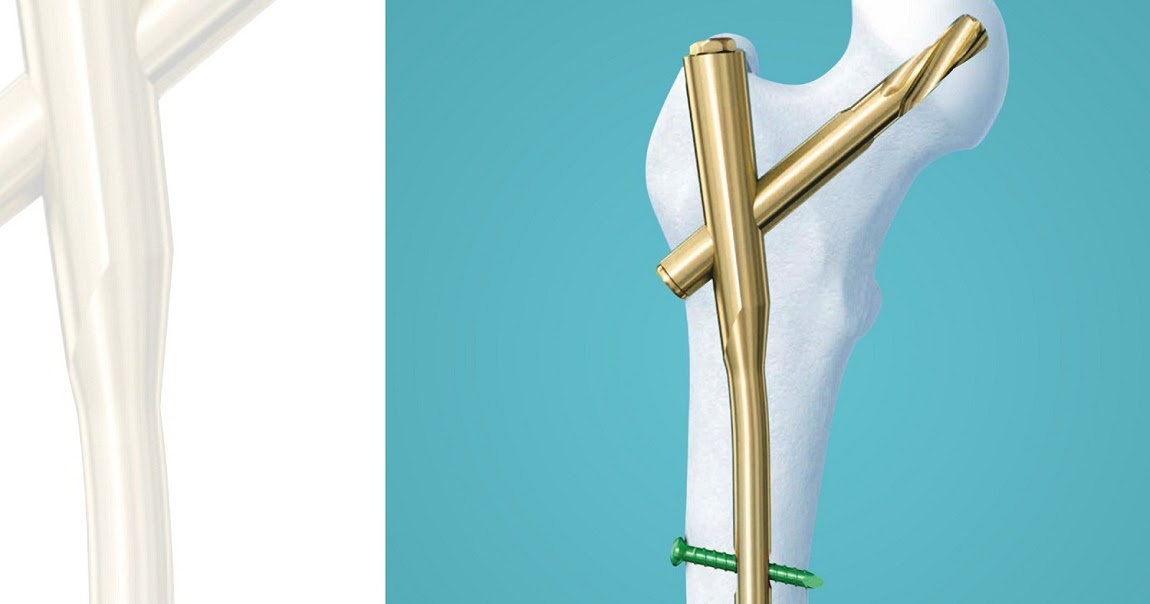
Proximal Femoral Nail Antirotation (PFNA): An Advanced Solution for Femur Fractures
Welcome to this comprehensive guide on Proximal Femoral Nail Antirotation (PFNA), an innovative and highly effective surgical technique used to treat certain types of fractures in the upper part of the thigh bone (femur). As an expert orthopedic specialist, Dr. Mohammed Hutaif is dedicated to providing patients with the most advanced and evidence-based treatments available. This guide aims to demystify PFNA, offering a clear, authoritative, and exhaustive overview for patients seeking to understand their treatment options.
Please note: The information provided here is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider for any medical concerns.
1. Comprehensive Introduction & Overview
Proximal Femoral Nail Antirotation (PFNA) represents a significant advancement in the field of orthopedic trauma surgery. It is a specialized type of intramedullary nailing, a procedure where a metal rod (nail) is inserted into the medullary canal (the hollow center) of a bone to stabilize a fracture. PFNA is specifically designed to address complex fractures of the proximal femur, which include the head, neck, and trochanteric regions – areas critical for hip joint function and weight-bearing.
Historically, these fractures were often treated with plates and screws, or in some cases, hip replacement. While effective, these methods could sometimes be associated with challenges such as extensive soft tissue dissection, higher rates of non-union, or difficulties with early weight-bearing. The evolution of intramedullary nailing, and specifically the development of devices like PFNA, has revolutionized the treatment of these challenging fractures by offering a less invasive, biomechanically superior, and often quicker recovery pathway.
