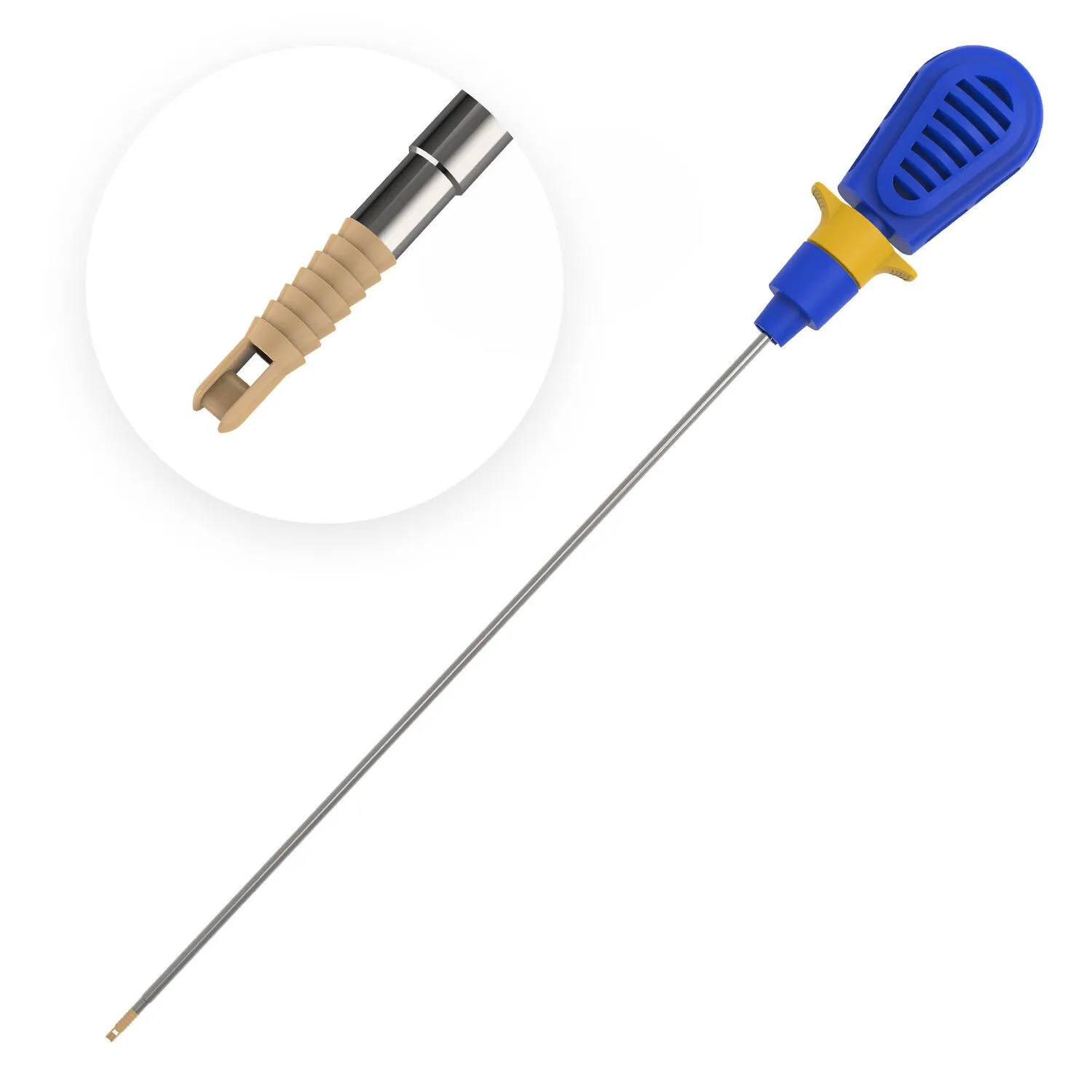
PEEK Suture Anchors (2.5mm - 6.5mm): Revolutionizing Orthopedic Fixation
Welcome to an in-depth guide on PEEK Suture Anchors, a cornerstone technology in modern orthopedic surgery. As an expert medical resource, this guide aims to provide comprehensive, authoritative, and easy-to-understand information about these advanced implants. While this content offers valuable insights, it is intended for patient education only and should not be considered medical advice. Always consult with a qualified healthcare professional for personalized medical guidance.
