Introduction and Initial Resuscitation
The evaluation and management of patients sustaining severe thermal burns must strictly adhere to Advanced Trauma Life Support (ATLS) protocols. In the polytraumatized patient, life-threatening injuries and extensive total body surface area (TBSA) burns take absolute precedence over isolated hand burns. A critical component of the primary survey is the assessment of concomitant inhalation injury. The presence of an inhalation injury drastically alters the patient's prognosis; mortality from burns with associated inhalation injury approaches 35%, whereas mortality from burns without inhalation injury is approximately 2%.
Once systemic stabilization is achieved—encompassing securing the airway, establishing large-bore intravenous access, initiating Parkland formula fluid resuscitation, administering tetanus prophylaxis, and providing broad-spectrum antibiotics if indicated—attention may be directed to the extremities.
The primary orthopedic objectives in the management of thermal hand burns are the preservation of viable tissue, prevention of invasive burn wound sepsis, control of interstitial fibrosis, and the avoidance of severe deforming contractures. The functional and cosmetic outcome of a burned hand is directly proportional to the accuracy of the initial depth assessment, the timeliness of surgical intervention, and the rigor of postoperative rehabilitation.
Clinical Pearl: The initial examination of a burned hand is often confounded by severe pain, profound edema, and patient altered mental status. Despite these challenges, an accurate estimation of burn depth (superficial, deep partial-thickness, full-thickness) and the involvement of deep structures (tendon, joint capsule, bone) is the most critical determinant of the surgical algorithm.
Burn Depth Classification and Pathophysiology
The judgment of the treating surgeon remains the gold standard for estimating burn depth, though adjunctive technologies such as noncontact laser Doppler imaging have demonstrated high accuracy in predicting microvascular viability. Burns are anatomically classified based on the extent of dermal and subcutaneous destruction:
- Superficial Burns (First-Degree): Confined to the epidermis. Characterized by erythema, absence of blisters, brisk capillary refill, and intact sensation. The underlying dermis is unharmed, and spontaneous healing occurs without scarring.
- Partial-Thickness Burns (Second-Degree): Subdivided into superficial and deep categories based on the depth of dermal necrosis.
- Superficial Partial-Thickness: Involves the epidermis and the papillary dermis. Blisters (vesicles) are hallmark features. The wound bed is pink, moist, exquisitely painful, and demonstrates rapid capillary refill.
- Deep Partial-Thickness: Extends into the reticular dermis. The wound appears mottled pink and white, is relatively dry, and capillary refill is sluggish or absent. Sensation is markedly diminished, and thrombosed subcutaneous veins may be visible.
- Full-Thickness Burns (Third and Fourth-Degree): Complete destruction of the epidermis and dermis, extending into the subcutaneous fat, fascia, muscle, or bone. The skin appears leathery, charred (brown to black), or translucent white. The eschar is insensate and avascular.
Vascular Assessment and Compartment Syndrome
The most urgent local determination in a burned upper extremity is the adequacy of distal perfusion. The inelastic nature of full-thickness, circumferentially burned skin creates a rigid envelope. As obligatory burn edema accumulates within this unyielding space, interstitial pressures rise rapidly, creating a tourniquet effect.
Circulation is deemed adequate if the hand and digits exhibit rapid capillary refill, remain pink and warm, and demonstrate pulsatile flow in the palmar arch and digital vessels via a handheld Doppler probe.
Surgical Warning: If a circumferential burn is present and distal perfusion is compromised (manifested by pale, cool, firm digits with delayed capillary refill and diminished or absent Doppler signals), immediate escharotomy is mandatory. If intracompartmental pressures remain elevated (>30 mm Hg) despite escharotomy, formal fasciotomies of the forearm and hand are required to prevent irreversible ischemic contracture.
Pathomechanics of Severe Thermal and Electrical Burns
While thermal burns cause direct coagulative necrosis via heat transfer, high-voltage electrical burns represent a unique and often more devastating injury pattern that frequently involves the upper extremity as the primary contact point.
