The Arm Sling: An Essential Orthopedic Therapeutic Intervention
As expert orthopedic specialists, we understand the critical role of proper immobilization and support in the healing process of upper limb injuries. The arm sling, often perceived as a simple device, is in fact a sophisticated therapeutic intervention with specific mechanisms of action, indications, and protocols for optimal patient outcomes. This comprehensive guide delves into the arm sling, treating it as a prescribed medical device whose application and management mirror the precision required for any pharmaceutical "medication" to ensure effective recovery and minimize complications.
Comprehensive Introduction & Overview of the Arm Sling
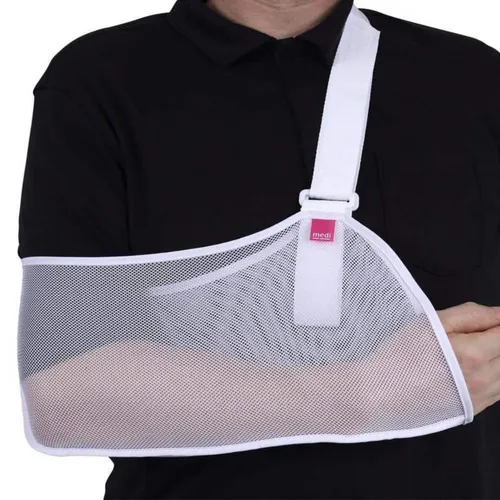
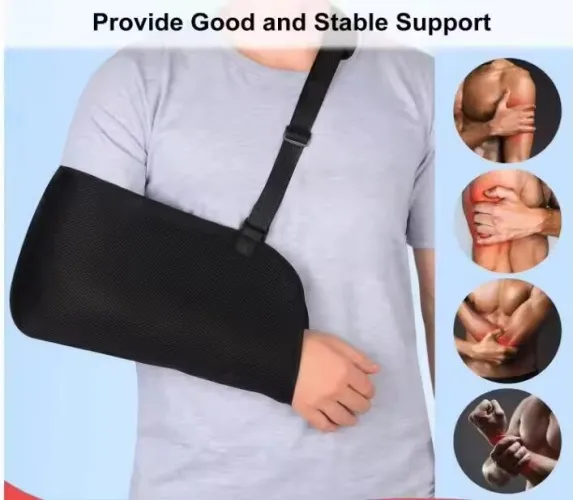
An arm sling is a medical device designed to support and immobilize the upper limb, typically the arm, wrist, and hand. Its primary function is to keep the arm in a stable, elevated position, reducing movement and stress on an injured or surgically repaired area. While seemingly straightforward, the correct selection, fitting, and wear schedule of an arm sling are paramount to achieving its therapeutic goals.
Key Functions of an Arm Sling:
- Immobilization: Prevents unwanted movement of the injured joint or bone, crucial for fracture healing and ligament repair.
- Support: Elevates the arm, counteracting gravity's pull, which reduces pain and muscle fatigue.
- Protection: Shields the injured area from accidental bumps or further trauma.
- Edema Control: Elevating the limb can aid in reducing swelling, especially in acute injuries.
- Comfort: Provides significant pain relief by stabilizing the limb.
- Patient Compliance: Acts as a visual reminder to the patient and others about the injury, promoting caution.
Different types of arm slings exist, ranging from basic envelope slings to more complex shoulder immobilizers, each tailored to specific injury patterns and therapeutic requirements. Understanding its "mechanism of action" and "therapeutic kinetics" is vital for its effective "prescription" and "administration."
Deep-Dive into Technical Specifications & Therapeutic Mechanisms
While an arm sling isn't a drug, its therapeutic effects can be analyzed through a similar lens, focusing on its physical "mechanism of action" and the "kinetics" of its interaction with the body to facilitate healing.
Mechanism of Action (Physical & Biomechanical)
The "mechanism of action" of an arm sling refers to the biomechanical principles by which it achieves its therapeutic effects:
- Gravity Counteraction & Weight Distribution: The sling's primary role is to suspend the weight of the arm, distributing it across the shoulder and neck. This offloads the injured joint or bone, reducing tensile and shear forces that could impede healing or cause pain.
- Effect: Reduces muscle spasm, alleviates joint compression, and minimizes stress on ligaments and tendons.
- Immobilization & Restricted Range of Motion (ROM): By cradling the forearm and wrist against the torso, the sling limits abduction, adduction, rotation, and flexion/extension of the shoulder and elbow.
- Effect: Promotes callus formation in fractures, prevents re-dislocation, protects surgical repairs, and allows soft tissues to rest and repair.
