Welcome, colleagues and fellows, to the operating theater. Today, we are undertaking a comprehensive exploration of a condition that frequently challenges the acumen of pediatric and sports medicine orthopaedic surgeons: Osteochondritis Dissecans (OCD) of the knee. This pathology remains a prevalent cause of knee pain, effusion, and mechanical dysfunction in our juvenile and adolescent patient populations. Mastering its arthroscopic management—specifically the nuanced decision-making between transarticular and retrograde drilling, as well as fragment fixation—is absolutely crucial for preserving long-term joint health and preventing early-onset osteoarthritis. This masterclass will provide an exhaustive, step-by-step technical guide to the operative management of OCD.
Comprehensive Introduction and Patho-Epidemiology
Osteochondritis Dissecans is defined as an acquired, potentially reversible, idiopathic focal lesion affecting the subchondral bone, which can subsequently lead to the delamination, instability, and eventual sequestration of the overlying articular cartilage. Historically, the nomenclature "osteochondritis" heavily implied a primary inflammatory etiology. However, contemporary histopathological analyses and advanced imaging have definitively shifted our understanding; inflammation is universally absent in the early stages. Instead, the pathology is fundamentally characterized by a failure of endochondral ossification or a focal subchondral osseous necrosis, leading to a structural compromise of the subchondral bone plate.
The precise etiology of OCD remains a subject of intense academic debate, though a multifactorial consensus has emerged. Chronic, repetitive microtrauma is currently the most widely accepted primary instigator. In the highly active pediatric population, repetitive impact loading generates shear stresses that exceed the remodeling capacity of the immature subchondral bone, leading to subchondral stress fractures. Vascular insufficiency is another critical component; the epiphyseal cartilage in a growing child has a tenuous blood supply, and microthrombosis or focal ischemia can precipitate localized bone death. Furthermore, a genetic predisposition is strongly suspected, particularly in families demonstrating bilateral presentations or multiple joint involvements, suggesting underlying variations in epiphyseal development or collagen matrix integrity.
Epidemiologically, we must strictly differentiate between Juvenile Osteochondritis Dissecans (JOCD), which occurs in patients with open physes, and Adult Osteochondritis Dissecans (AOCD), occurring post-physeal closure. JOCD has a significantly higher propensity for spontaneous healing with conservative management, whereas AOCD lesions are notoriously recalcitrant and frequently require surgical intervention. The incidence of JOCD has seen a measurable rise over the last two decades, a trend strongly correlated with the increasing prevalence of early single-sport specialization and year-round rigorous training regimens in youth athletics.
Clinically, the presentation of OCD exists on a spectrum dictated by the stability of the osteochondral fragment. Stable, intact lesions often present insidiously with vague, poorly localized anterior knee pain, often exacerbated by activity. Patients may exhibit a subtle antalgic gait or keep the knee externally rotated during ambulation to offload the classic medial femoral condyle lesion. The Wilson sign—pain elicited over the medial femoral condyle with internal tibial rotation during active knee extension from 90 degrees, which is relieved by external rotation—can be a helpful diagnostic adjunct, though its sensitivity is limited. Conversely, unstable lesions with chondral breaching present with pronounced mechanical symptoms, including locking, catching, palpable crepitus, and recurrent effusions, necessitating prompt surgical evaluation.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of knee osteology and soft tissue anatomy is paramount for safe and efficacious arthroscopic intervention. Our primary focus in this masterclass is the medial femoral condyle (MFC). Approximately 70% to 80% of all knee OCD lesions are localized to the lateral aspect of the MFC. This specific anatomical predilection is not coincidental; it corresponds precisely to the region of maximal contact stress against the tibial spine during the stance phase of gait, particularly when the knee is in internal rotation.
At the microstructural level, the operative zone encompasses the articular cartilage, the calcified tidemark, and the underlying subchondral bone. The articular surface is composed of hyaline cartilage, which relies on the diffusion of synovial fluid for nutrition. The subchondral bone provides the critical structural scaffolding. In OCD, the primary pathological process is localized to this subchondral bone. Our surgical objective during drilling procedures is to breach the sclerotic margin surrounding the necrotic subchondral crater, thereby creating vascular channels that allow for the influx of mesenchymal stem cells, angiogenic factors, and bone marrow elements to stimulate osseous remodeling and healing.
