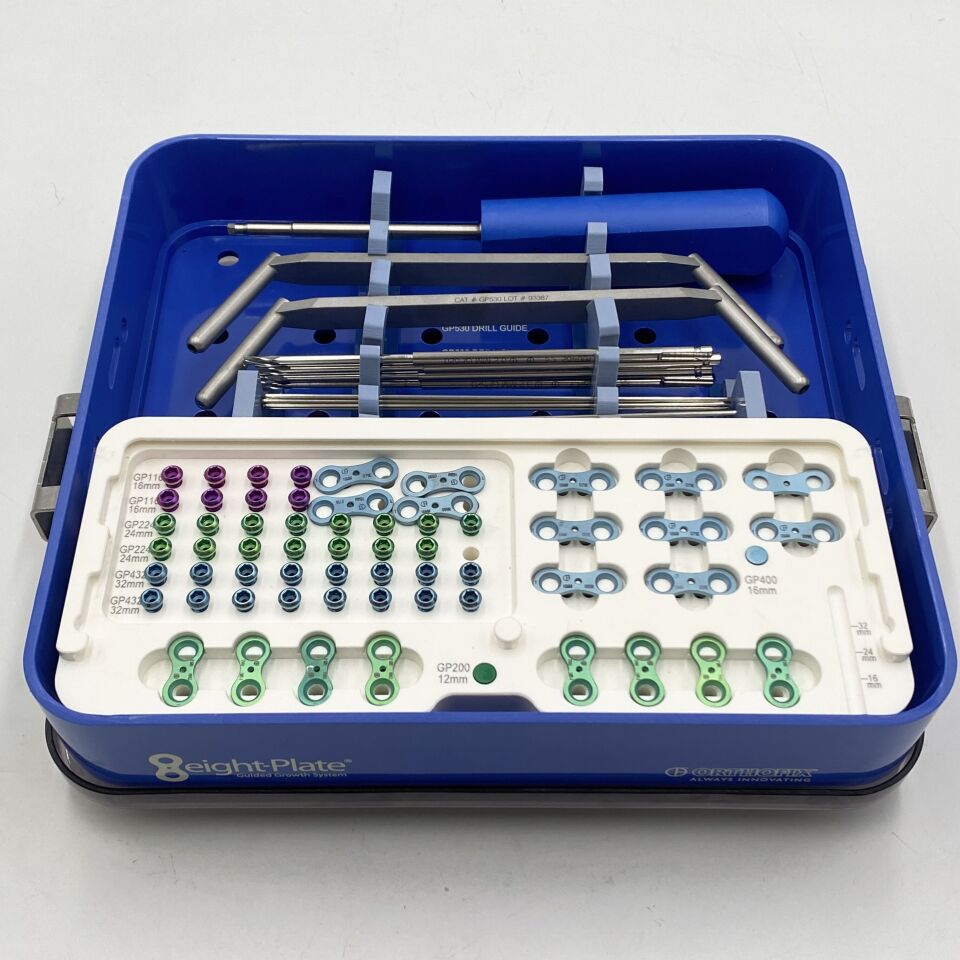
The Guided Growth Plate (Eight-Plate): Revolutionizing Pediatric Limb Deformity Correction
In the specialized field of pediatric orthopedics, the precise and timely management of limb deformities is paramount to ensuring healthy development and functional mobility for children. Among the most innovative and widely adopted solutions is the Guided Growth Plate, commonly known as the Eight-Plate. This sophisticated orthopedic instrument has transformed the approach to correcting angular limb deformities and addressing limb length discrepancies in skeletally immature patients.
As expert medical SEO copywriters and orthopedic specialists, we delve deep into the technical prowess, clinical applications, and profound patient benefits offered by the Eight-Plate system. This comprehensive guide aims to provide an exhaustive overview for healthcare professionals, parents, and anyone seeking authoritative information on this critical surgical tool.
Comprehensive Introduction & Overview
The Guided Growth Plate (Eight-Plate) is a small, biocompatible implant designed for temporary hemiepiphysiodesis – a procedure that involves slowing down growth on one side of a growth plate (physis) to allow the other side to catch up, thereby correcting an angular deformity. Its unique figure-of-eight design and non-locking screw fixation distinguish it from traditional methods, offering a less invasive, reversible, and highly effective solution for a range of pediatric orthopedic conditions.
Key Advantages of the Eight-Plate System:
- Minimally Invasive: Requires smaller incisions compared to osteotomies or permanent epiphysiodesis.
