forces exerted by the soft tissue envelope during lengthening.
3. Surgical Approach and Periosteal Preservation
* Make a precise 2-cm longitudinal incision along the medial border of the metatarsal, positioned exactly between the second and third pins.
* Carry the dissection sharply down to the bone.
* Incise the periosteum longitudinally. It is absolutely critical to leave the periosteum intact laterally, anteriorly, and posteriorly.
* In the specific area of the proposed osteotomy, use a fine periosteal elevator to minimally strip the periosteum. Preserve this tissue meticulously, as it is the primary source of osteoprogenitor cells for the regenerate bone.
Surgical Warning: Excessive periosteal stripping will lead to delayed consolidation, nonunion, or premature consolidation of the regenerate. The periosteum must be treated as a delicate, vital organ.
4. The Osteotomy (Corticotomy)
* Utilize a mini-sagittal saw to perform a transverse osteotomy between the second and third pins.
* Thermal Necrosis Prevention: Continuously cool the saw blade with copious normal saline irrigation throughout the cut. Thermal necrosis of the bone ends is a primary cause of regenerate failure.
* Confirm the adequacy and distractibility of the osteotomy by manually distracting the external fixator by 5 mm. Obtain a fluoroscopic image to verify complete separation of the cortices.
* Once confirmed, compress the distractor to achieve firm bone-on-bone contact and lock the fixator tightly.
5. Closure
* Approximate the preserved periosteal sleeve over the osteotomy site using a 4-0 absorbable polyglactin suture.
* Close the skin with simple interrupted sutures of 4-0 nylon.
* Apply a sterile, soft, non-constrictive dressing.
Postoperative Care and the Distraction Protocol
The postoperative phase is divided into three distinct periods: latency, distraction, and consolidation.
- Latency Phase: The patient is discharged home on the day of surgery and instructed to remain strictly non-weight bearing on the operative extremity. The initial dressing remains intact for 1 week.
- Distraction Phase: At the 1-week postoperative clinic visit, sutures are removed, and baseline radiographs are obtained. The patient is instructed on the distraction protocol: turning the external fixator key one-quarter turn, four times a day. This equates to a distraction rate of exactly 1 mm per day.
- Goal: The distraction continues until the first and second metatarsals are of equal length, thereby restoring the normal windlass mechanism.
- Weight Bearing: The patient remains strictly non-weight bearing during the entire lengthening phase.
- Rehabilitation: Daily passive range of motion (ROM) of the metatarsophalangeal (MTP) joint is mandatory to prevent joint stiffness and contracture.
- Consolidation Phase: Once the desired length is achieved, distraction is halted. When radiographic evidence of consolidation (corticalization of the regenerate) is observed, partial weight bearing is permitted. The external fixator remains in place until full, robust consolidation is visible on multiple radiographic views. Following fixator removal, the patient may transition to full weight bearing and normal shoe wear as tolerated.
ACQUIRED HALLUX VARUS AND INTRINSIC MINUS HALLUX
Acquired hallux varus is a notoriously challenging iatrogenic complication following hallux valgus (bunion) surgery. It was not widely recognized in the orthopedic literature until McBride, in 1935, reported its occurrence in approximately 5% of patients treated with his eponymous procedure (which involved medial eminence removal, medial capsulorrhaphy, and fibular sesamoidectomy).
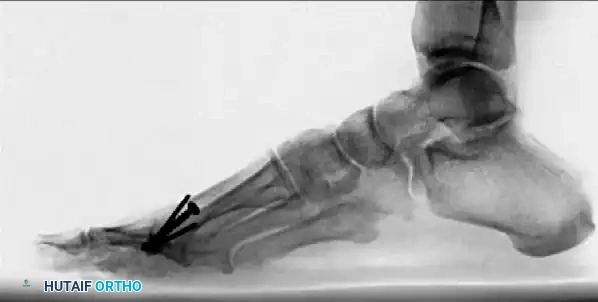
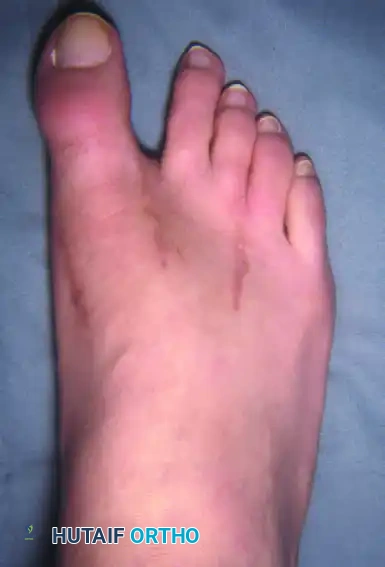
Figure 81-77: (A) Fixed hallux varus after a McBride bunionectomy. (B) Hallux varus after a McBride bunionectomy with fibular sesamoid excision. Removing the fibular sesamoid eliminates the valgus-producing moments of the adductor hallucis and the lateral head of the flexor hallucis brevis.
