Understanding the Reverse Total Shoulder Prosthesis: A Comprehensive Guide
The shoulder joint is a marvel of human engineering, offering an unparalleled range of motion. However, it is also susceptible to debilitating conditions, especially those affecting the rotator cuff. For severe cases, particularly when the rotator cuff is irreparably damaged, a revolutionary surgical solution known as the Reverse Total Shoulder Prosthesis (RTSP) has transformed patient outcomes. This extensive guide, crafted by an expert Medical SEO Copywriter and Orthopedic Specialist, aims to provide patients with an authoritative, comprehensive, yet easy-to-understand overview of this advanced orthopedic procedure.
1. Comprehensive Introduction & Overview
What is a Reverse Total Shoulder Prosthesis?
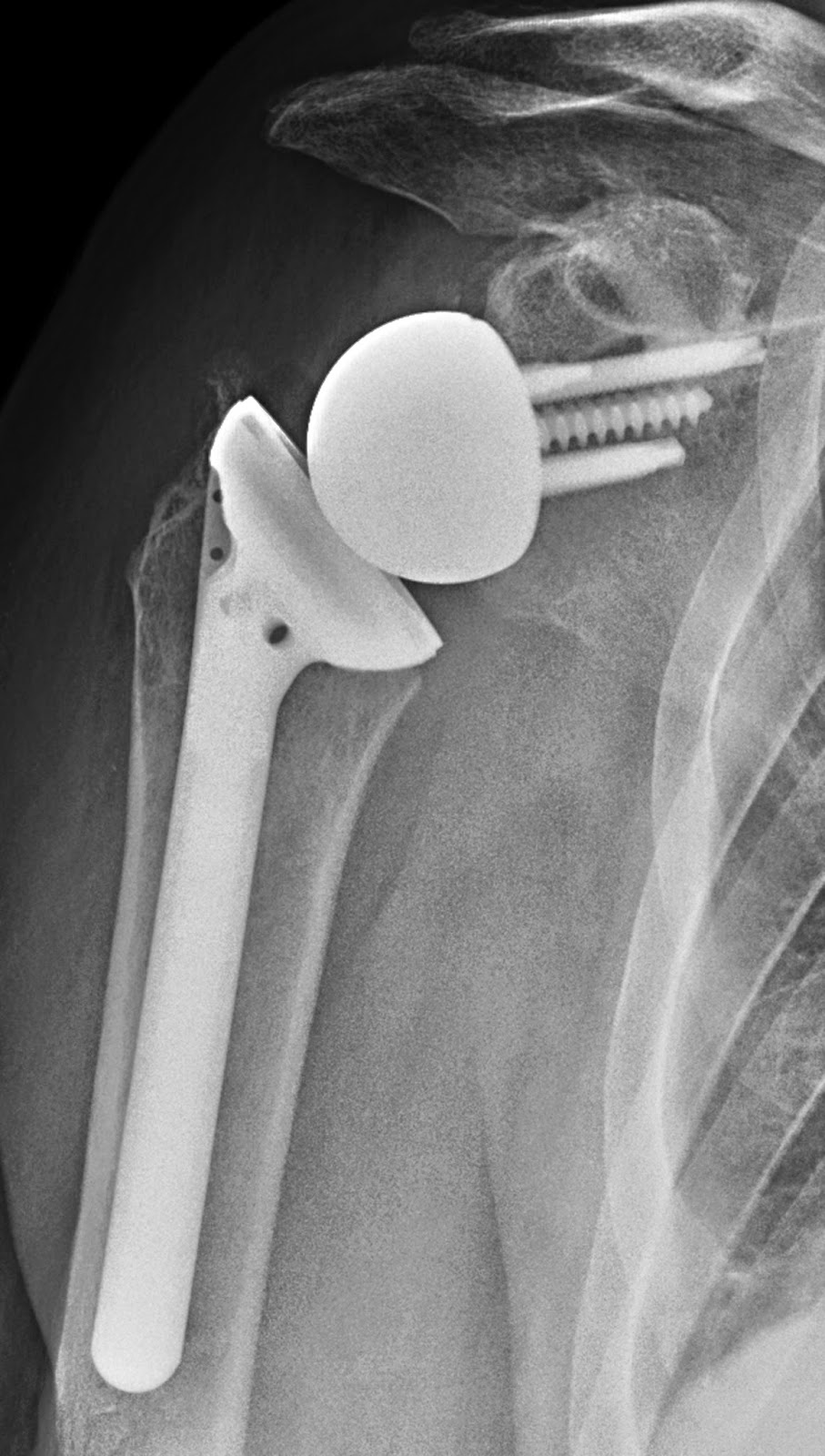
A Reverse Total Shoulder Prosthesis (RTSP), often referred to as a reverse shoulder replacement, is a specialized type of shoulder arthroplasty (joint replacement surgery). Unlike a conventional total shoulder replacement where the natural anatomy is mimicked (ball on the humerus, socket on the scapula), the RTSP literally reverses this configuration. In a reverse replacement, a metal ball (glenosphere) is fixed to the shoulder blade (scapula), and a plastic socket (humeral cup) is attached to the upper arm bone (humerus).