- Reversible: The effect on growth ceases upon implant removal, allowing for continued growth if desired.
- Controlled Correction: Facilitates gradual and guided correction of deformities.
- Versatile: Applicable to various angular deformities and limb length discrepancies.
- Reduced Morbidity: Generally associated with less pain, faster recovery, and fewer complications than more invasive procedures.
This system represents a paradigm shift from irreversible permanent growth arrest to a dynamic, temporary, and adjustable method of growth modulation, significantly improving outcomes for children facing growth plate-related challenges.
Deep-Dive into Technical Specifications & Mechanisms
The efficacy of the Eight-Plate lies in its ingenious design and its biomechanical interaction with the growing bone.
Design & Materials
The Eight-Plate system is characterized by its simplicity and robust engineering, ensuring both biocompatibility and mechanical stability.
- Plate Design:
- Figure-of-Eight Shape: This distinctive shape is not merely aesthetic; it allows for the placement of two screws parallel to each other, effectively straddling the growth plate without crossing it. This design prevents plate rotation and ensures stable fixation.
- Low Profile: The plate is designed to be as thin and unobtrusive as possible, minimizing soft tissue irritation and prominence under the skin.
- Material: Typically fabricated from high-grade, implantable titanium alloy (e.g., Ti-6Al-4V ELI) or medical-grade stainless steel (e.g., 316LVM). These materials are chosen for their:
- Biocompatibility: Non-toxic and well-tolerated by the human body, reducing the risk of adverse reactions.
- Corrosion Resistance: Essential for long-term implantation.
- Strength-to-Weight Ratio: Provides necessary mechanical strength without excessive bulk.
- Radiolucency (Titanium): While titanium is radiopaque, it causes less artifact on imaging compared to some other metals, aiding in post-operative assessment.
- Screw Design:
- Non-locking, Cannulated Screws: The system utilizes non-locking, typically cannulated, self-tapping screws.
- Non-locking: Crucial for the guided growth mechanism. The screws are not rigidly fixed to the plate, allowing for micro-motion and dynamic compression.
- Cannulated: Facilitates precise placement over a K-wire, enhancing surgical accuracy and minimizing growth plate injury.
- Self-tapping: Simplifies insertion by eliminating the need for pre-drilling a tap hole.
- Material: Screws are made from the same high-grade titanium alloy or stainless steel as the plate.
- Length: Available in various lengths to accommodate different bone sizes and achieve optimal bicortical purchase.
- Non-locking, Cannulated Screws: The system utilizes non-locking, typically cannulated, self-tapping screws.
Biomechanics: The Growth Modulation Principle
The fundamental principle behind the Eight-Plate's action is tension band plating applied to the physis (growth plate).
- Bridging the Physis: The Eight-Plate is surgically positioned to span the growth plate on one side of the bone. The two screws are inserted, one into the epiphysis (the end of the bone forming a joint) and the other into the metaphysis (the wider part of the bone shaft adjacent to the growth plate).
- Dynamic Compression: Unlike rigid locking plates, the non-locking screws allow for controlled micromotion. As the bone grows, the plate acts as a tension band, applying a compressive force across the growth plate on the side where it is implanted.
- Hemiepiphysiodesis: This localized compression subtly slows down or temporarily arrests growth on the plated side. The unplated side of the growth plate continues to grow at its normal rate.
- Gradual Correction: The differential growth rate causes the limb to gradually straighten or lengthen, correcting the angular deformity over time. The rate of correction is directly proportional to the remaining growth potential of the child.
- Reversibility: The key advantage is that the effect is reversible. Once the desired correction is achieved, the plate and screws can be removed. Upon removal, the growth plate typically resumes its normal growth pattern, provided it was not permanently damaged.
This dynamic interaction ensures a physiological and adaptable method of correction, harnessing the child's natural growth processes.
Extensive Clinical Indications & Usage
The Eight-Plate has a broad spectrum of clinical applications in pediatric orthopedics, primarily targeting conditions where growth modulation can effectively address deformities.
Primary Clinical Indications
- Angular Limb Deformities:
- Genu Valgum (Knock-knees): Excess growth on the medial (inner) side of the knee. The Eight-Plate is applied to the medial distal femur or proximal tibia.
- Genu Varum (Bowlegs): Excess growth on the lateral (outer) side of the knee. The Eight-Plate is applied to the lateral distal femur or proximal tibia.
- Ankle Deformities: Varus or valgus deformities of the ankle.
