Introduction & Epidemiology
The intricate vascular network of the upper extremity is fundamental to its unique functionality, providing rich perfusion essential for a wide range of movements, sensory perceptions, and metabolic demands. For the orthopedic surgeon, a profound understanding of this vascular anatomy is not merely academic but critically important for safe and effective surgical intervention, particularly in the context of trauma, tumor resection, and reconstructive procedures. Ignorance or oversight of vascular structures can lead to devastating complications, including limb ischemia, loss of function, and, in severe cases, amputation.
Epidemiologically, vascular injuries of the upper extremity represent a significant portion of peripheral vascular trauma, with incidence rates varying based on the mechanism of injury. Penetrating trauma (e.g., stab wounds, gunshot wounds) is a common etiology, but blunt trauma (e.g., dislocations, complex fractures, crush injuries) also carries a substantial risk. Iatrogenic vascular injury, though less common, can occur during orthopedic procedures such as percutaneous pinning, open reduction and internal fixation, arthroscopy, or joint replacement, underscoring the necessity for meticulous surgical technique and anatomical knowledge. The brachial artery is particularly vulnerable due to its relatively superficial course and proximity to bone structures at the elbow and mid-humerus. Axillary artery injuries, while less frequent, are often associated with high-energy trauma or anterior shoulder dislocations. Early recognition and appropriate management of these injuries are paramount for limb salvage and optimization of functional outcomes.
Surgical Anatomy & Biomechanics
The vascular supply to the upper extremity originates from the subclavian artery, a major conduit that undergoes several name changes as it traverses the shoulder, arm, and forearm, ultimately branching to supply the hand. Its intricate collateral networks are crucial for maintaining tissue viability following proximal injury.
Subclavian Artery
-
Origin and Course:
- The left subclavian artery originates directly from the aortic arch.
- The right subclavian artery arises from the brachiocephalic trunk.
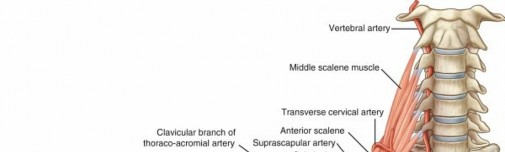
- Both arteries emerge between the anterior and middle scalene muscles, posterior to the anterior scalene, typically passing superior to the first rib.
- At the outer border of the first rib, the subclavian artery becomes the axillary artery.
- Clinical Relevance: This region is critical in Thoracic Outlet Syndrome (TOS), where neurovascular compression can occur. The subclavian artery also gives rise to the vertebral artery, internal thoracic artery, thyrocervical trunk, and costocervical trunk, which contribute to regional and spinal cord circulation.
Axillary Artery
The axillary artery is a direct continuation of the subclavian artery, extending from the outer border of the first rib to the lower border of the teres major tendon. It is intimately associated with the brachial plexus and axillary vein within the axillary sheath.

This image illustrates the complex neurovascular relationships within the axilla, highlighting the axillary artery and its branches relative to the brachial plexus.
-
Divisions and Branches:
The pectoralis minor muscle serves as an anatomical landmark, dividing the axillary artery into three distinct parts:
-
First Part (Medial to Pectoralis Minor):
Gives off
one
branch.
- Superior thoracic artery: Supplies the subclavius, first two intercostal spaces, and serratus anterior.
-
Second Part (Deep to Pectoralis Minor):
Gives off
two
branches.
- Thoracoacromial artery: Divides into pectoral, deltoid, acromial, and clavicular branches, supplying the anterior shoulder and pectoral region.
- Lateral thoracic artery: Supplies the serratus anterior, pectoralis major, and minor, and is clinically relevant for breast blood supply.
-
Third Part (Lateral to Pectoralis Minor):
Gives off
three
branches.
- Subscapular artery: A large vessel that quickly divides into the circumflex scapular artery (contributing to scapular anastomoses) and the thoracodorsal artery (supplying latissimus dorsi, critical for flap procedures).
- Anterior humeral circumflex artery: Winds anteriorly around the surgical neck of the humerus, anastomosing with the posterior humeral circumflex.
- Posterior humeral circumflex artery: Larger than its anterior counterpart, it travels with the axillary nerve through the quadrangular space, supplying the deltoid and shoulder joint capsule.
-
Vulnerability:
The
third part
of the axillary artery, particularly at the origin of the anterior and posterior humeral circumflex arteries, is the most vulnerable to traumatic vascular injury, often associated with anterior shoulder dislocations or proximal humeral fractures. Its tethered position makes it susceptible to stretch and shear forces.

