Introduction and Epidemiology
Bilateral cervical facet dislocation represents a severe, high-energy injury to the cervical spine, characterized by complete disruption of the posterior ligamentous complex and often associated with significant anterior subluxation of the superior vertebral body on the inferior. These injuries typically result from a combination of hyperflexion and distraction forces, commonly seen in motor vehicle collisions, falls from height, or diving accidents. Due to the profound ligamentous instability, bilateral cervical facet dislocation inherently carries a high risk of spinal cord injury, with reported neurological deficit rates ranging from 40% to 70% at presentation. The extent of neurological compromise can range from transient radiculopathy to complete tetraplegia, underscoring the urgency and criticality of expert management.
Epidemiologically, cervical spine trauma constitutes a significant portion of all spinal injuries, with facet dislocations accounting for approximately 10% to 20% of these cases. While unilateral facet dislocations are more common and typically result from flexion-rotation mechanisms, bilateral dislocations are indicative of greater force vectors across the sagittal plane and thus produce more severe three-column instability. The C5-C6 and C6-C7 levels are most frequently involved due to their greater mobility, acting as transitional zones between the highly mobile upper cervical spine and the relatively rigid thoracic spine.
Patient demographics typically follow a bimodal distribution. The first peak occurs in young adult males (ages 15 to 35) subjected to high-velocity blunt trauma. The second peak is observed in the elderly population (over 65 years of age), where lower-energy mechanisms such as ground-level falls can induce catastrophic failure of the cervical column due to pre-existing spondylosis, ankylosing spondylitis, or diffuse idiopathic skeletal hyperostosis. Prompt diagnosis, meticulous neurological assessment utilizing the American Spinal Injury Association Impairment Scale, and timely, appropriate surgical intervention are paramount to optimize patient outcomes, decompress neural elements, and prevent further neurological deterioration secondary to secondary injury cascades.
Surgical Anatomy and Biomechanics
A thorough understanding of cervical spine anatomy and biomechanics is fundamental to managing bilateral cervical facet dislocation. The subaxial cervical spine comprises vertebrae C3 through C7, each articulating through anterior intervertebral discs and paired posterior zygapophyseal joints. The facet joints are true diarthrodial synovial joints, formed by the superior articular process of the vertebra below and the inferior articular process of the vertebra above. Their orientation, typically 45 degrees to the horizontal plane in the coronal axis, allows for significant flexion, extension, lateral bending, and coupled rotation, but also dictates their vulnerability to dislocation under extreme shear and tensile loads.
Key supporting structures defining the stability of the cervical column include the anterior longitudinal ligament which resists extension, and the posterior longitudinal ligament which resists flexion. The posterior ligamentous complex is the primary tension band of the cervical spine, comprising the ligamentum flavum, interspinous ligaments, supraspinous ligaments, and the facet joint capsules. The capsular ligaments enclose the facet joints, providing significant stability against translation and rotation. The intervertebral discs contribute significantly to anterior column stability and bear axial compressive loads.
In bilateral cervical facet dislocation, the mechanism involves severe hyperflexion with simultaneous distraction. This aligns with Stage 3 or Stage 4 of the Allen and Ferguson mechanistic classification for Distraction-Flexion injuries. This force vector leads to complete, catastrophic disruption of the posterior ligamentous complex. As the energy propagates anteriorly, the posterior longitudinal ligament and the intervertebral disc annulus fail. The anterior longitudinal ligament may also be stripped from the periosteum or completely torn.
The facet joints become completely dislocated, with the inferior articular processes of the superior vertebra translating anteriorly and superiorly over the superior articular processes of the inferior vertebra. They ultimately drop into the intervertebral foramina, creating a locked configuration. This profound instability results in significant anterior translation of the superior vertebral body, often exceeding 50% of the vertebral body width on lateral radiography.