- Elbow Deformities: Varus or valgus deformities of the elbow (less common but possible).
- Limb Length Discrepancies (LLD):
- Used for temporary epiphysiodesis to slow growth in a longer limb to allow the shorter limb to catch up, particularly in the distal femur or proximal tibia.
- Specific Pediatric Conditions:
- Blount's Disease (Tibia Vara): A progressive growth disorder of the proximal medial tibia, often requiring correction.
- Rickets Sequelae: Deformities resulting from metabolic bone disorders.
- Post-traumatic Deformities: Angular deformities that develop after physeal fractures.
- Skeletal Dysplasias: In selected cases, to manage specific deformities.
Pre-operative Planning
Meticulous pre-operative planning is crucial for successful outcomes.
- Comprehensive Clinical Evaluation: Assessment of the child's age, skeletal maturity, gait, and overall health.
- Radiographic Imaging: Full-length standing anteroposterior (AP) radiographs of the lower extremities are essential to assess:
- Mechanical axis deviation (MAD).
- Location and severity of the deformity (e.g., femoral vs. tibial component).
- Growth plate status.
- Skeletal age (e.g., using a hand-wrist X-ray).
- Growth Prediction: Utilizing growth charts and established methods (e.g., Moseley straight-line graph, multiplier method) to estimate remaining growth and determine the optimal timing for intervention and implant removal.
- Patient Selection: Identifying patients with sufficient remaining growth potential for effective correction.
Surgical Technique (Fitting & Usage Instructions)
The Eight-Plate procedure is considered minimally invasive, typically performed under general anesthesia.
- Patient Positioning & Anesthesia: Supine position for lower limb procedures. Sterile preparation and draping of the surgical site.
- Incision Planning: Small, typically 1.5-2 cm longitudinal skin incisions are made over the identified physis, aiming for minimal soft tissue dissection.
- Exposure of the Physis: Careful dissection through subcutaneous tissue and muscle layers to expose the periosteum overlying the growth plate. Fluoroscopy is used to precisely locate the physis.
- Plate Placement:
- A K-wire is often used to mark the center of the physis.
- The Eight-Plate is centered over the physis, ensuring the central bridge of the figure-of-eight design overlies the growth plate.
- The plate should be positioned to lie flat against the bone cortex.
- Screw Insertion:
- A guidewire (K-wire) is inserted through the cannulated holes of the plate, one into the epiphysis and one into the metaphysis, ensuring they are parallel and bicortical (penetrating both cortices). Care is taken to avoid crossing or damaging the physis with the guidewire.
- Drill bit is used over the K-wire to create the screw pilot hole.
- The appropriate length self-tapping screw is then inserted over the guidewire until snug. It is crucial not to overtighten, as this could compress the growth plate permanently or cause stress fractures.
- Intra-operative Imaging: Fluoroscopy is used throughout the procedure to confirm correct plate and screw placement, ensuring the screws are perpendicular to the long axis of the bone and do not violate the physis.
- Wound Closure: After confirming satisfactory implant placement, the incisions are closed in layers.
Post-operative Care
- Weight-Bearing: Patients are typically allowed to weight-bear as tolerated immediately or shortly after surgery, often with crutches for initial comfort.
- Pain Management: Mild analgesics are usually sufficient.
- Follow-up: Regular clinical and radiographic follow-ups (e.g., every 3-6 months) are essential to monitor the progress of correction and assess the mechanical axis.
- Implant Removal: Once the desired correction is achieved, the implants are removed in a second, usually simpler, surgical procedure. The timing of removal is critical to prevent overcorrection.
Maintenance & Sterilization Protocols for Instrumentation
While the Eight-Plate implants themselves are single-use, sterile-packaged devices, the associated surgical instrumentation (screwdrivers, K-wire guides, plate holders, etc.) requires stringent maintenance and sterilization.
General Principles:
- Follow Manufacturer's Instructions: Always adhere to the specific guidelines provided by the Eight-Plate system manufacturer.
- Dedicated Instrument Sets: Keep instrument sets for orthopedic implants separate from general surgical instruments to prevent cross-contamination and ensure proper handling.
Protocols:
- Point-of-Use Cleaning: Immediately after surgery, remove gross contaminants (blood, tissue) by wiping instruments with a damp cloth or sponge. This prevents drying of bioburden, which makes cleaning more difficult.
- Disassembly: If instruments are designed to be disassembled (e.g., cannulated handles), take them apart before cleaning to allow thorough access to all surfaces.