1. Comprehensive Introduction & Overview
In the realm of orthopedic surgery, the ability to securely reattach soft tissues—such as tendons and ligaments—to bone is paramount for successful patient recovery. PEEK Suture Anchors represent a significant advancement in achieving this crucial fixation. PEEK, an acronym for Polyetheretherketone, is a high-performance polymer renowned for its exceptional properties. These anchors, available in a versatile range of sizes from 2.5mm to 6.5mm, offer orthopedic surgeons a reliable and robust solution for a multitude of reconstructive procedures.
The introduction of PEEK technology has revolutionized how surgeons approach soft tissue repair, moving beyond traditional methods to offer enhanced strength, biocompatibility, and imaging compatibility. Their design allows for firm engagement with bone, providing a stable platform from which sutures can secure damaged tissues, facilitating the body's natural healing process. This guide will delve into the intricate details of their design, diverse applications, biomechanical advantages, and the profound impact they have on patient outcomes.
2. Deep-dive into Technical Specifications / Mechanisms
2.1 Design and Materials: The PEEK Advantage
PEEK suture anchors are engineered with precision, leveraging the unique characteristics of Polyetheretherketone.
* What is PEEK? PEEK is a semi-crystalline thermoplastic with a remarkable combination of properties that make it ideal for medical implants:
* Biocompatibility: PEEK is highly inert, meaning it does not react adversely with biological tissue, minimizing the risk of adverse reactions or inflammation.
* High Strength-to-Weight Ratio: It possesses mechanical properties similar to cortical bone, providing robust fixation without excessive bulk.
* Radiolucency: Unlike metal implants, PEEK is radiolucent, meaning it does not obscure X-ray images. This allows for clearer post-operative imaging, enabling surgeons to better visualize bone healing and tissue integration without artifact interference.
* Chemical Resistance: It is resistant to degradation by bodily fluids, ensuring long-term stability within the body.
* Sterilizability: PEEK can withstand various sterilization methods without degradation, ensuring patient safety.
* Anchor Design Variations:
* Threaded Anchors: Most PEEK anchors feature a threaded design, similar to a screw, which allows them to be securely screwed into a pre-drilled pilot hole in the bone. This provides excellent pull-out strength.
* Barbed Anchors: Some designs incorporate barbs or fins to enhance initial fixation and resistance to dislodgement.
* Cannulated vs. Solid: Cannulated anchors have a hollow core, sometimes allowing for easier insertion over a guide wire, while solid anchors offer maximum material strength.
* Self-Tapping Features: Many anchors are designed with self-tapping threads, simplifying the insertion process by eliminating the need for a separate tapping step after drilling.
* Size Range (2.5mm - 6.5mm): The availability of PEEK anchors in this broad size spectrum allows for tailored solutions for various anatomical sites and tissue repair needs:
* Smaller Anchors (2.5mm - 3.5mm): Ideal for smaller joints or delicate tissue repairs, such as in the wrist, ankle, or for glenoid labrum repairs in the shoulder.
* Medium Anchors (3.5mm - 4.5mm): Commonly used for rotator cuff repairs, biceps tenodesis, and MPFL reconstructions.
* Larger Anchors (5.0mm - 6.5mm): Employed in areas requiring maximum pull-out strength, such as large rotator cuff tears, Achilles tendon repairs, or in areas with softer bone.
* Suture Attachment Mechanisms: PEEK anchors are designed to securely hold sutures. This can involve:
* Eyelets: A closed loop or eyelet through which sutures are pre-loaded or threaded during surgery.
* Open Eyelets/Loops: Designs that allow for easier suture loading.
* Pre-loaded Sutures: Many anchors come with high-strength sutures already attached, streamlining the surgical procedure.
2.2 Mechanism of Action
The primary function of a PEEK suture anchor is to provide a robust point of fixation in bone, from which sutures can then be used to secure soft tissue.
1. Bone Preparation: A small pilot hole is precisely drilled into the bone at the desired anatomical location.
2. Anchor Insertion: The PEEK anchor, often pre-loaded with sutures, is then carefully inserted into the pilot hole. Its threaded design ensures a tight, secure fit within the bone.
3. Tissue Capture: Once the anchor is firmly seated, the attached sutures are passed through the torn or detached soft tissue (e.g., rotator cuff tendon).
