DEFINITION
Rheumatoid arthritis is a progressive disease that, if uncontrolled, leads to joint destruction, secondary to progressive synovitis, ligament instability, joint dislocation or subluxation, and attrition of adjacent tendons either by bony erosion or direct tenosynovial infiltration.When tendon rupture occurs on the dorsum of the hand or wrist, patients cannot extend their fingers and have difficulty grasping objects.The most common tendon ruptures on the dorsum of the hand begin on the ulnar side and usually are a result of subluxation of the distal radioulnar joint (DRUJ), the so-called Vaughan-Jackson or caput ulnaesyndrome.13On the volar side of the wrist, the most common tendons to rupture are the flexor pollicis longus and the adjacent flexor digitorum profundus (FDP) tendon to the index finger or possibly the long finger. This isreferred to asMannerfelt syndrome.9
ANATOMY
The extensor tendons of the hand and forearm pass beneath the extensor retinaculum at the wrist. The retinaculum is divided into six separate compartments lined by tenosynovium, which can become involved in the pathology of rheumatoid arthritis.The first compartment contains the tendons of the abductor pollicis longus and the extensor pollicis brevis. The former tendon often contains multiple slips, which can contribute to limited space in its respective compartment and secondary de Quervain tenosynovitis.The second compartment consists of the extensor carpi radialis longus (ECRL) and extensor carpi radialis brevis (ECRB), the former tendon inserting at the base of the index metacarpal and the latter at the base of the long finger.The third compartment contains only the tendon of the extensor pollicis longus (EPL), which passes around the tubercle of Lister at a fairly sharp angle. Although frequently involved in tendon ruptures in rheumatoid arthritis, the EPL may also present as an isolated tendon rupture after nondisplaced fractures of the distal radius.The fourth compartment contains the extensor indicis proprius (EIP) and the extensor digitorum communis (EDC), sending tendons from the common extensor muscle in the forearm to each of the fingers. The EIP is a separate muscle tendon unit located within the fourth compartment. It can be differentiated by its distal muscle belly.The fifth extensor compartment contains the extensor digiti quinti (EDQ), often consisting of two slips and passing almost directly over the DRUJ.The sixth compartment contains only the extensor carpi ulnaris (ECU).On the palmar side of the wrist, the flexor pollicis longus is located most radially and passes over the radiocarpal joint adjacent to the trapeziometacarpal joint of the thumb. The flexor pollicis, along with the median nerve and the profundus and sublimis tendons to each digit, passes beneath the deep transverse carpal ligament and represents the contents of the carpal canal.Tenosynovial proliferation can exist within the carpal tunnel, arising from the undersurface of the ligament but more commonly proliferating along the tendons themselves.
PATHOGENESIS
Tendon rupture on the dorsum of the wrist is usually the result of instability in the DRUJ, leading to secondary subluxation and bony erosion through the capsule of the joint and then the tendon.The tendon initially affected is the EDQ. As the carpus supinates and subluxates volarly, causing the distal ulna to be more dorsal, tendons typically rupture sequentially in an ulnar to radial direction.The tendons may also be compromised by direct infiltration from the tenosynovium.Although the ulnar tendons are involved most commonly, it is possible for all of the tendons crossing the dorsum of the wrist to rupture, making reconstruction more difficult.On the volar side of the wrist, the flexor pollicis longus may become compromised through erosion by osteophytes and rough bony surfaces at the level of the trapeziometacarpal joint of the thumb or the scaphotrapezial articulation. The adjacent profundus tendon to the index and, occasionally, the long finger can rupture as well.Tendons of the flexor surface of the wrist and forearm are also subject to rupture via direct tenosynovial infiltration, but this is less common.In addition to tendon attrition and eventual rupture, tenosynovitis in the carpal tunnel may cause median nerve compression that leads to weakness of the median nerve innervated intrinsics. These include the opponens pollicis and abductor pollicis brevis (APB), the flexor pollicis brevis (usually only the deep head), and the radial two lumbricals. Weakness of these muscles is uncommon but should be checked in all patients with carpal tunnel syndrome (CTS).
NATURAL HISTORY
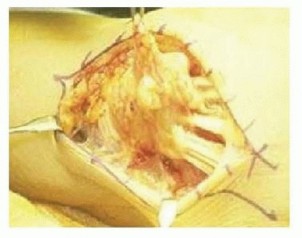
FIG 1 • Exposure of the extensor tendons of the wrist shows proliferative tenosynovitis originating from the tenosynovial lining of the extensor retinaculum. If left unchecked, such proliferative tenosynovitis can contribute to extensor tendon rupture at the level of the wrist.

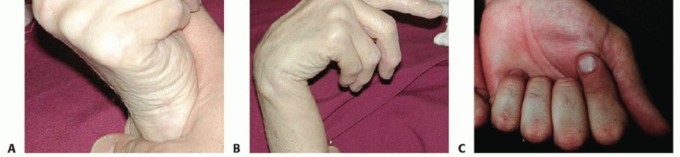
FIG 2 • A. Passive wrist extension results in passive finger flexion with intact finger flexors. B. Passive wrist flexion should result in passive finger extension when the finger extensor tendons are intact. In this situation, however, those tendons are not intact and passive wrist flexion results in the long, ring, and small extensor fingers remaining in a flexed position. C. In a patient with Mannerfelt syndrome, attempted active flexion of the thumb and fingers results in absent flexion of the interphalangeal joint of the thumb and, in this situation, the distal interphalangeal joint of the index finger. Clinically, this is similar to anterior interosseous nerve syndrome and must be distinguished clinically and often by electromyography.
