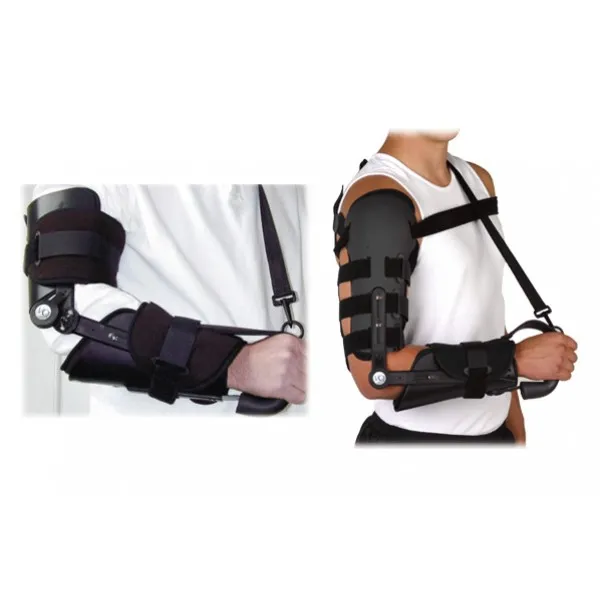
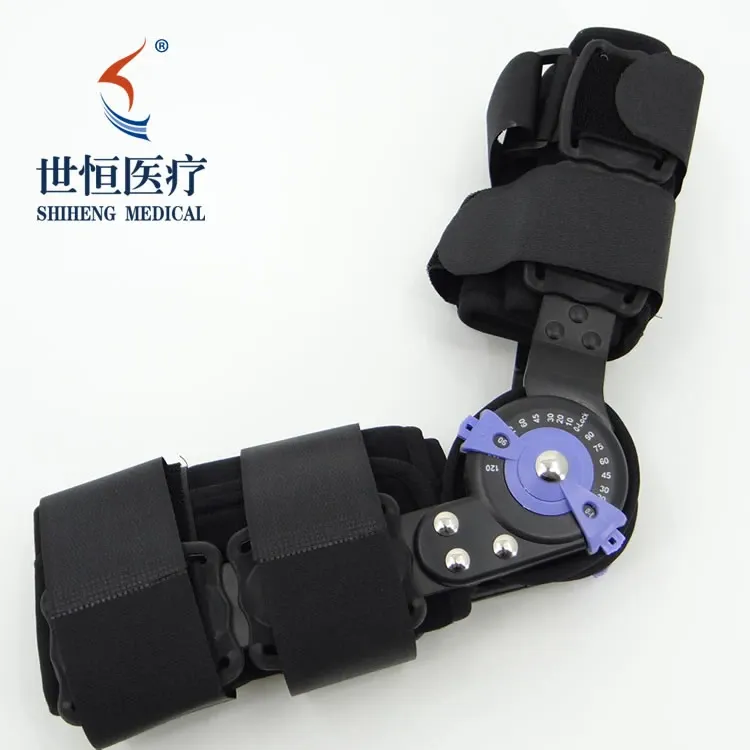
The Definitive Medical SEO Guide to Arm Braces: Support, Stabilization, and Rehabilitation
An arm brace, often referred to as an orthopedic arm support or immobilizer, is a crucial medical device designed to provide external support, stability, and protection to the arm, wrist, and hand. Far from being a mere accessory, an arm brace plays a pivotal role in the healing process following injuries, surgeries, or in managing chronic conditions affecting the upper limb. As expert Medical SEO Copywriters and Orthopedic Specialists, we understand the critical importance of accurate, comprehensive information regarding these devices. This exhaustive guide delves into every aspect of arm braces, offering unparalleled insights for patients, caregivers, and healthcare professionals alike.
Understanding Arm Braces: A Comprehensive Overview
Arm braces come in various forms, each tailored to specific anatomical regions and functional requirements. From simple slings that support the weight of the arm to rigid splints that completely immobilize a joint, their primary goal remains consistent: to facilitate optimal healing, reduce pain, and prevent further injury. While the prompt categorizes "Arm Brace" under "Medication," it is imperative to clarify that an arm brace is a medical device, not a pharmacological agent. Therefore, traditional concepts of "mechanism of action" (in a biochemical sense), "pharmacokinetics," "drug interactions," or "overdose management" as applied to drugs do not directly apply. Instead, we will interpret these concepts within the biomechanical and clinical framework relevant to orthopedic devices.
Deep Dive into Biomechanical Mechanisms and Technical Specifications
Unlike medications that exert their effects at a cellular or molecular level, arm braces function through biomechanical principles. Their "mechanism of action" is entirely physical and structural, designed to interact with the body's musculoskeletal system.