The core principle behind PFNA is to provide robust internal fixation that allows for early mobilization and weight-bearing, facilitating faster rehabilitation and improved patient outcomes. Its unique design features, particularly the helical blade, offer superior rotational stability and controlled impaction, which are crucial for optimal healing in these high-stress areas of the femur.
2. Deep-Dive into Technical Specifications / Mechanisms
The efficacy of PFNA lies in its meticulously engineered design and sophisticated biomechanical principles.
2.1. Design and Materials
The PFNA system is typically composed of a few key components, all manufactured to exacting standards:
-
The Intramedullary Nail: This is the main body of the implant.
- Material: Most PFNA nails are made from advanced biocompatible materials, predominantly titanium alloys (e.g., Ti-6Al-4V). Titanium is chosen for its excellent strength-to-weight ratio, corrosion resistance, and inertness within the human body, minimizing adverse reactions.
- Anatomical Design: The nail is pre-contoured with a specific anterior bow (curvature) to match the natural anatomy of the femur, ensuring a precise fit and reducing stress points.
- Proximal Section: This part is wider and features specific holes for the helical blade and, in some designs, a secondary antirotation screw. The design is optimized for secure engagement with the femoral head and neck.
- Distal Section: The nail tapers distally and includes holes for locking screws, which further stabilize the implant within the femoral shaft.
-
The Helical Blade: This is the most distinctive feature of the PFNA system.
- Mechanism: Unlike traditional screws that cut bone threads, the helical blade compresses cancellous (spongy) bone around it as it is inserted. This controlled impaction significantly enhances resistance to cut-out (when the implant migrates out of the bone) and provides superior rotational stability to the femoral head fragment.
- Material: Also titanium alloy, ensuring compatibility and strength.
- Design: It has a unique helical (spiral) shape, designed for optimal purchase in the bone and to distribute stress over a larger surface area than a conventional screw.
-
Distal Locking Screws: These screws are inserted through holes in the distal part of the nail and into the femoral cortex.
- Purpose: They prevent rotational movement of the nail within the bone shaft and control axial migration, ensuring the entire construct functions as a stable unit.
- Types: Available in various lengths and diameters, often with dynamic or static locking options depending on the fracture pattern and surgeon's preference.
2.2. Mechanism of Action and Biomechanics
The PFNA system operates on several critical biomechanical principles:
- Intramedullary Fixation (Load Sharing): By placing the nail within the medullary canal, PFNA acts as an internal splint. This central placement allows the implant to share axial loads with the surrounding bone, rather than primarily bearing the load (as plates do). Load sharing promotes callus formation and biological healing, reducing the risk of stress shielding (where the implant carries too much load, causing the bone to weaken).
- Antirotation Stability: This is where PFNA truly excels. The combination of the large-diameter helical blade, which compacts bone and resists rotation, and the potential for a secondary antirotation screw (in some PFNA-II designs) provides unparalleled rotational control of the femoral head and neck fragments. This is crucial for preventing malunion and ensuring proper anatomical alignment during healing.
- Controlled Impaction: The helical blade's design allows for controlled impaction of the cancellous bone around it. This creates a highly stable construct, significantly reducing the risk of the blade cutting out, especially in osteoporotic (weakened) bone, which is common in older patients suffering these fractures.
- Minimally Invasive Approach: The procedure typically involves a small incision at the greater trochanter. This minimally invasive technique reduces soft tissue disruption, preserves periosteal blood supply (essential for bone healing), and often leads to less post-operative pain and faster recovery compared to open reduction and internal fixation with plates.
- Dynamic vs. Static Locking: Depending on the fracture pattern and desired outcome, the distal locking screws can be inserted statically (preventing any movement) or dynamically (allowing for controlled micromotion, which can stimulate bone healing).
3. Extensive Clinical Indications & Usage
PFNA is a versatile implant, indicated for a broad spectrum of proximal femoral fractures, particularly those that involve the trochanteric region.
