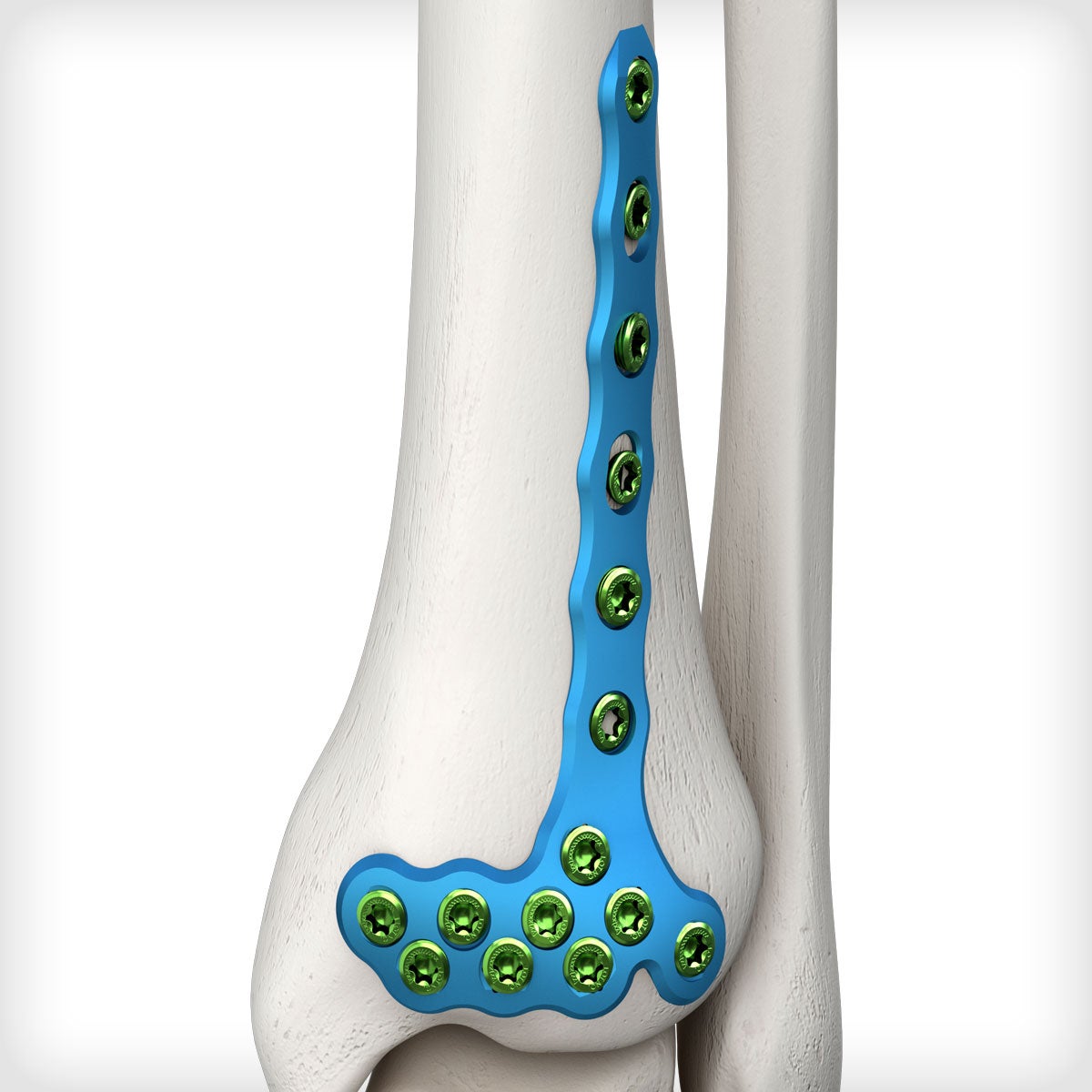
The Anterolateral Distal Tibia (Pilon) Plate: A Comprehensive Medical SEO Guide
Pilon fractures, or distal tibia plafond fractures, represent some of the most challenging injuries encountered in orthopedic trauma surgery. These high-energy injuries often result in significant comminution, articular surface disruption, and extensive soft tissue damage. Effective management requires meticulous surgical planning, precise anatomical reduction, and stable internal fixation to restore joint congruity and optimize patient outcomes. Among the array of fixation devices, the Anterolateral Distal Tibia (Pilon) Plate has emerged as a cornerstone in the surgical armamentarium for specific patterns of these complex fractures.
