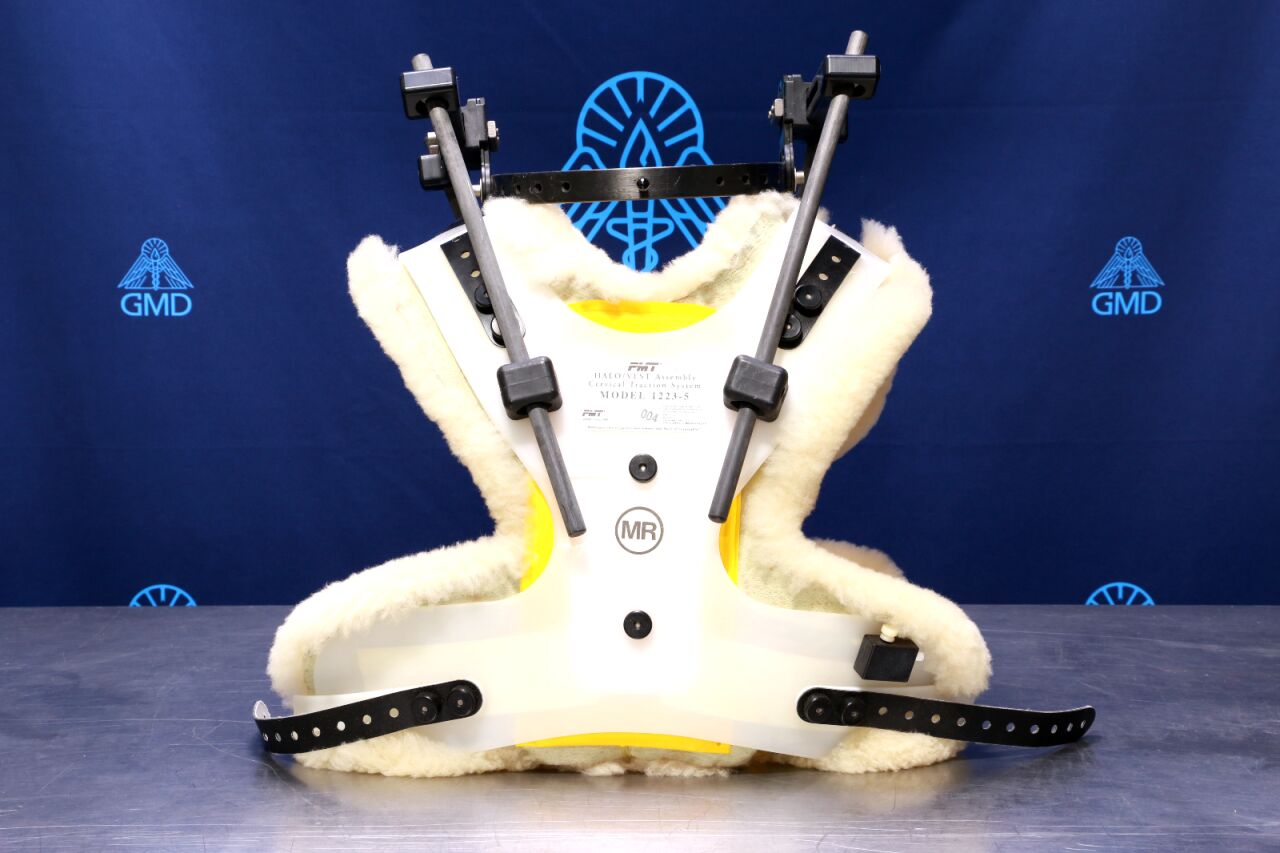
The Halo Vest Immobilizer System: A Comprehensive Orthopedic Guide
Introduction & Overview
The Halo Vest Immobilizer System stands as a cornerstone in the non-operative and post-operative management of severe cervical (neck) and upper thoracic spine injuries. Representing the gold standard for external spinal immobilization, this sophisticated device provides unparalleled rigidity, significantly restricting motion in all planes. Developed in the mid-20th century, its design has evolved to enhance patient comfort and efficacy, offering a critical alternative or adjunct to surgical intervention for a range of complex spinal pathologies.