In the skeletally immature patient, the distal femoral physis (growth plate) represents the most critical anatomical hazard. The distal femoral physis is highly undulated, contributing up to 70% of the longitudinal growth of the femur and 40% of the overall growth of the lower extremity. Extreme caution, meticulous preoperative templating, and rigorous intraoperative fluoroscopic guidance are mandatory to avoid iatrogenic physeal arrest. When performing extra-articular (retrograde) drilling, the starting trajectory must be carefully established distal to the physis, typically utilizing the medial epicondyle as a safe landmark, to ensure the drill path remains entirely within the epiphysis.
Furthermore, the surgeon must maintain acute spatial awareness of the posterior neurovascular structures. The popliteal artery and vein, along with the tibial nerve, reside within the popliteal fossa, directly posterior to the posterior capsule. While standard anterior arthroscopic portals generally keep instruments well away from these structures, over-penetration during transarticular drilling—especially when addressing posterior lesions—poses a catastrophic risk. Drill bits must be equipped with depth stops, and the surgeon must possess an exact tactile understanding of the subchondral bone depth to prevent plunging through the posterior cortex of the femoral condyle.
Exhaustive Indications and Contraindications
The decision-making algorithm for the management of OCD is complex and heavily reliant on the patient's skeletal maturity, the clinical presentation, and the precise morphological characteristics of the lesion as defined by magnetic resonance imaging (MRI). Non-operative management, consisting of activity modification, protected weight-bearing, and immobilization, is the absolute first-line treatment for stable JOCD lesions. Surgical intervention is indicated only when a comprehensive trial of conservative management (typically 3 to 6 months) fails to yield clinical or radiographic improvement.
Operative indications are strictly defined. For stable lesions in skeletally immature patients that have failed conservative therapy, arthroscopic drilling is the gold standard. The choice between transarticular (ante-grade) and extra-articular (retrograde) drilling depends on the lesion's location and the status of the articular cartilage. Transarticular drilling is technically simpler but violates intact articular cartilage; it is generally reserved for skeletally mature patients or lesions located far anteriorly where the drill angle is perpendicular. Retrograde epiphyseal drilling is the procedure of choice for JOCD with intact cartilage, as it preserves the articular surface while decompressing the subchondral sclerosis, provided the physis can be safely avoided.
Unstable lesions—characterized by a breach in the articular cartilage, synovial fluid tracking behind the fragment on MRI, or frank separation—mandate surgical fixation or reconstruction. If the osteochondral fragment contains sufficient bone stock and the cartilage is viable, in situ fixation using bioabsorbable compression screws, darts, or variable-pitch titanium screws is indicated. If the fragment is fragmented, devoid of bone, or frankly necrotic, it must be excised, and the resulting defect managed with cartilage restoration techniques such as microfracture, Osteochondral Autograft Transfer System (OATS), or Matrix-Induced Autologous Chondrocyte Implantation (MACI).
Contraindications to joint-preserving OCD surgery include advanced, widespread osteoarthritic changes, active intra-articular infection, and severe, uncorrected malalignment (such as profound genu varum or valgum). In cases of significant mechanical axis deviation, an isolated cartilage procedure will invariably fail due to excessive localized contact pressures; a concomitant or staged corrective osteotomy (e.g., High Tibial Osteotomy or Distal Femoral Osteotomy) is an absolute prerequisite.