The integrity of the intervertebral disc is frequently compromised, with a reported incidence of traumatic disc herniation ranging from 30% to 60% of cases. The potential for the herniated disc material to retropulse into the spinal canal upon reduction is a critical consideration. If closed reduction is attempted in an awake patient, continuous neurological monitoring is mandatory. If attempted under general anesthesia without prior magnetic resonance imaging, unappreciated disc retropulsion can lead to acute, irreversible neurological deterioration. Furthermore, the vertebral arteries, ascending through the foramina transversaria from C6 to C1, are at risk of traction injury, dissection, or occlusion due to the severe sagittal translation.
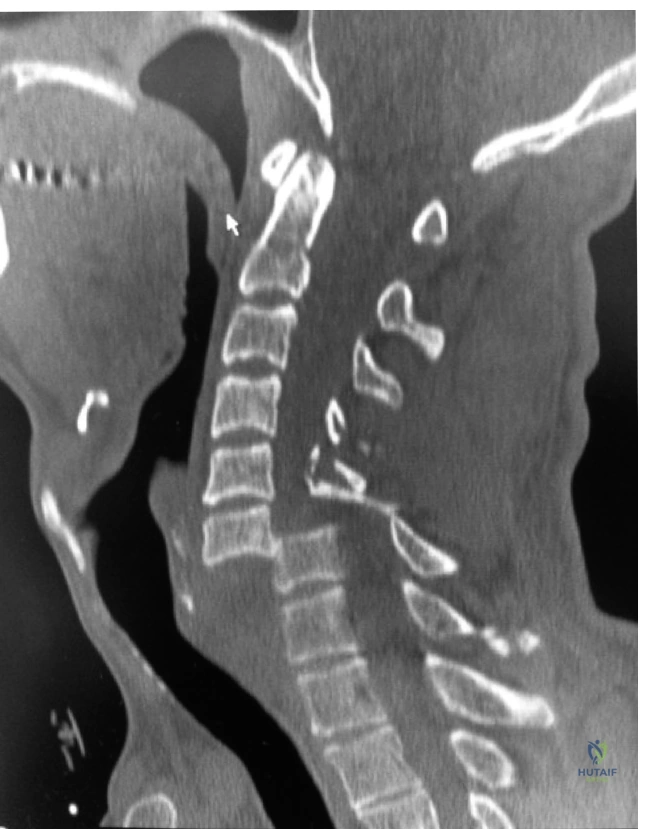
The image below illustrates the complex anatomical relationships in the cervical spine during a dislocation event.
Indications and Contraindications
The management of bilateral cervical facet dislocation is almost exclusively operative. The complete disruption of the posterior tension band and the anterior disc space renders the segment grossly unstable, failing all criteria for clinical and radiographic stability as defined by Panjabi and White. Non-operative management is historically associated with unacceptable rates of progressive kyphotic deformity, chronic pain, and delayed neurological deterioration.
The primary goals of intervention are immediate realignment of the spinal canal, decompression of the spinal cord and nerve roots, and rigid internal fixation to facilitate early mobilization. The Subaxial Cervical Spine Injury Severity score assigns a minimum of 8 points to a bilateral facet dislocation (3 points for morphology, 2 points for complete posterior ligamentous complex disruption, and at least 3 points for complete spinal cord injury or incomplete spinal cord injury), heavily favoring surgical intervention.
| Clinical Scenario | Operative Indication | Non Operative Indication | Rationale |
|---|---|---|---|
| Neurologically Intact with Locked Facets | Urgent Open Reduction and Internal Fixation | Contraindicated | Prevent delayed spinal cord injury; restore biomechanical stability. |
| Incomplete Spinal Cord Injury | Emergent Surgical Decompression and Stabilization | Contraindicated | Maximize potential for neurological recovery; halt secondary injury cascade. |
| Complete Spinal Cord Injury | Urgent Surgical Decompression and Stabilization | Contraindicated | Facilitate early mobilization; improve nursing care; prevent ascending edema. |
| Severe Medical Comorbidities or Moribund Status | Relative Contraindication | Halo Vest Immobilization | Surgical risk outweighs benefit; palliative or temporizing measure only. |
| Traumatic Disc Herniation present on MRI | Anterior Approach for Discectomy prior to Reduction | Contraindicated | Prevent retropulsion of disc material into the cord during reduction maneuvers. |
Contraindications to surgical intervention are exceedingly rare and generally limited to patients who are medically unstable to tolerate anesthesia, those with unsurvivable concomitant traumatic injuries, or patients who have explicitly documented advance directives refusing surgical intervention.
