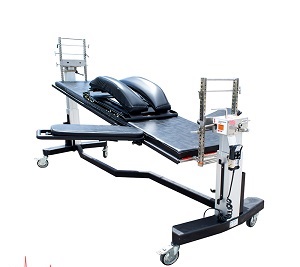
The Jackson Spinal Table System: Revolutionizing Spine Surgery
Comprehensive Introduction & Overview
In the realm of modern spinal surgery, precision, safety, and optimal surgical access are paramount. The Jackson Spinal Table System stands as a cornerstone technology, representing a significant advancement over conventional operating tables, specifically designed to meet the complex demands of various spinal procedures. Developed by Mizuho OSI, this state-of-the-art platform is engineered to provide surgeons with unparalleled flexibility in patient positioning, critical for achieving superior outcomes in intricate spinal operations.
The Jackson table is not just an operating table; it is a sophisticated system that integrates modular components, advanced materials, and ergonomic design principles. Its primary purpose is to facilitate optimal patient positioning, which directly impacts surgical exposure, reduction of blood loss, and minimization of intraoperative complications. By allowing for precise adjustments and maintaining physiological spinal alignment, the system empowers surgical teams to perform challenging procedures with enhanced confidence and control. This guide aims to provide patients with a comprehensive understanding of this remarkable technology, explaining its components, applications, and the profound benefits it offers in modern spinal care.
Deep-Dive into Technical Specifications & Mechanisms
The Jackson Spinal Table System's ingenuity lies in its meticulous design, choice of materials, and biomechanical principles that guide its functionality.
Design & Materials: Engineering for Excellence
The core of the Jackson system is its modularity and radiolucent construction:
- Modular Design: The system comprises interchangeable frames (e.g., Andrews Spinal Positioning Device, ProneView Protective Helmet and Mirror System, various bolsters, and pads) that can be configured to suit specific surgical approaches and patient anatomies. This adaptability ensures that the table can be customized for different spinal segments (cervical, thoracic, lumbar, sacral) and surgical positions (prone, lateral).
- Radiolucent Carbon Fiber Construction: A key differentiating feature is the extensive use of carbon fiber in its frame and components. Carbon fiber is highly radiolucent, meaning it allows X-rays and fluoroscopic imaging to pass through with minimal obstruction. This is crucial for intraoperative imaging, enabling surgeons to visualize spinal structures and instrument placement in real-time without having to reposition the patient or move metallic components that would otherwise obscure the view.
- Advanced Adjustability: The table offers multi-axis adjustability, including:
- Flexion and Extension: To optimize spinal lordosis or kyphosis, facilitating access to the posterior or anterior elements.
- Lateral Tilt: For side-bending, useful in scoliosis correction or lateral access procedures.
- Trendelenburg/Reverse Trendelenburg: For managing blood pressure or venous pooling.
- Height Adjustment: To provide ergonomic working conditions for the surgical team.
- Powered Mechanisms: Many Jackson systems feature powered controls, allowing for smooth, precise, and effortless adjustments during surgery, enhancing efficiency and patient safety.
Biomechanics & Patient Positioning Principles
The biomechanical principles behind the Jackson table are critical for patient safety and surgical efficacy:
- Optimized Spinal Alignment: The system is designed to maintain or correct the natural curvature of the spine (lordosis in the lumbar spine, kyphosis in the thoracic spine). Achieving the correct spinal alignment during prone positioning can significantly improve surgical exposure, reduce tension on neural structures, and facilitate easier hardware placement.
- Minimizing Pressure Points: Traditional flat operating tables can create excessive pressure on vulnerable areas, leading to nerve damage (e.g., brachial plexus injury, ulnar neuropathy) or pressure ulcers. The Jackson table's specialized bolsters and pads distribute pressure evenly, supporting the chest, pelvis, and limbs, thereby minimizing the risk of such complications. The open frame design, particularly for prone positions, allows the abdomen to hang freely, reducing intra-abdominal pressure.