Since McBride's initial report, the incidence of acquired hallux varus has been reported to range from 2% (Peterson et al.) to as high as 17% (Trnka et al.) following almost all variations of hallux valgus operations, including both distal and proximal metatarsal osteotomies.
Interestingly, few patients with hallux varus present with primary complaints regarding cosmesis unless the varus angulation exceeds 10 to 15 degrees. Discomfort is relatively rare in supple deformities but becomes a primary complaint when associated with degenerative joint disease of the first MTP joint or when the deformity becomes rigid.
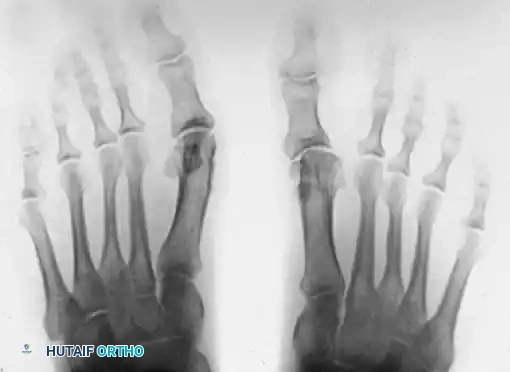
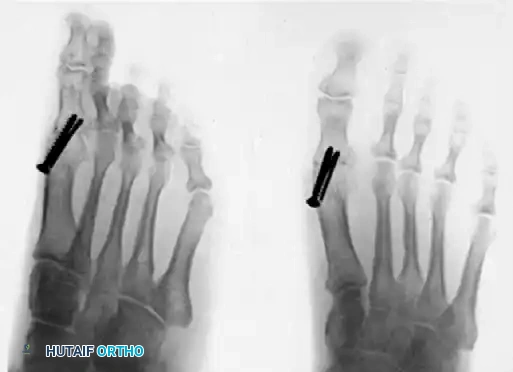
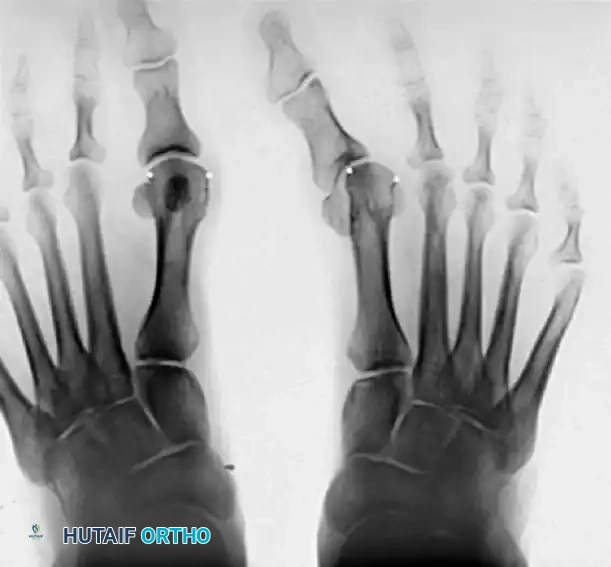
Figure 81-76: (A) Relatively mild hallux varus with symptomatic degenerative arthritis of the first metatarsophalangeal joint. (B and C) Arthrodesis was chosen as the definitive treatment due to the presence of advanced degenerative joint disease.
Etiology and Pathogenesis
The development of acquired hallux varus is almost exclusively tied to the disruption of the delicate soft-tissue and bony balance surrounding the first MTP joint. The main surgical causes include:
- Overzealous Soft Tissue Balancing: Complete release of the lateral structures (lateral capsule, adductor hallucis) combined with excessive plication of the medial capsule. This forcefully pulls the sesamoid apparatus too far medially.
- Excessive Medial Eminence Resection: Resecting the medial eminence at or lateral to the sagittal groove removes the critical medial bony buttress that stabilizes the proximal phalanx, allowing it to slide into varus.
