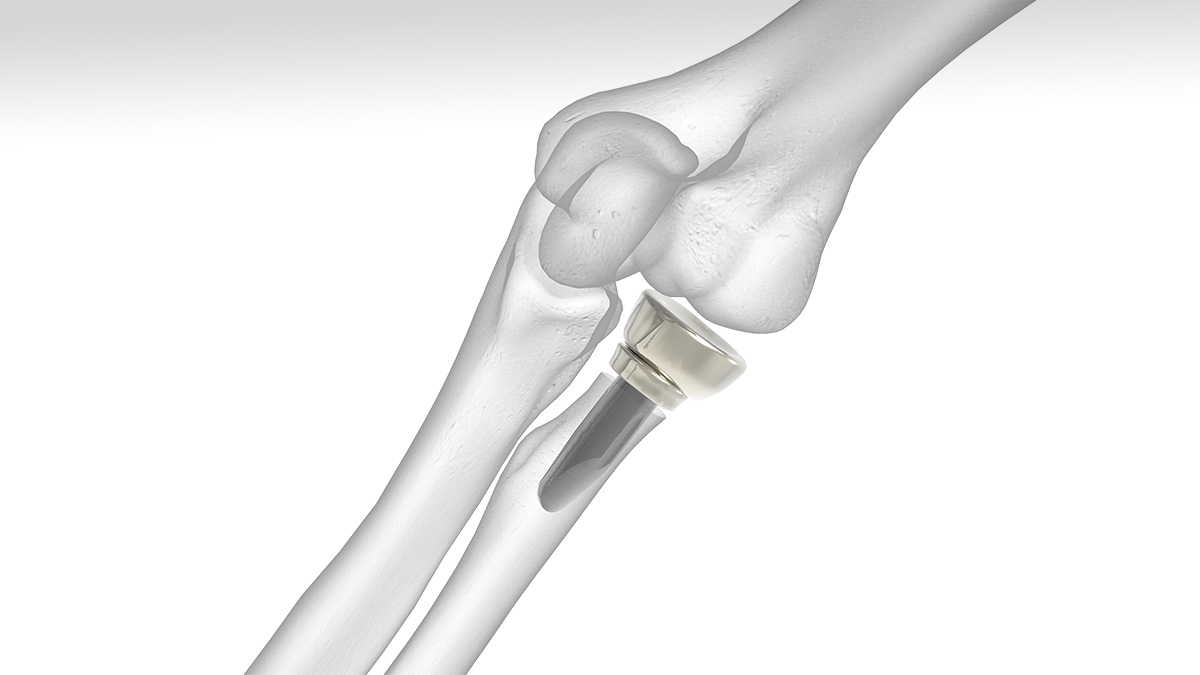
Understanding Radial Head Prosthesis: Modular vs. Monoblock
Welcome to this comprehensive guide on radial head prostheses, a critical component in modern orthopedic surgery for restoring elbow function. As an expert in orthopedic care, Dr. Mohammed Hutaif is dedicated to providing you with clear, authoritative, and easy-to-understand information about this advanced treatment option. This guide will delve into the intricacies of both modular and monoblock radial head prostheses, covering their design, applications, benefits, and what you can expect as a patient.
1. Comprehensive Introduction & Overview
The radial head is a vital part of the elbow joint, contributing significantly to its stability and range of motion, particularly in forearm rotation (pronation and supination). When the radial head is severely damaged, often due to trauma like fractures or dislocations, it can lead to pain, instability, and impaired function of the entire elbow. In such cases where the natural radial head cannot be effectively repaired or reconstructed, a radial head prosthesis offers a robust solution.
A radial head prosthesis is an artificial implant designed to replace the damaged portion of the radial bone in the elbow. Its primary goals are to:
* Restore stability to the elbow joint.
* Alleviate pain.
* Preserve or improve the elbow's range of motion.
* Prevent long-term complications such as arthritis or chronic instability.
There are two main types of radial head prostheses: modular and monoblock. While both serve the same fundamental purpose, they differ in their construction and offer distinct advantages depending on the patient's specific injury and anatomical needs. This guide will explore these differences in detail, helping you understand which approach might be most suitable.
2. Deep-dive into Technical Specifications / Mechanisms
Radial head prostheses are marvels of biomechanical engineering, designed to mimic the complex movements of the natural elbow joint. Their effectiveness hinges on precise design, material selection, and proper surgical implantation.