This image details the three parts of the axillary artery and its specific branches, emphasizing the anatomical relationship with the pectoralis minor.
-
First Part (Medial to Pectoralis Minor):
Gives off
one
branch.
Brachial Artery
The brachial artery is the primary arterial supply to the arm, beginning at the lower border of the teres major and terminating in the cubital fossa.

This image provides a clear view of the brachial artery's course in the arm and its relationship to the median nerve and profunda brachii artery.
-
Course and Relationships:
- It courses with the median nerve (initially lateral, then anterior, then medial to the artery) in the medial arm, anterior to the intermuscular septum.
- Deep to the brachial artery lies the triceps brachii proximally and the brachialis distally.
- The basilic vein lies superficial to the brachial artery in the distal arm.
-
Branches:
- Deep muscular branch (profunda brachii artery): The largest branch, it accompanies the radial nerve posteriorly in the spiral groove (triangular interval), supplying the triceps and contributing to the elbow collateral circulation.
- Superior ulnar collateral artery: Arises near the mid-humerus, accompanies the ulnar nerve, and contributes to the medial elbow anastomoses.
- Inferior ulnar collateral artery: Arises just above the elbow, passes anterior to the medial epicondyle, and joins the medial elbow collateral network.
- Radial collateral artery: While not explicitly listed in the seed, this artery, a branch of the profunda brachii, descends with the radial nerve, anastomosing with the radial recurrent artery anterior to the lateral epicondyle.
-
Supratrochlear branch:
The seed states this is the "least flexible branch"; this likely refers to its involvement in the highly anastomotic network around the elbow, rather than its individual flexibility. These collateral branches around the elbow are vital for maintaining perfusion after brachial artery occlusion, especially if it occurs proximally.

This detailed illustration highlights the extensive collateral circulation around the elbow joint, crucial for maintaining distal perfusion in the event of brachial artery injury.

This image emphasizes the anatomical relationships of the brachial artery, particularly at the elbow, and its role in supplying the antecubital fossa.
-
Cubital Fossa:
- The brachial artery enters the antecubital fossa, bordered by the two epicondyles, the brachioradialis laterally, and the pronator teres medially. It passes anterior to the brachialis and supinator muscles.
- Within the fossa, it is typically superficial to the brachialis muscle, deep to the bicipital aponeurosis, and medial to the biceps tendon.
- It divides at the level of the radial neck (or slightly more distally, just distal to the elbow joint) into the radial artery and ulnar artery .
Radial Artery
-
Course and Branches:
- The radial artery continues distally from the brachial artery bifurcation, running along the lateral side of the forearm.
- It lies deep to the brachioradialis muscle in the proximal forearm, then becomes superficial between the tendons of brachioradialis and flexor carpi radialis in the distal forearm, making it a common site for pulse palpation.
- Radial recurrent artery: Originates proximally, contributes to the elbow anastomoses.
- Muscular branches: Supply the lateral forearm muscles.
- Palmar carpal branch: Contributes to the palmar carpal arch.
- Dorsal carpal branch: Contributes to the dorsal carpal arch.
- Superficial palmar branch: Descends into the hand to contribute to the superficial palmar arch, often anastomosing with the ulnar artery.
-
At the wrist, it curves dorsally around the scaphoid and trapezium within the anatomical snuffbox, passing between the heads of the first dorsal interosseous muscle to enter the palm and form the deep palmar arch.

This image illustrates the course of the radial and ulnar arteries in the forearm, including their recurrent and interosseous branches.
Ulnar Artery
-
Course and Branches:
- The ulnar artery is the larger of the two terminal branches of the brachial artery, continuing distally along the medial side of the forearm.
- It passes deep to the pronator teres and flexor carpi ulnaris muscles, then courses between the flexor digitorum superficialis and profundus.
- Anterior and posterior ulnar recurrent arteries: Contribute to the elbow anastomoses.
- Common interosseous artery: A short, major branch that quickly divides into the anterior interosseous artery (running on the interosseous membrane with the anterior interosseous nerve) and the posterior interosseous artery (passing superior to the interosseous membrane and running with the posterior interosseous nerve). Both supply deep forearm muscles and contribute to carpal arches.
- Muscular branches: Supply medial and deep forearm muscles.
- Palmar carpal branch: Contributes to the palmar carpal arch.
- Dorsal carpal branch: Contributes to the dorsal carpal arch.
-
At the wrist, the ulnar artery passes superficial to the flexor retinaculum, through Guyon's canal (alongside the ulnar nerve), and forms the superficial palmar arch in the hand.