4. Tissue Compression: The sutures are then tensioned and tied, bringing the soft tissue into direct apposition with the bone. This compression is crucial for promoting biological healing and reattachment.
5. Mechanical Fixation: The anchor provides immediate mechanical stability, allowing the healing process to begin without excessive strain on the repaired tissue.
2.3 Biomechanics
PEEK suture anchors offer significant biomechanical advantages:
* Initial Fixation Strength: PEEK's high strength and the anchor's threaded design provide excellent initial pull-out strength, crucial for immediate post-operative stability.
* Cyclic Loading Performance: They demonstrate superior resistance to cyclic loading (repeated stress), which is important as patients begin rehabilitation and controlled movement.
* Load Sharing: The anchor system effectively transfers load from the healing tissue to the robust bone interface, protecting the repair during the critical early healing phase.
* Stiffness and Strength: PEEK's mechanical properties are closer to cortical bone than some other synthetic materials, offering a good balance of stiffness and flexibility, reducing stress shielding effects often seen with much stiffer metal implants.
* Comparison to Other Materials:
* Metal Anchors: While strong, metal anchors are radiopaque, hindering post-operative imaging. PEEK offers comparable strength with imaging benefits.
* Bioabsorbable Anchors: These anchors gradually dissolve over time, which can be beneficial in some cases, but they may have lower initial strength and can sometimes induce inflammatory responses or leave cysts. PEEK provides permanent, stable fixation without degradation.
3. Extensive Clinical Indications & Usage
PEEK suture anchors are versatile tools used across a broad spectrum of orthopedic procedures. Their application is typically performed arthroscopically (minimally invasive) or through small open incisions.
3.1 Shoulder Surgery
- Rotator Cuff Repair: A primary application, used to reattach torn supraspinatus, infraspinatus, subscapularis, or teres minor tendons to the humeral head.
- Labral Repair: Essential for stabilizing the glenoid labrum in cases of Bankart lesions (anterior instability), SLAP lesions (superior labrum anterior to posterior), or other labral tears.
- Biceps Tenodesis: Used to secure the long head of the biceps tendon to the humerus, often for pain relief or instability.
- Capsular Shift/Plication: To tighten loose shoulder capsular tissue in cases of shoulder instability.
3.2 Knee Surgery
- ACL/PCL Reconstruction: While grafts are used for the main reconstruction, PEEK anchors can be used for secondary fixation of soft tissue grafts or to repair associated meniscal/capsular injuries.
- MPFL Reconstruction: To reconstruct the Medial Patellofemoral Ligament, stabilizing the kneecap.
- Collateral Ligament Repair: For reattaching torn Medial or Lateral Collateral Ligaments to bone.
3.3 Hip Surgery
- Labral Repair: Similar to the shoulder, PEEK anchors are used to reattach the acetabular labrum in hip arthroscopy, addressing pain and instability.
- Capsular Repair/Plication: To address hip capsular laxity.
3.4 Foot & Ankle Surgery
- Achilles Tendon Repair: For reattaching the Achilles tendon to the calcaneus (heel bone) after a rupture.
- Lateral Ankle Ligament Reconstruction (Brostrom Repair): To stabilize the ankle by reattaching the ATFL and CFL ligaments to the fibula.
- Midfoot/Forefoot Ligament Repairs: For various ligamentous injuries in the foot.
3.5 Elbow & Wrist Surgery
- UCL Reconstruction (Tommy John Surgery): Used to reconstruct the Ulnar Collateral Ligament in the elbow, common in overhead athletes.
- Lateral Epicondylitis Repair (Tennis Elbow): To reattach extensor tendons to the lateral epicondyle.
- TFCC Repair (Triangular Fibrocartilage Complex): For stabilizing injuries within the wrist.
3.6 Fitting/Usage Instructions (General Principles for Surgeons - simplified for patients)
- Pre-operative Planning: Careful assessment of the injury, bone quality, and appropriate anchor size selection.
- Pilot Hole Creation: Using specialized drills to create a precise hole in the bone, matching the anchor's diameter.
- Anchor Insertion: The anchor is carefully inserted into the pilot hole, either by hand, with an impactor, or by screwing it in, ensuring full engagement with the bone.
- Suture Management: The pre-loaded sutures are then passed through the soft tissue using specialized instruments.
- Tensioning and Knot Tying: Sutures are tensioned to bring the tissue to bone and secured with appropriate surgical knots.