At its core, the Halo Vest System comprises a lightweight, circumferential metal ring (the "halo") secured directly to the skull via a series of specialized pins. This halo is then meticulously connected by adjustable upright rods to a padded, supportive plastic vest worn around the patient's torso. This intricate three-point fixation system effectively isolates the cervical spine, creating a stable environment conducive to healing and preventing further neurological compromise. As expert orthopedic specialists, we understand the profound impact this device has on patient outcomes, transforming potentially devastating injuries into manageable conditions with favorable recovery prospects.
Deep-Dive into Technical Specifications & Mechanisms
The efficacy of the Halo Vest Immobilizer is rooted in its ingenious design and the biomechanical principles it employs. Understanding its components and how they interact is crucial for both clinicians and patients.
Design & Materials
The Halo Vest System is a complex assembly of specialized components, each engineered for specific functions:
-
Halo Ring:
- Material: Typically crafted from lightweight, radiolucent materials such as graphite, carbon fiber composites, or aluminum alloys. Some older or specialized rings may be titanium. These materials allow for clear imaging (X-ray, CT, MRI) without significant artifact.
- Structure: A rigid, circumferential ring designed to fit snugly around the patient's head, positioned above the eyebrows and below the greatest circumference of the skull.
- Pin Holes: Contains multiple evenly spaced holes (typically 8-12) for the insertion of skull pins.
-
Skull Pins:
- Material: Made from biocompatible, high-strength materials like titanium or stainless steel to minimize tissue reaction and ensure secure purchase in the skull.
- Design: Self-tapping, conical tips designed for controlled penetration into the outer cortical bone of the skull. They often feature a blunt or rounded tip after the thread to prevent over-penetration.
- Number & Placement: Typically 4 to 8 pins are used. Anterior pins are placed in the superolateral aspect of the orbital rim, avoiding the supraorbital nerves and temporal arteries. Posterior pins are placed in the posterolateral aspect of the skull, avoiding the mastoid process and major vessels.
- Torque Settings: Applied with a specialized torque wrench to a precise setting (e.g., 6-8 inch-pounds for adults) to ensure adequate purchase without over-tightening, which could lead to bone necrosis or pin loosening.
-
Uprights (Rods):
- Material: High-strength, lightweight materials such as carbon fiber or aluminum, offering rigidity and adjustability.
- Function: Connect the halo ring to the thoracic vest. They are typically four rods (two anterior, two posterior) that can be adjusted in length and angle to achieve optimal spinal alignment and immobilization.
- Connectors: Feature universal joints or locking mechanisms to allow for precise positioning and secure fastening.
-
Thoracic Vest:
- Material: Molded from rigid thermoplastics like polyethylene or polypropylene, designed to conform to the patient's torso.
- Lining: Lined with soft, breathable materials such as sheepskin, synthetic foam, or specialized moisture-wicking fabrics to prevent skin breakdown and enhance comfort. These linings are often removable for cleaning or replacement.
- Straps & Buckles: Multiple adjustable straps with quick-release buckles ensure a snug, secure fit, distributing pressure evenly across the torso.
-
Specialized Tools:
- Torque Wrench/Driver: Essential for controlled pin insertion and tightening, ensuring consistent pressure and preventing overtightening.
- Hex Wrenches: Used for adjusting and tightening the various bolts and connectors on the uprights and vest.
Biomechanics
The biomechanical superiority of the Halo Vest System lies in its ability to create a rigid, three-dimensional skeletal fixation that effectively neutralizes motion in the cervical spine.
- Rigid Fixation: By directly attaching to the skull, the halo bypasses soft tissue and provides a direct interface with the skeletal system. This allows for superior control compared to collars that rely on external pressure.