Design Considerations: Modular vs. Monoblock
Modular Prosthesis
- Construction: A modular prosthesis consists of multiple separate components that are assembled during surgery. Typically, these include:
- Stem: Inserted into the radial canal.
- Head: The articulating surface that replaces the natural radial head.
- Neck/Collar: Connects the head to the stem, often allowing for adjustment of length and rotation.
- Advantages:
- Customization: The surgeon can select different sizes for the stem, head, and neck independently, allowing for a highly customized fit that closely matches the patient's unique anatomy.
- Intraoperative Flexibility: Provides the surgeon with the ability to adjust component sizes and alignment during the procedure, optimizing joint stability and range of motion.
- Revision Potential: If one component fails, it may be possible to replace just that component rather than the entire prosthesis.
- Disadvantages:
- Potential for component dissociation or wear at the interfaces over time.
- More complex surgical procedure due to assembly.
Monoblock Prosthesis
- Construction: A monoblock prosthesis is a single, pre-assembled unit where the stem, head, and often the neck are integrated into one piece.
- Advantages:
- Simplicity of Insertion: Requires fewer steps for implantation, potentially reducing operative time.
- Reduced Risk of Dissociation: Being a single unit, there is no risk of individual components separating.
- Streamlined Design: Often has a lower profile, which can be advantageous in certain anatomical situations.
- Disadvantages:
- Less flexibility for intraoperative adjustments to size and length.
- If any part fails, the entire prosthesis typically needs to be replaced.
Materials Used in Radial Head Prostheses
The choice of materials is crucial for biocompatibility, durability, and functional performance. Common materials include:
* Cobalt-Chrome (CoCr) Alloys: Often used for the prosthetic head due to their excellent wear resistance, strength, and biocompatibility.
* Titanium Alloys: Frequently used for the stem due to their superior biocompatibility, lighter weight, and ability to promote bone ingrowth (osseointegration) for uncemented fixation.
* Surface Coatings: Some prostheses may feature porous or hydroxyapatite coatings on the stem to encourage bone ingrowth, providing long-term biological fixation.
Biomechanics and Mechanism of Action
The radial head prosthesis functions by:
1. Restoring Radial Length: Crucial for maintaining proper tension in the interosseous membrane and stability of the distal radioulnar joint (DRUJ).
2. Providing an Articulating Surface: The prosthetic head articulates with the capitellum of the humerus and the radial notch of the ulna, allowing for smooth flexion/extension and pronation/supination.
3. Stabilizing the Elbow: By replacing the damaged radial head, the prosthesis helps to restore the bony buttress against valgus (outward) stress and prevents posterior displacement of the ulna relative to the humerus.
4. Preserving Soft Tissue Integrity: Proper radial head replacement can protect surrounding ligaments and soft tissues from excessive strain, which is vital for long-term elbow health.
Maintenance and Sterilization Protocols (Device Specific)
For patient safety, radial head prostheses are manufactured under strict quality control standards. They are typically:
* Pre-sterilized: Most prostheses are supplied sterile by the manufacturer, often using gamma irradiation or ethylene oxide.
* Single-Use Devices: Designed for implantation in a single patient to prevent cross-contamination and ensure optimal performance.
* Strict Packaging: Provided in sterile, sealed packaging to maintain their integrity until the moment of surgery.
* Material Properties: The materials used are chosen for their inertness and resistance to degradation within the body.
3. Extensive Clinical Indications & Usage
Radial head prosthesis is a highly effective treatment for specific types of elbow injuries and conditions where repair of the natural radial head is not feasible or would yield poor results.
Primary Indications:
- Comminuted Radial Head Fractures (Mason Type III & IV): These are severe fractures where the bone is broken into multiple pieces, making surgical repair impossible or unlikely to succeed.
- Mason Type III: Severely comminuted, displaced fracture involving the entire radial head.
- Mason Type IV: Fracture of the radial head associated with elbow dislocation.
- Terrible Triad Injuries: A complex elbow injury involving a radial head fracture, a coronoid fracture, and an elbow dislocation. Radial head replacement is often critical for restoring stability in these cases.
- Essex-Lopresti Injuries: A severe injury characterized by a radial head fracture, disruption of the interosseous membrane (between the radius and ulna), and instability of the distal radioulnar joint (DRUJ). Radial head replacement is crucial to restore radial length and prevent chronic wrist pain and instability.