- Fibular Sesamoidectomy: Excision of the fibular sesamoid inherently removes the insertion point for the adductor hallucis and the lateral head of the flexor hallucis brevis (FHB), destroying the lateral stabilizing forces.
- Iatrogenic FHB Release: Inadvertent release of the lateral head of the FHB at its insertion into the fibular sesamoid during lateral release.
- Overcorrection of the Intermetatarsal Angle (IMA): Closing the IMA to neutral (0 degrees) or a negative value.
Clinical Pitfall: Normally, the hallux rests on the first metatarsal head in approximately 10 degrees of valgus. If the IMA is surgically reduced to less than 5 degrees, and the hallux is reduced congruously, the necessary valgus angulation must be 15 degrees. A clinically "straight" toe in this scenario actually places the hallux into varus relative to the articular surface.
Clinical Classification: Static vs. Dynamic Deformity
Proper presurgical planning requires differentiating between static and dynamic hallux varus, as the underlying muscle imbalances and required reconstructive techniques differ vastly.
Static (Supple) Hallux Varus
Static hallux varus is a supple, uniplanar deformity that is passively correctable. It is usually asymptomatic and presents primarily as a cosmetic concern.
* Clinical Presentation: In a weight-bearing stance, the hallux rests in varus. However, the MTP joint remains in a normal sagittal plane position (10 degrees to the plantar surface of the foot), and the interphalangeal (IP) joint is not contracted.
* Characteristics: The hallux is not abnormally rotated in the axial plane and lacks the multiplanar "snake-in-the-grass" appearance. The deformity is isolated to the transverse or frontal plane at the MTP joint.
Dynamic (Fixed) Hallux Varus
Dynamic hallux varus is a complex, multiplanar deformity that is frequently fixed, highly symptomatic, and surgically demanding to correct.
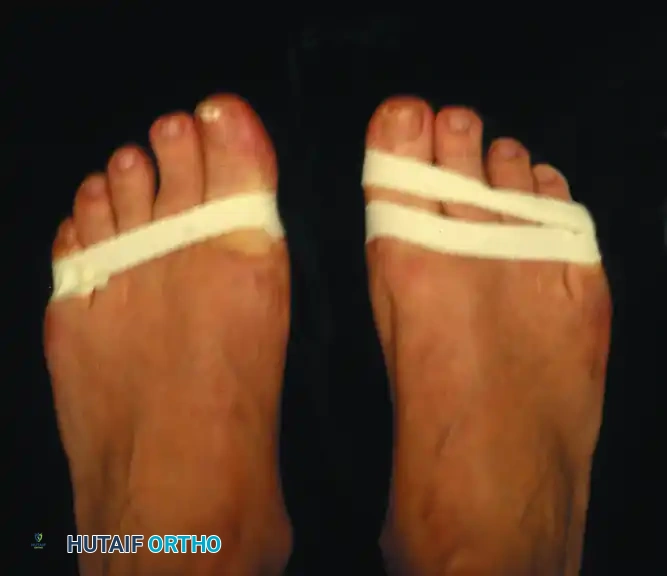
Figure 81-78: A passively correctable dynamic hallux varus deformity, demonstrating the multiplanar nature of the condition prior to becoming rigidly fixed.
- Pathoanatomy: The most accurate descriptive term is an intrinsic minus deformity of the hallux with a varus component. This represents a profound intrinsic-extrinsic muscle imbalance.
- Clinical Presentation: The first MTP joint is rigidly hyperextended (due to soft tissue contracture), and the IP joint is acutely flexed. The hallux is axially rotated.
- Patient Complaints: The extended and varus posture makes normal shoe wear nearly impossible. Patients frequently complain of the toe box rubbing against the dorsomedial surface of the IP joint. A painful plantar keratotic lesion often develops beneath the first metatarsal head because the extended hallux drives the metatarsal head plantarward during the stance phase. Furthermore, the lesser toes may develop hammer toe deformities and transfer metatarsalgia as the incompetent hallux fails to bear weight during the toe-off phase of gait.
Anatomical and Biomechanical Considerations
To understand the pathogenesis, one must understand the normal anatomy. The intrinsic muscles (abductor hallucis, adductor hallucis, and both heads of the FHB) balance the hallux congruently on the shallow ball-and-socket MTP joint. The extrinsic muscles (EHL, FHL) provide gross movement and power.