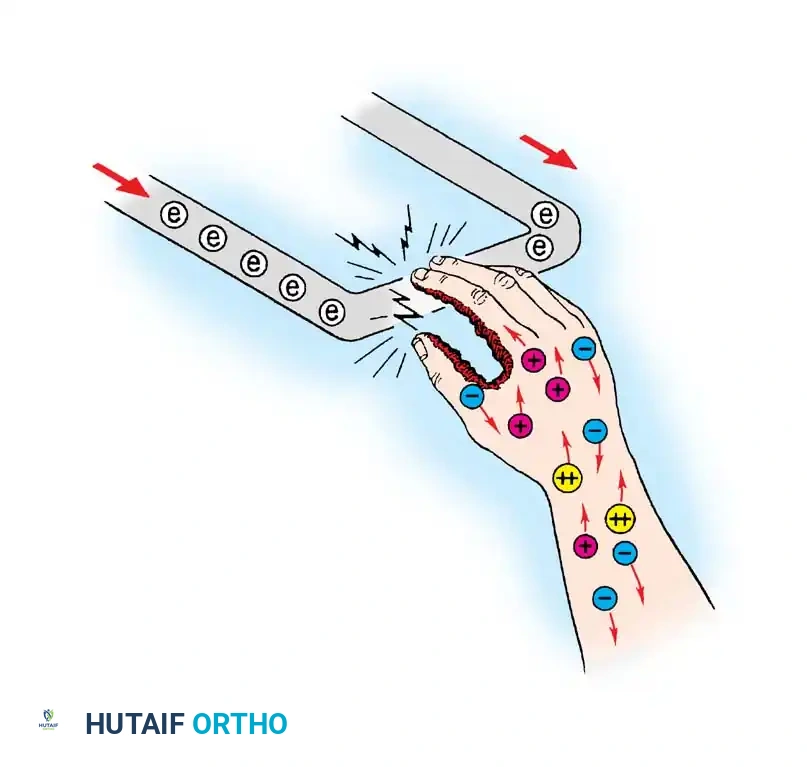
Electrical injuries cause deep tissue destruction that is often disproportionate to the overlying skin manifestations. As electrical current traverses the limb, tissues with higher resistance (such as bone and tendon) generate massive amounts of heat, leading to deep periosseous muscle necrosis. This "inside-out" thermal damage necessitates a high index of suspicion for deep compartment syndrome. The management principles for both severe deep thermal burns and electrical burns converge on the need for urgent decompression (escharotomy/fasciotomy) and aggressive, often serial, surgical débridement of non-viable tissue.
Non-Operative vs. Operative Management Paradigms
The management of hand burns is dictated by depth, location, and patient factors (age, compliance).
Superficial Burns
Superficial burns require only conservative management. Protected from secondary trauma and infection, these injuries re-epithelialize within 14 to 21 days with no significant impairment of hand function or cosmesis. Outpatient management with topical antimicrobials and non-adherent dressings is appropriate.
Partial-Thickness Burns
The treatment of deep dermal and superficial full-thickness burns remains a topic of debate, with two primary approaches:
1. The "Wait-and-See" Conservative Method: Involves daily hydrotherapy, topical chemotherapy (silver sulfadiazine, mafenide acetate, povidone-iodine), and aggressive physiotherapy. Advocates argue that with meticulous care, patients can achieve long-term results comparable to surgery while avoiding operative morbidity.
2. The Early Operative Approach: Involves tangential or full-thickness excision and skin grafting within the first 3 to 5 days. Proponents cite earlier physiological healing, rapid rehabilitation, and the avoidance of hypertrophic scarring and severe contractures associated with prolonged secondary intention healing.