- Elevation for Edema Control: Maintaining the hand and forearm above heart level, particularly with proper sling adjustment, leverages gravity to facilitate venous return and lymphatic drainage.
- Effect: Reduces post-traumatic or post-surgical swelling (edema), which can decrease pain and improve tissue oxygenation.
- Proprioceptive Feedback & Protection: The physical presence of the sling provides constant proprioceptive input, reminding the patient of the injury and encouraging cautious movement. It also acts as a physical barrier against external trauma.
- Effect: Enhances patient compliance, prevents accidental re-injury, and fosters a sense of security.
Therapeutic Kinetics (Reinterpreted "Pharmacokinetics")
While true pharmacokinetics (absorption, distribution, metabolism, excretion) don't apply, we can conceptualize the "therapeutic kinetics" of an arm sling regarding its onset, duration, and factors influencing its efficacy over time.
- Onset of Therapeutic Effect:
- Immediate: Upon correct application, the sling immediately provides support, immobilization, and pain relief. The physical offloading of weight and stabilization are instantaneous.
- Analogy: Similar to the rapid onset of an analgesic administered intravenously.
- Distribution of Support:
- The "distribution" refers to how the supportive forces are spread across the patient's body. A well-fitted sling distributes pressure evenly across the shoulder and neck via the strap, and cradles the forearm and hand without creating focal pressure points.
- Factors: Proper sling size, adjustable straps, padding, and material conformity are crucial for optimal "distribution."
- "Metabolism" (Duration & Maintenance of Effect):
- The "therapeutic effect" of the sling is maintained as long as it is worn correctly and remains structurally sound. Factors affecting this "metabolism" include:
- Patient Compliance: Adherence to wear schedule.
- Sling Integrity: Wear and tear, material degradation.
- Hygiene: Cleanliness of the sling and underlying skin.
- Fit Adjustments: Changes in swelling or patient posture may necessitate readjustments to maintain optimal support.
- Analogy: Like a sustained-release medication, the sling provides continuous therapeutic benefit, but its efficacy can diminish without proper maintenance and adherence.
- The "therapeutic effect" of the sling is maintained as long as it is worn correctly and remains structurally sound. Factors affecting this "metabolism" include:
- "Elimination" (Discontinuation of Use):
- The "elimination" of the sling's therapeutic role occurs when it is no longer medically necessary. This is determined by clinical assessment of healing, pain levels, and functional recovery. Gradual weaning from the sling is often recommended to prevent stiffness and muscle atrophy.
- Analogy: Similar to tapering off a medication to avoid withdrawal symptoms or rebound effects.
Extensive Clinical Indications & Usage
The arm sling is indicated for a wide array of orthopedic conditions affecting the shoulder, arm, elbow, wrist, and hand. Its "prescription" is based on the specific injury, the desired degree of immobilization, and the stage of healing.
Detailed Indications
| Injury/Condition | Specific Rationale for Sling Use | Desired Outcome |
|---|---|---|
| Clavicle Fractures | Provides support and reduces movement at the fracture site, promoting healing and pain relief. Often used with a figure-of-8 brace. | Stable union, pain reduction, improved alignment. |
| Proximal Humerus Fractures | Immobilizes the shoulder joint, preventing rotation and translation of fracture fragments. | Fracture healing, minimized displacement, pain control. |
| Scapular Fractures | Supports the shoulder girdle, reducing pain and allowing soft tissue healing around the scapula. | Pain relief, stable fracture healing. |
| Shoulder Dislocations/Subluxations | Keeps the humerus head reduced in the glenoid fossa, allowing capsular and ligamentous structures to heal. | Prevention of re-dislocation, ligamentous healing, pain reduction. |
| Rotator Cuff Tears/Repairs | Protects the surgical repair or allows acute tears to rest, preventing abduction and external rotation. | Tendon healing, reduced tension on repair, pain management. |
| Elbow Fractures/Dislocations | Immobilizes the elbow in a flexed position, preventing harmful movements during healing. | Stable fracture union, ligamentous healing, pain control. |
| Forearm Fractures (Radius/Ulna) | Provides additional support to a cast or splint, elevating the limb and reducing swelling. | Enhanced stability, edema control, patient comfort. |
| Wrist Fractures/Sprains | Elevates the hand and wrist, reducing swelling and providing gentle support, often used with a wrist brace. | Edema reduction, pain relief, support during healing. |
| Hand Fractures/Surgery | Elevates the hand to reduce swelling and protect delicate repairs. | Edema control, protection of surgical sites, improved comfort. |
| Acute Soft Tissue Injuries | Provides temporary rest and support for severe sprains, strains, or contusions of the upper limb. | Pain relief, reduced inflammation, protection from further injury. |
| Post-Surgical Recovery | Standard protocol after many upper limb surgeries (e.g., arthroscopy, open reduction internal fixation). | Protection of surgical site, reduced stress on repairs, comfort. |
Dosage Guidelines (Proper Application & Wear Protocol)
The "dosage" of an arm sling refers to its correct application, duration of wear, and necessary adjustments. This is critical for maximizing its therapeutic benefit and avoiding complications.
