Robotic-Arm Assisted Arthroplasty System (e.g., Mako): A Comprehensive Patient Guide
1. Comprehensive Introduction & Overview
Welcome to an in-depth exploration of Robotic-Arm Assisted Arthroplasty, a groundbreaking advancement in orthopedic surgery that is transforming joint replacement procedures. At the forefront of this technology is the Mako System, a sophisticated platform designed to enhance precision and personalization in hip and knee replacement surgeries. For patients suffering from debilitating joint pain due to conditions like osteoarthritis, this innovative approach offers a path to improved quality of life with potentially better outcomes.
Traditional joint replacement surgery relies heavily on the surgeon's skill and experience, which remain paramount. However, robotic-arm assisted systems like Mako augment the surgeon's capabilities by providing a detailed, patient-specific 3D surgical plan and real-time guidance during the procedure. This integration of human expertise with advanced technology aims to achieve unparalleled accuracy in implant positioning and alignment, which are critical factors for the longevity and function of a new joint.
This guide will delve into the intricacies of robotic-arm assisted arthroplasty, covering its technical foundations, clinical applications, patient benefits, and what you can expect if you are considering this advanced treatment option. Our goal is to provide you with clear, comprehensive, and authoritative information to help you make informed decisions about your orthopedic health.
2. Deep-dive into Technical Specifications & Mechanisms
The Mako System represents a pinnacle of surgical engineering, combining cutting-edge robotics with sophisticated imaging and software. Understanding its technical components and how they work together provides insight into the precision it brings to the operating room.
Design & Materials of the Mako System
The Mako System is not an autonomous robot performing surgery alone; rather, it is a surgeon-controlled robotic arm. Its core components include:
- Robotic Arm: A highly articulated, stable arm equipped with specialized surgical instruments (e.g., burrs, saws). The arm itself is constructed from durable, medical-grade metals and composites, designed for stability, precision, and sterile compatibility.
- Computer Workstation: This is the brain of the system, featuring high-resolution monitors and powerful processors. It runs proprietary software that processes CT scan data to create a 3D model of the patient's joint.
- Optical Trackers (Navigation System): Small, reflective spheres attached to the patient's bone and surgical instruments. Infrared cameras track these spheres in real-time, providing continuous feedback on the exact position and orientation of the anatomy and instruments to the computer workstation.
- Haptic Feedback Technology: This is a crucial safety feature. The robotic arm provides tactile resistance (haptic feedback) to the surgeon if they attempt to move outside the pre-defined surgical boundaries. This "virtual boundary" ensures that bone resections are performed exactly as planned, preventing over-resection or damage to healthy tissue.
Pre-operative Planning: The Blueprint for Precision
Before surgery, a patient undergoes a CT (Computed Tomography) scan of the affected joint. This scan generates highly detailed cross-sectional images, which the Mako software then uses to create a precise 3D virtual model of the individual's anatomy.
- Personalized 3D Model: This model allows your surgeon to virtually assess the bone structure, joint alignment, and soft tissue balance unique to your body.
- Virtual Implant Placement: The surgeon uses this 3D model to select the optimal implant size, type, and position, simulating various scenarios to achieve the best fit and function. This personalized planning phase is critical for addressing individual anatomical variations.
- Bone Cut Planning: Precise bone resections are planned in the virtual environment, determining the exact angles and depths required for optimal implant seating and joint kinematics.
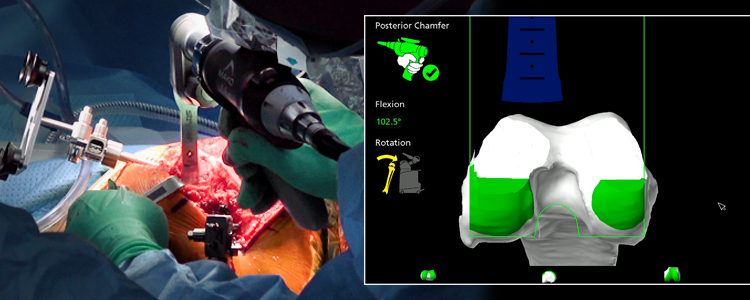
Intra-operative Guidance: Real-Time Accuracy
During the surgery, the pre-operative plan is brought to life:
- Anatomical Registration: The surgeon registers the patient's actual anatomy with the 3D virtual plan using the optical trackers. This ensures the virtual model accurately reflects the patient's position on the operating table.
- Real-time Adjustments & Soft Tissue Balancing: The system provides real-time data on joint kinematics and soft tissue tension throughout the range of motion. This allows the surgeon to make dynamic adjustments to the plan, if necessary, to achieve optimal soft tissue balance, which is vital for post-operative stability and function.
