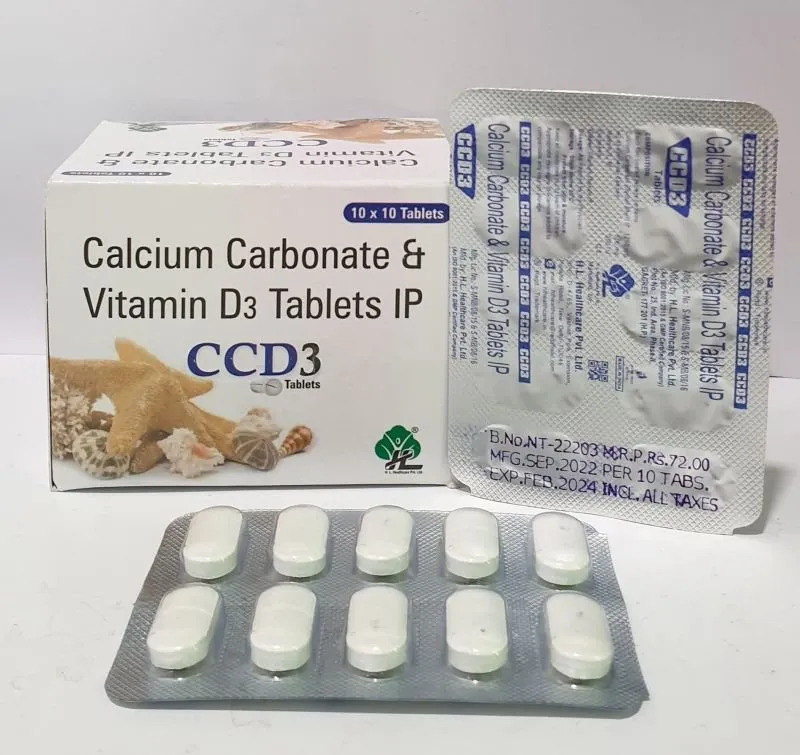
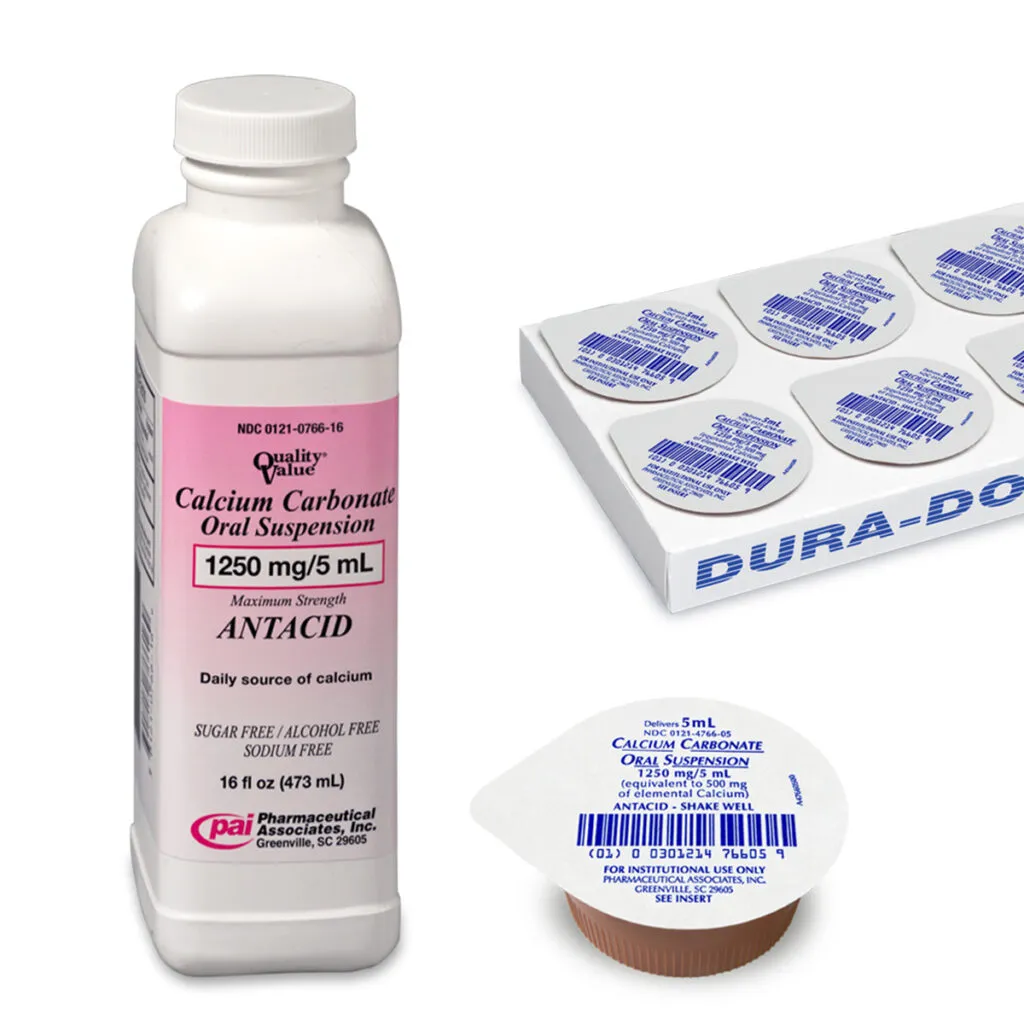
The Comprehensive Guide to Calcium Carbonate + Cholecalciferol (Vitamin D3) Tablets
As an expert in orthopedic health and medical SEO, we understand the critical role that proper nutritional supplementation plays in maintaining robust skeletal integrity and overall well-being. Among the most fundamental supplements for bone health is the combination of Calcium Carbonate and Cholecalciferol (Vitamin D3). This guide provides an exhaustive, authoritative, and medically accurate overview of this crucial medication, designed to inform both patients and healthcare professionals.
