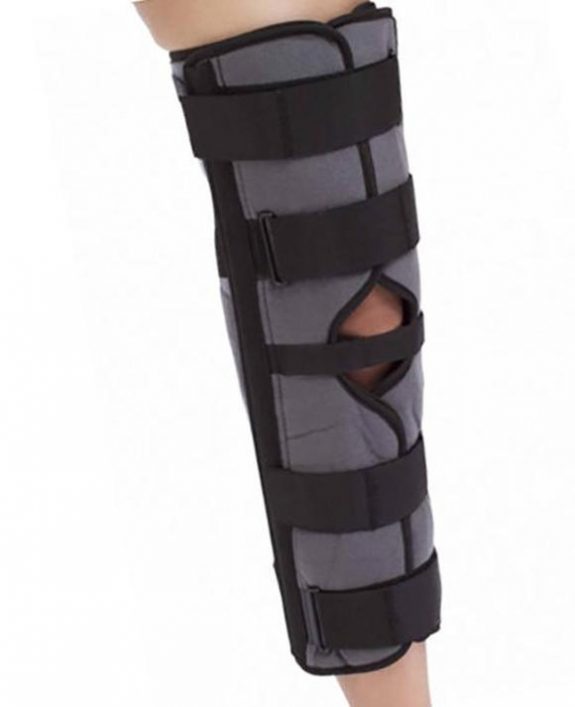
The Knee Immobilizer (Zimmer Splint): A Comprehensive Orthopedic Guide
The knee joint, a marvel of biomechanical engineering, is susceptible to a wide range of injuries and conditions, from acute trauma to degenerative diseases. In many scenarios, effective immobilization is a cornerstone of conservative management and post-operative recovery. Among the most widely recognized and utilized devices for this purpose is the Knee Immobilizer, often colloquially referred to as a Zimmer Splint. This exhaustive guide delves into every facet of the Knee Immobilizer, providing authoritative insights for patients, caregivers, and healthcare professionals alike.
1. Comprehensive Introduction & Overview
A Knee Immobilizer is an orthopedic assistive device designed to provide rigid support and stabilization to the knee joint, limiting its range of motion, particularly flexion and extension. Its primary objective is to hold the knee in a straight, extended position (typically 0-20 degrees of flexion), thereby minimizing movement, reducing pain, preventing further injury, and creating an optimal environment for healing.
While often called a "Zimmer Splint" due to the historical prominence of Zimmer Biomet in orthopedic devices, the term broadly refers to any rigid knee immobilizer. These devices are indispensable in both pre-hospital emergency care and long-term rehabilitation settings. They serve as a temporary solution for acute injuries, a protective measure post-surgery, and a supportive aid during periods of severe pain or instability. By restricting unwanted movement, the immobilizer effectively unloads stress from damaged tissues, promotes proper alignment, and facilitates the body's natural healing processes.
2. Deep-Dive into Technical Specifications & Mechanisms
The efficacy of a Knee Immobilizer lies in its thoughtful design and the biomechanical principles it employs.
2.1 Design and Materials
Knee immobilizers are typically composed of several key components working in concert to provide robust support:
- Rigid Stays: These are the backbone of the immobilizer, usually made from lightweight yet strong materials like aluminum or reinforced plastic. They run vertically along the posterior and sometimes medial/lateral aspects of the leg, providing structural integrity and preventing knee flexion. Modern designs often incorporate malleable stays that can be contoured slightly by a clinician to fit individual patient anatomy.
- Circumferential Straps: Multiple adjustable straps, commonly made of durable nylon or elastic webbing with hook-and-loop (Velcro) closures, encircle the leg at various points (thigh, knee, calf). These straps secure the rigid stays against the limb, ensuring a snug fit and preventing migration of the splint.
- Padding and Lining: The interior of the immobilizer is lined with soft, breathable foam padding or a fabric blend. This serves several critical functions:
- Comfort: Prevents direct contact between rigid components and skin.
- Pressure Distribution: Minimizes pressure points, reducing the risk of skin irritation or breakdown.
- Moisture Wicking: Some advanced materials help manage sweat and heat, enhancing patient comfort during prolonged wear.
- Outer Fabric: Often a durable, washable fabric (e.g., polyester, nylon blend) that encases the padding and provides structural support for the straps.
Immobilizers come in various lengths (e.g., 12", 16", 20", 24") to accommodate different patient heights and injury locations, ensuring the splint extends adequately above and below the knee joint for effective immobilization.
2.2 Biomechanics
The Knee Immobilizer functions through several biomechanical principles:
- Three-Point Fixation: The primary mechanism involves three points of pressure: one superior to the knee (on the distal thigh), one inferior to the knee (on the proximal calf), and one at the knee joint itself (often anteriorly). These points create a stabilizing force that resists unwanted flexion or extension.