This synchronous balance is catastrophically disrupted if the tendon insertions are altered relative to the axis of rotation.
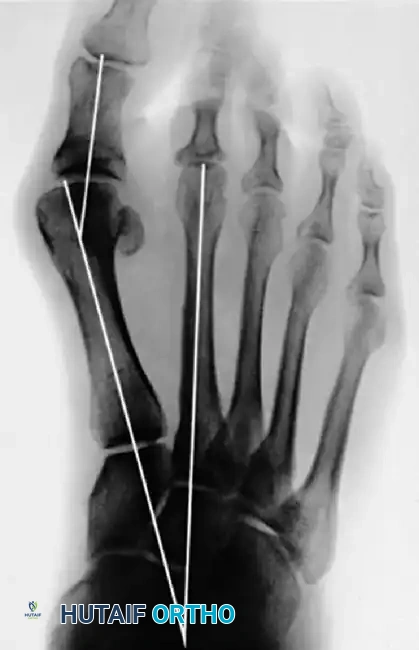
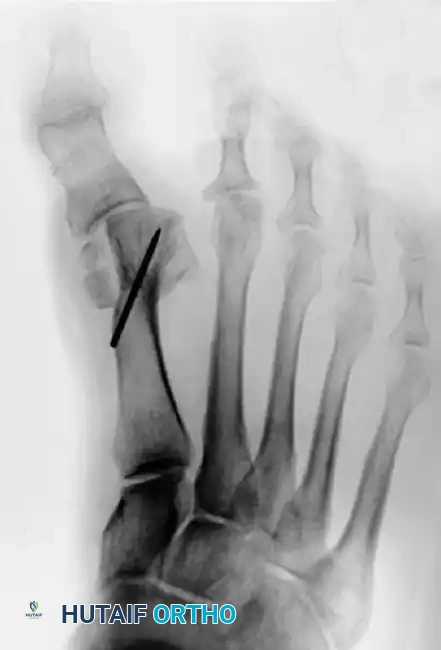
Figure 81-79: (A) Preoperative hallux valgus deformity. (B) Postoperative dislocation of the tibial sesamoid following a distal metatarsal osteotomy combined with a fibular sesamoidectomy, leading to profound muscle imbalance.
The Pathogenic Cascade of the McBride Procedure:
When a fibular sesamoidectomy is performed alongside an adductor tendon release, the tibial sesamoid (housing the medial head of the FHB) is allowed to drift medially. This exerts a massive, unopposed varus moment on the proximal phalanx. The abductor hallucis tendon completely overpowers its now-absent antagonist (the adductor).
As the MTP joint drifts into varus, the EHL, FHL, and the medial head of the FHB shift medial to the axial midline. This medial shift increases the varus deformity—a direct biomechanical reversal of the pathology seen in hallux valgus (where lateral subluxation of these structures drives valgus).
Development of the Intrinsic Minus (Clawed) Hallux:
Following the release of the lateral head of the FHB and the medial subluxation of the tibial sesamoid, the medial head of the FHB loses its mechanical advantage as a flexor of the MTP joint. It is rapidly overpowered by the intact extensors (EHL, EHB), driving the MTP joint into severe extension.
As the MTP joint hyperextends, the FHL tendon is placed under immense tension (tightens), while the EHL tendon relatively slackens distally. This tenodesis effect forces the IP joint into acute, rigid flexion.