Mechanism of Support and Immobilization
The primary mechanisms by which an arm brace achieves its therapeutic effect include:
- Immobilization: By restricting movement at a joint or along a bone, braces prevent further damage to injured tissues (e.g., fractured bones, torn ligaments, healing surgical sites). This is achieved through rigid components (plastic, metal) molded to the limb's contours.
- Stabilization: Braces provide external stability to weakened or unstable joints, reducing the load on injured structures and promoting proper anatomical alignment. This is crucial for conditions like ligamentous laxity or post-dislocation recovery.
- Compression: Many braces incorporate compressive elements (elastic fabrics, adjustable straps) that reduce swelling (edema), improve proprioception (the body's sense of position), and provide warmth, which can aid in pain relief and tissue healing.
- Protection: A brace acts as an external shield, protecting the injured area from accidental bumps or impacts during daily activities.
- Pain Reduction: By limiting movement and providing support, braces indirectly reduce pain by preventing painful motions and decreasing muscle spasm.
- Load Reduction: Certain braces redistribute forces away from an injured area, allowing it to rest and heal without constant stress.
Device Kinetics and Biomechanical Interaction (Reinterpreting "Pharmacokinetics")
While "pharmacokinetics" (absorption, distribution, metabolism, excretion) is entirely irrelevant for a medical device, we can discuss "device kinetics" or how the brace interacts dynamically with the body and external forces.
- Application and Fit: The "distribution" of therapeutic effect depends entirely on the correct application and fit of the brace. An improperly fitted brace may not provide adequate support, could cause pressure points, nerve compression, or skin irritation.
- Material Science: The "metabolism" of a drug is its breakdown in the body. For a brace, this translates to the material's durability and how it withstands wear and tear, perspiration, and environmental factors over time. Materials like thermoplastics, neoprene, aluminum, and various fabrics are chosen for their specific properties (rigidity, flexibility, breathability, hypoallergenic nature).
- Patient Compliance: The "excretion" of a drug refers to its removal from the body. For a brace, this can be likened to patient compliance – how consistently and correctly the brace is worn and maintained. Non-compliance significantly reduces the device's therapeutic efficacy.
Table: Common Arm Brace Types and Their Primary Mechanisms
| Brace Type | Primary Mechanism(s) | Common Indications |
|---|---|---|
| Sling | Support, elevation, pain relief | Shoulder dislocations, humerus fractures, post-surgical |
| Wrist Splint | Immobilization of wrist, support | Carpal tunnel syndrome, wrist sprains/fractures, tendinitis |
| Elbow Brace | Immobilization, range-of-motion control | Epicondylitis (tennis/golfer's elbow), elbow fractures |
| Humerus Fracture Brace | Compression, alignment, stabilization | Mid-shaft humerus fractures |
| Forearm Brace | Immobilization of forearm, support | Forearm fractures, severe sprains |
| Thumb Spica Splint | Immobilization of thumb CMC joint | De Quervain's tenosynovitis, thumb fractures/sprains |
Extensive Clinical Indications and Usage Guidelines
The application of an arm brace is dictated by a wide array of orthopedic conditions, requiring careful assessment by a healthcare professional.
Detailed Indications
Arm braces are indicated for:
- Fractures:
- Humerus Fractures: Especially non-displaced or stable mid-shaft fractures.
- Forearm Fractures: Radial or ulnar shaft fractures.
- Wrist Fractures: Distal radius (Colles', Smith's fractures), scaphoid fractures.
- Hand and Finger Fractures: Metacarpal or phalangeal fractures requiring stabilization.
- Sprains and Strains:
- Wrist Sprains: Ligamentous injuries of the wrist.
- Elbow Sprains: Ligament injuries around the elbow joint.
- Thumb Sprains: Ulnar collateral ligament (UCL) injuries (skier's thumb).
- Tendinitis and Tenosynovitis:
- De Quervain's Tenosynovitis: Inflammation of thumb tendons.
- Epicondylitis (Tennis/Golfer's Elbow): Tendon inflammation at the elbow.
- Wrist Tendinitis: Inflammation of wrist tendons.
- Post-Surgical Immobilization:
- Following fracture repair, ligament reconstruction, tendon repair, or joint arthroplasty to protect the surgical site and promote healing.
- Dislocations and Subluxations:
- Post-reduction stabilization of shoulder, elbow, or wrist dislocations.
- Neurological Conditions:
- To prevent contractures or support a flaccid limb in conditions like stroke or nerve damage (e.g., wrist drop splint).
- Repetitive Strain Injuries (RSIs):
- To provide rest and support for conditions like carpal tunnel syndrome or cubital tunnel syndrome.
