Surgical Navigation Systems: Revolutionizing Orthopedic and Neurosurgical Precision
In the complex landscape of modern surgery, precision is paramount. Surgical Navigation Systems (SNS), exemplified by leading platforms like Medtronic's StealthStation, represent a monumental leap forward in achieving unparalleled accuracy during intricate procedures. These advanced technologies integrate sophisticated imaging, real-time tracking, and computational power to provide surgeons with a "GPS for the body," guiding instruments and implants with extraordinary exactitude. This comprehensive guide delves into the core aspects of surgical navigation, from its underlying technology and diverse applications to its profound impact on patient outcomes.
Comprehensive Introduction & Overview
Surgical navigation systems are sophisticated computer-assisted technologies designed to enhance a surgeon's ability to operate with greater precision and confidence. By creating a virtual, interactive map of the patient's anatomy, SNS allows surgeons to track the real-time position of surgical instruments relative to critical structures, thus minimizing the risk of error and improving procedural safety.
Historically, surgeons relied on anatomical landmarks, fluoroscopy (X-ray imaging), and their extensive experience. While effective, these methods could be limited by two-dimensional views, radiation exposure, and the inherent variability of human anatomy. The advent of surgical navigation has transformed this paradigm, offering:
- Enhanced Visualization: 3D models of patient anatomy.
- Real-time Guidance: Live tracking of instruments within the 3D model.
- Improved Accuracy: Millimeter-level precision for critical maneuvers.
- Reduced Complications: Lower incidence of nerve damage, malposition, and other adverse events.
- Optimized Outcomes: Better functional recovery and implant longevity.
The StealthStation, a pioneering system from Medtronic, is a prime example of this technology, widely adopted in neurosurgery and orthopedic spine applications for its robust performance and comprehensive capabilities.
Deep-dive into Technical Specifications & Mechanisms
Understanding the power of surgical navigation requires appreciating its intricate design and operational mechanisms.
Design and Materials
A typical surgical navigation system comprises several key components, each engineered for precision and durability:
- Computer Workstation: A high-performance computer with specialized software for image processing, 3D reconstruction, planning, and real-time visualization. It features high-resolution monitors, often touch-enabled, for intuitive interaction.
- Tracking System: The heart of the navigation system, responsible for locating instruments and patient anatomy in space.
- Optical Trackers: Utilize infrared cameras to detect passive (reflective spheres) or active (LEDs) markers attached to instruments and the patient. These markers are typically made of lightweight, biocompatible plastics or metals.
- Electromagnetic Trackers: Employ a low-frequency electromagnetic field generator and miniature sensors embedded in instruments. These sensors are often made with coils of fine wire, encased in medical-grade polymers.
- Reference Arrays/Frames: Rigid structures attached to the patient (e.g., via a small pin in bone or a clamp) that carry tracking markers. These are generally made from surgical-grade aluminum or composite materials to be lightweight and radiolucent (transparent to X-rays).
- Navigated Instruments: Standard surgical instruments (drills, probes, osteotomes, reamers) fitted with tracking markers. These instruments maintain their conventional materials (e.g., stainless steel, titanium) but are adapted for navigation.
- Image Acquisition Systems: Interfaces with various imaging modalities such as CT, MRI, C-arm fluoroscopy, and intraoperative O-arm/CT scanners.
Mechanism of Action: How it Works
The operational principle of surgical navigation is a sophisticated interplay of imaging, registration, and tracking:
- Preoperative Imaging: The process begins with acquiring high-resolution 2D images (e.g., CT, MRI) of the patient's anatomy. These images provide the detailed anatomical data necessary for surgical planning.
- 3D Reconstruction & Planning: The system's software processes these 2D images to create a precise 3D virtual model of the target anatomy. The surgeon uses this model to plan the optimal surgical approach, define trajectories, select implant sizes, and identify critical structures (nerves, vessels).
- Patient Registration: This crucial step links the virtual 3D model with the actual patient on the operating table. It involves:
- Attaching Reference Arrays: A reference array with tracking markers is rigidly attached to the patient, typically to a stable bone structure near the surgical site.
- Matching Landmarks: The surgeon uses a navigated probe to touch a series of identifiable anatomical points on the patient. The system simultaneously matches these physical points to their corresponding locations on the 3D virtual model. This establishes a precise spatial relationship between the patient and the computer model.
