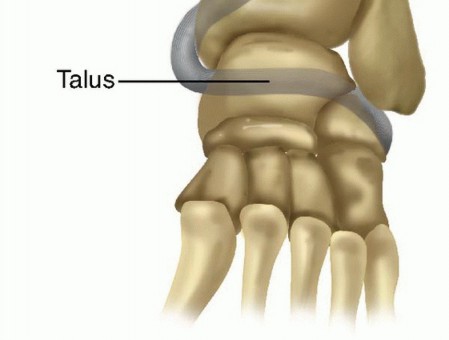
Comprehensive Diagnosis and Management of Ankle Ligament Injuries
Key Takeaway
Accurate diagnosis of ankle ligament injuries requires meticulous physical examination, often optimized by delaying assessment for five days post-injury. Key diagnostic maneuvers include the anterior drawer and inversion stress tests, evaluating the anterior talofibular and calcaneofibular ligaments. While functional rehabilitation remains the gold standard for acute sprains, chronic instability may necessitate advanced MRI evaluation and subsequent surgical reconstruction, such as the modified Broström procedure, to restore joint kinematics and prevent long-term arthropathy.
INTRODUCTION AND BIOMECHANICS
Ankle ligament injuries represent one of the most ubiquitous pathologies encountered in both emergency departments and specialized orthopedic clinics. Despite their frequency, they are frequently underappreciated, leading to chronic lateral ankle instability (CLAI), osteochondral lesions, and early-onset post-traumatic osteoarthritis. A profound understanding of ankle biomechanics is paramount. The lateral ligamentous complex consists of the anterior talofibular ligament (ATFL), the calcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL). The ATFL is the primary restraint to anterior talar translation and internal rotation when the ankle is in plantar flexion. The CFL, crossing both the tibiotalar and subtalar joints, becomes the primary restraint to inversion when the ankle is dorsiflexed.
Conversely, the medial side is stabilized by the robust deltoid ligament complex, which is rarely ruptured in isolation without an associated syndesmotic injury or fibular fracture. The distal tibiofibular syndesmosis maintains the integrity of the ankle mortise and is composed of the anterior inferior tibiofibular ligament (AITFL), the posterior inferior tibiofibular ligament (PITFL), the transverse ligament, and the interosseous membrane.
CLINICAL EVALUATION AND DIAGNOSIS
A meticulous, systematic physical examination is essential to avoid misdiagnosis and to formulate an appropriate treatment algorithm. The clinical presentation of an acute ankle sprain is often clouded by diffuse edema, ecchymosis, and significant patient guarding, which can obscure underlying structural deficits.
Systematic Palpation
The following anatomical structures must be systematically palpated, as tenderness in these regions may indicate specific associated pathologies:
* Lateral Complex: Anterior tibiofibular, calcaneofibular, and bifurcate ligaments.
* Medial Complex: Superficial and deep components of the deltoid ligament.
* Syndesmosis: The anterior and posterior aspects of the distal tibiofibular joint.
* Bony Landmarks: The medial and lateral malleoli, the anterior process of the calcaneus, and the lateral process of the talus.
* Foot Structures: The fifth metatarsal base and the insertion of the peroneus tertius onto the dorsal fifth metatarsal base (to rule out avulsion fractures or Jones fractures).
* Tendinous Structures: The Achilles, peroneal (longus and brevis), posterior tibial, flexor hallucis longus (FHL), and flexor digitorum longus (FDL) tendons.
Clinical Pearl: Frey et al. demonstrated that physical examination is 100% accurate in the diagnosis of Grade III (complete) ligament injuries but only 25% accurate in the diagnosis of Grade II (partial) injuries when compared with MRI findings. Clinicians most often underestimate the structural damage associated with a Grade II ligament tear.