Pre Operative Planning and Patient Positioning
Thorough preoperative imaging is mandatory. Standard trauma protocols dictate initial non-contrast computed tomography of the cervical spine. Computed tomography provides superior bony detail, confirming the locked status of the facets, identifying associated lamina or pedicle fractures, and quantifying the degree of anterolisthesis.
The role and timing of magnetic resonance imaging remain highly debated. For awake, alert, and cooperative patients, rapid closed reduction via cranial traction (Gardner-Wells tongs) can be attempted prior to magnetic resonance imaging, provided serial neurological examinations are performed after each weight addition. If the patient is uncooperative, intoxicated, or comatose, magnetic resonance imaging must be obtained prior to any reduction attempt to evaluate for a traumatic disc herniation. If a massive disc herniation is present behind the intact posterior longitudinal ligament, an anterior cervical discectomy must be performed before reduction to prevent catastrophic cord compression.
Vascular imaging, such as computed tomography angiography, should be considered if there is a high index of suspicion for vertebral artery injury, particularly in cases involving severe translation, facet fractures extending into the foramen transversarium, or unexplained neurological deficits discordant with the spinal cord injury level.
Patient positioning is dictated by the chosen surgical approach.
For an anterior approach, the patient is positioned supine on a radiolucent Jackson table. A bump is placed between the scapulae to facilitate cervical extension, though extreme caution must be exercised to avoid exacerbating the deformity before decompression. The head is supported on a foam donut or secured with Mayfield tongs if intraoperative traction is required. The shoulders are taped down to allow adequate lateral fluoroscopic visualization of the lower cervical spine.
For a posterior approach, the patient is intubated supine (often requiring awake fiberoptic intubation with manual in-line stabilization). Mayfield skull clamps are applied, and the patient is carefully flipped prone onto a Jackson frame. The neck is maintained in a neutral position. Reverse Trendelenburg positioning can help decrease venous engorgement and minimize intraoperative bleeding.
Detailed Surgical Approach and Technique
The choice of surgical approach—anterior, posterior, or combined—depends on the presence of disc herniation, the ease of reduction, the quality of the bone, and the surgeon's preference.
Anterior Approach and Anterior Cervical Discectomy and Fusion
The anterior approach utilizes the standard Smith-Robinson technique. A transverse incision is made within a skin crease on the side of the surgeon's preference, typically corresponding to the C5-C6 or C6-C7 level. The platysma is divided in line with the incision. The superficial layer of the deep cervical fascia is incised anterior to the sternocleidomastoid muscle.
The internervous plane is developed between the sternocleidomastoid and the carotid sheath laterally, and the strap muscles, trachea, and esophagus medially. The pretracheal fascia is divided, and the prevertebral fascia is exposed. The longus colli muscles are identified bilaterally and mobilized laterally using electrocautery to create a safe bed for retractor placement, ensuring the sympathetic chain is protected.
Once the correct level is confirmed via fluoroscopy, a complete discectomy is performed. In the setting of bilateral cervical facet dislocation, the disc is often completely disrupted. The posterior longitudinal ligament is resected to ensure no disc fragments have migrated into the epidural space.
Reduction is then achieved. Caspar distraction pins are placed into the vertebral bodies above and below the dislocation. The pins must be placed parallel to the endplates and convergent in the axial plane. Distraction is applied. A Cobb elevator or a specialized reduction tool can be inserted into the disc space to gently lever the superior vertebral body posteriorly while the distraction unlocks the facets. Once reduced, the distraction is released, and the alignment is confirmed fluoroscopically.
