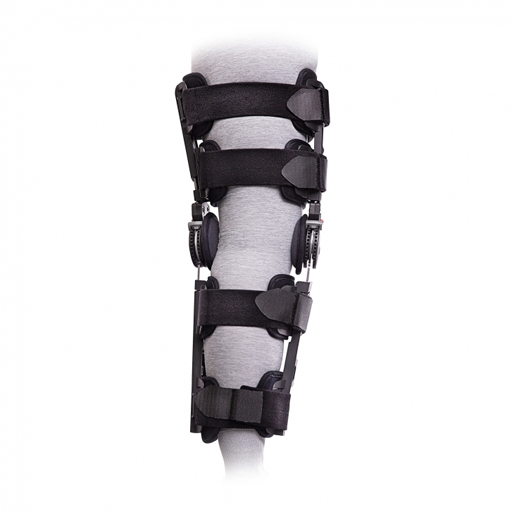
Comprehensive Introduction & Overview
A Post-Operative Range of Motion (ROM) Knee Brace is a critical orthopedic device meticulously engineered to provide essential support, protection, and controlled mobilization to the knee joint following various surgical procedures. Far from being a mere support garment, these specialized braces are precision instruments designed to facilitate optimal healing, mitigate the risk of re-injury, and guide the rehabilitation process by limiting or allowing specific degrees of knee flexion and extension.
The primary objective of a ROM knee brace is multifaceted:
* Protection: Shielding delicate surgical repairs (e.g., ligament grafts, meniscal sutures, cartilage resurfacing) from undue stress or sudden movements that could compromise healing.
* Stabilization: Providing external stability to the knee joint, compensating for temporary weakness or instability post-surgery.
* Controlled Mobilization: Allowing for a prescribed, gradual increase in range of motion as per the surgeon's protocol, preventing stiffness while safeguarding healing tissues.
* Pain Management: Reducing pain by stabilizing the joint and preventing uncontrolled movements.
* Proprioception: Enhancing the patient's awareness of their knee's position in space, which can be diminished after injury or surgery.
These braces are an indispensable component of modern orthopedic rehabilitation, bridging the gap between surgical intervention and full functional recovery. Their design varies from simple hinged models to highly sophisticated adjustable systems, each tailored to specific clinical needs and recovery phases.
Deep-dive into Technical Specifications & Mechanisms
The efficacy of a post-operative ROM knee brace lies in its sophisticated design, choice of advanced materials, and precise biomechanical principles.
Design and Materials
The construction of a high-quality ROM knee brace involves several key components, each chosen for specific performance characteristics:
- Frame:
- Materials: Typically constructed from lightweight yet robust aerospace-grade aluminum alloys or advanced carbon fiber composites. These materials offer an excellent strength-to-weight ratio, ensuring durability without adding excessive bulk.
- Functionality: The frame provides the structural integrity of the brace, supporting the hinges and strap systems. Its contoured design is crucial for anatomical fit, reducing pressure points and enhancing patient compliance.
- Hinges:
- Types:
- Polycentric Hinges: Mimic the natural rolling and gliding motion of the knee joint, providing a more anatomical and comfortable movement. They are often preferred for their ability to reduce shear forces on the joint.
- Single-Axis Hinges: Simpler in design, offering a rotational pivot point.
- Adjustable ROM Stops: The most critical feature. These mechanical stops allow the orthopedic surgeon or physical therapist to precisely set the permissible range of flexion and extension.
- Flexion Limits: Can be set from 0° (full extension) to 120° or more, often in 10-15° increments.
- Extension Limits: Typically range from -10° (hyperextension) to 40°, often set at 0° or 10° for protective purposes.
- Mechanism: Simple, tool-free adjustment mechanisms (e.g., push-button, slide-and-lock) enable quick and accurate changes to the ROM settings as the rehabilitation protocol progresses.
- Types:
- Straps:
- Materials: High-grade neoprene, elasticized fabrics, or silicone-lined straps are common. These materials are chosen for their elasticity, durability, and ability to provide secure compression without constricting circulation.
- Functionality: Multiple straps (typically 4-6) encircle the thigh and calf, anchoring the brace to the limb. They are designed to prevent brace migration, ensuring the hinges remain correctly aligned with the knee's axis of rotation.
- Features: Quick-release buckles facilitate easy application and removal. Padded sections enhance comfort and prevent skin irritation.
- Pads/Liners:
- Materials: Breathable, moisture-wicking foam (e.g., open-cell foam, EVA foam) or silicone-based materials. Many are hypoallergenic.