Why "Reverse"? The Biomechanical Shift
This "reversal" is not arbitrary; it's a brilliant biomechanical solution designed to address specific problems. The primary reason for this design is to allow the deltoid muscle – the large muscle covering the shoulder – to take over the function of a damaged or non-existent rotator cuff. By moving the center of rotation of the shoulder joint medially and distally, the deltoid muscle gains a mechanical advantage, enabling patients to lift their arm even without a functional rotator cuff.
Who Benefits from RTSP?
The RTSP is typically recommended for patients suffering from conditions where the rotator cuff is severely damaged and unable to function, often accompanied by arthritis. It has significantly improved the quality of life for countless individuals who previously had limited options for pain relief and functional restoration.
2. Deep-Dive into Technical Specifications / Mechanisms
Design and Materials: The Components of an RTSP
An RTSP is a sophisticated implant system composed of several key components, each engineered for durability and biocompatibility:
- Glenosphere: This is the metallic ball component that is fixed to the glenoid (socket) of the scapula. It's typically made of highly polished cobalt-chromium alloy, known for its strength and wear resistance.
- Glenoid Baseplate: A titanium baseplate is typically secured to the scapula with screws. The glenosphere then attaches to this baseplate. Titanium is favored for its excellent biocompatibility and ability to integrate with bone (osseointegration).
- Humeral Stem: This component is inserted into the intramedullary canal (marrow cavity) of the humerus (upper arm bone). It's usually made of titanium or cobalt-chromium. The stem provides stability and a platform for the humeral cup.
- Humeral Cup: This is the polyethylene (plastic) socket component that articulates with the glenosphere. It is typically made of ultra-high molecular weight polyethylene (UHMWPE), a material chosen for its low friction, wear resistance, and excellent biocompatibility.
- Humeral Tray: The humeral cup often sits within a metallic humeral tray, usually made of titanium or cobalt-chromium, which is then affixed to the humeral stem.
Materials Overview:
| Component | Primary Material | Key Properties |
| :-------- | :--------------- | :------------- |
| Glenosphere | Cobalt-Chromium | Strength, wear resistance, polished surface |
| Glenoid Baseplate | Titanium | Biocompatibility, osseointegration |
| Humeral Stem | Titanium/Cobalt-Chromium | Strength, stability |
| Humeral Cup | UHMWPE | Low friction, wear resistance, biocompatibility |
| Humeral Tray | Titanium/Cobalt-Chromium | Stability, structural support |
Biomechanics: How the Reversal Works
The genius of the RTSP lies in its altered biomechanics:
- Medialization and Distalization of the Center of Rotation: By placing the ball on the glenoid, the center of rotation of the joint is moved inward (medially) and downward (distally). This subtle but critical change has profound effects.
- Enhanced Deltoid Leverage: This new center of rotation effectively lengthens the deltoid muscle's lever arm. This means the deltoid muscle can generate more force for a given contraction, compensating for the absent or damaged rotator cuff.
- Improved Abduction and Elevation: The primary functional improvement seen with RTSP is the ability to lift the arm away from the body (abduction) and overhead (elevation), movements that are severely impaired when the rotator cuff is non-functional.
- Limitations: While excellent for elevation and abduction, external rotation (rotating the arm outwards) can be limited with an RTSP, as the original external rotators (part of the rotator cuff) are often deficient.