Indications and Contraindications Summary
| Category | Transarticular Drilling | Retrograde Drilling | Fragment Fixation | Salvage/Reconstruction (OATS/MACI) |
|---|---|---|---|---|
| Primary Indications | Failed conservative tx; Stable lesion; Skeletally mature (AOCD); Anterior lesions | Failed conservative tx; Stable lesion; Skeletally immature (JOCD); Intact cartilage | Unstable, salvageable fragment; Fluid behind lesion on MRI; Hinge lesions | Unsalvageable, fragmented, or missing lesion; Failed prior fixation |
| Contraindications | Open physes (relative); Posterior lesions (poor angle) | Lesions crossing the physis; Inadequate epiphyseal height | Fragmented, avascular, or purely chondral fragments | Active infection; Kissing lesions; Uncorrected malalignment |
| Key Advantage | Technically straightforward; Direct visualization | Preserves intact articular cartilage | Restores native articular congruity | Provides definitive biological resurfacing |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the cornerstone of a successful arthroscopic OCD intervention. The foundation of this planning relies on a comprehensive, high-quality imaging suite. Standard plain radiographs must include weight-bearing anteroposterior (AP), lateral, Merchant (patellofemoral), and posteroanterior (PA) flexion weight-bearing (notch or tunnel) views. The tunnel view is particularly critical, as the classic OCD lesion resides on the flexion weight-bearing surface of the lateral aspect of the medial femoral condyle, a region often obscured by the tibial plateau on a standard extension AP radiograph.
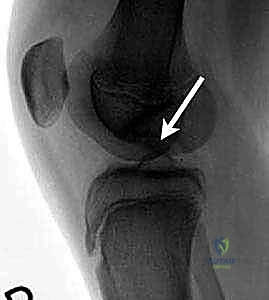
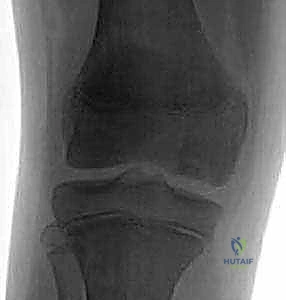
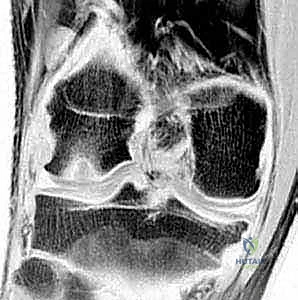
FIG 1 • AP (A), lateral (B), and Tunnel (C) radiographs of the knee demonstrating a classic osteochondritis dissecans lesion. The tunnel view is uniquely positioned to profile the flexion surface of the medial femoral condyle.
While radiographs provide the initial diagnosis, Magnetic Resonance Imaging (MRI) is the definitive modality for staging the lesion and dictating the surgical approach. We mandate high-resolution, non-contrast MRI with specific cartilage sequences (such as T2 mapping or delayed gadolinium-enhanced MRI of cartilage - dGEMRIC, if available). MRI accurately quantifies the dimensions of the osseous and chondral defects. Crucially, T2-weighted images are scrutinized for a high-signal intensity line tracking deep to the osteochondral fragment. This "fluid sign" unequivocally indicates instability and dictates that drilling alone will be insufficient; fixation or reconstruction is required.
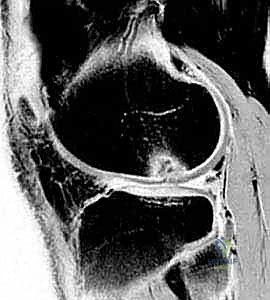
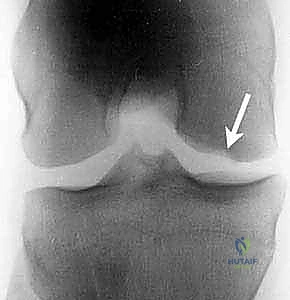
FIG 1 • D,E. T1-weighted and T2-weighted MR images of the knee demonstrating the precise extent of the osteochondritis dissecans lesion, allowing for evaluation of subchondral edema and fragment stability.
Patient positioning in the operating room must be standardized to ensure reproducible access and flawless fluoroscopic integration. The patient is positioned supine on a standard radiolucent operating table. We strongly advocate for the use of a thigh post or a circumferential leg holder positioned proximally on the thigh. This setup allows the knee to be manipulated through a full arc of motion—from full extension to hyperflexion (greater than 120 degrees)—which is absolutely necessary to bring posterior condylar lesions into the operative window of the anterior portals. A well-padded pneumatic tourniquet is applied to the proximal thigh to ensure a bloodless field during the critical phases of visualization and drilling.