1. Proper Fitting & Application:
- Sizing: Select the appropriate sling size. The forearm should rest comfortably within the sling, with the wrist supported and the hand extending slightly beyond the opening. The elbow should be at a 90-degree angle (or as prescribed).
- Positioning: Place the injured arm into the sling, ensuring the elbow is deep within the sling's pocket. The hand should be slightly higher than the elbow to promote edema reduction.
- Strap Adjustment: The neck strap should be adjusted so the arm is comfortably supported and elevated. It should not cause excessive pressure on the neck or pull the shoulder too high. Ensure the strap lies flat to prevent digging into the skin.
- Neurovascular Check: After application, always check for signs of neurovascular compromise:
- Color: Fingers should be pink, not pale or blue.
- Temperature: Fingers should be warm, not cold.
- Capillary Refill: Press on a fingernail; color should return within 2 seconds.
- Sensation: Ask the patient if they can feel touch in their fingertips.
- Movement: Ask the patient to wiggle their fingers.
- If any issues are noted, readjust the sling immediately.
2. Duration & Wear Schedule:
- Continuous Wear: For acute fractures, dislocations, or post-surgical immobilization, the sling may need to be worn continuously (24/7), only removed for hygiene or prescribed exercises.
- Intermittent Wear: For less severe injuries or later stages of healing, the sling may be worn for specific activities or during periods of increased risk, with planned removal for exercises.
- Total Duration: This varies widely, from a few days for minor sprains to 6-12 weeks for complex fractures or rotator cuff repairs. Always follow the specific instructions of your orthopedic specialist.
- Sleeping: The sling should typically be worn during sleep to prevent inadvertent movement. Specific sleeping positions may be recommended.
3. Hygiene & Skin Care:
- Sling Cleaning: Follow manufacturer guidelines. Most fabric slings can be hand-washed with mild soap and air-dried.
- Skin Inspection: Regularly inspect the skin under the sling, especially at pressure points (neck, armpit, elbow), for redness, irritation, or breakdown.
- Personal Hygiene: Remove the sling for showering/bathing (if medically permitted) to clean the arm and shoulder. Ensure the skin is thoroughly dried before reapplying the sling.
Risks, Side Effects, and Contraindications
While generally safe and highly beneficial, arm slings are not without potential "side effects" or "contraindications" if used improperly or when not indicated.
Contraindications
- Unstable Fractures Requiring Different Immobilization: Some fractures (e.g., certain humeral shaft fractures, spiral fractures) may require a rigid cast, brace, or surgical fixation rather than just a sling to maintain alignment.
- Open Wounds Requiring Air Exposure: Slings can cover and occlude wounds, potentially hindering healing or promoting infection if not managed properly.
- Severe Neurovascular Compromise: If the sling exacerbates nerve compression or arterial/venous compromise, it should be immediately removed and adjusted or alternative immobilization sought.
- Risk of Frozen Shoulder (Adhesive Capsulitis): Prolonged, complete immobilization of the shoulder, particularly in older adults or those predisposed, can lead to stiffness. A balance between support and early, controlled motion is often critical.
- Conditions Requiring Immediate Surgical Intervention: A sling is a temporary measure; it should not delay definitive treatment for injuries requiring urgent surgery.
Potential "Side Effects" / Complications of Improper or Prolonged Use
- Stiffness and Reduced Range of Motion: Prolonged immobilization can lead to joint stiffness (e.g., frozen shoulder), muscle contractures, and atrophy.
- Muscle Atrophy: Disuse of the immobilized limb results in muscle wasting, which requires rehabilitation to regain strength.
- Nerve Compression: Improperly adjusted straps can compress nerves (e.g., superficial radial nerve, ulnar nerve, brachial plexus), leading to numbness, tingling, or weakness.
- Skin Irritation/Breakdown: Pressure points, friction, moisture, or inadequate hygiene can cause rashes, pressure sores, or skin maceration.