PATIENT HISTORY AND PHYSICAL FINDINGS
Patients often note a spontaneous loss of finger motion, but there may be minimal swelling and discomfort. Patients occasionally report a snap or twinge of discomfort as the tendon ruptures.With an extensor tendon rupture, patients cannot actively extend the metacarpophalangeal (MCP) joints of the involved digit.In the case of isolated rupture of the EDQ, an intact EDC to the small finger may make it difficult to confirm the diagnosis.The proximal and distal interphalangeal joints of the finger may be extended through the intrinsics even when the extensors are ruptured.Wrist flexion should result in MCP joint extension through tenodesis if the extensor tendons are intact. When the finger extensors are ruptured, this tenodesis effect is absent (FIG 2A,B).The patient should also be examined for subluxation of the extensor tendons, which may mimic tendon rupture. In this case, the tendon will subluxate ulnarly to lie between the MCP joints. Patients with subluxation rather than rupture should be able to maintain extended position if the MCP joints are passively extended.On the volar side of the wrist, the examiner should check closely for the possibility of associated tenosynovial proliferation proximal and deep to the transverse carpal ligament.Active digital motion may cause palpable crepitus at this level.Such proliferation may result in coexisting CTS. The examiner should question the patient regarding symptoms of CTS and should assess for signs of CTS.Examination findings suggestive of CTS include decreased sensation or paresthesias in the thumb, index, middle, and radial ring finger; thenar pain; Phalen compression test; and APB weakness.P.787The patient should also be examined carefully for active flexion at the distal interphalangeal joints of the index and long fingers as well as the interphalangeal joint of the thumb.Absence of flexion should alert the surgeon to the possibility of rupture of the flexor pollicis longus and the FDP to the index and occasionally the long finger.These tendons are particularly vulnerable when subluxation and spur formation are present at the trapeziometacarpal or scaphotrapezial joints as well as the volar radiocarpal joint.Tendon rupture at this level is referred to as Mannerfelt syndrome (FIG 2C) and needs to be differentiated from anterior interosseous nerve palsy.Direct pressure on the flexor pollicis longus muscle in the forearm should lead to passive flexion in the interphalangeal joint of the thumb if the tendon is intact.The tenodesis test also is effective for the flexor pollicis longus and profundus and sublimis tendons to the fingers; however, in patients with progressive rheumatoid arthritis, the radiocarpal joint and the interphalangeal joints may become arthritic, making passive motion of the wrist and fingers somewhatmore difficult and therefore the test more unreliable.
IMAGING AND OTHER DIAGNOSTIC STUDIES
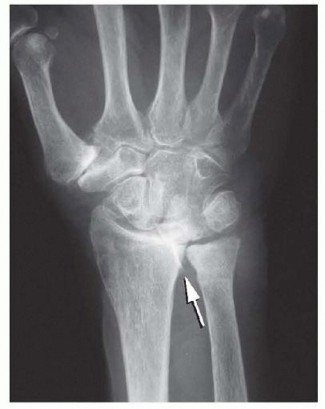
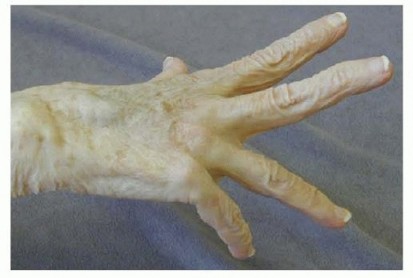
FIG 4 • The clinical consequences of a spur in the DRUJ: rupture of the EDQ and EDC to the ring and small fingers. When the patient attempts to actively extend the fingers, the ring and small fingers remain flexed. (From Lubahn JD, Wolfe TL. Surgical treatment and rehabilitation and tendon ruptures in the rheumatoid hand. In: Mackin EJ, Callahan AD, Skirven TM, et al, eds. Rehabilitation of the Hand and Upper Extremity, ed 5. St. Louis: Mosby, 2002:1598-1607.)Electromyography and nerve conduction studies may be helpful in the evaluation of the patient with potential tendon ruptures, particularly if tenodesis testing is normal in the face of a loss of active finger extension or flexion.Compression of both the anterior interosseous and posterior interosseous nerves can occur in rheumatoid arthritis, usually secondary to ganglion cyst formation at the level of the elbow joint.
DIFFERENTIAL DIAGNOSIS
In the case of tendon ruptures on the dorsum of the hand and wrist, the differential diagnosis is primarily that of posterior interosseous nerve compression or posterior interosseous nerve syndrome.Compression of the posterior interosseous branch of the radial nerve, or the radial nerve itself more proximally, needs to be considered as the cause of the patient's inability to extend the fingers. Careful physical examination of the proximal forearm and elbow is therefore important to include a large cyst, lipoma, radiocapitellar effusion, or other elbow abnormality that may be causing compression of the radial nerve more proximally and leading to muscle paralysis. Electrophysiologic testing may also prove helpful.With respect to Mannerfelt syndrome, absence of flexion at the interphalangeal joint of the thumb and the distal interphalangeal joints in the index and long fingers should be differentiated from the anterior interosseous nerve syndrome, which when present in rheumatoid arthritis is usually due to a large ganglion originating on the volar surface of the elbow.