- Surface Matching (Optional): In some systems, a navigated probe can be used to "paint" the surface of the anatomy, generating a point cloud that the software matches to the 3D model.
- Real-time Tracking & Guidance: Once registered, any surgical instrument equipped with tracking markers can be accurately localized in real-time within the 3D anatomical model displayed on the monitor. As the surgeon moves the instrument, its position and orientation are continuously updated, providing dynamic visual feedback. This allows the surgeon to see the instrument's tip relative to planned trajectories, tumors, nerves, and other vital structures.
- Verification: Throughout the procedure, the surgeon can verify instrument position, implant placement, and trajectory accuracy, making adjustments as needed.
Key Technologies
- Image Fusion: The ability to combine data from different imaging modalities (e.g., CT for bone detail, MRI for soft tissue) to create a more comprehensive anatomical view.
- 3D Reconstruction Algorithms: Advanced software that converts 2D slice data into highly accurate, manipulable 3D models.
- Haptic Feedback (Emerging): Some advanced systems incorporate haptic feedback, providing tactile resistance or vibration to the surgeon when an instrument approaches a predefined "no-go zone."
- Augmented Reality (AR): Future iterations may overlay the virtual 3D model directly onto the patient's body in the surgeon's field of view, further enhancing real-time guidance.
Extensive Clinical Indications & Usage
Surgical navigation systems have a wide array of clinical applications, significantly impacting the precision and safety of numerous complex procedures across orthopedic and neurosurgical disciplines.
Detailed Surgical or Clinical Applications
- Spine Surgery:
- Pedicle Screw Placement: The most common application. Navigation ensures accurate placement of pedicle screws in the thoracic, lumbar, and sacral spine, minimizing the risk of neurological injury, vascular damage, or screw malposition that could lead to construct failure. This is particularly crucial in patients with challenging anatomy (e.g., severe scoliosis, previous surgery, spinal tumors).
- Scoliosis Correction: Precise planning and execution of vertebral derotation and instrumentation.
- Spinal Tumor Resection: Defining tumor margins and safe resection pathways while preserving critical neural structures.
- Fusion Procedures: Optimizing cage placement and bone graft integration.
- Neurosurgery:
- Brain Tumor Resection: Precisely locating tumors, defining resection margins, and navigating around eloquent (functionally critical) brain regions.
- Deep Brain Stimulation (DBS): Highly accurate placement of electrodes for treating Parkinson's disease, essential tremor, and dystonia.
- Cranial Navigation for Biopsies: Guiding biopsy needles to target lesions with minimal invasiveness.
- Ventricular Shunting: Precise placement of catheters for hydrocephalus treatment.
- Skull Base Surgery: Navigating complex anatomy with critical nerves and vessels.
- Orthopedic Trauma:
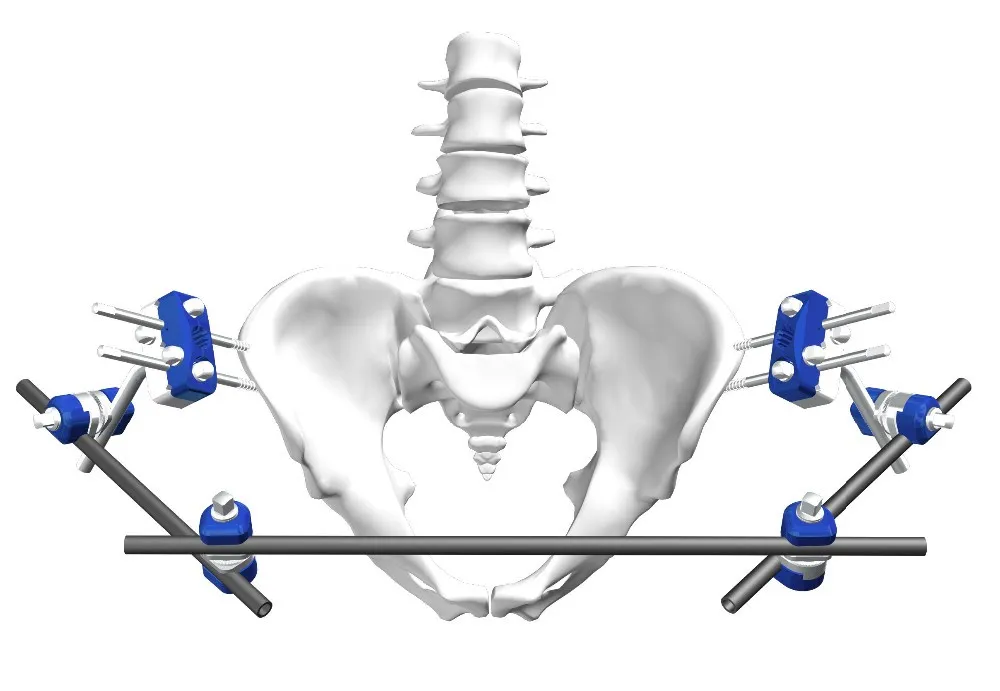
- Complex Fracture Fixation: Especially for fractures of the pelvis, acetabulum, and long bones, where precise reduction and screw placement are vital for restoring function and preventing malunion.