- Improved Cardiopulmonary Function: By allowing the abdomen to hang freely in the prone position, the Jackson table reduces pressure on the inferior vena cava, which can otherwise impede venous return to the heart. This helps maintain stable hemodynamics, reduces epidural venous bleeding (leading to a clearer surgical field), and improves lung compliance and ventilation.
- Unobstructed Surgical Field: The open frame and radiolucent design provide ample space and clear access for the surgical team, intraoperative imaging equipment, and instrumentation, which is vital for complex, multi-level spinal procedures.
Extensive Clinical Indications & Usage
The versatility and advanced features of the Jackson Spinal Table System make it indispensable across a broad spectrum of spinal surgeries.
Primary Clinical Applications:
- Lumbar Fusion Procedures:
- Posterior Lumbar Interbody Fusion (PLIF) / Transforaminal Lumbar Interbody Fusion (TLIF): The table's ability to create a controlled lumbar lordosis is crucial for optimizing disc space distraction and achieving proper fusion alignment.
- Direct Lateral Interbody Fusion (DLIF)/Extreme Lateral Interbody Fusion (XLIF): While these often use a lateral decubitus position, specific configurations of the Jackson table can support these approaches, providing stability and fluoroscopic access.
- Spinal Deformity Correction:
- Scoliosis Correction: The table allows for precise positioning to facilitate vertebral column decancellation, rod contouring, and segmental correction, often involving multi-level fusions. Its stability is vital during complex osteotomies.
- Kyphosis Correction: Similar to scoliosis, the table aids in achieving the desired spinal profile correction.
- Minimally Invasive Spine Surgery (MISS):
- The radiolucent frame and precise positioning capabilities are perfectly suited for MISS techniques, where real-time fluoroscopic guidance is essential for small incisions and targeted instrumentation.
- Decompression Procedures:
- Laminectomy, Discectomy, Foraminotomy: The table provides excellent exposure and stability for these common procedures aimed at relieving nerve compression.
- Spinal Tumor Resection: The clear imaging capabilities and stable platform are critical for precise tumor removal and subsequent reconstruction.
- Spinal Trauma: In cases of vertebral fractures, the table assists in careful positioning to stabilize the spine and facilitate reconstructive surgery.
Usage & Fitting Instructions (General Principles for Patients):
While patients are not directly involved in the technical setup, understanding the process can alleviate concerns:
- Pre-operative Assessment: Before surgery, the surgical team meticulously plans the patient's positioning based on their anatomy, surgical needs, and co-morbidities.
- Anesthesia and Transfer: After induction of anesthesia, the patient is carefully transferred to the Jackson table by a trained team, ensuring spinal precautions are maintained if necessary.
- Secure Positioning: The patient is then meticulously positioned, often in a prone (face-down) position for posterior spinal surgeries. Specialized pads, bolsters, and supports are used to cradle the body, ensuring even pressure distribution and preventing nerve compression. The head is typically secured in a padded headrest, often with a mirror system (e.g., ProneView) for anesthesia staff to monitor the patient's face.
- Verification and Monitoring: Once positioned, the team verifies proper alignment, ensures airways are clear, and checks all pressure points. Throughout the surgery, the patient's vital signs and neurological status are continuously monitored.
Risks, Side Effects, or Contraindications
While the Jackson Spinal Table System significantly enhances safety and outcomes, it's important for patients to be aware of general risks associated with prolonged surgical positioning and specific equipment considerations.
General Risks Associated with Surgical Positioning:
- Pressure Injuries (Pressure Ulcers/Bedsores): Prolonged pressure on bony prominences can lead to skin breakdown, though the Jackson table's design aims to minimize this risk through pressure-relieving pads.
- Nerve Compression: Although rare with proper positioning, nerves can be susceptible to compression, leading to temporary or, in very rare cases, permanent numbness, tingling, or weakness. Common areas include the brachial plexus (shoulder/arm), ulnar nerve (elbow), and peroneal nerve (leg).
- Ocular Complications: In prone positions, direct pressure on the eyes can, in extremely rare instances, lead to vision loss. The use of specialized headrests and careful positioning protocols aims to prevent this.