- Three-Point Fixation: The system operates on a principle of three-point fixation:
- Proximal Anchor: The halo ring, securely fixed to the skull.
- Distal Anchor: The thoracic vest, securely fixed to the torso.
- Connecting Elements: The adjustable uprights, which bridge the halo and vest, maintaining a fixed relationship between the head and torso.
- Motion Restriction: This rigid connection effectively eliminates or severely limits motion in all cardinal planes:
- Flexion/Extension: The anterior and posterior uprights prevent forward and backward bending.
- Lateral Bending: The side uprights and the overall rigidity prevent side-to-side bending.
- Rotation: The circumferential fixation of the halo and the fixed relationship with the vest virtually eliminate rotational movement.
- Force Distribution: Forces transmitted through the cervical spine are largely absorbed and distributed by the Halo Vest System, offloading the injured vertebral segments. This provides a stable environment for bone and ligamentous healing.
- Superior Immobilization: Compared to soft collars (e.g., soft foam collars), semi-rigid collars (e.g., Philadelphia collar), or even rigid cervicothoracic orthoses (e.g., SOMI brace), the Halo Vest offers the highest degree of immobilization, typically restricting cervical motion to less than 1-3 degrees in all planes.
Extensive Clinical Indications & Usage
The Halo Vest Immobilizer is a critical tool in the management of a variety of complex cervical spine conditions, both acute and chronic.
Detailed Surgical or Clinical Applications
The primary indications for a Halo Vest are conditions requiring maximal external cervical spine immobilization, often to promote healing without surgery or to augment post-surgical stability.
- Unstable Cervical Spine Fractures:
- Atlas (C1) Fractures: Especially Jefferson fractures (burst fractures of C1) that are stable or minimally displaced.
- Axis (C2) Fractures:
- Odontoid Fractures: Type II and Type III odontoid fractures (fractures of the dens) are common indications, particularly in younger patients where fusion is undesirable or in older patients where surgical risks are high.
- Hangman's Fractures: Traumatic spondylolisthesis of C2, where the Halo Vest can provide stability and promote healing of the pedicle fractures.
- Subaxial Cervical Fractures (C3-C7): Certain stable or minimally displaced burst fractures, compression fractures, or lamina fractures that demonstrate instability but are deemed suitable for non-operative management.
- Cervical Dislocations/Subluxations:
- Unilateral or bilateral facet dislocations that have been successfully reduced, requiring prolonged stabilization to prevent recurrence and allow ligamentous healing.
- Post-Surgical Stabilization:
- Following cervical fusion procedures (anterior or posterior) to provide additional external support during the initial healing phase, particularly in cases of multi-level fusion, poor bone quality, or high-risk patients.
- After decompression surgeries where immediate stability is paramount.
- Severe Ligamentous Injuries:
- Disruptions of the transverse ligament, alar ligaments, or other critical stabilizing ligaments of the craniocervical junction or subaxial spine, where surgical repair is not immediately indicated or feasible.
- Cervical Spondylosis with Instability:
- In rare cases, severe degenerative changes leading to instability might be managed with a Halo Vest if surgical intervention is contraindicated.
- Tumors Affecting Cervical Stability:
- To provide palliative stabilization and pain relief in patients with metastatic disease affecting cervical vertebrae, where surgical fixation is not an option.
- Congenital Anomalies:
- Conditions like os odontoideum or other developmental abnormalities leading to craniocervical instability, often used in pediatric populations.
Fitting & Usage Instructions (Clinical & Patient)
Clinical Application (Performed by Trained Medical Professionals):
- Patient Positioning: Patient is supine, head in neutral alignment, often with gentle cervical traction if needed for reduction.
- Halo Ring Placement: The halo ring is carefully positioned around the skull, typically 1 cm above the eyebrows anteriorly and above the tip of the ears laterally, ensuring it clears the temporal arteries.
- Pin Site Preparation: Scalp at pin sites is shaved (if necessary), meticulously cleaned, and sterilized. Local anesthetic is injected at each pin site.