Mechanism of Action: Empowering the Deltoid
In a healthy shoulder, the rotator cuff muscles (supraspinatus, infraspinatus, teres minor, subscapularis) are crucial for initiating and controlling arm movements, especially overhead lifting and rotation. When these muscles are severely damaged or torn, the deltoid muscle, despite being powerful, cannot effectively lift the arm because it lacks the stable fulcrum provided by a healthy rotator cuff.
The RTSP creates an artificial, stable fulcrum by reversing the ball and socket. This new fulcrum allows the deltoid muscle to effectively pull the humerus and lift the arm, restoring significant functional movement for patients who previously suffered from "pseudoparalysis" (inability to lift the arm despite having an intact deltoid).
3. Extensive Clinical Indications & Usage
The Reverse Total Shoulder Prosthesis is a highly effective treatment for specific, often complex, shoulder conditions.
Primary Indications:
- Rotator Cuff Tear Arthropathy (RCTOA): This is the most common indication. It occurs when a long-standing, massive, irreparable rotator cuff tear leads to superior migration of the humeral head, causing cartilage damage and severe arthritis. The RTSP is uniquely suited to address both the cuff deficiency and the arthritis.
- Failed Conventional Total Shoulder Arthroplasty (TSA) with Rotator Cuff Deficiency: If a traditional shoulder replacement fails due to progressive rotator cuff tearing, leading to instability or pain, conversion to an RTSP may be necessary.
- Complex Proximal Humerus Fractures: In elderly patients with poor bone quality or in cases where the fracture fragments are too numerous or small to reconstruct, an RTSP can provide a predictable outcome for pain relief and function, especially when the rotator cuff is compromised by the fracture.
- Irreparable Rotator Cuff Tears with Pseudoparalysis: Patients who cannot actively lift their arm above 90 degrees due to a massive, irreparable rotator cuff tear, even without significant arthritis, may be candidates.
- Severe Glenohumeral Arthritis with Significant Rotator Cuff Deficiency: Similar to RCTOA, but perhaps without the classic superior migration pattern, if both conditions are present, RTSP is often preferred.
- Tumor Resection Reconstruction: In rare cases, after the removal of tumors in the proximal humerus or glenoid, an RTSP can be used for reconstruction.
The Surgical Procedure (Patient Overview):
The surgery is performed under general anesthesia, often with a regional nerve block for extended pain relief.
- Pre-operative Planning: Detailed X-rays, CT scans, and sometimes MRI are used to assess bone quality, rotator cuff status, and plan implant sizing and positioning.
- Incision: Typically, an incision is made on the front of the shoulder (deltopectoral approach) or a superior approach, allowing access to the joint.
- Joint Exposure: The surgeon carefully navigates through muscles and soft tissues to expose the glenohumeral joint.
- Glenoid Preparation: The damaged cartilage and bone on the glenoid are removed, and the glenoid baseplate is secured to the scapula using screws. The glenosphere is then attached to this baseplate.
- Humeral Preparation: The humeral head is resected (removed). The intramedullary canal of the humerus is prepared, and the humeral stem is inserted.
- Component Assembly: The humeral cup (with its polyethylene liner) is attached to the humeral stem.
- Reduction and Testing: The joint is "reduced" (the humeral cup is seated onto the glenosphere), and the surgeon tests the range of motion and stability to ensure proper function.
- Closure: The soft tissues are meticulously repaired, and the incision is closed.
Post-operative Care and Rehabilitation: The Road to Recovery
Successful outcomes depend significantly on diligent post-operative care and rehabilitation.
- Immobilization: The arm is typically placed in a sling for several weeks (e.g., 4-6 weeks) to protect the healing tissues. Specific positioning may be advised.
- Pain Management: Pain medication will be prescribed to manage discomfort.
- Physical Therapy: This is CRUCIAL. A structured physical therapy program will begin soon after surgery, often starting with passive range of motion (the therapist moves your arm) and progressing to active-assisted and then active exercises. The goals are to restore motion, strengthen the deltoid, and improve overall function.
- Restrictions: Patients will have specific restrictions on lifting, pushing, pulling, and certain rotational movements (especially external rotation) for several months to prevent complications like dislocation or implant loosening.
- Maintenance of the Implant: Once implanted, the RTSP requires no active "maintenance" from the patient beyond following post-operative instructions and attending follow-up appointments. Longevity depends on patient activity levels, bone quality, and absence of complications.
