Tibial Plateau Fractures: Anatomy, Classification, Treatment, and Complications
Tibial plateau fractures are periarticular injuries of the proximal tibia that are frequently associated with soft tissue injury. Here's what you need to know about their diagnosis, treatment, and prognosis:
Mohammad Hutaif
(
 ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
__Save
__Cite
__Cited by
__Related articles
__All versions
__Import into BibTeX
Anatomy
Osteology: The lateral tibial plateau is convex in shape and proximal to the medial plateau. The medial tibial plateau is concave in shape and distal to the lateral plateau. The alignment of the proximal tibia includes the posterior tibial slope, varus slope, and tibial rotation. Ligaments: Important ligaments of the knee include the anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL), and lateral collateral ligament (LCL). 3-Column Concept: The proximal tibia can be divided into three columns; medial, lateral, and posterior.
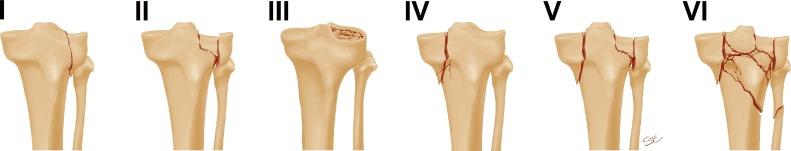
Classification Schatzker Classification: This classification system is based on the type of fracture, including lateral split, lateral split-depressed, lateral pure depression, medial plateau fracture, bicondylar fracture, and metaphyseal-diaphyseal disassociation. 3-Column Concept: This classification system divides the proximal tibia into three columns; medial, lateral, and posterior.
Presentation
Patients with tibial plateau fractures may present with pain, inability to bear weight, and baseline functional status. Physical exam may reveal swelling, tenderness, and joint instability.
Imaging
Radiographs are the recommended initial evaluation for a tibial plateau fracture, but patients may require a CT scan for surgical planning. MRI may be useful to assess meniscal and ligamentous pathology.
Treatment
Nonoperative treatment may include closed reduction and immobilization using a knee immobilizer, while operative treatment may involve ORIF, external fixation, or arthroplasty.
Complications
Complications that may occur following a tibial plateau fracture include post-traumatic arthritis, compartment syndrome, infection, nonunion/malunion, knee stiffness, and loss of reduction.
Figure 1: Anatomy of the Tibial Plateau (Source: Hutaif Orthopedic Center)
Figure 2: Alignment of the Proximal Tibia (Source: Hutaif Orthopedic Center)
Figure 3: 3-Column Concept of the Tibial Plateau (Source: Hutaif Orthopedic Center)
Test Your Knowledge
Take the following quiz to see what you know about tibial plateau fractures: 1. What are some of the risk factors for post-traumatic arthritis following a tibial plateau fracture? Age and gender
Severity of fracture and presence of comorbidities
Both a and b
None of the above 2. What is the recommended initial evaluation for a patient with a suspected tibial plateau fracture? CT scan
MRI
Radiographs
Ultrasound 3. What ligament is the primary restraint against anterior tibial translation in the knee? Posterior cruciate ligament (PCL)
Medial collateral ligament (MCL)
Lateral collateral ligament (LCL)
Anterior cruciate ligament (ACL) 4. What is the primary goal of operative treatment for a tibial plateau fracture? To minimize additional soft tissue trauma
To restore joint stability and alignment
To minimize postoperative infection
To minimize postoperative pain 5. What is the recommended treatment for low-energy fractures that are stable to varus/valgus alignment? External fixation
ORIF
Arthroplasty
Closed reduction and immobilization
6. What is the most common complication following a tibial plateau fracture?
Post-traumatic arthritis
Compartment syndrome
Infection
Loss of reduction 7. What is the best way to address knee stiffness following a tibial plateau fracture?
Open reduction and internal fixation
External fixation
Arthroscopic lysis of adhesions with MUA
None of the above
Submit