NONOPERATIVE MANAGEMENT
Nonoperative management probably is more feasible with respect to Mannerfelt syndrome than with the Vaughn-Jackson or caput ulnae syndrome. Although the functional deficit is generally greater with loss of finger extensors than loss of active flexion of the interphalangeal joint of the thumb and distal interphalangealjoints of the index and long fingers, some patients may still function remarkably well.Supportive measures in patients who for one reason or another are not deemed suitable surgical candidates may be provided by a certified hand therapist or occupational therapist able to assist the patient with his or her activities of daily living.P.788With median nerve entrapment and compression from the proliferative tenosynovitis at the level of theradiocarpal joint, disability becomes more progressive and nonsurgical treatment more difficult. There may be a role for corticosteroid injection at the level of the radiocarpal joint, and certainly, referral to a rheumatologist is crucial for the control and management of the disease before any surgical intervention.In the case of wrist or finger extensor tendon rupture, nonsurgical treatment may be beneficial in terms of resting the radiocarpal joint and interphalangeal joints of the fingers to prevent further tendon rupture by attrition. Splinting the wrist or hand may prove beneficial for pain control and to prevent further damage to the joints and soft tissues.Nonoperative management of thenar atrophy may be justified if there is an ulnar innervated deep muscle head of the flexor pollicis brevis to serve as a strong palmar flexor of the thumb. Lack of opposition may be of minimal functional significance, especially in the nondominant hand. If there is lack of sensation, the benefits of opposition transfer will be even smaller. Careful patient selection is critical.
SURGICAL MANAGEMENT
BASIC PRINCIPLES OF TENDON TRANSFER
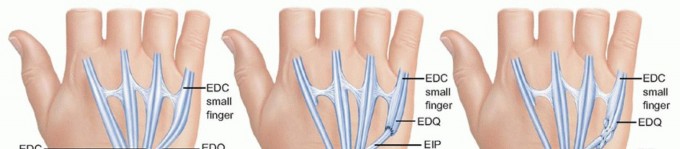
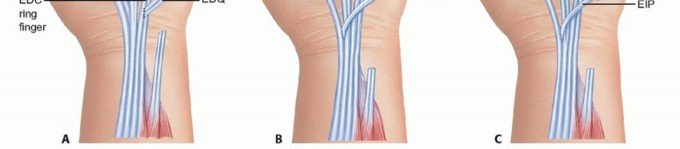
FIG 5 • A. When extensor tendon rupture leads to loss of extension in only one digit, such as the small finger, end-to-side transfer of the distal ruptured tendon to the more proximal adjacent EDC tendon of the ring finger can be performed. B. If the ruptured end is distal to the midmetacarpal region, this transfer may lead to abduction of the small finger metacarpal, and under these circumstances, tendon transfer of the EIP to the distal stump of the EDQ is undertaken (depicted here as an end-to-end transfer). C. EIP to EDQ, depicted here as a Pulvertaft weave between the distal tendon and the proximal transferred EIP. Insensate areas are less likely to benefit from transfer.If diagnosed early, an interposition graft may be used to reconstruct the ruptured tendon.7 The palmaris tendon, a strip of the flexor carpi radialis (FCR), and a slip of the EDQ are suitable choices.Outcomes are similar between tendon transfer and tendon reconstruction with graft. Results correlate inversely with number of fingers involved or chronicity of injury.5
EXTENSOR TENDON RUPTURE
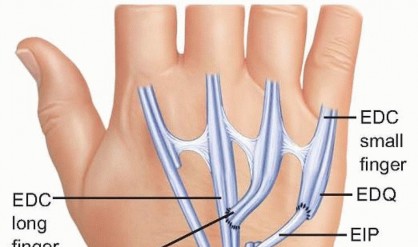
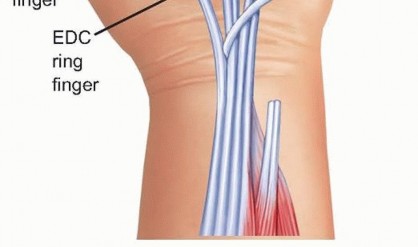
FIG 6 • In cases of double rupture in the ring and small fingers, transfer of the EIP to the distal EDQ, with end-to-side transfer of the distal EDC of the ring finger to the adjacent EDC to the long finger, is a standard transfer.
