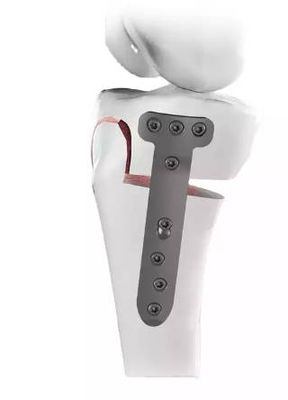
The High Tibial Osteotomy (HTO) Plate (TomoFix): A Comprehensive Guide to Advanced Knee Realignment
Introduction to High Tibial Osteotomy (HTO)
High Tibial Osteotomy (HTO) is a well-established surgical procedure designed to realign the lower limb, specifically targeting deformities in the knee joint. It is primarily performed to treat unicompartmental osteoarthritis (OA) of the knee, particularly when associated with varus malalignment (bow-leggedness), which places excessive stress on the medial compartment of the knee. By surgically altering the angle of the tibia (shin bone) just below the knee, HTO shifts the weight-bearing axis from the diseased, overloaded compartment to the healthier, less affected compartment. This offloading can significantly reduce pain, improve function, and potentially delay the need for total knee arthroplasty (TKA), especially in younger, active patients.
The success of HTO heavily relies on stable and robust internal fixation to maintain the achieved correction and facilitate bone healing. This is where advanced plating systems like the TomoFix HTO Plate come into play, providing the necessary mechanical stability for optimal patient outcomes.
Introducing the TomoFix HTO Plate System
The TomoFix HTO Plate, a leading solution in orthopedic surgery, represents the pinnacle of design and engineering for high tibial osteotomy fixation. Developed by DePuy Synthes (a Johnson & Johnson MedTech company), the TomoFix system is renowned for its anatomical pre-contouring, locking screw technology, and biomechanical stability, making it a preferred choice for surgeons worldwide. It is specifically engineered to provide rigid fixation for opening wedge osteotomies of the proximal tibia, ensuring precise correction and promoting an environment conducive to bone union.
Key Advantages of the TomoFix System:
- Anatomical Pre-contouring: Designed to perfectly fit the medial or lateral proximal tibia, minimizing the need for intraoperative bending.
- Locking Technology: Provides angular stability, creating a fixed-angle construct that enhances stability, especially in osteoporotic bone.
- Minimally Invasive Potential: Low-profile design and specific instrumentation can facilitate less extensive soft tissue dissection.
- Early Mobilization: The rigid fixation allows for earlier weight-bearing and rehabilitation, accelerating patient recovery.
- Versatility: Available in various sizes and configurations to accommodate different patient anatomies and osteotomy gaps.
Deep Dive into Design, Materials, and Biomechanics
The TomoFix HTO Plate's superior performance stems from its meticulous design, choice of materials, and adherence to sound biomechanical principles.
Advanced Plate Design and Materials
The TomoFix plate is crafted from high-quality titanium alloy (Ti6Al4V), a material widely recognized in orthopedics for its excellent biocompatibility, high strength-to-weight ratio, and corrosion resistance. These properties ensure the implant is well-tolerated by the body and can withstand the physiological stresses of the lower limb.
Key Design Features:
- Material: Titanium alloy (Ti6Al4V) for biocompatibility, strength, and MRI compatibility.
- Anatomical Pre-contouring: Each plate is precisely shaped to match the complex anatomy of the proximal medial or lateral tibia. This pre-contouring reduces the need for intraoperative plate bending, saving surgical time and minimizing the risk of material fatigue or stress risers from improper bending.
- Low-Profile Design: The plate's slim profile minimizes soft tissue irritation, which is crucial for patient comfort and reducing the risk of implant prominence post-surgery.
- Locking Screw Technology: A cornerstone of the TomoFix system. The plate features threaded screw holes that mate with threaded locking screws. This creates a fixed-angle construct, where the screws "lock" into the plate, providing angular stability independent of bone quality. This is particularly advantageous in osteoporotic bone or when a large osteotomy gap is created.
- Combi-Holes: Many TomoFix plates incorporate "Combi-holes," which allow for the use of both locking screws (for fixed-angle stability) and cortical screws (for compression and lag screw effect). This versatility enables the surgeon to customize fixation based on the specific needs of the osteotomy.