This exhaustive guide, crafted by an expert Medical SEO Copywriter and Orthopedic Specialist, delves deep into the "Anterolateral Distal Tibia (Pilon) Plate," providing a highly authoritative overview of its design, clinical applications, biomechanical principles, maintenance, and profound impact on patient recovery.
1. Comprehensive Introduction & Overview
Pilon fractures typically result from axial loading combined with rotational forces, often seen in falls from height or motor vehicle accidents. The term "pilon" is derived from the French word for "pestle," aptly describing the crushing mechanism that drives the talus into the distal tibia. These fractures are characterized by their involvement of the weight-bearing articular surface of the distal tibia, leading to a high risk of post-traumatic arthritis, malunion, and chronic pain if not managed appropriately.
The surgical management of pilon fractures aims to:
* Restore the articular surface congruity.
* Reconstruct the metaphyseal bone stock.
* Achieve stable fixation to allow early range of motion.
* Minimize soft tissue complications.
Historically, these fractures were associated with high complication rates. Advances in surgical techniques, particularly the understanding of soft tissue envelopes and the evolution of anatomically contoured locking plates, have significantly improved outcomes. The Anterolateral Distal Tibia (Pilon) Plate is specifically designed to address fracture patterns involving the anterolateral aspect of the distal tibia, offering a stable and anatomically precise solution. Its low-profile design and locking screw technology minimize periosteal stripping and provide robust fixation, crucial for healing in this often compromised vascular environment.
2. Deep-Dive into Technical Specifications / Mechanisms
The Anterolateral Distal Tibia (Pilon) Plate is a sophisticated orthopedic implant engineered for precision and stability. Its design reflects a deep understanding of distal tibial anatomy and the biomechanics of pilon fractures.
2.1 Design and Materials
The plate's primary material is typically a high-strength, biocompatible alloy, most commonly Titanium (Ti-6Al-4V).
* Titanium Advantages:
* Biocompatibility: Excellent integration with bone and soft tissues, minimizing adverse reactions.
* Corrosion Resistance: Highly resistant to physiological corrosion.
* High Strength-to-Weight Ratio: Provides robust fixation without excessive bulk.
* Elastic Modulus: Closer to that of cortical bone compared to stainless steel, potentially reducing stress shielding.
* MRI Compatibility: Non-ferromagnetic, allowing for safe MRI imaging post-surgery.
The plate itself is characterized by:
* Anatomical Contouring: Pre-contoured to match the complex anatomy of the anterolateral distal tibia, including the articular surface and metaphysis. This minimizes the need for intraoperative bending, reducing operative time and potential stress risers in the plate.
* Low Profile Design: Minimizes soft tissue irritation and prominence, reducing the need for subsequent hardware removal.
* Fixed-Angle Locking Screw Technology: The cornerstone of modern plate fixation. Locking screws thread into the plate, creating a fixed-angle construct that acts as an internal fixator. This offers several advantages:
* Angular stability independent of bone purchase.
* Reduced risk of screw pull-out, especially in osteoporotic bone.
* Minimal compression of the plate to the periosteum, preserving blood supply.
* Ability to create a stable construct even with comminuted fractures.
* Combi-Holes (Combination Holes): These holes allow for the use of both locking screws and standard cortical screws.
* Locking Screw Portion: For fixed-angle stability.
* Dynamic Compression Unit (DCU) Portion: For conventional compression of fracture fragments, or for lag screw placement through the plate to achieve interfragmentary compression.
* Screw Configurations: The plate incorporates multiple screw holes angled to capture specific fragments of the distal tibia, including the anterolateral fragment, and to provide robust support for the articular surface. Distal screw clusters are designed to support the subchondral bone.