The Timing of Examination
Acute pain and muscle spasm frequently limit the utility of stress testing immediately following an injury. Van Dijk et al. suggested that an accurate diagnosis is highly possible if the physical examination is performed 5 days after the injury rather than within the first 48 hours. Delayed physical examination yields information of diagnostic quality that is equal to that of arthrography, while causing significantly less discomfort to the patient.
When instability is not immediately apparent, the clinician must answer two critical questions:
1. Is a ligament completely ruptured (Grade III sprain)?
2. How many of the ligaments, especially on the lateral side, are completely ruptured?
PROVOCATIVE TESTING AND STRESS MANEUVERS
Diagnosis by stressing the ankle for instability without general anesthesia is often difficult or impossible, even with an appropriate regional block. However, the injection of local anesthetic (e.g., 1% lidocaine) into the peroneal sheath and the lateral gutter of the ankle before provocative maneuvers often dramatically improves the examination of the lateral ligaments by decreasing guarding and muscle spasm.
Inversion and eversion stress testing, along with anteroposterior stress testing (anterior drawer sign), are utilized to evaluate both acute and chronic instability. For stress tests to be considered diagnostic, they must clearly demonstrate a significant, reproducible difference between the abnormal and normal contralateral ankle.
Anteroposterior Stress Test (Anterior Drawer Sign)
The anterior drawer sign is the hallmark clinical test for evaluating the integrity of the ATFL.
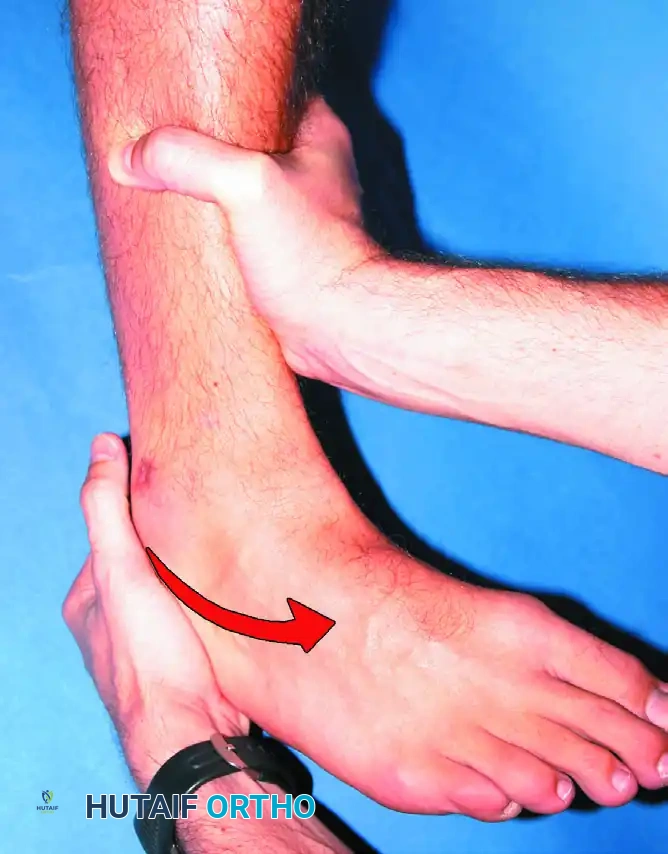
Demonstration of anterior drawer sign positioning for radiograph.
Technique: Clinically, it is highly effective to place the tip of the thumb on the tip of the lateral malleolus while palpating the lateral talar process with the base of the thumb. The ankle is held in neutral or slight plantar flexion (10 to 15 degrees) to isolate the ATFL, and the foot is allowed to internally rotate slightly. With gentle, steady anterior stress applied to the heel while stabilizing the distal tibia, the examiner assesses the degree of anterior displacement of the talus relative to the tibia.