- Plate Geometry: TomoFix plates are available in various lengths and configurations (e.g., standard, small, long) to accommodate different patient sizes and the required length of fixation. Specific designs are optimized for opening wedge osteotomies, providing robust support for the created gap.
- Strategic Perforations/Slots: Some designs incorporate features that allow for the placement of bone graft material or facilitate biological incorporation, crucial for encouraging bone union across the osteotomy site.
Table: TomoFix Plate Design Features
| Feature | Description | Benefit |
|---|---|---|
| Material | Titanium Alloy (Ti6Al4V) | Biocompatible, high strength, corrosion resistant, MRI compatible. |
| Pre-contouring | Anatomically shaped for proximal tibia | Minimizes intraoperative bending, ensures optimal fit, reduces surgical time. |
| Low Profile | Slim design | Reduces soft tissue irritation, improves patient comfort. |
| Locking Screws | Threaded screws lock into plate | Provides angular stability, fixed-angle construct, robust fixation, ideal for osteoporotic bone. |
| Combi-Holes | Accommodates both locking and cortical screws | Versatile fixation options (compression + angular stability). |
| Plate Geometry | Various lengths and configurations | Adaptable to diverse patient anatomies and osteotomy gaps. |
| Bone Graft Slots | Designed to facilitate bone graft placement | Promotes bone healing and integration across the osteotomy site. |
Biomechanical Principles of TomoFix Fixation
The biomechanical efficacy of the TomoFix plate is rooted in its ability to create a stable, fixed-angle construct, which is paramount for successful osteotomy healing.
- Fixed-Angle Construct Stability: Unlike conventional plating systems where screws purchase only in the bone, locking screws in the TomoFix system create a "fixed-angle" or "internal fixator" construct. This means the screws are rigidly fixed to the plate, and together they act as a single unit. This provides superior resistance to bending, torsion, and shear forces, even in comminuted osteotomies or poor bone quality.
- Load Sharing vs. Load Bearing: The TomoFix system is designed to provide stable fixation while allowing for some load sharing with the healing bone. While it initially bears a significant portion of the mechanical load, its controlled stiffness aims to promote secondary bone healing through callus formation, rather than complete stress shielding, which can inhibit bone formation.
- Optimized Stiffness and Strength: The plate's design balances stiffness to provide immediate stability with enough flexibility to allow for physiological stresses that stimulate bone growth. This optimized mechanical environment is critical for preventing nonunion and promoting timely consolidation of the osteotomy.
- Contribution to Early Mobilization: The robust stability provided by the TomoFix system allows for earlier controlled weight-bearing and initiation of physical therapy. This reduces the risks associated with prolonged immobilization (e.g., joint stiffness, muscle atrophy, DVT) and significantly contributes to faster functional recovery and improved patient satisfaction.
- Prevention of Loss of Correction: The fixed-angle construct is highly resistant to forces that could lead to a loss of the achieved angular correction, ensuring the long-term efficacy of the osteotomy.
Extensive Clinical Indications and Surgical Applications
The TomoFix HTO Plate is indicated for a range of conditions where precise and stable correction of proximal tibial alignment is required.
Primary Indications for HTO with TomoFix
- Medial Compartment Osteoarthritis with Varus Malalignment: This is the most common indication. HTO shifts the weight-bearing axis laterally, offloading the degenerated medial compartment and reducing pain.
- Osteochondral Defects: In conjunction with procedures like microfracture or cartilage transplantation, HTO can optimize the mechanical environment for healing by correcting underlying malalignment.
- Patellofemoral Instability: In cases where patellofemoral instability is exacerbated by tibial malalignment, HTO can help normalize the tracking of the patella.
- Post-Traumatic Deformities: Correction of malunion or nonunion following fractures of the proximal tibia that result in angular deformity.
- Younger, Active Patients: HTO is often preferred over total knee arthroplasty in younger individuals (typically under 60-65) with unicompartmental disease, as it preserves the native joint and allows for a more active lifestyle.