* Plate Lengths: Available in various lengths to accommodate different fracture patterns and patient anatomies.
2.2 Biomechanics
The biomechanical principles underlying the Anterolateral Distal Tibia Plate are critical for achieving stable fixation and promoting healing.
* Fixed-Angle Stability: Locking screws create a rigid construct where the screws and plate act as a single unit. This provides excellent resistance to bending, shear, and torsional forces, essential in a weight-bearing joint.
* Load Sharing vs. Load Bearing: Depending on the fracture pattern and reduction quality, the construct can be primarily load-sharing (where bone fragments bear some load) or load-bearing (where the plate carries most of the load). The goal is often load sharing to promote bone healing.
* Bridge Plating: For highly comminuted metaphyseal fractures, the plate can act as a bridge, maintaining length, alignment, and rotation without directly compressing the comminuted zone. The fixed-angle screws provide stability to the articular block and the diaphysis.
* Minimal Periosteal Disruption: The non-compressing nature of locking plates means less disruption to the periosteal blood supply, which is crucial for fracture healing, especially in the distal tibia where vascularity can be precarious.
* Construct Stiffness: The rigidity of the locking plate construct allows for early, controlled mobilization, which is beneficial for articular cartilage health and rehabilitation, while protecting the healing fracture.
3. Extensive Clinical Indications & Usage
The Anterolateral Distal Tibia (Pilon) Plate is specifically indicated for complex distal tibia fractures, particularly those involving the anterolateral aspect. Its utility is best understood in the context of fracture classification and surgical approaches.
3.1 Clinical Indications
The primary indication is for articular and metaphyseal fractures of the distal tibia (pilon fractures), especially those classified as:
* AO/OTA Classification 43-C: These are complex articular and metaphyseal fractures of the distal tibia. The anterolateral plate is particularly suited for patterns with a distinct anterolateral fragment.
* Fractures with a Large Anterolateral Fragment: Many pilon fractures, particularly those resulting from external rotation and axial load, create a large, often displaced, anterolateral fragment involving the anterior aspect of the tibial plafond. This plate is anatomically designed to capture and stabilize this specific fragment.
* Open Fractures (Gustilo-Anderson Types I, II, IIIa): After debridement and appropriate soft tissue management, definitive fixation with a locking plate can be considered.
* Fractures with Significant Metaphyseal Comminution: The bridge plating capabilities of the locking plate system are highly advantageous in these scenarios.
* Fractures Requiring Indirect Reduction Techniques: The stability of the locking construct allows for indirect reduction strategies, minimizing further soft tissue damage.
3.2 Surgical Approach and Usage
The plate is typically applied via an anterolateral approach to the distal tibia.
* Patient Positioning: Supine on a radiolucent table, often with a bump under the ipsilateral hip.
* Incision: A longitudinal incision centered over the anterolateral aspect of the distal tibia, extending distally to the ankle joint line. Careful dissection is performed to protect neurovascular structures (superficial peroneal nerve, dorsalis pedis artery).
* Soft Tissue Management: A critical aspect. Often, a staged approach is employed, with initial external fixation and delayed definitive plating (7-14 days) to allow soft tissue swelling to subside, reducing the risk of wound complications.
* Fracture Reduction:
* Ligamentotaxis: Traction applied to the foot can help reduce articular fragments.
* Direct Visualization: The anterolateral approach allows for direct visualization of the anterolateral fragment and often a portion of the articular surface.
* Temporary Fixation: K-wires or small clamps are used to provisionally reduce and hold articular fragments.
* Bone Grafting: If significant metaphyseal defects exist after reduction, bone graft (autograft or allograft) may be used to support the articular surface.
* Plate Application and Fixation:
1. Plate Placement: The pre-contoured plate is carefully positioned on the anterolateral surface of the tibia. Optimal placement ensures maximal coverage of the fracture fragments while avoiding impingement on tendons or neurovascular structures. Fluoroscopy is used extensively to confirm plate position relative to the joint line and fracture fragments.
2. Proximal Fixation: The plate is initially secured to the tibial diaphysis proximally with a cortical screw through a DCU hole, allowing for compression if needed, or with locking screws.