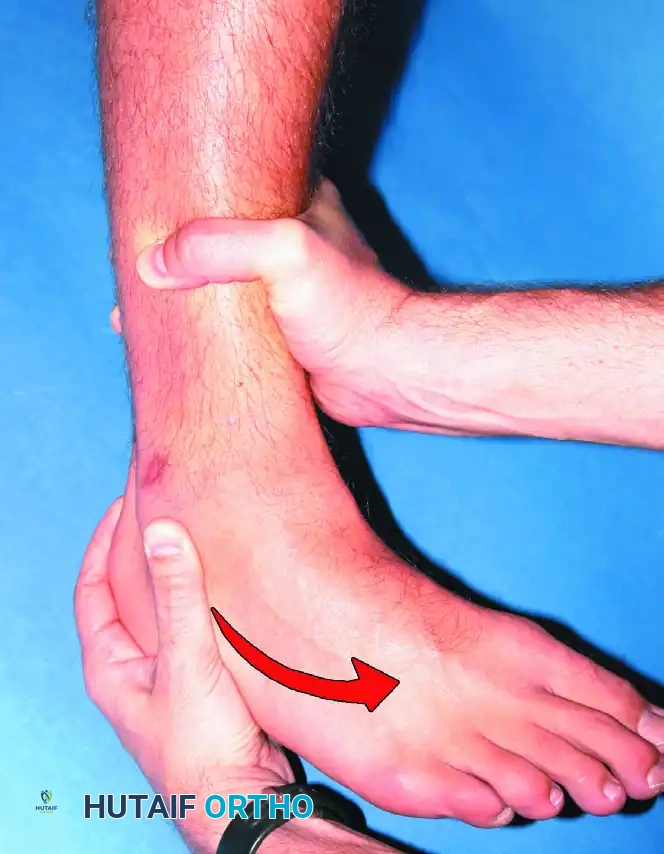
Clinical demonstration of the anterior drawer sign.
A relatively low-magnitude load is all that is required when evaluating the integrity of the ATFL in an acute ligamentous injury.
Surgical Warning: More important than the absolute number of millimeters of displacement is the clinical, tactile impression that the talus is subluxating out of the mortise. A "clunk" or a soft endpoint is highly indicative of a complete ATFL rupture.
Positive anterior drawer test demonstrated on stress radiography.
Inversion and Eversion Stress Tests
Inversion stress testing primarily evaluates the integrity of the CFL, though the ATFL is also implicated if the ankle is plantarflexed. Eversion stress testing evaluates the deltoid ligament. Complete rupture of the deltoid ligament, including the deep intra-articular portion, is rare without concomitant fractures.
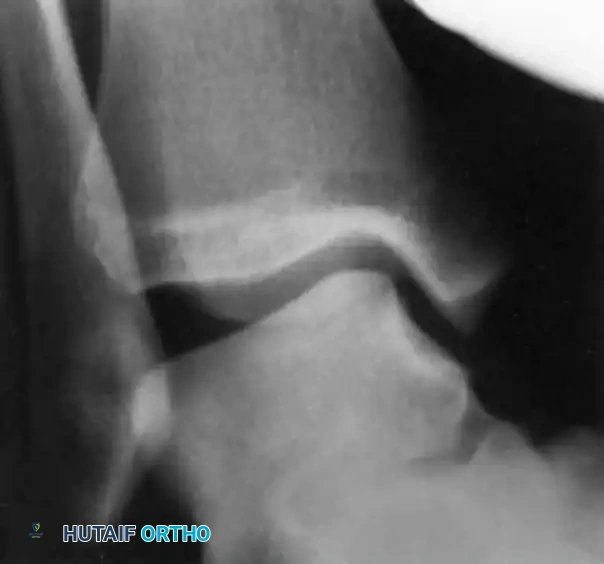
Positive inversion stress test demonstrating significant lateral laxity.
At our institution, we stress both ankles and maintain that more than 10 degrees of talar tilt over that of the normal, contralateral side indicates a significant lateral ligamentous injury. Recently, subtalar sprains have garnered more attention. Although it is clinically difficult to differentiate between a subtalar sprain and a tibiotalar sprain, severe inversion injuries often involve the cervical and interosseous ligaments of the subtalar joint.