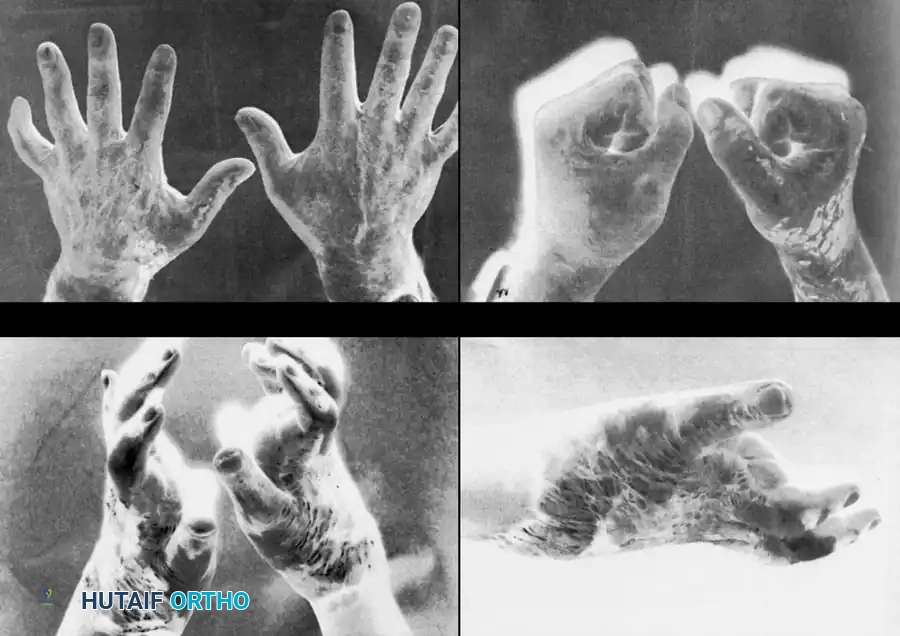
Anatomical Considerations: Dorsum vs. Volar
The unique soft tissue architecture of the hand allows for a combined approach. The dorsal skin is thin and highly mobile, offering minimal protection to the underlying extensor mechanism. Dorsal deep partial-thickness burns benefit immensely from early excision (within 14 days) and grafting to provide protective coverage and allow early mobilization of the interphalangeal joints, preventing devastating extension contractures. Conversely, the thick, glabrous skin of the volar surface provides robust protection to the flexor tendons and neurovascular bundles, often tolerating a delay of up to 3 weeks to allow for potential spontaneous re-epithelialization.
Surgical Technique: Escharotomy
Escharotomy is a limb-saving procedure designed to release the rigid eschar and restore distal perfusion.
Preoperative Preparation
- Ensure adequate fluid resuscitation and prepare for potential blood transfusion, as escharotomies can result in significant blood loss once perfusion is restored.
- Position the patient supine with the upper extremity extended on a radiolucent hand table.
- Administer general anesthesia or regional block, though in critically ill patients with insensate full-thickness burns, escharotomy can occasionally be performed at the bedside without anesthesia.
Step-by-Step Procedure (Sheridan et al.)
- Incision Placement: Utilize an electrocautery cutting current to make medial and lateral midaxial longitudinal incisions through the eschar. The incision must extend through the entire burned area, from healthy skin proximally to healthy skin distally.
- Elbow Considerations: At the elbow, carefully route the medial incision anterior to the medial epicondyle to strictly avoid iatrogenic injury to the ulnar nerve within the cubital tunnel.
- Hand Extension: Extend the incisions distally, stopping at the metacarpophalangeal (MCP) joints.
- Fasciotomy Assessment: Palpate the muscle compartments. If they remain tense, or if intracompartmental pressure monitoring reveals elevated pressures, proceed immediately to formal fasciotomies of the forearm (volar and dorsal) and hand (interosseous) compartments.
- Digital Escharotomy: Re-evaluate distal perfusion using a Doppler probe. If digital perfusion remains compromised, perform digital escharotomies.
- Use pinpoint electrocautery to make a longitudinal incision strictly along the ulnar midaxial line of the involved digits (index, middle, ring, little) from the distal phalanx to the web space. This avoids the primary radial pinch contact surfaces.