- Robotic-Arm Assisted Resection: The surgeon guides the robotic arm to perform the planned bone resections. The haptic feedback system ensures that the surgeon stays within the pre-defined boundaries, preventing inadvertent damage to surrounding healthy bone or ligaments. This controlled environment significantly enhances the accuracy of bone preparation compared to manual techniques.
Biomechanics: Optimizing Joint Function
The precision afforded by robotic-arm assisted arthroplasty has significant biomechanical implications:
- Improved Implant Positioning: Accurate placement of implants ensures proper load distribution across the joint surfaces, reducing stress concentrations and potentially extending implant lifespan.
- Restored Kinematics: By precisely recreating the patient's natural joint alignment and soft tissue balance, the robotic system helps restore the natural motion and stability of the joint, leading to a more natural feel and improved function post-surgery.
- Enhanced Soft Tissue Balance: Achieving optimal soft tissue tension is crucial for preventing instability or stiffness. The real-time feedback from the Mako system allows surgeons to finely tune this balance, contributing to better post-operative outcomes.
Maintenance & Sterilization Protocols
While not directly handled by the patient, it's reassuring to know that the Mako system and its instruments adhere to rigorous standards:
- Instrument Sterilization: All surgical instruments used with the Mako system are thoroughly cleaned and sterilized according to strict hospital protocols, just like instruments used in traditional surgery.
- System Maintenance: The Mako robotic system itself undergoes regular preventative maintenance and calibration by certified technicians to ensure its accuracy, functionality, and safety. This includes software updates and hardware checks to maintain peak performance.
3. Extensive Clinical Indications & Usage
Robotic-arm assisted arthroplasty is indicated for specific types of joint replacement, primarily focusing on the hip and knee.
Clinical Applications
The Mako System is currently approved and widely used for:
- Total Knee Arthroplasty (TKA): For patients with severe osteoarthritis or other forms of degenerative knee disease affecting all compartments of the knee.
- Partial Knee Arthroplasty (PKA): Also known as unicompartmental knee replacement, this is for patients with osteoarthritis confined to only one compartment of the knee (medial, lateral, or patellofemoral). Mako's precision is particularly beneficial here, allowing for preservation of healthy bone and ligaments.
- Total Hip Arthroplasty (THA): For patients with severe osteoarthritis, avascular necrosis, or other conditions leading to significant hip pain and disability. The robotic arm assists in precise acetabular (hip socket) reaming and cup placement, as well as femoral component positioning.
Patient Selection Criteria
While Mako offers significant advantages, not every patient is a candidate. Your surgeon will evaluate several factors, including:
- Diagnosis: Primarily patients with moderate to severe degenerative joint disease (osteoarthritis), rheumatoid arthritis, or post-traumatic arthritis.
- Functional Impairment: Significant pain, stiffness, and loss of function that interferes with daily activities and has not responded to conservative treatments (e.g., medication, physical therapy, injections).
- Bone Quality: Sufficient bone stock to support the implants.
- Overall Health: Patients must be medically fit to undergo major surgery and anesthesia.
- Specific Anatomy: In some rare cases of extreme deformity or previous surgery, the system might be less suitable.
Surgical Workflow Overview
The Mako surgical procedure typically follows these steps:
- Pre-operative CT Scan: As described, a detailed CT scan is performed to create the 3D model.
- Surgical Planning: Your surgeon meticulously plans the implant size, placement, and bone resections using the 3D model on the Mako workstation.
- Anesthesia: You will receive appropriate anesthesia (general or regional) as determined by your surgical team.
- Incision: A standard surgical incision is made to access the joint.
- Anatomical Registration: Small trackers are temporarily affixed to your bone, and the surgeon uses the Mako system to register your actual joint anatomy with the pre-operative 3D plan.
- Bone Preparation: The surgeon guides the robotic arm to prepare the bone surfaces. The robotic arm's haptic feedback ensures that cuts are made precisely within the planned boundaries.
- Trial Implants (Optional): In some cases, trial implants may be used to verify fit and soft tissue balance.
- Permanent Implant Placement: The actual prosthetic components are then securely implanted.
- Wound Closure: The incision is closed, and you are moved to recovery.
Patient Outcome Improvements
Studies and clinical experience suggest several potential benefits of robotic-arm assisted arthroplasty:
- Increased Accuracy & Precision: Consistently achieving accurate implant positioning and alignment, which is crucial for long-term implant survival and joint function.
- Reduced Pain & Faster Recovery: While recovery is still a journey, some patients report less post-operative pain and a quicker return to activities due to less soft tissue disruption and more precise bone cuts.
- Improved Joint Function: Better restoration of the natural mechanics of the joint can lead to a more natural feeling knee or hip and improved range of motion.
- Potential for Longer Implant Lifespan: Optimal implant positioning can reduce wear and tear on the prosthetic components, potentially delaying the need for revision surgery.