3.1. Clinical Indications
- Intertrochanteric Fractures: These are fractures occurring between the greater and lesser trochanters. PFNA is highly effective for both stable and unstable intertrochanteric fractures (e.g., AO/OTA 31-A1, A2, A3 classifications). Its superior rotational stability is especially beneficial for unstable patterns.
- Subtrochanteric Fractures: Fractures occurring below the lesser trochanter. These are often high-energy injuries and can be very challenging due to significant deforming muscle forces. PFNA's robust fixation and long nail options are well-suited for these complex fractures.
- Combined Intertrochanteric and Subtrochanteric Fractures: For fractures extending across both regions, PFNA provides a comprehensive solution.
- Pathological Fractures: Fractures occurring through bone weakened by conditions such as metastatic tumors or primary bone tumors. PFNA can provide immediate stability and pain relief, improving quality of life for these patients.
- Impending Pathological Fractures: In cases where a tumor has significantly weakened the bone, prophylactic nailing with PFNA can prevent a fracture from occurring, sparing the patient from acute pain and a more complex emergency surgery.
- Non-unions or Mal-unions: In some instances, PFNA can be used as a revision surgery for fractures that have failed to heal (non-union) or have healed in an unacceptable position (mal-union) after previous treatment.
- Osteoporotic Fractures: Due to its excellent rotational stability and resistance to cut-out, PFNA is particularly advantageous in elderly patients with osteoporotic bone, where traditional screw fixation might be prone to failure.
3.2. Surgical Procedure: A Patient's Overview
The PFNA surgical procedure is performed under strict sterile conditions and typically involves the following steps:
- Pre-operative Planning: Dr. Hutaif will conduct a thorough assessment, including X-rays and often CT scans, to precisely characterize the fracture. Digital templating is used to select the appropriate nail length, diameter, and blade size.
- Anesthesia: The procedure is performed under general anesthesia or regional anesthesia (spinal/epidural) combined with sedation.
- Patient Positioning: The patient is positioned on a specialized orthopedic traction table, which allows for closed reduction (realigning the bone fragments without an open incision) and controlled traction of the limb.
- Incision and Entry Point: A small incision (typically 3-5 cm) is made over the greater trochanter. A guide wire is then inserted into the medullary canal through a precise entry point on the tip of the greater trochanter.
- Reaming (Optional): Depending on the bone size and nail diameter, the medullary canal may be reamed (widened) to ensure smooth passage of the nail.
- Nail Insertion: The PFNA nail is carefully inserted over the guide wire into the medullary canal, passing across the fracture site.
- Helical Blade Insertion: Using specialized instrumentation and fluoroscopic guidance (real-time X-ray imaging), the helical blade is accurately inserted into the femoral head, providing primary stability and antirotation.
- Distal Locking: Fluoroscopy is again used to guide the insertion of distal locking screws through the nail and into the femoral shaft, securing the distal end of the implant.
- Wound Closure: The incision is thoroughly irrigated, and the layers of tissue are closed.
3.3. Fitting/Usage Instructions (Post-operative Care for Patients)
Post-operative care is critical for optimal recovery and patient outcome. Dr. Hutaif and his team will provide detailed, individualized instructions.
- Weight-Bearing: This is often the most important instruction. Depending on the fracture stability, bone quality, and patient factors, you may be advised:
- Non-Weight Bearing (NWB): No weight on the operated leg.
- Touch-Down Weight Bearing (TDWB): Only the toes touch the ground for balance, no significant weight.
- Partial Weight Bearing (PWB): A specific percentage of body weight is allowed (e.g., 25-50%), often with crutches or a walker.
- Weight Bearing As Tolerated (WBAT): Gradually increasing weight as comfort allows.
- Full Weight Bearing (FWB): Full weight on the leg.
- Early weight-bearing is a significant advantage of PFNA, often starting soon after surgery under supervision.
- Physical Therapy & Rehabilitation: This is paramount. A structured rehabilitation program will begin almost immediately after surgery, focusing on:
- Early Mobilization: Getting out of bed and moving helps prevent complications like DVT and pneumonia.