- Post-operative Care: Crucial for success, involving immobilization, pain management, and a structured rehabilitation program.
3.7 Maintenance/Sterilization Protocols (Relevant to product handling, not the implant itself after insertion)
PEEK suture anchors are supplied in sterile packaging and are single-use devices.
* Sterilization: Manufacturers sterilize PEEK anchors using validated methods, typically gamma irradiation or ethylene oxide, ensuring they are ready for immediate use in the operating room.
* Handling: Implants must be handled with sterile technique at all times. Any anchor with compromised packaging or past its expiration date must be discarded. The delivery system (inserter) associated with the anchor is also sterile and designed for single use.
* Storage: Anchors should be stored in their original, unopened packaging in a cool, dry place away from direct sunlight, as per manufacturer's instructions.
4. Risks, Side Effects, or Contraindications
While PEEK suture anchors are generally safe and effective, like any surgical procedure involving implants, there are potential risks and considerations:
4.1 General Surgical Risks
- Infection: Risk associated with any surgery, though minimized with sterile technique and antibiotics.
- Bleeding/Hematoma: Accumulation of blood near the surgical site.
- Nerve or Vascular Damage: Potential injury to surrounding nerves or blood vessels.
- Anesthesia Risks: Adverse reactions to anesthetic agents.
4.2 Anchor-Specific Risks
- Anchor Pull-out or Loosening: Though rare due to strong fixation, the anchor can potentially dislodge from the bone, especially with inadequate bone quality or excessive early stress.
- Suture Breakage or Cut-out: The sutures themselves can break, or they might cut through the soft tissue, leading to failure of the repair.
- Implant Migration: The anchor could potentially move from its intended position.
- Bone Fracture During Insertion: Very rare, but aggressive or improper insertion technique can potentially lead to a localized bone fracture.
- Pain or Irritation: Patients may occasionally experience localized pain or irritation at the anchor site.
- Re-tear of Repaired Tissue: Despite successful fixation, the repaired tissue can re-tear, especially if post-operative rehabilitation protocols are not followed.
- Adverse Reaction to Implant Material: Extremely rare with PEEK due to its inert nature, but theoretical allergic reactions or tissue responses are possible.
4.3 Contraindications
- Active Infection: Surgery should not proceed in the presence of an active infection in the surgical area or elsewhere in the body.
- Insufficient Bone Quality/Density: Patients with severe osteoporosis or very poor bone quality may not be suitable candidates, as the anchor may not achieve adequate purchase.
- Known Allergy to PEEK: While exceptionally rare, a documented allergy would contraindicate its use.
- Patient's General Health: Certain systemic medical conditions (e.g., uncontrolled diabetes, severe cardiovascular disease) may preclude surgical intervention.
- Inability to Comply with Post-operative Rehabilitation: Successful outcomes heavily rely on patient adherence to post-operative instructions and rehabilitation.
5. Expert Tips from Dr. Mohammed Hutaif
"As an orthopedic surgeon, I've witnessed firsthand the transformative impact of PEEK Suture Anchors in restoring function and alleviating pain for my patients. The consistent strength and reliable fixation they offer are invaluable. Here are my key insights for optimal outcomes:
- Patient Selection is Paramount: Not every patient or every tear is the same. Careful pre-operative assessment, including detailed imaging and understanding bone quality, is crucial to selecting the right anchor size and type for the specific repair.
- Precision in Technique: The success of PEEK anchors lies heavily in meticulous surgical technique. This includes creating the ideal pilot hole, ensuring proper insertion angle, and achieving optimal suture tensioning to maximize tissue-to-bone contact.
- Rehabilitation is Non-Negotiable: The surgical repair is only half the journey. A well-structured, progressive post-operative rehabilitation program is absolutely critical. Patient adherence to this program, including activity restrictions and guided exercises, directly impacts long-term success and prevents re-injury.
- Educate Your Patients: Empowering patients with a clear understanding of their procedure, the role of the PEEK anchor, and what to expect during their recovery journey builds confidence and encourages compliance.
- Long-Term Stability: PEEK anchors provide permanent, stable fixation without degradation, offering patients a lasting solution. This gives both the surgeon and the patient confidence in the durability of the repair, allowing for a more robust return to activity over time.
- Imaging Clarity: One of the unsung heroes of PEEK is its radiolucency. This allows for superior post-operative imaging, enabling us to clearly visualize bone healing and the state of the repair without the artifacts that metal implants often create."