- Monteggia Fractures: Involving a fracture of the ulna with an associated dislocation of the radial head. While some radial head dislocations can be reduced, severe damage to the radial head may necessitate replacement.
- Failed Radial Head Excision: In some older cases, the radial head might have been surgically removed (excised) after a fracture, leading to chronic instability, pain, or proximal migration of the radius. A prosthesis can address these issues.
- Chronic Elbow Instability: In rare cases, chronic instability related to radial head deficiency, even without acute fracture, may benefit from prosthetic replacement.
Surgical Procedure (Simplified Patient Explanation):
The surgery is typically performed under general anesthesia or regional block.
1. Incision and Exposure: An incision is made on the outer side of the elbow to expose the radial head.
2. Resection of Damaged Radial Head: The fractured or damaged radial head is carefully removed.
3. Radial Canal Preparation: The medullary canal of the radius is prepared using specialized reamers to create a precise fit for the prosthetic stem.
4. Trial Implantation: Trial components (for modular) or a trial prosthesis (for monoblock) are inserted to assess fit, stability, and range of motion. This step is crucial for selecting the correct size and ensuring optimal biomechanics.
5. Final Implantation: The chosen prosthesis is then implanted. It can be cemented (using bone cement for immediate fixation) or uncemented (relying on a press-fit and eventual bone ingrowth for long-term fixation).
6. Soft Tissue Repair: Any damaged ligaments or the joint capsule are repaired to further enhance elbow stability.
7. Closure: The incision is closed in layers.
8. Post-operative Care: The elbow is typically immobilized in a splint or brace, followed by a structured rehabilitation program.
4. Risks, Side Effects, or Contraindications
While radial head replacement is a safe and effective procedure, like all surgeries, it carries potential risks and possible side effects. Understanding these is important for informed decision-making.
Potential Risks and Complications:
- Infection: Though rare, infection can occur at the surgical site, potentially requiring antibiotics or further surgery.
- Nerve or Blood Vessel Damage: Injury to nerves (e.g., posterior interosseous nerve) or blood vessels around the elbow is a rare but serious complication.
- Prosthesis Loosening or Failure: Over time, the prosthesis may loosen from the bone or components may wear out, necessitating revision surgery.
- Dislocation or Subluxation: The prosthetic head can dislocate from its articulation, especially if soft tissue repairs are inadequate or if there is excessive trauma.
- Stiffness or Limited Range of Motion: Despite successful surgery, some patients may experience residual stiffness or difficulty regaining full elbow movement.
- Heterotopic Ossification: Abnormal bone formation in the soft tissues around the elbow, which can restrict motion.
- Aseptic Loosening: Loosening of the implant without infection, often due to mechanical factors or biological response to wear particles.
- Fracture: Periprosthetic fracture (a fracture around the implant) can occur during or after surgery.
- Pain: Persistent pain can occur despite successful surgery.
- Component Dissociation (Modular only): In modular prostheses, the head or stem components can rarely separate.
Side Effects:
- Temporary Swelling and Bruising: Common after surgery, usually subsides within weeks.
- Discomfort and Pain: Managed with medication.
- Scarring: A visible scar at the incision site.
Contraindications:
- Active Infection: Presence of an active infection in the elbow or elsewhere in the body is an absolute contraindication, as it significantly increases the risk of prosthetic joint infection.
- Insufficient Bone Stock: In cases of severe bone loss, there may not be enough healthy bone to support the implant.
- Severe Osteoporosis: While not an absolute contraindication, extremely poor bone quality can compromise implant fixation.
- Inability to Comply with Rehabilitation: Successful outcomes heavily rely on patient adherence to a post-operative physical therapy program.
- Certain Severe Soft Tissue Injuries: If the surrounding ligaments and capsule are too severely damaged to provide adequate stability, prosthesis alone may not suffice.
- Unrealistic Patient Expectations: Patients must have a clear understanding of the potential outcomes and limitations of the surgery.
5. Expert Tips from Dr. Mohammed Hutaif
As an orthopedic specialist, I've seen firsthand the transformative impact a properly performed radial head replacement can have on a patient's quality of life. Here are some key insights and tips I share with my patients:
- Early Diagnosis is Key: Don't delay seeking medical attention for elbow injuries. Timely and accurate diagnosis of radial head fractures and associated ligamentous injuries is crucial for optimal surgical planning and outcomes.