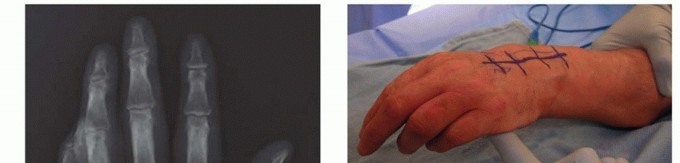
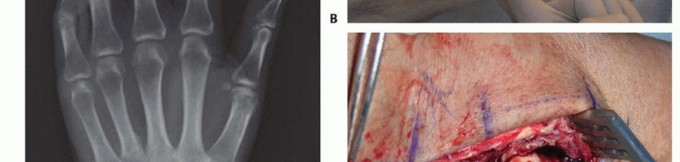
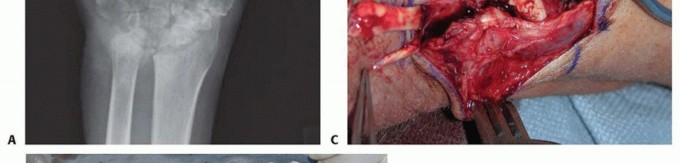
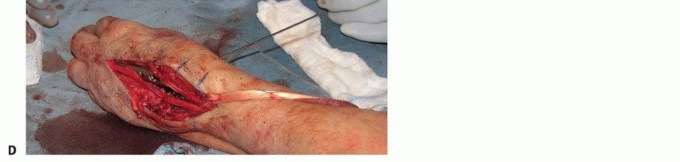
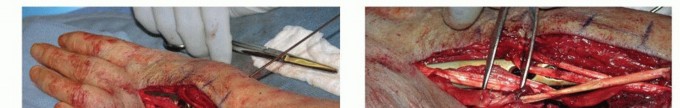
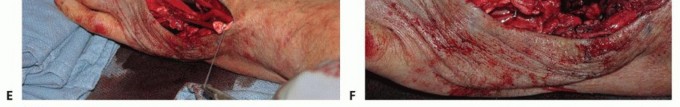
FIG 7 •(continued)E. A suture is first placed at the distal most portion of the FCR before splitting the
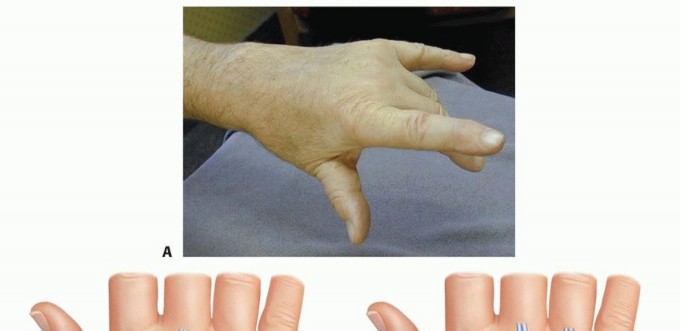
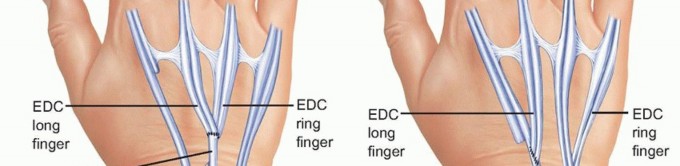
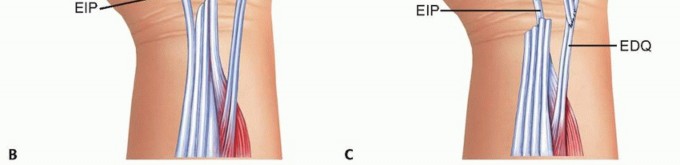
FIG 8 • A. Clinical appearance of a hand with rupture of the EDC to the long and ring fingers. B. Optional tendon transfer when the EDC to the index finger is intact is transfer of the EIP to the distal stumps of the long and ring fingers. C. When the EDC to the index finger has been ruptured and EIP transfer is not an option, transfer of the distal EDC of the long finger to the adjacent EIP of the index and transfer of the distal ring EDC to the adjacent small finger extensor, is shown here. (A: From Lubahn JD, Wolfe TL. Surgical treatment and rehabilitation and tendon ruptures in the rheumatoid hand. In: Mackin EJ, Callahan AD, Skirven TM, et al, eds. Rehabilitation of the Hand and Upper Extremity, ed 5. St. Louis: Mosby, 2002:1598-1607; B,C: From Williams DP, Lubahn JD. Reconstruction of extensor tendons. Atlas Hand Clin 2005;10:209-222.)
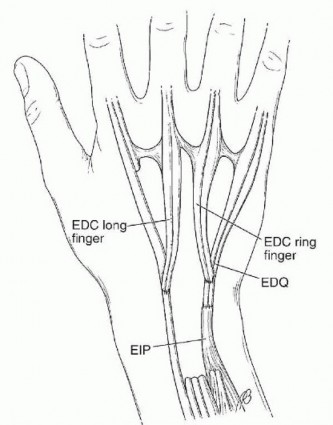
FIG 9 • Rupture of the common extensors to the long, ring, and small fingers with extensor digiti quinti
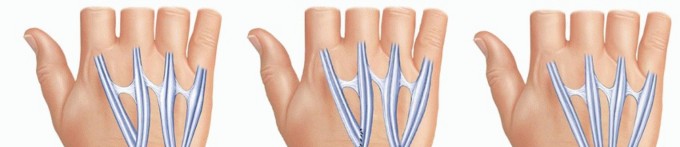
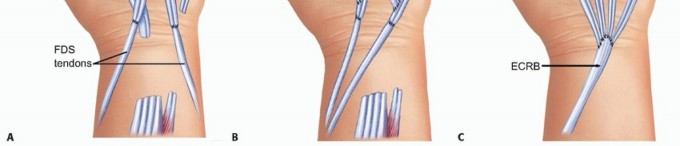
FIG 10 • A. Rupture of all four finger extensors may be treated alternatively with transfer of the flexor digitorum superficialis (FDS) to the long and ring fingers, harvested in the distal palm and transferred around the radius and ulna, with the two forearm bones serving as pulleys for the transferred tendon. B. Alternatively, both FDS tendons may be transferred around the radial side of the forearm and sutured to the distal stumps of the EDC tendons. C. With rupture of all common extensor tendons to the fingers as well as the EIP and the EDQ, extension may be restored through transfer of one of the radial wrist extensors. This is ideal when a partial wrist fusion is being planned, as shown.