- Arthritis:
- To support painful or unstable joints in conditions like osteoarthritis or rheumatoid arthritis, particularly in the wrist or thumb.
Usage Guidelines and Application Protocols (Reinterpreting "Dosage Guidelines")
Proper application and adherence to wearing schedules are paramount for the efficacy of an arm brace. These are the "dosage guidelines" for a medical device.
- Prescription and Fitting:
- An arm brace should always be prescribed and fitted by a qualified healthcare professional (physician, orthopedic specialist, physical therapist, occupational therapist).
- Custom-molded braces offer superior fit and function for complex injuries.
- Wearing Schedule:
- Continuous Wear: Often required for fractures or immediately post-surgery, removing only for hygiene or specific therapy as instructed.
- Intermittent Wear: For chronic conditions, tendinitis, or during later stages of rehabilitation, wearing the brace during activities that exacerbate symptoms or for specific periods of rest.
- Nighttime Wear: Common for conditions like carpal tunnel syndrome or tendinitis to maintain a neutral position during sleep.
- Skin Care and Hygiene:
- Regularly inspect the skin under the brace for redness, irritation, pressure sores, or blisters.
- Keep the skin clean and dry. Use a mild soap and water, and ensure the skin is completely dry before re-applying the brace.
- Clean the brace according to manufacturer instructions.
- Adjustment and Maintenance:
- Straps should be snug but not excessively tight, allowing for proper circulation. Two fingers should comfortably fit under the straps.
- Regularly check for wear and tear, especially on straps, padding, and rigid components. Replace worn parts or the entire brace if integrity is compromised.
- Monitoring for Complications:
- Patients should be educated on signs of complications such as increased pain, numbness, tingling, swelling, coolness, or discoloration of the limb, which may indicate nerve compression, circulatory issues, or improper fit.
Risks, Side Effects, and Contraindications
While arm braces are generally safe and highly beneficial, their improper use or application can lead to adverse effects.
Potential Adverse Effects (Side Effects)
- Skin Irritation and Breakdown: Pressure points, friction, moisture retention, or allergic reactions to brace materials can lead to redness, rash, blisters, or even pressure ulcers.
- Nerve Compression: Overtightening or improper positioning of a brace can compress superficial nerves, leading to numbness, tingling, weakness, or pain in the distribution of the affected nerve (e.g., radial nerve palsy from a humerus brace).
- Circulatory Impairment: Excessive compression can restrict blood flow, leading to swelling, coolness, pallor, or cyanosis of the distal limb.
- Muscle Atrophy and Joint Stiffness: Prolonged immobilization, while necessary for healing, can lead to disuse atrophy of muscles and stiffness in immobilized joints. This necessitates a structured rehabilitation program post-bracing.
- Dependence: In some cases, prolonged use for non-critical conditions can lead to psychological or physical dependence, hindering the natural strengthening of supporting musculature.
- Discomfort and inconvenience: Braces can be bulky, interfere with daily activities, and cause general discomfort, potentially impacting patient compliance.
Contraindications
While specific contraindications vary by brace type and individual patient factors, general contraindications or situations requiring extreme caution include:
- Severe Open Wounds or Active Infections: A brace should not be applied directly over an open wound or infected area without proper dressing and medical supervision, as it can impede wound healing or exacerbate infection.
- Compromised Circulation: Patients with severe peripheral vascular disease, deep vein thrombosis (DVT) in the affected limb, or other circulatory impairments may be at increased risk of complications from compression.
- Severe Edema (Swelling): While some compression is beneficial, a brace applied to a severely swollen limb can worsen edema or lead to nerve/circulatory compromise. Edema should be managed first.
- Unstable Fractures Requiring Surgical Intervention: Braces are often used for stable fractures. Highly unstable or displaced fractures typically require surgical fixation before or instead of bracing.
- Allergies to Brace Materials: Rare, but patients with known allergies to neoprene, latex, or certain plastics should use alternative materials.
- Certain Neurological Conditions: In cases where a brace might exacerbate spasticity or interfere with sensory feedback critical for balance/function.
- Lack of Patient Compliance or Understanding: If a patient cannot or will not follow instructions for brace wear and care, the brace may do more harm than good.
Interactions with Other Therapies (Reinterpreting "Drug Interactions")
While "drug interactions" are not relevant, an arm brace can interact with other medical therapies:
- Physical and Occupational Therapy: Braces are often used in conjunction with therapy. The therapist will guide when to wear the brace, when to remove it for exercises, and how to gradually wean off it. Incorrect brace use can hinder therapy progress.
- Medications: A brace does not interact chemically with medications. However, its use can reduce the need for pain medications by