An interbody graft (allograft or synthetic cage) is sized and impacted into the disc space. An anterior cervical plate is then secured to the anterior vertebral bodies with fixed or variable angle screws, providing immediate anterior column stabilization.
Posterior Approach and Lateral Mass Fixation
If an anterior approach fails to achieve reduction, or if there is no disc herniation and the primary pathology is purely posterior ligamentous disruption, a posterior approach may be utilized.
A midline longitudinal incision is made through the ligamentum nuchae. Subperiosteal dissection is carried out bilaterally, stripping the paraspinal musculature off the spinous processes, laminae, and lateral masses to the lateral border of the facet joints. Care must be taken to preserve the facet capsules of the adjacent, uninjured levels to prevent iatrogenic instability.
To reduce the locked facets, a Penfield number 4 or a small Cobb elevator is carefully introduced between the dislocated articular processes. The superior articular process of the inferior vertebra is levered posteriorly and inferiorly, while the inferior articular process of the superior vertebra is coaxed anteriorly and superiorly. If manual leverage fails, a partial superior facetectomy of the inferior vertebra may be required to uncouple the locked joints.
Once reduced, lateral mass screw fixation is performed. The Magerl technique is commonly employed: the starting point is 1 millimeter medial and 1 millimeter cephalad to the center of the lateral mass. The trajectory is 25 degrees lateral (to avoid the vertebral artery) and parallel to the superior articular facet in the sagittal plane (typically 20 to 30 degrees cephalad, avoiding the exiting nerve root). Alternatively, the Roy-Camille technique utilizes a starting point at the exact center of the lateral mass with a straight anterior trajectory.

Following screw placement, titanium or cobalt-chrome rods are contoured to match the physiological cervical lordosis and secured with set screws. The posterior elements are then decorticated using a high-speed burr, and bone graft (autograft from the spinous processes or allograft) is packed over the decorticated lateral masses and within the facet joints to promote a robust posterolateral arthrodesis.
Combined Anterior and Posterior Approaches
A combined 360-degree approach (anterior-posterior or posterior-anterior-posterior) is indicated in cases of severe instability, osteoporosis where screw purchase is compromised, or when an anterior reduction fails, necessitating a posterior release followed by anterior grafting and plating. While biomechanically superior, offering the highest pullout strength and rotational stability, combined approaches significantly increase operative time, blood loss, and perioperative morbidity.
Complications and Management
Surgical management of bilateral cervical facet dislocation is fraught with potential complications due to the proximity of critical neurovascular structures and the high-energy nature of the initial trauma. Meticulous surgical technique and rigorous postoperative monitoring are essential.
| Complication | Estimated Incidence | Salvage Strategy and Management |
|---|---|---|
| Neurological Deterioration | 1% to 3% | Immediate cessation of reduction maneuver. Ensure MAP > 85 mmHg. Obtain emergent MRI to rule out epidural hematoma or disc retropulsion. Re-explore and decompress if indicated. |
| Vertebral Artery Injury | 0.5% to 2% | Intraoperative: Control bleeding with hemostatic agents, tamponade, or direct repair if accessible. Postoperative: Endovascular embolization or stenting. Monitor for posterior circulation stroke. |
| C5 Nerve Root Palsy | 5% to 10% | Often secondary to cord shift or root tethering post-reduction. Typically managed conservatively with physical therapy. Most cases spontaneously resolve within 6 to 12 months. |
| Dysphagia | 10% to 30% (Anterior) | Usually transient secondary to esophageal retraction. Manage with soft diet, speech therapy evaluation, and short-term corticosteroids. Severe cases may require enteral feeding. |
| Recurrent Laryngeal Nerve Palsy | 1% to 5% (Anterior) | Presents as hoarseness. Otolaryngology evaluation for vocal cord assessment. Often transient, but permanent injury may require vocal cord injection or medialization thyroplasty. |
| Hardware Failure or Pseudoarthrosis | 2% to 5% | Monitor radiographically. If symptomatic or progressive deformity occurs, revision surgery with extension of fusion construct or combined anterior-posterior approach is required. |
| Surgical Site Infection | 1% to 4% | Superficial: Oral antibiotics. Deep: Emergent surgical debridement, hardware retention (if stable), and prolonged culture-directed intravenous antibiotic therapy. |
Post Operative Rehabilitation Protocols
The immediate postoperative phase is typically managed in an intensive care unit setting, particularly for patients presenting with spinal cord injury. Hemodynamic management is critical; current guidelines recommend maintaining the Mean Arterial Pressure greater than 85 mmHg for 7 days post-injury to optimize spinal cord perfusion and minimize the penumbra of ischemic secondary injury.