- Functionality: These soft interfaces between the brace frame/straps and the skin provide cushioning, distribute pressure evenly, and manage perspiration, crucial for prolonged wear and skin integrity. They are often removable for cleaning.
- Overall Ergonomics: Modern braces prioritize a low-profile, lightweight design that minimizes bulk and allows for wear under loose clothing. Bilateral use (adaptable for either leg) is a common feature, simplifying inventory for clinics.
Biomechanics of Controlled Range of Motion
The biomechanical principles governing ROM knee braces are fundamental to their therapeutic action:
- Protection of Healing Tissues: By restricting movement beyond safe limits, the brace prevents excessive tensile or compressive forces on healing ligaments, menisci, and cartilage. For example, after an ACL reconstruction, limiting full extension prevents undue stress on the graft, while restricting deep flexion protects meniscal repairs from shear forces.
- Prevention of Excessive Stress: The rigid frame and controlled hinges absorb external forces that might otherwise impact the healing joint, such as accidental bumps or twists.
- Facilitating Early, Controlled Mobilization: While protection is key, complete immobilization can lead to joint stiffness (arthrofibrosis) and muscle atrophy. The brace allows for carefully prescribed, incremental increases in ROM, which is vital for:
- Cartilage Nutrition: Movement helps circulate synovial fluid, nourishing articular cartilage.
- Collagen Fiber Alignment: Controlled stress can guide the proper alignment of collagen fibers during tissue remodeling.
- Prevention of Adhesions: Early movement helps prevent the formation of scar tissue adhesions that can restrict motion.
- Proprioception and Stability: The external support and slight compression from the brace can enhance proprioceptive feedback to the brain, improving the patient's awareness of their knee's position and contributing to a sense of stability, which is especially important during ambulation.
Extensive Clinical Indications & Usage
Post-operative ROM knee braces are prescribed across a wide spectrum of orthopedic knee surgeries, each with specific protocols dictating brace settings and duration.
Detailed Surgical Applications
| Surgical Procedure | Primary Goal of Bracing | Typical ROM Protocol Considerations |
|---|---|---|
| ACL Reconstruction | Protect graft, prevent hyperextension, controlled flexion progression | Initial: 0°-90° flexion, gradually increasing. Often locked in extension for ambulation initially. Duration: 4-6 weeks (or longer). |
| PCL Reconstruction | Protect graft, prevent posterior tibial sag, limit deep flexion | Initial: Often restricted to 0°-60° or 0°-90° flexion. Posterior support pads may be used. Duration: 6-12 weeks. |
| MCL/LCL Repair/Reconstruction | Stabilize collateral ligaments, prevent varus/valgus stress | Initial: Limited flexion/extension to protect healing ligaments, often locked for weight-bearing. Gradual increase. Duration: 4-8 weeks. |
| Meniscus Repair | Protect repair site from shear & compression forces | Initial: Limited flexion (e.g., 0°-30° or 0°-90°), restricted weight-bearing in flexion. Duration: 4-6 weeks, sometimes longer. |
| Patellar Tendon Repair | Protect repair, control knee extension | Initial: Locked in extension or slight flexion (e.g., 0°-30°), gradual increase in flexion. Duration: 6-8 weeks. |
| Osteochondral Autograft/Allograft (OATS) | Protect cartilage repair, limit weight-bearing & shear forces | Initial: Non-weight-bearing, limited ROM (e.g., 0°-30°). Gradual increase in ROM and weight-bearing. Duration: 6-12 weeks. |
| High Tibial Osteotomy (HTO) / Distal Femoral Osteotomy (DFO) | Protect bone healing, maintain alignment | Initial: Locked in extension for weight-bearing, gradual increase in flexion as bone heals. Duration: 6-12 weeks or until bone union. |
| Knee Fracture Management (non-surgical or post-fixation) | Immobilize fracture, protect healing bone | Protocols vary widely based on fracture type. May involve initial complete immobilization, then controlled ROM. Duration: Weeks to months. |
Fitting and Usage Instructions
Correct fitting and consistent usage are paramount for brace effectiveness and patient comfort.
Pre-fitting Considerations:
- Patient Measurement: Precise measurements of thigh circumference, calf circumference, and limb length (from mid-thigh to mid-calf) are crucial to select the correct brace size.
- Limb Edema: Account for potential post-operative swelling, which may fluctuate.
- Skin Integrity: Inspect the skin for any pre-existing wounds, rashes, or pressure areas that might be exacerbated by the brace.
Step-by-Step Application:
- Positioning: The patient should be seated or lying down comfortably with the knee slightly bent (if allowed).