Prior to sterile preparation, a rigorous Examination Under Anesthesia (EUA) is performed. The contralateral, unaffected knee is examined first to establish a baseline for physiological laxity. The operative knee is then evaluated for range of motion deficits, subtle effusions, and ligamentous instability. The C-arm fluoroscopy unit is brought into the field to confirm unimpeded access for perfect AP and lateral orthogonal imaging. The monitor must be positioned directly in the surgeon's line of sight. Only once the positioning, equipment, and imaging are verified do we proceed with the sterile prep and drape.
Step-by-Step Surgical Approach and Fixation Technique
The procedure commences with the establishment of standard anterolateral and anteromedial arthroscopic portals. The anterolateral portal serves as the primary viewing portal and is established first, utilizing a #11 blade to make a vertical incision adjacent to the lateral border of the patellar tendon. A blunt trocar is utilized to sweep the retropatellar fat pad anteriorly, minimizing iatrogenic trauma to the articular cartilage. The anteromedial portal is then established under direct intra-articular visualization utilizing a spinal needle to ensure optimal trajectory toward the OCD lesion.
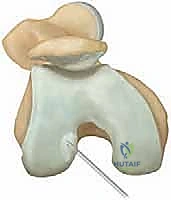
FIG 2 • Standard arthroscopic portals are utilized for visualization and instrumentation. Accessory portals may be localized via spinal needle to achieve a perpendicular approach to the lesion.
A systematic diagnostic arthroscopy is performed, evaluating all compartments. Upon reaching the medial compartment, the OCD lesion is meticulously evaluated. An arthroscopic probe is the most critical diagnostic tool at this stage. The surgeon must palpate the cartilage overlying the lesion, assessing for softening (malacia), ballotability, or frank breaching of the articular surface. The International Cartilage Repair Society (ICRS) classification is utilized intraoperatively to stage the lesion, grading it from intact but soft cartilage (Stage I) to a completely detached, loose osteochondral fragment (Stage IV).
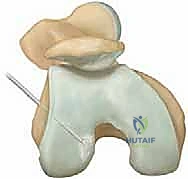
FIG 3 • Arthroscopic probing of the osteochondritis dissecans lesion. Tactile feedback is essential to determine the stability of the overlying articular cartilage.
Transarticular Drilling Technique
If the lesion is stable, the patient is skeletally mature, or the lesion is situated anteriorly enough to allow perpendicular access, transarticular drilling is executed. The objective is to penetrate the sclerotic subchondral bone base to stimulate vascular ingrowth. Using a 0.062-inch (1.6 mm) Kirschner wire or a specialized 1.5 mm cannulated drill bit, multiple perforations are made directly through the intact articular cartilage and into the subchondral bone.
The trajectory of the K-wire must be as perpendicular to the articular surface as possible to minimize chondral skiving and iatrogenic damage. The K-wire is advanced to a depth of approximately 15 to 20 mm, ensuring penetration past the sclerotic rim into healthy, vascularized cancellous bone. The surgeon will note a distinct change in resistance—a "give"—once the dense sclerotic bone is breached. Drilling is repeated systematically, creating a grid pattern with perforations spaced approximately 3 to 5 mm apart across the entire footprint of the lesion.
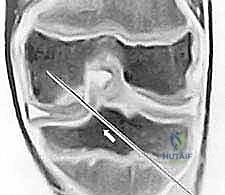


FIG 4 • Sequential steps of transarticular drilling. A K-wire is introduced perpendicularly through the cartilage, penetrating the sclerotic subchondral base in a systematic grid pattern to stimulate a healing response.
Retrograde (Epiphyseal) Drilling Technique
For the skeletally immature patient with an intact articular surface, retrograde drilling is the preferred, albeit technically demanding, alternative. This technique preserves the hyaline cartilage while decompressing the lesion. An anterior cruciate ligament (ACL) tibial or femoral aiming guide is frequently utilized. The intra-articular tip of the guide is placed precisely at the center of the OCD lesion. The extra-articular sleeve is positioned over the medial epicondyle, ensuring the starting point is strictly distal to the distal femoral physis.