- Minimally Invasive Approaches: Facilitating accurate screw or plate placement through smaller incisions, reducing soft tissue damage.
- Joint Replacement Surgery:
- Total Knee Arthroplasty (TKA): Achieving optimal component alignment, precise bone cuts, and balancing ligaments to improve knee kinematics, reduce wear, and enhance long-term implant survival.
- Total Hip Arthroplasty (THA): Ensuring correct acetabular cup orientation, leg length restoration, and offset reconstruction to prevent dislocation, impingement, and improve biomechanics.
- ENT/Maxillofacial Surgery:
- Endoscopic Sinus Surgery: Navigating complex sinus anatomy to remove polyps or clear blockages while avoiding critical structures like the orbit and skull base.
- Skull Base Procedures: Assisting in tumor removal and reconstruction.
Fitting/Usage Instructions (General Workflow)
The surgical navigation workflow is standardized but requires meticulous attention to detail:
- Preoperative Planning:
- Upload patient's CT/MRI scans to the navigation workstation.
- Surgeon identifies anatomical landmarks, defines target points, and plans instrument trajectories on the 3D model.
- Selects appropriate implant sizes and positions.
- Patient Setup:
- Patient is positioned on the operating table.
- A reference array is rigidly fixed to the patient's anatomy, typically to a stable bone structure (e.g., iliac crest for spine, femur for hip, cranium for neurosurgery).
- The optical camera (or electromagnetic field generator) is positioned to have an unobstructed view of the reference array and the surgical field.
- Registration:
- The surgeon uses a navigated probe to touch predefined anatomical points on the patient, matching them to the corresponding points on the 3D virtual model.
- The system confirms successful registration and displays the accuracy.
- Intraoperative Navigation:
- As the surgeon uses navigated instruments, their real-time position and trajectory are displayed on the monitor, providing continuous visual guidance.
- The surgeon can verify instrument depth, angle, and proximity to critical structures.
- Post-Procedure Verification:
- Some systems allow for intraoperative imaging (e.g., O-arm scan) to verify implant placement and make immediate adjustments if necessary.
Biomechanics and Patient Outcome Improvements
Surgical navigation significantly impacts biomechanics and patient outcomes by ensuring optimal anatomical reconstruction and implant placement.
Biomechanics
- Improved Load Distribution: In joint replacements, precise alignment of prosthetic components ensures even load distribution across the joint surfaces, reducing stress concentrations and minimizing polyethylene wear, thereby extending implant longevity.
- Enhanced Stability: Accurate pedicle screw placement in spine surgery creates a more stable construct, reducing the risk of screw loosening, pull-out, and pseudoarthrosis, ultimately promoting successful fusion.
- Restored Kinematics: In knee arthroplasty, navigation helps restore the natural kinematics of the knee joint by achieving precise limb alignment and ligamentous balance.
- Reduced Soft Tissue Disruption: By enabling more targeted access and minimally invasive approaches, navigation can reduce muscle damage, preserve surrounding soft tissues, and potentially lead to faster recovery.
Patient Outcome Improvements
- Reduced Complication Rates: Significantly lowers the incidence of nerve damage, vascular injury, malposition of implants, and revision surgeries.
- Faster Recovery: Minimally invasive approaches facilitated by navigation can lead to less postoperative pain, reduced blood loss, and quicker mobilization.
- Improved Functional Outcomes: Patients often experience better range of motion, reduced pain, and enhanced overall function due to precise anatomical restoration and implant positioning.