3. Distal Fixation: This is the most critical step. Locking screws are inserted into the distal cluster of holes, aimed at capturing the articular fragments and providing subchondral support. Specific angles of the screw holes are designed to maximize fragment capture. Lag screws can be inserted through the plate or separately to achieve interfragmentary compression of specific fragments.
4. Confirmation: Repeated fluoroscopic images (AP, lateral, oblique views) are taken to confirm anatomical reduction, joint congruity, and optimal screw placement, ensuring no intra-articular screw penetration.
* Wound Closure: Meticulous layered closure, often with drains, to minimize dead space and reduce hematoma formation.
3.3 Advantages over Other Fixation Methods
- Superior Stability: Locking plates provide fixed-angle stability, which is often superior to conventional plating in comminuted or osteoporotic bone.
- Anatomical Fit: Pre-contoured design minimizes intraoperative adjustments and ensures optimal load distribution.
- Soft Tissue Preservation: Low-profile design and minimal periosteal contact reduce soft tissue irritation and preserve vascularity.
- Early Mobilization: The robust fixation allows for earlier, controlled range of motion exercises, crucial for preventing joint stiffness and improving functional outcomes.
- Reduced Complication Rates: Compared to older techniques, modern locking plates have shown lower rates of malunion, nonunion, and implant failure in appropriately selected cases.
4. Risks, Side Effects, or Contraindications
While the Anterolateral Distal Tibia (Pilon) Plate offers significant advantages, like any surgical procedure and implant, it carries inherent risks and potential complications.
4.1 General Surgical Risks
- Infection: Superficial or deep wound infection, potentially leading to osteomyelitis and hardware removal.
- Bleeding/Hematoma: Accumulation of blood under the skin, requiring drainage.
- Neurovascular Injury: Damage to nerves (e.g., superficial peroneal nerve) or blood vessels during the approach or screw insertion, leading to numbness, weakness, or vascular compromise.
- Anesthesia Risks: Adverse reactions to anesthetic agents.
- Thromboembolic Events: Deep vein thrombosis (DVT) or pulmonary embolism (PE).
4.2 Implant-Specific Risks and Side Effects
- Nonunion or Delayed Union: Failure of the bone to heal, or healing taking longer than expected, potentially requiring revision surgery.
- Malunion: Healing of the fracture in an incorrect anatomical position, leading to deformity, altered biomechanics, and potentially post-traumatic arthritis.
- Implant Prominence/Irritation: The plate or screws may be palpable under the skin, causing discomfort or irritation to tendons, necessitating hardware removal.
- Hardware Failure: Breakage of the plate or screws, usually due to excessive load or incomplete bone healing.
- Post-Traumatic Arthritis: Despite anatomical reduction and stable fixation, the initial articular cartilage damage can lead to progressive degeneration of the joint, requiring future fusion or arthroplasty.
- Complex Regional Pain Syndrome (CRPS): A chronic pain condition that can develop after trauma or surgery.
- Stiffness: Restricted ankle joint motion despite early rehabilitation.
4.3 Contraindications
- Active Infection: Absolute contraindication. Infection must be cleared before implanting hardware.
- Severe Open Fractures (Gustilo-Anderson Types IIIb/IIIc): Where extensive soft tissue loss, contamination, or devitalization makes internal fixation too risky. External fixation is usually preferred initially.
- Extensive Comminution with Insufficient Bone Stock: If there's truly no viable bone to achieve stable fixation, alternative strategies may be needed.
- Severe Peripheral Vascular Disease: Compromised blood supply to the limb may impair healing and increase infection risk.
- Poor Skin Quality/Extensive Soft Tissue Damage: If the soft tissue envelope is too severely compromised to tolerate an incision and plating, other options like external fixation or limited internal fixation might be considered.
- Patient Unwillingness or Inability to Comply with Postoperative Protocol: Non-compliance with weight-bearing restrictions or rehabilitation can jeopardize the outcome.