This comprehensive diagram provides an overview of the entire arterial tree of the upper extremity, from the subclavian to the digital arteries.
Arterial Arches of the Hand
The rich vascular supply of the hand relies on two primary arterial arches, providing crucial anastomotic redundancy.
-
Superficial Palmar Arch:
- Primarily formed by the continuation of the ulnar artery , reinforced by the superficial palmar branch of the radial artery .
- Located just deep to the palmar aponeurosis and superficial to the flexor tendons and median nerve branches.
- Gives rise to three common palmar digital arteries, which then bifurcate into proper palmar digital arteries supplying the fingers. The ulnar side of the little finger is supplied directly by the ulnar artery.
-
Deep Palmar Arch:
- Primarily formed by the continuation of the radial artery , reinforced by the deep palmar branch of the ulnar artery .
- Located more proximally and deeply than the superficial arch, lying on the bases of the metacarpals.
-
Gives rise to palmar metacarpal arteries, which anastomose with the common palmar digital arteries from the superficial arch, and perforating arteries to the dorsal carpal arch. It also supplies the thumb and radial side of the index finger via the princeps pollicis and radialis indicis arteries.

This image distinctly labels the superficial and deep palmar arches, their contributions, and their digital branches, which are critical for hand perfusion.
Venous Drainage
The venous system parallels the arterial supply, consisting of both superficial and deep veins. The superficial veins (cephalic, basilic, median cubital) are often targeted for venous access but can be encountered during surgical approaches. The deep veins (paired radial, ulnar, and brachial veins) accompany the respective arteries and eventually drain into the axillary vein. Awareness of these venous structures is essential to prevent iatrogenic injury and manage intraoperative bleeding.
Biomechanics
The vascular structures of the upper extremity, while somewhat protected by surrounding muscles and fascia, are susceptible to injury due to their relatively fixed points (e.g., origin from aorta, passage through fascial planes) and the significant forces encountered in trauma.
*
Tethering Points:
The subclavian artery's fixation at the first rib, the axillary artery's passage through the axillary sheath, and the brachial artery's course in the relatively confined arm can lead to stretch injuries during dislocations or fracture displacement.
*
Shear and Compression:
Direct blunt trauma, fracture fragments, or forceful retraction during surgery can cause arterial transection, contusion, intimal injury, or vasospasm.
*
Collateral Circulation:
The rich anastomotic networks around the shoulder (scapular anastomosis), elbow (supra- and intercondylar), and wrist/hand (palmar/dorsal carpal arches, palmar digital arches) provide critical redundancy. However, the efficacy of these collaterals can be compromised by age, atherosclerotic disease, or extensive soft tissue injury.
Indications & Contraindications
Understanding the vascularity of the upper extremity is crucial for orthopedic surgeons in determining indications for both operative and non-operative management, especially when vascular compromise is present or anticipated.
Indications for Orthopedic Surgical Intervention with Vascular Considerations
-
Acute Trauma with Vascular Injury:
- Open Fractures with Vascular Damage: Immediate operative intervention is indicated for debridement, stabilization, and vascular repair/reconstruction.
- Closed Fractures/Dislocations with Acute Ischemia: Requires urgent reduction and stabilization, followed by vascular assessment and potential repair if ischemia persists.
- Compartment Syndrome: Fasciotomy is indicated to prevent irreversible muscle and nerve damage, often secondary to revascularization following arterial injury or severe crush injury.
-
Elective Procedures in High-Risk Zones:
- Tumor Resection: May involve planned vascular sacrifice or reconstruction, requiring detailed pre-operative vascular mapping (CTA/MRA).
- Reconstructive Surgery: Microvascular free tissue transfer mandates meticulous vascular anastomoses.
- Revision Surgery: Previous surgical scarring can obscure vascular planes, increasing risk.
-
Chronic Vascular Pathology:
- Pseudoaneurysm/Arteriovenous Fistula: May require surgical repair or embolization if causing symptoms or risk of rupture.
- Thoracic Outlet Syndrome (TOS): Decompression (e.g., first rib resection) if arterial compression is confirmed.
Contraindications for Orthopedic Surgical Intervention
-
Absolute Contraindications (rare for limb salvage):
- Irretrievable Ischemia: Prolonged warm ischemia time (>6 hours, though variable) with extensive tissue necrosis may preclude successful revascularization and functional limb salvage, potentially leading to primary amputation.
- Patient Instability: Uncontrolled hemorrhage or severe systemic instability may necessitate delaying definitive limb reconstruction until the patient is resuscitated, focusing initially on life-saving measures.