- Pin Insertion: Pins are advanced through the outer cortical bone of the skull. A specialized torque wrench is used to tighten each pin to the prescribed inch-pounds (e.g., 6-8 in-lbs for adults, 2-4 in-lbs for children), ensuring secure purchase without over-tightening. Pins are often tightened in a diagonal pattern to ensure even pressure.
- Vest Application: The thoracic vest is applied to the torso, ensuring a snug but comfortable fit. The sheepskin or foam lining is positioned to prevent pressure points.
- Upright Connection & Alignment: The four upright rods are attached to the halo ring and then to the vest. They are adjusted to achieve neutral cervical spine alignment, verified by lateral X-rays. The rods are tightened securely.
- Final Checks: All screws and bolts are double-checked for tightness. Post-application X-rays are taken to confirm spinal alignment and ensure no pin penetration into the cranial cavity.
Patient Daily Usage & Instructions:
- Hygiene:
- Bathing: Sponge baths are necessary. Hair can be washed by leaning the head back over a sink with assistance, ensuring the vest remains dry.
- Vest Care: The vest lining should be changed or cleaned regularly (e.g., weekly) to prevent skin irritation and odor. The plastic vest can be wiped clean with a damp cloth and mild soap.
- Pin Site Care:
- Daily Cleaning: Pin sites must be cleaned daily with sterile saline, hydrogen peroxide (diluted), or an antiseptic solution as instructed by the medical team. Use sterile cotton swabs to gently clean around each pin, removing any crusts or drainage.
- Monitoring: Inspect pin sites for signs of infection (redness, swelling, warmth, pain, pus). Report any concerns immediately.
- No Manipulation: Do not touch or manipulate the pins or attempt to tighten them.
- Sleeping: Sleep on your back with pillows supporting the head and neck to maintain alignment. A small pillow or rolled towel can be placed under the shoulders to prevent the head from tilting forward.
- Dressing: Wear loose-fitting, button-down shirts or oversized garments that can be put on over the vest.
- Mobility:
- Walking: Walk carefully, using handrails or assistance, as balance may be affected.
- Driving: Driving is strictly prohibited due to severely restricted head movement.
- Diet & Swallowing: Eating and swallowing may initially feel awkward. Soft foods may be easier to consume. Report persistent difficulty swallowing or breathing to your doctor.
- Psychological Support: Wearing a Halo Vest can be challenging. Seek support from family, friends, and healthcare providers. Counseling may be beneficial.
- Emergency Contact: Keep emergency contact information readily available.
Patient Outcome Improvements
The Halo Vest Immobilizer significantly contributes to positive patient outcomes in several critical ways:
- Enhanced Spinal Stability: Provides the most rigid form of external immobilization, creating an optimal environment for bone and ligamentous healing.
- Reduced Pain: By stabilizing the injured segments, the Halo Vest minimizes movement-induced pain, improving patient comfort.
- Prevention of Further Neurological Damage: Crucially, it prevents harmful motion that could exacerbate existing spinal cord injury or cause new neurological deficits.
- Avoidance of More Invasive Surgery: For many unstable fractures, the Halo Vest allows for successful non-operative management, avoiding the risks and recovery time associated with surgical fusion.
- Improved Functional Recovery: By promoting proper healing and preventing complications, patients often achieve better long-term functional recovery and a higher quality of life post-removal.
- High Success Rates: For appropriately selected odontoid fractures (Type II and III), non-operative management with a Halo Vest can yield success rates of 70-90%.
Maintenance & Sterilization Protocols
Proper maintenance and hygiene are paramount to prevent complications and ensure the Halo Vest's effectiveness.
Pin Site Care
- Daily Cleaning: As described above, daily cleaning with an antiseptic solution (e.g., chlorhexidine or diluted hydrogen peroxide) and sterile cotton swabs is essential.