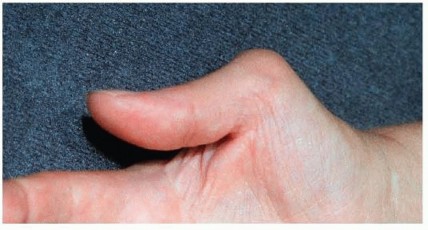
FIG 11 • Extensor pollicis brevis rupture. Boutonnière deformity of the thumb (Nalebuff type I). Chronic synovitis at the thumb MCP joint may lead to attritional rupture of the dorsal capsule and the extensorpollicis brevis.This boutonnière deformity of the thumb is a type I as described by Nalebuff10 and Nalebuff and Millender11 (FIG 11).The deformity usually progresses after extensor pollicis brevis rupture. The EPL shifts ulnarly, the collateral ligaments weaken, and the thumb metacarpal becomes abducted radially. The interphalangeal joint hyperextends as a reciprocal response to the MCP joint flexion.Transfer of the EPL to the extensor pollicis brevis insertion in the base of the proximal phalanx and the dorsal capsule of the MCP joint of the thumb is performed. Local anesthesia is typically adequate.
FLEXOR TENDON RUPTURE
Tendon transfer for the treatment of flexor tendon disruption in the rheumatoid patient is much less common than for extensor tendon rupture.Mannerfelt syndrome should be treated by transfer of the brachioradialis tendon to the flexor pollicis longus.Associated disruption of a FDP tendon is usually treated by transferring the distal stump end to side to the adjacent digit's FDP tendon.
LACK OF OPPOSITION
Lack of opposition function may cause minimal functional deficit in patients with advanced rheumatoid arthritis. Many patients may be managed conservatively.If chronic CTS is the underlying cause, division of the transverse carpal ligament in combination with tenosynovectomy (as in open carpal tunnel release) will alleviate median nerve compression.If intrinsic wasting is already present, however, decompression of the median nerve may not restore thenar function.Consideration should thus be given to simultaneous tendon transfer to restore opposition at the time of carpal tunnel decompression in the setting of intrinsic weaknessRecovery of opposition after carpal tunnel release will be delayed in the best of cases. Tendon transfer provides rapid return of function and so should be considered in most patients.A variety of tendon transfers may be used to restore opposition. These include the palmaris longus,3 EIP, FDS, and abductor digiti minimi.8If performed at the same time as carpal tunnel release, the palmaris longus transfer is preferred, as it is done through the same incision and has minimal extra morbidity.Otherwise, transfer of the extensor indicis is reliable, has minimal morbidity, and has the most reliable pulley (ulnar border of the wrist).FDS transfer is also very reliable. It has two main drawbacks. Sacrifice of a FDS tendon may decrease grip strength. Donor site morbidity including swan-neck deformity or flexion contracture of the proximal interphalangeal joint may occur. Women tend to be more at risk for the former and men the latter. Donor site morbidity may be minimized by not removing the tendon portion distal to the A1 pulley.A variety of insertion sites may be used. Typically, the tendon is sutured to the APB tendon using a Pulvertaft weave. Suture anchors or a bone tunnel may also be used.Additional insertions have been described including the proximal phalanx, the extensor mechanism, or dorsal capsule. A portion of the tendon may also be used to reconstruct the collateral ligament. This allows the tendon transfer to restore additional functions including thumb MCP extension or stability. In these cases, a dual insertion is generally performed, with the tendon being attached to the APB tendon as well as a second location. This second insertion may weaken tendon transfer function and is generally unnecessary unless there is additional deficit of the thumb (eg, extensor pollicis brevis dysfunction or collateral ligament insufficiency).
PREOPERATIVE PLANNING
All patients with rheumatoid arthritis require a thorough general physical examination as well as careful evaluation of their cervical spine, including posteroanterior and lateral radiographs, often with flexion and extension views to evaluate cervical spine instability.Limited joint mobility is a contraindication to tendon transfer.Directed therapy may be used to improve contracture.For example, brachioradialis tendon transfer to the flexor pollicis longus is an ideal transfer and is likely to yield an excellent result but only if there is adequate passive motion at the interphalangeal joint and MCP joint as well as the basal joint and the thumb. If these joints are stiff, the brachioradialis might be better saved for other needs as the patient's arthritis progresses.With lack of opposition, the thumb metacarpal will be adducted and supinated. Contracture of the first web space may also be present. Intraoperatively, web space contracture may be treated by release of the fascia of adductor pollicis and first dorsal interosseous. The skin may be lengthened by skin graft, flap, or Z-plasty. Severe contractures may require metacarpal base osteotomy or trapeziectomy.The carpus should be examined for stability. In particular, the DRUJ on the ulnar side of the wrist should be checked for dorsal instability and subluxation and the volar radial side of the wrist for palmar subluxation.Planning needs to take into consideration the results of preoperative radiographs of the wrist, hand, and cervical spine as well as electromyographic tests.If the findings on electromyography are negative and the surgeon is certain that tendon rupture is responsible for the lack of active finger motion, plans should be made to transfer expendable existing tendons to those thatP.793have ruptured. In the case of multiple extensor tendon ruptures to the fingers, the ECRL and the FDS from the long and ring fingers are two of the most common donor tendons.If radiographs reveal significant joint destruction and instability, appropriate arthrodesis or arthroplasty should be considered rather than tendon transfer.Instruments designed for tendon weaves are extremely valuable.Sharp tendon passers facilitate a Pulvertaft weave. When sharp, pointed tendon passers are not available, a no. 11 blade can be passed through the tendon followed by a hemostat to grasp the knife and guide the hemostat through the tendon. The hemostat then grasps the transferred tendon, weaving it through the recipient tendon.3-0 and 4-0 braided nonabsorbable sutures on appropriate needles are recommended for tendon repairs.