-
Relative Contraindications:
- Severe Comorbidities: Uncontrolled cardiac disease, severe coagulopathy, or advanced peripheral vascular disease may increase surgical risk and require careful risk-benefit analysis or modification of surgical approach.
- Pre-existing Vascular Disease: Significant atherosclerosis may complicate vascular repair and necessitate alternative strategies or bypass grafting.
- Infection: Active infection in the surgical field may contraindicate immediate vascular grafting, potentially requiring debridement and delayed reconstruction or temporary shunting.
Table: Operative vs. Non-Operative Indications with Vascular Implications
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Acute Trauma | - Open fracture with vascular injury | - Stable closed fracture without vascular compromise (monitor closely for delayed compromise) |
| (Vascular Injury Suspected) | - Closed fracture/dislocation with acute limb ischemia | - Minor intimal injury/spasm without distal ischemia (conservative management with anticoagulation, observation) |
| - Compartment syndrome (fasciotomy) | - Penetrating injury without signs of active bleeding or ischemia (serial clinical exams, Doppler, observe) | |
| Iatrogenic Injury | - Arterial laceration/transection during surgery | - Small, contained pseudoaneurysm without rupture risk (conservative management with surveillance) |
| - Graft infection (excision, debridement, distant tissue transfer) | - Transient vasospasm (medical management, local anesthetics) | |
| Chronic/Elective | - Symptomatic pseudoaneurysm or AV fistula | - Asymptomatic small pseudoaneurysm (serial imaging) |
| - Planned vascular sacrifice for tumor resection or limb lengthening | - Mild, stable claudication without critical limb ischemia (exercise therapy, medical management) | |
| - Replantation/revascularization of amputated/ischemic limb | - Chronic nerve compression without arterial compromise (e.g., mild cubital tunnel syndrome without ulnar artery involvement, often managed with splinting and physical therapy initially) |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical to optimize outcomes and minimize iatrogenic vascular injury during upper extremity surgery.
Pre-Operative Planning
-
Vascular Assessment:
- Clinical Examination: Always include bilateral pulse examination (carotid, subclavian, axillary, brachial, radial, ulnar), capillary refill, skin color, temperature, and sensory/motor evaluation. Auscultate for bruits.
- Ankle-Brachial Index (ABI): For lower extremity vascular assessment, but upper extremity equivalent measurements may be used in specific contexts.
- Doppler Ultrasound: Non-invasive, provides flow information and can detect stenoses or occlusions. Essential for screening and follow-up.
- Advanced Imaging (CTA/MRA): Crucial for detailed anatomical mapping of injuries, planning vascular reconstruction, or identifying anatomical variations. Digital subtraction angiography (DSA) remains the gold standard for definitive diagnosis and can allow for endovascular intervention.
- Allen's Test: Performed before radial artery harvest (e.g., for vascular grafts or bypass) to confirm adequate ulnar collateral circulation to the hand.
-
Multidisciplinary Consultation:
- For complex vascular injuries or anticipated vascular involvement, early consultation with a vascular surgeon or plastic/microvascular surgeon is paramount. This ensures coordinated care, appropriate surgical team assembly, and access to specialized instrumentation and expertise.
-
Tourniquet Considerations:
- Inflation Pressure: Typically 250-300 mmHg for the upper arm, or 50-75 mmHg above systolic blood pressure.
- Inflation Time: Generally limited to 90-120 minutes to minimize ischemia-reperfusion injury, nerve palsy, or muscle damage. Longer durations require intermittent reperfusion periods.
- Contralateral Tourniquet: May be required if proximal vascular injury makes ipsilateral tourniquet use unsafe or ineffective.
- Exsanguination: Proper exsanguination prior to inflation reduces intraoperative blood loss.
- Blood Products: Type and cross-match blood should be readily available, especially for high-risk cases.
- Equipment: Ensure specialized vascular instruments (fine forceps, vessel loops, microvascular clamps), suture materials (e.g., 6-0 to 8-0 monofilament), and potentially microscope or loupes are available.
Patient Positioning
-
Supine Position:
- Common for shoulder, arm, and elbow surgery. The arm can be placed on an arm board, allowing for free movement.
- Considerations: Ensure adequate padding to prevent brachial plexus compression (especially if the arm is abducted beyond 90 degrees), ulnar nerve compression at the elbow, and axillary artery compression if shoulder rolls are improperly placed.
-
Beach Chair Position:
- Often used for shoulder surgery.