- Observation: Meticulously inspect each pin site daily for:
- Redness
- Swelling
- Warmth
- Pus-like discharge
- Increased pain
- Loosening of the pin (a gap between the skin and the halo ring).
- Reporting: Any signs of infection or a loose pin must be reported to the orthopedic team immediately. Prompt intervention can prevent serious complications like osteomyelitis or intracranial infection.
- Antibiotic Ointment: If prescribed, a thin layer of topical antibiotic ointment may be applied to pin sites after cleaning.
- No Removal/Tightening by Patient: Patients must never attempt to remove or tighten the pins themselves.
Vest Care
- Lining Hygiene: The vest lining (sheepskin, foam) should be kept clean and dry. Many linings are removable and washable (following manufacturer instructions) or can be wiped clean. Linings should be changed if they become soiled or worn.
- Plastic Vest Cleaning: The rigid plastic vest can be wiped down with a damp cloth and mild soap. Ensure it is thoroughly dried afterward.
- Strap Inspection: Regularly check the straps and buckles for wear, fraying, or damage. Ensure they remain securely fastened and at the appropriate tension.
- Avoid Moisture: Keep the vest as dry as possible to prevent skin maceration and irritation.
Professional Checks
- Regular Follow-ups: Patients require regular follow-up appointments with their orthopedic surgeon or spine specialist.
- Pin Tightening: Pins may require periodic re-tightening by the medical team to their original torque settings, especially in the first few weeks as soft tissue swelling subsides.
- Vest Adjustments: The vest may need minor adjustments to maintain optimal fit and comfort as the patient's body adapts.
- Radiographic Monitoring: Serial X-rays or CT scans are often performed to monitor spinal alignment and assess fracture healing progress.
Risks, Side Effects, or Contraindications
While highly effective, the Halo Vest Immobilizer is not without potential risks and side effects. Patient selection and meticulous care are crucial.
Risks & Side Effects
- Pin Site Infection: The most common complication, ranging from superficial cellulitis to osteomyelitis or, rarely, intracranial infection.
- Pin Loosening: Can occur due to inadequate torque, bone resorption, or patient activity, leading to loss of immobilization. Requires re-tightening or replacement.
- Skin Breakdown/Pressure Sores: Can develop under the vest, especially over bony prominences, if the vest is too tight, ill-fitting, or if the lining is soiled/wet.
- Nerve Damage:
- Supraorbital Nerve Palsy: If anterior pins are placed too low or medial.
- Facial Nerve Damage: Rare, if pins are placed incorrectly near the temporal bone.
- Cranial Nerve Palsies: Extremely rare, but possible with improper pin placement.
- Dural Penetration/Intracranial Injury: Extremely rare but serious complication if pins are over-tightened or inserted incorrectly, potentially leading to CSF leak, meningitis, or brain injury.
- Difficulty Swallowing (Dysphagia) / Breathing: The vest and halo can restrict neck movement and occasionally compress the airway or esophagus, especially in patients with pre-existing conditions.
- Discomfort & Pain: Patients often experience discomfort or localized pain at pin sites, which usually subsides but can persist.
- Psychological Impact: The visible and restrictive nature of the halo can lead to anxiety, depression, claustrophobia, and body image issues.
- Falls: Altered balance and restricted head movement increase the risk of falls, especially in elderly patients.
- Scarring: Small scars may remain at the pin sites after removal.
- Halo Displacement: In rare instances, the entire halo apparatus can shift or become dislodged, requiring immediate medical attention.
Contraindications
- Severe Head Trauma with Elevated Intracranial Pressure (ICP): The halo ring can potentially impede venous outflow or worsen ICP.
- Unstable Skull Fractures: The presence of skull fractures at or near potential pin sites contraindicates halo application.
- Active Scalp or Pin Site Infection: An existing infection must be treated before halo application.
- Morbid Obesity: Difficult to achieve a secure and comfortable fit of the vest, increasing the risk of skin complications and ineffective immobilization.