- Prevention of Flexion/Extension: By maintaining the knee in a neutral or slightly extended position, the immobilizer effectively eliminates the leverage required for knee movement. This is crucial for protecting healing ligaments, tendons, and bony structures.
- Reduction of Rotational Forces: While not its primary design feature, a well-fitted immobilizer can offer some resistance to excessive internal or external rotation of the tibia relative to the femur, which can be detrimental in certain injuries (e.g., multi-ligament tears).
- Load Distribution: The broad surface area of the immobilizer helps to distribute pressure evenly around the limb, reducing localized stress on any single point, which is particularly important over bony prominences.
2.3 Mechanism of Action
The core mechanism of a Knee Immobilizer is straightforward:
- Immobilization: It mechanically restricts movement of the tibiofemoral and patellofemoral joints, holding the knee in a desired, often fully extended, position.
- Pain Relief: By preventing movement of injured tissues, it significantly reduces nociceptive input (pain signals) from mechanoreceptors and free nerve endings. This reduction in movement also minimizes muscle spasm, a common source of pain post-injury.
- Protection: It acts as an external shield, protecting the injured knee from accidental bumps, knocks, or inadvertent movements that could compromise healing or cause re-injury.
- Facilitation of Healing: By providing a stable environment, the immobilizer allows damaged tissues (ligaments, tendons, bone) to heal without mechanical disruption, promoting proper collagen formation and tissue remodeling.
3. Extensive Clinical Indications & Usage
Knee immobilizers are versatile tools in orthopedic practice, indicated for a wide array of conditions.
3.1 Detailed Surgical Applications
Post-operative immobilization is critical for protecting surgical repairs and reconstructions during the initial healing phase.
| Surgical Procedure | Rationale for Immobilizer Use |
|---|---|
| ACL/PCL Reconstruction | Protects graft integrity, limits early stress, prevents excessive anterior/posterior tibial translation. |
| Meniscus Repair | Safeguards repair site, prevents shear forces and extreme flexion that could disrupt sutures. |
| Patellar Fracture Fixation | Stabilizes the patella, prevents knee flexion that could displace fragments or stress fixation hardware. |
| Tibial Plateau Fractures | Post-surgical stabilization, maintains alignment, offloads articular surface during initial healing. |
| Quadriceps/Patellar Tendon Repair | Protects the repaired tendon from tensile forces during knee flexion, allowing for robust healing. |
| Osteochondral Repair | Prevents weight-bearing and shear forces on the repaired cartilage, promoting integration of graft/repair. |
| Total Knee Arthroplasty (TKA) | Occasionally used in immediate post-op to manage severe pain, swelling, or if early ROM is contraindicated. |
3.2 Non-Surgical/Clinical Applications
Knee immobilizers are also invaluable in managing acute injuries and chronic conditions conservatively.
- Acute Knee Sprains/Strains: Especially for Grade II or III collateral ligament (MCL, LCL) injuries, providing stability and pain relief.
- Patellar Subluxation/Dislocation: Immobilizes the knee in extension to allow soft tissue healing around the patella, preventing recurrence in the acute phase.
- Acute Arthritis Flares: For severe flare-ups of conditions like gout or osteoarthritis, temporary immobilization can significantly reduce pain and inflammation.
- Osgood-Schlatter Disease (Severe): In adolescents with severe pain and inflammation at the tibial tubercle, immobilization can provide symptomatic relief.
- Suspected Fractures: Used in emergency settings to stabilize the knee during transport, preventing further damage to bone, soft tissues, and neurovascular structures.
- Pre-operative Stabilization: To manage pain and protect an injured knee while awaiting surgical intervention.
3.3 Fitting and Usage Instructions
Proper fitting is paramount for the immobilizer's effectiveness and patient comfort.
- Pre-fitting Assessment:
- Measurement: Measure the length of the leg from the groin fold to just above the ankle. Select an immobilizer length that extends approximately 2-3 inches above the knee and 2-3 inches below, ensuring adequate leverage.
- Circumference: Note the circumference of the thigh and calf to ensure appropriate strap length and overall fit.
- Skin Integrity: Inspect the skin for any pre-existing wounds, rashes, or pressure areas.
- Application:
- Patient Positioning: Have the patient lie supine with the leg as straight as comfortably possible.
- Splint Placement: Position the posterior rigid stays centrally along the back of the leg, ensuring the knee joint is aligned with the center of the immobilizer.
- Secure Straps: Begin by securing the strap directly above the knee and then the strap directly below the knee. These are crucial for initial stabilization. Then, proceed to secure the proximal (thigh) and distal (calf) straps. Finally, secure any intermediate straps.