- Considerations: Potential for cerebrovascular hypoperfusion due to head elevation and hypotension. Monitor blood pressure closely. Excessive neck rotation can compress vertebral arteries.
-
Lateral Decubitus Position:
- Can be used for shoulder, humerus, or elbow surgery.
- Considerations: Ensure the dependent arm is well-padded and not compressed. The non-dependent arm (operative limb) is typically draped over a bolster or suspended in traction. Avoid axillary compression by supporting the chest wall, not the axilla.
-
General Principles:
- Adequate Padding: Protect all pressure points, especially ulnar nerve at the elbow, radial nerve at the humerus, and brachial plexus in the axilla.
- Access: Position for optimal surgical exposure while maintaining physiological stability and protecting neurovascular structures.
- Tourniquet Placement: High on the arm, over appropriate padding, ensuring the skin is protected.
Detailed Surgical Approach / Technique
Orthopedic surgical approaches in the upper extremity are designed to provide access to skeletal and soft tissue structures while minimizing damage to critical neurovascular elements. A thorough understanding of vascular anatomy is paramount for safe dissection, reduction, and fixation.
General Principles of Vascular Preservation
- Meticulous Dissection: Use blunt dissection where possible to identify and isolate vessels. Sharp dissection should be precise and performed with direct visualization.
- Magnification: Loupes (2.5x to 4.5x) or a surgical microscope are highly recommended for working near critical vessels, particularly in the hand or during microvascular procedures.
- Gentle Handling: Vessels should be handled gently with non-crushing instruments (e.g., vascular forceps, vessel loops). Avoid excessive traction, clamping, or electrocautery directly on vessels.
- Identify Internervous Planes: Utilizing established internervous planes allows access to deeper structures with reduced risk of neurovascular injury. These planes often lie between muscle groups supplied by different nerves, thereby protecting the main vascular pedicles.
- Control of Hemorrhage: Be prepared for significant bleeding. Have appropriate suction, clamps, and ligatures ready. In cases of arterial injury, direct pressure, temporary clamping, or vascular shunting may be necessary prior to definitive repair.
Surgical Approaches and Vascular Considerations
1. Shoulder and Proximal Humerus
-
Deltopectoral Approach:
(For proximal humerus fractures, shoulder arthroplasty)
- Internervous Plane: Between the deltoid (axillary nerve) and pectoralis major (medial and lateral pectoral nerves).
-
Vascular Structures:
- Cephalic Vein: Runs in the deltopectoral groove; often retracted laterally but can be ligated if necessary.
- Axillary Artery/Vein and Brachial Plexus: Lie deep in the axilla, medial to the coracobrachialis. Risk of injury with aggressive medial retraction or deep dissection.
- Anterior Humeral Circumflex Artery: Located near the surgical neck of the humerus, running transversely. May require ligation during fracture exposure or humeral head replacement.
-
Deltoid-Splitting Approach:
(For humeral shaft fractures, rotator cuff repair)
- Internervous Plane: Splits the deltoid muscle fibers.
-
Vascular Structures:
- Axillary Nerve and Posterior Humeral Circumflex Artery: Emerge from the quadrangular space (inferior to teres minor, superior to teres major, medial to triceps long head, lateral to humerus) and pass around the surgical neck. They are vulnerable if the deltoid split extends more than 5 cm distal to the acromion.
-
Posterior Approach (Judet):
(For posterior shoulder dislocation, posterior glenoid fractures)
- Vascular Structures: Awareness of the subscapular artery (divides into circumflex scapular and thoracodorsal) and posterior humeral circumflex artery is crucial in deep dissection near the scapular spine and glenoid.
2. Humeral Shaft
-
Anterolateral Approach (Henry):
(For humeral shaft fractures)
- Internervous Plane: Between the deltoid/brachialis (musculocutaneous nerve) laterally and biceps/brachialis (musculocutaneous nerve) medially proximally. Distally, between brachialis (musculocutaneous/radial nerve) and brachioradialis (radial nerve).
-
Vascular Structures:
- Brachial Artery and Median Nerve: Lie medial to the biceps and brachialis. Medial retraction of the biceps protects these structures.
- Profunda Brachii Artery: Accompanies the radial nerve posteriorly in the spiral groove. Deep dissection or posterior plating can injure this vessel.
-
Posterior Approach:
(For humeral shaft fractures)
- Internervous Plane: Between the medial and lateral heads of the triceps (radial nerve).
-
Vascular Structures:
- Radial Nerve and Profunda Brachii Artery: Located in the spiral groove (posterior aspect of the humerus). They are extremely vulnerable during fracture exposure, plating, or with over-penetration of screws. Careful subperiosteal dissection is required to protect them.