- Choosing the Right Prosthesis: The decision between a modular and monoblock prosthesis is highly individualized. It depends on the specific fracture pattern, the patient's anatomy, the extent of soft tissue injury, and the surgeon's experience. A modular prosthesis offers greater flexibility for complex cases, while a monoblock may be suitable for simpler reconstructions. We will discuss which option is best for your unique situation.
- Rehabilitation is Paramount: Surgery is only half the battle. A dedicated and consistent post-operative physical therapy program is absolutely vital for regaining strength, flexibility, and function. Your commitment to rehabilitation directly impacts your long-term success.
- Listen to Your Body: While pushing yourself in therapy is important, always respect your body's signals. Pain is a warning sign. Communicate any unusual symptoms or discomfort to your physical therapist and medical team immediately.
- Realistic Expectations: While radial head replacement can restore significant function and alleviate pain, it's important to have realistic expectations. The goal is to improve your quality of life and functional capacity, not necessarily to return to pre-injury levels of extreme activity, especially in highly demanding sports.
- Surgeon's Experience Matters: Radial head arthroplasty, particularly in the context of complex elbow trauma, requires specialized expertise. Choose a surgeon with extensive experience in elbow reconstruction.
6. Massive FAQ Section
Q1: What is the radial head and why is it important?
A1: The radial head is the top, rounded part of the radius bone, one of the two bones in your forearm. It's crucial for elbow stability, articulating with the humerus (upper arm bone) and ulna (other forearm bone) to allow for smooth flexion/extension and rotation of your forearm (pronation and supination).
Q2: When is a radial head prosthesis typically recommended?
A2: A prosthesis is typically recommended for severe radial head fractures (Mason Type III or IV) that cannot be effectively repaired, especially when associated with elbow dislocation or instability (e.g., terrible triad, Essex-Lopresti injuries). It's also considered for failed previous radial head excisions.
Q3: What is the difference between a modular and a monoblock prosthesis?
A3: A modular prosthesis consists of separate components (stem, head, neck) that are assembled during surgery, allowing for customized sizing. A monoblock prosthesis is a single, pre-assembled unit. Modular offers more flexibility, while monoblock is simpler to implant.
Q4: How long does the surgery take?
A4: The surgery typically takes between 1 to 2 hours, but this can vary depending on the complexity of the injury and whether other structures (like ligaments) also need repair.
Q5: What is the recovery period like after radial head replacement?
A5: Initial recovery involves immobilization for a short period, followed by several weeks to months of physical therapy. Most patients regain significant function within 3-6 months, but full recovery can take up to a year. Adherence to physical therapy is key.
Q6: Will I regain full function of my elbow?
A6: The goal is to restore as much function as possible, reduce pain, and improve stability. Many patients achieve excellent functional outcomes, but "full" function, especially for highly demanding activities, might not always be completely restored to pre-injury levels. Significant improvement in daily activities is very common.
Q7: Are there any restrictions after getting a radial head prosthesis?
A7: Yes, initially there will be restrictions on weight-bearing and certain movements. Long-term, high-impact activities or heavy lifting might be limited to protect the implant. Your surgeon and physical therapist will provide specific guidelines based on your individual recovery.
Q8: How long does a radial head prosthesis typically last?
A8: The lifespan of a radial head prosthesis varies, but many can last 10-15 years or more. Factors like patient activity level, bone quality, and the original injury can influence durability. Regular follow-ups are important to monitor the implant.
Q9: What are the signs that something might be wrong with my prosthesis?
A9: Signs of a potential problem include new or worsening pain, swelling, redness, warmth around the elbow, clicking or grinding sensations, instability, or a sudden loss of motion. You should contact your doctor immediately if you experience any of these symptoms.
Q10: Is the surgery painful?
A10: You will receive anesthesia during the surgery, so you won't feel pain. After surgery, pain is managed with medication. Discomfort is normal during the initial recovery and rehabilitation phases, but it should gradually improve.
Q11: Will I need physical therapy?
A11: Absolutely. Physical therapy is a crucial part of the recovery process. It helps restore range of motion, strength, and overall function to your elbow and forearm.
Q12: Can I play sports after a radial head replacement?
A12: The ability to return to sports depends on the type of sport, your individual recovery, and the stability of your elbow. Low-impact activities are often possible, but high-impact or contact sports may be restricted. Always discuss your specific activity goals with Dr. Hutaif.
This content is for patient information only and is not medical advice. Always consult with a qualified healthcare professional for diagnosis and treatment.