- Severe Osteoporosis: Compromised bone quality may lead to poor pin purchase, increased risk of pin loosening, and complications.
- Patient Non-Compliance/Cognitive Impairment: Patients must be able to understand and adhere to strict care instructions. Non-compliance significantly increases complication risks.
- Certain Types of Cervical Instability Requiring Immediate Surgical Fixation: Some highly unstable or irreducible injuries are better managed surgically from the outset.
- Severe Burns or Skin Conditions: Extensive burns or dermatological issues on the scalp or torso may preclude halo application.
Massive FAQ Section
Here are some frequently asked questions regarding the Halo Vest Immobilizer System:
1. What is a Halo Vest Immobilizer used for?
A Halo Vest is primarily used for rigid immobilization of the cervical (neck) and upper thoracic spine. It's indicated for severe cervical spine fractures, dislocations, ligamentous injuries, and for post-surgical stabilization to promote healing and prevent further injury.
2. How long do I need to wear a Halo Vest?
The duration of wear varies depending on the specific injury, patient's healing rate, and the orthopedic surgeon's assessment. Typically, it is worn for 8 to 12 weeks, but it can range from 6 weeks to 3-4 months. Regular X-rays will monitor bone healing.
3. Can I shower with a Halo Vest?
No, you cannot take a traditional shower or submerge the vest in water. The vest and pin sites must be kept dry to prevent skin irritation and infection. Sponge baths are recommended, and hair washing can be done by leaning your head back over a sink with assistance, ensuring the vest remains dry.
4. How do I clean the pin sites?
Pin sites must be cleaned daily with sterile saline, diluted hydrogen peroxide, or an antiseptic solution as instructed by your medical team. Use a sterile cotton swab to gently clean around each pin, removing any crusts or drainage. Always wash your hands thoroughly before and after pin care.
5. What are the signs of a pin site infection?
Signs of a pin site infection include increased redness, swelling, warmth, tenderness, pus-like drainage, or fever. If you notice any of these symptoms, contact your orthopedic team immediately.
6. Can I sleep on my side with a Halo Vest?
It is generally recommended to sleep on your back while wearing a Halo Vest to maintain proper spinal alignment. You can use pillows to support your head and neck comfortably. Sleeping on your side can put undue pressure on the vest and potentially compromise spinal alignment.
7. Will I be able to drive or work with a Halo Vest?
No, driving is strictly prohibited while wearing a Halo Vest due to the severe restriction of head and neck movement, which impairs your ability to safely operate a vehicle. The ability to work depends entirely on your job's physical demands; most physically active jobs will be impossible, while some sedentary roles might be possible with accommodations.
8. How is the Halo Vest removed?
The Halo Vest is removed in a clinical setting by your orthopedic team. The pins are loosened and removed, the halo ring is detached from the uprights, and then the vest is taken off. This process is usually quick and causes minimal discomfort. You may feel a sensation of lightness or instability immediately after removal.
9. What should I do if a pin becomes loose?
If a pin feels loose, wiggles, or if you notice a gap between the pin and your skin, contact your orthopedic team immediately. Do not attempt to tighten it yourself. A loose pin can compromise immobilization and increase the risk of infection.
10. Is the Halo Vest painful?
Initial discomfort and localized pain at the pin sites are common, especially in the first few days after application. This pain usually subsides and can be managed with prescribed pain medication. If you experience severe or increasing pain, report it to your doctor.
11. Are there any dietary restrictions while wearing a Halo Vest?
Generally, there are no specific dietary restrictions. However, some patients may find it initially difficult to chew or swallow due to restricted head movement. Opting for softer foods or smaller bites can help. Maintain a healthy, balanced diet to support healing.
12. What activities are restricted while wearing a Halo Vest?
Most strenuous activities are restricted. This includes lifting heavy objects, bending, twisting, running, jumping, swimming, and any contact sports. Your balance will be affected, so avoid uneven surfaces and use caution when walking. Your medical team will provide specific activity guidelines tailored to your recovery.