POSITIONING
Most tendon transfers are done with the patient in the supine position on the operating table.The contralateral arm or lower extremity may be sterilely draped in the event that a tendon graft is needed.Anesthesia may be either general or an axillary block, depending on the patient's preference and the stability of the cervical spine.Although isolated carpal tunnel release may be performed under local anesthesia, carpal tunnel release combined with palmaris longus opponensplasty requires block or general anesthesia.
TECHNIQUES
EXTENSOR INDICIS PROPRIUS TENDON TRANSFER
Flexor Carpi Radialis Tendon Transfer for Finger Extension Flexor Digitorum Superficialis Tendon Transfer for Finger Extension
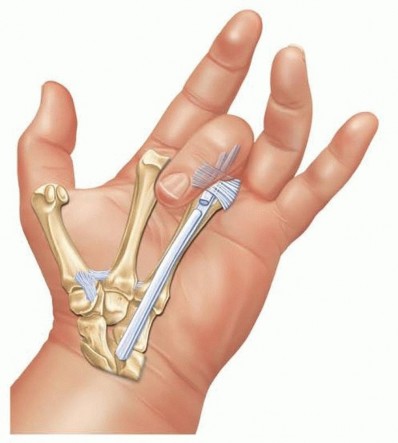
TECH FIG 1 • Transfer of the FDS to the long and ring fingers. The distal incision in the palm is used to isolate the sublimis tendon as far distal as possible by flexing the finger so that the chiasm of Camper is visible in the wound. The tendon is divided just proximal to the chiasm, leaving enough distal tendon to contribute to the stability of the proximal interphalangeal joint in extension and thereby avoiding a secondary instability of that joint and possible swan-neck deformity.
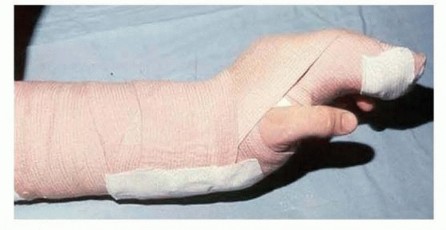
TECH FIG 2 • The ideal splint for transfer to the extensor tendons of the finger immobilizes the wrist in the so-called safe position. With wrist extension, tension at the site of transfer is usually minimal. Finger flexion at the MCP joint is ideal to prevent scarring of the collateral ligaments and secondary loss of finger flexion. The amount of flexion possible is judged in the operating room by passive flexion of the finger until a minimum amount of tension is seen at the repair site. (From Williams DP, Lubahn JD. Reconstruction of extensor tendons. Atlas Hand Clin 2005;10:209-222.)
Extensor Carpi Radialis Longus or Brevis Transfer Brachioradialis Tendon Transfer (Reconstruction of Mannerfelt Syndrome)
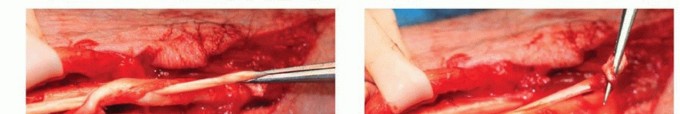
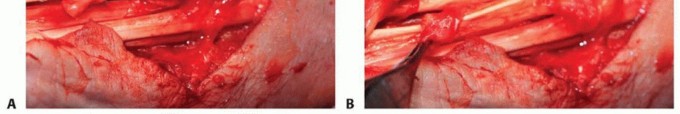
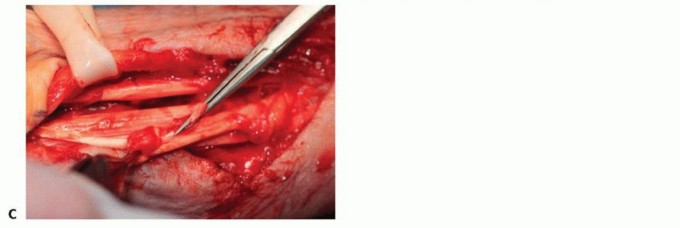
TECH FIG 3 • A,B. Pulvertaft weave shown sequentially as a sharp tendon passer is used to puncture the tendon through and through and then grasp the tendon being transferred and weave it through the recipient tendon. C. The transfer is secured at each weave with one or two nonabsorbable braided nylon sutures. (From Lubahn JD, Wolfe TL. Surgical treatment and rehabilitation and tendon ruptures in the rheumatoid hand. In: Mackin EJ, Callahan AD, Skirven TM, et al, eds. Rehabilitation of the Hand and Upper Extremity, ed 5. St. Louis: Mosby, 2002:1598-1607.)
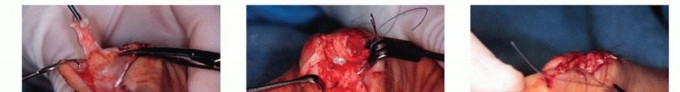
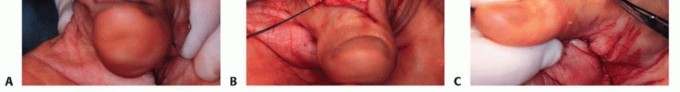

TECH FIG 4 • Extensor pollicis brevis rupture. A,B. Tendon transfer of the EPL proximally to the site of insertion of the extensor pollicis brevis, allowing the hyperextended interphalangeal joint to drop into a more flexed position and allowing active extension at the level of the MCP joint. C,D. EPL is anchored through drill holes to the base of the proximal phalanx. (From Lubahn JD, Wolfe TL. Surgical treatment and rehabilitation and tendon ruptures in the rheumatoid hand. In: Mackin EJ, Callahan AD, Skirven TM, et al, eds. Rehabilitation of the Hand and Upper Extremity, ed 5. St. Louis: Mosby, 2002:1598-1607.)