- Range of Motion Exercises: Restoring hip and knee flexibility.
- Strengthening Exercises: Rebuilding muscle strength in the leg and core.
- Gait Training: Learning to walk safely and efficiently.
- Pain Management: You will receive medication to manage post-operative pain. It's important to take these as prescribed and communicate your pain levels to your care team.
- Wound Care: Keep the incision site clean and dry. Instructions on dressing changes and signs of infection will be provided.
- Follow-up Appointments: Regular visits with Dr. Hutaif are essential to monitor healing progress through X-rays and clinical examination.
- Activity Restrictions: You will be advised to avoid certain movements (e.g., extreme hip rotation, high-impact activities) for a period to protect the healing bone.
- Expected Recovery Timeline: Recovery varies, but typically involves several months of dedicated rehabilitation. Full return to pre-injury activities can take 6-12 months.
3.4. Patient Outcome Improvements
PFNA has demonstrably improved patient outcomes for proximal femoral fractures:
- Reduced Morbidity and Mortality: By facilitating earlier mobilization, PFNA helps reduce complications associated with prolonged bed rest in elderly patients, such as pneumonia, pressure sores, and deep vein thrombosis (DVT).
- Faster Recovery and Rehabilitation: The stable fixation allows for quicker initiation of weight-bearing and physical therapy, leading to a faster return to functional independence.
- Lower Rates of Complications: Compared to some traditional methods, PFNA has shown lower rates of implant failure, non-union, and mal-union, particularly in challenging fracture patterns and osteoporotic bone.
- Improved Quality of Life: Patients often experience less pain and greater mobility post-surgery, allowing them to resume daily activities and maintain their independence.
- Minimally Invasive Benefits: Smaller incisions mean less blood loss, reduced infection risk, and often better cosmetic results.
4. Risks, Side Effects, or Contraindications
While PFNA is a highly successful procedure, like any surgical intervention, it carries potential risks and contraindications. Dr. Hutaif will discuss these thoroughly with you.
4.1. General Surgical Risks
- Infection: Despite sterile techniques, infection can occur at the surgical site.
- Bleeding: Blood loss during or after surgery.
- Nerve or Vascular Injury: Damage to nerves or blood vessels near the surgical site.
- Anesthesia Risks: Adverse reactions to anesthesia.
- Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE): Blood clots forming in the legs, which can travel to the lungs. Prophylactic measures are always taken.
4.2. PFNA-Specific Risks and Side Effects
- Malreduction or Non-Union: The fracture fragments may not heal correctly or at all.
- Delayed Union: The fracture takes longer than expected to heal.
- Implant Cut-out or Back-out: The helical blade or screws may migrate out of the bone, particularly in very osteoporotic bone or with poor initial reduction.
- Periprosthetic Fracture: A new fracture occurring around the implant, often due to trauma or stress concentrations.
- Leg Length Discrepancy: The operated leg may become slightly shorter or longer.
- Fat Embolism: Rare but serious complication where fat particles from the bone marrow enter the bloodstream.
- Implant Breakage: Extremely rare, but the nail or screws could break under excessive stress.
- Pain around the Implant: Some patients experience discomfort or irritation from the nail or screws, especially at the entry site or distal locking screws. This may necessitate implant removal after healing.
- Rotational Malalignment: While PFNA is designed for antirotation, improper surgical technique or highly unstable fractures can still lead to some rotational deformity.
4.3. Contraindications
- Active Infection: An ongoing infection in the hip or femur area is a absolute contraindication. It must be treated before considering surgery.
- Severe Comminution of the Femoral Head/Neck: If the femoral head or neck is too shattered to allow for stable fixation of the helical blade, PFNA may not be suitable.
- Insufficient Bone Stock: Extremely poor bone quality that cannot adequately hold the implant.
- Patient Unwillingness or Inability to Follow Post-operative Instructions: Successful recovery heavily relies on patient compliance with weight-bearing restrictions and physical therapy.