3. Elbow
-
Medial Approach (Medial Epicondyle, Ulnar Nerve Transposition):
-
Vascular Structures:
- Brachial Artery/Veins, Median Nerve: Lie anterior to the joint, protected by the brachialis and bicipital aponeurosis.
- Ulnar Collateral Arteries (Superior & Inferior): Contribute to the medial elbow anastomoses and are found in close proximity to the ulnar nerve.
-
Vascular Structures:
-
Lateral Approach (Lateral Epicondyle, Radial Head Fracture):
-
Vascular Structures:
- Radial Recurrent Artery: Contributes to the lateral elbow anastomosis and can be injured during exposure of the radial head.
- Brachial Artery Bifurcation: Awareness of its location (often at the radial neck level) is important for distal procedures.
-
Vascular Structures:
-
Anterior Approach (Cubital Fossa):
-
Vascular Structures:
- Brachial Artery: Lies within the cubital fossa, medial to the biceps tendon, under the bicipital aponeurosis. Highly susceptible to injury during anterior elbow procedures (e.g., distal biceps repair, anterior capsulectomy).
- Median Nerve: Immediately adjacent to the brachial artery.
-
Vascular Structures:
4. Forearm
-
Volvar Approach (Henry Approach for Radius):
- Internervous Plane: Between brachioradialis (radial nerve) and flexor carpi radialis (median nerve).
-
Vascular Structures:
- Radial Artery: Lies deep to the brachioradialis and is often mobilized medially with the flexor carpi radialis. Care must be taken to protect its recurrent branches and the superficial palmar branch at the wrist.
- Radial Recurrent Artery: Proximally, it courses near the radial neck.
- Anterior Interosseous Artery: Deep in the forearm, accompanied by the anterior interosseous nerve, vulnerable to injury during deep dissection or plate application on the interosseous membrane.
-
Ulnar Approach:
(For ulnar shaft fractures, distal ulna)
- Internervous Plane: Between flexor carpi ulnaris (ulnar nerve) and flexor digitorum profundus (ulnar nerve/median nerve).
-
Vascular Structures:
- Ulnar Artery and Ulnar Nerve: Lie together on the medial side of the forearm, deep to the flexor carpi ulnaris distally. They are protected by retracting the flexor carpi ulnaris medially.
- Common Interosseous Artery: Originates high in the forearm from the ulnar artery, then divides into anterior and posterior interosseous arteries, which are at risk during deep forearm dissection.
-
Dorsal Approach (Thompson Approach for Radius):
-
Vascular Structures:
- Posterior Interosseous Artery: Accompanies the posterior interosseous nerve through the supinator. Vulnerable during exposure of the proximal radius or deep dissection for fracture fixation.
-
Vascular Structures:
5. Wrist and Hand
-
Distal Radius Fixation (Volvar Approach):
-
Vascular Structures:
- Radial Artery: Its superficial palmar branch is at risk during carpal tunnel release or distal radius plate placement on the radial side. The main radial artery lies lateral to the flexor carpi radialis tendon.
-
Vascular Structures:
-
Carpal Tunnel Release:
-
Vascular Structures:
- Superficial Palmar Arch: Located distal to the flexor retinaculum, it is vulnerable during extensile approaches or inadequate release of the distal arch.
- Ulnar Artery and Nerve: Medial to the carpal tunnel, within Guyon's canal, susceptible to injury during medial approaches.
-
Vascular Structures:
-
Hand Surgery (Fracture Fixation, Tendon Repair):
-
Vascular Structures:
- Digital Arteries (Proper and Common Palmar): Run along the sides of the fingers. High risk of injury during incision, dissection, or fixation of phalangeal/metacarpal fractures. Meticulous technique and magnification are essential.
- Deep Palmar Arch: Deep and more proximal, generally less vulnerable to superficial hand incisions but at risk during deep metacarpal dissection.
-
Vascular Structures:
Complications & Management
Vascular complications in upper extremity orthopedic surgery range from minor vasospasm to limb-threatening ischemia. Prompt recognition and appropriate management are critical.