Flexor Digitorum Superficialis Opposition Transfer(TECH FIG 5A-F)
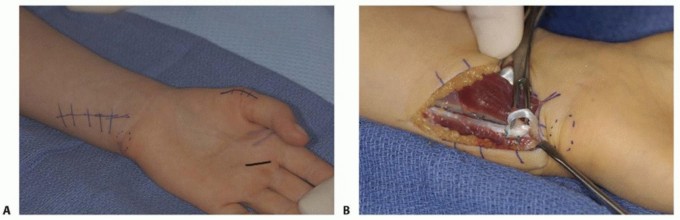
TECH FIG 5 • Flexor digitorum superficialis transfer. A. The skin markings are at the distal palmar crease (middle finger was used in this patient only because the ring finger FDS had been previously used), radial thumb, and ulnar forearm. B. Through the forearm incision, a portion of FCU is used to create a pulley.(continued)
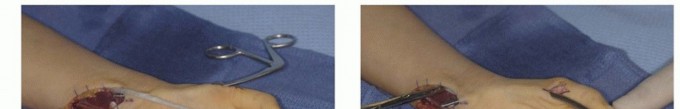
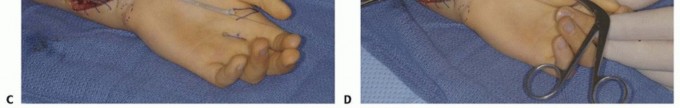

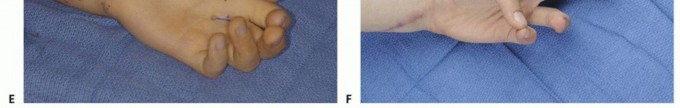
TECH FIG 5 •(continued)C,D. After dividing the superficialis tendon in the distal palm and drawing it into forearm, a tunnel is made from the thumb to forearm. E. The tendon graft is then passed through the FCU loop and the subcutaneous tunnel to its point of attachment at the thumb. F. Excellent opposition was restored in this patient.
Palmaris Longus Opposition Transfer
Preoperatively, confirm presence of the palmaris longus by physical examination. Because the tendon is not long enough to reach the thumb, it is augmented by including a strip of the palmar fascia.
A longitudinal incision is made from the proximal palmar crease to the forearm. The palmar cutaneous branch of the median nerve arises radial to the palmaris longus tendon and should be identified and protected. After division of the skin, a 1-cm band of the palmar fascia is removed in continuity with the palmaris longus tendon. This additional tissue provides the length required for the palmaris longus to reach the thumb. This will also accomplish the carpal tunnel release. The tendon is then freed from the forearm to palm.
A second incision is made on the radial aspect of the thumb MCP joint. A subcutaneous tunnel is made between this and the forearm incision.
The tendon with attached fascia is passed from the forearm to second incision. It is inserted into the APB tendon with a weave.
The transfer is tensioned with the thumb in full opposition, MCP joint in full extension, and wrist in neutral.
A thumb spica cast is worn for 4 weeks and then transitioned to a removable splint.Extensor Indicis Proprius Transfer for Lack of Opposition
The EIP tendon is obtained as in the section Extensor Indicis Proprius Tendon Transfer and passed around the ulnar side of the distal dorsal forearm.
A second incision is made along the radial aspect of thumb MCP joint.
A subcutaneous tunnel is around the ulnar border of the wrist from the dorsal forearm incision to this second incision. Care should be taken to not entrap or damage the ulnar neurovascular bundle. This can be done by staying superficial to the FCU. This task is made easier by making an additional small incision proximal to the pisiform. The tendon is first passed into this incision, then a second time across the palm.
The EIP is passed around the ulnar side of the wrist through the tunnel and inserted into the APB tendon with a weave.
The transfer is tensioned with the thumb in full opposition and the wrist in slight flexion.
A thumb spica cast is worn for 4 weeks and then transitioned to a removable splint.
P.798
PEARLS AND PITFALLS
PALMARIS LONGUS OPPOSITION TRANSFER
Extensor Indicis Proprius Transfer for Lack of Opposition
|||EIPharvest|1. Obtain the EIP transfer by tracing the ulnar most inserting tendon in the MCP joint region of the index finger proximally at the level of the wrist. In a certain percentage of patients, the ulnar most tendon is in fact the EDC rather than the EIP. The EIP, however, is always the deeper, more volar tendon at the level of the wrist. Tracing this independent muscle tendon unit from the wrist to the index finger MCP joint will help assure the surgeon that the correct tendon is being released for transfer.2. Distal repair of the dorsal apparatus at the site of EIP harvest is somewhat controversial. Although some experts recommend repair, others feel confident that the|EDQtransfers|1. Sufficient length of the distal segment of the EDQ should be available to allow tendon transfer to the adjacent EDC without abducting the small finger. If this transfer is tight, the side-to-side transfer of EDQ to the EDC of the ring finger should be abandoned and tendon transfer to the EIP or another suitable donor pursued.---|---Unstable DRUJ|1. At the time of tendon transfer, inspect the DRUJ to be certain that any osteophytes have been débrided and a localized flap rotated to cover the exposed bone created. If the DRUJ is deemed unstable, transfer of the pronator quadratus dorsally may be used to stabilize the distal ulna.Suturing|1. When suturing tendon grafts at the site of tendon weave (ie, where a graft or transfer is passed through another tendon), one or two sutures should be sufficient. Take care that the needle does not pass through the tendon near the thread from another suture. If this occurs, the suture is weakened or possibly cut in two by the needle and the graft or transfer is predisposed to rupture. Cutting needles should never be used, as they place both the suture and the tendon at risk.Tendon transfer|1. Ensure adequate size of tunnel for passage of tendon.2. When passing tendons from one compartment to another, make sure to pull in line with the tendon instead of up and out of the wound, as this may avulse the tendon. This may be accomplished by “winding” the tendon using an Allis retractor placed into the wound.3. Avoid passing tendon through scarred areas.4. Avoid surgery in the setting of open wounds.5. Full range of motion should be obtainedpriorto transfer.defect can be left with no risk of extensor lag. The surgeon needs to be aware of thepotential risk of extensor lag, and we recommend attention to the defect by suture repair.