Syndesmotic Evaluation
High ankle sprains involve the distal tibiofibular syndesmosis. When the deltoid ligament is completely ruptured in conjunction with a rupture of the tibiofibular syndesmosis, the mortise becomes grossly unstable.
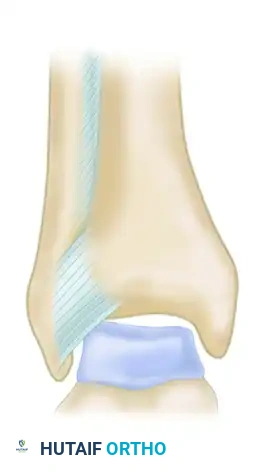
Ligamentous attachments of the syndesmosis (Anterior view A).
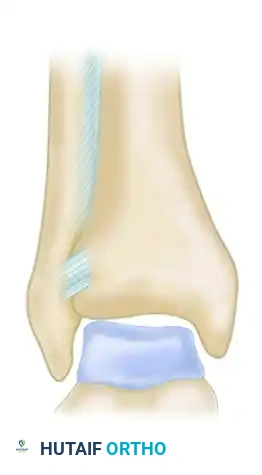
Ligamentous attachments of the syndesmosis (Anterior view B).
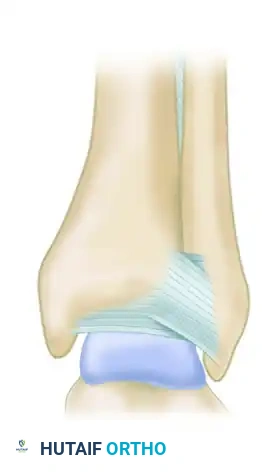
Ligamentous attachments of the syndesmosis (Posterior view C).
Provocative tests for the syndesmosis include the Squeeze Test (compressing the tibia and fibula at the mid-calf) and the External Rotation Stress Test (dorsiflexing and externally rotating the foot). Pain elicited at the distal tibiofibular joint is considered a positive sign.
RADIOGRAPHIC AND ADVANCED IMAGING
Standard and Stress Radiography
Standard weight-bearing orthogonal radiographs (AP, Lateral, and Mortise views) are mandatory to rule out fractures, osteochondral lesions, and malalignment.
An os subfibulare (an accessory ossicle adjacent to the inferior tip of the fibula) most likely represents an old avulsion fracture rather than a normal anatomical variant. It may or may not be associated with chronic laxity of the ATFL. Recurrent inversion sprains of the ankle and continuous discomfort are strict indications for stress radiographs to determine any tibiotalar joint laxity and to assess any pathological movement of the os subfibulare.
Magnetic Resonance Imaging (MRI)
Verhaven et al. determined that three-dimensional MRI was 90% accurate in diagnosing ruptures of the ATFL and CFL. In their study comparing preoperative MRI findings with operative findings in young athletes undergoing surgical exploration for instability, they concluded that 3D, fast-imaging MRI is a noninvasive, highly accurate diagnostic tool that aids in the surgical planning of double ligamentous tears in competitive athletes.
However, MRI has been shown to be more specific than sensitive, especially regarding the CFL.
* Bone Bruises: Bone bruises occur in a significant number of ankle sprains. Multiple bone bruises occur more frequently in patients with multi-ligamentous injuries. Although these lesions peak around 8.4 weeks, they can persist for more than 1 year post-injury.
* Cost-Benefit Ratio: Although MRI is effective in identifying lateral ankle ligament injuries, many experts believe the costs outweigh the benefits for routine acute sprains.
* Indications for MRI: If a peroneal tendon pathological process (e.g., split tear, subluxation) or an osteochondral lesion of the talus (OCLT) is suspected, MRI is highly beneficial. It should not, however, be used routinely to diagnose simple lateral ligament injuries.