- Lateral Compartment Osteoarthritis with Valgus Malalignment: While less common for HTO (distal femoral osteotomy is often preferred for valgus correction), specific TomoFix plates can be used for lateral opening wedge osteotomies of the proximal tibia if indicated.
Detailed Surgical Technique and Usage Instructions
The surgical procedure for HTO with the TomoFix plate requires meticulous planning and execution.
- Preoperative Planning:
- Radiographic Assessment: Full-length weight-bearing anteroposterior (AP) and lateral X-rays of the entire lower limb are crucial to accurately determine the mechanical axis deviation.
- Templating: Digital or traditional templating helps determine the precise osteotomy angle, the size of the opening wedge, and the appropriate TomoFix plate length and screw positions.
- Deformity Analysis: Measurements such as Mechanical Axis Deviation (MAD), Mechanical Lateral Distal Femoral Angle (mLDFA), and Medial Proximal Tibial Angle (MPTA) guide the correction.
- Patient Positioning and Approach:
- The patient is typically positioned supine. A tourniquet may be used.
- A medial incision is made over the proximal tibia, carefully dissecting through subcutaneous tissue and fascia. The superficial medial collateral ligament (sMCL) is often released to facilitate correction.
- Osteotomy Creation:
- Guide wires are inserted under fluoroscopic guidance to define the osteotomy plane, typically starting just distal to the articular surface and extending obliquely downwards.
- A specialized oscillating saw is used to create the osteotomy, leaving a small medial hinge intact to control the opening.
- Correction and Gap Creation:
- Specialized osteotomy distractors or wedges are used to gradually open the osteotomy gap to the pre-planned correction angle. Intraoperative fluoroscopy confirms the desired mechanical axis shift.
- The size of the opening wedge is determined by the required correction.
- Plate Selection and Placement:
- The appropriate TomoFix plate (e.g., Medial High Tibial Plate) is selected based on preoperative templating and intraoperative assessment.
- The plate is positioned on the proximal tibia, ensuring it lies flat and respects the anatomical contours. Temporary fixation with K-wires or clamps may be used.
- Screw Insertion:
- Distal Screws: Often, cortical screws are inserted distally first to provide initial compression of the plate to the bone.
- Proximal Locking Screws: Locking screws are then inserted through the threaded holes in the plate into the proximal fragment. These screws engage the plate, creating the fixed-angle construct. The sequence and number of locking screws are critical for stability.
- Bone Graft: If a large opening wedge is created (typically >10-12mm), bone graft (autograft, allograft, or synthetic bone substitute) is often packed into the osteotomy gap to promote healing.
- Intraoperative Imaging: Fluoroscopy is used throughout the procedure to verify guide wire placement, osteotomy creation, correction angle, and plate/screw position.
- Wound Closure: The wound is irrigated, and layers are closed meticulously.
Table: Key Surgical Steps for HTO with TomoFix
| Step | Description | Purpose |
|---|---|---|
| Preoperative Planning | X-rays, templating, deformity analysis | Accurate correction, plate/screw size determination. |
| Surgical Approach | Medial incision, soft tissue dissection | Access to proximal tibia. |
| Osteotomy Creation | Guide wires, oscillating saw, leaving medial hinge | Precise bone cut for realignment. |
| Correction & Gap | Distractors/wedges, fluoroscopy | Achieve desired mechanical axis shift. |
| Plate Placement | TomoFix plate positioned, temporary fixation | Optimal anatomical fit and stability. |
| Screw Insertion | Cortical (compression) then Locking (angular stability) screws | Secure plate fixation, create fixed-angle construct. |
| Bone Grafting | Packing graft into large osteotomy gaps | Promote bone union and fill void. |
| Wound Closure | Irrigation, layered closure | Prevent infection, facilitate healing. |
Patient Outcome Improvements
The use of the TomoFix HTO Plate significantly contributes to improved patient outcomes post-HTO surgery:
- Pain Reduction: By offloading the diseased compartment, patients experience substantial relief from activity-related knee pain.
- Functional Improvement: Patients often regain improved knee function, including increased range of motion and better stability, allowing them to return to daily activities and even some sports.
- Delaying Total Knee Arthroplasty (TKA): HTO effectively postpones the need for joint replacement surgery, which is particularly beneficial for younger patients, allowing them to remain active for many years before potentially requiring a TKA.