1. Comprehensive Introduction & Overview
Calcium and Vitamin D are two indispensable nutrients vital for numerous physiological processes, with their most renowned role being in bone metabolism and maintenance. Calcium provides the structural framework for bones and teeth, while Vitamin D acts as the primary regulator of calcium and phosphate homeostasis, ensuring their proper absorption and utilization.
The "Calcium Carbonate + Cholecalciferol (Vitamin D3) Tablet" is a widely prescribed and over-the-counter medication formulated to address deficiencies in these critical nutrients or to support increased demand, particularly in conditions affecting bone density. This combination offers a synergistic approach, where Vitamin D3 significantly enhances the absorption of dietary and supplemental calcium, thereby maximizing its benefits for skeletal health.
This guide will delve into the intricate mechanisms by which these components function, their pharmacokinetic profiles, extensive clinical indications, precise dosage guidelines, potential risks, drug interactions, and crucial considerations for specific populations like pregnant or lactating individuals.
2. Deep-Dive into Technical Specifications / Mechanisms
Understanding how Calcium Carbonate and Cholecalciferol work at a molecular level is key to appreciating their therapeutic value.
2.1. Mechanism of Action
Calcium Carbonate
Calcium Carbonate is a salt of calcium, providing a high percentage of elemental calcium (approximately 40%). When ingested, it dissociates in the acidic environment of the stomach into calcium ions (Ca2+). These ions are then absorbed primarily in the duodenum and jejunum of the small intestine through both active transport (vitamin D-dependent) and passive diffusion.
- Bone Mineralization: Calcium is the primary mineral component of hydroxyapatite crystals, which give bones their strength and rigidity. Adequate calcium intake is essential for bone formation, remodeling, and preventing bone loss.
- Neuromuscular Function: Calcium ions play a crucial role in nerve impulse transmission, muscle contraction (including cardiac muscle), and neurotransmitter release.
- Blood Coagulation: Calcium is a vital co-factor in the cascade of reactions leading to blood clot formation.
- Cellular Signaling: It participates in various intracellular signaling pathways, hormone secretion, and enzyme activation.
Cholecalciferol (Vitamin D3)
Cholecalciferol, or Vitamin D3, is a fat-soluble vitamin that is either synthesized in the skin upon exposure to ultraviolet B (UVB) radiation or obtained from dietary sources and supplements. It is biologically inactive until it undergoes two hydroxylation steps:
- First Hydroxylation (Liver): Cholecalciferol is hydroxylated in the liver by the enzyme 25-hydroxylase (CYP2R1) to form 25-hydroxyvitamin D [25(OH)D], also known as calcifediol. This is the primary circulating form of Vitamin D and the best indicator of Vitamin D status.
- Second Hydroxylation (Kidney): 25(OH)D is further hydroxylated in the kidneys by the enzyme 1-alpha-hydroxylase (CYP27B1) to form 1,25-dihydroxyvitamin D [1,25(OH)2D], also known as calcitriol. Calcitriol is the biologically active form of Vitamin D and a potent steroid hormone.
Actions of Calcitriol:
- Intestinal Calcium Absorption: Calcitriol is the most important regulator of intestinal calcium absorption. It stimulates the synthesis of calcium-binding proteins (e.g., calbindin) in enterocytes, facilitating active transport of calcium across the intestinal wall.