Strict fluoroscopic control in both AP and lateral planes is non-negotiable during this step. A K-wire is advanced from the extra-articular starting point, through the epiphysis, and directed toward the subchondral sclerosis of the lesion. The surgeon must continuously verify that the wire trajectory does not violate the physis and does not breach the articular cartilage. Once the primary trajectory is confirmed, a cannulated drill is used to over-drill the K-wire, stopping millimeters short of the articular surface. Multiple divergent passes can be made from a single cortical entry point to thoroughly decompress the lesion.
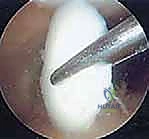
FIG 5 • Retrograde epiphyseal drilling utilizing an aiming guide and strict fluoroscopic imaging. The trajectory must remain distal to the physis and halt just prior to breaching the articular cartilage.
If the intraoperative assessment reveals an unstable but salvageable fragment (ICRS Stage III), in situ fixation is required. The fibrous tissue interposed between the fragment and the crater bed must be meticulously debrided using an arthroscopic shaver and curettes down to bleeding bone. The fragment is then reduced and provisionally stabilized with K-wires. Definitive fixation is achieved using bioabsorbable compression screws or headless titanium screws, countersunk below the level of the articular cartilage to prevent opposing "kissing" lesions on the tibial plateau.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, the arthroscopic management of OCD carries inherent risks. The most devastating complication in the pediatric population is iatrogenic physeal arrest, which can lead to progressive angular deformity or limb length discrepancy. The incidence of this complication is exceedingly low when strict fluoroscopic protocols are adhered to, but it underscores the necessity of maintaining a healthy respect for the undulations of the distal femoral physis during retrograde approaches.
Hardware-related complications are particularly prevalent when utilizing metallic or bioabsorbable fixation devices. Bioabsorbable screws can induce a sterile inflammatory response, leading to localized osteolysis or cyst formation. Metallic screws, if not adequately countersunk or if they back out postoperatively, will cause catastrophic mechanical abrasion to the opposing tibial articular cartilage. Furthermore, failure of the osteochondral fragment to unite (nonunion) occurs in approximately 10-20% of surgically treated AOCD cases, often resulting in fragment fragmentation and the generation of loose bodies within the joint space.
When primary drilling or fixation fails, or if the initial presentation involves a massive, unsalvageable crater, salvage procedures must be employed. Microfracture can be utilized for small defects (<2 cm²), but it yields mechanically inferior fibrocartilage. For larger defects, Osteochondral Autograft Transfer System (OATS) procedures—harvesting cylindrical osteochondral plugs from the non-weight-bearing periphery of the trochlea to fill the defect—provide excellent restoration of hyaline cartilage. For massive defects (>3-4 cm²), fresh osteochondral allografts or Matrix-Induced Autologous Chondrocyte Implantation (MACI) are the definitive salvage options, requiring a staged, open approach.
Complications and Management Strategies
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Iatrogenic Physeal Arrest | < 1% | Violation of physis during retrograde drilling | Epiphysiodesis (contralateral or completion); Corrective osteotomy |
| Hardware Prominence/Failure | 5 - 15% | Inadequate countersinking; Loss of fixation | Immediate arthroscopic hardware removal; Assess for chondral damage |
| Nonunion / Loose Body | 10 - 20% (AOCD) | Inadequate debridement of fibrous base; Poor vascularity | Fragment excision; OATS, MACI, or Fresh Osteochondral Allograft |
| Sterile Cystic Formation | 2 - 8% | Reaction to bioabsorbable implants (PLLA/PGA) | Observation if asymptomatic; Curettage and bone grafting if expansive |
Phased Post-Operative Rehabilitation Protocols
The surgical intervention is merely the first step; a rigidly adhered-to, phased postoperative rehabilitation protocol is equally critical to achieving a successful clinical outcome. The primary objective of the initial postoperative phase is the protection of the healing subchondral bone and the preservation of the articular cartilage surface, while simultaneously preventing joint stiffness and muscular atrophy.
Phase I: Maximal Protection (Weeks 0-6). Immediately postoperatively, the patient is placed in a hinged knee brace locked in extension for ambulation. Weight-bearing status is strictly dictated by the lesion location and the surgical intervention