- Tightness Check: Ensure the straps are snug enough to prevent movement of the knee but not so tight as to cause discomfort, restrict circulation, or impede nerve function. A "two-finger rule" (being able to slide two fingers under the straps) is often a good guideline.
- Circulation and Sensation Check: Assess capillary refill in the toes, ask about numbness, tingling, or excessive coolness/warmth in the foot.
- Patient Education:
- Wearing Schedule: Adhere strictly to the prescribed wearing schedule (e.g., continuous wear, during ambulation only).
- Skin Care: Instruct the patient to perform daily skin checks for redness, irritation, or breakdown, especially over bony prominences (patella, tibial tuberosity, fibular head).
- Hygiene: Advise on how to manage personal hygiene (e.g., sponge baths, or temporary removal for showering if cleared by the surgeon).
- Activity Restrictions: Clearly communicate weight-bearing status, range of motion limitations, and prohibited activities.
- Warning Signs: Educate on signs requiring immediate medical attention: increased pain, numbness, tingling, swelling, coolness/blueness of the foot, or signs of DVT (see Risks section).
3.4 Patient Outcome Improvements
The judicious use of a Knee Immobilizer can significantly enhance patient outcomes:
- Enhanced Healing Environment: By providing a stable, protected environment, the immobilizer facilitates optimal biological healing of damaged tissues.
- Reduced Post-operative Pain: Immobilization minimizes movement-induced pain, leading to less reliance on analgesics and improved patient comfort.
- Prevention of Re-injury: It acts as a mechanical barrier, safeguarding the healing knee from accidental stresses or movements that could compromise surgical repairs or delay recovery.
- Improved Patient Confidence: Knowing the knee is protected can alleviate patient anxiety, allowing them to focus on other aspects of recovery.
- Facilitates Proper Tissue Alignment: In cases of fracture or ligamentous injury, it helps maintain anatomical alignment crucial for functional recovery.
4. Risks, Side Effects, or Contraindications
While beneficial, the use of a Knee Immobilizer is not without potential risks and contraindications.
4.1 Risks and Side Effects
- Skin Irritation and Pressure Sores: Prolonged pressure, especially over bony prominences (patella, fibular head, tibial tuberosity), can lead to redness, blistering, or even skin breakdown. Poor hygiene can exacerbate this.
- Deep Vein Thrombosis (DVT): Immobilization of a limb significantly increases the risk of DVT due to venous stasis. This is a serious complication requiring prompt medical attention.
- Muscle Atrophy: Disuse of the muscles supporting the knee joint can lead to rapid muscle wasting, particularly of the quadriceps.
- Joint Stiffness (Contractures): Prolonged immobilization can result in capsular and ligamentous shortening, leading to a loss of joint range of motion, particularly knee flexion contractures.
- Nerve Compression: Improper application or excessive tightness, especially around the fibular head, can compress the common peroneal nerve, leading to foot drop or sensory disturbances in the lower leg and foot.
- Swelling: While immobilization can help reduce inflammation, an overly tight splint can impede venous and lymphatic return, potentially exacerbating distal swelling.
- Psychological Impact: Patients may experience frustration, dependence, or a sense of confinement due to limited mobility.
4.2 Contraindications
- Certain Unstable Fractures: Some complex or highly unstable fractures may require alternative fixation methods (e.g., external fixators, internal plating) that allow for controlled movement or are incompatible with a standard immobilizer.
- Conditions Requiring Early Range of Motion: In some post-operative protocols (e.g., certain TKA or meniscectomy procedures), early, controlled range of motion is crucial to prevent stiffness and promote cartilage health. A rigid immobilizer would be contraindicated.
- Severe Peripheral Vascular Disease: In patients with compromised circulation, an immobilizer could further impair blood flow, leading to ischemic complications. Careful assessment is required.
- Open Wounds/Infections: An immobilizer should not be applied directly over open wounds or active infections without appropriate sterile dressings and careful monitoring, as it could trap moisture and impede wound healing.
- Allergic Reaction to Materials: Though rare, patients may exhibit allergic reactions to certain materials used in the splint.
5. Maintenance and Sterilization Protocols
Proper care of the Knee Immobilizer is essential for hygiene, durability, and preventing skin complications.
- Cleaning:
- Hand Washing: Most immobilizers are designed for hand washing with mild soap and lukewarm water. Avoid harsh detergents or bleach, which can degrade materials.
- Rinsing: Rinse thoroughly to remove all soap residue.
- Air Drying: Allow the immobilizer to air dry completely, preferably laid flat, away from direct sunlight or heat sources. Ensure the foam padding is entirely dry before reapplication to prevent skin maceration and bacterial growth.
- DO NOT Machine Wash/Dry: Machine washing can damage rigid stays, compromise foam integrity, and degrade Velcro closures. Tumble drying can shrink or melt materials.