- Cleaning:
- Manual Cleaning: Immerse instruments in an enzymatic detergent solution. Use soft brushes to scrub all surfaces, lumens, and crevices. Rinse thoroughly with purified water.
- Automated Cleaning (Ultrasonic Cleaner/Washer-Disinfector): Follow validated cycles. Ensure instruments are correctly loaded to allow water and detergent to reach all surfaces. Use appropriate detergents specific for medical instruments.
- Rinsing: Rinse instruments thoroughly with deionized or distilled water to remove all detergent residues.
- Inspection: Visually inspect all instruments for cleanliness, damage (e.g., corrosion, pitting, dullness), and proper function. Replace or repair damaged instruments.
- Lubrication: Apply water-soluble, steam-permeable lubricant to hinged instruments if recommended by the manufacturer.
- Packaging: Place instruments in appropriate sterilization containers or wraps, ensuring proper spacing for steam penetration. Protect delicate tips.
- Sterilization:
- Steam Sterilization (Autoclaving): The most common and preferred method. Use validated cycles (e.g., gravity displacement or prevacuum steam sterilization) at specified temperatures and durations (e.g., 121°C for 30 minutes, or 132°C for 4 minutes, followed by a drying cycle).
- Flash Sterilization: Should be avoided if possible. If necessary, use only for urgent situations and follow strict parameters.
- Storage: Store sterilized instruments in a clean, dry, and protected environment until use.
Adherence to these protocols is critical to prevent surgical site infections and ensure the longevity and reliability of the surgical instrumentation.
Patient Outcome Improvements
The introduction and widespread adoption of the Eight-Plate system have significantly improved patient outcomes in pediatric orthopedics.
- Effective Deformity Correction: High rates of successful correction of angular deformities and management of limb length discrepancies.
- Avoidance of Major Surgery: In many cases, the Eight-Plate can prevent the need for more complex and invasive procedures like osteotomies (bone cutting and realignment) or permanent epiphysiodesis (which sacrifices future growth potential).
- Minimally Invasive: Leads to smaller scars, reduced post-operative pain, shorter hospital stays, and faster return to normal activities, including school and sports.
- Reversibility: The ability to remove the implant and allow the growth plate to resume normal growth is a major psychological and clinical benefit, offering more control over the child's development.
- Improved Cosmesis and Function: Corrected limb alignment leads to better gait, reduced joint strain, improved appearance, and enhanced self-esteem for children.
- Reduced Complications: Compared to more invasive methods, the Eight-Plate generally has a lower risk of major complications, though specific risks still exist.
Risks, Side Effects, or Contraindications
While highly effective, the Eight-Plate system is not without potential risks, side effects, or contraindications. Comprehensive patient and parental counseling is essential.
Potential Risks & Side Effects
- Infection: As with any surgical procedure, there is a risk of superficial or deep surgical site infection, potentially requiring antibiotic treatment or implant removal.
- Screw Breakage, Loosening, or Migration: Although rare with proper technique, screws can loosen or break, necessitating revision surgery. Migration can cause soft tissue irritation.
- Overcorrection or Undercorrection: Inaccurate growth prediction or delayed implant removal/premature removal can lead to the deformity being overcorrected or not fully corrected, potentially requiring further intervention.
- Growth Plate Damage: Improper screw placement or overtightening can potentially damage the physis, leading to permanent growth arrest or growth disturbance.
- Pain/Irritation: The implant may cause localized pain or irritation, especially if it becomes prominent under the skin, often necessitating earlier removal.
- Neurovascular Injury: Although rare, damage to nearby nerves or blood vessels is a potential surgical risk.
- Stress Fractures: Rarely, stress fractures around the screw holes can occur.
- Rebound Growth: After implant removal, there can sometimes be a temporary acceleration of growth on the previously constrained side, though this is usually self-limiting.
- Allergic Reaction: Extremely rare, but possible reaction to implant materials.
Contraindications
- Insufficient Remaining Growth Potential: If a child is too close to skeletal maturity, there may not be enough growth remaining to achieve the desired correction. The Eight-Plate relies on active growth.
- Skeletal Maturity: Once growth plates are fused, the Eight-Plate is ineffective for growth modulation.
- Active Infection: Any active local or systemic infection is a contraindication, as it significantly increases the risk of implant infection.
- Severe Osteopenia/Osteoporosis: Poor bone quality may compromise screw fixation and increase the risk of complications.
- Non-compliant Patient/Family: If the patient or family cannot adhere to follow-up schedules or post-operative instructions, successful outcomes may be jeopardized.