- Cardiovascular and Respiratory Compromise: While the Jackson table is designed to improve cardiopulmonary function in prone, patients with severe pre-existing conditions might still be at higher risk.
- Compartment Syndrome: Extremely rare, but can occur if limbs are positioned improperly, leading to restricted blood flow.
Equipment-Specific Considerations:
- Equipment Malfunction: As with any medical device, there's a minimal risk of mechanical or electrical malfunction. However, these systems undergo rigorous maintenance and pre-operative checks.
- Improper Setup: The risks mentioned above are largely mitigated by the highly trained surgical and anesthesia teams who meticulously set up and monitor the patient on the table.
Contraindications (General, not exhaustive):
- Extreme Obesity: While the Jackson table can accommodate a wide range of patient sizes, extreme obesity might exceed weight limits or make safe positioning challenging.
- Severe Pre-existing Conditions: Certain severe cardiopulmonary diseases, uncontrolled hypertension, or specific spinal instabilities might make prone positioning or prolonged surgery on any table more risky. These are carefully evaluated pre-operatively.
- Allergies: Rare, but patients with known allergies to materials used in pads or components would need alternative solutions.
Expert Tips from Dr. Mohammed Hutaif
"As a spinal surgeon, the Jackson Spinal Table System is an invaluable tool that significantly elevates the standard of care we can offer our patients. My experience has shown that its precision, adaptability, and inherent safety features are critical for successful outcomes, especially in complex cases.
Here are my key insights regarding its use:
- Meticulous Pre-operative Planning: The journey to a successful surgery begins long before the patient enters the operating room. We meticulously plan the patient's positioning, considering their unique anatomy and the specific surgical goals. The Jackson table's modularity allows us to tailor the setup perfectly.
- Team Expertise is Paramount: While the technology is advanced, the skill and experience of the entire surgical and anesthesia team in patient positioning and monitoring are non-negotiable. Our team undergoes continuous training to ensure every patient is positioned optimally and safely.
- Facilitating Intraoperative Imaging: The radiolucent design of the Jackson table is a game-changer. It allows for seamless, high-quality intraoperative fluoroscopy and X-rays, providing real-time feedback on instrument placement and spinal alignment. This reduces surgical time and enhances accuracy, directly translating to better patient results.
- Reduced Complications, Improved Outcomes: By optimizing spinal alignment, minimizing pressure points, and improving cardiopulmonary dynamics, the Jackson table significantly reduces the risks of complications like nerve damage or excessive bleeding. This contributes to a smoother recovery and ultimately, better long-term outcomes for our patients.
- Patient Safety First: Every feature of the Jackson system, from its stable frame to its pressure-relieving pads, is designed with patient safety as the utmost priority. It allows us to focus on the intricate surgical task at hand, knowing that the patient is securely and physiologically supported."
Massive FAQ Section
Q1: What is the main advantage of the Jackson table over a standard operating table for spine surgery?
A1: The primary advantage lies in its specialized design for spinal procedures. Unlike standard tables, the Jackson system features a modular, open, and radiolucent frame that allows for optimal patient positioning (e.g., maintaining natural spinal curves, allowing the abdomen to hang free) and unobstructed intraoperative imaging. This leads to better surgical access, reduced blood loss, enhanced surgical precision, and minimized risks of pressure-related complications.
Q2: Is the Jackson table used for all types of spine surgery?
A2: While highly versatile, it is primarily used for complex posterior spinal surgeries, such as fusions, deformity corrections (scoliosis, kyphosis), tumor resections, and extensive decompressions. It's also excellent for minimally invasive spine surgeries due to its imaging capabilities. For purely anterior approaches (like some ALIFs), other specialized tables might be preferred, but its modularity allows for a wide range of applications.
Q3: How does the carbon fiber material help during surgery?
A3: Carbon fiber is uniquely radiolucent, meaning it's transparent to X-rays and fluoroscopy. This allows surgeons to take real-time images during surgery without having to move the patient or the table, or deal with artifacts caused by metallic components. This real-time imaging is crucial for accurate instrument placement, confirming spinal alignment, and ensuring the success of complex procedures.