6. Massive FAQ Section
Q1: What is a suture anchor and why is it used?
A: A suture anchor is a small, specialized implant used in orthopedic surgery to reattach soft tissues (like tendons or ligaments) to bone. It acts as a fixed point in the bone, from which sutures can be passed through the damaged tissue and then tied, pulling the tissue back into contact with the bone to facilitate healing.
Q2: What is PEEK and why is it used in suture anchors?
A: PEEK stands for Polyetheretherketone. It's a high-performance, biocompatible polymer used in medical implants because it's strong, durable, resistant to body fluids, and most importantly, radiolucent (doesn't show up on X-rays). This radiolucency allows doctors to get clear images of the healing bone and tissue without interference from the implant.
Q3: Are PEEK anchors permanent implants? Do they dissolve?
A: Yes, PEEK anchors are permanent implants. Unlike bioabsorbable anchors, PEEK anchors do not dissolve or degrade over time. They remain in the bone permanently to provide long-term fixation for the repaired tissue.
Q4: Will PEEK anchors set off metal detectors or affect airport security?
A: No. Since PEEK is a plastic (polymer) material and not metal, PEEK suture anchors will not trigger metal detectors at airports or other security checkpoints.
Q5: Can PEEK anchors be removed?
A: PEEK anchors are generally intended to be permanent and are not typically removed unless there's a specific complication, such as persistent irritation or infection. Removal would require another surgical procedure.
Q6: How long does it take to recover after surgery with PEEK anchors?
A: Recovery time varies significantly depending on the specific procedure, the severity of the injury, and individual patient factors. Generally, it involves an initial period of immobilization (weeks), followed by a structured physical therapy program that can last several months. Full recovery and return to strenuous activities can take anywhere from 6 months to a year or more.
Q7: What is the difference between PEEK and bioabsorbable anchors?
A: The main difference is permanence. PEEK anchors are permanent and provide lasting mechanical support. Bioabsorbable anchors are designed to gradually dissolve in the body over several months to a couple of years, eventually being replaced by bone or soft tissue. While bioabsorbable anchors eliminate the presence of a permanent implant, they may have different initial strength profiles and can sometimes elicit a localized tissue response during degradation.
Q8: Are there different sizes of PEEK anchors? Why is this important?
A: Yes, PEEK suture anchors come in a range of sizes, typically from 2.5mm to 6.5mm in diameter. This versatility is crucial because it allows the surgeon to select the most appropriate anchor size for different anatomical locations (e.g., smaller anchors for delicate wrist bones, larger for a robust rotator cuff repair) and varying bone qualities, optimizing fixation strength and minimizing bone removal.
Q9: What are the main benefits of using PEEK anchors for patients?
A: Key benefits for patients include:
* Strong and reliable fixation: Promotes optimal healing.
* Biocompatibility: Low risk of adverse reactions.
* Clear imaging: Allows for better post-operative assessment without X-ray interference.
* Durability: Provides long-term structural support.
* Reduced need for revision: Their strength and permanence can lower the chances of needing repeat surgery due to anchor failure.
Q10: Is surgery involving PEEK anchors typically performed arthroscopically?
A: Many procedures involving PEEK suture anchors, especially in joints like the shoulder, knee, and hip, are indeed performed using arthroscopic (minimally invasive) techniques. Arthroscopy involves small incisions and the use of a camera, leading to less pain, smaller scars, and often faster initial recovery compared to traditional open surgery. However, some complex repairs may still require an open approach.
Q11: Will I feel the anchor in my body after surgery?
A: Most patients do not feel the PEEK anchor once it's properly integrated into the bone. PEEK is very smooth and inert. If an anchor is placed very superficially or if there's significant inflammation, some patients might occasionally report a sensation or mild discomfort, but this is uncommon.
Q12: Can I undergo an MRI with a PEEK anchor?
A: Yes, PEEK material is non-metallic and non-magnetic, making PEEK suture anchors fully compatible with Magnetic Resonance Imaging (MRI). This is a significant advantage, as it allows for clear and detailed follow-up imaging of the soft tissues and bone without the artifacts or safety concerns associated with metallic implants.
Disclaimer: This information is for educational purposes only and is not intended as medical advice. Always consult with a qualified healthcare professional for diagnosis and treatment.