- Complex Multi-planar Deformities: For very severe or multi-planar deformities, an osteotomy may be a more appropriate and definitive solution.
- Physeal Bar: The Eight-Plate is not used to treat a physeal bar (bony bridge across the growth plate) directly, though it may be used as an adjunct after bar resection.
Massive FAQ Section: Your Questions Answered
Here are frequently asked questions about the Guided Growth Plate (Eight-Plate), providing clarity for patients, parents, and healthcare providers.
1. What exactly is the Guided Growth Plate (Eight-Plate)?
The Eight-Plate is a small, figure-of-eight shaped metal implant used in pediatric orthopedics to temporarily slow down growth on one side of a child's growth plate. This allows the other side of the growth plate to continue growing normally, gradually correcting angular limb deformities like knock-knees or bowlegs.
2. How does the Eight-Plate work to correct deformities?
The plate is strategically placed across the growth plate with two screws – one in the bone above and one in the bone below the growth plate. These screws are not locked to the plate, allowing for dynamic compression. As the child grows, the plate acts as a tension band, applying gentle pressure that slows growth on the side where it's implanted. The unplated side continues to grow, causing the limb to straighten over time.
3. What conditions can the Eight-Plate treat?
It is primarily used to treat angular limb deformities such as genu valgum (knock-knees), genu varum (bowlegs), and certain ankle deformities. It can also be used to manage limb length discrepancies by temporarily slowing growth in a longer limb. Conditions like Blount's disease and deformities from rickets are also common indications.
4. Is the surgery painful for my child?
The surgery is minimally invasive, typically involving small incisions. While there will be some post-operative discomfort, it is generally well-managed with over-the-counter pain relievers or mild prescription medication. Most children recover quickly and can return to normal activities within a few weeks.
5. How long does the Eight-Plate stay in my child's leg?
The duration varies greatly depending on the child's age, the severity of the deformity, and their remaining growth potential. It can range from several months to a few years. Regular follow-up appointments with X-rays are crucial to monitor the correction and determine the optimal time for implant removal.
6. Is the procedure reversible? What happens after the plate is removed?
Yes, a key advantage of the Eight-Plate is its reversibility. Once the desired correction is achieved, the plate and screws are surgically removed in a second, usually simpler, procedure. After removal, the growth plate typically resumes its normal growth rate, allowing for continued, unhindered growth.
7. What are the potential risks or side effects associated with the Eight-Plate?
While generally safe, potential risks include infection at the surgical site, screws loosening or breaking, overcorrection or undercorrection of the deformity, pain or irritation from the implant, and rarely, damage to the growth plate. Your surgeon will discuss all potential risks and benefits thoroughly.
8. How successful is the Eight-Plate in correcting deformities?
The Eight-Plate has a high success rate in correcting appropriate angular limb deformities, especially when applied at the correct time and with proper patient selection. It has significantly reduced the need for more invasive procedures and improved long-term outcomes for many children.
9. Will my child need physical therapy after the surgery?
In most cases, formal physical therapy is not extensively required after Eight-Plate surgery. Children are usually encouraged to return to normal activities as tolerated. However, your surgeon may recommend specific exercises or physical therapy if there are concerns about range of motion or muscle strength.
10. Can my child play sports or engage in normal activities with the Eight-Plate in place?
Generally, yes. Most children can resume their normal activities, including sports, once the initial post-operative healing period is complete and their surgeon approves. The plate is designed to be low-profile and durable, but contact sports or activities with a high risk of direct impact to the implant site might require caution or temporary restriction.
11. What if the deformity comes back after the plate is removed?
Recurrence of the deformity is rare but can happen, especially if there's significant growth remaining after implant removal or if the underlying condition is progressive. If a recurrence occurs, your orthopedic surgeon will assess the situation and discuss further treatment options, which may include re-implantation of the Eight-Plate or other interventions.
12. What is the typical recovery time after Eight-Plate insertion and removal?
After insertion, most children are walking with minimal assistance within a few days to a week and can return to school and light activities shortly thereafter. Full recovery for sports might take 4-6 weeks. For removal, the recovery is usually even faster, often involving just a few days of mild discomfort before resuming normal activities.
The Guided Growth Plate (Eight-Plate) stands as a testament to the advancements in pediatric orthopedic care, offering a refined, effective, and patient-friendly solution for managing complex growth-related deformities. Its continued evolution promises even brighter futures for children worldwide.