- Brace Placement: Position the brace on the leg so that the hinges are perfectly aligned with the center of the knee joint (epicondyles). The frame should run along the sides of the leg, not directly over the patella.
- Strap Sequence:
- Proximal Straps (Thigh): Secure the strap closest to the groin first, ensuring it's snug but not overly tight. Then secure the next thigh strap.
- Distal Straps (Calf): Secure the strap closest to the ankle, followed by the next calf strap.
- Mid-Calf/Thigh Straps: Secure any remaining straps.
- General Rule: Often, securing from proximal to distal (thigh to calf) is recommended, but always follow manufacturer guidelines or your orthotist's specific instructions.
- Fit Check:
- Ensure the brace is snug enough to prevent migration but not so tight as to cause discomfort, skin blanching, or restrict circulation.
- Check that the hinges remain aligned with the knee joint during gentle flexion and extension within the allowed ROM.
- There should be no pinching or excessive pressure points.
- ROM Settings: Confirm the flexion and extension limits are set precisely according to the surgeon's or physical therapist's prescribed protocol.
- Patient Education: Instruct the patient on:
- How to don and doff the brace correctly.
- The importance of wearing the brace exactly as prescribed (e.g., continuously, during ambulation only, during sleep).
- How to check for skin irritation and what to do if it occurs.
- Weight-bearing status and activity restrictions.
Duration of Use:
The duration for which a ROM knee brace is worn is highly individualized, depending on the type of surgery, the surgeon's protocol, the patient's healing progress, and their adherence to rehabilitation. It can range from a few weeks to several months.
Maintenance and Sterilization Protocols
Proper maintenance ensures the longevity, hygiene, and continued effectiveness of the brace.
- Daily Care:
- Wipe down the rigid frame and hinges with a damp cloth to remove sweat and debris.
- Inspect straps for fraying or damage.
- Check hinge mechanisms for smooth operation and ensure ROM stops are securely locked.
- Cleaning Liners/Pads:
- Most soft goods (liners, pads) are removable and should be hand-washed with mild soap (e.g., baby shampoo or gentle detergent) and lukewarm water.
- Rinse thoroughly and air dry completely away from direct heat or sunlight to prevent material degradation. Do NOT machine wash or tumble dry unless explicitly stated by the manufacturer.
- Skin Care: Regularly inspect the skin under the brace for redness, irritation, or breakdown. Clean and dry the skin thoroughly before reapplying the brace. A thin, moisture-wicking sock or sleeve can sometimes be worn under the brace for added comfort and skin protection, if approved by the clinician.
- Professional Maintenance: If the brace becomes damaged, hinges malfunction, or if the fit changes significantly (due to swelling reduction or weight changes), consult an orthotist or your orthopedic team for adjustment or repair.
- Sterilization (for multi-patient use - rare for post-op ROM braces): Post-operative ROM braces are almost exclusively single-patient use. If, in a rare clinical scenario, a brace needs to be repurposed, rigorous disinfection protocols would be required for the frame using hospital-grade disinfectants, and all soft goods would need to be replaced. This is generally not recommended due to the risk of cross-contamination and the customized fit required for each patient.
Risks, Side Effects, or Contraindications
While highly beneficial, ROM knee braces are not without potential risks or side effects, and certain conditions may contraindicate their use.
- Skin Irritation/Pressure Sores: The most common side effect. Improper fit, brace migration, excessive strap tightness, or material sensitivity can lead to redness, chafing, blistering, or even pressure ulcers, especially over bony prominences.
- Nerve Compression: Overtightening of straps, particularly around the fibular head (lateral aspect of the knee), can compress the common peroneal nerve, leading to numbness, tingling, or weakness in the foot (foot drop).
- Deep Vein Thrombosis (DVT): While the brace itself doesn't directly cause DVT, any prolonged immobilization, combined with potential improper fit that impedes circulation, could theoretically contribute. The brace should never be so tight as to restrict blood flow. Early controlled movement, as facilitated by the brace, and prescribed anti-coagulation are often used to mitigate DVT risk.
- Muscle Atrophy: Any period of immobilization or reduced activity can lead to muscle wasting. While the brace allows for controlled movement, it still limits full, unrestricted activity. This is addressed through a structured physical therapy program.
- Joint Stiffness (Arthrofibrosis): If the ROM progression is too slow, or if the patient is non-compliant with their physical therapy, the knee can become stiff, requiring more aggressive rehabilitation or even further intervention.
- Discomfort/Pain: Some patients may experience general discomfort, especially during the initial adjustment period. Pain should be reported to the medical team immediately.
- Brace Migration: If not fitted correctly, the brace can slide up or down the leg, compromising its effectiveness and potentially causing skin irritation.