- Allergy to Implant Materials: While rare with titanium alloys, any known allergy to the implant materials would be a contraindication.
- Medullary Canal Obstruction: Prior implants or bone deformities that prevent proper nail insertion.
5. Expert Tips from Dr. Mohammed Hutaif
"As an orthopedic specialist, my primary goal is to restore function and improve the quality of life for my patients. PFNA is a powerful tool in achieving this, but successful outcomes are a partnership between the surgeon and the patient. Here are my key tips for anyone considering or undergoing PFNA surgery:
- Early Diagnosis and Intervention are Key: Don't delay seeking medical attention for a suspected fracture. Prompt diagnosis and surgical intervention for proximal femoral fractures significantly improve outcomes and reduce complications.
- Trust Your Surgical Team: We spend countless hours planning your surgery, selecting the right implant, and executing the procedure with precision. Have confidence in our expertise and ask any questions you have.
- Adherence to Rehabilitation is Non-Negotiable: The surgery is only half the battle. Your commitment to physical therapy, weight-bearing restrictions, and home exercises is absolutely critical for regaining strength, mobility, and preventing re-injury. Think of your physical therapist as your coach.
- Manage Expectations Realistically: Recovery from a major fracture takes time. While PFNA allows for early mobilization, full recovery can take many months. Celebrate small victories, but understand that patience and persistence are your greatest allies.
- Prioritize Bone Health: Many proximal femoral fractures are linked to osteoporosis. Discuss bone density screening and treatment options with me. Adequate calcium and Vitamin D intake, along with regular weight-bearing exercise (once cleared), are vital for long-term bone health.
- Communicate Openly: If you experience unexpected pain, swelling, fever, or any concerns, contact my office immediately. Open communication ensures that any potential issues are addressed promptly.
- Lifestyle Modifications: Consider modifications to your home environment to prevent falls. Remove tripping hazards, ensure adequate lighting, and use assistive devices as recommended.
- Stay Hydrated and Maintain a Healthy Diet: Good nutrition is essential for wound healing and bone regeneration. Your body needs fuel to recover."
6. Massive FAQ Section
Q1: How long does the PFNA surgery typically take?
A1: The actual surgical time for PFNA can vary depending on the complexity of the fracture, the patient's anatomy, and the surgeon's experience. Generally, the procedure takes between 1 to 2 hours. This does not include preparation time (anesthesia, positioning) or recovery room time. Dr. Hutaif will provide a more specific estimate based on your individual case during pre-operative discussions.
Q2: How long will I stay in the hospital after PFNA surgery?
A2: Most patients stay in the hospital for approximately 3 to 7 days after PFNA surgery. The length of stay depends on several factors, including your overall health, the stability of the fracture, how quickly you can mobilize, and your pain control. The goal is to ensure you are safe and comfortable enough to be discharged, often to a rehabilitation facility or home with outpatient physical therapy.
Q3: When can I put weight on my leg after PFNA?
A3: One of the significant advantages of PFNA is that it often allows for early weight-bearing. Depending on the fracture pattern, bone quality, and stability of the fixation achieved during surgery, Dr. Hutaif may allow touch-down weight bearing (TDWB) or partial weight bearing (PWB) almost immediately or within a few days post-surgery. Full weight bearing (FWB) is typically progressive and guided by your physical therapist and surgeon, often achieved over several weeks to months.
Q4: Will the PFNA implant need to be removed?
A4: In most cases, the PFNA implant is designed to be a permanent fixture and does not need to be removed unless complications arise. Reasons for removal might include persistent pain or irritation from the implant (e.g., at the entry site or distal screws), infection, or very rarely, implant failure after the fracture has healed. Removal surgery is typically less involved than the initial implantation, but it is a separate procedure. Dr. Hutaif will discuss the pros and cons of implant removal if it becomes a consideration.
Q5: What kind of pain can I expect after PFNA surgery, and how will it be managed?