5. Maintenance/Sterilization Protocols (for Associated Instruments)
It is crucial to clarify that the Anterolateral Distal Tibia (Pilon) Plate itself is a single-use, sterile implant. It arrives pre-sterilized from the manufacturer (typically via gamma irradiation or ethylene oxide) and is opened in the sterile field just prior to implantation. Therefore, there are no "maintenance" or "sterilization" protocols for the plate itself by the end-user (hospital/surgeon).
However, the associated surgical instrumentation used to implant the plate (e.g., drills, drill guides, screwdrivers, plate holders, temporary reduction clamps, depth gauges, bone tampers, plate benders) are reusable and require stringent maintenance and sterilization protocols.
5.1 Cleaning and Decontamination
Immediately after surgery:
1. Gross Debris Removal: Instruments should be wiped clean of blood and tissue at the point of use.
2. Pre-soak/Enzymatic Cleaner: Instruments are placed in an enzymatic detergent solution or water to prevent drying of organic material.
3. Manual Cleaning: Thorough manual scrubbing with brushes and appropriate detergents to remove all visible debris from surfaces, lumens, and crevices. Disassembly of multi-part instruments as per manufacturer guidelines.
4. Ultrasonic Cleaning: Many instruments benefit from ultrasonic cleaning to remove microscopic debris.
5. Rinsing: Thorough rinsing with purified water to remove all detergent residues.
5.2 Inspection and Maintenance
After cleaning and before sterilization:
1. Visual Inspection: Each instrument is meticulously inspected for cleanliness, damage (e.g., bent tips, dull edges, cracks, corrosion), and functionality.
2. Lubrication: Moving parts (e.g., scissors, forceps, drivers) are lubricated with surgical-grade lubricant.
3. Assembly: Multi-part instruments are reassembled if required for sterilization.
4. Tray Preparation: Instruments are organized into specific trays according to manufacturer guidelines, ensuring proper spacing for steam penetration.
5.3 Sterilization
The most common and effective method for sterilizing heat- and moisture-stable orthopedic instruments is steam sterilization (autoclaving).
* Parameters: Specific time, temperature, and pressure cycles vary based on the type of sterilizer (e.g., gravity displacement, pre-vacuum), load size, and packaging. Typical parameters include:
* Pre-vacuum: 4 minutes at 132°C (270°F) or 3 minutes at 135°C (275°F).
* Gravity: 15-30 minutes at 121°C (250°F).
* Biological and Chemical Indicators: Sterilization cycles are routinely monitored using biological indicators (spore tests) and chemical indicators (strips, tapes) to confirm sterility assurance levels.
* Packaging: Instruments are typically wrapped in sterilization wrap or placed in rigid sterilization containers designed to maintain sterility post-sterilization.
5.4 Storage
Sterile instruments are stored in a clean, dry, temperature-controlled environment, protected from dust, moisture, and physical damage, until needed for surgery.
Adherence to these rigorous protocols is paramount to prevent surgical site infections and ensure the longevity and functionality of the surgical instrumentation.
6. Patient Outcome Improvements
The judicious use of the Anterolateral Distal Tibia (Pilon) Plate significantly contributes to improved patient outcomes following complex pilon fractures.
- Restoration of Anatomical Alignment and Joint Congruity: The pre-contoured design and precise screw placement allow for accurate reduction of the articular surface and metaphyseal segments. This is fundamental in minimizing post-traumatic arthritis.
- Enhanced Stability and Early Mobilization: The fixed-angle locking screw technology provides a rigid construct, enabling surgeons to initiate early, controlled range of motion exercises. This prevents joint stiffness, promotes cartilage health, and accelerates rehabilitation.
- Reduced Rates of Nonunion and Malunion: By providing stable fixation that respects the biological environment, the plate helps create optimal conditions for bone healing, thereby reducing the incidence of these debilitating complications.
- Lower Incidence of Implant Failure: The robust design and biomechanical advantages of locking plates contribute to greater implant longevity and reduced rates of hardware breakage.
- Improved Functional Outcomes: Patients typically experience better ankle range of motion, reduced pain, and a higher likelihood of returning to pre-injury activity levels compared to historical treatment methods.