Table: Common Vascular Complications, Incidence, and Salvage Strategies
| Complication | Description | Incidence (approx.) | Salvage Strategies |
|---|---|---|---|
| Iatrogenic Arterial Injury | Laceration, transection, intimal tear, avulsion during surgery or trauma. | 0.1-2% in elective orthopedics; higher in trauma (5-20% for major trauma) | Immediate recognition: Direct pressure, temporary clamping (vascular loops/bulldog clamps), systemic heparinization (if no contraindication). Repair: Primary end-to-end anastomosis (preferred), interposition vein graft (autologous saphenous vein from lower extremity or forearm veins), synthetic graft (rarely). |
| Arterial Thrombosis/Occlusion | Clot formation within a vessel, leading to distal ischemia. | 1-5% post-repair or in conservative management of intimal injury. | Thrombectomy: Fogarty catheter embolectomy, mechanical thrombectomy, or thrombolysis (pharmacological). Revision of repair if technical fault identified. |
| Compartment Syndrome | Increased pressure within a closed fascial compartment, compromising blood flow. | 2-10% following trauma, revascularization, or crush injury. | Urgent Fasciotomy: Single- or dual-incision approaches for forearm and hand compartments. Release of all affected compartments. |
| Vasospasm | Sustained vasoconstriction of an artery, reducing flow. | Variable; common in microvascular surgery or after direct trauma. | Local Measures: Warm irrigation, papaverine (topical or intra-arterial), lidocaine. Systemic Measures: Nifedipine (calcium channel blocker). Gentle handling of vessels. |
| Pseudoaneurysm | Contained hematoma communicating with the arterial lumen, without all layers of the vessel wall. | <1% post-trauma or iatrogenic puncture. | Small, asymptomatic: Observation, ultrasound surveillance. Large/symptomatic/expanding: Surgical repair (excision and primary repair/patch/graft), endovascular coil embolization or stent-grafting. |
| Arteriovenous (AV) Fistula | Abnormal communication between an artery and a vein. | Rare; typically post-penetrating injury or iatrogenic. | Small, asymptomatic: Observation. Large/symptomatic (high output cardiac failure, thrill/bruit, venous hypertension): Surgical ligation and repair of vessels, endovascular embolization. |
| Ischemia-Reperfusion Injury | Damage to tissue caused by restoration of blood supply after ischemia. | Universal phenomenon after significant ischemia (>4-6 hours). | Prevention: Minimizing ischemia time. Management: Fluid resuscitation, control of hyperkalemia/acidosis, antioxidants, potentially fasciotomy to prevent secondary compartment syndrome. |
| Vessel Graft Failure/Infection | Occlusion or infection of a vascular graft used for reconstruction. | 5-15% (depending on graft type and patient comorbidities). | Occlusion: Thrombectomy, repeat grafting. Infection: Excision of infected graft, extensive debridement, antibiotics, possibly rerouting bypass through uninfected tissue, or muscle flap coverage. |
| Nerve Injury (Secondary to Ischemia) | Neuropraxia, axonotmesis, or neurotmesis due to prolonged ischemia. | Directly related to ischemia severity and duration. | Prevention: Timely revascularization, fasciotomy. Management: Physical therapy, nerve blocks, delayed nerve repair/grafting if neurotmesis. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following upper extremity surgery, especially when vascular injury or repair has occurred, requires a nuanced approach to ensure both vascular integrity and functional recovery. The specific protocol will be highly individualized based on the nature of the vascular injury, type of repair, stability of orthopedic fixation, and overall patient condition.
-
Immediate Post-Operative Period (Days 0-7):
- Vascular Monitoring: Continuous, meticulous monitoring of distal perfusion (pulses, capillary refill, skin color/temperature, Doppler signals). Any signs of ischemia warrant immediate surgical re-exploration.
- Edema Control: Elevation of the extremity above heart level, gentle compression dressings, active range of motion of unaffected joints (e.g., shoulder if hand surgery).
- Pain Management: Adequate analgesia to allow for early, gentle movement and reduce sympathetic vasoconstriction.
- Wound Care: Strict sterile dressing changes, monitoring for signs of infection, especially around vascular grafts.
- Immobilization: Immobilization in a splint or cast may be necessary to protect vascular repairs and orthopedic fixation. The position should avoid tension on vascular anastomoses (e.g., slight flexion for brachial artery repairs, neutral for radial/ulnar artery repairs).
- Anticoagulation/Antiplatelet Therapy: Often initiated based on vascular surgeon recommendation (e.g., aspirin, clopidogrel, heparin) to prevent thrombosis, particularly after vascular repair or microvascular anastomoses.
- Compartment Syndrome Surveillance: Vigilant monitoring for signs of compartment syndrome, particularly after revascularization or crush injuries.