NON-OPERATIVE MANAGEMENT
Stress radiographs do not need to be obtained routinely in the acute setting because the vast majority of unstable ligamentous injuries are treated functionally with excellent long-term results.
"Functional" treatment refers to the immediate implementation of RICE (Rest, Ice, Compression, Elevation) combined with a short, semirigid brace or walking boot. This initial phase is rapidly followed by:
1. Early Range-of-Motion (ROM) Exercises: Emphasizing Achilles stretching and sagittal plane motion.
2. Early Weight-Bearing: Progressing as tolerated to stimulate collagen alignment.
3. Neuromuscular Training: Proprioceptive rehabilitation (e.g., wobble board exercises) is the cornerstone of preventing recurrent instability.
SURGICAL MANAGEMENT: THE MODIFIED BROSTRÖM-GOULD PROCEDURE
While functional rehabilitation is the gold standard for acute injuries, approximately 20% of patients will develop Chronic Lateral Ankle Instability (CLAI). When patients fail 3 to 6 months of dedicated physical therapy and continue to experience recurrent "giving way" episodes, surgical intervention is indicated. The Modified Broström-Gould procedure is the internationally recognized standard of care for anatomic lateral ligament reconstruction.
Surgical Indications
- Documented chronic lateral ankle instability failing conservative management.
- High-demand athletes with acute Grade III multi-ligamentous ruptures (relative indication).
- Concomitant intra-articular pathology requiring arthroscopic debridement (e.g., OCLT, anterior impingement).
Patient Positioning and Preparation
- The patient is placed in the supine position on the operating table.
- A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the lateral malleolus directly anterior for optimal visualization.
- A non-sterile thigh tourniquet is applied.
- Standard prophylactic intravenous antibiotics are administered.
Step-by-Step Surgical Approach
1. Diagnostic Arthroscopy (Optional but Recommended):
Prior to open reconstruction, an anterior ankle arthroscopy is frequently performed to address intra-articular pathology, debride hypertrophic synovitis in the lateral gutter, and assess the articular cartilage.
2. Incision and Dissection:
* A 4 to 5 cm curvilinear incision is made along the anterior border of the distal fibula, extending toward the base of the fourth metatarsal.
* Careful blunt dissection is utilized in the subcutaneous tissues to identify and protect the intermediate dorsal cutaneous branch of the superficial peroneal nerve (SPN) anteriorly, and the sural nerve posteriorly.
3. Mobilization of the Extensor Retinaculum:
* The inferior extensor retinaculum (IER) is identified and carefully mobilized off the underlying joint capsule. This structure will be utilized later for the Gould modification.
4. Capsulotomy and Ligament Identification:
* An arthrotomy is performed 2 to 3 mm anterior to the fibular margin.
* The attenuated remnants of the ATFL and CFL are identified. In chronic cases, these ligaments may be scarred into the capsule.
5. Fibular Preparation and Anchor Placement:
* The anterior and inferior footprint of the fibula is decorticated using a rongeur or burr to create a bleeding bone bed, which promotes ligamentous healing.
* Two suture anchors (typically 2.5 mm to 3.0 mm) are placed into the fibula: one at the ATFL footprint (approximately 10 mm proximal to the distal tip) and one at the CFL footprint (at the distal tip).
6. Ligament Imbrication and Tying:
* The sutures are passed through the ATFL and CFL remnants, as well as the lateral capsule, using a pants-over-vest imbrication technique.
* Crucial Step: The ankle is held in neutral dorsiflexion and slight eversion while the sutures are tied. This restores the appropriate tension to the lateral complex. Tying the sutures in plantarflexion will result in a construct that is too loose, leading to recurrent instability.
7. The Gould Modification:
* The previously mobilized inferior extensor retinaculum is advanced proximally and sutured over the repaired ATFL and CFL to the fibular periosteum.
* This modification reinforces the repair, limits inversion, and helps correct any subtle subtalar instability.