- For the thumb, place the incision along the radial midaxial line to preserve the ulnar collateral ligament complex and ulnar pinch surface.
- Ensure the incision is placed precisely between the volar digital neurovascular bundle and the dorsal extensor tendon apparatus.
- Intermetacarpal Release: If the intrinsic compartments are tight, make additional dorsal longitudinal incisions between the index-middle and ring-little metacarpals to release the dorsal interosseous fascia.
- Hemostasis and Dressing: Obtain meticulous hemostasis. Apply a non-adherent medicated gauze (e.g., Xeroform) followed by a bulky, non-constricting, highly absorptive dressing. Elevate the limb continuously postoperatively.
Surgical Technique: Tangential Excision
Tangential excision is indicated for deep partial-thickness burns. The goal is the sequential removal of necrotic tissue while preserving the maximum amount of viable deep dermis and superficial subcutaneous tissue to optimize graft take and functional outcome.
Step-by-Step Procedure
- Preparation: Under general anesthesia, place the patient supine with the arm on a hand table. Apply a well-padded pneumatic tourniquet. Exsanguinate the limb by elevation (avoiding Esmarch bandages over necrotic tissue) and inflate the tourniquet.
- Excision: Using a guarded knife (e.g., Watson or Braithwaite) or a powered dermatome, shave the burned areas tangentially in thin layers (approximately 0.010-inch thick).
- Endpoint Determination: Continue shaving through the dermal and subcutaneous tissues containing thrombosed veins until a healthy, uniform tissue bed is reached. The clinical endpoint is the appearance of brisk, punctate bleeding when the tourniquet is temporarily deflated.
- Hemostasis: Deflate the tourniquet and achieve absolute hemostasis using pinpoint electrocautery and topical thrombin application. Cover the hand with warm, saline-soaked sponges.
- Grafting: Once hemostasis is secure, apply a split-thickness skin graft (STSG). For the dorsum of the hand, unmeshed sheet grafts are strongly preferred to minimize secondary contracture and optimize cosmesis.
- Fixation: Secure the graft with sutures or surgical staples. Place strategic darts in the skin folds at the interdigital webs and the first web space to prevent linear scar contractures.
Surgical Technique: Full-Thickness Excision and Grafting
Deep full-thickness burns (third and fourth degree) require primary full-thickness excision down to viable fascia.
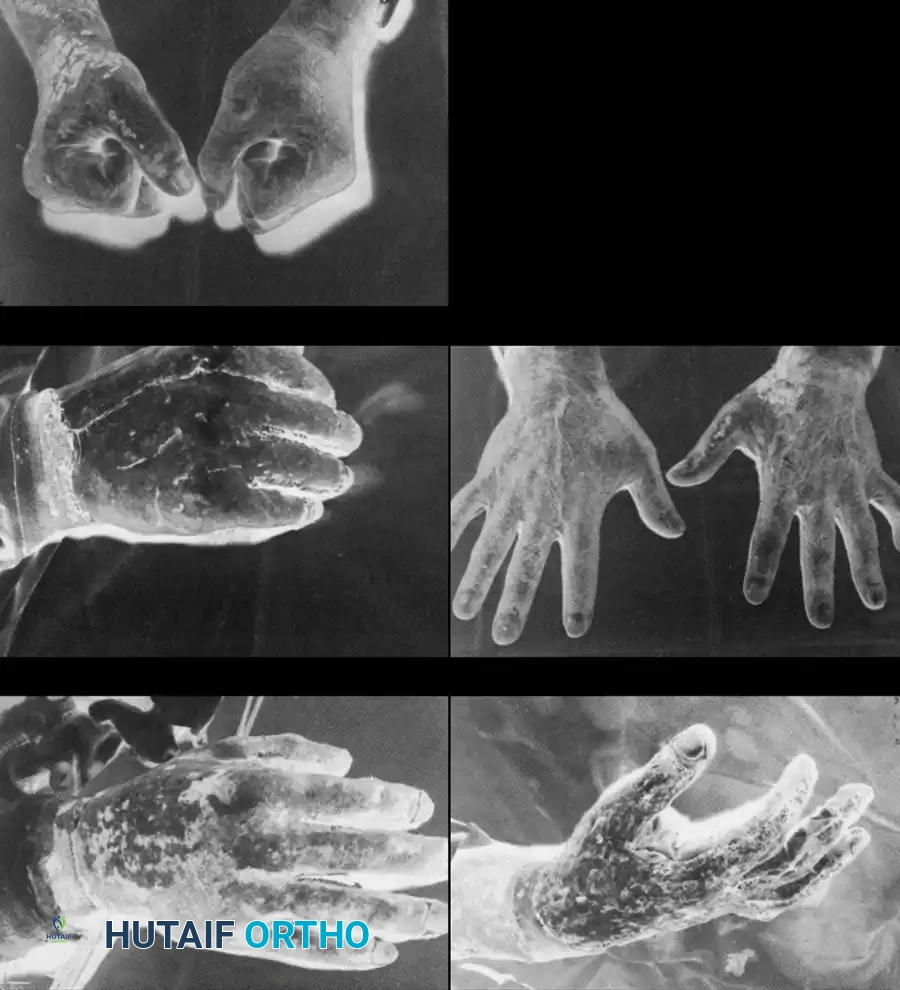
Step-by-Step Procedure