4. Risks, Side Effects, or Contraindications
While RTSP offers remarkable benefits, it is a major surgical procedure with potential risks and considerations.
Potential Risks and Complications:
- Infection: As with any surgery, there's a risk of infection, which can be superficial or deep, potentially requiring further surgery or removal of the implant.
- Dislocation: Although less common than with traditional TSA, the RTSP can dislocate, especially with extreme movements.
- Scapular Notching: This is a unique complication to RTSP, where the polyethylene humeral cup impinges on the inferior pillar of the scapula during adduction and internal rotation, potentially causing erosion (notching) of the bone. While not always symptomatic, severe notching can lead to pain or loosening.
- Nerve or Vascular Injury: Nerves (e.g., axillary nerve) and blood vessels around the shoulder can be injured during surgery.
- Humeral Fracture (Periprosthetic Fracture): A fracture of the humerus can occur during or after surgery.
- Loosening of Components: Over time, the glenoid or humeral components can loosen from the bone, requiring revision surgery.
- Deltoid Dysfunction: If the deltoid muscle is compromised (e.g., nerve injury, detachment), the RTSP may not function effectively.
- Heterotopic Ossification: Abnormal bone formation in the soft tissues around the joint can occur, potentially limiting motion.
- Persistent Pain: While the goal is pain relief, some patients may experience persistent pain.
Common Side Effects:
- Limited External Rotation: As mentioned, due to the biomechanical design and often deficient external rotator muscles, achieving full external rotation can be challenging.
- Initial Weakness and Stiffness: Expected during the recovery phase, gradually improving with therapy.
Contraindications:
- Active Infection: Surgery is contraindicated if there is an active infection in the shoulder or elsewhere in the body.
- Non-functional Deltoid Muscle: The RTSP relies heavily on a functional deltoid. If the deltoid is paralyzed or severely compromised, the surgery is unlikely to be successful.
- Insufficient Glenoid Bone Stock: Adequate bone on the scapula is required to securely fix the glenoid baseplate. Severe bone loss may preclude RTSP.
- Unrealistic Patient Expectations: Patients must understand the limitations and expected outcomes of the surgery.
- Severe Medical Comorbidities: Patients with significant heart, lung, or other medical conditions that make surgery too risky may not be candidates.
5. Expert Tips from Dr. Mohammed Hutaif
"As an orthopedic specialist, I've seen firsthand the transformative impact of the Reverse Total Shoulder Prosthesis on patients' lives. My advice focuses on ensuring the best possible outcomes:
- Patient Selection is Paramount: The success of an RTSP hinges on careful patient selection. It's not a one-size-fits-all solution. A thorough evaluation, including advanced imaging and a detailed discussion of your specific condition and lifestyle, is essential to determine if you are an ideal candidate.
- Realistic Expectations are Key: While RTSP can dramatically improve pain and the ability to lift your arm, it's important to have realistic expectations. You will regain significant function, but it's unlikely to be a 'normal' shoulder, especially regarding heavy lifting or certain rotational movements. Discuss your goals with your surgeon.
- Commitment to Rehabilitation: Surgery is only half the journey. Your dedication to the prescribed physical therapy program is absolutely critical for regaining strength, mobility, and maximizing your functional recovery. Skipping sessions or not following instructions can compromise your results.
- Long-Term Follow-up: Regular follow-up appointments with your surgeon are important to monitor the implant's longevity, address any concerns, and ensure continued success. Even years down the line, these check-ups are valuable.
- Protect Your New Shoulder: Avoid activities that place excessive stress on the implant, especially heavy lifting or repetitive overhead activities, beyond what your surgeon and therapist recommend. Think of it as a finely tuned instrument that requires careful handling.
- Choose an Experienced Surgeon: Reverse total shoulder arthroplasty is a complex procedure. Seek a surgeon with extensive experience and specialized training in shoulder surgery to ensure the highest level of expertise and care."
6. Massive FAQ Section
Q1: What is the typical recovery time after a Reverse Total Shoulder Prosthesis?
A: Recovery varies significantly among individuals, but generally involves several phases. You'll likely be in a sling for 4-6 weeks. Physical therapy usually begins within the first week or two. Most patients regain significant functional use of their arm by 3-6 months, with continued strength and mobility improvements for up to a year or more. Full recovery and maximum improvement can take 12-18 months.