Postoperative Protocol
- Weeks 0-2: The patient is placed in a non-weight-bearing short leg cast or rigid splint in neutral dorsiflexion and slight eversion.
- Weeks 2-6: The patient is transitioned to a Controlled Ankle Motion (CAM) boot. Weight-bearing is progressed as tolerated. Active dorsiflexion and plantarflexion exercises are initiated, but inversion and eversion are strictly prohibited.
- Weeks 6-12: The CAM boot is discontinued, and the patient transitions to an ankle-lacing brace (e.g., ASO brace). Formal physical therapy focuses on peroneal strengthening, proprioception, and dynamic stabilization.
- Months 3-6: Return to sport-specific activities and cutting maneuvers is permitted once the patient demonstrates symmetrical strength, full ROM, and negative provocative testing.
CONCLUSION
The management of ankle ligament injuries demands a high index of suspicion, a thorough understanding of regional biomechanics, and a meticulously timed physical examination. While the anterior drawer and talar tilt tests remain the clinical mainstays for diagnosing ATFL and CFL ruptures, advanced imaging such as MRI should be reserved for complex cases involving suspected osteochondral or tendinous pathology. By adhering to evidence-based functional rehabilitation protocols for acute injuries and employing precise anatomical surgical reconstructions for chronic instability, orthopedic surgeons can reliably restore joint kinematics and prevent the debilitating sequelae of post-traumatic ankle arthropathy.
📚 Medical References
- ankle ligament injuries, J Bone Joint Surg 76A:1103, 1994.
- Marks KL: Flake fracture of the talus progressing to osteochondritis dissecans, J Bone Joint Surg 34B:90, 1952.
- Martin DE, Kaplan PA, Kahler DM, et al: Retrospective evaluation of graded stress examination of the ankle, Clin Orthop Relat Res 328:165, 1996.
- McConkey JP, Lloyd-Smith R, Li D: Complete rupture of the deltoid ligament of the ankle, Clin J Sports Med 1:133, 1991.
- McConnell T, Creevy W, Tornetta P III: Stress examination of supination external rotation-type fi bular fractures, J Bone Joint Surg 86A:2171, 2004.
- Meislin RJ, Rose DJ, Parisien JS, et al: Arthroscopic treatment of synovial impingement of the ankle, Am J Sports Med 21:186, 1993.
- Meyer JM, Garcia J, Hoffmeyer P, et al: The subtalar sprain: a roentgenographic study, Clin Orthop Relat Res 226:169, 1988.
- Muhle C, Frank LR, Rand T, et al: Collateral ligaments of the ankle: high-resolution MR imaging with a local gradient coil and anatomic correlation in cadavers, Radiographics 19:673, 1999.
- Mukherjee K, Gangopadhyay P: Extensor digitorum brevis transfer in chronic unstakle ankles, J R Coll Surg Edinb 28:250, 1983.
- Mukherjee SK, Young AB: Dome fractures of the talus: a report of ten cases, J Bone Joint Surg 55B:319, 1973.
- Myerson MA, ed: Current therapy in foot and ankle surgery , St. Louis, 1993, Mosby-Year Book. Myerson M, ed: Reconstructive foot and ankle surgery , Philadelphia, 2005, Saunders. Nash WC, Baker CL: Transchondral talar dome fractures: not just a sprained ankle, South Med J 77:560, 1984.
- O’Connor D: Sinus tarsi syndrome: a clinical entity, J Bone Joint Surg 40A:720, 1958.
- O’Doherty DP, Lowrie IG, Gregg PJ: Caisson disease of the talus: brief report, J Bone Joint Surg 69B:847, 1987.
- O’Donoghue DH: Impingement exostoses of the talus and tibia, J Bone Joint Surg 39A:835, 1957.
- Ogilvie-Harris DJ, Mahomed N, Demaziére A: Anterior impingement of the ankle treated by arthroscopic removal of bony spurs, J Bone Joint Surg 75B:437, 1993.