- Excision Depth: Excisional débridement is carried down through the entire layer of necrotic tissue. Dorsally, this typically means excising superficial to the dorsal venous network and the extensor tenosynovium. Volarly, excision proceeds superficial to the flexor tenosynovium and digital neurovascular bundles.
- Management of Deep Structures: If thermal injury has destroyed tendons, nerves, or joint capsules, simple STSG is insufficient. Exposed avascular structures (bone without periosteum, tendon without paratenon) will not support a skin graft.
- Complex Reconstruction: In such severe cases, the surgeon must be prepared to perform stabilization of destroyed joints with Kirschner wires, primary arthrodesis, or the application of local, regional, or free microvascular tissue transfers (e.g., anterolateral thigh flap, lateral arm flap) to provide robust, vascularized coverage.
- Staged Closure: If tissue viability remains questionable after excision, or if excessive bloody oozing precludes immediate grafting, apply a biological dressing (e.g., Biobrane, allograft, or xenograft) and splint the hand. Return to the operating room in 24 to 48 hours for definitive autografting once the wound bed is optimized.
Postoperative Rehabilitation and Splinting
The surgical reconstruction of a burned hand is only the first phase of treatment; an organized, rigorous rehabilitation plan is paramount to success.
Immobilization Phase
Immediately postoperatively, the hand must be immobilized to allow for graft adherence (plasmatic imbibition and subsequent inosculation). The hand is placed in a fiberglass or plaster splint in the Position of Safe Immobilization (Intrinsic-Plus Position):
* Wrist extended 20° to 30°.
* Metacarpophalangeal (MCP) joints flexed 70° to 90° (to maintain collateral ligament length).
* Interphalangeal (IP) joints in full extension (to prevent volar plate contracture).
* Thumb in wide palmar abduction (to maintain the first web space).
Mobilization Phase
Once the graft is fully adherent (typically post-operative day 5 to 7), the splint is converted to a removable orthosis, and active and active-assisted range-of-motion (ROM) exercises are initiated.
The rehabilitation team—comprising hand therapists, occupational therapists, and physical medicine specialists—must focus on:
* Edema Control: Utilizing compressive wraps and elevation.
* Scar Management: Implementing custom-fitted compression garments (e.g., Jobst gloves) once the grafts are stable, worn 23 hours a day for 12 to 18 months to control hypertrophic scarring.
* Dynamic Splinting: To address developing contractures, particularly first web space adduction contractures and PIP joint flexion contractures.