- Preservation of Healthy Tissue: Especially in partial knee replacements, the precision allows for minimal resection of healthy bone and ligaments.
- Reduced Risk of Complications: Precision can reduce the risk of issues like leg length discrepancies in hip replacement or malalignment.
4. Risks, Side Effects, or Contraindications
While robotic-arm assisted arthroplasty offers significant advantages, it is still a major surgical procedure with inherent risks. It's crucial to discuss these thoroughly with Dr. Mohammed Hutaif.
General Surgical Risks (Applicable to all joint replacements):
- Infection: Despite sterile techniques, infection is a rare but serious complication.
- Blood Clots: Deep vein thrombosis (DVT) or pulmonary embolism (PE) can occur. Prophylactic measures are taken to minimize this risk.
- Nerve or Blood Vessel Damage: Although rare, damage to surrounding nerves or blood vessels can occur during surgery.
- Anesthesia Risks: Allergic reactions or other complications related to anesthesia.
- Stiffness or Instability: The new joint may become stiff or feel unstable.
- Implant Loosening or Wear: Over time, implants can loosen or the bearing surfaces can wear out, potentially requiring revision surgery.
- Leg Length Discrepancy (Hip): While Mako aims to minimize this, slight differences can still occur.
Specific Risks Associated with Robotic-Arm Assisted Arthroplasty:
- Radiation Exposure: The pre-operative CT scan involves a small amount of radiation exposure. Your doctor will weigh the benefits against this risk.
- Potential for System Malfunction: While rare, any technological system can experience issues. Hospitals have protocols in place for such events, and the surgeon always maintains control.
- Pin Site Complications: The small pins used to attach optical trackers to the bone can rarely become infected or cause minor discomfort.
- Learning Curve: Surgeons require specialized training and experience with the Mako system. Ensure your surgeon is highly experienced with this technology.
Contraindications:
Conditions that may make you unsuitable for robotic-arm assisted arthroplasty include:
- Active Infection: Any active infection in the joint or elsewhere in the body must be treated before surgery.
- Severe Peripheral Vascular Disease: Impaired blood flow can hinder healing.
- Neuromuscular Deficits: Conditions that severely impair muscle function or sensation.
- Skeletal Immaturity: Not performed on growing bones.
- Insufficient Bone Stock: Inability to securely implant the components.
- Severe Obesity: Can increase surgical risks and may affect implant longevity.
- Unrealistic Patient Expectations: It's important for patients to understand the limitations and expected outcomes.
- Allergy to Implant Materials: Rare, but must be identified.
5. Expert Tips from Dr. Mohammed Hutaif
"As an orthopedic specialist, I am committed to providing my patients with the most advanced and effective treatments available. Robotic-arm assisted arthroplasty, particularly systems like Mako, represents a significant leap forward in joint replacement surgery. However, it's crucial to understand that this technology is a sophisticated tool that assists the surgeon; it does not replace their expertise, judgment, or surgical skill.
Here are my expert tips for patients considering this procedure:
- Choose Your Surgeon Wisely: The robotic system enhances precision, but the ultimate success of your surgery still depends on the surgeon's experience, training, and understanding of joint biomechanics. Ensure your surgeon is highly proficient and experienced with robotic-arm assisted techniques.
- Understand the Personalization: Embrace the fact that this technology allows for a truly personalized surgical plan tailored to your unique anatomy. This isn't a 'one-size-fits-all' approach; it's designed specifically for you.
- Active Participation in Recovery is Key: While precision during surgery can contribute to a smoother recovery, your commitment to post-operative physical therapy and rehabilitation is paramount. Follow your rehabilitation program diligently to maximize your functional outcome.
- Manage Expectations Realistically: Robotic surgery aims for excellent outcomes, but it's important to have realistic expectations. Joint replacement surgery can significantly reduce pain and improve function, but it may not restore your joint to its pre-arthritic state, nor will it allow you to engage in high-impact activities typically. Discuss your goals with me openly.
- Ask Questions! Don't hesitate to ask me or my team any questions you have about the procedure, the technology, recovery, or potential risks. An informed patient is an empowered patient.
- Focus on Pre-operative Health: Optimizing your health before surgery (e.g., managing diabetes, quitting smoking, maintaining a healthy weight) can significantly improve your surgical outcome and recovery."
6. Massive FAQ Section
Q1: What is Robotic-Arm Assisted Arthroplasty (e.g., Mako)?
A1: Robotic-Arm Assisted Arthroplasty, exemplified by the Mako system, is an advanced surgical technique for joint replacement (hip and knee). It uses a robotic arm, guided by the surgeon, to enhance precision during bone preparation and implant placement. It integrates pre-operative 3D planning based on your unique anatomy with real-time intra-operative feedback.