Contraindications:
* Open Wounds: The brace should not be applied directly over open wounds, active infections, or severe skin conditions in the area of brace application.
* Severe Peripheral Vascular Disease: Conditions that severely compromise circulation in the limb may be a contraindication due to the risk of exacerbating ischemia.
* Compartment Syndrome: The brace should not be used if there is a risk of or existing compartment syndrome.
* Patient Non-Compliance: If a patient is unable or unwilling to follow instructions for brace wear and care, the risks may outweigh the benefits.
Massive FAQ Section
Here are some frequently asked questions regarding Post-Operative ROM Knee Braces:
1. What is the primary purpose of a post-operative ROM knee brace?
The primary purpose is to protect the surgically repaired knee joint from excessive stress, provide stability, and allow for a carefully controlled and progressive range of motion during the healing and rehabilitation process. This prevents re-injury while facilitating optimal recovery.
2. How long will I need to wear my knee brace?
The duration of brace wear is highly individualized and depends on your specific surgery, the surgeon's protocol, and your healing progress. It can range from a few weeks to several months. Always adhere strictly to your surgeon's or physical therapist's instructions regarding wear time.
3. Can I take my brace off to shower or sleep?
This depends entirely on your surgeon's specific post-operative protocol. In many cases, you may be instructed to keep the brace on even during sleep, especially in the early stages, to protect the knee. For showering, you might be allowed to remove it, but often with specific instructions on how to keep the knee protected. Always clarify these instructions with your medical team.
4. How do I clean my knee brace?
The rigid frame can be wiped down with a damp cloth. The soft pads and liners are usually removable and should be hand-washed with mild soap and lukewarm water, then air-dried completely. Avoid machine washing or drying, and harsh chemicals, unless explicitly stated by the manufacturer. Regular cleaning prevents skin irritation and maintains hygiene.
5. What are the adjustable ROM settings for?
The adjustable range of motion (ROM) settings on the brace hinges allow your surgeon or physical therapist to precisely control how far your knee can bend (flexion) and straighten (extension). These settings are crucial for protecting healing tissues and gradually increasing your mobility as your recovery progresses, according to a carefully planned rehabilitation protocol.
6. How do I know if my brace is fitted correctly?
A correctly fitted brace should feel snug and secure, preventing it from sliding up or down your leg, but it should not feel uncomfortably tight or cause any pinching or numbness. The hinges should align perfectly with the center of your knee joint. If you experience pain, numbness, tingling, or significant discomfort, contact your orthopedic team or orthotist immediately.
7. What should I do if my brace causes skin irritation?
If you notice redness, chafing, or irritation, first ensure the brace is not too tight and is properly positioned. You can try wearing a thin, seamless, moisture-wicking sleeve or stockinette under the brace. If irritation persists or worsens, or if you develop blisters or open sores, contact your medical team immediately. Do not self-treat severe skin issues.
8. Can I drive while wearing my knee brace?
Generally, it is not recommended to drive while wearing a post-operative knee brace, especially if it's on your right leg (for automatic vehicles) or either leg (for manual vehicles). The brace can restrict your ability to safely operate pedals or react quickly in an emergency. Always consult your surgeon before resuming driving.
9. Will the brace restrict my ability to walk or do physical therapy?
Yes, the brace is designed to restrict certain movements to protect your knee. While it allows for controlled walking and specific physical therapy exercises within the prescribed ROM limits, it will prevent full, unrestricted movement. This restriction is temporary and necessary for optimal healing. Your physical therapist will guide you through exercises compatible with your brace settings.
10. Is it normal for my knee to swell while wearing the brace?
Some degree of swelling is normal after knee surgery, and the brace itself might contribute to minor swelling if it's slightly too tight or if it's worn for extended periods without elevation. However, excessive or sudden increase in swelling, accompanied by severe pain, redness, or warmth, should be reported to your surgeon immediately as it could indicate a complication.
11. What materials are typically used in these braces?
Post-operative ROM knee braces commonly feature frames made from lightweight aluminum alloys or carbon fiber composites for strength and durability. Straps often use neoprene or elasticized fabrics, and soft pads/liners are typically made from breathable, moisture-wicking foams or silicone for comfort and skin protection.
12. How does the brace protect my knee after surgery?
The brace protects your knee by providing external stability, limiting excessive or uncontrolled movements (like hyperextension or deep flexion) that could stress healing tissues, and absorbing external impacts. Its rigid frame and adjustable hinges ensure that your knee only moves within a safe, prescribed range, allowing your surgical repair to heal without disruption.