Q4: How is patient safety ensured when using this table?
A4: Patient safety is paramount. The Jackson table ensures safety through:
1. Ergonomic Design: Specialized pads and bolsters distribute pressure evenly, preventing nerve damage and skin breakdown.
2. Stable Platform: Provides a secure and stable base, preventing unwanted patient movement.
3. Reduced Intra-abdominal Pressure: The open frame in prone position reduces pressure on internal organs and major blood vessels, improving cardiopulmonary function and reducing epidural bleeding.
4. Expert Team: Highly trained surgical and anesthesia teams meticulously position and monitor the patient throughout the procedure.
Q5: Can the table accommodate patients of all sizes?
A5: The Jackson Spinal Table System is designed to accommodate a broad range of patient sizes, from pediatric to bariatric, within specified weight limits. Its modular components allow for customization to fit individual patient anatomies, ensuring optimal and safe positioning for diverse body types.
Q6: What specific conditions benefit most from surgery on a Jackson table?
A6: Patients undergoing complex spinal fusions for degenerative conditions, severe scoliosis or kyphosis correction, tumor removal, or multi-level decompression procedures benefit significantly. Its ability to optimize spinal alignment and provide superior surgical access is particularly advantageous for these challenging cases.
Q7: How does the table help surgeons perform complex procedures?
A7: It helps in several ways:
* Optimal Exposure: Provides an unobstructed view and access to the surgical site.
* Precise Positioning: Allows for exact adjustment of spinal curvature (lordosis/kyphosis) to facilitate surgical goals.
* Real-time Imaging: Radiolucent components enable continuous fluoroscopic guidance, essential for accurate screw placement and deformity correction.
* Stability: A rigid platform minimizes patient movement during delicate maneuvers.
Q8: Are there any risks specifically associated with the table itself?
A8: While the Jackson table significantly reduces risks compared to traditional methods, potential risks, though rare and largely preventable with proper protocols, include pressure-related injuries (skin breakdown, nerve compression) if positioning is not meticulous, or, in extremely rare cases, equipment malfunction. These are mitigated by rigorous protocols, experienced staff, and regular maintenance.
Q9: What happens during patient positioning on the Jackson table?
A9: After anesthesia, a specialized team carefully transfers the patient to the table. They use specific pads and bolsters to support the body, ensuring the spine is aligned correctly, pressure points are relieved, and airways are clear. The head is often secured in a special headrest. This is a meticulous process, critical for patient safety and surgical success.
Q10: Does using this table improve recovery time for patients?
A10: While recovery time is influenced by many factors (patient health, type of surgery, post-operative care), the Jackson table contributes positively by facilitating a more precise and efficient surgery. Reduced intraoperative blood loss, minimized surgical trauma due to better access, and fewer intraoperative complications can indirectly lead to a smoother and potentially faster recovery.
Q11: How is the Jackson Spinal Table System maintained and sterilized?
A11: Maintenance and sterilization are critical for patient safety and equipment longevity.
* Cleaning: After each use, all surfaces and removable components are thoroughly cleaned with hospital-grade disinfectants, following strict infection control protocols.
* Sterilization: Reusable components that come into contact with the sterile surgical field are typically sterilized using methods like steam sterilization (autoclaving), in accordance with manufacturer guidelines and hospital policies.
* Regular Inspection: The system undergoes routine preventive maintenance checks by biomedical engineers to ensure all mechanical and electrical components are functioning correctly and safely.
Q12: What role does Dr. Hutaif's team play in utilizing this advanced technology?
A12: Dr. Hutaif's team plays a central role. From the initial pre-operative assessment and planning, where the optimal table configuration is determined, to the meticulous patient transfer and positioning, and continuous intraoperative monitoring, their expertise ensures the Jackson table is utilized to its full potential. Their commitment to patient safety and precision surgery, combined with the capabilities of the Jackson system, aims to deliver the best possible outcomes.
Disclaimer: This content is for informational purposes only and does not constitute medical advice. Please consult with a qualified healthcare professional for any medical concerns or before making any decisions related to your health or treatment.