Q2: How is Mako different from traditional joint replacement surgery?
A2: The primary difference lies in the level of precision and personalization. Traditional surgery relies on manual instruments and the surgeon's visual and tactile assessment. Mako uses a pre-operative CT scan to create a personalized 3D plan, and then, during surgery, the robotic arm provides haptic (tactile) feedback to the surgeon, ensuring bone cuts and implant positioning are executed exactly as planned, within fractions of a millimeter. This can lead to more accurate alignment and soft tissue balance.
Q3: Is the Mako robot performing the surgery independently?
A3: No, absolutely not. The Mako system is a surgeon-controlled robotic arm. The surgeon is always in control, guiding the robotic arm. The system acts as a sophisticated tool that provides real-time data, visual guidance, and haptic feedback (a virtual boundary) to assist the surgeon in executing the surgical plan with extreme precision. It enhances the surgeon's capabilities, it does not replace them.
Q4: What are the main benefits of Mako robotic-arm assisted surgery?
A4: Potential benefits include:
* Enhanced Precision: More accurate implant positioning and alignment.
* Personalized Plan: A surgical plan tailored to your unique anatomy.
* Improved Outcomes: Potentially less post-operative pain, faster recovery, and improved joint function.
* Increased Implant Longevity: Optimal implant placement may reduce wear and tear.
* Preservation of Healthy Tissue: More precise bone removal means less disruption to surrounding healthy structures.
Q5: What joints can be treated with the Mako system?
A5: Currently, the Mako system is used for Total Knee Arthroplasty (TKA), Partial Knee Arthroplasty (PKA), and Total Hip Arthroplasty (THA).
Q6: What is the recovery process like after Mako surgery?
A6: The recovery process is similar to traditional joint replacement surgery, involving initial pain management, early mobilization, and a structured physical therapy program. While some patients report less initial pain and a potentially faster return to certain activities due to the precision of the surgery, consistent adherence to your rehabilitation plan is crucial for optimal long-term results.
Q7: Are there any specific risks associated with Mako robotic surgery?
A7: In addition to general surgical risks (infection, blood clots, nerve damage), Mako specific considerations include: a small amount of radiation exposure from the pre-operative CT scan, rare potential for system malfunction (though protocols are in place), and complications at pin sites used for tracking. These risks are generally low and are discussed in detail by your surgeon.
Q8: Will my insurance cover Mako robotic-arm assisted arthroplasty?
A8: Most insurance providers recognize robotic-arm assisted arthroplasty as a standard and often preferred method for joint replacement. However, coverage can vary depending on your specific insurance plan and policy. It's always advisable to contact your insurance provider directly and consult with our office staff to understand your coverage details.
Q9: Am I a candidate for Mako robotic-arm assisted surgery?
A9: Candidacy depends on various factors, including the severity of your joint condition (typically moderate to severe osteoarthritis), your overall health, bone quality, and functional limitations. Dr. Mohammed Hutaif will conduct a thorough evaluation, including physical examination and imaging, to determine if this advanced procedure is the best option for you.
Q10: Does Mako surgery leave a larger scar?
A10: The incision size for Mako robotic-arm assisted surgery is generally comparable to traditional joint replacement procedures. While the system provides high precision internally, the external incision is primarily determined by the need to access the joint for implant placement. Scarring is a natural part of any surgery and varies by individual.
Q11: Is robotic-arm assisted surgery safer than traditional surgery?
A11: Both traditional and robotic-arm assisted surgeries are safe procedures when performed by experienced surgeons. The "safety" aspect of Mako comes from its enhanced precision, which can potentially reduce complications related to malalignment or improper implant positioning. The haptic feedback mechanism also adds a layer of safety by preventing the surgeon from cutting outside the planned boundaries. It's about optimizing safety through precision.
Q12: How long does the Mako procedure take compared to traditional surgery?
A12: The surgical time for Mako robotic-arm assisted arthroplasty can be comparable to or sometimes slightly longer than traditional surgery, especially during the initial learning curve for the surgical team. This is due to the additional steps involved in pre-operative planning, anatomical registration, and using the robotic arm. However, the benefits of precision often outweigh any minor increase in operative time.
Conclusion
Robotic-arm assisted arthroplasty, with the Mako System leading the way, represents a significant evolution in orthopedic care. By synergizing the unparalleled skill of a human surgeon with the precision and data-driven insights of advanced robotics, this technology offers a highly personalized and accurate approach to joint replacement. For patients suffering from debilitating hip and knee conditions, it holds the promise of reduced pain, improved function, and a faster return to the activities they love. As with any medical decision, a thorough discussion with Dr. Mohammed Hutaif is essential to determine if this innovative treatment is the right choice for your individual needs.