- Enhanced Implant Longevity: Optimal alignment and load distribution translate to reduced wear and tear on implants, extending their functional lifespan.
- Decreased Radiation Exposure: For procedures traditionally relying heavily on fluoroscopy, navigation can reduce intraoperative radiation exposure for both the patient and surgical staff.
Risks, Side Effects, or Contraindications
While highly beneficial, surgical navigation systems are not without potential considerations and limitations.
Risks
- Registration Errors: Inaccurate registration between the patient and the virtual model can lead to erroneous navigation guidance. This can be caused by patient movement, instability of the reference array, or errors during landmark identification. Rigorous verification steps are crucial to mitigate this.
- System Malfunction: Like any complex electronic device, the system can experience software glitches, hardware failures (e.g., camera issues, tracker malfunction), or power interruptions. Redundancy checks and immediate troubleshooting are essential.
- Increased Setup Time: Especially during the initial learning curve, setting up and registering the navigation system can add time to the overall surgical procedure. With experience, this time typically decreases.
- Cost Implications: The initial investment in a surgical navigation system, as well as ongoing maintenance and disposable tracker costs, can be substantial for healthcare facilities.
- Over-reliance: There is a potential risk of surgeons, particularly less experienced ones, becoming overly reliant on the navigation system and neglecting their fundamental anatomical knowledge and surgical feel. The system is a tool to augment, not replace, surgical skill.
- Line-of-Sight Obstruction (Optical Systems): For optical systems, maintaining an unobstructed line of sight between the cameras and the tracking markers is critical. Draping, instruments, or staff can inadvertently block this view, temporarily interrupting navigation.
Side Effects (Indirect)
Surgical navigation systems themselves do not cause direct "side effects." However, the goal of navigation is to reduce the side effects or complications associated with the surgical procedure itself. For example, by preventing nerve injury, it mitigates potential postoperative numbness or weakness.
Contraindications
There are very few absolute contraindications to the use of the navigation system itself. Most contraindications relate to the underlying surgical procedure, not the navigation technology.
- Inability to Remain Still: For procedures requiring rigid registration, a patient who cannot remain still or whose anatomy cannot be adequately stabilized might pose a challenge for accurate navigation.
- Severely Distorted Anatomy: In rare cases of extreme anatomical distortion (e.g., massive tumors, severe congenital deformities), the ability to accurately register the patient to the imaging data might be compromised.
- Lack of Appropriate Imaging: Inadequate or poor-quality preoperative imaging data will hinder the system's ability to create an accurate 3D model.
Maintenance & Sterilization Protocols
Ensuring the longevity, accuracy, and sterility of surgical navigation systems is paramount for patient safety and operational efficiency.
Maintenance Protocols
- Software Updates: Regular software updates provided by the manufacturer are critical for improving performance, adding new features, and addressing bugs.
- Hardware Calibration: Optical cameras, electromagnetic field generators, and navigated instruments require periodic calibration checks according to manufacturer guidelines to ensure ongoing accuracy. This is often performed by certified service technicians.
- Preventative Maintenance (PM): Scheduled PM visits by manufacturer-trained technicians are essential to inspect components, perform diagnostics, and replace wear-and-tear parts.
- Environmental Control: The workstation and tracking units should be operated within specified temperature and humidity ranges to prevent damage to sensitive electronics.
- Cable Management: Proper handling and organization of cables prevent damage and ensure reliable connections.
- System Checks: Routine power-on self-tests and functionality checks before each use can identify minor issues proactively.
Sterilization Protocols
Strict adherence to manufacturer's Instructions for Use (IFU) is non-negotiable for all components coming into contact with the sterile field.
- Reusable Trackers/Reference Arrays: These components, if designed for reuse, typically undergo steam sterilization (autoclave). They must be thoroughly cleaned to remove all bioburden before sterilization. Specific temperature, pressure, and cycle times must be followed.
- Navigated Instruments: Similar to other surgical instruments, reusable navigated instruments are cleaned and then sterilized, most commonly via steam sterilization. Some delicate instruments might require low-temperature sterilization methods (e.g., ethylene oxide, hydrogen peroxide gas plasma).
- Disposable Components: Many tracking markers, instrument tips, or reference pins are designed for single-use and come in sterile packaging. They are discarded after one use.