Immobilization strategies depend on the rigidity of the fixation. With modern segmental instrumentation (anterior plating or posterior lateral mass screws), a rigid cervical orthosis (such as an Aspen or Miami J collar) is typically utilized for 6 to 12 weeks primarily for comfort and to limit extremes of motion while the arthrodesis matures. In cases of combined 360-degree fusion, collar use may be abbreviated.
Mobilization should begin as soon as hemodynamically and neurologically tolerated. For patients with complete spinal cord injuries, early mobilization into a wheelchair is vital to prevent decubitus ulcers, deep vein thrombosis, and pulmonary complications. Deep vein thrombosis prophylaxis should be initiated within 72 hours of surgery, provided there is no evidence of expanding epidural hematoma.
Radiographic follow-up includes upright anteroposterior and lateral cervical spine radiographs prior to discharge, at 6 weeks, 3 months, 6 months, and 1 year postoperatively. These imaging modalities assess the maintenance of sagittal alignment, hardware integrity, and the progression of bony fusion. Dynamic flexion-extension radiographs are typically obtained at the 3-month mark to confirm segmental stability before discontinuing the cervical orthosis.
Summary of Key Literature and Guidelines
The management of bilateral cervical facet dislocation is guided by several pivotal studies and established guidelines within the orthopedic and neurosurgical literature.
The Surgical Timing in Acute Spinal Cord Injury Study (STASCIS) revolutionized the approach to cervical spine trauma. This prospective, multicenter cohort study demonstrated that early surgical decompression (within 24 hours of injury) in patients with acute spinal cord injury resulted in significantly improved neurological outcomes at 6-month follow-up compared to delayed decompression, without an increase in complication rates. This cemented the paradigm of emergent surgical intervention for facet dislocations presenting with neurological deficits.
The Subaxial Cervical Spine Injury Severity (SLIC) classification, developed by Vaccaro et al., provides a validated, reliable algorithm for surgical decision-making. By incorporating injury morphology, integrity of the discoligamentous complex, and neurological status, the SLIC system objectively quantifies the severity of bilateral facet dislocations. As previously noted, these injuries universally score high enough to mandate surgical stabilization, standardizing treatment protocols across trauma centers.
The controversy surrounding the timing of magnetic resonance imaging in relation to closed reduction was extensively evaluated by Vaccaro and colleagues. Their research highlighted the high incidence of traumatic disc herniations associated with facet dislocations. The current consensus guidelines recommend that in the awake, neurologically examinable patient, closed reduction can be performed safely prior to magnetic resonance imaging. However, in the obtunded patient, magnetic resonance imaging is an absolute prerequisite before any reduction maneuver to prevent iatrogenic spinal cord injury from an unappreciated herniated disc.
Finally, biomechanical studies by Panjabi and White remain the foundational texts defining clinical instability of the cervical spine. Their criteria for posterior element disruption and sagittal translation dictate the necessity for rigid, multi-column internal fixation to restore the load-bearing capacity of the cervical axis following bilateral facet dislocation.