- Inspection:
- Regular Checks: Periodically inspect the immobilizer for signs of wear and tear, such as frayed straps, weakened Velcro, bent or cracked rigid stays, or flattened/damaged padding.
- Replace if Damaged: A compromised immobilizer may not provide adequate support and should be replaced.
- Storage:
- Store the immobilizer flat or rolled loosely in a dry, clean place, away from direct sunlight or extreme temperatures when not in use.
- Patient Hygiene:
- Daily Skin Checks: Patients should be instructed to check their skin daily, especially over bony prominences, for any signs of redness, irritation, or breakdown.
- Undergarment: Wearing a thin, breathable cotton stockinette or sleeve underneath the immobilizer can help absorb moisture, reduce friction, and improve comfort. This undergarment should be changed and washed daily.
6. Frequently Asked Questions (FAQ)
Q1: What is a Knee Immobilizer (Zimmer Splint) used for?
A Knee Immobilizer is an orthopedic device used to keep the knee straight and still. It's commonly prescribed after knee surgery (like ACL repair or meniscus repair), for acute knee injuries (sprains, dislocations), or for fractures to prevent movement, reduce pain, and promote healing.
Q2: How long do I need to wear a Zimmer Splint?
The duration of wear varies significantly depending on the specific injury, surgical procedure, and your doctor's protocol. It could range from a few days for acute sprains to several weeks (typically 2-6 weeks) post-surgery. Always follow your orthopedic surgeon or physical therapist's instructions precisely.
Q3: Can I take off my Zimmer Splint to shower?
In most cases, you should NOT remove your immobilizer without explicit permission from your doctor or surgeon. Removing it too early or incorrectly could jeopardize the healing process or re-injure the knee. If permitted, you might be advised to take sponge baths or use a waterproof cover for showering. Always consult your healthcare provider first.
Q4: What should I do if my Zimmer Splint feels too tight or causes pain?
If your immobilizer feels too tight, causes numbness, tingling, increased pain, or noticeable swelling below the knee, loosen the straps slightly. If symptoms persist or worsen, contact your doctor immediately. These could be signs of nerve compression or circulatory issues.
Q5: How do I clean my Knee Immobilizer?
Most knee immobilizers can be hand washed with mild soap and lukewarm water. Rinse thoroughly and allow it to air dry completely before re-applying. Do NOT machine wash or tumble dry, as this can damage the rigid stays, padding, and Velcro.
Q6: Can I sleep with my Zimmer Splint on?
Yes, in most cases, you will be required to sleep with your Zimmer Splint on, especially during the initial phase of recovery or if your doctor has prescribed continuous wear. This prevents inadvertent movements during sleep that could disrupt healing.
Q7: What are the signs of a DVT (Deep Vein Thrombosis) to look out for?
Signs of a DVT, a serious complication of immobility, include sudden onset of swelling, pain, tenderness, warmth, or redness in the calf or thigh. If you experience any of these symptoms, seek immediate medical attention.
Q8: Will wearing a Zimmer Splint weaken my leg muscles?
Yes, prolonged immobilization can lead to muscle atrophy (weakening) due to disuse, particularly of the quadriceps. Your doctor or physical therapist will guide you on appropriate exercises or a rehabilitation program to regain strength once the immobilizer is removed.
Q9: When can I start physical therapy after wearing a splint?
The timing for starting physical therapy is highly individualized. It depends on your injury, the surgical procedure (if applicable), and your surgeon's specific protocol. Many protocols incorporate early, controlled range of motion exercises, sometimes even while still wearing the immobilizer, while others require complete immobilization for a period before therapy begins.
Q10: Is a Zimmer Splint the same as a knee brace?
No, while both support the knee, they serve different primary functions. A Knee Immobilizer (Zimmer Splint) provides rigid, complete immobilization, preventing almost all movement. A knee brace, particularly a functional brace, allows for controlled range of motion, often used to support and protect the knee during activity or specific phases of rehabilitation.
Q11: Can I drive while wearing a Knee Immobilizer?
Generally, no. Wearing a knee immobilizer significantly restricts your ability to operate the brake or accelerator pedals safely and effectively. Driving with an immobilizer on your driving leg is usually illegal and highly unsafe. Always consult your doctor regarding when it is safe to resume driving.
Q12: What's the difference between a custom brace and an off-the-shelf immobilizer?
An off-the-shelf immobilizer is a pre-manufactured device available in standard sizes, chosen based on general measurements. A custom brace is specifically molded or fabricated to fit an individual's unique anatomy, often providing a more precise fit and higher level of support for complex injuries or specific functional needs. Knee immobilizers are typically off-the-shelf, while complex functional knee braces can be custom-made.