- Renal Calcium and Phosphate Reabsorption: It promotes the reabsorption of calcium and phosphate in the renal tubules, reducing their excretion in urine.
- Bone Remodeling: Calcitriol works in conjunction with parathyroid hormone (PTH) to maintain calcium and phosphate homeostasis. While high levels can stimulate bone resorption, physiological levels are crucial for optimal bone mineralization and remodeling by regulating osteoblast and osteoclast activity.
- Other Roles: Vitamin D receptors are found in nearly all tissues, indicating its broader roles in immune function, cell growth, and differentiation.
2.2. Pharmacokinetics
Absorption
- Calcium Carbonate: Absorption is variable, typically ranging from 20-40% of the ingested dose. It is significantly enhanced by gastric acid and is best absorbed when taken with food. The presence of Vitamin D3 further boosts its absorption.
- Cholecalciferol (Vitamin D3): Being fat-soluble, Vitamin D3 is absorbed from the small intestine primarily via lymphatic pathways, similar to other dietary fats. Its absorption is improved when taken with a fatty meal.
Distribution
- Calcium: Circulates in the blood in three forms: protein-bound (approximately 40-45%, mainly to albumin), complexed with anions (e.g., citrate, phosphate, 10-15%), and ionized (free Ca2+, 45-50%). Only the ionized form is biologically active.
- Vitamin D3: After absorption, cholecalciferol enters the bloodstream, binds to vitamin D-binding protein (DBP), and is transported to the liver for its initial hydroxylation. 25(OH)D also circulates bound to DBP and is stored in adipose tissue and muscle.
Metabolism
- Calcium: Calcium itself is not metabolized in the traditional sense; its levels are tightly regulated by PTH, calcitonin, and calcitriol.
- Vitamin D3: Undergoes two main hydroxylation steps as described above (liver to 25(OH)D, kidney to 1,25(OH)2D). Further metabolism of 1,25(OH)2D occurs via 24-hydroxylase (CYP24A1) to inactive metabolites, which is an important regulatory pathway.
Excretion
- Calcium: Primarily excreted via feces (unabsorbed calcium). A smaller portion is excreted renally, with the amount regulated by PTH and calcitriol.
- Vitamin D3: Inactive metabolites of Vitamin D and its active forms are primarily excreted via the bile into the feces. A small amount is excreted renally.
3. Extensive Clinical Indications & Usage
The combination of Calcium Carbonate and Cholecalciferol is indicated for a wide array of conditions, primarily those related to calcium and vitamin D deficiencies or increased requirements.
3.1. Primary Indications
- Prevention and Treatment of Osteoporosis: This is a cornerstone indication. Calcium and Vitamin D are fundamental for maintaining bone mineral density, reducing fracture risk in post-menopausal women, elderly men, and individuals on long-term corticosteroid therapy.
- Osteopenia: For individuals with reduced bone density but not yet meeting osteoporosis criteria, supplementation helps prevent progression.
- Vitamin D Deficiency: Direct treatment of insufficient or deficient vitamin D levels.
- Calcium Deficiency (Hypocalcemia): To correct low blood calcium levels, which can arise from various conditions including hypoparathyroidism, renal failure (with specific monitoring), or malabsorption.
- Nutritional Support: For individuals with inadequate dietary intake of calcium and vitamin D, such as those with lactose intolerance, vegans, or individuals with restrictive diets.
- Adolescent Bone Development: To ensure peak bone mass attainment during critical growth phases.
- Pregnancy and Lactation: To meet the increased demands for calcium and vitamin D during these periods, supporting both maternal and fetal/infant bone health.
- Adjunct to Corticosteroid Therapy: Corticosteroids can induce osteoporosis by impairing calcium absorption and increasing bone resorption. Supplementation helps counteract these effects.
- Certain Malabsorption Syndromes: Conditions like Crohn's disease, celiac disease, or gastric bypass surgery can impair nutrient absorption, necessitating supplementation.
- Chronic Kidney Disease (CKD) and Renal Osteodystrophy: While requiring careful monitoring and sometimes specific active vitamin D analogs, calcium and vitamin D supplementation can be part of the management plan under strict medical supervision to prevent secondary hyperparathyroidism and bone disease.
3.2. Dosage Guidelines
Dosage varies significantly based on age, specific indication, severity of deficiency, and individual patient characteristics. It is crucial to follow a healthcare provider's recommendations.
| Patient Group / Condition | Recommended Elemental Calcium | Recommended Vitamin D3 | Notes |
|---|---|---|---|