- Ogilvie-Harris DJ, Sarrosa EA: Arthroscopic treatment after previous failed open surgery for osteochondritis dissecans of the talus, Arthroscopy 15:809, 1999.
- Ogilvie-Harris DJ, Sarrosa EA: Arthroscopic treatment of osteochondritis dissecans of the talus, Arthroscopy 15:805, 1999.
- Olson RW: Arthrography of the ankle: its use in the evaluation of ankle sprains, Radiology 92:1439, 1969.
- Pankovich AM: Maisonneuve fracture of the fi bula, J Bone Joint Surg 58A:337, 1976.
- Parisien JS: Diagnostic and surgical arthroscopy of the ankle: technique and indications, Bull Hosp Jt Dis 45:38, 1985.
- Parisien JS: Arthroscopic treatment of osteochondral lesions of the talus, Am J Sports Med 14:211, 1986.
- Pettine KA, Morrey BF: Osteochondral fractures of the talus: a long-term follow-up, J Bone Joint Surg 69B:89, 1987.
- Pijnenberg AC, Bogaard K, Krips R, et al: Operative and functional treatment of rupture of the lateral ligament of the ankle: a randomized, prospective trial, J Bone Joint Surg 85B:525, 2003.
- Povacz P, Unger SF, Miller WK, et al: A randomized, prospective study of operative and nonoperative treatment of injuries of the fi bular collateral ligaments of the ankle, J Bone Joint Surg 80:345, 1998.
- Pritsch M, Horoshovski H, Farine I: Arthroscopic treatment of osteochondral lesions of the talus, J Bone Joint Surg 68A:862, 1986.
- Raatikainen T, Puranen J: Arthrography for the diagnosis of acute lateral ligament injuries of the ankle, Am J Sports Med 21:343, 1993.
- Ramsey PL, Hamilton W: Changes in tibiotalar areas of contact caused by lateral talar shift, J Bone Joint Surg 58A:356, 1976.
- Ray RG, Christensen JC, Gusman DN: Critical evaluation of anterior drawer measurement methods in the ankle, Clin Orthop Relat Res 334:215, 1997.
- Redfern D, Myerson M: The management of concomitant tears of the peroneus longus and brevis tendons, Foot Ankle Int 25:695, 2004.
- Regnauld B: Sinus tarsi syndrome. In: The foot: pathology, etiology, semiology, clinical investigation, and therapy, New York, 1986, Springer-Verlag. Rendu A: Fracture intra-articulaire parcellaire de la poûlie astraglienne, Lyon Med 150:220, 1932.
- Rijke AM, Jones B, Vierhout PA: Injury to the lateral ankle ligaments of athletes: a posttraumatic follow-up, Am J Sports Med 16:256, 1988.
- Rödén S, Tillegàrd P, Unander-Scharin L: Osteochondritis dissecans and similar lesions of the talus, Acta Orthop Scand 23:51, 1953.
- Rosenbaum D, Becker HP, Sterk J, et al: Functional evaluation of the 10-year outcome after modifi ed Evans repair for chronic ankle instability, Foot Ankle Int 18:765, 1997.
- Rosenbaum D, Becker HP, Wilke HJ, et al: Tenodeses destroy the kinematic coupling of ankle joint complex: a three-dimensional in vitro analysis of joint movement, J Bone Joint Surg 80B:162, 1998.
- Rubin G, Witten M: The talar-tilt angle and the fi bular collateral ligaments: a method for the determination of talar tilt, J Bone Joint Surg 42A:311, 1960.
- Rudert M, Wulker N, Wirth CJ: Reconstruction of the lateral ligaments of the ankle using regional periosteal fl ap, J Bone Joint Surg 79B:446, 1997.
- Ruth CJ: The surgical treatment of injuries of the fi bular collateral ligaments of the ankle, J Bone Joint Surg 43A:229, 1961.
- Sammarco GJ, Carrasquillo HA: Surgical revision after failed
You Might Also Like