POSTOPERATIVE CARE
Postoperative care for each of these tendon transfers is similar.In the case of tendon transfer to restore loss of finger extensors, the hand and wrist are immobilized with the wrist extended about 40 degrees. More may be desirable in certain instances, but too much extension could damage already fragile joints.The MCP joints are brought into flexion until tension is noted at the suture line. Forty degrees or more is ideal to maintain the desired length of the collateral ligaments and prevent MCP joint extension contractures.Immobilization is continued for 3.5 to 4 weeks, and gentle active motion is begun, maintaining the hand in a splint for protection.At 6 weeks, some resistive exercises may be added to the program. By 12 weeks, the patient should be able to resume normal activities.In the case of flexor tendon rupture, the hand and wrist are immobilized with the wrist in 60 degrees of flexion,the MCP joints in 40 degrees of flexion, and the interphalangeal joints allowed to extend until tension is noted at the suture line. Immobilization is continued for 6 weeks, at which time a gentle active range-of-motion program is begun without resistance.At 12 weeks, resistive exercises are added and the patient is permitted to gradually resume normal activity.In the case of opposition transfer, the thumb is immobilized in full opposition and the wrist in neutral to slight flexion. A thumb spica cast is worn for 4 weeks and then transitioned to a removable splint.
OUTCOMES
Outcomes in tendon transfer surgery in rheumatoid arthritis are highly dependent on the patient's medical condition and ability to cooperate with the postoperative splinting and rehabilitation program. Most patients who are supervised by a therapist achieve a better result than those who try to make it on their own.With good medical management of rheumatoid arthritis, when the disease is well controlled, and in cooperative patients who are motivated to improve, good results should be expected.Tendon transfer should always be delayed in patients with active disease, as results will be poor.The only surgical procedure to be performed in poorly controlled patients is synovectomy and with the caveat that success hinges on eventual good medical control of the disease.Outcomes correlate inversely with the number of ruptured tendons and chronicity of injury.5
COMPLICATIONS
InfectionSkin or surgical wound breakdown Attenuation of the transferred tendon Rerupture of the tendonsLoss of motion due to improper tensioning of the transferred tendon Joint stiffnessP.799
REFERENCES
- Boyes JH. Bunnell's Surgery of the Hand, ed 5. Philadelphia: JB Lippincott, 1970.
- Breen TF. Jupiter JB. Extensor carpi ulnaris and flexor carpi ulnaris tenodesis of the unstable distal ulna. J Hand Surg Am 2012;14: 612-617.
- Camitz H. Surgical treatment of paralysis of opponens muscle of thumbs. Acta Chir Scand 1929;65:77-81.
- Chetta MD, Ono S, Chung KC. Partial extensor carpi radialis longus turn-over tendon transfer for reconstruction of the extensor pollicis longus tendon in the rheumatoid hand: case report. J Hand Surg Am2012;37:1217-1220.
- Chung US, Kim JH, Seo WS, et al. Tendon transfer or tendon graft for ruptured finger extensor tendons in rheumatoid hands. J Hand Surg Eur Vol 2010;35:279-282.
- Davis TR. Median and ulnar nerve palsy. In: Wolfe SW, Hotchkiss RN, Pederson WC, et al, eds. Green's Operative Hand Surgery, vol 2, ed 6. Philadelphia: Elsevier, 2011:1093-1137.
- Hamlin C, Littler JW. Restoration of the extensor pollicis longus tendon by an intercalated graft. J Bone Joint Surg Am 1977;59(3):412-414.
- Littler JW, Cooley SG. Opposition of the thumb and its restoration by abductor digiti quinti transfer. J Bone Joint Surg Am 1963;45: 1389-1396.
- Mannerfelt L, Norman O. Attrition ruptures of flexor tendons in rheumatoid arthritis caused by bony spurs in the carpal tunnel: a clinical and radiological study. J Bone Joint Surg Br 1969;51(2):270-277.
- Nalebuff EA. Diagnosis, classification and management of rheumatoid thumb deformities. Bull Hosp Joint Dis 1968;29:119-137.
- Nalebuff EA, Millender LH. Surgical treatment of the boutonniere deformity in rheumatoid arthritis. Orthop Clin North Am 1975;6: 753-763.
- Pulvertaft RG. Tendon grafts for flexor tendon injuries in the fingers and thumb: a study of technique and results. J Bone Joint Surg 1956;38B:175-194.
- Vaughan-Jackson OJ. Rupture of extensor tendons by attrition at the inferior radio-ulnar joint: report of two cases. J Bone Joint Surg Br 1948;30B(3):528-530.
- Williamson SC, Feldon P. Extensor tendon ruptures in rheumatoid arthritis. Hand Clin 1995;11:449-459.