- System Console/Monitors: The main computer workstation and monitors are considered non-critical devices. Their surfaces are disinfected with hospital-approved germicidal wipes or sprays, ensuring the agents are compatible with the device materials to prevent damage. Draping may be used to maintain sterility during the procedure.
- Camera/Field Generator: These components are typically covered with sterile drapes or barriers during surgery to prevent contamination. Their external surfaces are disinfected.
Frequently Asked Questions (FAQ)
Q1: What is a Surgical Navigation System?
A1: A Surgical Navigation System is a computer-assisted technology that provides surgeons with real-time, 3D guidance during operations. It uses imaging data and tracking technology to show the exact position of surgical instruments relative to the patient's anatomy, much like a GPS system for the body.
Q2: How does a system like StealthStation work?
A2: StealthStation works by integrating preoperative imaging (CT, MRI) to create a 3D model of the patient's anatomy. During surgery, small tracking markers are attached to the patient and surgical instruments. An optical camera system (or electromagnetic field) tracks these markers, displaying the instrument's real-time position on the 3D model, guiding the surgeon with high precision.
Q3: What types of surgeries commonly use surgical navigation?
A3: Surgical navigation is widely used in complex orthopedic spine surgery (e.g., pedicle screw placement, scoliosis correction), neurosurgery (e.g., brain tumor resection, deep brain stimulation), orthopedic trauma (e.g., pelvic fracture fixation), and joint replacement (e.g., total knee and hip arthroplasty).
Q4: Is surgical navigation safer than traditional surgery?
A4: Yes, generally. By providing enhanced visualization and real-time guidance, surgical navigation significantly reduces the risk of errors such as nerve damage, vascular injury, or implant malposition, thereby improving patient safety and reducing complication rates compared to traditional methods that rely solely on fluoroscopy and anatomical landmarks.
Q5: Does surgical navigation reduce recovery time?
A5: While it doesn't directly reduce recovery time for all procedures, by enabling more precise, and often minimally invasive, approaches, navigation can lead to less tissue damage, reduced blood loss, and fewer complications. This can indirectly contribute to less postoperative pain and a faster, smoother recovery for many patients.
Q6: Are there any risks associated with using surgical navigation?
A6: Potential risks include registration errors (if the system isn't accurately matched to the patient), system malfunction, or increased initial setup time. However, these risks are mitigated by rigorous protocols, surgeon training, and system redundancy, and are generally far outweighed by the benefits of enhanced precision.
Q7: How accurate is surgical navigation?
A7: Surgical navigation systems are designed to provide sub-millimeter accuracy, often in the range of 1-2 millimeters or even less, depending on the system and application. This level of precision is critical for procedures involving delicate structures like the brain or spinal cord.
Q8: Does surgical navigation replace the surgeon's skill?
A8: Absolutely not. Surgical navigation is a sophisticated tool that augments the surgeon's skill, knowledge, and experience. It provides enhanced information and guidance, allowing the surgeon to perform complex tasks with greater confidence and precision, but the surgeon remains in complete control and is responsible for all surgical decisions.
Q9: What is the difference between optical and electromagnetic navigation?
A9: Optical navigation uses infrared cameras to track reflective or active markers on instruments and the patient, requiring a clear line of sight. Electromagnetic navigation uses a magnetic field generator and small sensors embedded in instruments, which can track through tissue and don't require line of sight, but can be susceptible to interference from metal objects.
Q10: How are surgical navigation systems and their instruments maintained and sterilized?
A10: The system's console and monitors are disinfected with medical-grade wipes. Reusable components like trackers and instruments are thoroughly cleaned and then sterilized, typically using steam sterilization (autoclave), following strict manufacturer guidelines to ensure patient safety and device longevity. Regular software updates and hardware calibration are also performed by trained technicians.
Q11: Is surgical navigation covered by insurance?
A11: The use of surgical navigation is generally part of the overall surgical procedure and is typically covered by insurance when the underlying surgery is deemed medically necessary. Patients should always confirm coverage specifics with their insurance provider.
Q12: What is the future of surgical navigation technology?
A12: The future of surgical navigation is exciting, with developments in augmented reality (AR) to overlay 3D models directly onto the patient, artificial intelligence (AI) for enhanced planning and real-time feedback, integration with robotics for automated tasks, and miniaturization of tracking components for even less invasive procedures.