- Minimized Soft Tissue Complications: The low-profile design and ability to use indirect reduction techniques or a staged approach (to allow soft tissue swelling to subside) reduce the risk of wound dehiscence, infection, and skin necrosis, which are significant concerns in pilon fractures.
- Reduced Need for Secondary Procedures: Optimal primary fixation can decrease the necessity for hardware removal due to prominence or revision surgery for nonunion/malunion, thereby reducing the overall burden of care.
7. Massive FAQ Section
Q1: What is a Pilon Fracture?
A1: A pilon fracture is a severe break of the distal (lower) end of the tibia (shin bone) that extends into the ankle joint. These are typically high-energy injuries that crush the articular surface, making them complex and challenging to treat.
Q2: Why is the Anterolateral Distal Tibia Plate specifically used for these fractures?
A2: This plate is anatomically pre-contoured to fit the specific shape of the anterolateral aspect of the distal tibia. Many pilon fractures, particularly those involving an anterolateral fragment, benefit from this plate's ability to precisely capture and stabilize these crucial pieces, restoring the joint's surface.
Q3: What material is the plate made from? Is it safe?
A3: The plate is typically made from a high-strength, biocompatible titanium alloy (Ti-6Al-4V). Titanium is widely used in orthopedic implants due to its excellent biocompatibility, corrosion resistance, and favorable mechanical properties, making it very safe for long-term implantation in the human body.
Q4: What are "locking screws" and why are they important?
A4: Locking screws thread directly into the plate, creating a fixed-angle construct. This means the screws don't rely on compression against the bone for stability, making the overall fixation much stronger and more stable, especially in comminuted fractures or poor bone quality. They act like an "internal fixator."
Q5: Will I need to have the plate removed?
A5: Not necessarily. Hardware removal is typically considered if the plate causes symptoms like pain, soft tissue irritation, or infection. If it's not causing any problems, it can often remain in place indefinitely. Your surgeon will discuss this with you.
Q6: How long is the recovery period after surgery with this plate?
A6: Recovery from a pilon fracture is prolonged and highly individualized. Initial non-weight-bearing is common for 6-12 weeks, followed by a gradual progression to full weight-bearing. Full recovery of function can take 6-12 months or even longer, with ongoing physical therapy being crucial.
Q7: What are the main risks associated with using this plate?
A7: Risks include general surgical complications (infection, bleeding, nerve damage) and specific implant-related issues such as nonunion (failure to heal), malunion (healing in a poor position), implant prominence, post-traumatic arthritis, and hardware failure. Your surgeon will discuss these in detail.
Q8: Can I get an MRI with this titanium plate in my leg?
A8: Yes, titanium implants are generally considered MRI-compatible and safe for diagnostic imaging. You should always inform the MRI technician about your implant before the scan.
Q9: How does this plate improve patient outcomes?
A9: By providing stable, anatomical fixation, the plate helps to restore the ankle joint's congruity, allowing for earlier, controlled mobilization. This reduces the risk of joint stiffness, speeds up rehabilitation, minimizes complications like nonunion, and ultimately leads to better long-term functional results and less pain.
Q10: Are there alternatives to this plate for pilon fractures?
A10: Yes, depending on the fracture pattern and surgeon's preference, other fixation methods may be used. These can include external fixation, alternative plate designs (e.g., medial, posterior, or combined plating), or in rare cases, intramedullary nailing for certain fracture types. The choice depends on a thorough assessment of the individual fracture.
Q11: What is the significance of the "low profile" design?
A11: A low-profile design means the plate sits very close to the bone surface, minimizing its projection under the skin. This reduces the likelihood of soft tissue irritation, tendon impingement, and discomfort, thereby decreasing the need for subsequent hardware removal surgery.
Q12: Is this plate always used in a single surgery?
A12: Not always. For severe pilon fractures, especially those with significant soft tissue swelling or open wounds, a "staged" approach is often preferred. This involves initial temporary external fixation to stabilize the fracture and allow soft tissues to recover, followed by definitive internal fixation with the Anterolateral Distal Tibia Plate a week or two later. This strategy helps reduce wound complications.