- Improved Quality of Life: Reduced pain and improved function translate directly into a higher quality of life, enabling patients to pursue hobbies and maintain an active lifestyle.
- Long-Term Stability and Durability: The robust fixation provided by TomoFix helps maintain the correction over the long term, contributing to the durability of the surgical outcome.
Risks, Side Effects, and Contraindications
While HTO with the TomoFix plate is generally a safe and effective procedure, like all surgeries, it carries potential risks and is not suitable for all patients.
Potential Surgical Risks and Complications
- Infection: Superficial or deep surgical site infection, potentially requiring antibiotics or further surgery.
- Neurovascular Injury: Damage to nerves (e.g., common peroneal nerve) or blood vessels around the knee.
- Nonunion or Delayed Union: Failure of the osteotomy site to heal, or healing taking longer than expected, potentially requiring revision surgery or bone stimulation.
- Hardware Irritation or Failure: The plate or screws may become prominent or cause irritation to soft tissues, sometimes necessitating hardware removal. Rarely, hardware can fracture.
- Loss of Correction: Despite rigid fixation, forces can sometimes lead to a partial loss of the achieved angular correction.
- Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE): Blood clots in the leg veins or lungs, a general risk of lower limb surgery.
- Compartment Syndrome: A rare but serious condition where increased pressure within a muscle compartment compromises circulation.
- Stiffness or Reduced Range of Motion: Despite rehabilitation, some patients may experience residual knee stiffness.
- Patella Baja: A complication where the patella (kneecap) sits lower than normal, potentially affecting patellofemoral mechanics.
Contraindications
- Advanced Tricompartmental Osteoarthritis: HTO is primarily for unicompartmental disease; severe degeneration in multiple compartments is a contraindication.
- Inflammatory Arthritis: Conditions like rheumatoid arthritis are generally contraindications.
- Severe Obesity: Excess weight can place undue stress on the osteotomy and hardware, increasing failure risk.
- Poor Bone Quality (Severe Osteoporosis): Compromised bone density may not provide adequate purchase for screws, increasing the risk of nonunion or hardware failure.
- Active Infection: Any active infection in the knee or elsewhere in the body must be resolved before surgery.
- Limited Preoperative Range of Motion: Patients with significant knee stiffness (e.g., less than 90 degrees flexion) may not benefit as much from HTO.
- Peripheral Vascular Disease: Compromised blood supply can impair healing.
- Unrealistic Patient Expectations: Patients must understand the recovery process and realistic outcomes.
Maintenance, Sterilization, and Post-Operative Care
Sterilization Protocols
The TomoFix HTO plates are typically supplied sterile and intended for single-use. The associated surgical instrumentation (drills, guides, screwdrivers, plate holders, distractors, etc.) are reusable and must adhere to strict hospital sterilization protocols.
- Cleaning: All reusable instruments must be thoroughly cleaned immediately after use to remove blood and tissue debris. Manual cleaning followed by ultrasonic cleaning is common.
- Inspection: Instruments are inspected for damage, wear, or corrosion.
- Packaging: Instruments are packaged in sterilization wraps or containers designed to maintain sterility.
- Sterilization: Autoclaving (steam sterilization) is the standard method for orthopedic instruments. Specific parameters (temperature, pressure, time) must be followed as per manufacturer guidelines and hospital policies.
- Storage: Sterile implants and instruments must be stored in a clean, dry environment, protected from contamination, until ready for use.
Post-Operative Management
Successful HTO with TomoFix depends heavily on a structured post-operative rehabilitation program.
- Weight-Bearing Restrictions: Patients typically follow a protected weight-bearing protocol, often non-weight-bearing or partial weight-bearing for 6-12 weeks, gradually progressing as bone healing occurs. Crutches or a walker are essential.
- Physical Therapy (PT): PT begins early, focusing on:
- Pain and Swelling Management: Ice, elevation, medication.
- Range of Motion (ROM): Gentle, controlled knee flexion and extension exercises to prevent stiffness.
- Muscle Strengthening: Quadriceps, hamstring, and gluteal strengthening exercises.