- Edema (if improperly positioned): If the hand is allowed to hang lower than the elbow, the sling can worsen swelling in the hand.
- Deep Vein Thrombosis (DVT): While less common in upper limbs, reduced mobility and venous stasis, especially in patients with pre-existing risk factors, can increase DVT risk.
- Postural Changes/Back Pain: Carrying the arm in a sling for extended periods can alter posture, leading to neck, shoulder, or back pain.
"Drug Interactions" (Interactions with Concurrent Treatments)
The arm sling's therapeutic role exists within a broader treatment plan, and its use can "interact" with other interventions.
- Physical Therapy & Rehabilitation: The sling's use must be coordinated with physical therapy. It may need to be removed for specific exercises, and its duration of use will be gradually reduced as rehabilitation progresses.
- Pain Management Medications: While the sling provides significant pain relief, it may be used in conjunction with analgesics. Patients should be aware that the sling's support can reduce the need for strong pain medications. However, masking pain entirely might lead to overexertion when the sling is removed.
- Other Immobilization Devices: If a cast or splint is also applied, the sling provides additional elevation and protection. Ensure the sling accommodates the other device without causing new pressure points.
- Ice/Heat Therapy: The sling can facilitate the application of ice packs (by holding them in place) or heat pads, but care must be taken to protect the skin and prevent cold/heat injury.
- Mobility Aids: Patients using crutches or walkers must ensure the sling does not impede their balance or ability to safely use these aids.
Pregnancy & Lactation Warnings (Special Population Considerations)
While not a pharmacological agent, the use of an arm sling in pregnant or lactating individuals requires special considerations to ensure safety and comfort for both mother and baby.
- Pregnancy:
- Balance & Posture: The altered center of gravity during pregnancy can be further impacted by an arm sling, increasing the risk of falls. Careful gait assessment and advice are necessary.
- Comfort: The weight of the sling on the neck and shoulder can exacerbate pre-existing discomfort common in pregnancy (e.g., neck strain, upper back pain). Wider, padded straps or alternative support methods may be beneficial.
- Skin Integrity: Hormonal changes and increased skin sensitivity during pregnancy can make skin more prone to irritation or breakdown under pressure points. Frequent skin checks are advised.
- DVT Risk: Pregnancy is a hypercoagulable state. Immobilization from an arm sling, especially if combined with reduced overall activity, can further increase the risk of DVT. Encourage leg exercises and hydration.
- Lactation:
- Comfort & Fit: Breast enlargement during lactation may affect the fit and comfort of the sling, particularly the chest strap or how the arm rests against the body. Adjustments or specific sling designs may be needed.
- Infant Care: An arm sling significantly impairs the ability to hold, lift, or nurse an infant. This can be a major practical challenge and requires careful planning and support from caregivers.
- Pressure on Breasts: Ensure the sling does not exert undue pressure on the breasts, which could lead to discomfort or interfere with milk flow.
Overdose Management (Management of Misuse or Complications)
There is no "overdose" in the pharmacological sense for an arm sling. However, prolonged or improper use can lead to adverse effects, which require management similar to addressing drug-related complications.
Symptoms of "Overuse" or Misuse:
- Severe Joint Stiffness: Inability to move the shoulder or elbow through its normal range after the prescribed immobilization period.
- Persistent Muscle Weakness/Atrophy: Marked reduction in muscle mass and strength in the affected limb.
- Neurological Symptoms: Numbness, tingling, burning, or weakness in the hand/fingers that worsens with sling use, indicating nerve compression.
- Skin Lesions: Redness, blistering, open sores, or signs of infection under the sling.
- Increased Pain (paradoxical): If the sling is ill-fitting, it can cause new pain rather than relieve it.
- Signs of DVT: Swelling, pain, warmth, or redness in the arm, shoulder, or neck.
Management of "Overdose" / Complications:
- Sling Removal & Reassessment: Immediately remove the sling. A thorough clinical examination of the affected limb and neurovascular status is paramount.
- Addressing Specific Complications:
- Stiffness/Atrophy: Referral to physical therapy for range of motion exercises, strengthening, and mobilization techniques.
- Nerve Compression: Adjust sling fit, provide padding, or consider alternative immobilization. In severe cases, nerve decompression may be required.
- Skin Issues: Wound care, infection management (if applicable), and adjustment of sling type or padding.
- DVT: Immediate medical evaluation, potentially involving ultrasound and anticoagulation therapy.
- Patient Education: Reinforce proper sling application, wear schedule, hygiene, and warning signs. Emphasize the importance of following prescribed activity levels.