A5: You can expect moderate to severe pain immediately after surgery, which will gradually decrease over days and weeks. Your pain management plan will be tailored to your needs and may include intravenous (IV) pain medications initially, followed by oral pain medications (opioids, NSAIDs, acetaminophen) as you recover. Nerve blocks may also be used to provide regional pain relief. It's crucial to communicate your pain levels to your healthcare team so they can adjust your medication effectively.
Q6: How long is the full recovery period after PFNA surgery?
A6: Full recovery from a proximal femoral fracture treated with PFNA is a gradual process. While you may be able to walk with assistance within days or weeks, achieving full strength, mobility, and returning to most pre-injury activities can take anywhere from 6 to 12 months, or sometimes longer. The recovery timeline is highly individual and depends on factors like age, overall health, fracture severity, and adherence to rehabilitation.
Q7: Can I resume all my normal activities, including sports, after PFNA?
A7: The goal of PFNA is to help you return to your pre-injury activity levels as much as possible. However, the extent to which you can resume all normal activities, especially high-impact sports, will depend on your individual recovery, the specific fracture, and Dr. Hutaif's recommendations. Low-impact activities like swimming, cycling, and walking are often encouraged relatively early. High-impact sports or activities involving significant twisting or heavy lifting may be restricted or modified long-term.
Q8: What are the signs of complications I should watch for after PFNA surgery?
A8: It's vital to be aware of potential signs of complications. Contact Dr. Hutaif's office immediately if you experience:
* Increasing pain that is not relieved by medication.
* Fever (above 101°F or 38.3°C) or chills.
* Redness, warmth, increased swelling, or discharge from the incision site.
* Numbness, tingling, or weakness in your foot or toes.
* Sudden, severe pain in your leg or hip, especially with weight-bearing.
* Calf pain, swelling, or tenderness (signs of DVT).
* Shortness of breath or chest pain (signs of PE).
Q9: Is PFNA suitable for all types of femur fractures?
A9: No, PFNA is specifically designed and indicated for certain types of proximal femoral fractures, primarily intertrochanteric and subtrochanteric fractures. It is not typically used for fractures of the femoral shaft (mid-thigh) or for isolated femoral neck fractures that may require different implants or even hip replacement. Dr. Hutaif will determine the most appropriate treatment based on the specific location and pattern of your fracture.
Q10: What is the success rate of PFNA in treating proximal femoral fractures?
A10: PFNA boasts a very high success rate in appropriately selected patients, often exceeding 90-95% for achieving fracture union and good functional outcomes. Success is measured by fracture healing, restoration of function, reduction of pain, and return to activity. Factors influencing success include the initial fracture pattern, bone quality, surgical technique, and patient compliance with post-operative care.
Q11: How does PFNA differ from a total hip replacement?
A11: PFNA and total hip replacement (arthroplasty) are distinct procedures for different indications. PFNA is a fracture fixation procedure designed to stabilize and allow your own bone to heal after a break, preserving your natural hip joint. Total hip replacement, on the other hand, is a joint replacement procedure where the damaged bone and cartilage of the hip joint are removed and replaced with artificial components. Hip replacement is typically indicated for severe arthritis or certain types of femoral neck fractures where the blood supply to the femoral head is compromised, making healing unlikely.
Q12: Can I go through airport security with a PFNA implant?
A12: Yes, you can go through airport security with a PFNA implant. As the implant is made of metal (titanium alloy), it will likely trigger metal detectors. It's advisable to inform security personnel about your implant beforehand. You may carry a letter from Dr. Hutaif confirming the presence of the implant, though it is often not strictly necessary. The implant will not interfere with electronic devices or cause any harm.
Conclusion
PFNA represents a pinnacle in modern orthopedic trauma care, offering patients with proximal femoral fractures a pathway to effective healing, reduced complications, and improved functional recovery. Dr. Mohammed Hutaif and his team are committed to leveraging such advanced techniques to ensure the best possible outcomes for every patient. We encourage you to discuss any questions or concerns you may have about your specific condition and treatment plan with us directly.