-
Early Mobilization Phase (Weeks 1-6):
- Gradual Increase in Range of Motion (ROM): Initiated as per orthopedic and vascular surgeon's directives. Passive and active-assisted ROM, progressing to active ROM, typically within pain tolerance. Specific limits on joint flexion/extension may be imposed to protect vessel repairs.
- Gentle Strengthening: Isometrics or very light resistance exercises may be introduced, avoiding any movements that cause vascular compromise or excessive strain.
- Scar Management: Gentle massage, silicone sheeting to prevent hypertrophic scarring, especially over repaired vessels.
- Sensory Re-education: If nerve injury coexists, sensory re-education protocols are initiated.
- Functional Activities: Begin with light, non-weight-bearing activities.
-
Intermediate to Advanced Rehabilitation (Weeks 6-12+):
- Progressive Strengthening: Increase resistance and intensity of exercises, focusing on restoring muscle bulk and power.
- Endurance Training: Activities to improve overall limb endurance.
- Proprioception and Coordination: Specific exercises to regain fine motor control and coordination.
- Return to Activity: Gradually progress to sport-specific or work-specific activities, ensuring no undue stress on the healed vascular structures. Patient education on avoiding repetitive trauma or positions that could compromise blood flow.
- Long-term Monitoring: Regular follow-up with clinical examination and potentially Doppler ultrasound to assess graft patency or detect late complications (e.g., pseudoaneurysm, stenosis).
Summary of Key Literature / Guidelines
A thorough understanding of upper extremity vascularity and its surgical implications is underpinned by a robust body of literature and professional guidelines. These resources emphasize a multidisciplinary approach and evidence-based practices for optimal patient outcomes.
-
Trauma Management Guidelines:
- The American Academy of Orthopaedic Surgeons (AAOS) and the Orthopaedic Trauma Association (OTA) consistently publish clinical practice guidelines and instructional courses that address the management of complex upper extremity trauma, including those with associated vascular injuries. These guidelines typically advocate for prompt recognition of vascular compromise, emergent reduction of dislocations/fractures, and the need for a vascular surgery consult when arterial injury is suspected or confirmed.
- Key principles include the "hard" signs of vascular injury (pulsatile bleeding, rapidly expanding hematoma, bruit/thrill, distal ischemia) mandating immediate exploration, and "soft" signs (non-pulsatile hematoma, decreased pulse, nerve deficit) warranting further diagnostic workup (e.g., CTA/MRA).
- The importance of minimizing warm ischemia time in revascularization procedures is a recurrent theme, with studies consistently showing better outcomes with revascularization within 6-8 hours of complete ischemia.
-
Microvascular Surgery Principles:
- Literature on microvascular free tissue transfer and replantation highlights the critical techniques for successful vascular anastomoses. Seminal works by Buncke, Kleinert, and others established the foundations of microvascular surgery. These papers emphasize meticulous dissection, minimal vessel handling, fine suture material (e.g., 8-0 to 10-0 nylon), and prevention of vasospasm and thrombosis.
- Guidelines for replantation emphasize appropriate patient selection, warm ischemia time, and the sequence of repair (bone, extensor tendons, flexor tendons, arteries, nerves, veins, skin). The ratio of venous to arterial repairs (typically 2:1 veins to arteries) is often cited as a factor in successful microvascular free flap and replant survival.
-
Anatomical Studies and Variations:
- Anatomical dissection studies and imaging research continue to refine our understanding of common variations in upper extremity vascular anatomy (e.g., high bifurcation of the brachial artery, persistent median artery, variations in palmar arches). Awareness of these variations is critical for pre-operative planning and avoiding iatrogenic injury. For example, a significant percentage of patients may have an incomplete superficial palmar arch, emphasizing the importance of Allen's test prior to radial artery harvest.
-
Peripheral Artery Disease and Aneurysmal Disease:
- Although less common in the upper extremity compared to the lower, the literature addresses the management of peripheral artery disease and aneurysms (e.g., subclavian artery aneurysm in TOS, ulnar artery aneurysm in hypothenar hammer syndrome). These studies guide diagnosis, indications for intervention, and surgical techniques (e.g., patch angioplasty, graft interposition, endovascular repair).
In conclusion, the orthopedic surgeon's expertise in upper extremity vascularity is a cornerstone of safe and effective practice. From detailed anatomical knowledge to understanding the biomechanics of vascular injury, and from meticulous surgical technique to comprehensive post-operative management, integrating vascular principles into orthopedic care is essential for optimizing limb function and patient well-being. A collaborative approach with vascular and plastic surgeons is often crucial for managing complex cases, ensuring the best possible outcomes.
Clinical & Radiographic Imaging