- Gradual Weaning: If complications arose from prolonged immobilization, a structured plan for gradual reduction of sling use and increased activity is crucial.
Massive FAQ Section: Your Questions Answered
Q1: How do I know if my arm sling is fitted correctly?
A1: Your arm sling is fitted correctly if your elbow is comfortably seated at the back of the sling, your wrist is fully supported, and your hand extends slightly beyond the front opening. Your arm should be bent at approximately a 90-degree angle, and the strap should distribute the weight evenly across your shoulder and neck without digging in. Your fingers should be warm, pink, and you should be able to wiggle them freely.
Q2: Can I remove my arm sling to shower or sleep?
A2: For most acute injuries or post-surgical recovery, it is recommended to wear the sling during sleep to prevent inadvertent movement. You may be advised to remove the sling for showering, but only if cleared by your doctor, and you must support your arm carefully with your other hand. Always follow your surgeon's or doctor's specific instructions.
Q3: How long do I need to wear an arm sling?
A3: The duration of arm sling use varies significantly based on the type and severity of your injury, as well as your individual healing process. It can range from a few days for minor sprains to 6-12 weeks or more for complex fractures or extensive surgical repairs. Your orthopedic specialist will provide a specific timeline and advise you on when to gradually reduce or discontinue use.
Q4: What are the signs that my arm sling might be too tight or causing a problem?
A4: Signs of a problem include:
* Numbness, tingling, or "pins and needles" in your fingers or hand.
* Your fingers becoming pale, blue, or cold.
* Increased pain that doesn't subside with repositioning.
* Redness, skin irritation, or sores developing under the sling or strap.
* Swelling in your hand or fingers that worsens.
If you experience any of these, loosen or adjust the sling immediately and contact your doctor if symptoms persist.
Q5: Can I drive while wearing an arm sling?
A5: Generally, it is NOT recommended to drive while wearing an arm sling, especially if it's on your dominant arm. The sling restricts your range of motion, interferes with your ability to operate controls safely, and could impair your reaction time. It can also be seen as an impairment by insurance companies in the event of an accident. Always consult your doctor and check local traffic laws.
Q6: How do I clean my arm sling?
A6: Most fabric arm slings can be hand-washed with mild soap and cold water. Gently squeeze out excess water and air dry completely. Avoid machine washing or drying, as this can damage the material or affect the sling's shape and integrity. Ensure the sling is fully dry before reapplying to prevent skin irritation.
Q7: What exercises can I do while wearing an arm sling?
A7: While your arm is immobilized, your doctor or physical therapist may prescribe specific "pendulum exercises" (gentle swinging of the arm while leaning forward, letting gravity assist) or finger/wrist mobility exercises to prevent stiffness. It's crucial not to perform any exercises beyond what is specifically instructed, as this could re-injure the healing area.
Q8: My uninjured shoulder and neck are starting to hurt. Is this normal?
A8: Yes, it can be common to experience discomfort in your uninjured shoulder, neck, or back. This is often due to altered posture, muscle strain from compensating for the immobilized arm, and the weight of the sling itself. Ensure your sling is properly adjusted, consider using extra padding under the strap, and practice gentle neck and back stretches if approved by your doctor.
Q9: What should I do if my arm starts to swell while in the sling?
A9: If your arm or hand starts to swell, ensure your hand is elevated slightly higher than your elbow within the sling. Check that the sling isn't too tight anywhere. Apply ice packs (if advised by your doctor) to the affected area for 15-20 minutes at a time, protecting your skin. If swelling persists, worsens, or is accompanied by severe pain, numbness, or color changes, contact your doctor immediately.
Q10: When can I stop wearing my arm sling completely?
A10: You should only stop wearing your arm sling completely when your orthopedic specialist advises you to do so. This decision will be based on clinical examination, imaging results (if applicable), your pain levels, and your ability to perform certain movements without pain or instability. Often, a gradual weaning process is recommended to allow your muscles and joints to regain strength and mobility.
Q11: Can I wear clothing over my arm sling?
A11: Yes, you can typically wear loose-fitting clothing over your arm sling. Choose shirts or jackets that are easy to put on and take off, preferably with wide sleeves or front openings. Avoid tight clothing that could restrict circulation or interfere with the sling's proper positioning.
Q12: What if my arm feels stiff after being in the sling for a long time?
A12: Stiffness is a common consequence of immobilization. Once your doctor clears you to remove the sling, a structured physical therapy program will be essential. This will focus on regaining range of motion, flexibility, and strength in your shoulder, elbow, and wrist. Do not force movements, and always follow the guidance of your therapist.