Q2: How long does a Reverse Total Shoulder Prosthesis last?
A: Modern RTSP implants are designed for long-term durability. Studies show good survival rates, with many implants lasting 10-15 years or more. Factors affecting longevity include patient activity level, bone quality, adherence to post-operative instructions, and absence of complications like infection or loosening.
Q3: Will I regain full range of motion after RTSP?
A: While you will experience a significant improvement in your ability to lift your arm (abduction and elevation), especially if you had pseudoparalysis before surgery, it's unlikely to regain "full" range of motion as in a healthy natural shoulder. External rotation is often limited. The goal is functional range of motion for daily activities, not necessarily pre-injury athletic range.
Q4: Can I play sports or lift heavy objects after RTSP?
A: Most high-impact or overhead sports, as well as heavy lifting (typically exceeding 10-15 lbs), are generally discouraged to protect the implant and prevent complications. Low-impact activities like walking, swimming (once cleared), and golf (with modifications) may be possible. Always follow your surgeon's specific recommendations.
Q5: How is RTSA different from a traditional Total Shoulder Arthroplasty (TSA)?
A: The key difference is the "reverse" anatomy. In traditional TSA, a metal ball replaces the humeral head, and a plastic socket replaces the glenoid. It requires a functional rotator cuff. RTSA reverses this, placing the ball on the scapula and the socket on the humerus, allowing the deltoid muscle to compensate for a non-functional rotator cuff.
Q6: What are the signs of a complication after RTSP?
A: Seek immediate medical attention if you experience:
* Increasing, severe pain that isn't controlled by medication.
* Fever, chills, or redness/swelling/drainage around the incision site (signs of infection).
* Sudden inability to move your arm, or a "clunking" sensation (may indicate dislocation).
* Numbness, tingling, or weakness in your arm or hand that wasn't present before.
Q7: What if my deltoid muscle is weak or non-functional?
A: A functional deltoid muscle is crucial for the success of an RTSP. If your deltoid is paralyzed or severely damaged, an RTSP may not be a suitable option, as it relies on this muscle to power arm movement. Your surgeon will carefully assess your deltoid function during the evaluation.
Q8: Are there non-surgical alternatives to RTSP?
A: For conditions requiring an RTSP (like rotator cuff tear arthropathy), non-surgical options typically provide only temporary symptom relief. These may include pain medication, injections, and physical therapy to manage symptoms, but they cannot restore function or repair irreparable rotator cuff damage. RTSP is generally considered when conservative treatments have failed and quality of life is severely impacted.
Q9: What is "scapular notching" and should I be concerned?
A: Scapular notching is a common radiographic finding unique to RTSP, where the humeral cup rubs against the lower edge of the scapula during certain movements, causing bone erosion. While common, it's not always symptomatic. Your surgeon will monitor for it. In severe cases, it can cause pain or lead to implant loosening, but many patients with notching remain asymptomatic and functional.
Q10: Will I need to take special precautions for dental procedures or other surgeries after RTSP?
A: It is generally recommended to inform your dentist or other surgeons that you have a joint replacement. While the need for antibiotic prophylaxis (pre-treatment with antibiotics) for dental procedures is debated and less commonly recommended for joint replacements than it once was, your orthopedic surgeon will provide specific guidance based on your individual risk factors and current guidelines.
Q11: Can I fly on an airplane after having an RTSP?
A: Yes, you can fly after an RTSP. The metal components in the implant may trigger airport metal detectors, so it's advisable to carry a card from your surgeon indicating you have an orthopedic implant. Discuss with your surgeon when it's safe to fly, especially regarding immediate post-operative travel and potential swelling or discomfort.
Q12: How long after surgery can I drive?
A: You should not drive while taking narcotic pain medication. Additionally, you typically cannot drive until you are out of your sling and have regained sufficient strength, reaction time, and range of motion to safely operate a vehicle, especially your dominant arm. This usually takes several weeks to a few months, depending on individual recovery and which arm was operated on. Your surgeon will advise you when it is safe to resume driving.
Disclaimer: This information is for educational purposes only and is not intended as medical advice. Always consult with a qualified healthcare professional for diagnosis and treatment of any medical condition.