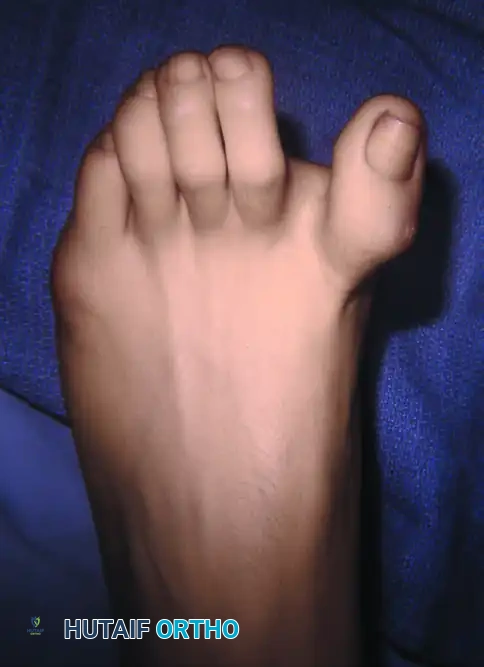
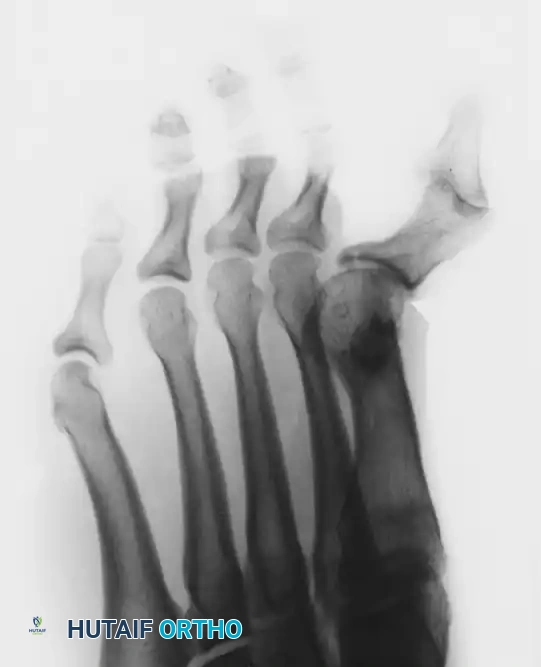
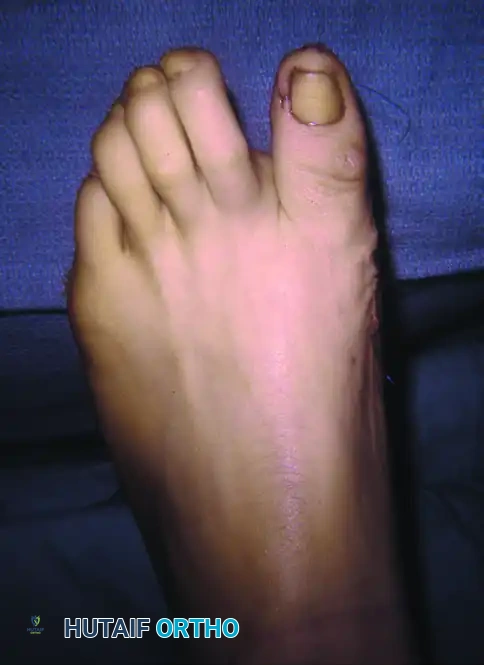
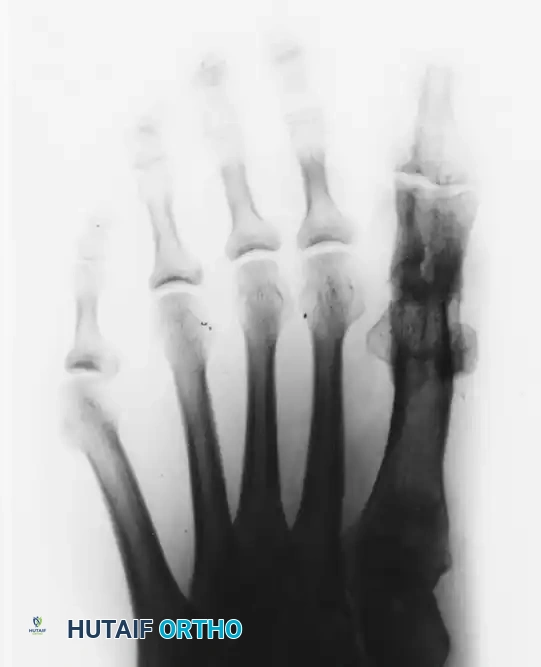
Figure 81-80: (A and B) Severe hyperextension of the metatarsophalangeal joint and hyperflexion of the interphalangeal joint, accompanied by varus and axial rotation of the hallux (the classic intrinsic minus claw toe). (C and D) This dynamic, supple deformity was successfully treated by arthrodesis of the first metatarsophalangeal joint combined with a plantar release of the interphalangeal joint to restore alignment.
This resulting deformity—the clawed hallux—is the hallmark of the intrinsic minus state. If left untreated, the soft tissues rapidly contract, converting a supple, dynamic deformity into a rigid, fixed multiplanar deformity that often necessitates salvage procedures such as first MTP joint arthrodesis to restore a plantigrade, braceable, and pain-free foot.
You Might Also Like