- Gait Training: Re-education of proper walking mechanics.
- Pain Management: A combination of analgesics, anti-inflammatory drugs, and nerve blocks may be used to control post-operative pain.
- Follow-up Schedule and Imaging: Regular clinical follow-ups and X-rays are crucial to monitor bone healing and ensure the correction is maintained. This typically occurs at 2 weeks, 6 weeks, 3 months, 6 months, and 1 year post-surgery.
- Hardware Removal: While the TomoFix plate is designed to be permanent, it may be removed in a secondary procedure if it causes symptoms such as irritation, pain, or discomfort, or if there's a risk of infection. This is usually done no sooner than 12-18 months after the initial surgery, once the osteotomy is fully healed.
Frequently Asked Questions (FAQ) about the TomoFix HTO Plate
1. What is a High Tibial Osteotomy (HTO)?
A High Tibial Osteotomy (HTO) is a surgical procedure that involves cutting and realigning the tibia (shin bone) just below the knee. Its primary goal is to shift the weight-bearing load from a damaged or arthritic compartment of the knee (usually the medial) to a healthier compartment, thereby reducing pain and slowing the progression of osteoarthritis.
2. Why is the TomoFix plate used for HTO?
The TomoFix plate is specifically designed for HTO procedures, providing robust and stable internal fixation. Its anatomical pre-contouring, locking screw technology, and biomechanical design ensure precise correction is maintained, facilitating optimal bone healing and allowing for earlier rehabilitation.
3. What are the benefits of HTO with TomoFix?
Benefits include significant pain reduction, improved knee function, preservation of the native knee joint, and the potential to delay or avoid total knee replacement surgery, especially in younger, active patients. The TomoFix system's stability contributes to these positive outcomes.
4. What materials is the TomoFix plate made from?
The TomoFix HTO Plate is made from titanium alloy (Ti6Al4V), a highly biocompatible material known for its strength, corrosion resistance, and suitability for long-term implantation in the human body.
5. How long does the HTO surgery take?
The duration of HTO surgery can vary, but it typically takes between 1 to 2 hours, depending on the complexity of the deformity, the surgeon's experience, and whether additional procedures (like cartilage repair or bone grafting) are performed.
6. What is the recovery time after HTO?
Initial recovery involves a period of protected weight-bearing (often 6-12 weeks) using crutches or a walker. Full recovery, including a return to most activities, can take 6 months to a year, with ongoing physical therapy playing a crucial role. Bone healing typically takes 3-6 months.
7. Will I need physical therapy after HTO?
Yes, physical therapy is absolutely essential after HTO with TomoFix. It plays a vital role in restoring knee range of motion, strengthening muscles, improving gait, and ultimately ensuring a successful return to function.
8. Is the TomoFix plate ever removed?
The TomoFix plate is designed to be a permanent implant. However, it may be removed in a secondary procedure if it causes symptoms such as irritation, pain, infection, or if hardware failure occurs. This decision is made in consultation with your surgeon, usually after the osteotomy has fully healed (typically 12-18 months post-surgery).
9. What are the risks associated with HTO and the TomoFix plate?
Potential risks include infection, nerve or blood vessel damage, nonunion (failure of the bone to heal), hardware irritation or failure, loss of correction, blood clots (DVT/PE), and knee stiffness. Your surgeon will discuss these risks thoroughly.
10. How does the TomoFix plate improve biomechanics?
By providing a fixed-angle, rigid construct, the TomoFix plate maintains the precise angular correction achieved during surgery. This shifts the weight-bearing axis of the knee, offloading the damaged compartment and redistributing forces more evenly across the healthier parts of the joint, thereby improving overall knee biomechanics.
11. Can I return to sports after HTO with TomoFix?
Many patients can return to low-impact sports and activities after successful HTO with TomoFix and appropriate rehabilitation. High-impact sports may be possible for some, but this depends on the individual's healing, knee condition, and the sport itself. This should be discussed with your surgeon and physical therapist.
12. How long does the TomoFix plate last?
The TomoFix plate is designed for long-term implantation. Made from durable titanium alloy, it is intended to remain in place indefinitely unless complications arise. Its longevity is supported by its robust design and the stability it provides to the healing bone.